Introduction & Epidemiology
Erosive osteoarthritis (EOA), also known as inflammatory osteoarthritis or generalized nodal osteoarthritis, is a distinct phenotype of osteoarthritis characterized by periods of acute inflammation, synovial proliferation, and rapid cartilage loss, often with subchondral bone erosions. While classic osteoarthritis (OA) typically involves gradual cartilage degeneration, EOA exhibits an aggressive, inflammatory component leading to more pronounced joint destruction and often greater pain and functional impairment. The index finger proximal interphalangeal (PIP) joint is a frequently affected site, presenting unique diagnostic and management challenges given its critical role in prehension and fine motor tasks.
Epidemiologically, EOA predominantly affects middle-aged and older women, with a female-to-male ratio ranging from 5:1 to 12:1. The onset typically occurs between the fourth and sixth decades of life. Its prevalence is estimated to be between 1-5% in the general population, although specific studies on hand OA may show higher rates among those with symptomatic disease. A familial predisposition has been suggested, indicating a genetic component, though specific genetic markers are still under investigation. The index finger PIP joint, due to its involvement in power grip and pinch activities, is particularly susceptible to the mechanical stresses that, when coupled with the inflammatory process of EOA, can lead to significant morbidity. Characteristic radiographic findings include central erosions (often termed "gull-wing deformity"), joint space narrowing, subchondral sclerosis, and osteophyte formation. The inflammatory episodes can mimic seronegative inflammatory arthritis, necessitating careful differential diagnosis.
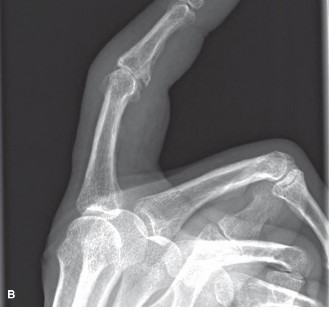
Figure 1: Radiographic presentation of erosive osteoarthritis of the PIP joint, demonstrating classic "gull-wing" deformity with central erosion and peripheral osteophytes.
Surgical Anatomy & Biomechanics
The proximal interphalangeal joint of the index finger is a diarthrodial hinge joint formed by the head of the proximal phalanx and the base of the middle phalanx. Its stability and function are critically dependent on a complex interplay of osseous congruity and soft tissue restraints.
Osseous Anatomy
- Proximal Phalanx Head: Features two condyles separated by an intercondylar groove, articulating with corresponding depressions in the middle phalanx base. The condyles are slightly spool-shaped, providing inherent collateral stability.
- Middle Phalanx Base: Contains two concave fossae separated by a sagittal ridge, which engages the intercondylar groove of the proximal phalanx. The articular surface is broader dorsally than volarly, facilitating greater extension than flexion range of motion when fully congruent.
Ligamentous Structures
-
Collateral Ligaments:
Comprise true collateral ligaments and accessory collateral ligaments.
- True Collateral Ligaments: Originate from the sides of the proximal phalanx head, dorsal to its axis of rotation, and insert into the lateral aspects of the middle phalanx base and the lateral bands of the extensor mechanism. These ligaments are taut in flexion and relaxed in extension, contributing significantly to mediolateral stability, particularly at 30-45 degrees of flexion.
- Accessory Collateral Ligaments: Originate volarly to the true collaterals and insert into the volar plate. These are taut in extension and relaxed in flexion.
- Volar Plate: A strong, fibrocartilaginous structure located on the volar aspect of the joint. It originates proximally from the proximal phalanx (meniscoid attachments) and inserts distally into the middle phalanx base. It prevents hyperextension and provides significant volar stability. Its paired check-rein ligaments (collateral ligament extensions) anchor it to the proximal phalanx.
Extensor Mechanism
The extensor mechanism over the PIP joint is formed by the confluence of the central slip of the extensor digitorum communis and the lateral bands from the intrinsic muscles (lumbricals and interossei).
*
Central Slip:
Inserts onto the dorsal base of the middle phalanx, directly extending the PIP joint.
