Comprehensive Diagnosis of Plantar Plate Rupture in Athletes: A Challenging Football Injury Case Study
Key Takeaway
Plantar plate rupture in athletes is diagnosed through a meticulous clinical exam revealing dorsal hammertoe deformity, interdigital splaying, and MTP joint instability (positive vertical stress test). Crucial imaging includes weight-bearing radiographs showing dorsal subluxation and definitive high-resolution MRI, often after initial misdiagnosis as a forefoot sprain.
Patient Presentation and History
We present the case of a 22-year-old male, a semi-professional wide receiver, who sustained an acute foot injury during a competitive football match. The mechanism of injury involved a rapid deceleration followed by a sharp cutting maneuver, during which his foot was forcibly planted and then hyperdorsiflexed at the forefoot, with the second metatarsophalangeal joint bearing significant axial load. He reported an immediate, sharp, tearing sensation beneath the second metatarsophalangeal joint, accompanied by acute pain and difficulty pushing off or weight-bearing through the forefoot.
Initially, he presented to an external emergency department approximately two hours post-injury. Physical examination at that time reportedly identified diffuse forefoot swelling, tenderness over the dorsal aspect of the second metatarsophalangeal joint, and pain exacerbated by passive dorsiflexion of the second toe. Initial radiographic evaluation utilizing non-weight-bearing views was interpreted as unremarkable for fracture or dislocation. He was discharged with a diagnosis of a forefoot sprain, prescribed analgesia, and advised rest, ice, compression, and elevation.
Despite conservative measures, his symptoms persisted and worsened over the subsequent two weeks. He developed localized pain specifically on the plantar aspect of the second metatarsophalangeal joint, along with persistent swelling, and noted a feeling of instability or giving way in the toe, particularly during ambulation or attempts at sports-related movements. He described difficulty wearing athletic footwear due to forefoot splaying and increasing discomfort. There was no history of prior foot injuries, inflammatory arthropathies, or systemic comorbidities. He denied any neurological deficits or vascular compromise in the affected limb.
Biomechanical Context of the Injury Mechanism
To fully appreciate the pathology in this athlete, one must consider the unique biomechanical demands placed upon the lesser metatarsophalangeal joints during elite athletic maneuvers. The second metatarsal is typically the longest in the human foot, and its base is rigidly constrained within the mortise formed by the medial, intermediate, and lateral cuneiforms. This rigid proximal articulation limits sagittal plane mobility of the second ray compared to the first and third rays.
During the terminal stance phase of gait, and exponentially magnified during a dynamic athletic push-off or cutting maneuver, the load is disproportionately concentrated on the second metatarsophalangeal joint. The plantar plate, a robust, rectangular fibrocartilaginous structure composed primarily of type I collagen, serves as the primary static stabilizer against dorsal translation of the proximal phalanx. When the athlete planted his foot and decelerated, the sudden forced dorsiflexion generated massive axial and shear forces that exceeded the ultimate tensile strength of the plantar plate. In acute traumatic settings, this typically results in an avulsion of the plate from its distal insertion at the base of the proximal phalanx, often accompanied by attenuation or rupture of the collateral ligaments.
Clinical Examination Findings
Upon presentation to our trauma service two weeks post-injury, a meticulous clinical examination was performed to accurately delineate the extent of the capsuloligamentous disruption.
Inspection of the Forefoot
Inspection revealed notable diffuse edema across the dorsal and plantar aspects of the forefoot, most pronounced around the second metatarsophalangeal joint. Subtle but discernible ecchymosis was present on the plantar aspect of the second toe and distal forefoot, indicative of deep tissue hemorrhage tracking along fascial planes. A critical observation was a mild but definite dorsal hammertoe deformity of the second digit, indicative of proximal phalanx dorsal subluxation relative to the metatarsal head. This deformity arises due to the loss of the plantar tethering effect of the intact plantar plate, allowing the extensor digitorum longus and brevis to exert an unopposed dorsal pull. Furthermore, there was an apparent widening of the interdigital space between the second and third toes, suggestive of splaying and potential disruption of the deep transverse metatarsal ligament.
