Introduction & Epidemiology
Bunionette deformity, also known as Tailor's Bunion, is a prevalent and often painful condition affecting the lateral aspect of the forefoot. It is characterized by prominence of the lateral aspect of the fifth metatarsal head, leading to pain, callus formation, and difficulty with shoe wear. While less common than hallux valgus, bunionette deformities can be equally disabling, impacting patient quality of life and functional mobility.
Epidemiologically, bunionettes are observed across various demographics, though they are more commonly reported in women, often associated with constrictive footwear. The exact incidence is not precisely quantified in large-scale studies, but clinical experience suggests it is a significant contributor to lateral foot pain presenting in orthopedic clinics. The etiology is multifactorial, encompassing congenital factors (e.g., splayfoot, genetic predisposition), biomechanical imbalances (e.g., pronated foot type, equinus), and acquired factors, predominantly ill-fitting or narrow shoes that exert excessive pressure on the lateral forefoot.
The pathoanatomy of a bunionette can involve one or a combination of three primary components, as classically described by Kilmartin and others:
1.
Type I:
Isolated lateral hypertrophy of the fifth metatarsal head (enlarged lateral condyle), with normal intermetatarsal angle (IMA) between the fourth and fifth metatarsals, and normal fifth metatarsal shaft alignment.
2.
Type II:
Lateral bowing of the fifth metatarsal shaft, often leading to a wide metatarsal head-neck angle but normal 4-5 IMA.
3.
Type III:
Increased intermetatarsal angle between the fourth and fifth metatarsals (splayfoot deformity), pushing the fifth metatarsal head laterally.
Understanding these types is critical for guiding treatment, as the optimal surgical strategy varies depending on the underlying bony pathology. Lateral condylar resection, the focus of this discussion, is primarily indicated for Type I deformities where the principal issue is an enlarged lateral condyle causing direct impingement and pain.
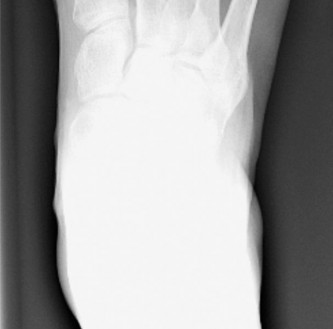
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the fifth metatarsophalangeal (MTP) joint is paramount to successful bunionette correction and prevention of complications.
The fifth metatarsal is the most lateral of the metatarsals. Its head articulates with the proximal phalanx of the fifth toe, forming the fifth MTP joint. The characteristic feature relevant to bunionettes is the often prominent lateral condyle of the fifth metatarsal head. This condyle can be congenitally enlarged or develop hypertrophy due to chronic irritation and pressure. The medial aspect of the head is relatively flat, and the articular surface is curved, allowing for plantarflexion-dorsiflexion and some abduction-adduction of the toe.
Soft tissue structures
surrounding the joint are crucial:
*
Joint Capsule:
Provides stability and contains the synovial fluid. A thickened or inflamed lateral capsule often accompanies the bony prominence.
*
Lateral Collateral Ligament:
Stabilizes the joint laterally. Over-resection of the condyle can compromise its integrity.
*
Extensor Digiti Minimi Brevis (EDMB) and Longus (EDML) Tendons:
Lie dorsally. The EDML is generally a slender slip of the extensor digitorum longus, while the EDMB originates from the cuboid and courses to the base of the proximal phalanx.
*
Abductor Digiti Minimi (ADM):
Originates from the calcaneal tuberosity and inserts into the lateral aspect of the base of the proximal phalanx and the lateral sesamoid. Its tendon runs along the plantar-lateral aspect of the metatarsal head.
*
Flexor Digiti Minimi Brevis (FDMB):
Originates from the base of the fifth metatarsal and inserts into the base of the proximal phalanx, often via a lateral sesamoid.
Neurovascular structures
requiring meticulous protection include:
*
Lateral Dorsal Cutaneous Nerve:
A terminal branch of the sural nerve, it typically runs dorsally and superficially along the lateral aspect of the fifth metatarsal and fifth MTP joint. It supplies sensation to the lateral aspect of the fifth toe and can be particularly vulnerable during incision and dissection, leading to neuroma formation or paresthesias if injured. Its course can be highly variable.
