This document provides an exhaustive, high-yield academic review of lesser toe arthrodesis, intended for orthopedic surgeons, residents, and medical students. It adheres strictly to an objective, scientific tone, devoid of patient education or promotional content.
Introduction & Epidemiology
Lesser toe deformities represent a common presenting complaint in orthopedic foot and ankle clinics, significantly impacting patient quality of life through pain, difficulty with shoe wear, and gait abnormalities. These deformities include hammertoe, claw toe, and mallet toe, characterized by contracture at the proximal interphalangeal (PIP), metatarsophalangeal (MTP), and distal interphalangeal (DIP) joints, respectively. While initially flexible, these deformities can progress to rigid contractures, often accompanied by dorsal callosities over the PIPJ, tip callosities in mallet toes, or plantar MTPJ callosities in claw toes due to subluxation.
The epidemiology of lesser toe deformities indicates a higher prevalence in older populations and females, often associated with ill-fitting footwear. The impact extends beyond local pain, affecting overall foot mechanics and potentially exacerbating other forefoot pathologies such as bunions or metatarsalgia. When conservative measures—including wider shoes, silicone pads, toe splints, and activity modification—fail to alleviate symptoms in patients with rigid deformities, surgical intervention becomes necessary.
Arthrodesis of the interphalangeal joints, particularly the PIPJ, stands as a definitive and durable surgical solution for rigid lesser toe deformities. This procedure aims to eliminate pain, correct the deformity, resolve callosities, and restore functional alignment of the toe. While soft tissue releases and arthroplasties offer alternative solutions for flexible or semi-rigid deformities, arthrodesis provides superior long-term stability and correction for recalcitrant and rigid contractures by creating a solid bony fusion.
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate anatomy and biomechanics of the lesser toes is paramount for successful surgical outcomes in arthrodesis.
Surgical Anatomy
The lesser toes (digits 2-5) are composed of three phalanges: proximal, middle, and distal, except for the fifth digit which typically has two (proximal and distal).
*
Joints
: The MTP joint connects the metatarsal head to the proximal phalanx, the PIP joint connects the proximal and middle phalanges, and the DIP joint connects the middle and distal phalanges.
*
Bony Architecture
: The phalanges are relatively small bones, requiring precise bone cuts and careful handling during surgery. The articular surfaces of the interphalangeal joints are condylar, allowing for flexion and extension.
*
Ligamentous Structures
: Each joint is stabilized by a strong plantar plate (MTPJ) or volar plate (PIPJ, DIPJ), and paired collateral ligaments (medial and lateral). These structures are often contracted or attenuated in chronic deformities.
*
Tendinous Structures
:
*
Extensor Digitorum Longus (EDL)
: Inserts primarily on the distal phalanx, with slips to the middle phalanx. Responsible for MTPJ and interphalangeal joint extension.
*
Extensor Digitorum Brevis (EDB)
: Inserts on the dorsal aspect of the proximal phalanx. Primarily extends the MTPJ.
*
Flexor Digitorum Longus (FDL)
: Inserts on the plantar aspect of the distal phalanx. Primary flexor of the DIPJ and PIPJ.
*
Flexor Digitorum Brevis (FDB)
: Inserts on the plantar aspect of the middle phalanx, splitting around the FDL tendon. Primary flexor of the PIPJ.
*
Neurovascular Bundles
: Two dorsal and two plantar digital neurovascular bundles supply each toe. The plantar bundles are typically larger and run along the sides of the phalanges. Careful dissection is required, particularly with dorsal incisions, to avoid injury to the dorsal digital nerves.
*
Intrinsic Muscles
: The interossei and lumbricals play a crucial role in MTPJ flexion and interphalangeal joint extension. Imbalance between intrinsic and extrinsic musculature is a key driver of toe deformities.
Biomechanics
The lesser toes contribute significantly to forefoot stability during stance and propulsion during gait.
*
Normal Function
: During the stance phase, the toes extend at the MTPJs and flex at the PIPJs and DIPJs, allowing the toe pads to make contact with the ground, providing stability and grip. In the propulsive phase, the toes stiffen, acting as levers to transfer ground reaction forces.
