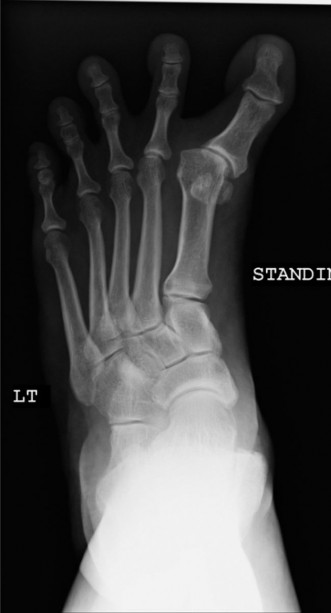
Understanding Hallux Varus: The Lateral Capsule's Lateral Support
Introduction & Epidemiology
Hallux varus, characterized by a pathological medial deviation of the great toe at the first metatarsophalangeal (MTP) joint, represents a distinct and considerably less common forefoot deformity compared to its counterpart, hallux valgus. While it can occur congenitally, post-traumatic, or secondary to inflammatory arthropathies or neurological conditions, the overwhelming majority of cases are iatrogenic, arising as a complication of hallux valgus corrective surgery.
The epidemiology of hallux varus is predominantly driven by surgical intervention for hallux valgus. Historical incidences ranged from 2% to 15% following various hallux valgus correction procedures, particularly those involving aggressive medial capsular plication or overzealous lateral soft tissue release, especially combined with first metatarsal head osteotomy or medial sesamoidectomy. With advancements in surgical techniques and a deeper understanding of MTP joint biomechanics, the incidence has decreased, but it remains a concerning complication. Contemporary series report iatrogenic hallux varus rates typically below 5%, though this can vary significantly based on the specific procedure performed and surgeon experience.
Clinically, patients present with pain, often localised to the medial aspect of the MTP joint, exacerbated by shoe wear. The medially deviated great toe can impinge on the second toe, leading to painful irritation, corns, or callosities between the toes. Difficulties with shoe fitting, cosmetic concerns, and altered gait mechanics leading to transfer metatarsalgia under the lesser metatarsal heads are also common presentations. The deformity can be dynamic, with medial deviation accentuated by toe-off during gait, or fixed, indicating more severe contracture of medial soft tissues and potential adaptive bony changes. Understanding the contributing factors and the intricate balance of forces around the MTP joint is paramount for both prevention and effective treatment.
Surgical Anatomy & Biomechanics
The first MTP joint is a condyloid joint, providing both stability and mobility essential for propulsion during gait. Its stability is maintained by a complex interplay of bony architecture, capsuloligamentous structures, and musculotendinous units.
Bony Architecture:
The proximal phalanx base articulates with the first metatarsal head. The shape of the metatarsal head, particularly the congruence of its articular surface, influences MTP stability. A prominent medial condyle or an overly pronated first metatarsal can predispose to varus.
Capsuloligamentous Structures:
*
Joint Capsule:
Surrounds the joint, blending with collateral ligaments. The medial capsule, in hallux varus, is typically contracted or scarred. The lateral capsule, often subject to release in hallux valgus correction, becomes deficient or scarred in a shortened position, potentially failing to resist medial deviation.
*
Collateral Ligaments:
The medial and lateral collateral ligaments are primary stabilizers. In hallux varus, the medial collateral ligament is contracted, while the lateral collateral ligament may be attenuated or absent (post-iatrogenic release).
*
Plantar Plate:
A fibrocartilaginous structure that reinforces the plantar aspect of the joint capsule, extending distally from the metatarsal head to the base of the proximal phalanx. It integrates the flexor hallucis brevis (FHB) tendons and the sesamoid bones, forming the sesamoid complex.
Musculotendinous Units:
*
Abductor Hallucis (AH) Muscle:
Originates from the medial tubercle of the calcaneus and the plantar aponeurosis, inserting onto the medial aspect of the proximal phalanx base and the medial sesamoid. Its primary action is abduction and plantarflexion of the great toe. In hallux varus, the AH is often contracted and becomes a primary deforming force, actively pulling the toe medially.
*
Adductor Hallucis (AD) Muscle:
Comprises oblique and transverse heads, originating from the metatarsal bases and plantar ligaments, inserting into the lateral aspect of the proximal phalanx base and the lateral sesamoid. Its primary action is adduction of the great toe. In iatrogenic hallux varus, the AD may be deficient due to extensive release during hallux valgus surgery, or it may be overwhelmed by the medial deforming forces.
*
Flexor Hallucis Brevis (FHB) Muscle:
Divides into medial and lateral heads, each incorporating a sesamoid bone, inserting onto the proximal phalanx base. It primarily plantarflexes the MTP joint. The balance between its two heads is crucial. An over-resected lateral sesamoid or an imbalanced FHB can contribute to varus.
