Introduction & Epidemiology
Fifth metatarsal base fractures represent a spectrum of injuries ranging from avulsion fractures of the styloid process to diaphyseal stress fractures. Among these, fractures of the metadiaphyseal junction, commonly known as Jones fractures (Zone II), are particularly challenging due to their propensity for delayed union and nonunion, especially in the athletic population. This predisposition stems from a critical compromise in vascularity and significant biomechanical stresses at this anatomical site.
Epidemiologically, fifth metatarsal fractures account for a substantial proportion of all foot fractures, with an estimated incidence of 1.4-1.9 per 1000 person-years. While Zone I avulsion fractures are the most common, Zone II and Zone III fractures, particularly stress fractures, are frequently observed in athletes engaging in high-impact or repetitive motion sports such as basketball, soccer, and running. The mechanism of injury for Jones fractures typically involves an adduction force to the forefoot with the ankle in plantarflexion, often during a sudden change in direction or landing from a jump. The high incidence of complications in Zone II fractures underscores the importance of precise diagnosis, risk stratification, and tailored management strategies to facilitate rapid and complete return to activity for athletes.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the fifth metatarsal is paramount for optimal management. The fifth metatarsal is subdivided into three critical zones by Stewart, Dameron, and Torg classification systems, which largely dictate treatment algorithms:
- Zone I (Styloid Process): Extends from the tip of the styloid to the metatarsal-cuboid articulation. Fractures here are typically avulsions caused by the pull of the peroneus brevis tendon or the lateral cord of the plantar aponeurosis. These usually have an excellent blood supply.
- Zone II (Metaphyseal-Diaphyseal Junction / Jones Fracture): Located approximately 1.5-3 cm distal to the tip of the styloid, involving the fourth and fifth metatarsal articulations. This watershed area is historically noted for its precarious blood supply, arising primarily from the nutrient artery entering the diaphysis and periosteal vessels. The distal fragment receives its supply via periosteal attachments, while the proximal fragment's supply is tenuous. Furthermore, this region is subjected to significant shear and bending forces during foot pronation and supination, particularly in athletic maneuvers.
- Zone III (Proximal Diaphysis): Extends distally from Zone II. Fractures in this zone are typically stress fractures, often seen in athletes due to repetitive microtrauma. These fractures usually have a better prognosis for healing than Zone II injuries but still require careful management.
The peroneus brevis tendon inserts on the dorsal surface of the tuberosity, while the peroneus tertius inserts on the dorsal aspect of the proximal fifth metatarsal shaft. The lateral cord of the plantar fascia also inserts into the tuberosity. These muscular and fascial attachments impart significant deforming forces across fracture lines, particularly with ankle inversion and adduction, which is the common mechanism for Jones fractures.
The blood supply to the fifth metatarsal is critical to understand the challenges of healing. The primary nutrient artery enters the diaphysis, running distally. The proximal metaphysis receives its supply from the periosteal vessels and small branches from the lateral plantar artery. The Zone II region lies at the junction of these two blood supply systems, making it a watershed area vulnerable to ischemia after fracture. This precarious vascularity, coupled with the high mechanical stresses, explains the historical high rates of delayed union and nonunion.
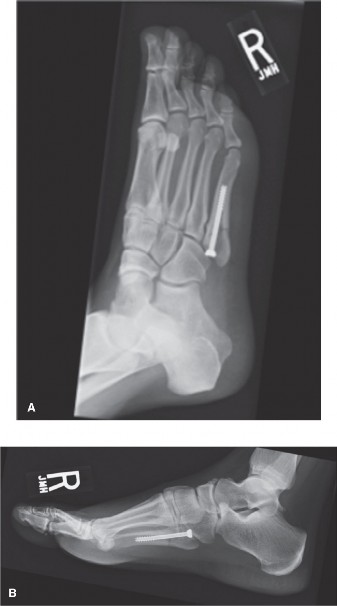
Image depicting the anatomical zones of the fifth metatarsal, highlighting the critical Zone II (Jones fracture) region.
Biomechanically, the fifth metatarsal plays a crucial role in lateral column stability, force transmission, and propulsion during gait. In athletes, the repetitive, high-magnitude forces generated during running, cutting, and jumping place considerable stress on this bone. The relatively narrow medullary canal and the anatomical angulation of the proximal metaphysis also contribute to its vulnerability to fracture and subsequent healing challenges.