*
Pathobiomechanics of Deformities
:
*
Hammertoe
: Characterized by MTPJ extension, PIPJ flexion, and DIPJ extension. Often caused by an imbalance between the FDL/FDB and EDL, or MTPJ hyperextension leading to a relative shortening of the EDL.
*
Claw Toe
: Involves MTPJ hyperextension, PIPJ flexion, and DIPJ flexion. Typically results from intrinsic muscle weakness or neuropathy, leading to an imbalance where the extrinsics dominate.
*
Mallet Toe
: Characterized by DIPJ flexion, with normal MTPJ and PIPJ alignment. Commonly caused by FDL overpull or distal phalanx trauma.
*
Role of Arthrodesis
: By fusing the PIPJ (most common site for arthrodesis), a rigid segment is created, addressing the PIPJ flexion deformity. This straightens the toe, eliminates dorsal prominence, and allows for better ground contact. It can indirectly improve MTPJ extension in hammertoes or prevent recurrence of flexion deformities. The challenge is to maintain appropriate toe length and provide sufficient plantar flexion (typically 5-10 degrees relative to the metatarsal) to ensure ground purchase without creating a "floating toe." Excessive shortening can lead to MTPJ instability or transfer metatarsalgia.
Indications & Contraindications
Careful patient selection based on clinical and radiographic assessment is crucial for optimizing outcomes following lesser toe arthrodesis.
Indications for Lesser Toe Arthrodesis
- Rigid Hammertoe, Claw Toe, or Mallet Toe Deformities : Primary indication for patients presenting with non-reducible contractures at the PIPJ or DIPJ.
- Painful Callosities : Resulting from dorsal prominence over the PIPJ or tip of the toe, or plantar callosities at the MTPJ due to hyperextension and MTPJ plantar plate overload.
- Failure of Conservative Management : Persistent pain, functional limitation, or difficulty with shoe wear despite adequate trials of non-operative treatments (e.g., accommodative footwear, toe padding, splinting).
- Recurrent Deformity : Following previous soft tissue procedures (e.g., flexor tenotomy, capsulotomy) where flexibility could not be maintained.
- Adjunct to Forefoot Reconstruction : To optimize toe alignment and stability when performing other procedures such as bunionectomy, metatarsal osteotomies, or MTPJ reconstruction.
- MTPJ Plantar Plate Pathology : In conjunction with MTPJ stabilization, straightening the toe via PIPJ arthrodesis can offload the MTPJ.
Contraindications for Lesser Toe Arthrodesis
-
Absolute Contraindications
:
- Active Local or Systemic Infection : Increased risk of non-union and osteomyelitis.
- Severe Peripheral Vascular Disease : Compromised healing capacity.
- Acute Charcot Arthropathy : Unstable bone architecture.
- Severe Uncorrectable MTPJ Instability/Deformity : The PIPJ arthrodesis alone will not address the primary instability, and may lead to transfer pain or continued MTPJ issues.
-
Relative Contraindications
:
- Poor Soft Tissue Envelope : Compromised skin viability, especially in revision cases.
- Significant Bone Loss or Osteoporosis : May hinder stable fixation and fusion.
- Non-ambulatory Patient : Limited functional benefit, increased complication risk.
- Unrealistic Patient Expectations : Essential to counsel patients on potential outcomes and limitations.
- Uncontrolled Diabetes with Neuropathy : Increased risk of infection, delayed healing, and Charcot neuroarthropathy.
Table: Operative vs. Non-Operative Indications for Lesser Toe Deformities
| Feature | Non-Operative Management | Operative Management (Arthrodesis) |
|---|---|---|
| Deformity Type | Flexible or Semi-Rigid | Rigid, fixed contracture (primary indication for arthrodesis) |
| Symptoms | Mild to moderate pain, intermittent discomfort, cosmetic concern | Severe, intractable pain, chronic callosities, functional impairment |
| Footwear Issues | Accommodated by wider shoes, toe boxes, padding | Unresolvable with conservative footwear modifications |
| Clinical Assessment | Passive correction possible, no fixed contracture | Fixed contracture, inability to passively correct deformity |
| Radiographic Findings | Minimal joint changes, no subluxation/dislocation | Fixed angular deformity, potential MTPJ subluxation, degenerative changes |
| Response to Therapy | Symptoms improved or resolved with conservative modalities | Failure of multiple conservative interventions |
| Associated Pathologies | Isolated deformity, no significant MTPJ instability | Concomitant MTPJ plantar plate pathology, severe metatarsalgia, adjacent toe deformity |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical steps to ensure a safe and effective surgical procedure.
