Introduction & Epidemiology
Midfoot pain is a common and often debilitating complaint in orthopedic practice, arising from a myriad of etiologies including degenerative arthritis, post-traumatic deformity, inflammatory conditions, and neuropathic arthropathy (Charcot foot). The intricate anatomy and complex biomechanics of the midfoot, serving as the critical link between the hindfoot and forefoot, make it particularly susceptible to abnormal loading patterns and subsequent painful sequelae. When conservative measures are pursued, the application of external shoe modifications, specifically the rocker bottom sole, represents a fundamental and highly effective non-surgical strategy for redistributing plantar pressures and mitigating pain.
A rocker bottom modification aims to alter the natural roll-over shape of the foot during gait, facilitating a smoother transition from heel strike to toe-off by effectively shortening the functional lever arm of the foot. This intervention reduces the range of motion required at painful joints, offloads specific plantar pressure points, and decreases muscular effort, thereby providing symptomatic relief. While the concept is decades old, its biomechanical principles remain robust, offering a versatile tool in the orthopedic surgeon's arsenal for managing various midfoot pathologies conservatively. The prevalence of conditions benefiting from rocker bottom soles, such as midfoot osteoarthritis, pes planus deformities, and diabetic foot complications, underscores the broad applicability and importance of understanding this non-operative approach.
Surgical Anatomy & Biomechanics
The midfoot comprises the navicular, cuboid, and three cuneiform bones, articulating with the talus and calcaneus proximally and the metatarsals distally. Key articulations include the talonavicular, calcaneocuboid (Chopart's joint), and the intercuneiform, cuneonavicular, and tarsometatarsal (Lisfranc's joint) articulations.
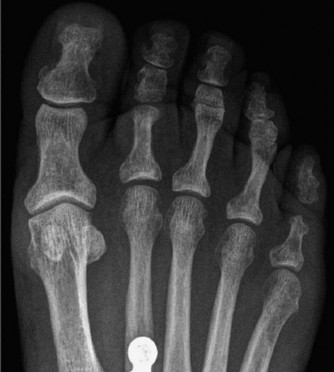
These joints, stabilized by an intricate network of ligaments (e.g., plantar calcaneonavicular or spring ligament, plantar fascia, interosseous ligaments) and musculotendinous units (e.g., tibialis posterior, peroneus longus), form the longitudinal and transverse arches of the foot, crucial for shock absorption and propulsion during ambulation.
Normal gait involves a complex sequence of pronation and supination, facilitated by coordinated muscle activity and joint motion. During the stance phase, the foot progresses through three rockers:
1.
Heel Rocker:
From heel strike to foot flat, primarily governed by the ankle dorsiflexors.
2.
Ankle Rocker:
From foot flat to heel off, involving progression over the tibiotalar joint.
3.
Forefoot Rocker:
From heel off to toe off, involving progression over the metatarsal heads and MTP joints.
Pathologies causing midfoot pain often disrupt the normal progression of these rockers, particularly by restricting motion or causing excessive strain within the midfoot segment.
A rocker bottom shoe modifies the effective rocker mechanism of the foot. By creating a convex sole from the heel to the forefoot, it effectively reduces the leverage of the foot, decreases motion at specific joints, and alters the plantar pressure distribution. The apex of the rocker, known as the "roll-off" point , is strategically placed to offload painful areas. For midfoot pain, the apex is typically positioned proximal to the painful region, often just anterior to the midtarsal joints or at the apex of a deformity, thus reducing forces across these structures. This shifts the center of pressure anteriorly and facilitates a smoother, less strenuous roll-over, bypassing or minimizing painful joint excursions.
Indications & Contraindications
The primary indication for a rocker bottom modification is the relief of midfoot pain stemming from conditions that cause limited or painful motion, abnormal pressure distribution, or structural instability. While this discussion focuses on non-surgical application, it is crucial to recognize the underlying pathologies that may eventually require surgical intervention if conservative measures, including rocker bottom soles, prove insufficient.
Non-Operative Indications for Rocker Bottom Modifications
- Midfoot Osteoarthritis: Degenerative changes in the TMT, cuneonavicular, or talonavicular joints, leading to pain with weight-bearing and motion. The rocker sole reduces joint loading and range of motion.
- Charcot Neuropathic Arthropathy (Midfoot Collapse): Particularly during the chronic, stable phase. The rocker bottom distributes pressure away from bony prominences and helps prevent further collapse or ulceration by creating a stable base and reducing shear forces.
