Introduction & Epidemiology
Instability of the second metatarsophalangeal (MTP) joint is a common and often debilitating forefoot pathology, characterized by pain, progressive deformity, and functional impairment. It represents a spectrum of conditions ranging from subtle synovitis and capsulitis to frank dorsal subluxation or dislocation, predominantly affecting the second toe. While various MTP joints can be affected, the second MTPJ is particularly susceptible due to its unique anatomical and biomechanical stresses.
Epidemiologically, second MTPJ instability is most frequently observed in middle-aged women, although it can affect individuals of any age or gender. Its prevalence is underestimated due to misdiagnosis or late presentation. Common etiologies include:
*
Biomechanical overload:
A long second metatarsal (Morton's toe), hallux valgus deformity (leading to transfer metatarsalgia), pes planovalgus, or an elevated first ray can cause excessive pressure on the second metatarsal head.
*
Trauma:
Acute or repetitive microtrauma to the plantar plate or collateral ligaments.
*
Inflammatory arthritis:
Rheumatoid arthritis or other seronegative spondyloarthropathies can cause capsular and ligamentous attenuation.
*
Iatrogenic:
Over-aggressive first ray surgery can lead to transfer load.
*
Degenerative changes:
Age-related wear and tear of the joint structures.
If left untreated, second MTPJ instability can lead to progressive dorsal subluxation, hammer toe or claw toe deformity, intractable plantar keratosis beneath the metatarsal head, and chronic pain, significantly impacting patient mobility and quality of life. Understanding its complex etiology and pathomechanics is crucial for effective management.
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate anatomy and biomechanics of the second MTPJ is paramount for accurate diagnosis and successful surgical intervention. The joint is a diarthrodial articulation designed for both stability and flexibility, crucial for propulsion during gait.
Osseous Anatomy
The second MTP joint consists of the convex head of the second metatarsal articulating with the concave base of the second proximal phalanx. The metatarsal head is somewhat flattened plantarly to accommodate the plantar plate. The alignment of the metatarsals, particularly the length of the second metatarsal relative to the first (often longer, known as Morton's toe), plays a critical role in load distribution across the forefoot. Dorsal subluxation of the phalanx on the metatarsal head is the hallmark of instability.
Capsuloligamentous Structures
The primary static stabilizers of the MTP joint include the plantar plate, collateral ligaments, and the joint capsule.
- Plantar Plate: This fibrocartilaginous structure is the most critical stabilizer of the MTP joint, resisting hyperextension and dorsal subluxation. It is a distal extension of the joint capsule, originating from the distal metatarsal neck via strong collagen fibers. Distally, it inserts firmly into the base of the proximal phalanx. Laterally, it blends with the proper and accessory collateral ligaments. The plantar plate provides a stable fulcrum for the intrinsic muscles and protects the metatarsal head from direct ground pressure. Tears most commonly occur at its proximal attachment to the metatarsal neck due to repetitive tensile and shear forces.
- Collateral Ligaments: The proper collateral ligaments run from the metatarsal head to the base of the proximal phalanx, providing medial and lateral stability. The accessory collateral ligaments extend from the metatarsal head to the plantar plate. These ligaments work in concert to restrict varus and valgus motion at the MTPJ.
- Joint Capsule: Surrounds the joint, blending dorsally with the extensor hood and plantar plate, and medially/laterally with the collateral ligaments. The dorsal capsule is thinner and less robust than the plantar structures.
Dynamic Stabilizers
The intrinsic foot muscles provide dynamic stability and control MTPJ motion:
*
Lumbricals:
The four lumbrical muscles originate from the flexor digitorum longus tendons. They pass plantar to the deep transverse metatarsal ligament (DTML) and insert into the medial aspect of the extensor hood of their respective toes. Their primary action is MTPJ flexion and interphalangeal (IP) joint extension. The second lumbrical, in particular, contributes to second MTPJ stability by pulling the toe into flexion.
*
Interossei:
The dorsal and plantar interossei muscles originate from the metatarsal shafts and insert into the bases of the proximal phalanges and extensor hoods. They assist with MTPJ flexion and abduction/adduction of the toes.
