Ankle Reduction Blocked? Check the Extensor Digitorum Brevis
Introduction & Epidemiology
Ankle fractures represent one of the most common skeletal injuries encountered by orthopedic surgeons, with an incidence estimated at 100-180 per 100,000 person-years. These injuries encompass a spectrum from simple, stable malleolar fractures to complex fracture-dislocations involving multiple osseous structures and the syndesmosis. The fundamental principle guiding treatment, particularly for displaced and unstable patterns, is the anatomical reduction of the ankle mortise and stable internal fixation to restore congruence and allow for early functional rehabilitation, thereby minimizing the risk of post-traumatic arthritis.
While successful closed reduction is often achievable, a significant challenge arises when anatomical reduction is blocked or incomplete despite appropriate manipulative techniques. Such a scenario mandates careful evaluation for mechanical impediments. Common causes of blocked reduction include interposed osteochondral fragments, incarcerated deltoid ligament, tibialis posterior tendon, flexor hallucis longus tendon, or even the posterior talofibular ligament. However, a less frequently recognized, yet critical, cause of blocked reduction, particularly in specific patterns of lateral malleolar fractures or posteromedial ankle dislocations, is the interposition of the Extensor Digitorum Brevis (EDB) muscle or its tendinous components. Awareness of this potential soft tissue block is paramount for achieving accurate and stable reduction during open reduction and internal fixation (ORIF) and preventing operative failure or subsequent complications.
Surgical Anatomy & Biomechanics
Successful management of ankle fractures necessitates a thorough understanding of the complex surgical anatomy and biomechanics of the talocrural joint.
Bony Anatomy
The ankle joint is a synovial hinge joint formed by the distal tibia (plafond, medial malleolus, and posterior malleolus), the distal fibula (lateral malleolus), and the talus. The tibial plafond forms the superior articulation, while the medial and lateral malleoli create a mortise that cradles the body of the talus. The integrity of this mortise is crucial for ankle stability and function.
Ligamentous Anatomy
Key ligamentous structures providing stability include:
*
Medial (Deltoid) Ligament Complex:
A strong, fan-shaped ligament connecting the medial malleolus to the talus, navicular, and calcaneus. It resists eversion and external rotation forces.
*
Lateral Ligament Complex:
Comprises the anterior talofibular ligament (ATFL), calcaneofibular ligament (CFL), and posterior talofibular ligament (PTFL). These resist inversion and internal rotation. The ATFL is the weakest and most commonly injured.
*
Syndesmotic Ligaments:
A group of ligaments (anterior inferior tibiofibular ligament (AITFL), posterior inferior tibiofibular ligament (PITFL), interosseous membrane, and inferior transverse ligament) that bind the distal tibia and fibula, maintaining the fibula's position within the incisura and preserving the mortise. Disruption leads to ankle instability.
Musculotendinous Structures and Neurovascular Bundles
Muscles and their tendons around the ankle are organized into four compartments:
*
Anterior Compartment:
Tibialis anterior, Extensor Hallucis Longus (EHL), Extensor Digitorum Longus (EDL), Peroneus Tertius. These tendons can occasionally block reduction. The deep peroneal nerve and anterior tibial artery course through this compartment.
*
Lateral Compartment:
Peroneus longus and brevis. The superficial peroneal nerve is superficial to the peronei.
*
Deep Posterior Compartment:
Tibialis posterior, Flexor Digitorum Longus (FDL), Flexor Hallucis Longus (FHL). The posterior tibial nerve and artery are found here. Both Tibialis posterior and FHL have been reported as causes of blocked reduction, particularly in posteromedial dislocations.
*
Superficial Posterior Compartment:
Gastrocnemius and Soleus (Achilles tendon).
Extensor Digitorum Brevis (EDB)
The EDB is a small, intrinsic muscle of the foot located on the dorsum.
*
Origin:
Superolateral surface of the calcaneus, anterior to the calcaneal sulcus, and from the lateral sinus tarsi.