Pre-Operative Planning
-
Clinical Assessment
:
- Detailed History : Ascertain the primary complaint (pain, callosities, difficulty with shoes), duration of symptoms, prior treatments, and functional limitations. Assess patient expectations.
-
Physical Examination
:
- Deformity Type : Identify hammertoe, claw toe, or mallet toe.
- Flexibility : Determine if the deformity is flexible or rigid by attempting passive correction of the MTPJ, PIPJ, and DIPJ.
- Callosities : Document location and severity (dorsal PIPJ, plantar MTPJ, distal tip).
- Neurovascular Status : Assess capillary refill, sensation (light touch, two-point discrimination), and presence of peripheral pulses (dorsalis pedis, posterior tibial). Document any pre-existing neuropathy.
- MTPJ Stability : Evaluate for MTPJ subluxation or instability, as this may require concomitant MTPJ release or stabilization.
- Overall Foot Alignment : Assess for other contributing factors such as hallux valgus, pes planus, or pes cavus.
-
Radiographic Evaluation
:
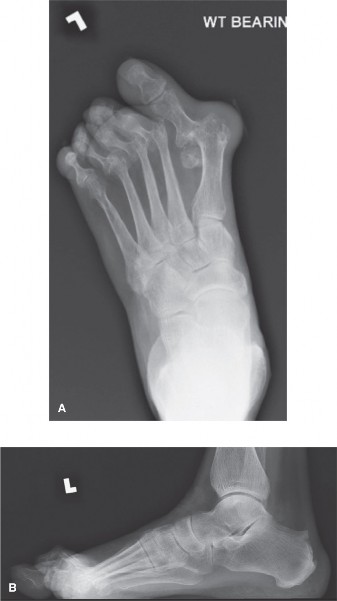
- Weight-bearing Anteroposterior (AP), Lateral, and Oblique Views of the Foot : Essential for assessing bony alignment, joint integrity, degenerative changes, and identification of any associated forefoot pathology.
- Specific Views : Lateral view helps in assessing the degree of PIPJ flexion and MTPJ extension/subluxation.
- Bone Quality : Evaluate bone stock for fixation planning.
-
Templating
:
- Pre-operative assessment of toe length and angulation is critical. Aim for a neutral to slightly plantarflexed position (typically 5-10 degrees relative to the metatarsal shaft) at the PIPJ to ensure ground contact without a "floating toe."
- Consider fixation options (K-wires, headless compression screws, intramedullary implants) and have appropriate sizes available.
-
Patient Counseling
:
- Thorough discussion with the patient regarding the nature of the deformity, the surgical plan, expected outcomes (pain relief, improved shoe wear, corrected alignment), potential complications (non-union, infection, recurrence, nerve injury, persistent swelling), and the post-operative rehabilitation protocol.
- Emphasis on smoking cessation if applicable, due to its negative impact on bone healing.
Patient Positioning & Anesthesia
-
Anesthesia
:
- Regional Anesthesia : A popliteal block or ankle block provides excellent post-operative pain control and can reduce the need for general anesthesia.
- General Anesthesia or Sedation : Often used in conjunction with a regional block, or as the sole anesthetic, depending on patient comorbidities and surgeon preference.
-
Patient Positioning
:
- Supine Position : The patient is placed supine on the operating table.
- Tourniquet : A pneumatic thigh tourniquet (typically inflated to 250-300 mmHg) or an ankle tourniquet (100 mmHg above systolic blood pressure) is applied to achieve a bloodless field, which is essential for precise dissection and fixation. The ankle tourniquet is preferred by some for shorter procedures, as it is less uncomfortable for the patient post-operatively.
- Leg Prep and Drape : The entire lower extremity is prepped with an antiseptic solution (e.g., chlorhexidine or povidone-iodine) and draped sterilely, allowing access to the foot and ankle.
- Image Intensifier : A C-arm fluoroscope should be available and positioned for easy intraoperative access to confirm hardware placement and alignment.