Biomechanics of Instability
The pathomechanism of second MTPJ instability often begins with repetitive overloading of the metatarsal head, particularly in individuals with a long second metatarsal or those with hallux valgus where load is transferred laterally. This chronic stress can lead to inflammation, attenuation, and eventually tearing of the plantar plate at its weakest point – the proximal insertion into the metatarsal neck.
Once the plantar plate is compromised, the intrinsic muscles (lumbricals and interossei) lose their stable fulcrum, and the extensor digitorum longus (EDL) tendon's pull becomes unopposed dorsally. This leads to progressive dorsal subluxation of the proximal phalanx, loss of MTPJ flexion, and compensatory hyperextension at the proximal interphalangeal (PIP) joint, resulting in a classic "claw toe" or "hammer toe" deformity. The plantar fat pad, normally beneath the metatarsal head, also displaces distally, contributing to increased pressure and pain under the metatarsal head.
Indications & Contraindications
Indications for Operative Intervention
Surgical management of second MTPJ instability is considered when conservative measures have failed to alleviate symptoms, or when there is significant structural deformity and functional impairment.
*
Persistent pain and dysfunction:
Despite an adequate course of non-operative treatment (e.g., orthotics, activity modification, anti-inflammatory medications, taping, shoe wear modifications), the patient continues to experience debilitating pain, limiting daily activities.
*
Irreducible dorsal subluxation or dislocation:
Clinical assessment reveals a fixed or severely subluxed/dislocated MTP joint that cannot be manually reduced, indicating significant capsuloligamentous compromise.
*
Progressive deformity:
Development or progression of a hammer toe/claw toe deformity directly attributable to MTPJ instability, causing pressure points, painful callosities, and shoe-fitting difficulties.
*
Documented plantar plate tear:
Imaging studies, particularly MRI, demonstrate a significant plantar plate tear (Grade 2 or 3) with clinical correlation of instability.
*
Functional limitation:
The instability causes significant gait disturbance, difficulty weight-bearing, or inability to participate in desired activities.
*
Failure of prior surgical intervention:
For cases of recurrent instability after previous MTPJ surgery, where revision is deemed appropriate.
Contraindications for Operative Intervention
Absolute and relative contraindications must be carefully considered to optimize patient outcomes and minimize risks.
*
Active local or systemic infection:
Surgery is deferred until infection is completely resolved.
*
Severe peripheral vascular disease:
Compromised blood supply can impair wound healing and increase complication rates.
*
Uncontrolled systemic inflammatory disease:
Conditions like poorly controlled rheumatoid arthritis may lead to poor soft tissue healing and recurrence.
*
Severe uncontrolled diabetes mellitus:
High risk of infection, wound healing complications, and neuropathy.
*
Severe osteopenia/osteoporosis:
May compromise fixation and increase risk of fracture or non-union with osteotomies.
*
Poor skin condition:
Prior radiation, severe dermatological conditions, or fragile skin over the surgical site.
*
Patient non-compliance:
Inability or unwillingness to adhere to post-operative weight-bearing restrictions, rehabilitation protocols, or activity modifications.
*
Mild, reducible deformities:
Cases that respond well to conservative management or have minimal symptoms.
*
Patient preference:
When the patient explicitly declines surgical intervention after thorough discussion of risks and benefits.
Operative vs. Non-Operative Indications
| Indication Category | Operative Intervention | Non-Operative Management |
|---|---|---|
| Pain & Dysfunction | Persistent, debilitating pain despite conservative care; significant functional limitation. | Mild to moderate pain, responsive to activity modification and analgesia; minimal functional impact. |
| Deformity | Irreducible dorsal subluxation/dislocation; progressive hammer/claw toe deformity. | Reducible subluxation; early stages of deformity; no painful callosities. |
| Plantar Plate Integrity | MRI-confirmed Grade 2-3 tear with clinical instability. | Mild plantar plate attenuation or synovitis without clear tear; Grade 1 tears. |
| Metatarsal Length | Significant second metatarsal protrusion with transfer metatarsalgia. | No significant metatarsal length discrepancy or transfer loading. |
| Conservative Failure | Failed comprehensive non-operative protocol (minimum 3-6 months). | Symptoms controlled with orthotics, taping, shoe modifications, physical therapy. |
| Comorbidities | Medically fit, good vascular status, controlled systemic conditions. | Significant comorbidities that preclude surgery; poor wound healing potential. |
Pre-Operative Planning & Patient Positioning
Careful pre-operative planning is critical for optimizing outcomes in second MTPJ instability. This involves thorough patient evaluation, appropriate imaging, and meticulous surgical preparation.