*
Lateral Bands:
Pass laterally to the PIP joint, converging distally to form the terminal tendon that inserts onto the distal phalanx, extending the DIP joint. The triangular ligament stabilizes the lateral bands dorsally, while the oblique retinacular ligament courses volarly to the PIP axis, connecting the flexor sheath to the terminal extensor tendon.
Flexor Tendons
The flexor digitorum superficialis (FDS) tendon inserts onto the middle phalanx, providing primary PIP flexion. The flexor digitorum profundus (FDP) tendon passes through the split FDS, inserting onto the distal phalanx, flexing both the PIP and DIP joints. The fibrous flexor sheath provides critical containment for these tendons.
Biomechanics of EOA
In EOA, the inflammatory process leads to active chondrolysis and subchondral bone erosion, often centrally, resulting in the characteristic "gull-wing" deformity. This central collapse disrupts the normal joint congruity and alters load distribution. Synovial hypertrophy and inflammation contribute to joint effusions, capsular distension, and potentially ligamentous laxity or contracture. Osteophyte formation at the joint margins, a compensatory response, can restrict motion, contribute to pain through impingement, and further distort joint mechanics. The index finger PIP joint's role in forceful pinch and grip exacerbates these changes, leading to increased pain, stiffness, deformity (e.g., flexion contracture, lateral deviation), and functional disability. The intrinsic muscles can become imbalanced, further contributing to progressive deformity.
Indications & Contraindications
Management of erosive osteoarthritis of the index finger PIP joint follows a staged approach, progressing from conservative measures to surgical intervention when symptoms persist or worsen despite appropriate non-operative care.
Non-Operative Indications
Initial management focuses on pain control, reduction of inflammation, and preservation of function.
*
Early disease:
Minimal joint destruction, mild to moderate pain, preserved range of motion, and absence of significant deformity.
*
Acute flares:
Intense pain and swelling during inflammatory episodes.
*
Patient preference:
For patients who wish to avoid surgery or are not surgical candidates.
*
Contraindications to surgery:
Uncontrolled medical comorbidities, active infection, or unrealistic patient expectations.
Operative Indications
Surgical intervention is considered when non-operative measures fail to provide adequate relief from pain, or when significant functional impairment or deformity develops.
*
Persistent severe pain:
Localized to the PIP joint, refractory to conservative management (NSAIDs, splinting, injections, therapy).
*
Progressive joint destruction:
Documented radiographic progression of cartilage loss and subchondral erosions despite conservative treatment.
*
Significant loss of function:
Inability to perform activities of daily living (ADLs) or occupational tasks due to stiffness, weakness, or pain.
*
Fixed deformity:
Such as a significant flexion contracture (>30 degrees), lateral deviation, or rotational deformity that impairs function and cannot be corrected by therapy.
*
Instability:
Severe laxity leading to subluxation or dislocation.
*
Failed previous surgical interventions:
Revision surgery may be indicated.
Contraindications
Absolute contraindications for most elective surgical procedures include active local or systemic infection, severe uncontrolled medical comorbidities precluding safe anesthesia and recovery, and insufficient soft tissue coverage or bone stock. Relative contraindications include poorly controlled diabetes, smoking, severe peripheral vascular disease, and patients with unrealistic expectations regarding surgical outcomes. Specific to PIP joint surgery, patients heavily reliant on grip strength in other digits may be better candidates for arthrodesis, whereas those prioritizing some degree of motion may opt for arthroplasty. For arthroplasty, insufficient bone stock or severe collateral ligament instability may contraindicate implant use.
| Indication Category | Operative Management | Non-Operative Management |
|---|---|---|
| Pain | Severe, persistent pain refractory to conservative care; pain limiting ADLs/work | Mild to moderate pain; acute inflammatory flares; pain responsive to conservative measures |
| Deformity | Fixed flexion contracture (>30 degrees); significant lateral deviation/rotational deformity; instability | Mild, flexible deformities; no functional limitation |
| Function | Significant loss of grip/pinch strength; inability to perform ADLs/occupational tasks | Minimal functional impairment; preserved range of motion |
| Radiographic | Advanced joint space narrowing, subchondral collapse, severe erosions, osteophytes with impingement | Early-to-moderate joint space narrowing; no significant erosions or collapse; absence of osteophyte impingement |
| Failed Tx | Failure of ≥3-6 months of comprehensive non-operative treatment | Initial presentation; patients initiating conservative therapy |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is essential for successful outcomes in PIP joint surgery for EOA.