- Severe Pes Planus (Adult Acquired Flatfoot Deformity): Especially when associated with midfoot collapse or arthritis. A rigid rocker sole can provide support and alleviate strain on the medial longitudinal arch structures.
- Plantar Fasciitis/Tendinopathies: While often forefoot or hindfoot related, chronic cases can cause compensatory midfoot pain. Rocker soles reduce strain on the plantar fascia and calf musculature.
- Metatarsalgia (Forefoot origin causing midfoot compensation): When pain in the forefoot (e.g., severe hallux rigidus, MTP synovitis) alters gait, leading to compensatory loading and pain in the midfoot.
- Post-Traumatic Midfoot Deformity: After fractures or dislocations (e.g., Lisfranc injury) that result in residual pain, stiffness, or deformity despite surgical fixation or non-operative healing.
- Rheumatoid Arthritis and other Inflammatory Arthropathies: Leading to midfoot joint destruction and deformity, where reducing motion and load can be beneficial.
- Diabetic Foot Ulcers: Prevention or healing of ulcers, particularly over midfoot prominences, by offloading specific areas.
Contraindications for Rocker Bottom Modifications
Absolute contraindications are few, primarily related to instability that cannot be controlled by the shoe, or open wounds that require direct offloading not achievable by general shoe modifications. Relative contraindications include:
* Acute, unstable fractures or dislocations.
* Severe, rapidly progressing Charcot neuroarthropathy (often requires total contact casting or surgical stabilization).
* Peripheral vascular disease with critical limb ischemia where any pressure alteration might compromise circulation.
* Significant balance impairment, as rocker soles can initially increase instability, especially in elderly patients or those with vestibular dysfunction.
Table of Operative vs. Non-Operative Indications
| Indication | Non-Operative Management (Rocker Bottom Efficacy) | Operative Management (If Non-Op Fails) |
|---|---|---|
| Midfoot Osteoarthritis | High: Reduces joint motion, decreases loading, smooths gait cycle. Often first-line for symptomatic relief. | Tarsometatarsal (TMT) Arthrodesis: For severe, intractable pain and deformity. May be followed by continued rocker sole use to protect adjacent joints. |
| Charcot Neuroarthropathy (Stable Phase) | High: Offloads bony prominences, distributes plantar pressure, prevents ulceration, accommodates deformity. Critical for long-term management. | Exostectomy/Osteotomy: For prominent bony deformities causing ulceration. Arthrodesis/Reconstructive Surgery: For unstable or progressive deformity, often utilizing internal fixation and external support. |
| Severe Pes Planus (Adult Acquired Flatfoot) | Moderate-High: Supports medial arch, reduces strain on Tibialis Posterior, limits excessive pronation. Used in conjunction with orthoses. | Medializing Calcaneal Osteotomy, FDL Transfer, Spring Ligament Repair/Reconstruction, Medial Cuneiform Osteotomy (Cotton osteotomy), Subtalar Arthrodesis, Triple Arthrodesis: Depending on flexibility and severity. |
| Post-Traumatic Midfoot Deformity | Moderate: Addresses residual pain and stiffness by minimizing joint stress. | Corrective Osteotomy, Arthrodesis (TMT or midtarsal): For symptomatic malunion, non-union, or debilitating arthritis following trauma. |
| Rheumatoid/Inflammatory Arthropathy | Moderate-High: Alleviates pain from inflamed/damaged joints, protects against further deformity. | Midfoot Arthrodesis, Synovectomy: For severe joint destruction, instability, or intractable pain. |
| Plantar Fasciitis/Tendinopathies | Low-Moderate: Reduces strain on the plantar fascia and Achilles tendon, indirectly relieving midfoot compensatory pain. Primarily adjunctive. | Gastrocnemius Recession, Plantar Fascia Release, Tendon Debridement/Repair: For refractory cases. |
| Diabetic Foot Ulcers (Midfoot) | High: Crucial for offloading pressure points and promoting ulcer healing. Integrated into a comprehensive wound care regimen. Often used with custom orthoses. | Surgical Debridement, Amputation, Local Flap Coverage: For non-healing ulcers, osteomyelitis, or severe infection. Exostectomy for focal pressure points. |
Pre-Operative Planning & Patient Positioning
While the core topic is non-surgical, understanding pre-operative planning is essential for cases where non-operative management, including rocker bottom modification, has failed and surgical intervention is contemplated for the underlying pathology contributing to midfoot pain. The surgical goal is often to stabilize the midfoot, correct deformity, and achieve a plantigrade foot that can then be effectively managed with continued orthotic and shoe modifications, including rocker bottoms.