Indications & Contraindications
Management of fifth metatarsal fractures, particularly those involving Zone II, demands a nuanced approach, balancing the risks of surgical intervention against the potential for delayed healing and prolonged disability with non-operative treatment. The patient's activity level, fracture displacement, chronicity, and the specific fracture zone are key determinants.
Indications for Operative Intervention:
- Acute Zone II Fractures (Jones Fractures) in Athletes: This is the most compelling indication. Due to high nonunion rates (up to 50% with conservative management) and the imperative for timely return to sport, internal fixation (typically intramedullary screw) is the standard of care.
- Displaced Zone II Fractures (>2mm): While displacement is less common in pure Jones fractures, any significant displacement (e.g., in comminuted patterns) often necessitates operative stabilization to achieve anatomical reduction and stability.
- Symptomatic Nonunion or Delayed Union of Zone II Fractures: After a trial of conservative management, persistent pain, disability, or clear radiographic signs of nonunion warrants surgical intervention, often with revision fixation and bone grafting.
- Zone I Fractures (Avulsion) with Significant Displacement or Incongruity: While most Zone I fractures are managed non-operatively, large, significantly displaced avulsion fragments (e.g., >2-3 mm) that compromise the cuboid-metatarsal articulation or cause persistent symptoms may require fixation.
- Zone III Stress Fractures (Proximal Diaphysis) Failing Conservative Management or in Elite Athletes: Persistent pain, imaging evidence of nonunion, or the need for accelerated return to play in high-level athletes may prompt intramedullary screw fixation, sometimes with bone grafting.
- Open Fractures: All open fractures require surgical debridement and stabilization, regardless of the zone.
- Polytrauma Patients: Often integrated into broader surgical management to ensure early mobilization.
Contraindications for Operative Intervention:
- Most Zone I Fractures (Avulsion Fractures): Unless significantly displaced or symptomatic, these respond well to conservative management.
- Minimally Displaced Zone II Fractures in Non-Athletic, Low-Demand Patients: A trial of non-weight-bearing cast immobilization may be considered, but patients must be counseled on the high risk of delayed union/nonunion and potential need for future surgery. This should be a cautious approach, as even in non-athletes, nonunion can be debilitating.
- Asymptomatic Nonunion: If a patient with a nonunion is completely asymptomatic and has no functional limitations, observation may be appropriate.
- Severe Comorbidities: Patients with significant medical comorbidities that preclude safe anesthesia and surgery (e.g., uncontrolled diabetes, severe peripheral vascular disease, active infection not related to the fracture site) may be better managed conservatively, accepting a higher risk of nonunion.
- Active Infection: Absolute contraindication to elective internal fixation at the fracture site.
The following table summarizes the general indications for operative versus non-operative management:
| Indication Type | Operative Management | Non-Operative Management |
|---|---|---|
| Zone I Fractures | - Displacement >2-3 mm, articular involvement, or persistent symptoms despite conservative care | - Most avulsion fractures, regardless of fragmentation, if minimally displaced and stable. Short leg cast/boot, NWB or PWB as tolerated. |
| Zone II Fractures |
-
Acute Jones fracture in athletes (mandatory)
- Acute Jones fracture in high-demand non-athletes desiring accelerated recovery - Displaced (e.g., >2mm angulation or translation) or comminuted fractures - Symptomatic delayed union or nonunion - Acute on chronic fractures |
- Select acute Jones fractures in low-demand, non-athletic patients who understand high nonunion risk and desire to avoid surgery. Strict NWB cast immobilization for 6-8 weeks, followed by progressive weight-bearing. |
| Zone III Fractures |
- Symptomatic stress fractures failing 3-6 months of conservative management
- Stress fractures in elite athletes requiring expedited return to sport |
- Most stress fractures initially managed with NWB/PWB in a boot/cast for 6-8 weeks, followed by gradual return to activity. |
| General Conditions |
- Open fractures
- Associated soft tissue injury requiring debridement |
- Asymptomatic nonunion in a low-demand patient
- Severe medical comorbidities precluding surgery |
Pre-Operative Planning & Patient Positioning
Pre-Operative Planning:
-
Imaging Review:
- Standard Radiographs: AP, lateral, and oblique views of the foot are essential. The lateral oblique view is particularly useful for visualizing the base of the fifth metatarsal. Look for fracture line configuration, displacement, comminution, and any signs of pre-existing stress changes.
