Diagnosing Plantar Plate Rupture: A Challenging Football Injury Case
Patient Presentation & History
We present the case of a 22-year-old male, a semi-professional wide receiver, who sustained an acute foot injury during a competitive football match. The mechanism of injury involved a rapid deceleration followed by a sharp cutting maneuver, during which his foot was forcibly planted and then hyperdorsiflexed at the forefoot, with the second metatarsophalangeal (MTP) joint bearing significant axial load. He reported an immediate, sharp, tearing sensation beneath the second MTP joint, accompanied by acute pain and difficulty pushing off or weight-bearing through the forefoot.
Initially, he presented to an external emergency department approximately two hours post-injury. Physical examination at that time reportedly identified diffuse forefoot swelling, tenderness over the dorsal aspect of the second MTP joint, and pain exacerbated by passive dorsiflexion of the second toe. Initial radiographic evaluation (non-weight-bearing) was interpreted as unremarkable for fracture or dislocation, and he was discharged with a diagnosis of a "forefoot sprain," prescribed analgesia, and advised rest, ice, compression, and elevation (RICE).
Despite conservative measures, his symptoms persisted and worsened over the subsequent two weeks. He developed localized pain specifically on the plantar aspect of the second MTP joint, along with persistent swelling, and noted a feeling of instability or "giving way" in the toe, particularly during ambulation or attempts at sports-related movements. He described difficulty wearing athletic footwear due to forefoot splaying and increasing discomfort. There was no history of prior foot injuries, inflammatory arthropathies, or systemic comorbidities. He denied any neurological deficits or vascular compromise in the affected limb.
Clinical Examination
Upon presentation to our trauma service two weeks post-injury, a meticulous clinical examination was performed.
Inspection
Inspection revealed notable diffuse edema across the dorsal and plantar aspects of the forefoot, most pronounced around the second MTP joint. Subtle but discernible ecchymosis was present on the plantar aspect of the second toe and distal forefoot. A critical observation was a mild but definite dorsal hammertoe deformity of the second digit, indicative of proximal phalanx dorsal subluxation relative to the metatarsal head. Furthermore, there was an apparent widening of the interdigital space between the second and third toes, suggestive of splaying.
Palpation
Palpation elicited exquisite, focal tenderness directly over the plantar aspect of the second MTP joint capsule. Significant pain was provoked with direct pressure on the plantar plate insertion point at the base of the proximal phalanx. Tenderness was also noted along the medial and lateral collateral ligaments of the second MTP joint, though less intense than the plantar tenderness. The metatarsal head was palpable, and no crepitus was elicited. Neurovascular status distally was intact, with palpable dorsalis pedis and posterior tibial pulses, and normal sensation to light touch in all interdigital webs.
Range of Motion (ROM)
Active and passive range of motion of the second MTP joint was significantly painful and restricted, particularly with dorsiflexion. Pain was exacerbated at the end range of passive dorsiflexion. Crucially, a positive "vertical stress test" or Lachman-like test for the MTP joint was elicited: with the metatarsal head stabilized, manual dorsiflexion of the proximal phalanx produced excessive dorsal translation and a palpable clunk, confirming MTP joint instability. Subluxation was evident even under light stress. Similarly, a positive drawer test (anteroposterior instability) was also noted. Medial and lateral collateral ligament stress testing (varus and valgus stress) demonstrated moderate laxity, suggesting concomitant capsular and possibly collateral ligament involvement, but the primary instability was in the sagittal plane.
Neurological/Vascular Assessment
Distal neurovascular assessment remained unremarkable. Capillary refill was brisk in all toes. Sensation to light touch and sharp/dull discrimination was intact in the distribution of the superficial and deep peroneal nerves.
Imaging & Diagnostics
Given the persistent symptoms, the positive findings on physical examination, and the high index of suspicion for a plantar plate injury despite initial "unremarkable" radiographs, a comprehensive imaging workup was initiated.
Radiographs
Repeat weight-bearing radiographs of the foot (AP, oblique, and lateral views) were performed.
* The
AP view
now demonstrated subtle widening of the second MTP joint space and a slight lateral deviation of the second toe (valgus angulation), often referred to as a "positive splay sign."
* The
lateral weight-bearing view
proved critical, revealing definite dorsal subluxation of the proximal phalanx relative to the second metatarsal head. The articular surface of the proximal phalanx was visibly displaced dorsally, losing normal congruity with the metatarsal head.