*
Proper Digital Nerves and Arteries:
These neurovascular bundles run along the plantar-lateral and plantar-medial aspects of the fifth toe and are deep to the ADM and FDMB muscles.
Biomechanics: During the gait cycle, the fifth MTP joint plays a role in forefoot stability and propulsion, though less significant than the first MTP joint. Weight-bearing on the lateral aspect of the foot, especially in the push-off phase, can exacerbate pain from a bunionette. A prominent lateral condyle can lead to increased pressure within shoes, causing chronic irritation of the overlying bursa and soft tissues, resulting in inflammation, pain, and eventual hypertrophic changes of the skin (callus) and bone.
Classification revisited:
The distinct types of bunionette deformities guide surgical selection:
*
Type I (Enlarged Metatarsal Head):
Characterized by an abnormally wide or prominent lateral condyle of the fifth metatarsal head. The 4-5 intermetatarsal angle (IMA) and the lateral bowing of the fifth metatarsal shaft are typically normal or minimally deviated. This is the primary indication for lateral condylar resection, as the deformity is localized to the articular prominence.
*
Type II (Lateral Bowing of Metatarsal Shaft):
The fifth metatarsal shaft itself bows laterally, leading to a prominent metatarsal head. While the condyle might be enlarged, the primary issue is the shaft angulation.
*
Type III (Increased 4-5 Intermetatarsal Angle):
A splayfoot deformity where the distance between the fourth and fifth metatarsals is abnormally increased, pushing the fifth metatarsal head laterally. This type often coexists with other forefoot deformities.
For Type II and III deformities, osteotomies (e.g., distal chevron, proximal closing wedge, oblique shaft osteotomy) are generally more appropriate to correct the underlying angular or splay deformity. Lateral condylar resection alone would be insufficient for these types and risks recurrence or suboptimal correction.
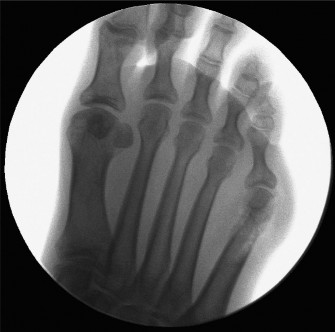
Indications & Contraindications
Careful patient selection based on clinical and radiographic findings is paramount for optimizing outcomes with lateral condylar resection. This procedure is generally reserved for specific types of bunionette deformities.
Indications for Lateral Condylar Resection
The primary indication for lateral condylar resection is a Type I bunionette deformity , characterized by an isolated lateral prominence or hypertrophy of the fifth metatarsal head, in the absence of significant lateral bowing of the fifth metatarsal shaft or an increased 4-5 intermetatarsal angle.
Specific indications include:
*
Persistent pain and discomfort
on the lateral aspect of the fifth MTP joint, refractory to adequate conservative management.
*
Clinical evidence of a prominent lateral condyle
of the fifth metatarsal head as the primary source of symptoms, often with associated callosity or bursitis.
*
Radiographic confirmation of Type I bunionette:
* Normal or near-normal 4-5 intermetatarsal angle (typically < 8-9 degrees).
* Absence of significant lateral bowing of the fifth metatarsal shaft.
* Clear hypertrophy or abnormal shape of the lateral condyle of the fifth metatarsal head.
*
Functional impairment:
Difficulty wearing standard footwear, participation in daily activities, or sports due to pain.
*
Stable 5th MTP joint:
No significant instability or severe degenerative arthrosis that would necessitate alternative procedures.
*
Adequate soft tissue envelope:
Sufficient skin and subcutaneous tissue to allow for uncomplicated closure.
Contraindications for Lateral Condylar Resection
Contraindications preclude the use of lateral condylar resection as a standalone procedure and often necessitate alternative surgical strategies:
*
Type II bunionette (lateral bowing of the fifth metatarsal shaft):
Resecting the condyle without addressing the shaft angulation will likely result in inadequate correction and recurrence.
*
Type III bunionette (increased 4-5 intermetatarsal angle):
The primary pathology here is metatarsal splay; condylar resection alone will not correct the underlying splay and may not relieve symptoms.
*
Severe degenerative arthritis of the fifth MTP joint:
Resection in this context may worsen joint mechanics and lead to pain or instability. Arthrodesis or arthroplasty might be more appropriate.
*
Fifth MTP joint instability:
If the joint is inherently unstable, condylar resection could exacerbate this.
*
Active local or systemic infection.