- CT Scan: Highly recommended for complex comminuted fractures, chronic nonunions, or when intra-articular extension is suspected. It provides detailed bony anatomy, helps assess the medullary canal dimensions (crucial for screw sizing), and guides surgical approach.
- MRI: Rarely indicated for acute Jones fractures but useful for diagnosing stress fractures (Zone III) that are occult on plain radiographs, assessing associated soft tissue injuries, or differentiating between acute and chronic injuries in ambiguous cases.
-
Screw Sizing and Planning:
Intramedullary screw fixation is the gold standard for Jones fractures.
- Measure the medullary canal diameter on CT or high-quality radiographs (typically 4.5-6.5 mm).
- Determine the appropriate screw length to achieve bicortical purchase proximally and distal to the fracture site, ensuring adequate stabilization. The ideal screw should fill at least 70-80% of the medullary canal to maximize construct stiffness.
- Consider fully threaded versus partially threaded screws. Fully threaded screws are often preferred for their compression and stability in this metaphyseal-diaphyseal region.
- Tourniquet Time and Positioning: Anticipate the need for a thigh or ankle tourniquet. Plan for estimated surgical time.
- Consent: Thoroughly discuss the risks and benefits of surgery, including nonunion, infection, nerve injury, hardware prominence, and the potential need for secondary procedures. Manage patient expectations regarding recovery and return to sport.
- Anesthesia Consultation: Standard pre-operative assessment for regional (e.g., ankle block, popliteal block) or general anesthesia.
Patient Positioning:
- Supine Position: The patient is typically placed supine on the operating table.
- Hip Bump (Optional): A small bump may be placed under the ipsilateral hip to internally rotate the leg slightly, facilitating easier access to the lateral aspect of the foot.
- Tourniquet Application: A pneumatic tourniquet is applied to the proximal thigh or ankle. A thigh tourniquet provides a larger, bloodless field for a longer duration, while an ankle tourniquet offers more comfort but with a shorter duration.
- C-Arm Setup: The fluoroscopy unit (C-arm) should be positioned to allow for clear AP, lateral, and oblique views of the foot without repositioning the patient or the foot during the procedure. This typically involves placing the C-arm on the contralateral side of the table, allowing the image intensifier to come over the foot.
- Sterile Prep and Drape: The entire lower extremity, from the knee to the toes, is prepped with an antiseptic solution (e.g., chlorhexidine or povidone-iodine) and draped in a sterile fashion, ensuring adequate exposure of the lateral foot and sufficient working room for instruments and the C-arm.
Detailed Surgical Approach / Technique
The goal of surgical fixation for Jones fractures is to achieve stable internal fixation, allowing for early weight-bearing and an expedited return to sport. Intramedullary screw fixation is the preferred technique due to its biomechanical advantages, providing axial compression and rigid fixation within the cancellous bone.
Surgical Steps:
-
Incision:
- A longitudinal incision, approximately 3-4 cm in length, is made over the lateral aspect of the fifth metatarsal base, centered over the fracture site. The incision should be carefully placed to avoid injury to the superficial peroneal nerve branches (intermediate dorsal cutaneous nerve). Palpate the palpable styloid process and draw a line distally along the fifth metatarsal.
- Pearl: An alternative is a slightly more dorsal incision, angling slightly plantar, to avoid the nerve branches.
-
Dissection:
- The incision is carried down through the skin and subcutaneous tissue.
- Careful blunt dissection is used to identify and protect branches of the superficial peroneal nerve, which typically cross the surgical field. These branches are retracted dorsally.
- The periosteum over the proximal fifth metatarsal is identified. It may be incised longitudinally and reflected minimally to expose the fracture site, but excessive stripping should be avoided to preserve remaining vascularity. Direct visualization of the fracture site is often not necessary if reduction can be achieved indirectly.
-
Fracture Reduction:
- For acute fractures, reduction is typically achieved closed or with minimal manipulation. Apply gentle axial compression and slight eversion to the forefoot to align the fracture fragments.