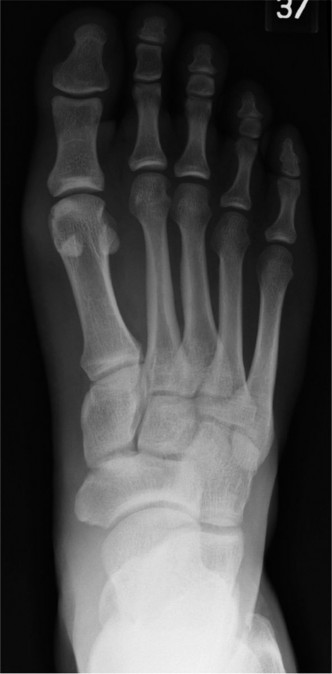
Figure 1: Lateral weight-bearing radiograph demonstrating dorsal subluxation of the proximal phalanx relative to the second metatarsal head, a key indicator of plantar plate incompetence.
No acute fractures, avulsion fractures, or significant osteochondral defects were identified on the plain films. However, the weight-bearing views were instrumental in revealing the dynamic instability that was missed on the initial non-weight-bearing series.
Magnetic Resonance Imaging (MRI)
Due to the persistent clinical suspicion and radiographic evidence of instability, a high-resolution MRI of the forefoot was obtained. This was the definitive diagnostic tool.
*
Sagittal views
clearly demonstrated a
complete rupture of the plantar plate at its distal insertion into the base of the second proximal phalanx
. There was significant retraction of the plantar plate, and a gap was visible between the detached fragment and its normal insertion site.
* Extensive periarticular edema and synovial thickening around the second MTP joint were noted.
*
Axial and coronal views
confirmed the MTP joint effusion and also showed evidence of
concomitant sprain of both the medial and lateral collateral ligaments
of the second MTP joint, contributing to the observed instability.

Figure 2: Sagittal T2-weighted MRI illustrating complete rupture of the second plantar plate (arrow), with discontinuity and retraction from its phalangeal insertion. Note the associated joint effusion and periarticular edema.
* No osteochondral lesions of the metatarsal head or phalangeal base were identified, and the metatarsal stress fracture was excluded.
* The MRI findings correlated perfectly with the clinical presentation of chronic MTP joint instability and dorsal subluxation.
Computed Tomography (CT)
While not strictly necessary for the diagnosis of a plantar plate rupture, a limited weight-bearing CT was considered to evaluate the extent of any subtle bony erosions or osteophytes that might be contributing to chronic irritation, or to assess for more complex anatomical variants if the initial MRI had been equivocal. In this specific case, given the clear MRI findings, a CT was not pursued, as the primary pathology was soft tissue. However, for complex cases or failed prior surgery, it can provide valuable information regarding bony alignment and morphology.
Differential Diagnosis
The presentation of forefoot pain, swelling, and instability, especially in an athletic population, warrants a broad differential diagnosis. Distinguishing plantar plate rupture from other pathologies is critical for appropriate management.
| Feature | Plantar Plate Rupture (Our Case) | MTP Joint Capsulitis/Synovitis | Metatarsal Stress Fracture (e.g., 2nd Metatarsal) | Collateral Ligament Sprain of MTP Joint |
|---|---|---|---|---|
| Mechanism | Acute, forced hyperextension/axial load (e.g., "Turf Toe" variant) | Overuse, repetitive microtrauma, abnormal biomechanics | Repetitive high-impact activity, sudden increase in training intensity | Acute valgus/varus stress to MTP joint |
| Onset | Acute, often with distinct "pop" or tearing sensation | Gradual, insidious | Gradual, progressive with activity | Acute, immediate pain with specific direction of force |
| Pain Location | Focal, plantar aspect of MTP joint (often 2nd/3rd) | Diffuse MTP joint pain, dorsal aspect often prominent | Diffuse metatarsal shaft pain, less localized to joint capsule | Medial or lateral aspect of MTP joint, depending on ligament affected |
| Swelling | Significant, periarticular, possibly with plantar ecchymosis | Mild to moderate, usually diffuse around joint | Mild, localized over metatarsal shaft, often delayed | Localized to medial or lateral aspect of joint, variable |
| Deformity/Instability | Classic: Dorsal subluxation/dislocation of toe, splaying; positive vertical stress test | No deformity, no instability (stable joint) | No deformity, stable joint (unless severe, rare displacement) | Localized instability with specific varus/valgus stress; no sagittal plane instability (unless concomitant plantar plate injury) |
| Palpation | Exquisite focal tenderness plantar plate, possible MTP crepitus | Diffuse MTP joint line tenderness, no instability | Tenderness over metatarsal shaft, percussion pain (tuning fork test) | Focal tenderness over affected collateral ligament, pain with stress |