Pre-Operative Evaluation
- Clinical Assessment: Detailed history of pain characteristics (intensity, duration, aggravating/alleviating factors), functional limitations, previous treatments and their efficacy. Physical examination should assess range of motion (active and passive), stability (collateral ligaments, volar plate), presence of fixed deformities, and neurovascular status.
-
Imaging:
- Standard Radiographs: Posteroanterior (PA), lateral, and oblique views of the hand are crucial. These will reveal joint space narrowing, osteophyte formation, subchondral sclerosis, characteristic central erosions ("gull-wing" deformity), cysts, and any subluxation or deformity.
- Stress Views: May be useful to assess instability if suspected.
- Advanced Imaging (MRI/CT): Rarely necessary but can be considered for complex cases, occult fractures, or to better delineate bone loss or soft tissue pathology. MRI can characterize synovial inflammation and cartilage integrity, which may inform the choice between synovectomy, debridement, arthroplasty, or arthrodesis.
- Patient Selection & Counseling: Discuss surgical options (arthrodesis vs. arthroplasty), their respective benefits (motion vs. stability/strength), risks (infection, non-union, implant failure, stiffness), and expected outcomes. Factors influencing the choice include patient age, activity level, functional demands, status of adjacent joints (DIP, MCP), and the severity of bone loss. For the index finger, stability and pinch strength are paramount, often favoring arthrodesis or a robust arthroplasty design.
- Anesthesia: Regional anesthesia (e.g., axillary block) combined with monitored anesthesia care (MAC) or general anesthesia is typically employed. A tourniquet is used for a bloodless field.
- Equipment: Ensure availability of appropriate instrumentation for small joint surgery, including osteotomes, rongeurs, curettes, K-wires, micro-oscillating saw, specialized plates and screws for PIP arthrodesis (e.g., mini-fragment plates), and implant components for arthroplasty (silicone, pyrocarbon, or total joint systems) if selected.
Patient Positioning
The patient is typically positioned supine on the operating table. The affected arm is abducted on a hand table, ensuring comfortable positioning and stable support.
*
Hand Position:
The hand is prepared and draped to allow full access to the dorsal, volar, and lateral aspects of the index finger. The fingers should be freely movable for intraoperative assessment of motion and alignment.
*
Tourniquet:
A pneumatic tourniquet is applied to the upper arm and inflated after exsanguination to create a bloodless field, crucial for precise dissection and visualization of small structures.
Detailed Surgical Approach / Technique
The choice between arthrodesis (fusion) and arthroplasty (joint replacement) depends on the patient's functional demands, pain levels, and the surgeon's assessment of joint pathology and stability. For the index finger PIP, given its crucial role in pinch and grip, stability is often prioritized.
Arthrodesis of the PIP Joint
Arthrodesis provides a stable, pain-free joint at the expense of motion. It is often preferred for the index finger due to the high demands placed on pinch stability.
Surgical Approach
- Incision: A dorsal longitudinal incision, slightly curvilinear or lazy-S to avoid scar contracture, centered over the PIP joint. Alternatively, a transverse elliptical incision can be used to excise excess skin and facilitate exposure.
- Dissection: Careful dissection through subcutaneous tissue, identifying and protecting dorsal digital nerves and veins.
- Extensor Mechanism: The central slip of the extensor digitorum communis tendon is sharply divided longitudinally, or a transverse U-shaped flap is raised and reflected proximally and distally, to expose the joint capsule. Alternatively, a lateral approach can be used, mobilizing the extensor mechanism subperiosteally off one side of the joint.
- Capsulotomy & Exposure: The dorsal joint capsule is incised longitudinally to expose the articular surfaces of the proximal phalanx head and middle phalanx base. Osteophytes are resected using osteotomes or rongeurs.
- Articular Surface Preparation: The remaining articular cartilage and subchondral bone are thoroughly denuded from both the proximal phalanx head and the middle phalanx base, exposing bleeding cancellous bone. This can be achieved with a small osteotome, rongeur, or burr. The goal is a broad, raw bony surface for fusion.