Detailed Surgical Approach / Technique
This section focuses on the detailed technique for proximal interphalangeal joint (PIPJ) arthrodesis, which is the most common site for fusion in lesser toe deformities.
1. Anesthesia and Tourniquet
- After induction of anesthesia (regional +/- general), the tourniquet is inflated. The limb is exsanguinated prior to inflation, if a thigh tourniquet is used.
2. Incision
- A dorsal longitudinal incision is made directly over the PIPJ of the affected lesser toe.
- The incision length is typically 2-3 cm, extending proximally over the proximal phalanx and distally over the middle phalanx.
- Care is taken to avoid the dorsal digital neurovascular structures, which are typically located slightly medial and lateral to the midline extensor tendon.
3. Dissection
- Skin and Subcutaneous Tissue : The incision is deepened through the skin and subcutaneous fat. Superficial veins are ligated or cauterized.
- Extensor Tendon : The extensor digitorum longus (EDL) tendon is identified. A longitudinal incision is made through the extensor tendon sheath and the tendon itself, directly over the PIPJ. The tendon edges are carefully retracted.
- Joint Capsule and Collateral Ligaments : The dorsal capsule of the PIPJ is incised. The collateral ligaments (medial and lateral) are released sharply to adequately expose the articular surfaces of the proximal phalanx head and middle phalanx base. A complete release, including the plantar plate, may be necessary to fully correct the deformity and allow for joint distraction.
4. Joint Preparation (Resection)
- The goal is to resect sufficient bone to achieve correction of the deformity while maintaining appropriate toe length and providing broad, cancellous bone-to-bone contact for fusion. The amount of bone removed influences toe length; excessive shortening can lead to MTPJ subluxation or transfer metatarsalgia.
-
Articular Cartilage Resection
:
- The articular cartilage from the head of the proximal phalanx and the base of the middle phalanx is completely removed.
-
Techniques
:
- Sagittal Saw : A small oscillating sagittal saw can be used to create flat, parallel bone cuts on the head of the proximal phalanx and the base of the middle phalanx. This technique is precise but requires careful angulation.
- Bone Nibblers/Ron-geurs : These can be used to remove cartilage and small amounts of subchondral bone, shaping the bone ends.
- Cone and Ream Technique : Using a specialized reamer, a conical shape is created on one phalanx (e.g., proximal phalanx head) and a corresponding concave shape on the other (e.g., middle phalanx base). This provides a larger surface area for fusion and inherent stability against rotation.
- Angulation : The fused PIPJ should be positioned in 5-10 degrees of plantarflexion relative to the metatarsal shaft. This ensures the toe makes contact with the ground during ambulation ("grounding") and prevents a "floating toe" deformity.
5. Reduction & Fixation
Once the joint surfaces are prepared and the desired alignment is achieved, the toes are reduced and held with temporary fixation.
- Temporary Fixation : Held manually or with small K-wires passed temporarily across the joint.
-
Definitive Fixation :
-
Kirschner Wires (K-wires) :
-
Technique
: Often, a 0.045-inch or 0.062-inch K-wire is used.
- Antegrade : The K-wire is inserted through the tip of the toe, across the DIPJ (if unstable or requiring concomitant fusion), then across the PIPJ, and advanced proximally into the medullary canal of the proximal phalanx.
- Retrograde : The K-wire is first driven from the resected surface of the middle phalanx base distally through the tip of the toe. Then, the toe is reduced, and the K-wire is driven retrogradely across the PIPJ into the proximal phalanx.
- Number : Typically one or two K-wires are used for rotational stability.
- Placement : The K-wire is then bent at 90 degrees and cut short, leaving it exposed externally (outside the skin) for easy removal post-operatively.
- Advantages : Simple, inexpensive, effective.
- Disadvantages : Pin tract infection, migration, breakage, need for external care, potential for delayed union if fixation is not rigid enough.
-
Technique
: Often, a 0.045-inch or 0.062-inch K-wire is used.
-
Intramedullary Implants (Headless Compression Screws, Specialized Arthrodesis Devices) :
-
Technique
:
- Headless Compression Screw : A small cannulated headless compression screw (e.g., 2.0 mm, 2.4 mm) can be used. A guide wire is inserted either antegrade or retrograde across the fusion site. The joint is over-drilled and tapped, and the screw is then inserted, achieving compression across the fusion site.