| ROM | Pain with passive dorsiflexion, restricted due to pain/subluxation | Pain at end range of motion, but full ROM possible | Pain with MTP motion (due to adjacent edema), but joint itself stable | Pain with specific varus/valgus stress, less with pure dorsi/plantarflexion |
| Weight-bearing X-ray | Dorsal subluxation, joint space widening, splaying | Normal or mild soft tissue swelling | May show periosteal reaction or cortical thickening; often normal initially | Normal or mild soft tissue swelling |
| MRI | Definitive: Plantar plate rupture/tear, edema, effusion | Synovitis, capsular thickening, no discrete tear | Bone marrow edema, cortical break (if progressed) | Ligamentous edema/tear, no plantar plate pathology |
| Management | Often operative for complete ruptures/instability | Conservative (RICE, orthotics, NSAIDs, injections) | Conservative (activity modification, immobilization, gradual return) | Conservative (RICE, immobilization), rarely operative for isolated complete tears |
Surgical Decision Making & Classification
Based on the clinical presentation of chronic pain, persistent functional limitation, and unequivocal evidence of dorsal subluxation and complete plantar plate rupture on MRI, an operative approach was deemed necessary. Conservative management, including prolonged immobilization and orthotics over the preceding two weeks, had failed to alleviate symptoms or restore stability. The presence of significant sagittal plane instability and the patient's young age and high activity level were strong indicators for surgical intervention to restore anatomical integrity and function.
Classification
The injury was classified using a combination of clinical and imaging-based systems:
*
Clinical Instability Classification:
This was a
Grade III injury
, characterized by gross MTP joint instability, constant dorsal subluxation, and significant functional impairment.
*
Yu and Hatch MRI Classification:
This case corresponded to a
Type IV rupture
, indicating a complete tear of the plantar plate with associated MTP joint subluxation/dislocation. This classification is crucial for guiding surgical planning, as Type III and IV injuries typically necessitate surgical repair.
*
Jahss Classification (adapted for 2nd MTP):
While primarily for the 1st MTP (Turf Toe), the principles can be extrapolated. Our case represented a
Grade III injury
, signifying a complete rupture of the plantar plate and often associated collateral ligament injury, leading to MTP joint instability and subluxation.
The decision for operative intervention was based on the failure of conservative treatment, the high-grade nature of the rupture, and the patient's demand for high-level athletic function. The goals of surgery were to restore the integrity of the plantar plate, achieve stable anatomical reduction of the MTP joint, alleviate pain, and prevent progressive deformity and subsequent arthrosis.
Surgical Technique / Intervention
The patient underwent open repair of the second MTP plantar plate.
Patient Positioning and Preparation
The patient was positioned supine on the operating table. A high thigh tourniquet was applied, and a non-sterile Esmarch bandage was used for exsanguination of the foot. The foot and ankle were prepped and draped in a standard sterile fashion. Prophylactic intravenous antibiotics (Cefazolin 2g) were administered prior to tourniquet inflation.
Surgical Approach
A dorsal longitudinal incision approximately 4-5 cm in length was made centered over the second MTP joint. This approach offers excellent exposure to the joint capsule and allows for identification and protection of the dorsal neurovascular structures. The incision was deepened through the skin and subcutaneous tissue. The extensor digitorum longus tendon to the second toe was identified and retracted medially or laterally to expose the dorsal MTP joint capsule. The extensor digitorum brevis tendon, if encountered, was similarly mobilized. Care was taken to protect the dorsal neurovascular bundle.
Joint Exposure and Pathology Identification
A longitudinal capsulotomy was performed along the dorsal aspect of the second MTP joint. Upon opening the capsule, the dorsal subluxation of the proximal phalanx on the metatarsal head was immediately apparent. The joint was gently distracted and inspected. The ruptured plantar plate was visualized. In this case, it was a
distal avulsion from the base of the proximal phalanx
, with the retracted plantar plate appearing as a thickened, frayed, and scarred structure in the plantar aspect of the joint. Associated tears in the medial and lateral collateral ligaments were also confirmed intraoperatively.