*
Extensor Hallucis Longus (EHL) Tendon:
Crosses dorsally over the MTP joint. In hallux varus, the EHL can become medially subluxed (bowstringing), exacerbating the varus deformity and leading to MTP joint hyperextension with interphalangeal (IP) joint flexion (a "claw toe" deformity of the hallux).
Biomechanics of Hallux Varus Development:
The pathomechanics of hallux varus are often multifactorial, particularly in iatrogenic cases:
1.
Overzealous Lateral Release:
Excessive release of the adductor hallucis tendon, lateral collateral ligament, and lateral joint capsule during hallux valgus correction disrupts the primary lateral stabilizers of the MTP joint. This effectively removes the "lateral capsule's lateral support" that resists medial deviation.
2.
Aggressive Medial Capsular Plication:
Over-tightening of the medial capsule and medial collateral ligament in an attempt to correct hallux valgus can pull the toe into a varus position.
3.
Resection of the Lateral Sesamoid:
Unilateral resection of the lateral sesamoid during bunionectomy can unbalance the FHB and alter the mechanical axis of the toe, shifting forces medially.
4.
Overcorrection of the Intermetatarsal (IM) Angle:
Inadvertent medial shift of the metatarsal head (e.g., overly aggressive medial translation in a Chevron or scarf osteotomy) can predispose to varus.
5.
Malunion of Osteotomies:
First metatarsal osteotomies or proximal phalanx osteotomies (Akin osteotomy) can heal in an overcorrected position, leading to varus.
6.
Transfer of EHL:
Rarely, transfer of the EHL for hallux valgus correction (e.g., Jones procedure for claw toe) can result in hallux varus if not balanced correctly.
7.
Abductor Hallucis Contracture/Overactivity:
This muscle, normally an abductor, becomes a powerful varus deforming force when contracted and unopposed by lateral structures. Its medial position relative to the MTP joint axis makes it a primary contributor to dynamic varus.
8.
EHL Bowstringing:
As the toe deviates medially, the EHL tendon can migrate medially, further accentuating the varus pull, particularly during dorsiflexion.
Understanding these biomechanical principles is critical for surgical planning, as correction often involves releasing contracted medial structures, rebalancing musculotendinous forces, and, if necessary, performing osteotomies to correct bony alignment.
Indications & Contraindications
The decision-making process for the management of hallux varus, whether operative or non-operative, hinges upon the patient's symptoms, the flexibility and severity of the deformity, and the underlying etiology.
Indications for Operative Intervention
Surgical correction is primarily indicated for symptomatic hallux varus that has failed conservative management. The severity of symptoms, often relating to pain, footwear difficulties, and functional limitations, dictates the need for surgery.
-
Symptomatic Deformity:
- Persistent pain at the first MTP joint, medial side of the great toe, or between the first and second toes due to impingement.
- Painful callosities or irritation from impingement of the great toe on the second toe.
- Difficulty with shoe wear due to the malposition of the great toe.
- Gait disturbance or functional limitations secondary to the deformity.
- Transfer metatarsalgia, particularly under the second metatarsal head, due to altered weight-bearing mechanics.
- Progressive Deformity: Evidence of increasing varus angle or worsening symptoms over time, despite conservative measures.
- Fixed Deformity: When the deformity is rigid and irreducible, necessitating surgical correction of bony or fibrotic soft tissue components.
- Failure of Non-Operative Management: Comprehensive conservative care, including footwear modifications, orthoses, and activity modification, has been trialed for at least 3-6 months without satisfactory relief.
- Dynamic Deformity with Strong Muscle Imbalance: When the abductor hallucis or EHL exerts a strong, unresisted medial pull, particularly evident during toe-off.
- Cosmetic Concerns: While not a primary indication for all surgeons, significant cosmetic distress can also be a factor, particularly in younger, active patients, provided realistic expectations are set.
Indications for Non-Operative Management
Conservative management is the initial approach for most patients with hallux varus, especially those with mild symptoms, flexible deformities, or contraindications to surgery.
- Asymptomatic or Mildly Symptomatic Deformity: Patients experiencing minimal to no pain or functional impairment.
- Flexible Deformity: When the great toe can be passively corrected to a neutral or near-neutral position, indicating that fixed contractures are not the primary issue.
- Responsive to Conservative Measures: Improvement in symptoms with appropriate non-surgical interventions.
- Patients Unwilling or Unfit for Surgery: Those who decline surgical intervention, or have significant medical comorbidities that elevate surgical risks.
- Neuropathic Hallux Varus: Often challenging to treat surgically, non-operative management to protect the foot may be preferred.
- Severe Peripheral Vascular Disease: Compromised vascular status significantly increases the risk of wound healing complications and infection.
Contraindications for Operative Intervention
Absolute and relative contraindications must be thoroughly evaluated during pre-operative planning.
-
Absolute Contraindications:
- Active infection in the foot or ankle.