- Specialized Arthrodesis Implants : Various devices are available, often made of nitinol (shape memory alloy) or PEEK, designed to provide internal compression and stability. These are typically inserted intramedullary.
- Advantages : No external hardware, rigid fixation, allows for earlier protected weight-bearing, lower risk of pin tract infection.
- Disadvantages : Higher cost, technically more demanding, potential for screw breakage or malposition, requires a secondary procedure for removal if symptomatic, may not be suitable for very small bones or poor bone stock.
-
Technique
:
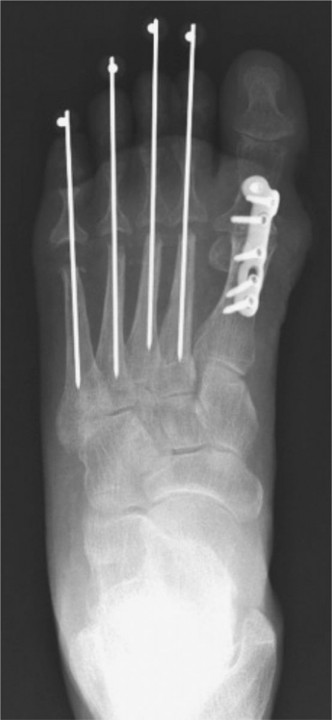- Considerations for MTPJ Stability : If there is significant MTPJ hyperextension or instability (common in claw toe deformities), a concomitant flexor digitorum longus (FDL) tenotomy or transfer, or an MTPJ capsulorrhaphy/plantar plate repair may be performed to improve MTPJ function and prevent recurrence. An extensor tendon lengthening or release at the MTPJ may also be required.
-
6. Wound Closure
- The extensor tendon is repaired (if incised), or the edges are coapted.
- The subcutaneous tissue is closed using absorbable sutures.
- The skin is closed with fine non-absorbable sutures (e.g., 4-0 nylon or prolene) in an interrupted or running fashion.
7. Dressing
- A soft, sterile dressing is applied, often incorporating gauze between the toes to maintain alignment and prevent maceration.
-
A post-operative surgical shoe or boot is applied.

Complications & Management
Despite high success rates, lesser toe arthrodesis is not without potential complications. Awareness of these, along with their incidence and management strategies, is crucial for optimal patient care.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence | Etiology | Management / Salvage Strategies |
|---|---|---|---|
| Non-union / Delayed union | 5-15% | Inadequate fixation, infection, poor bone stock, smoking, excessive motion at fusion site, inadequate surface preparation. | Revision surgery with débridement, bone grafting (autograft/allograft), more rigid internal fixation, pulsed electromagnetic stimulation. |
| Malunion | 5-10% | Inadequate intraoperative alignment, hardware failure, soft tissue imbalance. | Osteotomy for realignment, re-arthrodesis. |
| Infection (pin tract) | 1-5% (K-wires) | Poor pin care, patient hygiene, prolonged externalization. | Oral antibiotics, local wound care, early K-wire removal if union is progressing. If deep, IV antibiotics, débridement, hardware removal. |
| Infection (surgical site) | <1-2% | Contamination, poor wound healing, compromised soft tissues. | IV antibiotics, surgical débridement, hardware removal (once fusion confirmed or revised). |
| Hardware Failure/Migration | 5-10% (K-wires) | Premature weight-bearing, inadequate initial fixation, patient activity, osteoporosis. | Hardware removal, re-fixation with more stable construct, bracing. |
| Neurovascular Injury | <1% | Iatrogenic during dissection (dorsal digital nerves). | Micro-surgical repair (if recognized acutely), neuromas managed by excision, neurectomy, or desensitization. |
| Recurrence of Deformity | 2-5% | Inadequate soft tissue release, persistent muscle imbalance, MTPJ instability, inadequate fusion angle. | Revision surgery, further soft tissue releases, MTPJ stabilization, re-arthrodesis. |
| Adjacent Toe Deformity | Variable | Altered biomechanics, compensatory changes in adjacent toes post-fusion. | Conservative management (padding, shoe modifications), surgical correction of adjacent toe. |
| "Floating Toe" (Non-grounding) | 2-8% | Excessive shortening, insufficient plantarflexion of fused toe, MTPJ hyperextension. | Shoe modifications (toe fillers), MTPJ stabilization, revision with interpositional graft (rare). |
| Persistent Pain/Stiffness | Variable | Scar tissue, residual deformity, nerve irritation, MTPJ pathology, complex regional pain syndrome (CRPS). | Physical therapy, steroid injections, nerve blocks, neuromodulation, revision surgery for specific pathology. |
| Swelling | Common (months) | Normal post-operative inflammatory response. | Elevation, compression stockings, gentle ROM of non-fused joints. |
| Shortening of Toe | Variable | Amount of bone resected. Can be perceived as cosmetic deficit or affect shoe fit. | Patient education pre-operatively. Minimise bone resection. |
General Management Principles
- Prophylactic Antibiotics : Standard practice to reduce infection risk.