*
Insertion:
Divides into four tendons. The medial tendon, often larger and sometimes considered a separate muscle (Extensor Hallucis Brevis), inserts into the dorsal aspect of the proximal phalanx of the great toe. The other three tendons join the lateral three tendons of the Extensor Digitorum Longus (EDL) to insert into the middle and distal phalanges of the 2nd, 3rd, and 4th toes, forming the extensor hoods.
*
Innervation:
Deep peroneal nerve.
*
Blood Supply:
Dorsalis pedis artery (a continuation of the anterior tibial artery).
*
Relevance to Blocked Reduction:
In specific high-energy ankle fracture-dislocations, particularly those with significant talar displacement (e.g., posteromedial dislocation with lateral malleolus fracture), the EDB muscle belly or one of its tendinous slips can become entrapped within the fracture site of the lateral malleolus or between the talus and the distal fibula. This interposition mechanically prevents accurate reduction of the lateral malleolus to the fibular incisura or reduction of the talus into the mortise. Its anatomical position over the tarsal bones and its attachment to the calcaneus makes it susceptible to displacement and interposition during traumatic events that disrupt the lateral ankle structures.
Biomechanics of Ankle Stability
The ankle joint is inherently stable due to the congruent mortise and strong ligamentous restraints. Fracture-dislocations typically result from combined rotational and axial loading forces. Disruption of the lateral malleolus, medial malleolus/deltoid ligament, and/or syndesmosis leads to instability, allowing talar shift and mortise widening. Anatomical reduction restores the talar dome's contact with the tibial plafond, ensuring even load distribution and preventing abnormal stresses that can lead to post-traumatic arthrosis. Failure to achieve anatomical reduction, often due to soft tissue interposition like the EDB, directly compromises these biomechanical principles.
Indications & Contraindications
The decision for operative versus non-operative management of ankle fractures is guided by fracture stability, displacement, patient factors, and the presence of open wounds or neurovascular compromise.
Indications for Open Reduction Internal Fixation (ORIF)
-
Displaced, unstable ankle fractures:
- Bimalleolar fractures.
- Trimalleolar fractures.
- Unstable unimalleolar fractures (e.g., displaced lateral malleolus with medial clear space widening, or a displaced medial malleolus).
- Fractures with syndesmotic disruption (diastasis).
- Talar shift > 2 mm.
- Open ankle fractures: Require emergent irrigation, debridement, and stabilization.
- Fractures with neurovascular compromise: Prompt reduction and stabilization.
- Blocked reduction: The inability to achieve anatomical closed reduction due to mechanical obstruction, which is the primary focus of this discussion concerning EDB interposition.
- Pilon fractures: Intra-articular distal tibial fractures often requiring ORIF.
Specific Indication for EDB-Related Blockage
Suspicion of EDB interposition arises when:
* Closed reduction attempts repeatedly fail to achieve anatomical alignment, particularly in valgus-external rotation injuries with lateral malleolus fracture and talar displacement.
* Intraoperative findings during a lateral approach reveal soft tissue (muscle or tendon) caught within the fracture site or between the fibula and talus/tibia, preventing full reduction.
Contraindications for ORIF
-
Absolute Contraindications:
- Severe, uncontrolled systemic comorbidities precluding anesthesia and surgery.
- Active local infection (e.g., cellulitis) at the surgical site, though this may be delayed for management.
- Severe, irreparable soft tissue damage or extensive skin loss that prevents wound closure.
-
Relative Contraindications:
- Extensive peripheral vascular disease.
- Severe neuropathy (e.g., Charcot arthropathy).
- Poor skin integrity (e.g., severe blistering, edema) requiring staged management.
- Uncontrolled diabetes mellitus.
- Non-ambulatory or very low-demand patients who may tolerate malunion or non-union.