- Severe peripheral vascular disease with critical limb ischemia.
- Uncontrolled systemic diseases (e.g., diabetes, immune-compromised states) that significantly increase surgical risk.
- Acute Charcot arthropathy.
-
Relative Contraindications:
- Unrealistic patient expectations regarding surgical outcomes.
- Significant psychological comorbidities affecting compliance or recovery.
- Severe generalized osteoporosis (may complicate hardware fixation).
- History of previous failed attempts at hallux varus correction, which may warrant a more aggressive salvage procedure like arthrodesis.
- Poor skin quality or viability in the operative field.
- Ongoing litigation related to a prior surgery.
Table: Operative vs. Non-Operative Indications for Hallux Varus
| Feature/Category | Operative Indications | Non-Operative Indications |
|---|---|---|
| Symptom Severity | Persistent and disabling pain; significant functional limitations (gait, activity); severe shoe wear difficulties; nerve irritation from impingement. | Asymptomatic or mildly symptomatic deformity; pain managed effectively with conservative measures; minor cosmetic concerns without functional impact. |
| Deformity Flexibility | Fixed, rigid deformity (cannot be passively corrected to neutral); dynamic deformity with significant muscle imbalance (e.g., strong AH pull, EHL bowstringing). | Flexible deformity (can be passively corrected to neutral or near-neutral); no significant fixed contractures. |
| Response to Treatment | Failed adequate trial (typically 3-6 months) of non-operative management. | Symptoms are stable or improving with non-operative interventions (e.g., shoe modifications, orthoses, stretching). |
| Radiographic Findings | Significant bony malalignment requiring osteotomy; evidence of MTP joint subluxation or incongruity secondary to the varus; presence of symptomatic hardware from prior surgery contributing to varus. | Stable radiographic appearance; minimal MTP joint incongruity; absence of significant bony malalignment or hardware issues contributing to symptoms. |
| Patient Factors | Healthy, compliant patient with realistic expectations; desire for functional improvement and pain relief. | Significant comorbidities precluding surgery (e.g., severe vascular disease, uncontrolled diabetes); patient unwilling or unable to comply with post-operative regimen; neuropathic joint. |
| Etiology | Iatrogenic (post-bunionectomy), severe congenital, traumatic, or arthritic cases leading to severe, fixed deformity. | Mild congenital, inflammatory, or early-stage iatrogenic cases where compensation is effective. |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is the cornerstone of successful hallux varus correction, especially given its often iatrogenic and complex nature. It involves a detailed clinical and radiographic assessment, patient education, and meticulous surgical strategy.
Clinical Assessment
- History: Document the onset, duration, progression, and specific symptoms (pain, location, aggravating/alleviating factors, shoe wear difficulties, prior surgeries and complications). Crucially inquire about prior hallux valgus surgery, the type of procedure, and any immediate post-operative concerns.
-
Physical Examination:
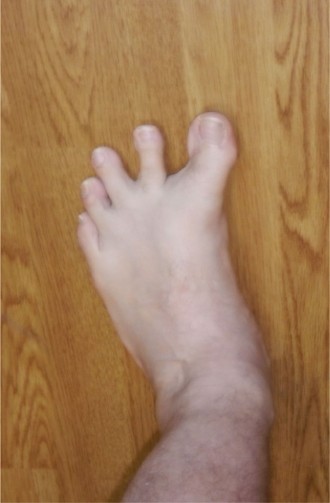
- Inspection: Observe the foot in both weight-bearing and non-weight-bearing positions. Note the degree of varus deviation, any MTP joint hyperextension, IP joint flexion (claw hallux), skin irritation, callosities, and the overall foot posture (e.g., pes planus, forefoot pronation).
- Palpation: Identify areas of tenderness, particularly around the MTP joint, medial capsule, and abductor hallucis origin/insertion. Assess for any palpable hardware.
-
Range of Motion (ROM):
- Passive ROM: Assess the MTP and IP joint ROM. Determine the flexibility of the varus deformity – can it be passively corrected to neutral or overcorrected? This distinguishes flexible from rigid deformities. Assess dorsiflexion and plantarflexion of the MTP joint.
- Active ROM: Observe how the great toe moves during active flexion and extension. Look for dynamic components like EHL bowstringing or prominent abductor hallucis activity.
- Neurovascular Status: Assess light touch sensation over the dorsal medial cutaneous nerve of the hallux (often at risk), two-point discrimination, capillary refill, and pedal pulses.
- Muscle Strength: Assess strength of the intrinsic foot muscles and long flexors/extensors.
- Gait Analysis: Observe the patient's gait, noting any compensations, toe-off mechanics, and the dynamic presentation of the hallux varus.
Radiographic Assessment
Standard weight-bearing radiographs are essential for evaluating bony alignment and joint pathology.
1.