Palpation and Provocative Testing
Palpation elicited exquisite, focal tenderness directly over the plantar aspect of the second metatarsophalangeal joint capsule. Significant pain was provoked with direct pressure on the plantar plate insertion point at the base of the proximal phalanx. Tenderness was also noted along the medial and lateral collateral ligaments of the second metatarsophalangeal joint, though less intense than the plantar tenderness. The metatarsal head was palpable, and no crepitus was elicited. Neurovascular status distally was intact, with palpable dorsalis pedis and posterior tibial pulses, and normal sensation to light touch in all interdigital webs.
Range of Motion and Joint Stability Assessment
Active and passive range of motion of the second metatarsophalangeal joint was significantly painful and restricted, particularly with dorsiflexion. Pain was exacerbated at the end range of passive dorsiflexion. Crucially, a positive vertical stress test, effectively a Lachman test for the metatarsophalangeal joint, was elicited. With the metatarsal head stabilized, manual dorsiflexion of the proximal phalanx produced excessive dorsal translation and a palpable clunk, confirming metatarsophalangeal joint instability. Subluxation was evident even under light stress.
Similarly, a positive drawer test demonstrating anteroposterior instability was also noted. Medial and lateral collateral ligament stress testing utilizing varus and valgus stress demonstrated moderate laxity, suggesting concomitant capsular and collateral ligament attenuation, a common sequela in high-energy hyperextension injuries of the forefoot. Mulder sign was negative, reducing the likelihood of an interdigital neuroma contributing to the clinical picture.
Imaging and Diagnostics
Accurate diagnosis of plantar plate pathology requires a highly specific imaging protocol, as standard non-weight-bearing radiographs often fail to capture the dynamic instability inherent in this injury.
Weight Bearing Radiographic Evaluation
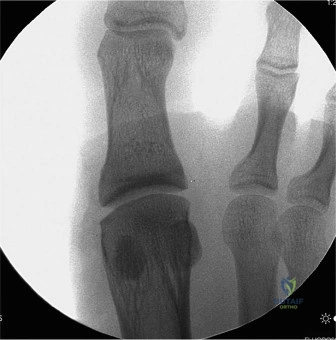
Standard weight-bearing anteroposterior, lateral, and oblique radiographs of the foot were obtained. The anteroposterior view demonstrated subtle widening of the second metatarsophalangeal joint space and early medial deviation of the second digit. The intermetatarsal angle between the first and second rays was within normal limits, but the distance between the second and third metatarsal heads appeared slightly increased.
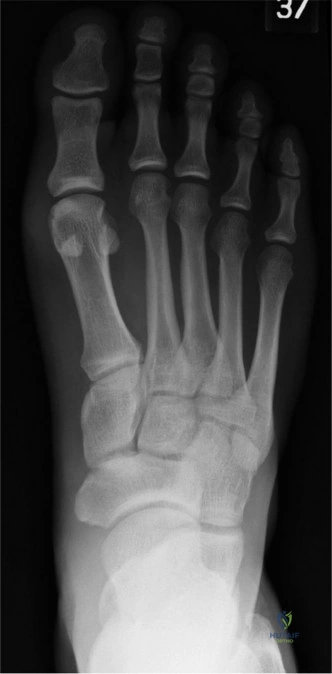
On the lateral weight-bearing projection, the dorsal subluxation of the second proximal phalanx relative to the metatarsal head was clearly visualized, confirming the clinical observation of the incipient hammertoe deformity. A careful review for a Fleck sign, representing a small cortical avulsion fracture from the base of the proximal phalanx, was negative. The lack of overt fracture highlights the purely soft-tissue nature of the failure in this specific athlete.
Advanced Imaging with Magnetic Resonance Imaging
Given the high suspicion for a complete plantar plate rupture and the need for precise preoperative surgical planning, a high-resolution, small field-of-view Magnetic Resonance Imaging scan of the forefoot was ordered. The protocol included T1-weighted, T2-weighted, and Short Tau Inversion Recovery sequences in the sagittal, coronal, and axial planes.