Summary Table: Operative vs. Non-Operative Indications
| Indication Type | Operative Management | Non-Operative Management |
|---|---|---|
| Fracture Pattern | Displaced bimalleolar, trimalleolar, unstable unimalleolar; pilon fractures | Stable unimalleolar (e.g., non-displaced lateral malleolus, non-displaced posterior malleolus <25% articular involvement) |
| Stability | Syndesmotic disruption, talar shift > 2mm, medial clear space widening, mortise incongruity | Intact syndesmosis, stable mortise, congruent talus on stress views (if indicated) |
| Soft Tissue | Open fractures, threatened skin (e.g., tenting), blocked reduction (e.g., EDB interposition, osteochondral fragments, deltoid interposition) | Closed, minimal soft tissue swelling, no skin compromise |
| Patient Factors | Young, active individuals requiring anatomical reduction and early mobilization; poly-trauma patients requiring definitive stabilization | Elderly, low demand, significant comorbidities precluding surgery, non-ambulatory status, severe osteopenia where hardware fixation is unlikely to hold |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for optimizing outcomes in ankle fracture management, particularly when anticipating potential challenges like blocked reduction.
Pre-Operative Assessment and Imaging
- Clinical Evaluation: Thorough history and physical examination, including neurovascular status, skin condition, and assessment of swelling and ecchymosis.
-
Standard Radiographs:
- Anteroposterior (AP), lateral, and mortise views of the affected ankle.
- Full-length tibia/fibula views to rule out proximal fibula fractures (Maisonneuve injury) in cases of syndesmotic disruption.
- Contralateral ankle views can be useful for comparison, especially for syndesmotic assessment.
-
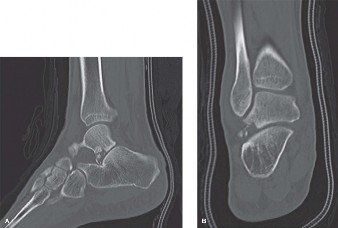
Computed Tomography (CT) Scan:
- Strongly recommended for complex fracture patterns (e.g., trimalleolar, pilon fractures) to delineate articular involvement, fracture comminution, and the presence of osteochondral fragments.
- Highly valuable in identifying potential soft tissue interposition pre-operatively, though EDB interposition might not always be clearly evident.
- Provides a 3D understanding of the deformity and helps plan implant placement.
- Stress Radiographs: May be considered in certain cases to assess syndesmotic stability, though intraoperative fluoroscopic stress testing is often preferred.
- Patient Optimization: Address any systemic comorbidities (diabetes, peripheral vascular disease), optimize nutritional status, and ensure smoking cessation if possible to minimize surgical risks. Delay surgery if significant soft tissue swelling or blistering is present, unless the injury is an open fracture or involves neurovascular compromise.
Anesthesia and Patient Positioning
- Anesthesia: Typically general anesthesia or regional anesthesia (spinal or epidural), often supplemented with a popliteal nerve block for post-operative pain control.
-
Patient Positioning:
- Supine position on a radiolucent table is standard.
- A small bump or roll is often placed under the ipsilateral hip to internally rotate the limb slightly, presenting the lateral malleolus more directly to the surgeon.
- The operative leg is draped free to allow for full range of motion of the knee and ankle, and access to fluoroscopy.
- Fluoroscopy: The C-arm should be positioned for easy access to obtain AP, lateral, and mortise views without repositioning the patient.
- Tourniquet: A thigh tourniquet is routinely used to maintain a bloodless field, typically inflated to 100 mmHg above systolic blood pressure, or a fixed pressure of 300-350 mmHg. This is essential for clear visualization, especially when searching for subtle soft tissue blocks.
- Ensure the ability to perform a posteromedial approach if needed for posterior malleolus or extensive medial displacement. This may necessitate a prone or lateral decubitus position for trimalleolar fractures with significant posterior fragment, but for EDB-related issues, supine is generally sufficient for the initial lateral approach.