- Confirm reduction with fluoroscopy (AP and lateral views). If reduction is inadequate, a small incision may be made directly over the fracture to allow for limited open reduction using a small periosteal elevator or a K-wire as a joystick. Avoid excessive disruption of the soft tissue envelope.
-
Guide Wire Placement:
- Entry Point: The crucial step for proper screw placement. The ideal entry point is located at the absolute tip of the fifth metatarsal tuberosity, approximately 5 mm proximal and slightly plantar to the palpable lateral margin of the metatarsal base. This allows for optimal alignment with the medullary canal.
- Using fluoroscopic guidance, a K-wire (e.g., 2.0 mm) is advanced from the entry point into the medullary canal. Ensure the wire is centered within the canal in both AP and lateral fluoroscopic views.
- The K-wire should cross the fracture site and advance well into the distal fragment, achieving bicortical purchase if possible. Confirm the position and length fluoroscopically.
-
Medullary Canal Preparation (Reaming):
- Once the guide wire is optimally positioned, the medullary canal may be reamed. Reaming is recommended, especially for smaller canals or when a larger diameter screw is desired. Reaming facilitates the passage of the screw and allows for the insertion of a larger diameter screw, which provides better fixation strength and rotational stability.
- Successively larger cannulated reamers are passed over the guide wire until the canal is adequately prepared for the planned screw diameter. The goal is to match the reamer size to the screw diameter or slightly undersize it, depending on bone quality and desired cortical purchase.
-
Screw Selection and Insertion:
- Select a fully threaded cannulated screw (typically 4.5 mm, 5.5 mm, or 6.5 mm in diameter) that approximates the reamed medullary canal diameter. The length should be chosen based on the pre-operative measurements and fluoroscopic confirmation during guide wire placement, aiming for maximum length while avoiding distal joint penetration.
- Pearl: A larger diameter screw (e.g., 5.5 mm or 6.5 mm) is generally preferred for active patients and athletes, as it provides greater torsional rigidity and decreases the risk of screw breakage or nonunion.
- Pass the cannulated screw over the guide wire. Advance the screw slowly under fluoroscopic guidance. Ensure it compresses the fracture site and achieves stable fixation. Avoid stripping the threads or over-tightening.
-
Once the screw is fully inserted, remove the guide wire.
markdown 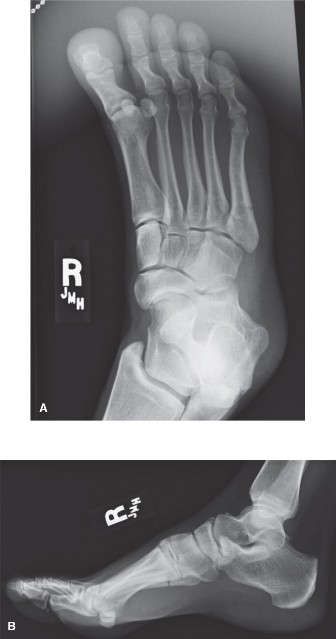
Image demonstrating intramedullary screw fixation of a fifth metatarsal fracture, with the screw centered within the medullary canal.
-
Final Assessment:
- Obtain final fluoroscopic images (AP, lateral, oblique) to confirm screw position, fracture reduction, and appropriate length. Ensure no distal joint penetration.
- Check for stability of the construct clinically by gently stressing the foot.
-
Closure:
- Irrigate the wound thoroughly.
- Close the periosteum (if incised), subcutaneous tissue, and skin in layers. Use absorbable sutures for deep layers and non-absorbable sutures or staples for skin.
- Apply a sterile dressing and a soft compressive wrap or a posterior splint for initial immobilization.
Technical Considerations and Pearls:
- Cannulated vs. Solid Screws: While cannulated screws facilitate placement over a guide wire, some surgeons prefer solid screws for their superior strength, particularly in younger, active patients.
- Thread Type: Fully threaded screws provide compression across the fracture site and increase stability. Partially threaded screws might be considered if significant compression is desired but careful attention to length and engagement is required.
- Over-reaming: In some cases, to ensure proper screw seating and to prevent fracture propagation, the medullary canal can be gently over-reamed by 0.5-1.0 mm compared to the screw diameter, especially in very dense bone.