Weight-Bearing Anteroposterior (AP) View:
*
Hallux Valgus Angle (HVA):
Although the name implies valgus, in varus, this angle is negative (medial deviation of the proximal phalanx from the first metatarsal axis).
*
Intermetatarsal (IM) Angle:
Measure the angle between the first and second metatarsals. An overcorrected IM angle (often excessively small or even negative) can indicate a medial shift of the first metatarsal head.
*
Distal Metatarsal Articular Angle (DMAA) / Proximal Phalangeal Articular Angle (PPAA):
Assess the orientation of the articular surfaces. A medial inclination of the metatarsal head articular surface can contribute to varus.
*
Sesamoid Position:
Note the position of the medial and lateral sesamoids relative to the first metatarsal head. In varus, the medial sesamoid may be displaced medially, and the lateral sesamoid may be absent (post-excision) or also displaced medially if the toe is severely pronated.
*
Joint Congruity:
Evaluate for MTP joint subluxation or degenerative changes.
*
Presence of Hardware:
Identify any previous osteotomy fixation and assess its position and integrity.
2.
Weight-Bearing Lateral View:
* Assess the MTP joint height, any MTP joint hyperextension, and the integrity of the plantar plate.
* Evaluate the position of the EHL tendon relative to the joint axis (dorsal subluxation indicates bowstringing).
3.
Oblique View:
Provides additional information on bony anatomy and any osteophyte formation.
4.
Stress Views (Optional):
May be considered to assess dynamic instability or specific soft tissue integrity, though less commonly used for hallux varus.
Pre-Operative Planning
- Deformity Analysis: Categorize the deformity as primarily soft tissue (flexible), bony (rigid malunion, overcorrection), or combined. Identify the primary deforming forces (e.g., contracted AH, EHL bowstringing).
- Procedure Selection: Based on the assessment, determine the appropriate surgical strategy. This may involve soft tissue releases, tendon transfers, osteotomies, or a combination.
- Hardware Planning: Plan for appropriate fixation for osteotomies (K-wires, screws) and suture anchors for tendon transfers/reconstructions.
- Patient Education: Discuss the rationale for the chosen procedure, expected outcomes, potential complications (e.g., recurrence, stiffness, nerve injury), and the rehabilitation protocol. Manage expectations regarding full correction and functional recovery.
Patient Positioning & Anesthesia
- Anesthesia: A regional ankle block (e.g., popliteal block or combined ankle block) is often preferred for excellent post-operative pain control, combined with light sedation or general anesthesia.
- Positioning: The patient is placed supine on the operating table. The operative leg is draped free to allow for full range of motion of the ankle and foot. A thigh tourniquet is applied for a bloodless field, typically inflated to 250-300 mmHg.
- Surgical Prep: The foot and ankle are prepped and draped in a sterile fashion. An iodine or chlorhexidine-based solution is commonly used.
- C-arm Fluoroscopy: While not always mandatory for soft tissue procedures, a C-arm is highly recommended for any bony osteotomy to confirm adequate correction and hardware placement.
Detailed Surgical Approach / Technique
Correction of hallux varus is a nuanced process, often requiring a multi-faceted approach addressing both soft tissue contractures and bony malalignment. The specific technique chosen depends on the etiology, flexibility, and severity of the deformity, as well as the presence of any previous hardware. The overarching goal is to rebalance the forces around the MTP joint and restore anatomical alignment.
General Principles
- Systematic Approach: Address the most significant deforming forces first, typically the contracted medial soft tissues and the abductor hallucis.
- Balance: Aim for a well-balanced MTP joint at the end of the procedure, with no residual varus or excessive valgus tendency.
- Preservation of Joint Mobility: Avoid procedures that unnecessarily stiffen the joint, unless arthrodesis is the planned salvage.
- Neurovascular Protection: Meticulous dissection to protect the dorsal medial cutaneous nerve of the hallux and other neurovascular structures.
Surgical Incisions and Exposure
Multiple incision options exist, depending on the components of the deformity to be addressed.
1.
Dorsomedial Longitudinal Incision:
Most common approach. Starts just proximal to the MTP joint and extends distally over the medial aspect of the joint to the mid-proximal phalanx. This allows access to the medial capsule, abductor hallucis, and the EHL tendon.
2.
Medial Incision:
Parallel to the medial aspect of the first metatarsal. Provides good exposure for medial capsular work and abductor hallucis release/transfer.
3.
Dorsal Longitudinal Incision:
Directly over the EHL tendon, if a primary EHL transfer is planned without extensive medial capsular work.
Careful subcutaneous dissection is performed to expose the deep fascia. The dorsal medial cutaneous nerve of the hallux should be identified and protected, retracting it dorsally or plantarly as needed.
Addressing Soft Tissue Contractures and Imbalances
This constitutes the primary focus in most flexible or reducible hallux varus deformities.