Pre-Operative Planning for Midfoot Surgery (e.g., Arthrodesis)
-
Clinical Assessment:
- Thorough history focusing on pain characteristics, duration, previous treatments (including rocker bottom modifications), functional limitations, and patient expectations.
- Physical examination: Assess skin integrity, neurovascular status, range of motion, flexibility vs. fixed deformity, alignment, and gait pattern. Identify specific areas of tenderness or crepitus.
- Associated comorbidities: Diabetes, peripheral neuropathy, peripheral vascular disease, smoking, inflammatory conditions. These critically impact healing and surgical outcomes.
-
Imaging Studies:
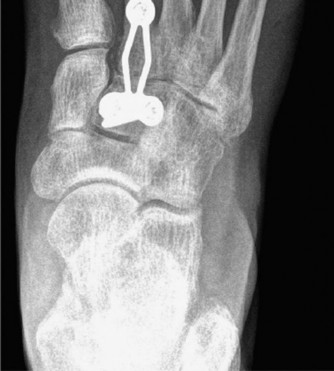
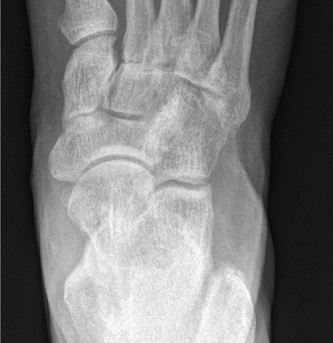
- Weight-bearing Radiographs: Standard anteroposterior, lateral, and oblique views are crucial for assessing bony alignment, joint space narrowing, osteophytes, and deformity. Specific angles (e.g., Meary's angle, lateral talo-first metatarsal angle) provide quantitative assessment of arch collapse.
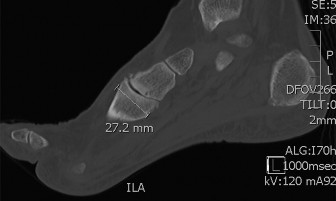
- Computed Tomography (CT): Essential for detailed evaluation of joint destruction, fragmentation (Charcot), fracture morphology, non-unions, and pre-operative planning for hardware placement.
- Magnetic Resonance Imaging (MRI): Useful for assessing soft tissue pathology, stress fractures, synovitis, osteomyelitis, and tendon integrity (e.g., PTTD).
- Bone Scan: May be used to differentiate active Charcot neuroarthropathy from osteomyelitis, though MRI is often preferred.
-
Conservative Management Trial (Prior to Surgery):
- Crucially, a comprehensive trial of non-operative measures, including custom orthoses and rocker bottom shoe modifications, should always precede surgical consideration for chronic midfoot pain. Failure of these measures, despite adequate adherence, is a key indicator for surgery.
- Physical therapy, NSAIDs, activity modification, and corticosteroid injections (if appropriate) should also be considered.
-
Surgical Strategy:
- Goal: Achieve a stable, plantigrade foot, alleviate pain, and optimize for future ambulation, often with external support. This may involve arthrodesis, osteotomy, or soft tissue reconstruction.
- Fixation Plan: Determine type and number of screws, plates, or external fixators based on bone quality, deformity, and stability requirements.
- Bone Grafting: Autograft (e.g., distal tibia, iliac crest) or allograft may be necessary, especially in cases of significant bone loss, Charcot neuroarthropathy, or revision surgery, to enhance fusion rates.
Patient Positioning
- Supine Position: Standard for most dorsal and medial midfoot approaches. A bump under the ipsilateral hip may be used to internally rotate the limb slightly for better access.
- Tourniquet: Applied to the thigh, ensuring adequate exsanguination and inflation pressure.
- Preparation and Draping: Standard sterile prep from mid-thigh to toes. Draping should allow for knee flexion to facilitate ankle dorsiflexion and planterflexion during intra-operative assessment.
- Fluoroscopy: Essential for intra-operative assessment of reduction and hardware placement. The C-arm should be positioned for easy access to obtain AP, lateral, and oblique views.
Detailed Surgical Approach / Technique
Given the non-surgical premise of rocker bottom modification, this section details surgical interventions for chronic midfoot pain that failed conservative management, including rocker bottom soles . The goal of these surgeries is to create a stable, often fused, construct that can then be effectively managed with shoe modifications, or to correct a deformity where a rocker bottom sole might be part of the post-operative management strategy. A common surgical procedure for intractable midfoot pain is midfoot arthrodesis.