Detailed Surgical Approach / Technique
The primary goal of surgical management for unstable ankle fractures is anatomical reduction of the joint surfaces and stable internal fixation, restoring mechanical axes and facilitating early rehabilitation. When faced with a blocked reduction, systematic exploration for mechanical impediments, including the EDB, is crucial.
General Principles of ORIF
- Incisions: Strategically placed to provide adequate exposure while respecting soft tissue envelopes, neurovascular structures, and potential future revisions.
- Soft Tissue Handling: Minimize soft tissue stripping to preserve periosteal blood supply.
- Reduction: Achieved indirectly (traction, manipulation) followed by direct reduction (clamps, elevators).
- Fixation: Stable, rigid fixation to allow for early motion.
Surgical Approach for Lateral Malleolus Fracture (Commonly Associated with EDB Interposition)
The lateral malleolus is most frequently involved in EDB-related blocked reductions.
1.
Incision:
A straight or slightly curvilinear longitudinal incision centered over the distal fibula. The incision typically extends from approximately 5 cm proximal to the tip of the lateral malleolus to the level of the calcaneus, respecting Langer's lines where possible.
2.
Dissection:
* Carefully incise the skin and subcutaneous tissue. Identify and protect the
superficial peroneal nerve (SPN)
and its branches, which cross the ankle anteriorly. Aggressive retraction or direct injury to the SPN can lead to sensory deficits or painful neuromas.
* Elevate full-thickness skin flaps (skin and subcutaneous fat) anteriorly and posteriorly to expose the distal fibula and fracture site.
* Incise the anterior ligamentous structures to visualize the fracture.
*
Crucial Step for EDB Interposition:
Once the fracture site of the lateral malleolus is exposed, if reduction is still difficult or incomplete despite direct manipulation, a high index of suspicion for soft tissue interposition is warranted.
* Visually inspect the fracture site between the fibula and the talus/tibia. The
Extensor Digitorum Brevis (EDB)
muscle belly or one of its tendinous slips can be seen interposed. It typically appears as a reddish-brown muscle belly or glistening white tendon within the fracture gap or wedged between the talus and fibular fragment.
*
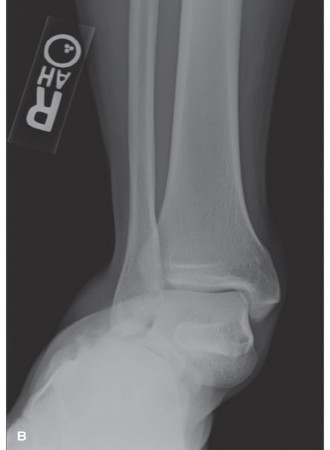
(Insert image of anatomical relationship of EDB in context of lateral malleolus or potential interposition)
*
Management of EDB Interposition:
Gently retract the EDB muscle belly or tendon, usually anteriorly or superiorly, using a small blunt retractor (e.g., Hohmann retractor, Senn retractor, or even a dental pick). Avoid excessive force to prevent muscle damage. Once the EDB is cleared from the fracture site, anatomical reduction should become readily achievable.
*
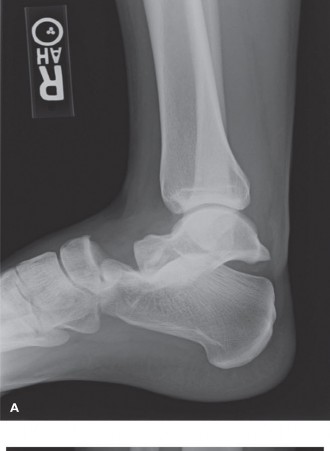
(Insert image potentially showing EDB interposition or intraoperative view of clearance)
Reduction and Fixation of Lateral Malleolus
- Reduction: Once the EDB or other soft tissue is cleared, reduce the lateral malleolus anatomically to the fibular shaft. This is often achieved using bone-holding clamps (e.g., pointed reduction forceps) placed carefully to avoid comminution. Ensure rotational and length restoration.
- Provisional Fixation: Secure the reduction with two K-wires.