*
Severe peripheral vascular disease or uncontrolled diabetes:
Compromises wound healing and increases infection risk.
*
Peripheral neuropathy:
Particularly insensate foot, as this increases the risk of undetected post-operative complications and non-compliance with rehabilitation.
*
Unrealistic patient expectations:
Patients must understand the goals and limitations of the procedure.
*
Inadequate conservative management trial:
Surgery should generally be considered only after a reasonable course of non-operative treatments has failed.
Operative vs. Non-Operative Indications
| Feature | Non-Operative Management | Operative Management (Lateral Condylar Resection) |
|---|---|---|
| Pain Level | Mild to moderate, intermittent, tolerable | Persistent, severe, disabling pain despite conservative measures |
| Functional Impact | Minimal interference with daily activities, adaptable with footwear | Significant limitation of daily activities, inability to wear standard shoes |
| Callus/Bursitis | Present, manageable with padding, local care | Recurrent, painful, unmanageable callosity or bursitis over prominence |
| Radiographic Findings | Any bunionette type, but especially Type I with minimal prominence | Confirmed Type I bunionette with clear lateral condylar hypertrophy |
| Response to Conservative | Symptomatic relief with shoe modification, padding, orthotics, NSAIDs | Failure of at least 3-6 months of comprehensive conservative therapy |
| Patient Desire | Willingness to manage symptoms non-surgically | Desire for definitive correction and improvement in shoe wear tolerance |
| Co-morbidities | Significant medical co-morbidities that increase surgical risk | Acceptable surgical risk profile, well-controlled systemic conditions |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are crucial for ensuring surgical safety, optimizing exposure, and achieving the desired outcome.
Pre-Operative Planning
-
Clinical Assessment:
- History: Document duration of symptoms, nature of pain (location, intensity, aggravating/alleviating factors), impact on shoe wear, previous treatments (and their efficacy), medical comorbidities (diabetes, vascular disease, neuropathy), and allergies.
-
Physical Examination:
- Visual Inspection: Assess the severity of the bunionette prominence, presence of callus, bursitis, skin integrity, and any toe deformities (e.g., hammertoe).
- Palpation: Identify the precise point of maximum tenderness and the extent of the bony prominence.
- Range of Motion (ROM): Assess active and passive ROM of the fifth MTP joint. Look for stiffness, crepitus, or pain with motion.
- Neurovascular Status: Evaluate sensation (particularly lateral dorsal cutaneous nerve distribution), capillary refill, and pedal pulses. Document any pre-existing neuropathy.
- Foot Type Assessment: Observe for pes planus or cavus foot deformities, forefoot splay, and gait analysis if relevant.
-
Radiographic Evaluation:
-
Weight-Bearing X-rays:
Essential for proper classification and surgical planning. Obtain standard views:
- Anteroposterior (AP): Measure the 4-5 intermetatarsal angle (IMA, normal < 8-9 degrees), assess the contour of the fifth metatarsal head, and evaluate the lateral bowing of the fifth metatarsal shaft.
- Lateral: Assess the fifth metatarsal head articulation and any plantarflexion of the fifth metatarsal.
- Oblique: Provides the best view of the lateral condyle of the fifth metatarsal head and shaft for Type I bunionettes. This view is crucial for identifying the extent of hypertrophy.
- Consider advanced imaging: Rarely indicated for bunionette, but MRI might be considered for evaluation of soft tissue masses or inflammatory conditions if the diagnosis is unclear.
-
Weight-Bearing X-rays:
Essential for proper classification and surgical planning. Obtain standard views:
- Medical Clearance: Obtain appropriate medical clearance from the patient's primary care physician or specialist as indicated by comorbidities.
- Informed Consent: Discuss the surgical procedure, potential benefits, risks (including nerve injury, infection, recurrence, stiffness, pain), alternatives, and expected recovery course. Emphasize that recurrence is possible if the primary pathology is not solely a condylar hypertrophy.
- Antibiotic Prophylaxis: Administer appropriate intravenous antibiotics (e.g., cefazolin) within one hour prior to incision.
Patient Positioning
- Anesthesia: The procedure can be performed under regional anesthesia (e.g., ankle block or popliteal block), general anesthesia, or a combination. The choice depends on patient preference, surgeon preference, and anesthesiologist assessment.
-
Positioning:
- The patient is typically positioned supine on the operating table.
