Introduction and Epidemiology
Midfoot pain is a common and often debilitating complaint in orthopedic practice, arising from a myriad of etiologies including degenerative arthritis, post-traumatic deformity, inflammatory conditions, and neuropathic arthropathy (Charcot foot). The intricate anatomy and complex biomechanics of the midfoot, serving as the critical link between the hindfoot and forefoot, make it particularly susceptible to abnormal loading patterns and subsequent painful sequelae. When conservative measures are pursued, the application of external shoe modifications, specifically the rocker bottom sole, represents a fundamental and highly effective non-surgical strategy for redistributing plantar pressures and mitigating pain.
A rocker bottom modification aims to alter the natural roll-over shape of the foot during gait, facilitating a smoother transition from heel strike to toe-off by effectively shortening the functional lever arm of the foot. This intervention reduces the range of motion required at painful joints, offloads specific plantar pressure points, and decreases muscular effort, thereby providing symptomatic relief. While the concept is decades old, its biomechanical principles remain robust, offering a versatile tool in the orthopedic surgeon's arsenal for managing various midfoot pathologies conservatively. The prevalence of conditions benefiting from rocker bottom soles, such as midfoot osteoarthritis, pes planus deformities, and diabetic foot complications, underscores the broad applicability and importance of understanding this non-operative approach.
Epidemiologically, midfoot osteoarthritis affects approximately 12% of the population over the age of 50, with a higher predilection in females and individuals with a history of significant foot trauma, such as Lisfranc fracture-dislocations. Neuropathic arthropathy, while less common in the general population, occurs in up to 13% of high-risk diabetic patients, frequently targeting the tarsometatarsal and midtarsal joints. The resulting structural collapse—often manifesting as a classic "rocker-bottom deformity" of the foot itself—paradoxically requires an external rocker-bottom shoe modification to prevent focal ulceration at the newly formed bony prominences. Understanding the epidemiological burden of these midfoot pathologies highlights the necessity for mastering both the conservative orthotic management and the definitive surgical interventions required when non-operative measures fail.
Surgical Anatomy and Biomechanics
The midfoot comprises the navicular, cuboid, and three cuneiform bones, articulating with the talus and calcaneus proximally and the metatarsals distally. Key articulations include the talonavicular, calcaneocuboid (Chopart's joint), and the intercuneiform, cuneonavicular, and tarsometatarsal (Lisfranc's joint) articulations.
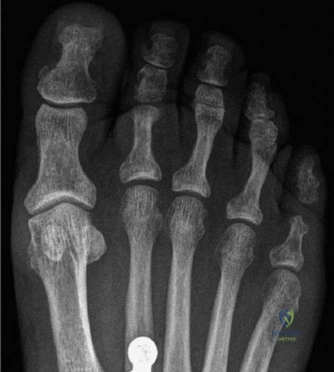
These joints, stabilized by an intricate network of ligaments (e.g., plantar calcaneonavicular or spring ligament, plantar fascia, interosseous ligaments) and musculotendinous units (e.g., tibialis posterior, peroneus longus), form the longitudinal and transverse arches of the foot, crucial for shock absorption and propulsion during ambulation. The osseous architecture forms a Roman arch configuration, dynamically supported by the windlass mechanism of the plantar fascia during the terminal stance phase of gait.
Normal gait involves a complex sequence of pronation and supination, facilitated by coordinated muscle activity and joint motion. During the stance phase, the foot progresses through three rockers:
1. Heel Rocker: From heel strike to foot flat, primarily governed by the ankle dorsiflexors.
2. Ankle Rocker: From foot flat to heel off, involving progression over the tibiotalar joint.
3. Forefoot Rocker: From heel off to toe off, involving progression over the metatarsal heads and MTP joints.
Pathologies causing midfoot pain often disrupt the normal progression of these rockers, particularly by restricting motion or causing excessive strain within the midfoot segment. A rocker bottom shoe modifies the effective rocker mechanism of the foot. By creating a convex sole from the heel to the forefoot, it effectively reduces the leverage of the foot, decreases motion at specific joints, and alters the plantar pressure distribution.