-
Definitive Fixation:
- Lag Screw(s): If the fracture pattern allows for a lag screw (oblique fracture line), place one or two partially threaded cortical screws across the fracture site for interfragmentary compression.
-
Neutralization Plate:
Apply a neutralization plate (e.g., one-third tubular plate, LCP, or pre-contoured locking plate) to the lateral or posterolateral aspect of the fibula. The plate neutralizes rotational and bending forces. Ensure adequate screw purchase proximal and distal to the fracture.
- Typically, 3-4 cortices of screw purchase proximally and distally are desired.
- Place the plate on the tension side (lateral aspect) or posterolaterally, which provides better biomechanical stability and potentially reduces skin irritation.
Surgical Approach for Medial Malleolus Fracture
- Incision: A longitudinal incision either anteromedial or posteromedial over the medial malleolus. The anteromedial approach provides better visualization of the ankle joint and potential osteochondral fragments.
- Dissection: Carefully identify and protect the saphenous nerve and vein anteriorly. If using a posteromedial approach, protect the posterior tibial neurovascular bundle and tibialis posterior tendon.
- Addressing Blocked Reduction (Medial Side): Inspect for deltoid ligament interposition or osteochondral fragments. If present, gently retract or remove.
- Reduction & Fixation: Reduce the medial malleolus anatomically. Fixation typically involves two cancellous screws (partially threaded, 3.5mm or 4.0mm) or K-wires with a tension band wiring technique, depending on fracture morphology and comminution.
Surgical Approach for Posterior Malleolus Fracture (Trimalleolar Fractures)
-
Approach Selection:
- Indirect Fixation (from anterior): If the fragment is small (<25% of articular surface) and can be reduced with ankle dorsiflexion, lag screws can be placed from anterior to posterior through the tibial metaphysis.
- Direct Fixation (from posterior): For larger fragments (>25-30% of articular surface, or those involving the posterolateral aspect and syndesmotic attachment), direct reduction and buttress plating are often preferred. This requires a posterolateral or posteromedial approach. A posterolateral approach (through interval between peroneals and FHL) provides good access to the posterolateral fragment.
- Reduction & Fixation: Anatomical reduction of the posterior malleolus is critical for joint congruence and syndesmotic stability. Provisional K-wire fixation, followed by lag screw fixation or buttress plating (e.g., 1/4 tubular or small fragment plate).
Syndesmotic Fixation
- Assessment: After fixing the malleolar fractures, assess syndesmotic stability using intraoperative stress tests (e.g., external rotation stress test, hook test). A stable syndesmosis is crucial for mortise integrity.
- Reduction: Reduce the fibula into the tibial incisura. Place the foot in neutral dorsiflexion and apply an anterior-to-posterior translational force on the fibula.
-
Fixation:
- Syndesmotic Screw(s): Typically one or two 3.5 mm or 4.5 mm cortical screws, placed 2-3 cm proximal to the tibial plafond, traversing 3 or 4 cortices. One tricortical screw is often sufficient for rotational stability; a quadricortical screw provides increased stiffness. The most common pitfall is over-compression.
- Suture Button Devices (e.g., TightRope): Increasingly popular, these devices provide dynamic fixation, allowing for micro-motion and avoiding the need for routine hardware removal. They are placed similarly to syndesmotic screws.
-
(Insert image showing syndesmotic fixation, e.g., screw or suture button)
- Final Assessment: Re-evaluate ankle mortise congruence and stability with fluoroscopy in AP, lateral, and mortise views, through a full range of motion.
Wound Closure
- Copious irrigation of the surgical site.
- Achieve meticulous hemostasis.
- Close the deep fascial layers where possible without tension.
- Subcutaneous and skin closure using non-absorbable sutures or staples.
- Apply a sterile dressing and a well-padded splint in a neutral position.
Complications & Management
Despite meticulous surgical technique, ankle fracture ORIF is associated with a range of potential complications. A clear understanding of these, their incidence, and management strategies is essential for effective patient care.