- A foot rest or small bump beneath the ipsilateral hip may be used to internally rotate the leg, presenting the lateral aspect of the foot to the surgeon more favorably.
- The foot should be positioned to allow for full range of motion of the ankle and MTP joints during the procedure.
- Tourniquet: A thigh or ankle tourniquet is routinely used to provide a bloodless field, which is critical for precise dissection and nerve identification. The tourniquet is inflated after exsanguination of the limb (e.g., with an Esmarch bandage).
- Sterile Preparation and Draping: The limb is prepped from the mid-calf to the toes using an antiseptic solution. Sterile draping isolates the operative foot, ensuring a sterile field. The toes should remain accessible for manipulation.
Detailed Surgical Approach / Technique
The goal of lateral condylar resection is to remove the hypertrophied lateral prominence of the fifth metatarsal head while preserving joint integrity, stability, and crucial neurovascular structures. The technique is relatively straightforward but requires meticulous execution.
1. Incision
- Approach: A dorsolateral longitudinal incision is typically employed.
- Location: The incision is centered over the lateral aspect of the fifth metatarsal head and fifth MTP joint.
- Length: Approximately 3-4 cm, extending from just proximal to the joint line to the mid-shaft of the proximal phalanx.
- Landmarks: Identify the prominence of the bunionette clinically. The incision should be directly over this prominence.
- Considerations: A curvilinear incision can also be used, curving slightly plantar or dorsal to minimize tension on the scar, though a straight incision provides excellent exposure. The incision should be made carefully through the skin only.
2. Dissection and Exposure
- Subcutaneous Dissection: Using sharp and blunt dissection, the subcutaneous tissues are carefully elevated. The most critical step here is to identify and protect the lateral dorsal cutaneous nerve (a branch of the sural nerve). This nerve typically runs superficially and parallel to the fifth metatarsal shaft and joint line. It can be quite superficial and is highly variable in its course. Employing small self-retaining retractors (e.g., Weitlaner) will help maintain exposure without excessive traction. Meticulous blunt dissection should be directed from proximal to distal and superficial to deep.
- Bursa Excision: If a significant adventitial bursa is present over the metatarsal head, it is usually excised at this stage, as it is often a source of inflammation.
- Capsular Incision: Once the nerve is safely retracted (typically dorsally), the joint capsule is identified. A longitudinal incision is made through the lateral aspect of the joint capsule, extending from the metatarsal neck distally to the base of the proximal phalanx. This exposes the lateral aspect of the fifth metatarsal head and its articular surface. The capsule and any underlying synovium can be elevated subperiosteally to expose the bony prominence.
3. Lateral Condylar Resection
- Identification of Prominence: With the joint capsule opened and retracted, clearly visualize the hypertrophied lateral condyle of the fifth metatarsal head. Flexing and extending the toe can help identify the points of impingement.
-
Osteotomy:
- A small oscillating saw with a narrow blade (e.g., 2.7 mm) is commonly used. Alternatively, an osteotome and mallet can be utilized.
- The cut is made parallel to the lateral articular surface of the metatarsal head, removing the prominent condyle. The aim is to create a smooth contour, restoring the normal anatomical shape of the metatarsal head.
-
Crucial Points:
- Avoid over-resection: Removing too much bone can lead to lateral instability of the joint, malalignment, or compromise of the lateral collateral ligament. Aim to resect just enough bone to alleviate the prominence, typically 3-5 mm.
- Avoid under-resection: Incomplete removal will lead to persistent symptoms and potential recurrence.
- Protect the articular cartilage: The saw blade should not violate the weight-bearing articular surface of the metatarsal head. The cut should be directed just lateral to the articular cartilage margin.
- Smooth contour: After the bone is resected, use a rasp or bone file to smooth any sharp edges, preventing soft tissue irritation.
- Intraoperative Assessment: Flex and extend the fifth toe to ensure there is no residual impingement and that the new lateral contour is smooth and free of any palpable prominence. The range of motion should be free.