The MRI findings were definitive. Sagittal Short Tau Inversion Recovery images revealed a full-thickness discontinuity of the plantar plate at its distal insertion onto the base of the second proximal phalanx, with a retraction gap of approximately 4 millimeters. Extensive pericapsular edema and fluid signal within the second metatarsophalangeal joint space were noted. Coronal images demonstrated attenuation of the lateral collateral ligament complex, explaining the early medial deviation observed clinically and radiographically. The articular cartilage of the metatarsal head and proximal phalanx base appeared intact, with no evidence of osteochondral lesions or avascular necrosis, which is critical for determining the viability of joint-preserving reconstructive surgery.
The Role of Diagnostic Ultrasound
While MRI remains the gold standard for comprehensive evaluation, high-frequency diagnostic ultrasound is increasingly utilized by orthopedic surgeons as a dynamic, point-of-care adjunct. In skilled hands, ultrasound can visualize the fibrillar pattern of the plantar plate and assess for discontinuity during dynamic dorsiflexion stress. In this case, ultrasound confirmed the hypoechoic defect at the distal insertion and demonstrated dynamic dorsal subluxation of the phalanx upon application of a vertical stress maneuver, perfectly correlating with the clinical Lachman test.
Differential Diagnosis
The presentation of acute or subacute forefoot pain localized to the lesser metatarsophalangeal joints necessitates a rigorous differential diagnosis. Misdiagnosis is common, leading to delayed appropriate surgical intervention and poorer functional outcomes in high-demand athletes.
| Pathologic Condition | Key Clinical Findings | Imaging Characteristics | Primary Differentiating Factor |
|---|---|---|---|
| Plantar Plate Rupture | Positive vertical stress test, dorsal hammertoe deformity, localized plantar MTP joint tenderness. | Dorsal subluxation on weight-bearing lateral X-ray. MRI shows plate discontinuity at phalangeal base. | Gross sagittal plane instability (Lachman test) and specific mechanism of hyperextension injury. |
| Freiberg Infraction | Insidious onset of pain, palpable dorsal osteophyte, crepitus during MTP joint range of motion. | Sclerosis, flattening, or fragmentation of the metatarsal head on standard radiographs. | Intra-articular pathology with bony architectural changes rather than purely soft tissue instability. |
| Morton Neuroma | Burning, neuropathic pain radiating into the toes. Positive Mulder click. Sensation of walking on a pebble. | Typically normal radiographs. MRI/Ultrasound shows a hypoechoic intermetatarsal mass. | Pain is primarily interdigital and neuropathic, lacking MTP joint instability or dorsal subluxation. |
| Metatarsal Stress Fracture | Point tenderness directly over the metatarsal shaft, pain exacerbated by weight-bearing and impact loading. | Periosteal reaction or visible fracture line on radiographs (often delayed). Bone marrow edema on MRI. | Tenderness is diaphyseal or metaphyseal, not localized to the plantar MTP joint capsule. |
| MTP Joint Synovitis | Diffuse joint swelling, pain with passive motion, often associated with systemic inflammatory arthropathies. | Joint effusion on MRI or ultrasound. No structural ligamentous disruption. | Lack of mechanical instability. Often bilateral or involving multiple joints. |
Expanding on the Differential Diagnosis
The distinction between a plantar plate rupture and Freiberg Infraction is critical. Freiberg Infraction involves avascular necrosis of the metatarsal head, most commonly the second. While it presents with pain at the second metatarsophalangeal joint, the pain is typically dorsal, and examination often reveals crepitus and restricted motion without the gross sagittal instability seen in plantar plate tears. Radiographs are usually diagnostic, showing flattening and sclerosis of the metatarsal head.
Morton Neuroma is frequently misdiagnosed in patients with early plantar plate pathology. Both conditions cause forefoot pain, but a neuroma involves the interdigital nerve, typically between the third and fourth metatarsals. The pain is neuropathic, and compression of the forefoot combined with direct plantar pressure often produces a palpable and painful Mulder click. Crucially, a neuroma does not cause structural deformity or joint instability.