- Revision Surgery: For nonunions, the technique may involve debridement of the fibrous nonunion, decortication of the fracture ends, autologous bone grafting (e.g., from the calcaneus or distal tibia), and larger diameter intramedullary screw fixation. Adjuvant bone stimulators may also be considered.
Complications & Management
Despite advancements in surgical technique, complications following fifth metatarsal fixation, particularly for Jones fractures, remain a concern. Understanding these and developing robust management strategies is crucial.
| Complication | Incidence | Management Strategy |
|---|---|---|
| Delayed Union / Nonunion | 5-15% (operative); up to 50% (non-operative) |
Delayed Union:
Continue immobilization, NWB/PWB, consider bone stimulator, observe.
Nonunion: Surgical revision (re-drilling canal, larger screw, autologous bone graft (e.g., calcaneal, iliac crest), debridement of fibrous tissue, PRP/BMPs). Address underlying factors (e.g., inadequate fixation, premature WB). |
| Hardware Prominence / Irritation | 10-20% | Most common complication. If symptomatic and fracture healed: Hardware removal after 6-12 months. If symptomatic and fracture unhealed: Assess for nonunion, revision fixation. |
| Screw Breakage | 2-5% | Indicates high stress and likely nonunion. Remove proximal fragment of screw. Treat as nonunion: Debridement, bone graft, larger diameter screw, potentially solid screw. Consider specific extraction tools if distal fragment is accessible. |
| Superficial Peroneal Nerve Injury | 5-10% (transient); <1% (permanent) |
Transient:
Observation, conservative management (neuropathic pain medications).
Persistent: Nerve block, neurolysis, rarely nerve repair if complete transection (uncommon). Prevention is key (careful dissection, appropriate incision). |
| Infection | 1-3% |
Superficial:
Oral antibiotics, local wound care.
Deep: Surgical debridement, IV antibiotics, cultures, potential hardware removal if fracture is healed. If nonunion and infection, staged approach (debridement, external fixation, delayed definitive fixation once infection controlled). |
| Malunion | Rare with IM screw | If asymptomatic, observe. If symptomatic (e.g., pain, gait alteration): Corrective osteotomy and internal fixation. |
| Complex Regional Pain Syndrome (CRPS) | <1% | Early diagnosis. Aggressive multidisciplinary management: Physical therapy, pain management (sympathetic blocks, medications), psychological support. |
| Refracture | <1% post-healing | Typically managed based on the new fracture pattern. Assess bone quality and biomechanical factors. If bone quality is poor, consider metabolic workup. |
Detailed Management Strategies:
-
Delayed Union / Nonunion:
This is the most significant concern with Zone II fractures.
- Assessment: Clinical symptoms (persistent pain, swelling), radiographic findings (sclerotic fracture margins, lack of bridging callus, lucency at fracture site), and sometimes CT scan.
- Revision Surgery: A common approach for established nonunion involves explantation of the original screw, re-debridement of the fracture site, freshening of the bone ends, meticulous re-reaming of the medullary canal, and insertion of a larger diameter, fully threaded intramedullary screw. Autologous bone grafting, typically from the ipsilateral calcaneus or iliac crest, is often combined to enhance biological healing. Adjunctive therapies such as pulsed electromagnetic fields (PEMF) or low-intensity pulsed ultrasound (LIPUS) bone stimulators may be initiated post-operatively.
- Hardware Prominence: Given the subcutaneous nature of the fifth metatarsal, hardware prominence is common. If symptomatic after fracture healing (usually 6-12 months post-op), removal is indicated. If symptomatic before healing, assess for nonunion, and if present, combine removal with revision fixation.
- Superficial Peroneal Nerve Injury: Prevention is paramount. Careful blunt dissection and identification/retraction of nerve branches are crucial. If a transient neuropraxia occurs, observe and manage symptoms. Persistent or severe symptoms warrant a neurological evaluation and potential consultation with a peripheral nerve specialist.
- Infection: Superficial infections are treated with local wound care and oral antibiotics. Deep infections require aggressive surgical debridement, often involving hardware removal, broad-spectrum IV antibiotics, and potentially a delayed or staged reconstruction.