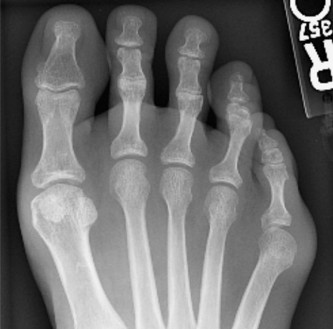
4. Soft Tissue Management
- Capsular Closure: The lateral joint capsule is closed with absorbable sutures (e.g., 3-0 absorbable). If there was excessive laxity or an attempt at slight tightening is desired, a small capsular plication can be performed, but this is less common with pure condylar resection and is more characteristic of procedures involving medial advancement or release. Ensure the joint moves freely after closure.
- Subcutaneous Closure: The subcutaneous layers are approximated using absorbable sutures (e.g., 3-0 or 4-0 absorbable), taking care to minimize dead space and protect the superficial nerves.
- Skin Closure: The skin is closed with non-absorbable sutures (e.g., 4-0 nylon) or staples, typically in a simple interrupted or running subcuticular fashion.
5. Dressing
- A sterile, non-adherent dressing is applied directly to the incision.
- A soft, compressive dressing is then applied to control edema and provide comfort. This often includes padding between the fourth and fifth toes to maintain alignment, though this is less critical than with hallux valgus surgery.
- A post-operative shoe or stiff-soled surgical shoe is applied, which allows for immediate weight-bearing.
Complications & Management
While lateral condylar resection is generally considered a safe procedure, a comprehensive understanding of potential complications, their incidence, and management strategies is vital for all orthopedic surgeons.
| Complication | Incidence (Approximate) | Management and Salvage Strategies |
|---|---|---|
| Lateral Dorsal Cutaneous Nerve Injury / Neuroma | 5-15% | Prevention: Meticulous blunt dissection, careful retraction, identification and protection of the nerve. Management: Early intervention with rest, NSAIDs, nerve gliding exercises, topical desensitization. If persistent, consider gabapentin/pregabalin, local anesthetic injections, pulsed radiofrequency ablation. For severe, recalcitrant symptoms, surgical exploration, neurectomy with proximal burial of nerve stump, or direct repair may be necessary. |
| Infection | < 1-2% | Prevention: Aseptic technique, pre-operative antibiotics. Management: Superficial infections may respond to oral antibiotics and local wound care. Deep infections require surgical debridement, intravenous antibiotics guided by culture, and potentially hardware removal (if any auxiliary fixation was used, which is rare for pure condylar resection). |
| Recurrence of Deformity | 5-10% | Prevention: Proper patient selection (true Type I bunionette), adequate resection of the condyle. Management: If due to under-resection, revision condylar resection. If due to underlying unaddressed biomechanical factors (e.g., misdiagnosis as Type I when it was Type II or III), a more extensive procedure like an osteotomy (e.g., distal chevron, proximal closing wedge) may be required. |
| Stiffness / Limited Range of Motion | 5-10% | Prevention: Early mobilization protocol, avoiding aggressive capsular plication. Management: Physical therapy, gentle stretching, mobilization exercises. If severe and persistent, manipulation under anesthesia or arthrolysis may be considered, though uncommon for this procedure. |
| Over-resection / Instability | Rare | Prevention: Conservative bone removal, preserving the lateral collateral ligament and articular surface. Management: Difficult to treat. For mild symptoms, physical therapy and bracing. For severe instability or pain, options are limited and may include arthrodesis of the 5th MTP joint, or in select cases, soft tissue reconstruction (lateral collateral ligament repair/reconstruction). |
| Metatarsalgia (Transfer Lesion) | < 5% | Prevention: Rarely seen with isolated condylar resection unless combined with other procedures altering forefoot mechanics significantly. Management: Orthotics, shoe modifications, metatarsal pads. Surgical correction of the primary cause of transfer metatarsalgia (e.g., shortening osteotomy of an adjacent metatarsal) if severe and persistent. |
| Chronic Pain / Complex Regional Pain Syndrome (CRPS) | < 1% | Prevention: Gentle tissue handling, good pain control. Management: Early recognition and multidisciplinary approach including physical therapy, pain management specialists, nerve blocks, medications (gabapentin, tricyclic antidepressants), and psychological support. |
| Cosmetic Dissatisfaction | Variable | Prevention: Realistic patient expectations, discussing potential for scarring and residual prominence. Management: Scar massage, silicone sheeting. Revision surgery is rarely indicated solely for cosmetic reasons unless significant prominence remains. |
| Non-union/Mal-union | Not applicable | Lateral condylar resection does not involve osteotomy of the metatarsal shaft where non-union or mal-union would be a concern. This complication is specific to osteotomy-based bunionette corrections. |
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is critical for pain management, edema control, restoration of function, and successful integration back into activities. The protocol for lateral condylar resection is generally less restrictive than for osteotomy-based procedures.
