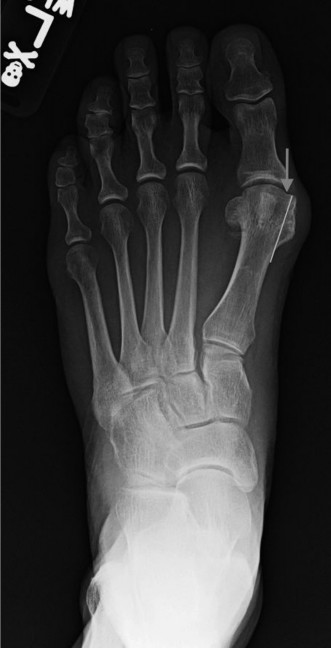
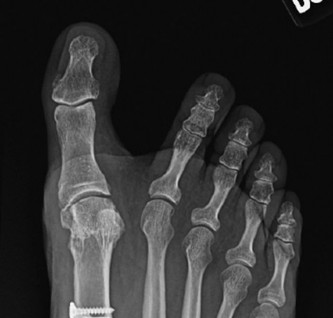
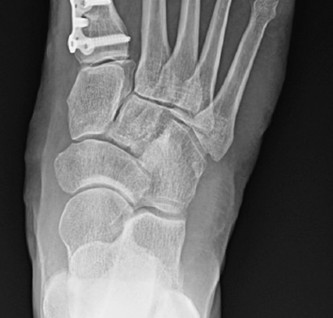
Introduction & Epidemiology
Hallux valgus is a complex, multiplanar deformity of the first ray characterized by lateral deviation of the great toe, medial deviation of the first metatarsal (increased intermetatarsal angle), and often pronation of the first metatarsal. The hallmark clinical finding, the "bunion," represents hypertrophy of the medial aspect of the first metatarsal head and an inflamed medial bursa. While often perceived as a cosmetic issue, hallux valgus is a progressive condition that can lead to significant pain, footwear difficulties, and transfer metatarsalgia.
Epidemiologically, hallux valgus affects a substantial portion of the adult population, with reported prevalence rates ranging from 23% in adults aged 18-65 years to 35.7% in those over 65 years. The etiology is multifactorial, involving genetic predisposition, intrinsic foot biomechanics (e.g., pes planus, hypermobility of the first ray), and extrinsic factors such as shoe wear.
Medial eminence resection, or "bunionectomy," is a fundamental component of nearly all surgical procedures for hallux valgus correction. Historically, simple exostectomy alone was performed (e.g., Silver procedure), but this often led to high rates of recurrence due to failure to address the underlying osseous and soft tissue deformities. Current surgical philosophy emphasizes a comprehensive approach that includes not only removal of the medial eminence but also correction of the intermetatarsal angle, reduction of metatarsal pronation, and balancing of the soft tissues around the first metatarsophalangeal (MTP) joint. The focus of modern techniques, therefore, is on precise and judicious resection of the eminence as part of a multi-component reconstruction to restore normal anatomy and biomechanics, thereby mitigating the risks of postoperative hallux varus and recurrence.
Surgical Anatomy & Biomechanics
A thorough understanding of the anatomical structures and biomechanical principles governing the first MTP joint is paramount for successful hallux valgus correction and complication avoidance.
Osseous Anatomy
- First Metatarsal: The first metatarsal head is crucial, articulating with the proximal phalanx and housing the sesamoid complex plantarly. Its medial aspect commonly hypertrophies to form the medial eminence. The shape of the metatarsal head and the distal metatarsal articular angle (DMAA) are important considerations.
- Proximal Phalanx: The base of the proximal phalanx articulates with the metatarsal head. Its orientation and the presence of any deformity (hallux valgus interphalangeus) must be assessed.
- Sesamoids: Two sesamoid bones, embedded within the flexor hallucis brevis tendon, articulate with the plantar aspect of the first metatarsal head via distinct grooves. In hallux valgus, the sesamoids typically sublux laterally, further accentuating the deformity and acting as a deforming force.
Soft Tissue Anatomy
-
Capsule and Ligaments:
The first MTP joint is enveloped by a joint capsule reinforced by collateral ligaments.
- Medial Collateral Ligament (MCL): Provides medial stability. Its integrity is critical for preventing hallux varus. Over-plication or aggressive tightening of this structure during closure can contribute to varus.
- Lateral Collateral Ligament (LCL): Stretched and attenuated in hallux valgus.
- Deep Transverse Metatarsal Ligament (DTML): Connects the metatarsal heads. It is often taut and contributes to the lateral pull on the great toe.