- CRPS: Early recognition and aggressive multimodal treatment are key to limiting its debilitating effects. This includes physiotherapy, pain medications, sympathetic blocks, and psychological support.
Post-Operative Rehabilitation Protocols
A structured and progressive rehabilitation protocol is essential for optimizing outcomes, restoring function, and facilitating a safe return to sport after surgical fixation of a fifth metatarsal fracture. The protocol generally proceeds in phases, guided by clinical symptoms, radiographic healing, and patient progress.
Phase I: Immediate Post-Operative (Weeks 0-2)
- Goals: Protect surgical repair, minimize pain and swelling, maintain ankle/toe range of motion (ROM).
- Weight-Bearing: Strict non-weight-bearing (NWB) on the operative extremity. Crutches or a knee scooter are used for ambulation.
- Immobilization: Short leg posterior splint or controlled ankle motion (CAM) boot for protection. Keep the foot elevated above heart level.
-
Exercises:
- Non-weight-bearing ankle ROM exercises (dorsiflexion, plantarflexion, inversion, eversion) within pain limits.
- Toe flexion/extension exercises.
- Quadriceps and gluteal isometric exercises for the operative leg.
- Wound Care: Maintain clean, dry dressing. Monitor for signs of infection. Suture/staple removal at 10-14 days.
Phase II: Early Healing & Protected Mobilization (Weeks 2-6)
- Goals: Gradual increase in weight-bearing, restore passive and active ankle/foot ROM, maintain fracture stability.
- Weight-Bearing: Progress from NWB to partial weight-bearing (PWB) in a CAM boot, guided by pain and radiographic signs of early healing. Typically 25% PWB at week 2-3, advancing to 50% PWB by week 4-5.
- Immobilization: Continue CAM boot. May remove for exercises and hygiene.
-
Exercises:
- Continue ankle and toe ROM exercises.
- Gentle calf stretches.
- Theraband exercises for ankle strengthening (dorsiflexion, plantarflexion, inversion, eversion) with minimal resistance.
- Proprioceptive exercises (e.g., single leg balance with support) once 50% PWB is tolerated.
- Stationary cycling with light resistance, NWB initially, then PWB.
Phase III: Advanced Healing & Strengthening (Weeks 6-12)
- Goals: Full weight-bearing, normalize gait pattern, restore full ROM, initiate progressive strengthening and proprioception.
- Weight-Bearing: Progress to full weight-bearing (FWB) out of the CAM boot, typically between 6-8 weeks post-op, assuming clinical and radiographic evidence of adequate healing. May transition to supportive shoes.
-
Exercises:
- Continue and advance ankle/foot strengthening (Theraband, resistance exercises).
- Calf raises (double leg to single leg).
- Balance and proprioception training (wobble board, single-leg stance, functional activities).
- Initiate light impact activities as tolerated (e.g., walking faster, light jogging on soft surfaces), once pain-free FWB is achieved and radiographic healing is confirmed.
- Return to sport-specific drills, initially at low intensity.
Phase IV: Return to Sport / Full Activity (Weeks 12+ or 4-6 months for athletes)
- Goals: Safely return to sport or full activity, achieve pre-injury strength and function, prevent re-injury.
-
Criteria for Return to Sport (RTS):
- Clinical criteria: No pain, full ROM, no tenderness over fracture site.
- Strength criteria: At least 90% strength symmetry compared to the contralateral limb.
- Functional criteria: Able to perform sport-specific activities without pain or compensatory movements. This includes agility drills, jumping, cutting, and running at increasing intensity.
- Radiographic criteria: Definitive evidence of cortical bridging and fracture consolidation.
- Progression: Gradual increase in intensity, duration, and frequency of sport-specific training. A supervised "return to play" protocol is essential, often involving phased progression over several weeks to months.
- Monitoring: Continued monitoring for pain, swelling, or signs of re-injury. Education on appropriate footwear and activity modification.
Important Considerations:
- Individualization: Rehabilitation protocols must be individualized based on the patient's specific fracture type, surgical technique, rate of healing, and activity demands.
- Radiographic Progression: Regular radiographic follow-up (e.g., at 6 weeks, 3 months, 6 months) is crucial to monitor healing and guide weight-bearing progression and return to activity.