Phase 1: Immediate Post-Operative (Days 0-14)
Goals: Pain control, edema reduction, wound healing, protective weight-bearing.
-
Weight-Bearing:
- Immediate full weight-bearing as tolerated in a stiff-soled post-operative shoe, surgical boot, or wide, stable shoe is typically allowed. Crutches or a walker may be used for balance and comfort initially, especially in the first few days.
- Patients should be instructed on a flat-foot gait pattern, avoiding push-off from the forefoot initially.
-
Elevation & Ice:
- Strict elevation of the foot above heart level for the first 48-72 hours, and then frequently for edema control.
- Ice application for 15-20 minutes every 2-3 hours to reduce swelling and pain.
-
Wound Care:
- Keep the surgical dressing clean, dry, and intact.
- First dressing change typically occurs at 1 week post-op.
- Sutures/staples are usually removed at 10-14 days post-op.
- Monitor for signs of infection (redness, increased pain, warmth, discharge).
-
Pain Management:
- Prescribe oral analgesics (opioids for short-term, NSAIDs if not contraindicated) and counsel on their appropriate use.
- Regional anesthesia (ankle block) can significantly aid in post-operative pain control.
-
Range of Motion (ROM):
- Gentle, active range of motion of the ankle and non-operated toes.
- Passive range of motion of the operated fifth MTP joint may be initiated by the surgeon or therapist after suture removal, depending on soft tissue healing and comfort.
Phase 2: Early Mobilization & Strengthening (Weeks 2-6)
Goals: Restore full non-painful ROM, progress weight-bearing, reduce swelling, improve muscle activation.
-
Weight-Bearing & Footwear:
- Gradual transition from the post-operative shoe to comfortable, wide-toe box athletic shoes or supportive lace-up shoes once the incision is well-healed and pain allows (typically around week 3-4).
- Avoid high heels, narrow shoes, or shoes that place direct pressure on the surgical site.
-
Range of Motion:
- Active and passive ROM exercises for the fifth MTP joint are initiated and progressed. This includes plantarflexion, dorsiflexion, abduction, and adduction exercises to prevent stiffness.
- Gentle mobilization techniques can be performed by a physical therapist.
- Edema Control: Continue with elevation, icing, and compression stockings if needed.
-
Scar Management:
- Once the wound is completely closed, initiate scar massage to prevent adhesions and improve scar pliability. Silicone gel sheeting may also be used.
-
Gentle Strengthening:
- Introduction of light resistance exercises for the foot and ankle musculature, focusing on intrinsic foot muscles.
- Toe curls, marble pick-ups, towel gathers.
Phase 3: Progressive Strengthening & Return to Activity (Weeks 6-12+)
Goals: Restore strength and endurance, improve balance and proprioception, gradual return to high-impact activities.
-
Strength & Endurance:
- Progressive strengthening exercises for the entire lower extremity, with an emphasis on ankle and foot muscles.
- Resistance band exercises for ankle eversion/inversion, plantarflexion/dorsiflexion.
- Calf raises, single-leg balance exercises.
-
Proprioception & Balance:
- Balance board exercises, single-leg stance, functional activities.
-
Activity Progression:
- Gradual return to low-impact activities (e.g., walking for longer distances, cycling, swimming).
- High-impact activities (running, jumping sports) are typically deferred until 3-4 months post-op and only after demonstrating adequate strength, ROM, and absence of pain. This progression should be guided by symptoms.
- Footwear: Continue to emphasize supportive, wide-toe box shoes. Orthotics may be considered if pre-existing biomechanical issues (e.g., pronation) were present.
- Long-Term Follow-up: Patients should be followed clinically for several months to ensure full recovery and address any residual issues.
Note: Individual rehabilitation protocols may vary based on surgeon preference, patient specific factors, and intraoperative findings. Communication between the surgeon, physical therapist, and patient is paramount for optimal outcomes.
Summary of Key Literature / Guidelines
The surgical treatment of bunionette deformities has evolved significantly, with a robust body of literature delineating various techniques. Lateral condylar resection, while a relatively straightforward procedure, is underscored by specific indications that must be meticulously adhered to for optimal results, as highlighted in key academic discussions and guidelines.