-
Bone Resection & Shaping:
To achieve optimal bone-to-bone contact, the joint surfaces are typically prepared using either a flat-cut or conical-cut technique.
- Flat Cut: Parallel resection of bone from the proximal phalanx head and middle phalanx base using an oscillating saw. This maintains bone length but may require slight compression.
- Conical Cut: Resection of opposing concave and convex surfaces, aiming for maximum surface area contact and inherent stability. This may be performed freehand or with specialized jigs. This technique often provides excellent primary stability.
- Desired Fusion Angle: The index PIP joint is typically fused in 30-45 degrees of flexion. This angle allows for optimal object manipulation, pinch, and grip without interfering with adjacent digits. For the index finger, a slightly more extended position (30-35 degrees) may be preferred to facilitate lateral pinch.
-
Fixation: Various methods can be used, aiming for rigid internal fixation to promote fusion and allow early mobilization of adjacent joints.
- K-wires: Two or three parallel or crossed K-wires (0.035 or 0.045 inch) can provide adequate fixation, especially if complemented by a tension band wire. This is a simpler method but provides less rigid fixation.
- Small Plate and Screws: A dorsal mini-fragment plate (e.g., 1.5mm or 2.0mm system) applied with cortical screws provides excellent rigid fixation. The plate is contoured to the dorsal surface of the phalanx and secured. This is often the preferred method for its stability and early rehabilitation potential.
- Intramedullary Devices: Newer intramedullary compression screws or devices offer an alternative, particularly for minimal soft tissue dissection, but may be more technically demanding.
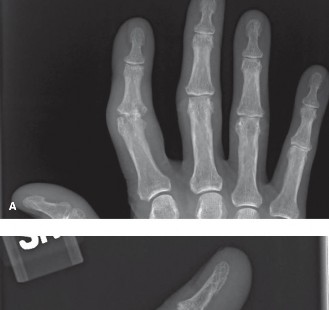
Figure 2: Intraoperative image illustrating rigid fixation of a PIP joint arthrodesis with a dorsal mini-fragment plate and screws, achieving the desired fusion angle. -
Joint Assessment: Confirm the desired angle and alignment are achieved. The joint should be completely stable.
- Closure: The extensor mechanism is meticulously repaired. The capsule may be closed, if possible, to provide additional stability. Subcutaneous tissues are closed, followed by skin closure.
Arthroplasty of the PIP Joint
Arthroplasty aims to preserve some motion while relieving pain. It is generally considered for patients who prioritize motion and have lower demands on pinch strength, or for patients with multi-joint involvement where preserving motion is critical for overall hand function. Given the high forces across the index PIP, arthroplasty outcomes can be less predictable than for other digits, and arthrodesis is often favored.
Types of Implants
- Silicone Arthroplasty (e.g., Swanson or Niebauer): Flexible hinge prostheses primarily acting as a spacer, relying on scar capsule formation for stability. Can be effective for pain relief and some motion but susceptible to wear, fracture, and instability, especially in high-demand joints.
- Pyrocarbon Arthroplasty: Anatomically shaped articulating surfaces made of pyrocarbon, a durable biocompatible material. These implants provide greater inherent stability and better kinematic matching compared to silicone. They require precise bone cuts and good collateral ligament integrity.
- Total Joint Arthroplasty (TJA): Less common for PIP joints, but specific designs exist, typically constrained or semi-constrained, aiming for true articulation. More complex technically and less extensively studied in the PIP joint than for larger joints.
Surgical Approach (Illustrative for Pyrocarbon Arthroplasty)
- Incision & Dissection: Similar dorsal approach as for arthrodesis.
- Exposure: The extensor mechanism is split or reflected to expose the joint capsule. A dorsal or dorsolateral capsulotomy is performed.
- Debridement & Osteophyte Resection: Remove all osteophytes and hypertrophic synovium.
-
Bone Preparation:
Precise bone cuts are critical for pyrocarbon implants. Using an oscillating saw and specific cutting guides provided by the implant system:
- Resect the proximal phalanx head, preserving the collateral ligament origins.