Biomechanics of Specific Rocker Sole Configurations
The apex of the rocker, known as the "roll-off" point, is strategically placed to offload painful areas. For midfoot pain, the apex is typically positioned proximal to the painful region, often just anterior to the midtarsal joints or at the apex of a deformity, thus reducing forces across these structures. This shifts the center of pressure anteriorly and facilitates a smoother, less strenuous roll-over, bypassing or minimizing painful joint excursions.
Several distinct rocker configurations are utilized in pedorthic practice, each with specific biomechanical objectives:
* Forefoot Rocker: The apex is positioned immediately proximal to the metatarsal heads. This is highly effective for offloading the forefoot and reducing the required dorsiflexion at the metatarsophalangeal joints, but also reduces the bending moment across the midfoot during terminal stance.
* Heel-to-Toe Rocker: Features a continuous convex curve from the posterior heel to the anterior toe. This configuration minimizes the requirement for ankle and midfoot motion throughout the entire stance phase, making it the modification of choice for severe midfoot arthrosis or rigid pes planus.
* Double Rocker: Features a concavity in the midsection of the sole with convexities at the heel and forefoot. This is specifically designed to completely offload a prominent midfoot, such as the collapsed arch seen in severe Charcot arthropathy, redirecting the ground reaction force (GRF) to the heel and forefoot.
Indications and Contraindications
The primary indication for a rocker bottom modification is the relief of midfoot pain stemming from conditions that cause limited or painful motion, abnormal plantar pressures, or progressive deformity. When conservative management with these orthotic modifications is exhausted, surgical intervention becomes indicated.
Indications for Rocker Bottom Modifications
Non-operative indications revolve around the need to mechanically bypass the midfoot during the stance phase of gait. Primary indications include:
* Midfoot Osteoarthritis: Idiopathic or post-traumatic (e.g., remote Lisfranc injuries) arthritis of the tarsometatarsal or intercuneiform joints. The rocker sole reduces the bending moment across the arthritic joints.
* Charcot Neuroarthropathy: In the quiescent, chronic phase (Eichenholtz Stage III), a double rocker sole is critical for accommodating the fixed rocker-bottom foot deformity and preventing midfoot ulceration.
* Rheumatoid Arthritis: Inflammatory arthropathy often leads to midfoot collapse and rigidity. The rocker sole compensates for the loss of the ankle and forefoot rockers.
* Adult Acquired Flatfoot Deformity: In rigid, late-stage posterior tibial tendon dysfunction (Johnson and Strom Stage III or IV), rocker soles facilitate forward progression without stressing the collapsed medial column.
Contraindications for Rocker Bottom Modifications
While generally benign, rocker bottom modifications are not universally appropriate. Contraindications include:
* Severe Balance Impairment: The convex nature of the sole inherently decreases the surface area in contact with the ground at any given moment, which can exacerbate proprioceptive deficits and increase fall risk in elderly or neurologically compromised patients.
* Acute Instability: In cases of acute, unstable midfoot fractures or active Eichenholtz Stage I Charcot arthropathy, rigid immobilization (e.g., total contact casting) is required. A rocker sole shoe does not provide sufficient stability for acute osseous fragmentation.
* Severe Knee or Hip Pathology: Altering the GRF vector with a rocker sole can inadvertently increase the flexion moment at the knee or hip, potentially exacerbating proximal joint arthrosis.
Operative Versus Non Operative Management
| Clinical Scenario | First-Line Management (Non-Operative) | Indications for Surgical Intervention (Operative) |
|---|---|---|
| Post-Traumatic Midfoot OA | Rigid carbon fiber plate, heel-to-toe rocker sole | Refractory pain, failure of orthotics, progressive arch collapse |
| Charcot Arthropathy (Stage I) | Total Contact Cast (TCC), non-weight bearing | Severe dislocation threatening soft tissue envelope, acute infection |
| Charcot Arthropathy (Stage III) | Custom orthoses, double rocker bottom shoe | Recurrent ulceration despite offloading, severe instability |
| Rheumatoid Midfoot Collapse | Accommodative orthoses, mild rocker sole | Intractable pain, progressive deformity affecting ambulation |
Pre Operative Planning and Patient Positioning
When pedorthic management with rocker bottom soles fails to provide adequate symptomatic relief, or when progressive deformity threatens the viability of the soft tissue envelope, definitive surgical intervention—most commonly midfoot arthrodesis—is indicated.