-
Tendons and Muscles:
- Adductor Hallucis: Consists of oblique and transverse heads, inserting into the lateral aspect of the proximal phalanx. Its contracture is a primary deforming force in hallux valgus, contributing to lateral deviation of the toe and lateral subluxation of the sesamoids.
- Abductor Hallucis: Inserts into the medial aspect of the proximal phalanx. In hallux valgus, it often displaces plantarly, losing its medial pull, or its insertion is stretched.
- Flexor Hallucis Brevis: Envelops the sesamoids. Its medial and lateral heads provide flexion and contribute to toe stability.
- Extensor Hallucis Longus (EHL): Located dorsally, its lateral bowstringing over the first MTP joint contributes to the valgus deformity and can lead to dorsiflexion of the hallux.
- Neurovascular Structures: The dorsomedial cutaneous nerve (branch of the superficial peroneal nerve) and small sensory branches from the medial plantar nerve typically lie superficially on the medial aspect of the foot, vulnerable to injury during incision and dissection.
Biomechanics of Hallux Valgus
The deformity results from a complex interplay of forces:
1.
Medial Deviation of the First Metatarsal:
Leads to an increased intermetatarsal angle (IMA).
2.
Lateral Deviation of the Hallux:
Leads to an increased hallux valgus angle (HVA).
3.
Lateral Subluxation of the Sesamoids:
Disrupts the mechanical advantage of the flexor hallucis brevis.
4.
Pronation of the First Metatarsal:
Rotates the metatarsal head, contributing to the medial eminence prominence and altering joint congruity.
5.
Imbalance of Soft Tissue Forces:
The adductor hallucis and tight lateral capsule/LCL exert a lateralizing force, while the abductor hallucis is often weakened or displaced. The EHL tendon bows laterally.
Medial eminence resection specifically addresses the prominent bony exostosis, alleviating pain and pressure from footwear. However, it does not correct the underlying osseous angles (IMA, HVA) or the soft tissue imbalance. Therefore, for most symptomatic deformities, medial eminence resection must be coupled with other corrective procedures, such as osteotomies (to correct IM angle) and lateral soft tissue release (to release deforming forces) and medial capsular plication (to realign the joint), to achieve stable and lasting correction.
Indications & Contraindications
Indications for Surgical Intervention
Surgical correction of hallux valgus, including medial eminence resection, is primarily indicated for symptomatic deformities that have failed appropriate non-operative management.
-
Pain:
The most common indication. Pain usually arises from:
- Irritation of the medial bunion (bursitis, skin irritation from shoe pressure).
- First MTP joint synovitis.
- Neuroma formation or nerve irritation around the bunion.
- Transfer metatarsalgia (pain under the lesser metatarsal heads due to altered weight-bearing).
-
Functional Limitations:
- Difficulty with shoe wear due to the bunion prominence.
- Limited range of motion (ROM) of the first MTP joint.
- Compromised walking or activity levels.
- Progressive Deformity: Evidence of increasing deformity on serial radiographs, especially in younger patients.
- Unrealistic Expectations of Non-Operative Treatment: After a thorough trial, some patients may desire surgery to prevent further progression or resolve persistent symptoms.
Contraindications for Surgical Intervention
Contraindications can be absolute or relative, depending on patient factors and the specific surgical plan.
- Asymptomatic Deformity: Surgery for cosmetic reasons alone is generally not indicated due to inherent risks.
- Active Infection: In the foot or elsewhere, requires eradication prior to elective surgery.
- Severe Peripheral Vascular Disease: Compromised healing potential.
- Severe Neuropathy (e.g., Charcot arthropathy): Risk of nonunion, recurrence, or further deformity.
- Unrealistic Patient Expectations: Poor understanding of potential outcomes, recovery, or complications.
- Severe Degenerative Arthritis of the First MTP Joint: While not an absolute contraindication, severe arthritis may necessitate alternative procedures such as arthrodesis or arthroplasty, rather than corrective osteotomies.
- Poor Skin Quality/Condition: Active dermatological conditions, ulcers, or very thin skin on the medial foot.
- Acute Gout Attack: In the involved joint.
- Inability to Comply with Post-Operative Protocol: Crucial for successful outcome.