Metatarsal stress fractures present with pain during weight-bearing activities, similar to plantar plate injuries. However, the exact location of point tenderness differentiates the two. Stress fractures elicit pain over the dorsal aspect of the metatarsal shaft or neck, whereas plantar plate injuries present with profound tenderness directly over the plantar aspect of the metatarsophalangeal joint articulation.
Surgical Decision Making and Classification
The management of plantar plate ruptures is dictated by the chronicity of the injury, the degree of anatomical disruption, the presence of fixed deformity, and the functional demands of the patient.
Anatomical Classification Systems
Plantar plate tears are frequently categorized using anatomical grading systems based on MRI or intraoperative findings. The most relevant classification divides tears based on location and severity. Type I tears involve attenuation or partial tearing without frank instability. Type II tears represent complete transverse ruptures, usually at the distal insertion, resulting in mild to moderate instability. Type III tears are complete ruptures with significant retraction and associated collateral ligament failure, leading to gross multiplanar instability and crossover toe deformity. Type IV tears involve chronic, fixed deformities with severe joint contractures.
Our patient presented with a Type III injury: an acute-on-subacute complete distal avulsion with significant sagittal plane instability and early coronal plane deviation, highly indicative of collateral ligament involvement.

Rationale for Operative Intervention
Conservative management, consisting of taping, rigid custom orthotics with a metatarsal pad, and activity modification, may be appropriate for low-demand patients with Type I or early Type II injuries. However, in a 22-year-old semi-professional athlete with a Type III complete rupture and gross clinical instability, non-operative management is universally associated with poor outcomes.
Failure to restore the anatomical tether of the plantar plate in this demographic leads to progressive dorsal subluxation, fixed hammertoe deformity, transfer metatarsalgia, and an inability to perform high-impact athletic maneuvers. The decision to proceed with operative intervention was based on the necessity to restore the static restraint of the second metatarsophalangeal joint, thereby facilitating a return to elite-level cutting and sprinting mechanics.
Surgical Technique and Intervention
The surgical reconstruction of the plantar plate can be approached via a dorsal or plantar incision. While the plantar approach offers direct visualization of the pathology, it carries a higher risk of painful plantar scarring and delayed wound healing, which can be devastating for an athlete. Therefore, a dorsal approach utilizing a Weil osteotomy for joint decompression and access was selected.
Patient Positioning and Initial Approach
The patient was positioned supine on the operating table with a bump under the ipsilateral hip to maintain the foot in a neutral position. A regional popliteal block was administered for postoperative analgesia, supplemented by general anesthesia. A pneumatic thigh tourniquet was applied and inflated to 250 mmHg after exsanguination.
A 4-centimeter longitudinal dorsal incision was made centered over the second metatarsophalangeal joint. Careful dissection was carried down through the subcutaneous tissues, taking care to identify and retract the dorsal cutaneous nerve branches. The extensor apparatus was exposed. A Z-lengthening of the extensor digitorum longus tendon was performed to address the extensor contracture contributing to the hammertoe deformity. A transverse tenotomy of the extensor digitorum brevis was also executed.
Joint Exposure and the Weil Osteotomy
A dorsal longitudinal capsulotomy was performed, exposing the metatarsal head and the base of the proximal phalanx. Severe synovitis was encountered and systematically debrided. A McGlamry elevator was utilized to release the plantar capsular adhesions, confirming the complete detachment of the plantar plate from the proximal phalanx.
To gain adequate exposure of the retracted plantar plate and to address the relative length of the second metatarsal, an intra-articular Weil osteotomy was performed. Using a microsagittal saw, an osteotomy was initiated at the dorsal aspect of the articular cartilage of the metatarsal head, angled strictly parallel to the plantar aspect of the foot. This parallel orientation is biomechanically critical; if the cut is angled plantarly, it will result in plantar displacement of the metatarsal head upon shortening, exacerbating metatarsalgia.