1. Abductor Hallucis (AH) Management
The contracted abductor hallucis is a major deforming force.
*
Release:
For mild, flexible varus, a simple release of the abductor hallucis tendon from its insertion at the base of the proximal phalanx and medial sesamoid may suffice. This can be done percutaneously or openly.
*
Abductor Hallucis Tendon Transfer (AHTR):
This is a powerful technique for more significant or recurrent varus.
* The abductor hallucis tendon is sharply detached from its insertion on the proximal phalanx and medial sesamoid.
* A drill hole is made from medial to lateral through the base of the proximal phalanx, approximately 5-7 mm distal to the articular surface. Alternatively, a suture anchor can be placed into the lateral aspect of the proximal phalanx base.
* The freed abductor hallucis tendon is then passed from medial to lateral through the drill hole (or woven through the suture anchor) and secured on the lateral aspect of the proximal phalanx. The tension should be sufficient to bring the toe into slight overcorrection (slight valgus), which will typically relax to neutral.
* This converts the AH from a varus deforming force to a valgus-producing force, simultaneously releasing the medial contracture and providing lateral dynamic support.
* This technique effectively addresses the "lateral capsule's lateral support" concept by creating a dynamic lateral pull.
2. Extensor Hallucis Longus (EHL) Management
The EHL can contribute to varus through bowstringing or direct medial pull.
*
Z-Lengthening:
If the EHL is tight and contributing to MTP joint hyperextension, a Z-plasty lengthening can be performed to allow for more plantarflexion and reduce the dorsal pull.
*
EHL Tenodesis / Split Tendon Transfer:
For persistent bowstringing or significant dynamic varus, transferring part or all of the EHL can be very effective.
*
Split EHL Transfer (Modified Jones Procedure):
The EHL tendon is longitudinally split in half, usually just proximal to the MTP joint. The lateral half is then detached distally and rerouted plantar-laterally, either through a drill hole in the lateral base of the proximal phalanx, or secured to the lateral sesamoid or lateral plantar plate. The medial half is reattached to the proximal phalanx or its original insertion. This provides lateral dynamic balance while retaining some EHL function.
*
Full EHL Transfer:
The entire EHL tendon is detached distally. A drill hole is made in the lateral aspect of the proximal phalanx base (similar to AHTR). The EHL tendon is then passed through the hole and sutured back onto itself, or secured with a suture anchor. The IP joint is then fused to compensate for the loss of EHL function, preventing a "floppy toe" deformity. This is a more powerful lateralizing force and reserved for severe, resistant cases.
*

(This image could represent the EHL split transfer technique with the lateral half being routed).
3. Capsular Management
- Medial Capsulotomy: If a significant medial capsular contracture persists after AH release, a longitudinal or T-shaped capsulotomy can be performed. Care must be taken to not over-release, as this can lead to instability.
- Lateral Capsular Plication/Reefing: In cases where the lateral capsule is severely attenuated or absent (often post-iatrogenic), and the toe still has a tendency for varus despite adequate medial release and tendon transfers, a lateral capsular plication may be considered to augment lateral stability. This is less commonly the primary intervention for established hallux varus, but can be used as an adjunctive balancing maneuver. It is essentially restoring the lost "lateral capsule's lateral support" in a controlled manner.
Addressing Bony Malalignment (Osteotomies)
Bony procedures are indicated when there is a structural deformity contributing to the varus, such as an overcorrected IM angle or an articular malalignment.
1. Proximal Phalangeal Osteotomies (Reverse Akin)
- Reverse Akin Osteotomy: A medially-based closing wedge osteotomy performed at the base of the proximal phalanx. A wedge of bone is removed from the medial side, and the remaining bone is closed and fixed with a K-wire or screw. This procedure is used to correct residual varus at the MTP joint level, similar to how an Akin osteotomy corrects valgus. It should be performed after soft tissue balancing to fine-tune the alignment.
2. Distal Metatarsal Osteotomies (Reverse Chevron / Reverse Weil)
- These are rarely indicated for primary hallux varus but may be considered if there is an overcorrected IM angle or a highly medially angulated distal metatarsal articular surface (DMAA).
- Reverse Chevron (or Reverse Weil) Osteotomy: A medially-based osteotomy that shifts the metatarsal head laterally. This can be used to increase the IM angle and reduce the varus force originating from the metatarsal head. Fixation is typically with a single screw.
3. First Metatarsal Osteotomies
- Opening Wedge Osteotomy: If the first metatarsal itself is in varus, or if an overzealous IM angle correction has created a negative IM angle, an opening wedge osteotomy of the first metatarsal can be considered to laterally displace the head or increase the IM angle. This is a more complex procedure often combined with MTP joint soft tissue work.
Salvage Procedures
For severe, rigid, painful, and often recurrent hallux varus with significant MTP joint arthrosis, arthrodesis (fusion) of the first MTP joint is a reliable salvage option.