- Resect the middle phalanx base, preserving the volar plate and collateral ligament insertions.
- Ream the medullary canals of both phalanges to accommodate the implant stems.
- Trial Reduction: Insert trial components to assess fit, stability, and range of motion. Ensure proper alignment and tension of collateral ligaments.
- Implant Insertion: Once satisfied with the trial, insert the definitive pyrocarbon implant components (proximal and distal). Ensure components are fully seated.
- Soft Tissue Balancing: Assess collateral ligament tension and repair if necessary. Ensure the extensor mechanism tracks centrally.
- Closure: Repair the extensor mechanism and capsule. Close subcutaneous tissues and skin.
Complications & Management
Complications following PIP joint surgery for erosive OA can significantly impact functional outcomes. Meticulous surgical technique and vigilant post-operative care are essential to minimize their incidence.
| Complication | Incidence (Approximate) | Management / Salvage Strategy |
|---|---|---|
| Non-Union | 5-20% (Arthrodesis) | Conservative: Prolonged immobilization, electrical stimulation. Surgical: Revision arthrodesis with bone grafting (autograft or allograft), more rigid internal fixation (e.g., plate and screws), re-preparation of bone ends. |
| Infection | 1-5% | Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, washout, IV antibiotics, implant removal if necessary (for arthroplasty), conversion to arthrodesis or staged reconstruction. |
| Stiffness / Loss of Motion | Common (Arthroplasty); expected (Arthrodesis) | Arthroplasty: Aggressive hand therapy, dynamic splinting, manipulation under anesthesia. Surgical: Capsulectomy, tenolysis, or conversion to arthrodesis. For arthrodesis, if adjacent joints stiffen, targeted therapy. |
| Implant Fracture/Wear | 5-15% (Silicone arthroplasty) | Surgical: Implant removal, synovectomy, often followed by conversion to arthrodesis or revision arthroplasty with a different implant type (e.g., pyrocarbon). |
| Instability / Dislocation | 5-10% (Arthroplasty, particularly silicone) | Conservative: Splinting, hand therapy for strengthening. Surgical: Collateral ligament reconstruction, implant revision with a more constrained design, or conversion to arthrodesis. |
| Persistent Pain | Variable | Conservative: NSAIDs, injections, therapy. Surgical: For arthrodesis, investigate for non-union or adjacent joint arthritis; for arthroplasty, evaluate for implant loosening, instability, or soft tissue impingement, potentially leading to revision or conversion to arthrodesis. |
| Neurovascular Injury | <1% | Acute: Immediate surgical exploration and repair of nerve or vessel. Chronic: Symptomatic management, nerve grafting if severe deficit and appropriate timing. |
| Complex Regional Pain Syndrome (CRPS) | <5% | Aggressive multi-modal pain management, physical therapy, sympathetic blocks, psychological support. Early recognition is key. |
| Malunion/Malalignment | <5% (Arthrodesis) | Surgical: Corrective osteotomy and refixation. May be challenging if fusion is solid. |
Salvage Strategies:
*
Failed Arthrodesis (Non-union, Malunion):
The primary salvage is revision arthrodesis. This involves re-exposure, debridement of fibrous tissue, fresh bone cuts, often bone grafting (iliac crest autograft is robust), and rigid internal fixation (e.g., dorsal plate).
*
Failed Arthroplasty (Instability, Fracture, Infection):
The most common and reliable salvage for a failed PIP arthroplasty, especially for the index finger, is conversion to arthrodesis. This provides stability and pain relief at the cost of motion. Implant removal, thorough debridement, bone preparation, and rigid fusion are key. In select cases, revision arthroplasty with a different implant (e.g., silicone to pyrocarbon, if bone stock allows) may be considered, but carries higher risks.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing outcomes and preventing complications after PIP joint surgery. Protocols differ significantly based on the chosen surgical procedure.
Following PIP Arthrodesis
The primary goal is to achieve solid bony fusion while maintaining function in adjacent joints.
1.
Immobilization (0-6 weeks):
*
Initial:
A dorsal or volar splint is applied in the operating room, maintaining the fused PIP joint in the desired angle (30-45 degrees of flexion for the index finger) while allowing full MCP and DIP joint motion.