Midfoot Arthrodesis (e.g., Tarsometatarsal Arthrodesis)
This procedure aims to fuse one or more TMT joints, commonly the first, second, or third TMT joints, to eliminate pain from degenerative or post-traumatic arthritis, or to correct deformity.
-
Incision and Dissection:
- First TMT Joint: A longitudinal incision centered over the joint, typically 6-8 cm, slightly dorsomedial to the tendon of the tibialis anterior. Care must be taken to protect the saphenous nerve and vein medially and the dorsalis pedis artery laterally.
-
Second and Third TMT Joints:
A second longitudinal incision, typically 8-10 cm, centered dorsally over the interval between the second and third metatarsal bases. The extensor hallucis longus (EHL) and extensor digitorum longus (EDL) tendons are retracted. The deep peroneal nerve and dorsalis pedis artery lie deep to the EHL and EDL, requiring careful retraction.
- Internervous Planes: Dorsal approaches typically utilize intervals between tendons (e.g., EHL and EDL for central TMT joints) to access the joint capsule. Careful subperiosteal dissection exposes the joint surfaces.
-
Joint Preparation:
- The joint capsule is incised, and all articular cartilage is meticulously removed from opposing surfaces of the cuneiforms and metatarsal bases using osteotomes, curettes, and burrs. Subchondral bone should be decorticated to expose cancellous bone, promoting bleeding and fusion.
- Any osteophytes obstructing reduction or contributing to deformity are removed.
-
If significant deformity exists (e.g., dorsal apex in pes planus), a wedge osteotomy may be performed to achieve a plantigrade foot position. Correct alignment is critical; malunion can lead to persistent pain or transfer pathology.
-
Reduction and Provisional Fixation:
- The foot is positioned in appropriate alignment (neutral dorsiflexion/plantarflexion, slight valgus/varus as determined by pre-operative planning).
-
Provisional fixation with K-wires is used to maintain the corrected position and achieve compression across the fusion site. Fluoroscopy is essential to confirm anatomical reduction and proper alignment in all planes.
-
Definitive Fixation:
- Screws: Typically, cannulated screws (e.g., 3.5mm or 4.0mm) are used. Screws should be placed to achieve maximum compression across the arthrodesis site. Bi-cortical purchase is generally preferred for stability. Screws can be placed perpendicular to the fusion site or lag screws across the joint.
- Dorsal Plates: Low-profile locking plates specifically designed for midfoot fusions provide enhanced stability, particularly in osteoporotic bone or complex deformities. Plates are contoured to the dorsal surface and fixed with locking screws.
- Bone Graft: If significant bone loss or poor bone quality is present, autograft or allograft material is packed into the fusion site to enhance healing.
- Final fluoroscopic images are obtained to confirm satisfactory reduction and hardware placement.
-
Closure:
- Irrigation of the surgical field.
- Layered closure of the deep fascia, subcutaneous tissue, and skin. Meticulous skin closure is important to prevent wound complications.
- Sterile dressing and a well-padded splint or cast are applied, maintaining the ankle and foot in a neutral position.
Complications & Management
Surgical interventions for midfoot pathologies carry inherent risks, and even non-surgical management like rocker bottom modifications can have unintended consequences. Understanding and managing these are crucial.