Historical Context and Classification:
The understanding of bunionette deformities greatly benefited from classification systems. Historically, Tailor's bunion was recognized, but a structured approach to its pathoanatomy and surgical management gained traction with classifications such as that by
Kilmartin and others
(1993), distinguishing types based on metatarsal head enlargement, lateral bowing of the shaft, and increased 4-5 intermetatarsal angle. This differentiation is fundamental to the appropriate application of lateral condylar resection, which is specifically indicated for
Type I deformities
(isolated lateral hypertrophy of the fifth metatarsal head).
Evidence Supporting Lateral Condylar Resection:
Numerous studies have demonstrated the efficacy of lateral condylar resection for appropriately selected patients.
*
Clinical Outcomes:
Studies, such as those by
Coughlin and Carlson (1998)
, have shown good to excellent outcomes in terms of pain relief, improved shoe wear, and patient satisfaction for Type I bunionettes treated with simple lateral condylar excision. They emphasized that this procedure effectively addresses the bony prominence without significantly altering the biomechanics of the joint or requiring osteotomies, thereby often allowing for faster recovery.
*
Radiographic Outcomes:
Radiographic assessment post-resection typically confirms the removal of the lateral prominence, without significant changes in the 4-5 intermetatarsal angle or lateral bowing, supporting its specific role in Type I corrections.
*
Comparison to Osteotomies:
When compared to osteotomy-based procedures (e.g., distal chevron osteotomy, proximal closing wedge osteotomy) which are indicated for Type II and III bunionettes, lateral condylar resection is associated with fewer complications related to bone healing (non-union, mal-union) and often a quicker return to full weight-bearing, reflecting its less invasive nature. However, it is crucial to recognize that applying condylar resection to Type II or III deformities will predictably lead to recurrence or inadequate correction, underscoring the importance of accurate classification.
Guidelines for Patient Selection:
The consensus in the literature strongly supports that the success of lateral condylar resection hinges on
rigorous patient selection
:
1.
Clinical Presentation:
Patients must present with a symptomatic, painful bunionette, primarily from direct pressure on the hypertrophied lateral aspect of the fifth metatarsal head. This pain should be refractory to a comprehensive trial of non-operative management (e.g., wider shoes, padding, orthotics, NSAIDs).
2.
Radiographic Confirmation:
Weight-bearing radiographs (AP, lateral, oblique) must definitively show a Type I bunionette. Key measurements to confirm include:
*
4-5 Intermetatarsal Angle:
Should be within normal limits (typically < 8-9 degrees). An increased angle indicates Type III, necessitating an osteotomy that shifts the entire metatarsal.
*
Lateral Bowing:
The fifth metatarsal shaft should not exhibit significant lateral bowing. Lateral bowing indicates a Type II deformity, which requires a corrective osteotomy of the metatarsal shaft.
*
Lateral Condylar Prominence:
Clear evidence of an enlarged or prominent lateral condyle of the fifth metatarsal head as the principal pathological finding.
Complications and Prevention:
The literature consistently highlights potential complications, with
lateral dorsal cutaneous nerve injury
being the most frequently cited concern (incidence varying from 5-15% depending on surgical diligence). Therefore, meticulous soft tissue dissection and nerve protection are paramount, as emphasized by anatomical studies detailing the nerve's variable course. Other potential issues, though less common, include inadequate resection leading to recurrence and over-resection leading to lateral instability of the joint.
Long-Term Outcomes:
Long-term studies generally report sustained pain relief and functional improvement for Type I bunionettes treated with lateral condylar resection, provided patient selection was appropriate. Patient satisfaction rates are high, and the procedure is recognized for its predictability in this specific subset of bunionette deformities.
Conclusion from Literature:
Lateral condylar resection is a well-established, effective, and relatively low-morbidity procedure for the treatment of
Type I bunionette deformities
. Its success is fundamentally linked to accurate pre-operative classification of the bunionette and meticulous surgical technique, particularly regarding nerve protection and appropriate bone resection. For Type II and III deformities, procedures involving metatarsal osteotomies remain the gold standard, as condylar resection alone would be insufficient to address the underlying skeletal malalignment. Thus, the question "Is Lateral Condylar Resection Right for You?" can only be answered definitively after a thorough clinical and radiographic assessment confirms a Type I bunionette.