Operative vs. Non-Operative Indications
| Feature | Non-Operative Indications | Operative Indications |
|---|---|---|
| Symptoms | Mild, intermittent pain; no functional limitations. | Persistent, severe pain despite conservative measures. |
| Deformity Severity | Mild, non-progressive deformity; flexible. | Moderate to severe, progressive, or rigid deformity. |
| Shoe Wear | Accommodated with wider shoes, bunion pads. | Significant difficulty finding comfortable shoes; persistent rubbing. |
| Functional Impact | Minimal impact on daily activities or sports. | Significant impact on ambulation, work, or recreational activities. |
| Radiographic | Mild HVA (<20°), mild IMA (<13°), congruent joint. | Moderate to severe HVA (>20°), moderate to severe IMA (>13°), sesamoid subluxation, joint incongruity. |
| Associated Pathology | No significant transfer metatarsalgia. | Significant transfer metatarsalgia, hammer toes, crossover toe. |
| Patient Desire | Prefers non-surgical options; unwilling to accept surgical risks. | Desires surgical correction after understanding risks/benefits; compliant. |
| Trial of Conservative Management | Initial or ongoing successful management. | Failed trial of conservative measures (shoe modifications, orthotics, NSAIDs, physical therapy). |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential for a predictable outcome, minimizing complications such as hallux varus and recurrence.
Clinical Assessment
- History: Elicit detailed information regarding the duration, nature, and severity of symptoms; previous treatments; and functional limitations. Assess shoe wear patterns.
-
Physical Examination:
- Visual Inspection: Assess the severity of the bunion, skin condition, presence of bursitis, and associated deformities (e.g., lesser toe deformities, hammertoes, hallux valgus interphalangeus, pes planus).
- Palpation: Identify areas of tenderness (e.g., medial eminence, MTP joint, plantar plate).
- Range of Motion (ROM): Assess dorsiflexion and plantarflexion of the first MTP joint. Note any limitations, crepitus, or pain indicative of degenerative changes. Assess first ray hypermobility.
- Neurological Exam: Document sensation, particularly along the dorsomedial aspect of the hallux (dorsomedial cutaneous nerve).
- Vascular Exam: Palpate pedal pulses.
- Dynamic Assessment: Observe gait to identify any pronation or compensatory mechanisms.
- Deformity Correctability: Assess whether the hallux valgus deformity is flexible or rigid by attempting to manually correct it. This influences the extent of soft tissue release required.
Radiographic Evaluation
Weight-bearing radiographs are mandatory for comprehensive assessment.
*
Anteroposterior (AP) View:
*
Hallux Valgus Angle (HVA):
Angle between the longitudinal axis of the first metatarsal and the proximal phalanx (normal <15-20°).
*
Intermetatarsal Angle (IMA):
Angle between the longitudinal axes of the first and second metatarsals (normal <9°).
*
Distal Metatarsal Articular Angle (DMAA):
Angle between the articular surface of the first metatarsral head and a line perpendicular to the metatarsal shaft (normal <10°). An increased DMAA (or PASA, Proximal Articular Set Angle) indicates a laterally deviated articular surface, requiring specific corrective osteotomies or considerations during eminence resection to avoid hallux varus.
*
Sesamoid Position:
Graded 0-7, indicating lateral subluxation. Position 0-3 is normal, 4-7 indicates increasing lateral displacement.
*
Joint Congruity:
Assess for subluxation or degenerative changes.
*
Lateral View:
* Evaluates metatarsal elevation or depression.
* Assesses pes planus or cavus foot deformities.
*
Oblique View:
* Provides additional information on joint space and presence of osteophytes.
Pre-Operative Planning Specifics
- Procedure Selection: Based on radiographic angles, joint congruity, and patient factors, determine the appropriate procedure (e.g., isolated medial eminence resection for very mild deformity/pain without significant angulation, distal osteotomy like Chevron/Austin, shaft osteotomy like Scarf/Ludloff, or proximal osteotomy for more severe deformities). The medial eminence resection is a component of these.
- Fixation Choice: Plan for screw fixation, K-wires, or other implants if an osteotomy is performed.
- Template Cuts: Mentally or physically template osteotomy cuts and the extent of eminence resection.
- Discuss Goals and Risks: Clearly communicate the surgical goals, expected outcomes, and potential complications, especially hallux varus and recurrence, to the patient.
Patient Positioning
- Supine Position: The patient is placed supine on the operating table.
- Tourniquet: A thigh or ankle tourniquet is applied to achieve a bloodless field, typically inflated to 250-300 mmHg.
- Foot Prep and Drape: The affected foot and ankle are prepped with an antiseptic solution and draped in a sterile fashion, ensuring adequate exposure of the first ray.
- Surgeon and Assistant Positioning: Surgeon typically sits or stands medial to the foot, assistant opposite.
- Fluoroscopy: Ensure a C-arm fluoroscope is available and positioned for intraoperative imaging, especially if an osteotomy is planned, to confirm cuts and hardware placement.
Detailed Surgical Approach / Technique
The medial eminence resection is a critical step in most hallux valgus correction procedures. Its precise execution, balancing adequate removal with avoidance of over-resection, is paramount to prevent hallux varus and recurrence. This section details the steps, often performed in conjunction with an osteotomy and soft tissue balancing.