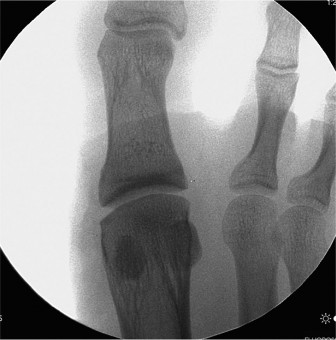
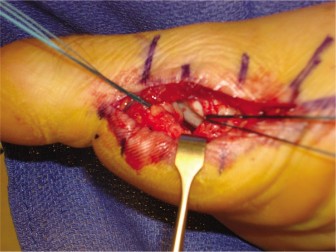
Figure 3: Intraoperative view following dorsal capsulotomy, demonstrating the exposed second MTP joint. The arrow indicates the retracted, torn edge of the plantar plate from its phalangeal insertion, confirming a complete rupture.
Reduction and Plantar Plate Repair
- Metatarsal Shortening Osteotomy (Weil Osteotomy): Given the chronicity of the injury (2 weeks) and the significant dorsal subluxation, a Weil osteotomy of the second metatarsal head was performed. A 2.0 mm dorsal incision was made distal to the joint, and the second metatarsal head was exposed. A dorsally-based wedge osteotomy was performed, removing approximately 4-5 mm of bone from the distal metatarsal, effectively shortening and plantarflexing the metatarsal head. This step is crucial in chronic cases to facilitate reduction of the subluxated phalanx, reduce tension on the plantar plate repair, and prevent recurrence of dorsal subluxation. The osteotomy was provisionally secured with a temporary K-wire.
- Accessing the Plantar Plate: The joint was further distracted, and the plantar plate was carefully mobilized.
- Repair Technique: Two mini bone anchors (e.g., 1.5 mm, bioabsorbable PEEK) were inserted into the plantar-proximal aspect of the second proximal phalanx base, near the anatomical footprint of the plantar plate. Each anchor had two high-strength non-absorbable sutures. The sutures were then passed through the retracted plantar plate in a mattress fashion, effectively reattaching the plate to its anatomical insertion point on the phalanx. The sutures were tied securely, bringing the plantar plate under appropriate tension and reducing the phalanx onto the metatarsal head.
- Capsular and Collateral Ligament Repair: The torn medial and lateral collateral ligaments were repaired using 3-0 non-absorbable sutures. The dorsal joint capsule was also repaired with interrupted 3-0 absorbable sutures to complete the capsular closure and further enhance stability.
- Temporary Transarticular K-wire Fixation: To protect the delicate plantar plate repair and maintain MTP joint reduction and alignment during the initial healing phase, a 0.045-inch (1.1 mm) smooth K-wire was inserted percutaneously from the tip of the second toe, across the second MTP joint, and into the metatarsal shaft. This provided temporary stability in a slightly plantarflexed position.
- Weil Osteotomy Fixation: The Weil osteotomy was definitively secured with a low-profile 2.0 mm cortical screw (e.g., headless compression screw) after removing the provisional K-wire. The K-wire for transarticular fixation was then confirmed to be in optimal position.
Closure
Layered closure was performed: subcutaneous tissue with absorbable sutures and skin with non-absorbable sutures. A sterile dressing was applied, and the foot was placed in a well-padded short-leg non-weight-bearing cast. The tourniquet was deflated, and pedal pulses were checked.
Post-Operative Protocol & Rehabilitation
Post-operative management is critical to protect the repair while facilitating functional recovery.
Phase I: Immobilization and Protection (Weeks 0-6)
- Immobilization: Short-leg non-weight-bearing cast for 2 weeks. The K-wire provides additional stability.
- Elevation: Strict elevation of the limb for the first 3-5 days to minimize swelling.
- Pain Management: Opioid analgesics as needed, transitioned to NSAIDs.
- K-wire Removal: At 2 weeks post-op, the transarticular K-wire is typically removed in the clinic.
- Transition to Boot: After K-wire removal, the patient is transitioned to a short-leg cam walker boot, maintaining non-weight-bearing for an additional 4 weeks (total 6 weeks non-weight-bearing).
- Toe Motion: Gentle, passive plantarflexion and limited dorsiflexion of the MTP joint (within comfort) can be initiated cautiously at 4 weeks, with care taken not to stress the repair. Avoid forced dorsiflexion.
Phase II: Gradual Weight-Bearing and Controlled Motion (Weeks 6-12)
- Weight-Bearing: At 6 weeks post-op, gradual protected weight-bearing is initiated in the cam walker boot. Progress from partial to full weight-bearing over 2-3 weeks.