*
Protection:
The splint is typically worn continuously for 4-6 weeks, or until radiographic signs of early fusion are evident.
*
Wound Care:
Meticulous wound care. K-wire care if applicable.
2.
Early Mobilization (0-6 weeks):
*
Adjacent Joints:
Active and passive range of motion exercises for the MCP and DIP joints of the operated finger, as well as the adjacent fingers, are encouraged immediately to prevent stiffness.
*
Avoid PIP Stress:
Strictly avoid any active or passive motion at the fused PIP joint.
3.
Weaning from Immobilization (6-12 weeks):
*
Radiographic Confirmation:
Once radiographic evidence of union is present (usually at 6 weeks), the splint can be gradually discontinued.
*
Strengthening:
Gentle progressive strengthening exercises for the entire hand, avoiding direct stress on the fused joint, are initiated.
*
Functional Activities:
Gradual return to light functional activities, emphasizing protective measures for the fused joint.
4.
Long-Term (12+ weeks):
*
Full Activities:
Return to full activities, including work and sport, as tolerated, typically by 3-4 months post-operatively, once union is robust and pain-free.
*
Patient Education:
Education on adapting grip and pinch mechanics to accommodate the fused joint.
Following PIP Arthroplasty (Silicone or Pyrocarbon)
The primary goal is to restore a functional range of motion, improve stability, and reduce pain. Early, controlled motion is typically emphasized.
-
Early Post-Operative (Day 1 - 2 weeks):
- Immobilization: A static volar or dorsal protective splint is applied in the operating room, holding the PIP joint in 0-20 degrees of flexion to protect the repair and implant, while allowing full MCP and DIP motion.
- Edema Control: Elevation, gentle compression, and ice.
- Early Motion (Active): Under the guidance of a hand therapist, controlled active flexion and extension exercises of the PIP joint are initiated within 24-48 hours post-surgery, within the protected range of the splint. Active flexion should be carefully performed to avoid excessive force, protecting extensor repair.
-
Intermediate Phase (2-6 weeks):
- Dynamic Splinting: Often, a dynamic extension splint (e.g., spring-loaded or rubber band traction) or a joint-specific motion device is used to assist with extension and prevent flexion contractures, particularly if full extension is difficult. The splint is typically worn at night and for periods during the day.
- Active & Passive ROM: Progressive active and gentle passive range of motion exercises for the PIP joint are advanced, carefully respecting pain and soft tissue healing. The arc of motion is gradually increased.
- Strengthening: Gentle isometric exercises for intrinsic and extrinsic muscles may be initiated, avoiding heavy resistance.
- Scar Management: Gentle scar massage and desensitization.
-
Advanced Phase (6-12 weeks):
- Discontinuation of Splinting: As pain subsides and motion improves, the dynamic splint is gradually weaned.
- Progressive Strengthening: Increase resistance in strengthening exercises for grip, pinch, and individual finger movements.
- Functional Activities: Integration of hand into functional activities, gradually increasing load and complexity.
- Joint Protection: Patient education on joint protection techniques and activity modification to prevent implant overload.
-
Long-Term (12+ weeks):
- Full Return: Gradual return to full activities, avoiding heavy manual labor or repetitive forceful gripping that could jeopardize implant longevity, especially for silicone prostheses.
- Continued Exercise: Patients are encouraged to continue a home exercise program to maintain motion and strength.
Throughout the rehabilitation process, close collaboration between the surgeon, hand therapist, and patient is paramount. Regular assessments of pain, range of motion, stability, and function guide the progression of therapy.
Summary of Key Literature / Guidelines
The management of erosive osteoarthritis of the index finger PIP joint is guided by clinical experience and evolving literature. While specific guidelines for EOA are less extensive than for generalized OA, principles derived from general hand OA management apply.
-
Diagnosis & Differentiation: The consensus is that accurate diagnosis distinguishing EOA from other inflammatory arthropathies (e.g., rheumatoid arthritis, psoriatic arthritis) and classic OA is critical. Radiographic features are central, with MRI providing additional detail on synovitis and erosions. Histological findings often reveal synovial inflammation resembling inflammatory arthritis, supporting the "inflammatory" component of EOA.