1. Incision
-
Medial Longitudinal Incision: The most common approach. A curvilinear incision is made dorsomedially over the bunion prominence, extending from the mid-diaphysis of the first metatarsal to the mid-diaphysis of the proximal phalanx. The incision should be carefully planned to avoid placing the scar directly on the weight-bearing surface or over areas of maximal pressure.
- Rationale: This incision provides excellent exposure of the medial eminence and the first MTP joint.
- Key consideration: Protect the dorsomedial cutaneous nerve, a terminal branch of the superficial peroneal nerve. This nerve typically runs superficially and dorsally to the operative field. Incise cautiously through the skin and subcutaneous tissue, identifying and retracting this nerve dorsally or plantarly to avoid injury.
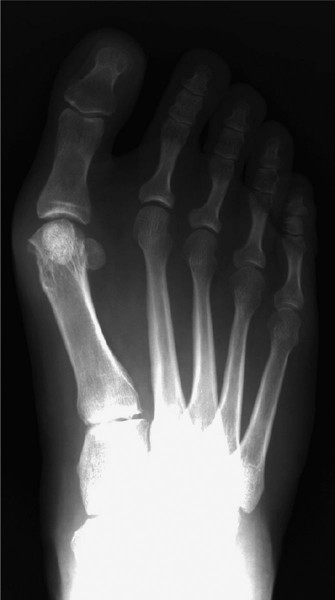
Figure 1: Medial longitudinal incision carefully planned to avoid neurovascular structures.
2. Dissection and Capsulotomy
- Subcutaneous Dissection: Blunt and sharp dissection is used to elevate skin and subcutaneous flaps. The medial bunion bursa, often inflamed and hypertrophied, is excised.
-
Medial Capsulotomy:
An appropriate capsulotomy is performed to expose the medial eminence and the first MTP joint. Common approaches include:
- L-shaped Capsulotomy: A longitudinal incision along the first metatarsal shaft, extending distally, then turning plantarly or dorsally to create a flap.
- Inverted L or T-shaped Capsulotomy: Provides good exposure and allows for subsequent tightening of the medial capsule.
- Rationale: The capsulotomy allows visualization of the metatarsal head and facilitates release of the tight medial capsule and plication during closure.
- Key consideration: Preserve a robust medial capsule and periosteal flap for later repair and potential tightening.
3. Medial Eminence Resection (Bunionectomy)
- Identification of the Eminence: The hypertrophied medial aspect of the first metatarsal head is clearly identified.
-
Resection Plane: This is the most critical step for avoiding hallux varus and recurrence.
- The cut should be made parallel to the medial shaft of the first metatarsal, extending distally.
- The resection should remove the prominent bone but not extend into the sagittal groove where the sesamoids articulate plantarly. Over-resection into this groove destabilizes the sesamoids and significantly increases the risk of hallux varus.
- The cut should ideally be just medial to the articular cartilage of the metatarsal head, preserving the cartilage surface.
- Technique: Use an oscillating saw. A common guideline is to resect the medial eminence flush with the medial cortex of the first metatarsal shaft. Visually inspect the joint after resection to ensure no violation of the plantar articular surface.
- Goal: To remove the bony prominence causing pain and shoe wear issues, while preserving the integrity and stability of the first MTP joint.
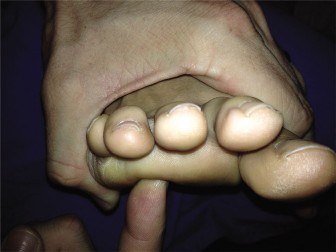
Figure 2: Intraoperative view depicting the medial eminence resection, ensuring the cut is parallel to the metatarsal shaft and avoids the plantar articulation.
Figure 3: Resected medial eminence fragment, demonstrating the size and orientation of the bone removed.
4. Lateral Soft Tissue Release (When Indicated)
For most moderate to severe hallux valgus deformities, medial eminence resection alone is insufficient. Lateral soft tissue release addresses the deforming forces contributing to the valgus and sesamoid subluxation.
*
Technique:
Performed through the same medial incision, or through a separate dorsal incision (less common).
* Access the lateral aspect of the joint by adducting the hallux.
* Release the conjoined adductor hallucis tendon insertion from the lateral aspect of the proximal phalanx and the lateral sesamoid.
* Release the lateral collateral ligament and the lateral aspect of the deep transverse metatarsal ligament (DTML).
*
Key consideration:
Perform this release judiciously. Excessive lateral release, especially without adequate medial stability or osteotomy, can contribute to hallux varus. The goal is to allow correction of the hallux alignment, not to create instability.