- Boot Discontinuation: At 8-10 weeks, transition from the cam walker boot to a stiff-soled post-operative shoe or a shoe with a rigid carbon fiber insert.
-
Physical Therapy:
Aggressive physical therapy begins.
- Range of Motion: Focus on restoring pain-free MTP joint range of motion (plantarflexion and dorsiflexion within limits). Manual therapy, joint mobilizations.
- Strengthening: Intrinsic foot muscle strengthening (e.g., towel crunches, marble pickups), extrinsic ankle musculature.
- Gait Training: Re-education of a normal heel-to-toe gait pattern.
- Orthotics: Custom orthotics with a forefoot pad or modified Morton's extension to offload the second MTP joint are often prescribed to protect the repair long-term.
Phase III: Progressive Strengthening and Functional Return (Months 3-6)
- Advanced Strengthening: Progress to resistance band exercises, calf raises, balance and proprioception training.
- Sport-Specific Drills: Begin light jogging, agility drills, and sport-specific movements in a controlled environment, gradually increasing intensity.
- Footwear: Transition to athletic shoes with good support and a rigid sole.
- Return to Play: Gradual return to full sports activity is typically permitted between 4-6 months post-operatively, provided there is no pain, full strength, and adequate stability. Clinical assessment, including repeat vertical stress testing, is crucial before clearance.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- High Index of Suspicion: Always suspect plantar plate rupture in athletes presenting with acute forefoot pain following a hyperdorsiflexion injury, even if initial radiographs are "normal."
- Weight-bearing Radiographs are Critical: Non-weight-bearing films can miss subtle dorsal subluxation. Weight-bearing views are essential to unmask instability.
- MRI is the Gold Standard: For definitive diagnosis of soft tissue injury, especially to confirm plantar plate integrity and assess concomitant pathology (collateral ligaments, synovitis).
- Clinical Examination Nuances: The "vertical stress test" (Lachman-like test) is highly sensitive for MTP joint instability. Palpation of the plantar plate insertion is key. Look for dorsal hammertoe deformity and toe splaying.
- Consider Metatarsal Shortening Osteotomy (Weil): In chronic cases, or where significant dorsal subluxation persists even after plantar plate repair, a Weil osteotomy offloads the repair, facilitates reduction, and prevents recurrence. It's a critical adjunct.
- Protect the Repair: Adequate post-operative immobilization and a structured, progressive rehabilitation program are paramount to prevent re-rupture and ensure successful outcomes. Temporary K-wire fixation offers essential initial protection.
- Address Concomitant Pathology: Always assess and address associated collateral ligament injuries or capsular tears, as these contribute to overall MTP joint instability.
- Custom Orthotics: Long-term use of orthotics with metatarsal pads or a rigid forefoot can help distribute pressure and protect the repaired joint.
Pitfalls
- Misdiagnosis as Simple Sprain: This is the most common pitfall, leading to delayed diagnosis and chronic instability, making subsequent repair more challenging.
- Inadequate Imaging: Relying solely on non-weight-bearing radiographs can lead to missed diagnoses.
- Failure to Appreciate Subtle Instability: A less experienced examiner might miss subtle MTP joint laxity on clinical testing, especially in acute settings with significant pain and swelling.
- Premature Return to Activity: Allowing the patient to return to high-impact activities too early can result in re-rupture of the plantar plate repair or exacerbation of instability.
- Overly Aggressive Rehabilitation: Pushing MTP joint dorsiflexion too early in the post-operative period can jeopardize the repair.
- Ignoring Mechanical Factors: Failure to address underlying biomechanical issues (e.g., long metatarsals, cavus foot deformity) can contribute to recurrence or overload of adjacent lesser MTP joints.
- Stiffness vs. Instability: The rehabilitation process must balance protecting the repair from re-rupture (which requires some immobilization) with preventing excessive MTP joint stiffness. Early controlled motion, as tolerated, is important.
- Neurovascular Injury: During a dorsal approach, meticulous dissection is required to avoid injury to the dorsal neurovascular structures.
- Incomplete Repair: Failure to adequately secure the plantar plate or address concomitant collateral ligament pathology can lead to persistent instability and unsatisfactory outcomes.
This challenging case highlights the importance of a meticulous clinical examination and appropriate imaging, particularly weight-bearing radiographs and MRI, for the accurate diagnosis of plantar plate ruptures in athletic individuals. Timely and comprehensive surgical intervention, followed by a structured rehabilitation protocol, is crucial for restoring function and enabling a successful return to sport.
Clinical & Radiographic Imaging