Complications of Midfoot Arthrodesis
| Complication | Incidence | Salvage Strategy |
|---|---|---|
| Non-union | 5-15% | Revision Arthrodesis: Debridement of the non-union site, fresh bone grafting (autograft preferred), rigid internal fixation (often with plates and multiple screws). Biologic augmentation (e.g., BMPs) may be considered. Electrical stimulation. Extended non-weight-bearing. |
| Malunion | 5-10% | Corrective Osteotomy/Revision Arthrodesis: If symptomatic and functionally limiting. May require bone wedge resection or opening wedge osteotomy to restore alignment, followed by stable fixation. Conservative management with custom orthotics/bracing and shoe modifications (e.g., rocker sole) for asymptomatic cases. |
| Infection | 2-5% | Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, intravenous antibiotics (culture-directed), hardware removal (if stable fusion or in acute phase). Irrigation and debridement with retention of hardware if fusion not achieved, followed by staged hardware removal. |
| Hardware Failure/Prominence | 5-10% | Hardware Removal: If symptomatic and fusion is solid. If associated with non-union, revise fixation and fusion. |
| Neurovascular Injury | <1% | Acute: Immediate exploration and repair of vessel/nerve. Chronic Neuropathy: Neuropathic pain management (medications, nerve blocks). Persistent numbness/paresthesia may require protective sensation counseling. |
| Delayed Wound Healing/Dehiscence | 5-15% | Local wound care, strict elevation, offloading, serial debridement. May require primary closure, secondary intention healing, or formal plastic surgical reconstruction (flaps) for severe cases. Risk factors include diabetes, smoking, PVD. |
| Transfer Metatarsalgia | 10-20% | Conservative: Metatarsal pads, custom orthotics, rocker bottom shoes to offload the affected metatarsal heads. Surgical: Shortening osteotomies (e.g., Weil osteotomy) or fusion of the affected MTP joint if conservative measures fail. |
| Complex Regional Pain Syndrome (CRPS) | <1% | Aggressive physical therapy, pharmacological management (e.g., gabapentin, amitriptyline), sympathetic nerve blocks, pain management consultation. |
| Adjacent Joint Arthritis | Long-term risk | Conservative: Activity modification, NSAIDs, orthotics, injections. Surgical: Arthrodesis of the adjacent symptomatic joint. |
Complications Related to Rocker Bottom Modifications (Non-Surgical)
While generally safe, improper application or patient factors can lead to:
*
Balance Instability:
Especially in elderly or neurologically compromised patients, the altered gait pattern can increase fall risk. Careful patient selection and gait training are essential.
*
Pressure Points/Skin Irritation:
If the shoe is not properly fitted or the orthosis is poorly designed, new pressure points can arise, leading to skin breakdown or ulceration.
*
Lack of Efficacy:
If the underlying pathology is too severe or the rocker profile is incorrect, pain relief may not be achieved, necessitating reassessment of the conservative plan or consideration for surgery.
*
Adaptation Period:
Patients may require a period of adjustment to the altered gait mechanics, potentially causing initial discomfort or fatigue.
Post-Operative Rehabilitation Protocols
The rehabilitation protocol following midfoot arthrodesis is crucial for successful fusion, pain management, and return to function. The specific protocol will vary based on the extent of the fusion, stability of fixation, bone quality, and surgeon preference. However, general principles apply.
Phase I: Immediate Post-Operative (Weeks 0-6)
- Goals: Protect fusion site, minimize swelling, pain control, wound healing.
- Weight-Bearing: Strictly non-weight-bearing (NWB) on the operative extremity. Use crutches, walker, or knee scooter.
- Immobilization: Short leg splint initially, followed by a non-weight-bearing cast (plaster or fiberglass).
- Elevation: Continuous elevation above heart level for the first 3-5 days to reduce swelling.
- Cryotherapy: Application of ice packs (intermittently) to further manage swelling and pain.
- Medications: Analgesics for pain control, anti-emetics as needed. Consideration of DVT prophylaxis.
- Wound Care: Monitor incision for signs of infection or delayed healing. Dressing changes as per surgeon protocol.
- Physical Therapy: Focus on exercises for the non-operative extremities and upper body strengthening for ambulation assistance. Gentle range of motion for knee and hip on the operative side.
Phase II: Early Consolidation (Weeks 6-12)
- Goals: Gradual transition to protected weight-bearing, maintain gains, initiation of gentle range of motion (non-fused joints).
- Imaging: Repeat weight-bearing radiographs at 6-8 weeks to assess early signs of fusion.
- Weight-Bearing: Transition from NWB to partial weight-bearing (PWB) in a controlled ankle motion (CAM) boot or short leg cast. Gradual increase in weight-bearing over several weeks, guided by pain and radiographic signs of healing.
- Immobilization: Continued use of CAM boot for protection. Boot can be removed for hygiene and gentle exercises (if indicated for non-fused joints).
-
Physical Therapy:
- Initiate gentle ankle range of motion (dorsiflexion/plantarflexion) and toe range of motion exercises (if not fused). Avoid motion at the fusion site.
- Isometrics for calf and intrinsic foot muscles (within pain limits).
- Balance and proprioception training (non-weight-bearing initially, progressing to PWB).
- Gait training with assistive devices.
Phase III: Advanced Consolidation & Strengthening (Weeks 12-24)
- Goals: Full weight-bearing, restore strength, improve gait mechanics, progress functional activities.