5. Metatarsal Osteotomy (If Performed)
Medial eminence resection alone does not correct the underlying metatarsus primus varus (increased IMA) or the valgus angulation of the proximal phalanx. An osteotomy is usually required to correct these angular deformities.
-
Distal Metatarsal Osteotomies (e.g., Chevron, Austin, Reverdin-Green): Used for mild to moderate deformities (IMA < 16-18°).
- A V-shaped or L-shaped cut is made in the metatarsal head or neck.
- The distal fragment (including the metatarsal head and articular surface) is translated laterally to reduce the IMA.
- Rotation can also be incorporated to address metatarsal pronation.
- Fixation is typically with a single screw, K-wire, or absorbable pin.

Figure 4: Intraoperative image demonstrating a distal metatarsal osteotomy (e.g., Chevron) with planned screw fixation. -
Shaft Osteotomies (e.g., Scarf, Ludloff): Used for moderate to severe deformities (IMA > 16-18°).
- These are more powerful corrections, allowing for greater translation, rotation, and plantarflexion/dorsiflexion adjustments.
- Fixation typically involves two screws.
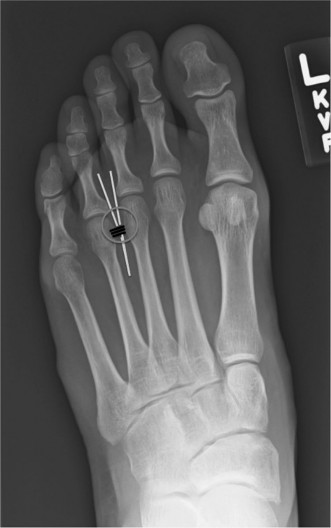
Figure 5: Radiographic depiction of a stabilized osteotomy (e.g., Scarf), demonstrating the correction of the IM angle and use of internal fixation. -
Proximal Metatarsal Osteotomies (e.g., Opening/Closing Wedge): Used for severe deformities or when significant IMA correction is needed.
- Often require plate and screw fixation or staples.
-
Key Consideration: After the osteotomy and translation, ensure the first MTP joint is stable and congruent. The goal is to achieve an HVA of 5-10° and an IMA of <9-10°.
6. Medial Capsular Plication and Closure
-
Medial Capsular Plication:
The medial capsular flap, previously preserved, is imbricated or plicated to tighten the medial capsule and help maintain the corrected alignment of the hallux. This reinforces the medial structures and prevents recurrence.
- Caution: Over-tightening the medial capsule is a common cause of postoperative hallux varus. The repair should be snug but allow for full, unrestricted range of motion of the MTP joint without placing the hallux in a varus position. Test the range of motion and alignment through the full arc of motion.
- Skin Closure: Close the subcutaneous layers and skin with absorbable and non-absorbable sutures, respectively.
-
Dressing: Apply a sterile dressing, often with a soft compression bandage or a specialized bunion dressing (e.g., a "bunionette dressing" or "figure-of-eight" bandage) that supports the corrected position without overcorrection.

Figure 6: Postoperative radiograph demonstrating appropriate alignment after hallux valgus correction, including medial eminence resection and osteotomy, with stable fixation.
Complications & Management
Despite meticulous technique, complications can arise following hallux valgus correction. Understanding their etiology, incidence, and management strategies is crucial.
Common Complications and Salvage Strategies
| Complication | Incidence | Etiology | Clinical Presentation | Management / Salvage Strategy |
|---|---|---|---|---|
| Hallux Varus | 2-10% (can be higher with aggressive techniques) |
- Over-resection of medial eminence
- Over-aggressive lateral soft tissue release - Over-plication of medial capsule - Lateral hardware irritation |
- Medial deviation of hallux, often with dorsiflexion
- Pain over medial joint, lateral aspect of toe - Difficulty with shoe wear - Callosity on lateral aspect of 1st MTP |
-
Conservative:
Taping, splinting (early, mild cases).
- Surgical (early/flexible): Lateral capsular release, medial capsular plication takedown, adductor hallucis transfer. - Surgical (rigid/late): Medial release, lateral augmentation (e.g., EHL tenodesis, abductor hallucis transfer), osteotomies (e.g., opening wedge medial proximal phalanx osteotomy, closing wedge distal metatarsal osteotomy), or 1st MTP fusion in severe cases. |
| Recurrence of Hallux Valgus | 10-25% (varies greatly by technique & patient) |
- Inadequate correction of IMA/HVA
- Inadequate lateral soft tissue release - Unaddressed metatarsal pronation - First ray hypermobility - Early weight-bearing with inadequate fixation |
- Gradual return of bunion prominence
- Lateral deviation of hallux - Pain, shoe wear difficulties |
-
Conservative:
Shoe modifications, orthotics.