Clinical and Radiographic Evaluation
Pre-operative planning begins with a meticulous clinical examination to identify the precise joints acting as pain generators. Diagnostic intra-articular injections of local anesthetic under fluoroscopic guidance can isolate pain to specific articulations (e.g., the first tarsometatarsal joint versus the naviculocuneiform joint), ensuring that the subsequent arthrodesis is targeted and avoids unnecessary fusion of asymptomatic joints.
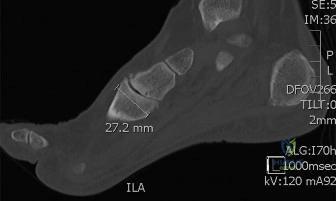
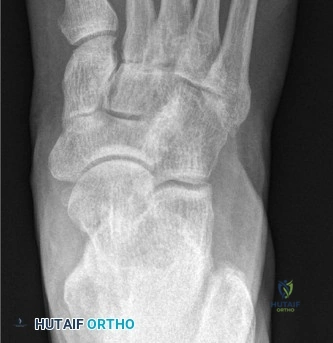
Radiographic evaluation must include weight-bearing anteroposterior (AP), lateral, and oblique views of the foot. On the AP view, the congruency of the medial border of the second metatarsal with the medial border of the middle cuneiform is assessed. On the lateral view, the Meary's angle (the angle between the long axis of the talus and the first metatarsal) is evaluated to quantify sagittal plane collapse. In complex deformities or post-traumatic settings, a non-contrast Computed Tomography (CT) scan is mandatory to map the extent of joint destruction, assess bone stock for hardware purchase, and evaluate for subchondral cysts or avascular necrosis of the navicular.
Patient Positioning and Setup
The patient is positioned supine on the operating table. A bump is placed under the ipsilateral hip to correct the natural external rotation of the lower extremity, ensuring the foot rests strictly in a neutral, upward-facing position. This is critical for accurate assessment of the intra-operative alignment of the medial column. A thigh tourniquet is applied to provide a bloodless surgical field. The fluoroscopy unit (C-arm) is positioned on the contralateral side of the table, draped sterilely, and brought in perpendicular to the foot to allow for unhindered AP, lateral, and oblique imaging throughout the procedure.
Detailed Surgical Approach and Technique
The surgical management of refractory midfoot pain typically involves arthrodesis of the affected joints. The goal is to eradicate pain by eliminating motion across arthritic surfaces while restoring the anatomic alignment of the longitudinal and transverse arches.
Surgical Incisions and Internervous Planes
Access to the midfoot is generally achieved through one or two dorsal longitudinal incisions, depending on the extent of the required arthrodesis.
1. Medial Incision: Centered over the first tarsometatarsal (TMT) joint, extending proximally over the naviculocuneiform (NC) joint if necessary. The dissection is carried down medial to the extensor hallucis longus (EHL) tendon. This approach avoids the primary neurovascular bundle.
2. Lateral Incision: Centered over the second and third TMT joints. The internervous plane lies between the EHL (innervated by the deep peroneal nerve) and the extensor digitorum longus (EDL) (innervated by the superficial peroneal nerve).
Deep dissection requires meticulous identification and mobilization of the extensor hallucis brevis (EHB) muscle belly, which is typically retracted laterally. The dorsalis pedis artery and the deep peroneal nerve run between the first and second metatarsal bases; these structures must be identified, mobilized, and protected with vessel loops throughout the procedure to prevent devastating ischemic or neuropathic complications.
Joint Preparation
Thorough joint preparation is the most critical step in achieving a successful arthrodesis. The capsules of the involved joints are incised, and a lamina spreader or Hintermann retractor is inserted to distract the joint spaces. All articular cartilage is meticulously debrided using curettes and osteotomes down to bleeding subchondral bone.
To preserve the anatomical length and contour of the midfoot, structural bone resection should be minimized unless a corrective wedge osteotomy is planned for severe deformity. Following cartilage removal, the subchondral plates are aggressively fenestrated using a 2.0mm drill bit or a small osteotome (fish-scaling technique) to expose cancellous bone and promote osteogenesis. If significant bone voids are present after debridement, autologous bone graft (often harvested from the proximal tibia or calcaneus) or allograft is packed into the interstices.