The capital fragment was translated proximally by 3 millimeters to decompress the joint and temporarily secured with a smooth 1.1-millimeter Kirschner wire. This proximal translation dramatically improved visualization of the plantar joint space and the retracted plantar plate.
Plantar Plate Mobilization and Repair
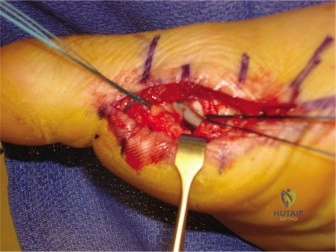
With the joint decompressed, the distal edge of the ruptured plantar plate was identified. It was mobilized from underlying adhesions using a combination of blunt and sharp dissection. A specialized plantar plate repair system was utilized. A pigtail suture passer was introduced through the dorsal exposure, navigating plantarly to capture the medial and lateral aspects of the plantar plate. Two high-strength, non-absorbable number 0 sutures were passed through the substance of the plate in a horizontal mattress configuration.
Attention was then directed to the base of the proximal phalanx. The articular cartilage at the plantar base was denuded to expose bleeding subchondral bone, creating an optimal biological environment for fibrocartilaginous healing. Two parallel drill holes were created from dorsal to plantar through the base of the proximal phalanx, exiting at the anatomic insertion footprint of the plantar plate.
The free ends of the high-strength sutures were retrieved through these osseous tunnels using a suture passing loop.
Fixation Construct and Closure
Before tying the sutures, the Weil osteotomy was definitively fixated. The temporary Kirschner wire was removed, and the osteotomy was secured using two 2.0-millimeter titanium snap-off twist-off screws. The dorsal prominence of the metatarsal shaft was meticulously planed flush with the capital fragment to prevent dorsal impingement.
With the osteotomy secured, the proximal phalanx was reduced onto the metatarsal head. The metatarsophalangeal joint was held in approximately 10 to 15 degrees of plantarflexion to appropriately tension the repair. The high-strength sutures were then tied securely over the dorsal bony bridge of the proximal phalanx.
Intraoperative assessment demonstrated excellent restoration of the plantar tether. A vertical stress test was repeated, confirming complete resolution of the sagittal plane instability. The toe rested in neutral alignment without any tendency for dorsal or medial deviation.
To protect the repair during the initial healing phase, a 1.6-millimeter smooth Kirschner wire was driven antegrade from the tip of the toe, across the distal and proximal interphalangeal joints, and across the repaired metatarsophalangeal joint into the metatarsal shaft.
The extensor digitorum longus Z-plasty was repaired with the toe in neutral alignment using 3-0 absorbable suture. The dorsal capsule was closed, followed by routine closure of the subcutaneous tissue and skin. A sterile, bulky compressive dressing was applied.
Post Operative Protocol and Rehabilitation
The postoperative rehabilitation protocol for a plantar plate repair in a high-level athlete must balance the biological requirements of tissue healing with the necessity of preventing severe joint stiffness and muscle atrophy.
Phase 1 Immediate Postoperative Period Weeks 0 to 2
The patient was placed in a rigid postoperative shoe and instructed to remain strictly non-weight-bearing on the operative extremity. Elevation and strict adherence to cryotherapy were emphasized to mitigate edema. Deep vein thrombosis prophylaxis was maintained according to institutional protocols. At the two-week mark, sutures were removed, and the surgical site was inspected. Radiographs were obtained to confirm the maintenance of joint reduction and hardware positioning.
Phase 2 Protective Weight Bearing Weeks 2 to 6
The patient was transitioned to a controlled ankle motion walker boot. Weight-bearing was permitted strictly on the heel, avoiding any loading of the forefoot. The transarticular Kirschner wire remained in place, maintaining the metatarsophalangeal joint in neutral alignment and protecting the repair from shear forces. During this phase, active range of motion of the ankle and subtalar joints was initiated, alongside proximal lower extremity strengthening exercises to prevent deconditioning.