- Surgical: Revision surgery (repeat osteotomy if angles are uncorrected, consider more powerful osteotomy, fusion in severe cases, addressing soft tissue imbalance). If due to hypermobility, consider Lapidus procedure. |
| Pain | Common, varying severity |
- Nerve irritation (dorsomedial cutaneous)
- Hardware irritation - Joint stiffness/arthrosis - Transfer metatarsalgia - CRPS |
- Localized pain, numbness, tingling
- Diffuse foot pain - Pain with activity |
-
Nerve:
Neurolysis, nerve blocks, neurectomy (rare).
- Hardware: Removal after healing. - Joint: NSAIDs, physical therapy, intra-articular injections; severe cases may require arthrodesis. - Transfer Metatarsalgia: Orthotics, lesser metatarsal osteotomies. - CRPS: Multidisciplinary pain management. |
| Infection | <1-2% |
- Skin contamination
- Immunocompromised patient - Poor surgical technique |
- Redness, swelling, warmth, pain, purulent discharge, fever |
-
Superficial:
Oral antibiotics, local wound care.
- Deep: Surgical debridement, IV antibiotics, hardware removal (if infected). - Consider culture-directed antibiotics. |
| Delayed Union / Nonunion | 1-5% (osteotomy specific) |
- Inadequate fixation
- Poor bone quality - Smoking - Aggressive early weight-bearing |
- Persistent pain at osteotomy site
- Radiographic lucency or instability |
-
Delayed Union:
Protected weight-bearing, bone stimulator.
- Nonunion: Revision surgery with bone graft, stable fixation, or consider arthrodesis. |
| Avascular Necrosis (AVN) of Metatarsal Head | <1% (higher with distal osteotomies) |
- Disruption of vascular supply to metatarsal head (especially dorsal branch)
- Overly aggressive distal osteotomy/soft tissue release |
- Persistent severe pain
- Radiographic collapse of metatarsal head, sclerosis, joint space narrowing |
-
Early:
Protected weight-bearing, NSAIDs.
- Late: MTP fusion, cheilectomy (for limited necrosis), or hemiarthroplasty/total arthroplasty (less common). |
| Nerve Injury | 2-10% (often transient) | - Laceration or traction injury to dorsomedial cutaneous nerve |
- Numbness, paresthesia on dorsomedial hallux
- Neuroma formation (painful) |
-
Initial:
Observation, nerve protection.
- Persistent: Nerve blocks, physical therapy. - Neuroma: Surgical excision (neurectomy). |
| Stiffness / Limited ROM | 5-15% |
- Excessive capsular scarring
- Over-tightening of soft tissues - Post-op immobilization - Degenerative changes |
- Restricted MTP joint motion (especially dorsiflexion)
- Pain with attempted motion |
- Early mobilization (if appropriate), physical therapy, stretching.
- Severe/Refractory: MUA (Manipulation Under Anesthesia), capsular release, cheilectomy, or fusion in severe cases of arthrosis. |
| Transfer Metatarsalgia | 5-15% |
- Shortening or excessive plantarflexion of first metatarsal (often after aggressive osteotomy)
- Unaddressed intrinsic foot imbalances |
- Pain under lesser metatarsal heads (typically 2nd/3rd)
- Callus formation under lesser metatarsal heads |
- Orthotics with metatarsal pads.
- Surgical: Lesser metatarsal shortening osteotomies, plantar plate repair (if indicated). |
Prevention Strategies
Prevention of these complications begins with meticulous pre-operative planning, precise surgical technique, and appropriate post-operative care:
*
Preventing Hallux Varus:
* Judicious medial eminence resection: Avoid extending the cut into the plantar sesamoid groove.
* Controlled lateral soft tissue release: Release only what is necessary to achieve correction.
* Appropriate medial capsular repair: Avoid over-tightening.
* Correct osteotomy translation and fixation: Ensure proper alignment.
*
Preventing Recurrence:
* Accurate pre-operative assessment of all angular deformities (HVA, IMA, DMAA, sesamoid position).
* Selection of the appropriate osteotomy (distal vs. shaft vs. proximal) to address the magnitude of the IMA.
* Comprehensive soft tissue balancing (lateral release and medial plication).
* Stable fixation of osteotomies.
* Patient adherence to post-operative protocols.
*
Protecting Neurovascular Structures:
Careful dissection, identification, and gentle retraction of the dorsomedial cutaneous nerve.
*
Maintaining Metatarsal Head Viability:
Preserve dorsal vascularity during osteotomy.