*
MTP Arthrodesis:
The joint surfaces are denuded of cartilage, and the joint is fused in a functional position (typically 10-15 degrees dorsiflexion, 0-5 degrees valgus, and slight pronation). This provides a stable, pain-free joint, albeit at the expense of motion. Fixation is usually achieved with screws or a plate.
*
(This image could depict an MTP joint fusion, showing internal fixation).
Intraoperative Assessment
After each step (soft tissue release, tendon transfer, osteotomy), the MTP joint should be assessed for stability and alignment. The toe should sit in a neutral or slightly overcorrected (valgus) position without undue tension. Dynamic assessment by simulating gait (flexing the ankle and knee, applying pressure to the forefoot) can help identify residual imbalances.
Wound Closure
After achieving satisfactory correction, the tourniquet is deflated. Hemostasis is achieved. The wound is closed in layers, paying attention to capsular repair (if indicated), subcutaneous tissue, and skin. A sterile dressing is applied, and a temporary splint or cast is often used to maintain the corrected position.
Complications & Management
Despite meticulous surgical technique, complications can arise following hallux varus correction. Understanding their incidence and having a robust management strategy are crucial.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence | Management / Salvage Strategy |
|---|---|---|
| Recurrence of Varus | 5-15% (variable) | Conservative: Splinting, orthotics. Surgical: Re-evaluation of deforming forces. Further soft tissue release (AH, EHL), stronger tendon transfer (e.g., full EHL transfer with IP fusion), additional osteotomy (e.g., reverse Akin), or ultimately MTP arthrodesis for recalcitrant cases. |
| Undercorrection | 5-10% | Conservative: Splinting, exercises. Surgical: Re-operation with more aggressive soft tissue release, additional osteotomy, or tendon transfer to achieve desired alignment. |
| Hallux Valgus Overcorrection | <5% | Initial management with dynamic splinting or taping. If persistent and symptomatic, soft tissue balancing (e.g., lateral capsule reefing, medial tendon transfer), or in severe cases, conversion to MTP arthrodesis. |
| Stiffness / Arthrofibrosis | 10-20% | Conservative: Early, aggressive physical therapy, passive and active range of motion exercises, stretching, dynamic splinting. Surgical: MUA (Manipulation Under Anesthesia) for early-stage stiffness. Arthroscopic or open arthrolysis for chronic, severe cases. |
| Infection | 1-5% (superficial: higher) | Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, intravenous antibiotics based on culture, hardware removal (if infected). May require staged reconstruction if osteomyelitis develops. |
| Neurovascular Injury | <1-5% (nerve) | Dorsal medial cutaneous nerve of hallux: Symptoms include numbness, dysesthesia, neuroma formation. Conservative: Desensitization, topical agents. Surgical: Neurolysis, neurectomy with proximal implantation, or nerve grafting in rare cases of transection. Vascular injury is exceedingly rare. |
| Hardware-Related Issues | 5-10% | Prominent hardware leading to irritation, breakage, or loosening. Management: Symptomatic hardware removal after bone healing (typically 3-6 months post-op). Revision fixation if non-union or instability. |
| Delayed Union / Non-union | <5% (osteotomy) | Conservative: Extended non-weight bearing, immobilization, bone stimulator. Surgical: Revision osteotomy with bone grafting, stable internal fixation. |
| Transfer Metatarsalgia | 5-15% | Often due to altered weight bearing. Conservative: Metatarsal pads, orthotics, shoe modifications. Surgical: Lesser metatarsal osteotomies (e.g., Weil osteotomy) for recalcitrant cases. |
| Complex Regional Pain Syndrome (CRPS) | <1-2% | Early recognition and multidisciplinary approach: Physical therapy, pain management (nerve blocks, medications), psychological support. Refer to pain specialist. |
| Wound Healing Complications | 5-10% | Hematoma, dehiscence, skin necrosis. Management: Local wound care, strict elevation, sterile dressings. Surgical debridement and closure for dehiscence, flap coverage in severe cases. |
| Phalangeal Fractures | <1% | Intra-operative or post-operative fracture, especially with aggressive manipulation or osteotomy. Management: K-wire fixation, immobilization. |
General Principles of Complication Management:
- Early Recognition: Prompt identification of complications is key to effective management.
- Conservative First: Many complications, especially mild stiffness or minor wound issues, can be managed non-operatively initially.
- Patient Education: Thoroughly discuss potential complications pre-operatively and manage patient expectations.
- Multidisciplinary Approach: Involve pain specialists, physical therapists, and infectious disease consultants when appropriate.
- Documentation: Maintain meticulous records of intraoperative findings, post-operative course, and complication management.
Hallux varus surgery is technically demanding, and surgeons performing these procedures must be well-versed in revision strategies and salvage options to achieve the best possible outcomes for their patients.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing outcomes, restoring function, and preventing recurrence or stiffness after hallux varus correction. Protocols are tailored to the specific surgical procedure performed, the stability achieved intraoperatively, and the patient's individual healing capacity.