General Complications
-
Surgical Site Infection (SSI):
Can be superficial or deep.
- Incidence: 1-5% for superficial, <1% for deep. Higher in open fractures, diabetic patients, smokers, and those with poor soft tissue envelopes.
- Management: Superficial infections often respond to oral antibiotics and local wound care. Deep infections require surgical debridement, intravenous antibiotics, and sometimes hardware removal, especially if fixation is compromised or union is achieved.
-
Wound Dehiscence/Necrosis:
Risk factors include excessive tension on skin edges, poor soft tissue quality, hematoma, and infection.
- Incidence: 1-3%.
- Management: Local wound care, negative pressure wound therapy (NPWT), secondary closure, or formal plastic surgery consultation for skin grafting or flap coverage.
-
Malunion/Nonunion:
Failure to achieve anatomical reduction or osseous healing.
- Incidence: 1-5%.
- Management: Symptomatic malunion may require corrective osteotomy and revision ORIF. Nonunion typically requires revision surgery with bone grafting and stable fixation.
-
Post-Traumatic Arthritis:
The most common long-term complication, occurring even with anatomical reduction, due to initial cartilage damage.
- Incidence: 10-20% at 5-10 years, increasing over time.
- Management: Initial conservative (NSAIDs, activity modification, bracing, intra-articular injections). For severe, symptomatic arthritis, surgical options include arthroscopic debridement, ankle arthrodesis, or total ankle arthroplasty in selected patients.
-
Hardware-Related Symptoms:
Irritation from prominent plates, screws, or syndesmotic screws.
- Incidence: 10-30%. Syndesmotic screws are often removed electively.
- Management: Symptomatic hardware removal after fracture healing (typically 6-12 months post-operatively).
-
Neurovascular Injury:
Direct injury to nerves (superficial peroneal, saphenous, sural) or vessels.
- Incidence: <1%.
- Management: Prevention through meticulous dissection. Intraoperative repair if identified. Post-operative management depends on the extent of injury.
-
Complex Regional Pain Syndrome (CRPS):
A chronic pain condition.
- Incidence: 2-5%.
- Management: Multimodal approach including physical therapy, pain medication, sympathetic blocks, and psychological support.
-
Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE):
Thromboembolic events.
- Incidence: 0.5-2%.
- Management: Prophylactic anticoagulation (LMWH, aspirin) in high-risk patients. Therapeutic anticoagulation for confirmed events.
Complications Specific to Blocked Reduction / EDB Interposition
-
Incomplete Reduction:
If EDB interposition is missed or inadequately addressed, the ankle joint will remain subluxed or malreduced, leading to early onset of post-traumatic arthritis, chronic pain, and functional limitations. This is a critical intraoperative error.
- Management: Immediate re-exploration and definitive clearance of the interposing tissue. If discovered post-operatively, revision surgery (osteotomy, hardware revision) may be required depending on the degree of malunion and patient symptoms.
-
Further Soft Tissue Damage:
Aggressive or repeated attempts at closed reduction against a mechanical block can cause further soft tissue tearing, increasing swelling, ecchymosis, and risk of wound complications.
- Management: Recognition and conversion to open reduction to directly address the block.