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is critical for maximizing surgical outcomes, reducing complications, and facilitating a safe return to activity. Protocols vary depending on the specific procedures performed (e.g., soft tissue vs. osteotomy, type of osteotomy, stability of fixation). The following outlines a general approach, with emphasis on preventing hallux varus and recurrence.
Phase 1: Immediate Post-Operative (Weeks 0-2)
- Goals: Protect surgical site, control pain and swelling, maintain corrected alignment, initiate limited weight-bearing.
-
Weight-Bearing:
- Soft Tissue Procedures (e.g., isolated eminence resection): May allow protected weight-bearing in a post-operative shoe immediately, as tolerated.
- Osteotomies (most common): Protected weight-bearing in a post-operative shoe (e.g., surgical shoe, stiff-soled shoe) with heel-only weight-bearing or partial weight-bearing (PWB) using crutches/walker. Full forefoot weight-bearing is typically restricted.
-
Immobilization:
- Soft dressings are applied in the operating room, often with a "bunion dressing" or taping to maintain toe alignment without overcorrection.
- Hard-soled surgical shoe or boot.
-
Activity:
- Elevation of the foot (above heart level) to minimize swelling.
- Ice application for pain and swelling control.
- Non-weight-bearing exercises for ankle and lesser toes.
- Pain management (analgesics, NSAIDs).
- Wound Care: Keep incision clean and dry. Dressing changes as per surgeon preference. Suture removal typically at 10-14 days.
Phase 2: Early Mobilization & Progressive Weight-Bearing (Weeks 2-6)
- Goals: Gradually increase weight-bearing, restore joint range of motion, maintain alignment, minimize stiffness.
-
Weight-Bearing:
- Progress to PWB or full weight-bearing (FWB) in the post-operative shoe, as tolerated, provided osteotomy fixation is stable (confirmed radiographically if needed).
- Transition to a wider, stiff-soled athletic shoe (e.g., sneaker) may begin towards the end of this phase, often around 4-6 weeks.
-
Range of Motion (ROM):
- Gentle active and passive ROM exercises for the first MTP joint, focusing on dorsiflexion and plantarflexion.
- Caution: Avoid aggressive forced ROM that could disrupt osteotomy healing or overstretch the medial capsule, potentially contributing to recurrence.
- Initiate gentle toe abduction and adduction exercises to encourage muscle balance.
- Strength: Isometric exercises for ankle and foot musculature.
- Manual Therapy: Soft tissue mobilization to address scar tissue.
- Monitoring: Continued monitoring for signs of hallux varus (medial deviation of toe, loss of lateral space) or recurrence (medial prominence, increasing valgus). If varus begins to develop, consider additional taping/splinting to encourage lateral deviation.
Phase 3: Advanced Strengthening & Functional Progression (Weeks 6-12)
- Goals: Restore full joint mobility and strength, improve balance and proprioception, prepare for return to advanced activities.
- Footwear: Gradual transition to regular, comfortable shoes. High heels and pointed-toe shoes are generally discouraged long-term to prevent recurrence.
-
ROM & Strength:
- Continue MTP joint ROM exercises, gradually increasing intensity.
- Progress to resistance exercises for intrinsic foot muscles and ankle stabilizers (e.g., toe curls, towel grabs, calf raises).
- Balance and proprioception exercises (e.g., single-leg stance).
-
Activity:
- Gradual return to light aerobic activities (e.g., walking, cycling).
- Avoid high-impact or pivoting sports until complete healing and strength return.
- Orthotics: Custom or off-the-shelf orthotics may be considered, especially for patients with intrinsic foot imbalances (e.g., pes planus, hypermobility) to provide long-term support and reduce recurrence risk.
Phase 4: Return to Full Activity (Months 3-6+)
- Goals: Full return to desired activities, maintenance of correction.
-
Activity:
- Progressive return to more demanding activities and sports, guided by pain and function.
- Continue strength and conditioning program for foot and ankle.
- Educate patients on proper shoe wear and activity modification to minimize risk of recurrence.
- Long-Term Follow-up: Periodic clinical and radiographic assessment to monitor alignment and identify any signs of recurrence or late complications.
Important Considerations for Preventing Hallux Varus and Recurrence:
- Patient Education: Emphasize the importance of adherence to rehabilitation protocols and footwear recommendations.
- Dynamic Taping/Splinting: If there is any tendency towards hallux varus post-operatively, targeted taping or splinting can be initiated early to guide the toe laterally.
- Gradual Progression: Avoid pushing ROM or weight-bearing too aggressively, especially in the early phases, to protect healing bone and soft tissues.