Clinical Assessment
- History: Detailed history of pain (location, character, exacerbating/alleviating factors), duration of symptoms, prior treatments, and impact on activity. Inquire about shoe-wear difficulties, callosities, and associated deformities (e.g., bunions).
-
Physical Examination:
- Observation: Assess for dorsal subluxation, hammer toe/claw toe deformity, splaying of the toes, plantar callosities under the second metatarsal head, and overall foot alignment (e.g., pes planovalgus).
- Palpation: Localize tenderness at the MTPJ, metatarsal head, or plantar plate.
- Range of Motion: Assess passive and active MTPJ motion. Note any stiffness or hypermobility.
-
Stability Testing:
- Lachman Test (Vertical Stress Test): While stabilizing the metatarsal head, apply dorsal pressure to the proximal phalanx. Increased dorsal translation compared to adjacent toes or the contralateral foot indicates plantar plate insufficiency.
- Drawer Test: Hold the metatarsal head and attempt to sublux the proximal phalanx dorsally and plantarly.
- Dynamic Assessment: Observe toe position during weight-bearing and gait.
- Neurovascular Status: Evaluate sensation and vascularity, particularly digital nerves.
Imaging
-
Weight-Bearing Radiographs:
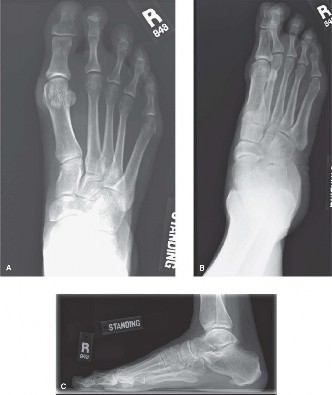
Standard anteroposterior (AP), lateral, and oblique views are essential.
- AP View: Assess MTPJ alignment, splaying of toes, presence of hallux valgus, metatarsal length pattern (e.g., long second metatarsal). A common indicator of instability is loss of parallelism between the second and third metatarsals.
- Lateral View: Crucial for identifying dorsal subluxation of the proximal phalanx relative to the metatarsal head. Also assesses overall arch structure.
- Oblique View: Provides additional visualization of osseous structures.
- Magnetic Resonance Imaging (MRI): The gold standard for assessing soft tissue structures, particularly the plantar plate. MRI can directly visualize plantar plate tears (most commonly at the metatarsal neck insertion), synovitis, and bone marrow edema.
- Ultrasound: Can be used dynamically to assess instability and visualize plantar plate tears, but it is highly operator-dependent.
Anesthesia
Regional anesthesia (e.g., ankle block or popliteal block) is often combined with general anesthesia to provide excellent post-operative pain control. General anesthesia ensures patient comfort and surgical field stillness.
Patient Positioning
The patient is positioned supine on the operating table.
* The operative foot is placed on a padded footboard or suspended in a foot holder to allow full range of motion during surgical manipulation.
* A thigh tourniquet (pneumatic) is applied to maintain a bloodless field. An ankle tourniquet can also be used for shorter procedures.
* The entire limb is prepped and draped in a sterile fashion from the knee or mid-calf distally.
Detailed Surgical Approach / Technique
Surgical correction of second MTPJ instability aims to restore anatomical alignment, stabilize the joint by repairing or reconstructing the plantar plate, and address any underlying biomechanical factors. The most common approach involves a dorsal incision, often combined with a shortening osteotomy of the metatarsal.
General Principles
The core objectives are:
1. Achieve stable reduction of the MTP joint.
2. Repair or reconstruct the compromised plantar plate.
3. Address contributing factors such as an excessively long metatarsal or toe deformity.
4. Minimize morbidity and facilitate early rehabilitation.
Incision
A
dorsal longitudinal incision
directly over the second MTP joint is the most widely adopted approach.