Summary Table: Common Complications and Management
| Complication | Incidence | Salvage Strategies |
|---|---|---|
| Surgical Site Infection | 1-5% (superficial), <1% (deep) | Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, IV antibiotics, hardware retention/removal depending on stability and pathogen, negative pressure wound therapy (NPWT). |
| Wound Dehiscence / Necrosis | 1-3% | Local wound care, NPWT, primary or secondary closure, skin grafting, flap coverage. |
| Malunion / Nonunion | 1-5% | Corrective osteotomy and revision ORIF with bone grafting for symptomatic malunion; revision ORIF, bone grafting, electrical stimulation for nonunion. |
| Post-Traumatic Arthritis | 10-20% | Non-operative management (NSAIDs, injections, bracing), ankle arthrodesis, total ankle arthroplasty (in selected patients). |
| Hardware-Related Symptoms | 10-30% | Symptomatic hardware removal (typically 6-12 months post-op for syndesmotic screws, longer for plates). |
| Neurovascular Injury | <1% | Intraoperative repair, watchful waiting, referral to vascular/neurosurgeon. Prevention by meticulous dissection. |
| Complex Regional Pain Syndrome | 2-5% | Multimodal pain management (medications, PT, O.T.), sympathetic blocks, psychological support. |
| DVT / Pulmonary Embolism | 0.5-2% | Prophylactic anticoagulation (LMWH, aspirin); therapeutic anticoagulation for confirmed events. |
| Missed Soft Tissue Interposition | Rare, but under-reported | Re-exploration and anatomical reduction with appropriate soft tissue release/retraction. Revision surgery if identified post-operatively and leading to malunion/nonunion. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing functional outcomes, preventing stiffness, and facilitating a safe return to activity after ankle fracture ORIF. Protocols vary based on fracture stability, quality of fixation, patient comorbidities, and surgeon preference.
Immediate Post-Operative Period (0-2 Weeks)
-
Immobilization:
- Initial bulky soft dressing and posterior splint, maintaining the ankle in a neutral position to accommodate swelling.
- Transition to a short leg cast or removable walking boot once swelling subsides and sutures are removed (typically 10-14 days).
- Weight-Bearing: Non-weight bearing (NWB) on the operative extremity. Crutches, walker, or knee scooter for ambulation.
- Elevation & Edema Control: Strict elevation above heart level to minimize swelling. Ice application.
-
Range of Motion (ROM):
- Active ROM of the toes, knee, and hip of the operative leg to prevent stiffness and promote circulation.
- Isometric quadriceps and gluteal strengthening exercises.
- Pain Management: Opioids, NSAIDs, nerve blocks, multimodal analgesia.
Early Mobilization Phase (2-6 Weeks)
- Immobilization: Continue use of a short leg cast or removable boot.
-
Weight-Bearing:
- Maintain NWB for fractures requiring longer healing (e.g., severe comminution, poor bone quality, syndesmotic injury without dynamic fixation).
- For stable fixations without syndesmotic repair or with suture button fixation, some surgeons may initiate protected weight-bearing (PWB) in a boot (25-50% body weight) at 3-4 weeks, gradually increasing.
-
Range of Motion (ROM):
- If in a removable boot, begin gentle active and passive ankle dorsiflexion, plantarflexion, inversion, and eversion exercises (e.g., ankle alphabet) 3-4 times daily, out of the boot.
- Focus on pain-free motion within tolerance.
- Strengthening: Continue isometric exercises for ankle musculature (e.g., pushing against a wall).
Progressive Rehabilitation Phase (6-12 Weeks)
-
Immobilization:
- Transition from boot to supportive lace-up ankle brace (e.g., ASO) once radiographic healing is evident and pain-free full weight-bearing (FWB) is achieved.
- Syndesmotic screws, if placed, may be removed around 8-12 weeks if symptomatic or if dynamic fixation was not used.
-
Weight-Bearing:
- Progress to FWB as tolerated, first in the boot, then in an athletic shoe with ankle brace support.
- Range of Motion (ROM): Continue aggressive ROM exercises to regain full ankle motion. Manual therapy by a physical therapist may be beneficial for joint mobilization.
-
Strengthening:
- Progressive strengthening exercises for all ankle muscle groups using resistance bands, light weights, and body weight.
- Focus on calf raises (bilateral, then unilateral), heel walks, toe walks.
- Initiate proprioception and balance training (e.g., single-leg stance, wobble board).
- Gait Training: Focus on normal heel-toe gait pattern.
Advanced Rehabilitation & Return to Activity (3-6+ Months)
- Bracing: Continue ankle brace for high-impact activities or sports for several months.