- Pain Management : Multi-modal approach (regional blocks, oral analgesics, NSAIDs).
- Early Detection : Close post-operative monitoring for signs of infection, neurovascular compromise, or hardware issues.
- Patient Education : Reinforce the importance of adherence to post-operative instructions, including weight-bearing restrictions, pin care (if applicable), and activity modifications.
Post-Operative Rehabilitation Protocols
A structured post-operative rehabilitation protocol is essential for optimizing outcomes, ensuring fusion, and facilitating a safe return to activity. Protocols may vary slightly based on the type of fixation used (K-wires vs. internal implants) and surgeon preference.
Phase 1: Immediate Post-Operative (Weeks 0-2)
-
Protection
:
- Weight-Bearing (WB) : Typically protected weight-bearing in a rigid-soled post-operative shoe or surgical boot. Some surgeons may prefer non-weight-bearing (NWB) with crutches for the first 2 weeks, particularly with K-wire fixation or multi-toe procedures.
- Dressings : Initial bulky dressing applied in the operating room. Dressings are changed at 1-week post-op. Pin care instructions provided for K-wire fixation.
-
Pain and Swelling Management
:
- Elevation : Maintain the foot elevated above heart level as much as possible to reduce swelling.
- Ice : Apply ice packs for 15-20 minutes, several times a day.
- Analgesia : Administer pain medication as prescribed.
-
Movement
:
- Ankle ROM : Gentle active and passive range of motion (ROM) exercises for the ankle and hindfoot, avoiding stress on the forefoot.
- Non-operated Toes : Encourage gentle active ROM for non-operated toes to prevent stiffness.
- Patient Education : Reinforce NWB/protected WB status, wound care, signs of infection, and the importance of smoking cessation for bone healing.
Phase 2: Early Mobilization & Consolidation (Weeks 2-6)
-
Weight-Bearing
:
- Progressive weight-bearing as tolerated in the post-operative shoe or boot, provided fixation is stable.
- If NWB initially, transition to protected WB as tolerated.
-
K-wire Removal (if applicable)
:
- K-wires are typically removed at 4-6 weeks post-operatively, once initial radiographic signs of consolidation or adequate callus formation are observed, and clinical stability is confirmed. The removal is usually performed in the clinic and is generally well-tolerated.
-
Shoe Wear
:
- Once K-wires are removed (if applicable) and clinical/radiographic stability is confirmed, transition from the post-operative shoe to a stiff-soled, roomy athletic shoe.
-
Physical Therapy (as needed)
:
- Initiate gentle exercises for foot intrinsic strength and balance.
- Scar massage once incision is fully healed.
- Address any residual swelling or stiffness in surrounding joints.
Phase 3: Strengthening & Return to Activity (Weeks 6-12+)
- Weight-Bearing : Full weight-bearing in comfortable, supportive shoes. Avoid high heels or restrictive footwear.
-
Activity Progression
:
- Gradually increase activity levels.
- Low-impact activities (e.g., walking, cycling, swimming) are encouraged.
- Avoid high-impact activities (e.g., running, jumping sports) until complete radiographic fusion is confirmed, usually by 10-12 weeks.
-
Strengthening
:
- Focus on foot intrinsic and extrinsic muscle strengthening exercises.
- Proprioceptive and balance exercises to restore neuromuscular control.
- Gait training to normalize walking patterns.