Phase 3 Pin Removal and Early Mobilization Weeks 6 to 8
At six weeks postoperatively, the transarticular Kirschner wire was removed in the clinic. Radiographs were obtained to confirm osteotomy healing and joint alignment. The patient was allowed to transition to a stiff-soled athletic shoe with a custom carbon fiber insert to limit metatarsophalangeal joint dorsiflexion.
Aggressive physical therapy was initiated. Passive and active-assisted range of motion of the second metatarsophalangeal joint was commenced, emphasizing plantarflexion initially to stretch the dorsal capsule while protecting the plantar repair. Joint mobilization techniques were employed to address capsular adhesions. Intrinsic foot muscle strengthening, specifically short foot exercises, was introduced to restore dynamic stability to the longitudinal and transverse arches.
Phase 4 Progressive Loading and Proprioception Weeks 8 to 12
As range of motion improved and pain subsided, the patient progressed to full weight-bearing in standard athletic footwear. The focus of rehabilitation shifted toward eccentric strengthening of the extrinsic flexors and extensors, proprioceptive training on unstable surfaces, and closed kinetic chain exercises. Light jogging on an anti-gravity treadmill was initiated at week 10, gradually increasing the percentage of body weight as tolerated.
Phase 5 Return to Sport Weeks 12 to 16
The final phase of rehabilitation focused on sport-specific functional restoration. Plyometric training, agility ladder drills, and multi-directional cutting maneuvers were systematically introduced. The patient underwent rigorous biomechanical assessment to ensure symmetrical force distribution during push-off and deceleration. Return to competitive football was permitted at 16 weeks postoperatively, contingent upon achieving full, pain-free athletic function, symmetrical strength, and psychological readiness. He was advised to utilize a turf toe plate or a rigid orthotic in his cleats for the remainder of the season to provide supplemental support to the forefoot.
Clinical Pearls and Pitfalls
The diagnosis and surgical management of plantar plate ruptures demand a high level of clinical acumen and technical precision. The following pearls and pitfalls are critical for orthopedic surgeons managing these complex injuries.
Diagnostic Pearls
- Maintain a High Index of Suspicion: Plantar plate injuries are frequently misdiagnosed as generic forefoot sprains or neuromas. Any patient presenting with localized plantar MTP joint pain and a positive Lachman test requires advanced imaging.
- The Importance of Weight-Bearing Radiographs: Non-weight-bearing films often mask dynamic instability. Weight-bearing lateral views are essential to visualize subtle dorsal subluxation of the proximal phalanx.
- Utilize the Vertical Stress Test: The Lachman test of the MTP joint is the most sensitive clinical maneuver for diagnosing sagittal plane instability indicative of a plantar plate rupture.
Surgical Pitfalls
- Inadequate Weil Osteotomy Trajectory: The most common technical error during a dorsal approach is angling the Weil osteotomy plantarly. This results in plantar depression of the metatarsal head upon shortening, leading to severe postoperative transfer metatarsalgia. The cut must be strictly parallel to the plantar weight-bearing surface.
- Failure to Address Extensor Contractures: Repairing the plantar plate without releasing the contracted extensor apparatus (via EDL lengthening or EDB tenotomy) places excessive tension on the repair, increasing the risk of failure and recurrent deformity.
- Over-tensioning the Repair: While restoring the plantar tether is critical, over-tensioning the sutures with the toe in excessive plantarflexion can result in a stiff, painful joint and a floating toe deformity. The joint should be tensioned in approximately 10 to 15 degrees of plantarflexion.
- Neglecting Collateral Ligament Pathology: Plantar plate ruptures, especially Type III injuries, are often accompanied by collateral ligament attenuation. Failure to address significant coronal plane laxity during the reconstruction will result in persistent crossover toe deformity.
The successful management of complex forefoot trauma in elite athletes requires a comprehensive understanding of biomechanics, meticulous surgical technique, and a rigidly structured, progressive rehabilitation protocol. By adhering to these principles, orthopedic surgeons can optimize functional outcomes and facilitate a successful return to high-demand athletic competition.