Reduction and Fixation Strategies
Reduction of the midfoot deformity must restore the Meary's line on the sagittal plane and close any diastasis between the first and second rays on the coronal plane. Reduction is provisionally held with stout Kirschner wires (K-wires) or reduction clamps.

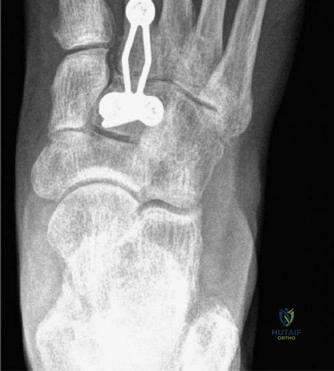
Fixation can be achieved using either solid compression screws or dorsal spanning plates.
* Screw Fixation: Traditional fixation utilizes 3.5mm or 4.0mm solid, fully threaded cortical screws placed in a lag fashion. A "home run" screw is often placed from the medial cuneiform into the base of the second metatarsal to recreate the Lisfranc ligament complex.
* Plate Fixation: Dorsal spanning plates have gained significant popularity, particularly in cases of poor bone quality or when avoiding articular surface violation is desired. Low-profile, pre-contoured locking plates provide rigid biomechanical stability and act as a tension band against the plantar-flexing forces of the forefoot.
Following final fixation, intra-operative fluoroscopy is utilized to confirm hardware placement, joint reduction, and the restoration of the osseous arches. The extensor retinaculum is meticulously repaired to prevent tendon bowstringing, and the skin is closed in a layered fashion.
Complications and Management
Complications can arise from both the conservative pedorthic management (the rocker sole itself) and the definitive surgical intervention. Recognizing and managing these complications is paramount for the orthopedic surgeon.
Pedorthic Complications
While non-invasive, rocker bottom modifications alter the biomechanics of the entire lower extremity kinetic chain. Improper placement of the rocker apex can shift plantar pressures to adjacent, unprotected areas, leading to transfer metatarsalgia or new ulcerations in diabetic patients. Furthermore, the inherent instability of a convex sole can lead to an increased incidence of falls in patients with pre-existing proprioceptive deficits or proximal muscle weakness. Management involves immediate reassessment by a certified pedorthist to adjust the apex position, decrease the angle of the rocker, or widen the base of support.
Surgical Complications
Surgical arthrodesis of the midfoot carries a distinct set of risks, primarily related to bone healing, soft tissue integrity, and hardware.
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage Strategy and Management |
|---|---|---|---|
| Nonunion / Delayed Union | 5% - 15% | Smoking, diabetes, inadequate joint preparation, insufficient rigid fixation. | Prolonged immobilization, bone stimulators. Revision arthrodesis with structural bone grafting and robust locking plate fixation. |
| Hardware Prominence / Pain | 10% - 20% | Thin dorsal soft tissue envelope, use of bulky dorsal plates, screw back-out. | Conservative management with shoe modifications. Hardware removal after definitive radiographic union is confirmed (typically >6-9 months). |
| Wound Dehiscence / Infection | 2% - 8% | Poor vascularity, excessive retraction during surgery, diabetes, smoking. | Aggressive local wound care, targeted oral/IV antibiotics. Surgical debridement and hardware removal if deep infection occurs. |
| Nerve Injury (Deep Peroneal) | 1% - 3% | Iatrogenic traction or direct laceration during the dorsal approach. | Intra-operative repair if recognized. Post-operative management includes gabapentinoids, desensitization, or surgical neurolysis for painful neuromas. |
| Adjacent Segment Disease | Variable | Altered biomechanics transferring stress to the Chopart or TMT joints not included in the fusion. | Conservative management with rocker bottom soles and custom orthotics. Extension of the arthrodesis in refractory cases. |
Post Operative Rehabilitation Protocols
The rehabilitation protocol following midfoot arthrodesis is stringent, designed to protect the delicate osseous healing process while preventing stiffness in the adjacent, unfused joints. The timeline is heavily dependent on patient-specific factors, bone quality, and the rigidity of the fixation achieved intra-operatively.