Phase 1: Immediate Post-Operative Period (Day 0 to 2 Weeks)
Goals:
* Pain and edema control.
* Protection of surgical correction.
* Maintain proper alignment.
* Prevent complications (infection, DVT).
Interventions:
*
Immobilization:
*
Dressing:
A bulky dressing with a splint (e.g., sugar tong or plaster splint) or a specific hallux varus splint is applied in the operating room to maintain the corrected position (often slight valgus overcorrection).
*
Surgical Shoe/Boot:
The patient wears a rigid-soled post-operative shoe or CAM walker boot.
*
Weight-Bearing:
*
Non-weight bearing (NWB) or Touch-down weight bearing (TDWB):
For procedures involving osteotomies, significant soft tissue release, or joint reconstruction, NWB or TDWB with crutches is typically prescribed for 2-4 weeks.
*
Partial weight bearing (PWB):
May be allowed in a surgical shoe for less extensive soft tissue procedures if stability permits.
*
Pain Management:
Oral analgesics, often including a non-opioid component (e.g., NSAIDs, acetaminophen), and judicious use of opioids. Regional nerve blocks performed pre-operatively provide excellent early pain control.
*
Edema Control:
Strict elevation above heart level, intermittent icing for 15-20 minutes several times a day.
*
Monitoring:
Regular wound checks for signs of infection, neurovascular compromise, or hardware migration.
*
Mobility:
Limited ankle ROM (plantarflexion/dorsiflexion) and non-weight bearing exercises for the knee and hip to prevent stiffness.
Phase 2: Early Mobilization & Progressive Weight-Bearing (Weeks 2-6)
Goals:
* Gradual restoration of MTP joint range of motion (ROM).
* Progressive weight-bearing.
* Maintain alignment.
* Reduce swelling.
Interventions:
*
Dressing/Splinting:
The initial bulky dressing and splint are typically removed at 2 weeks. Sutures/staples are removed.
* A smaller dressing and a toe spacer or dynamic hallux splint (e.g., nighttime splint) are often recommended to maintain great toe alignment and prevent recurrence, especially at night.
*
Weight-Bearing:
*
Progressive Weight-Bearing (PWB) to Full Weight-Bearing (FWB):
Gradually transition from NWB/TDWB to FWB in the surgical shoe or CAM walker boot, guided by surgeon protocol and radiographic healing (if osteotomies were performed). This usually occurs between weeks 2-6.
*
Range of Motion (ROM) Exercises:
*
Gentle Active and Passive MTP Joint ROM:
Initiate cautious flexion and extension exercises of the great toe, typically avoiding forceful end-range motion initially, particularly into varus.
*
IP Joint ROM:
If an EHL transfer with IP joint fusion was performed, maintain immobilization of the IP joint.
*
Physical Therapy:
May begin around week 3-4, focusing on:
* Manual therapy to reduce swelling and improve joint mobility.
* Gentle soft tissue mobilization around the MTP joint.
* Exercises to maintain ankle and foot mobility.
*
Edema Control:
Continued elevation and icing. Compression stockings for the lower leg may be beneficial.
Phase 3: Strengthening & Return to Activity (Weeks 6-12)
Goals:
* Restore full, pain-free MTP joint ROM.
* Improve intrinsic foot muscle strength.
* Normalize gait pattern.
* Prepare for return to daily activities.
Interventions:
*
Footwear:
Transition from surgical shoe/boot to a wide, supportive, comfortable athletic shoe with good arch support. Avoid narrow or high-heeled shoes.
*
Range of Motion & Flexibility:
* Progress MTP joint ROM exercises, actively working towards full flexion and extension.
* Gentle stretching of the Achilles tendon and calf muscles.
*
Strengthening Exercises:
*
Intrinsic Foot Muscles:
Toe curls (towel scrunches), marble pick-ups, short foot exercises to activate the intrinsic foot musculature.
*
Extrinsic Foot Muscles:
Calf raises, ankle inversion/eversion exercises.
* Specific exercises to activate the transferred tendon (e.g., abductor hallucis or split EHL).
*
Gait Training:
Address any compensatory gait patterns. Work on smooth heel-to-toe transition and toe-off.
*
Balance and Proprioception:
Single-leg standing, wobble board exercises.
*
Activity Progression:
Gradually increase walking distance and duration. Light aerobic activities (swimming, cycling) can typically be initiated after 8-10 weeks.
Phase 4: Advanced Strengthening & Return to Sport/High-Impact Activities (Weeks 12+)
Goals:
* Full restoration of strength, endurance, and agility.
* Return to sport or demanding work activities.
Interventions:
*
Sport-Specific Training:
For athletes, a progressive return to sport program, including agility drills, jumping, and running.