- Imaging: Repeat weight-bearing radiographs at 12-16 weeks to confirm union. CT scan may be considered if union remains equivocal and clinically indicated.
- Weight-Bearing: Progress to full weight-bearing (FWB) in the CAM boot, then transition to supportive shoes with custom orthotics and rocker bottom modification .
-
Physical Therapy:
- Continue range of motion for non-fused joints.
- Progress strengthening exercises: calf raises, toe raises, resistance band exercises for ankle eversion/inversion.
- Advanced balance and proprioception drills.
- Gait analysis and correction.
- Introduction of light impact activities (e.g., walking, elliptical) as tolerated and fusion progresses.
-
Shoe Wear:
Permanent use of supportive, rigid-soled footwear with custom orthoses and often a rocker bottom modification is advised to protect the fused segment and adjacent joints.

Phase IV: Return to Activity (Months 6+)
- Goals: Gradual return to desired activities, long-term maintenance.
- Activity Progression: Progressive return to higher impact activities or sports, guided by pain, strength, and functional assessment. This is often limited after midfoot fusions.
- Long-term Management: Lifelong commitment to appropriate footwear (supportive, rigid sole, rocker modification) and orthotics is crucial to prevent symptoms in adjacent joints or recurrence of deformity. Regular follow-up for monitoring.
Summary of Key Literature / Guidelines
The evidence supporting both the non-operative use of rocker bottom modifications and the surgical management of midfoot pathologies is robust, albeit with varying levels of evidence depending on the specific condition.
Rocker Bottom Modifications
- Biomechanics: Multiple studies, often using pressure plate analysis, have demonstrated that rocker bottom shoes significantly reduce plantar pressures, particularly under the forefoot and midfoot. For example, van Schie et al. (2009) showed that rocker soles effectively offload the metatarsal heads. A systematic review by Bus and Waaijman (2018) highlighted the effectiveness of various offloading devices, including rocker soles, in reducing plantar pressure in diabetic foot complications.
- Clinical Efficacy: For conditions like severe hallux rigidus, midfoot osteoarthritis, and Charcot neuroarthropathy, rocker bottom soles consistently show clinical benefit in pain reduction and functional improvement. Pinzur (2004) emphasized the role of shoe modifications in managing neuropathic foot deformities, including rocker soles for Charcot. Their utility in offloading and preventing ulceration in diabetic patients is well-established in guidelines by the International Working Group on the Diabetic Foot (IWGDF).
- Customization: The precise design of the rocker (apex location, radius of curvature) can be customized based on the specific pathology and pain location. Research by Telfer et al. (2010) demonstrated that different rocker profiles alter plantar pressures differently, underscoring the importance of tailored prescription.
Midfoot Arthrodesis
- Indications: Guidelines from the American Academy of Orthopaedic Surgeons (AAOS) and other professional bodies generally support midfoot arthrodesis for painful, debilitating, and often rigid deformities of the midfoot that have failed a comprehensive trial of non-operative management.
- Fusion Rates: Studies on midfoot arthrodesis (e.g., TMT fusion for osteoarthritis or pes planus correction) report fusion rates ranging from 80% to 95%. Factors affecting fusion include bone quality, extent of fusion, smoking status, and adequacy of fixation. Myerson et al. (2004) provided extensive outcomes for Lisfranc injuries and subsequent fusions.
- Outcomes: Patients typically report significant pain reduction and improved functional scores following successful midfoot arthrodesis. However, persistent gait abnormalities and the need for continued supportive footwear are common. Adjacent joint arthritis remains a long-term concern, with some studies indicating increased risk in unfused adjacent joints (Cho et al., 2005).
- Charcot Neuroarthropathy: Arthrodesis in Charcot foot management is complex but often necessary for unstable deformities. Studies by Schon et al. (2009) and Wukich et al. (2014) demonstrate acceptable fusion rates with improved stability, though complication rates (non-union, infection) are higher in this population. The overarching goal is a stable, plantigrade foot amenable to bracing and orthotic management, including specialized rocker bottom shoes.
In summary, rocker bottom modifications represent a cornerstone of conservative management for various midfoot pathologies, often providing substantial symptomatic relief by altering biomechanical forces. When conservative measures fail, surgical interventions, particularly arthrodesis, aim to stabilize and correct underlying deformities, with the understanding that post-operative rehabilitation and long-term management will frequently involve continued use of specialized footwear, often incorporating a rocker sole, to optimize function and protect the reconstructed foot.
Clinical & Radiographic Imaging