- References: Doherty M. Erosive osteoarthritis. Ann Rheum Dis . 1983;42(1):31-35. Punzi L, et al. Erosive osteoarthritis: definition, diagnosis, and management. Curr Rheumatol Rep . 2005;7(6):443-448.
-
Non-Operative Management: First-line treatment generally involves NSAIDs for pain and inflammation, activity modification, splinting for support and pain relief during flares, and hand therapy to maintain range of motion and strength. Intra-articular corticosteroid injections can provide temporary relief during acute inflammatory episodes, but their long-term efficacy and potential for cartilage damage remain considerations.
- References: Arthritis Foundation guidelines for osteoarthritis of the hand (while not specific to EOA, provide general recommendations).
-
Surgical Intervention - Arthrodesis vs. Arthroplasty: This remains a key area of discussion, particularly for the index finger.
-
Arthrodesis:
For the index finger PIP, arthrodesis is frequently advocated, particularly for patients with high functional demands requiring a stable and pain-free joint for pinch and grip. Studies consistently report high fusion rates (85-95%) and excellent pain relief. Downsides include loss of motion and potential compensatory strain on adjacent joints. Fixation with dorsal mini-plates is often cited as the gold standard for rigid fixation.
- References: Lane LB, et al. Proximal interphalangeal joint arthrodesis in the hand: a review. J Hand Surg Am . 2008;33(10):1858-1869. Stern PJ, et al. Proximal interphalangeal joint arthrodesis. A long-term review. J Hand Surg Am . 1987;12(5 Pt 1):691-697.
-
Arthroplasty:
While arthroplasty aims to preserve motion, outcomes for the index finger PIP joint can be less predictable than for other digits or for the MCP joints.
- Silicone Arthroplasty: Provides pain relief and preserves some motion, but concerns exist regarding implant durability, fracture, and instability, especially under high pinch loads. Long-term studies show variable results with a trend towards lower satisfaction and higher reoperation rates compared to arthrodesis.
- Pyrocarbon Arthroplasty: Represents a biomechanically more anatomical option, providing greater intrinsic stability. Early and mid-term results suggest good pain relief and motion preservation, with improved stability compared to silicone. However, larger, long-term studies specifically on index PIP joints are still maturing, and technical demands are higher.
- References: Cook PA, et al. Pyrocarbon versus silicone proximal interphalangeal joint arthroplasty: a systematic review. J Hand Surg Am . 2014;39(12):2422-2430. Van Heest AE, et al. Pyrocarbon proximal interphalangeal joint replacement. Hand Clin . 2010;26(3):355-364.
-
Arthrodesis:
For the index finger PIP, arthrodesis is frequently advocated, particularly for patients with high functional demands requiring a stable and pain-free joint for pinch and grip. Studies consistently report high fusion rates (85-95%) and excellent pain relief. Downsides include loss of motion and potential compensatory strain on adjacent joints. Fixation with dorsal mini-plates is often cited as the gold standard for rigid fixation.
- Complication Management: The literature supports aggressive management of non-union for arthrodesis, often with revision and bone grafting. For arthroplasty, implant failure (fracture, loosening, instability) or chronic infection often leads to conversion to arthrodesis as a reliable salvage procedure.
Current Consensus:
For severe, painful, and deforming EOA of the index finger PIP joint refractory to conservative management:
1.
Arthrodesis
remains a highly reliable option, especially for patients prioritizing stability, pain relief, and strength for pinch and grip. It is generally the preferred option for the index finger PIP joint among many hand surgeons.
2.
Pyrocarbon Arthroplasty
offers a viable alternative for select patients who place a very high premium on preserving motion and have good bone stock and stable soft tissues, provided they understand the potential for lower durability and the need for activity modification compared to arthrodesis. Silicone arthroplasty is generally less favored for the index PIP due to higher failure rates in this high-demand digit.
The decision-making process must be individualized, factoring in patient-specific demands, adjacent joint status, surgeon experience, and a thorough discussion of the risks and benefits of each procedure. Continued research into novel biomaterials and surgical techniques for PIP joint arthroplasty remains an active area of investigation.