- Athlete-Specific Considerations: For high-level athletes, the timeline for full return to competitive play can range from 4 to 6 months, even with optimal surgical fixation, due to the need for complete bone healing and restoration of high-level functional capacity.
- Bone Stimulators: In cases of delayed healing or high-risk patients, the use of a bone stimulator (electrical or ultrasound) may be considered as an adjunct.
Summary of Key Literature / Guidelines
The body of literature on fifth metatarsal fractures, particularly Zone II (Jones) fractures, consistently highlights the challenges associated with their unique anatomy and vascularity, driving consensus on management for athletic populations.
-
Torg et al. (1984, 1987): Landmark studies by Torg and colleagues established the understanding of the vascular compromise in Zone II and the high rates of nonunion with non-operative management, especially in acute and chronic stress fractures. They advocated for intramedullary screw fixation for athletic patients and those with established nonunions, noting superior and more predictable healing rates compared to cast immobilization. Their work categorized Jones fractures and emphasized the importance of aggressive management for athletes.
-
Intramedullary Screw Fixation as Gold Standard for Athletes: Numerous subsequent studies and systematic reviews have reinforced intramedullary screw fixation as the preferred treatment for acute Zone II fractures in athletes.
- Indications: This approach is indicated for acute Jones fractures in athletes and high-demand individuals, as well as for symptomatic delayed union or nonunion. It offers superior union rates (typically >90%), reduced time to union, and earlier return to sport compared to conservative management.
- Screw Size: A critical consensus point is the use of a large-diameter, fully threaded intramedullary screw (typically 4.5 mm to 6.5 mm). Studies by Richli and Rosenthal (1995), Kavanaugh et al. (2009), and others have demonstrated that larger diameter screws (filling at least 70-80% of the medullary canal) provide greater stability and decrease the risk of hardware failure and nonunion. A large diameter screw prevents cyclic shear at the fracture site by inhibiting torsional and bending forces.
- Reaming: While some early techniques involved non-reamed insertion, the current trend often favors limited reaming to allow for larger screw placement and ensure optimal canal fit, enhancing construct stiffness.
-
Non-Operative Management for Non-Athletes: For non-athletic, low-demand individuals with acute, minimally displaced Jones fractures, a trial of non-weight-bearing cast immobilization (typically 6-8 weeks) can be considered. However, patients must be thoroughly counseled on the significant risk of delayed union or nonunion (reported rates up to 50%) and the potential need for subsequent surgery. Close radiographic monitoring is essential. The threshold for surgical intervention should be low if healing is not progressing as expected.
-
Adjunctive Therapies:
- Bone Grafting: For recalcitrant nonunions or revision cases, autologous bone grafting (e.g., calcaneal, iliac crest) is a common adjunct to provide osteoinductive, osteoconductive, and osteogenic properties, thereby enhancing biological healing.
- Bone Stimulators: While evidence is somewhat mixed for acute fractures, non-invasive bone stimulators (pulsed electromagnetic fields or low-intensity pulsed ultrasound) are often considered for delayed unions or in conjunction with revision surgery for nonunions, to promote osteogenesis.
- Biologics (PRP, BMPs): The use of platelet-rich plasma (PRP) or bone morphogenetic proteins (BMPs) as biological adjuncts is emerging but still lacks strong, large-scale evidence for routine use in fifth metatarsal fractures. They are typically reserved for challenging nonunions or as part of experimental protocols.
-
Complications: The literature consistently reports hardware prominence as the most common post-operative complication, often necessitating removal after fracture healing. Delayed union and nonunion, even with surgery, remain a concern, particularly with smaller diameter screws or inadequate immobilization. Nerve injury (superficial peroneal nerve) is a recognized, albeit less frequent, risk requiring meticulous surgical technique.
In conclusion, the current paradigm for managing Zone II fifth metatarsal fractures, especially in the athletic population, strongly favors early intramedullary screw fixation with a large-diameter, fully threaded screw to achieve high union rates, reduce recovery time, and facilitate a safe return to sport. Conservative management, while an option for select low-demand patients, carries a significantly higher risk of complications and prolonged disability. Ongoing research continues to explore optimizing fixation techniques and biological augmentation strategies to further improve outcomes.