Phase 1: Immediate Post-Operative (Weeks 0-2)
The primary goals in the initial phase are wound healing, edema control, and pain management. The patient is placed in a well-padded, short-leg bulky Jones splint in neutral dorsiflexion immediately post-operatively. The patient is strictly non-weight-bearing (NWB) on the operative extremity. Elevation of the limb above the level of the heart is mandatory to mitigate swelling, which is a significant risk factor for dorsal wound dehiscence.
Phase 2: Protection and Early Healing (Weeks 2-6)
At the two-week mark, sutures are removed provided the surgical incisions are fully coapted. The patient is transitioned into a rigid fiberglass short-leg cast or a locked Controlled Ankle Motion (CAM) boot. Strict NWB status is maintained. If a CAM boot is utilized, patients may be permitted to remove it strictly for hygiene and gentle, passive range of motion (ROM) exercises of the ankle and metatarsophalangeal joints, provided the midfoot remains unstressed.
Phase 3: Progressive Weight Bearing (Weeks 6-12)
At six weeks post-operatively, updated weight-bearing radiographs are obtained to assess for early trabecular bridging across the arthrodesis sites. If clinical and radiographic signs of healing are progressing satisfactorily, the patient begins a graduated weight-bearing protocol in the CAM boot. This typically starts with 25% partial weight-bearing (PWB) using crutches or a walker, progressing by 25% each week until full weight-bearing (FWB) is achieved. Physical therapy is initiated to focus on intrinsic foot muscle strengthening, ankle ROM, and proprioceptive retraining.
Phase 4: Return to Function and Orthotic Integration (Weeks 12+)
Once clinical union is achieved and the patient is ambulating comfortably in the CAM boot, the transition to standard footwear begins. This is a critical juncture where the concepts of conservative pedorthic management re-enter the clinical pathway. Because the fused midfoot is now a rigid segment, the patient has permanently lost the normal midfoot contribution to the sagittal plane rockers of gait.
To protect the arthrodesis from excessive bending moments and to prevent adjacent segment disease (e.g., subsequent arthritis at the naviculocuneiform or metatarsophalangeal joints), patients are frequently transitioned into a stiff-soled shoe equipped with a custom orthotic and a rocker bottom modification. A mild forefoot or heel-to-toe rocker sole mechanically compensates for the surgically eliminated midfoot motion, facilitating a smooth roll-over during terminal stance and significantly improving long-term functional outcomes.
Summary of Key Literature and Guidelines
The efficacy of both rocker bottom shoe modifications and midfoot arthrodesis has been extensively documented in orthopedic and biomechanical literature.
Biomechanical studies by Janisse et al. have long established the foundational principles of pedorthic modifications, demonstrating that a properly placed rocker apex can reduce plantar pressures in the midfoot and forefoot by up to 30%. This is particularly critical in the management of the diabetic foot, where elevated peak plantar pressures are the primary catalyst for ulceration. Guidelines from the International Working Group on the Diabetic Foot (IWGDF) strongly recommend the use of custom-made footwear with rigid soles and rocker-bottom profiles to prevent the recurrence of plantar foot ulcers in high-risk patients.
In the realm of surgical management, literature regarding midfoot arthrodesis highlights the importance of anatomic reduction and rigid fixation. A landmark study by Kuo et al. on the outcomes of arthrodesis for primary and post-traumatic tarsometatarsal osteoarthritis demonstrated that solid fusion with restoration of the longitudinal arch yields satisfactory functional outcomes in over 80% of patients. However, the literature also consistently warns of the high nonunion rates associated with midfoot fusions, particularly in the diabetic and smoking populations, underscoring the necessity of meticulous joint preparation and robust fixation techniques.
Recent comparative biomechanical studies evaluating fixation constructs have shown that dorsal spanning plates offer superior biomechanical stability against plantar gapping compared to traditional transarticular lag screws. This has led to a paradigm shift in many academic centers toward plate fixation for complex midfoot reconstructions. Ultimately, the literature supports a stepwise approach to midfoot pain: exhausting the biomechanical advantages of rocker bottom soles and orthoses before proceeding to the definitive, yet technically demanding, surgical arthrodesis.