- Radiographic Assessment : Obtain follow-up X-rays (typically at 6-8 weeks and 10-12 weeks) to confirm radiographic fusion of the arthrodesis site. Fusion is typically complete by 8-12 weeks, but can take longer.
-
Long-Term Care
:
- Continue to wear supportive, comfortable footwear.
- Address any residual stiffness or discomfort with ongoing physical therapy.
- Monitor for any transfer metatarsalgia or adjacent toe issues.
Note : The specific timing and progression of rehabilitation should always be individualized based on the patient's healing capacity, co-morbidities, intraoperative findings, and the surgeon's assessment of fusion progress.
Summary of Key Literature / Guidelines
Lesser toe arthrodesis, particularly of the PIPJ, is a well-established and effective procedure for the correction of rigid lesser toe deformities. The literature predominantly supports its use as a definitive solution for symptomatic, fixed contractures unresponsive to conservative care.
Outcomes and Efficacy
:
* Numerous studies report high patient satisfaction and significant improvement in pain and function following PIPJ arthrodesis. Fusion rates for PIPJ arthrodesis typically range from
85% to 95%
, with slightly lower rates for DIPJ fusions.
* A systematic review by
Trnka et al. (2009)
highlighted that arthrodesis provides a stable, long-term correction with good functional outcomes, particularly for hammertoe deformities.
*
Coughlin and Shurnas (2003)
demonstrated in a large series that PIPJ arthrodesis is a predictable procedure with high fusion rates and low complication rates when performed meticulously.
Comparison of Fixation Methods
:
*
K-wires
: Remain the most common and cost-effective method of fixation. Studies by
Taylor et al. (2008)
and others confirm their efficacy. While associated with a higher risk of pin tract infection and hardware migration compared to internal fixation, their ease of use and removal make them a standard.
*
Intramedullary Implants (e.g., headless compression screws, shape-memory implants)
: Gaining popularity due to potential advantages of rigid internal fixation, elimination of external hardware, and potentially earlier mobilization.
*
A meta-analysis by Del Prete et al. (2015)
comparing K-wires to intramedullary implants for PIPJ arthrodesis found similar union rates, but intramedullary devices had a lower rate of pin tract infections and less patient discomfort associated with external hardware. However, they were associated with higher costs and a potential need for hardware removal if symptomatic.
*
Day and Dr. Mark Meyerson (2012)
published on the use of an intramedullary nitinol implant, showing favorable outcomes and improved patient satisfaction compared to K-wires in their series.
*
Headless compression screws
offer robust compression across the fusion site and are particularly useful in cases requiring high stability.
Geldwert et al. (2010)
have published on their successful application in lesser toe fusions.
Technical Considerations and Adjunct Procedures
:
* The importance of appropriate toe alignment, particularly achieving 5-10 degrees of plantarflexion, is consistently emphasized to prevent "floating toe" and ensure proper ground contact.
*
Flexor Tenotomy/Transfer
: The literature supports concomitant FDL tenotomy or transfer, especially in claw toe deformities or when significant MTPJ hyperextension is present, to rebalance the toe and prevent recurrence or transfer lesions.
Myerson (2005)
extensively discussed the importance of MTPJ stabilization in conjunction with PIPJ correction.
*
Bone Resection
: Minimizing excessive bone resection to prevent over-shortening and subsequent MTPJ instability is a recurrent theme.
Complications
:
* Non-union rates, while low, are higher in smokers and patients with poor bone quality.
* The incidence of transfer metatarsalgia or adjacent toe pain following lesser toe surgery is a recognized complication, underscoring the need for comprehensive forefoot assessment.
* Patient education regarding prolonged swelling and potential for residual stiffness is vital.
Conclusion
:
Lesser toe arthrodesis remains a cornerstone of surgical management for rigid lesser toe deformities. The choice of fixation method depends on surgeon preference, patient factors, and the specific characteristics of the deformity. Adherence to meticulous surgical technique, appropriate patient selection, and a structured rehabilitation protocol are crucial for achieving reliable fusion, sustained pain relief, and improved functional outcomes. Ongoing research continues to refine surgical techniques and implant designs, but the fundamental principles of stable bony fusion for rigid deformities remain consistently supported in the academic literature.
Clinical & Radiographic Imaging