*
Continued Strengthening:
Advanced exercises for foot and ankle muscles, core stability.
*
Footwear Modification:
Assessment for custom orthotics if needed to maintain alignment and support.
*
Long-Term Follow-up:
Regular follow-up with the surgeon to monitor progress and address any concerns. Continued use of toe spacers or night splints may be recommended for up to 6 months or longer, especially in cases of strong deforming forces or a history of recurrence.
Specific Considerations for MTP Arthrodesis:
* Immobilization is typically longer (6-8 weeks) in a CAM walker or cast until radiographic signs of fusion are evident.
* Weight-bearing is gradually progressed after the initial immobilization period.
* Rehabilitation focuses on regaining strength in other foot muscles and accommodating the loss of MTP motion.
Patient compliance with the rehabilitation protocol is paramount for a successful outcome. Clear instructions, regular communication, and ongoing support from the surgical and rehabilitation team are essential.
Summary of Key Literature / Guidelines
The literature on hallux varus is extensive, often focusing on its iatrogenic origins following hallux valgus surgery and the diverse surgical strategies for correction. While no single universally accepted guideline exists, several key principles and techniques have emerged as standard practice.
-
Iatrogenic Etiology Dominance: A consistent theme across the literature is that iatrogenic hallux varus accounts for the vast majority of cases. Early studies by Mann and Coughlin in the 1980s highlighted the critical role of excessive lateral release and medial capsular plication in its development. This underscores the importance of balanced soft tissue release and careful assessment of intraoperative correction during hallux valgus procedures.
-
Soft Tissue Balancing as the Cornerstone:
- Abductor Hallucis Tendon Transfer (AHTR): Multiple authors, including Henry and others, have advocated for the transfer of the abductor hallucis tendon to the lateral base of the proximal phalanx as a primary method for correcting flexible hallux varus. This technique effectively releases the primary medial deforming force and creates a dynamic lateral pull. The efficacy of this procedure has been supported by various case series demonstrating good to excellent results in terms of pain relief and correction.
- Extensor Hallucis Longus (EHL) Management: For dynamic varus with EHL bowstringing or contracture, EHL lengthening (Z-plasty) is commonly employed. For more significant or resistant cases, EHL tendon transfer, either split or full, has been a key surgical strategy. The split EHL tendon transfer (e.g., modified Jones procedure) to the lateral aspect of the proximal phalanx provides a dynamic lateral pull while preserving some EHL function. Full EHL transfer necessitates IP joint fusion to prevent a "floppy toe," as demonstrated in studies evaluating the biomechanical effects of such transfers.
-
Bony Correction for Fixed Deformities:
- When hallux varus is associated with bony malalignment, such as an overcorrected IM angle or an articular incongruity (e.g., negative DMAA), osteotomies are indicated. The reverse Akin osteotomy (medial closing wedge proximal phalangeal osteotomy) is a well-established technique to fine-tune the varus correction at the MTP joint level, as described by Yu and colleagues. Distal metatarsal osteotomies (e.g., reverse Chevron or Weil) are less commonly required but may be considered for significant first metatarsal head malposition.
- MTP Arthrodesis: For severe, rigid, painful hallux varus, particularly with significant MTP joint arthrosis or after multiple failed revisions, fusion of the first MTP joint remains the most reliable salvage procedure. Reviews by De Palma and others affirm the high rates of patient satisfaction and pain relief achieved with arthrodesis, albeit at the cost of motion.
-
Comprehensive Assessment and Individualized Treatment: The literature consistently emphasizes the need for a thorough clinical and radiographic assessment to identify the precise etiology and components of the deformity. Authors like Hattrup and Johnson advocate for a graded approach, starting with less invasive soft tissue releases and progressing to more complex tendon transfers and osteotomies as needed. The choice of procedure must be individualized, considering patient activity level, joint condition, and the flexibility of the deformity.
-
Prevention is Key: A significant portion of the literature focuses on preventing iatrogenic hallux varus during primary hallux valgus surgery. Guidelines stress careful soft tissue balancing, avoiding excessive lateral release, cautious medial capsular plication, and avoiding routine lateral sesamoidectomy. Intraoperative assessment of toe alignment and stability is critical to prevent overcorrection.
In conclusion, the understanding and management of hallux varus have evolved significantly. While iatrogenic causes remain predominant, current surgical principles revolve around precise identification of deforming forces, restoring soft tissue balance (often by releasing contracted medial structures and enhancing lateral dynamic support through tendon transfers), and correcting bony malalignment with judicious osteotomies. MTP arthrodesis serves as a robust salvage option. The focus on preserving the "lateral capsule's lateral support" in the context of hallux varus essentially translates to restoring the dynamic and static stability of the lateral aspect of the MTP joint to counteract the medializing forces, thereby preventing or correcting the deformity.
Clinical & Radiographic Imaging