-
Strengthening & Conditioning:
- Advanced strengthening exercises, plyometrics, agility drills, and sport-specific training.
- Address any residual strength or balance deficits.
-
Return to Activity:
- Gradual return to recreational activities and sports. High-impact sports typically require 4-6 months, sometimes longer, depending on the severity of the injury and functional recovery.
- Clearance for full activity should be based on pain levels, full ROM, adequate strength, and confidence in the injured ankle.
- Specific considerations for EDB-related issues: No significant deviation from general ankle fracture protocols. The focus remains on fracture healing and restoring ankle mechanics. Damage to the EDB is typically minimal due to careful retraction.
Summary of Key Literature / Guidelines
The management of ankle fractures has evolved significantly, underpinned by a robust body of literature and clinical guidelines. The principles of anatomical reduction and stable internal fixation, particularly for unstable injuries, are well-established and supported by Level I evidence, demonstrating improved functional outcomes and reduced rates of post-traumatic arthritis compared to non-operative management of displaced fractures.
Key literature and guidelines generally emphasize:
1.
AO/OTA Classification:
Widely used for classifying ankle fractures, providing a standardized language for describing fracture morphology and guiding treatment strategies.
2.
Lauge-Hansen Classification:
Describes the mechanism of injury (e.g., supination-eversion, pronation-abduction), which can help predict fracture patterns and associated ligamentous injuries, including the potential for soft tissue interposition.
3.
Importance of Syndesmotic Stability:
Numerous studies highlight that accurate assessment and reduction of the syndesmosis are critical. Malreduction of the syndesmosis (even 1-2 mm) has been shown to significantly alter contact pressures across the ankle joint, predisposing to early arthritis. Both traditional screw fixation and modern suture button devices (e.g., TightRope) have demonstrated comparable outcomes, with the latter offering potential advantages of dynamic fixation and avoiding routine hardware removal.
4.
Role of Posterior Malleolus Fixation:
Recent literature supports routine fixation of posterior malleolus fragments larger than 25% of the articular surface, especially those involving the posterolateral aspect, due to their significant contribution to ankle stability and risk of instability if left unaddressed.
5.
Soft Tissue Interposition as a Block to Reduction:
While osteochondral fragments and other larger structures like the deltoid ligament are well-documented causes of blocked reduction, the role of specific tendons and muscles is increasingly recognized.
*
Extensor Digitorum Brevis (EDB) Interposition:
Although historically less emphasized, case reports and small series in orthopedic literature have highlighted the EDB as a rare but definite cause of blocked ankle reduction. These reports often detail scenarios of high-energy pronation-abduction or supination-external rotation injuries resulting in lateral malleolus fractures and significant talar displacement (e.g., posteromedial subluxation). Intraoperative findings confirm the EDB muscle belly or one of its tendinous slips (particularly the EHB portion) entrapped within the fracture site or between the fibula and talus. The key takeaway from this literature is the necessity for
intraoperative vigilance
and thorough inspection of the fracture site when anatomical reduction cannot be easily achieved. Failure to recognize and address EDB interposition will inevitably lead to malreduction and poor long-term outcomes.
* Other soft tissue blocks like the tibialis posterior and flexor hallucis longus tendons have been reported, primarily in posteromedial dislocations of the talus.
Conclusion:
In summary, the optimal management of unstable ankle fractures demands not only a deep understanding of osseous and ligamentous anatomy but also an acute awareness of potential soft tissue interposition that can impede anatomical reduction. While rare, the Extensor Digitorum Brevis stands out as a critical, albeit often overlooked, cause of blocked ankle reduction. Meticulous pre-operative planning, systematic surgical exposure, and a high index of suspicion for mechanical blocks are paramount. Intraoperative identification and careful retraction of the EDB or other interposing structures are essential steps to achieve a true anatomical reduction, ensuring stable fixation, and ultimately promoting favorable long-term functional outcomes for patients. Continuous education and recognition of these less common challenges are hallmarks of advanced orthopedic practice.