*
Technique:
A 3-4 cm incision is made, centered over the second MTP joint, extending slightly proximally over the metatarsal shaft and distally over the proximal phalanx.
*
Advantages:
Provides direct access to the joint capsule, collateral ligaments, and extensor mechanism; generally good healing; less risk of creating a painful plantar scar.
*
Disadvantages:
Requires indirect access to the plantar plate, potentially requiring MTPJ distraction or subluxation for visualization; risk of damage to dorsal digital nerves and veins.
This image depicts the typical dorsal approach to the MTP joint, highlighting relevant anatomical structures and potential areas for capsular incision or plantar plate repair.
Dissection & Internervous Planes
- Skin and Subcutaneous Tissue: Incise the skin and subcutaneous tissue. Meticulously identify and protect the dorsal digital nerves (medial and lateral branches of the second common digital nerve) and veins, retracting them safely.
- Extensor Tendon and Hood: The extensor digitorum longus (EDL) tendon to the second toe is identified. A longitudinal incision is made through the extensor hood, either medial or lateral to the EDL tendon, or by splitting the hood longitudinally and retracting the tendon. This exposes the joint capsule.
- Capsulotomy: Perform a dorsal longitudinal capsulotomy. The joint is then inspected. At this stage, the MTP joint is often dorsally subluxated or dislocated, and hypertrophic synovium may be present.
Evaluation and Repair of the Plantar Plate
- Visualization: To adequately visualize the plantar plate, the MTP joint often needs to be further dislocated dorsally. A Hohmann retractor or narrow laminar spreader can be used to distract the joint, creating a gap between the metatarsal head and proximal phalanx. The use of a small dental mirror or endoscope may also aid visualization.
- Assessment: Carefully inspect the plantar plate. Tears most commonly occur at its proximal attachment to the metatarsal neck. The tear may be complete or partial, acute or chronic, and the tissue quality assessed.
- Debridement: Debride any hypertrophic synovium or frayed edges of the plantar plate to promote healing.
-
Repair:
- Direct Repair: If the tissue quality is good and the tear is fresh, direct repair is performed. Non-absorbable sutures (e.g., 2-0 or 3-0) are passed through the distal edge of the torn plantar plate. These sutures are then passed through drill holes created in the plantar aspect of the metatarsal neck (often 2-3 drill holes, 1.0 mm diameter). The sutures are tied dorsally, securing the plantar plate back to its anatomical origin. Suture anchors (e.g., micro-anchors) can also be used, placed into the metatarsal head/neck from a dorsal or dorsolateral approach, with sutures then passed through the plantar plate.
- Reconstruction/Augmentation: In cases of chronic, attenuated, or severely retracted plantar plate tears where direct repair is not feasible, reconstruction using a local tissue flap (e.g., extensor sling) or an allograft/autograft may be considered. However, this is less common for primary second MTPJ instability and often combined with other procedures.
Adjunct Procedures
Addressing associated biomechanical factors is crucial for successful and durable correction.
*
Weil Osteotomy (Shortening Metatarsal Osteotomy):
This is frequently performed concurrently, especially if the second metatarsal is long or there is significant dorsal subluxation.
*
Technique:
A transverse osteotomy is made through the metatarsal neck, typically with a dorsal-to-plantar trajectory, ensuring the plantar cortex is cut last to prevent plantar sag. A precise amount of bone is resected (e.g., 2-4 mm) to shorten the metatarsal and elevate the metatarsal head, thereby decompressing the MTP joint and facilitating plantar plate repair. The osteotomy is then fixed with one or two headless compression screws or a standard cortical screw.
*
Purpose:
Decompresses the MTP joint, allows easier reduction, reduces load on the metatarsal head, and can correct sagittal plane deformity.
*
Extensor Lengthening:
If a significant fixed claw toe deformity exists, the extensor digitorum longus tendon may be lengthened (Z-plasty or tenotomy) to correct the MTPJ hyperextension and improve toe alignment.
*
Proximal Interphalangeal (PIP) Joint Fusion/Arthroplasty:
For severe, fixed PIP joint contractures (hammer toe/claw toe), a PIP joint fusion (arthrodesis) or excisional arthroplasty may be necessary to straighten the toe.