- Radiographic Monitoring: Obtain post-operative radiographs at regular intervals to confirm correction and assess osteotomy healing.
Summary of Key Literature / Guidelines
The literature on hallux valgus correction is extensive and continues to evolve. Key themes related to "Medial Eminence Resection: Avoiding Hallux Varus & Recurrence" revolve around understanding the multiplanar nature of the deformity, the inadequacy of isolated eminence resection, and the critical role of biomechanical restoration.
1. Inadequacy of Isolated Medial Eminence Resection
- Historical Perspective: Early procedures like the Silver bunionectomy (simple exostectomy) often resulted in high recurrence rates (up to 60-70%) because they addressed only the bony prominence and not the underlying angular deformities (increased IMA, HVA) or soft tissue imbalance.
- Current Consensus: The vast majority of orthopedic surgeons now agree that isolated medial eminence resection is rarely indicated for primary hallux valgus correction, except possibly for very mild deformities with minimal angular deviation and primary pain from the bunion itself. For most symptomatic hallux valgus, a concomitant osteotomy to correct the IMA and HVA, coupled with a lateral soft tissue release and medial capsular plication, is essential.
2. Importance of Comprehensive Deformity Correction
-
Multiplanar Correction:
Modern approaches emphasize correction in all three planes:
- Transverse Plane: Correction of IMA (via metatarsal osteotomy) and HVA (via osteotomy and soft tissue balance).
- Sagittal Plane: Restoration of first metatarsal length and plantarflexion/dorsiflexion, avoiding transfer metatarsalgia.
- Frontal Plane: Addressing pronation of the first metatarsal, which can be achieved with specific osteotomies (e.g., Scarf) or rotational components.
-
Osteotomy Selection:
Guidelines often recommend selecting an osteotomy based on the severity of the IMA:
- Mild (IMA < 13°): Distal osteotomies (Chevron, Austin).
- Moderate (IMA 13-16°): Chevron, Scarf, or Ludloff osteotomy.
- Severe (IMA > 16-18°): Proximal metatarsal osteotomies (e.g., crescentic, opening/closing wedge) or the Lapidus procedure (first TMT arthrodesis), especially in cases of first ray hypermobility.
3. Preventing Hallux Varus
-
Etiology:
The literature consistently identifies several risk factors for hallux varus:
- Over-resection of the Medial Eminence: Particularly extending into the plantar articular surface, destabilizing the sesamoids.
- Aggressive Lateral Soft Tissue Release: Excessive release of the adductor hallucis and lateral capsule.
- Over-tightening of the Medial Capsule: During imbrication.
- Overcorrection of the Hallux Valgus Angle: Post-osteotomy.
-
Prevention Strategies:
Key recommendations from studies include:
- Precise Bunionectomy: Resecting only the prominent medial aspect, parallel to the metatarsal shaft, preserving the sesamoid groove.
- Judicious Lateral Release: Performed only to the extent necessary to allow correction.
- Balanced Capsular Repair: Ensuring the medial capsule is tightened appropriately without overcorrection.
- Maintaining Metatarsal Head Vascularity: Crucial during distal osteotomies to prevent AVN, which can secondarily lead to joint collapse and alignment issues.
4. Preventing Recurrence
- Comprehensive Correction: The most critical factor in preventing recurrence is to address all components of the deformity.
- Adequate IMA Correction: Failure to achieve sufficient reduction of the intermetatarsal angle is a primary cause of recurrence.
- Addressing First Ray Hypermobility: For patients with significant first ray hypermobility, a Lapidus procedure (proximal metatarsal-cuneiform arthrodesis) is often recommended to stabilize the first ray and prevent recurrence.
- Patient Compliance: Adherence to post-operative protocols, including protected weight-bearing and appropriate footwear, plays a significant role in long-term success.
5. Outcomes and Evidence-Based Practice
- Meta-analyses and Systematic Reviews: Demonstrate generally favorable outcomes for various bunion correction techniques, with high patient satisfaction rates (70-90%).
- Comparison of Techniques: No single procedure has been universally declared superior for all types of hallux valgus. The choice of procedure should be individualized based on the patient's deformity, anatomy, and surgeon's experience.
- Long-Term Follow-up: Studies indicate that while initial correction can be excellent, some degree of recurrence or loss of correction can occur over many years, underscoring the importance of comprehensive planning and execution.
In conclusion, medial eminence resection is an essential, but never isolated, component of hallux valgus correction. The academic literature and clinical guidelines strongly advocate for a holistic approach that combines precise bone resection with appropriate osteotomies and soft tissue balancing to achieve stable, long-lasting correction while meticulously guarding against the pitfalls of hallux varus and recurrence.
Clinical & Radiographic Imaging