*
Capsular Release:
If significant dorsal contracture of the MTP joint capsule limits reduction, a dorsal capsulotomy may be extended.
*
Gastrocnemius Recession/Achilles Lengthening:
For concomitant equinus deformity, which can increase forefoot pressure.
Reduction & Fixation
- MTPJ Reduction: Once the plantar plate is repaired and any osteotomies are fixed, the MTP joint is reduced.
- Temporary K-wire Fixation: To protect the repair and maintain reduction, especially after a Weil osteotomy, a 0.045" or 0.062" K-wire is commonly placed longitudinally across the MTP joint and into the metatarsal shaft. The toe is positioned in slight plantarflexion. This K-wire is usually left in place for 4-6 weeks.
Closure
The tourniquet is deflated, and hemostasis is achieved. The extensor hood is repaired, followed by meticulous layered closure of the subcutaneous tissue and skin using absorbable and non-absorbable sutures, respectively. A sterile dressing and a soft compressive wrap are applied, followed by a post-operative surgical shoe.
Complications & Management
Despite meticulous surgical technique, complications can arise following second MTPJ instability repair. Proactive identification and appropriate management are crucial for salvage and optimizing long-term outcomes.
General Complications
-
Infection:
Superficial or deep surgical site infection. Incidence is low (<1%).
- Management: Oral or intravenous antibiotics, debridement, hardware removal if necessary.
-
Nerve Injury:
Damage to dorsal digital nerves, leading to numbness, paresthesias, or painful neuroma.
- Management: Conservative (neuropathic pain medications), nerve block, or surgical neurolysis/neurectomy in severe cases.
-
Wound Healing Issues:
Delayed healing, dehiscence, or excessive scarring.
- Management: Local wound care, débridement, or plastic surgery consultation.
-
Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE):
Rare but serious.
- Management: Prophylactic measures (early mobilization, chemical prophylaxis for high-risk patients), anticoagulation.
Specific Complications and Management
| Complication | Incidence | Description | Salvage Strategy |
|---|---|---|---|
| Recurrence of Deformity/Instability | 10-20% | Persistent or recurrent dorsal subluxation or claw toe deformity. Often due to inadequate repair, continued biomechanical stressors (e.g., unaddressed long metatarsal), or premature return to activity. | Revision surgery: Re-evaluation of underlying biomechanics. May involve revision plantar plate repair/reconstruction, further metatarsal shortening osteotomy (e.g., revision Weil), or if joint integrity is severely compromised, MTPJ fusion (arthrodesis) as a salvage procedure. Orthotic intervention to offload the forefoot. |
| Stiffness / Limited Range of Motion | 5-15% | Restricted MTPJ motion, particularly dorsiflexion, leading to difficulty with shoe wear and gait. Can be due to prolonged immobilization, capsular adhesions, or overtightening of repairs. | Aggressive physical therapy: Early and sustained range-of-motion exercises, passive stretching. Manipulation under anesthesia: For recalcitrant stiffness. Surgical capsular release: If conservative measures fail, arthroscopic or open capsulotomy. |
| Persistent/Transfer Metatarsalgia | 5-10% | Pain beneath the operated metatarsal head (if inadequate shortening or insufficient plantar plate repair) or beneath an adjacent metatarsal head (transfer metatarsalgia), typically the third metatarsal, due to over-shortening of the second metatarsal (Weil osteotomy). | Conservative management: Custom orthotics with metatarsal pads. Revision Weil osteotomy: If the original shortening was inadequate. Adjacent metatarsal osteotomy: If transfer metatarsalgia is severe and persistent (e.g., third metatarsal Weil osteotomy). |
| Hardware Complications | 5-10% | Screw prominence (from Weil osteotomy), K-wire migration, fracture, or infection. Can cause pain, skin irritation, or soft tissue inflammation. | Hardware removal: Typically performed once bony union is achieved or if symptoms are severe. For K-wires, early removal if migration or infection occurs. |
| Malunion/Nonunion of Osteotomy | <1% | Poor healing of the Weil osteotomy, leading to persistent pain, deformity, or structural weakness. | Conservative: Protected weight-bearing, bone stimulation. Revision surgery: With bone grafting and revised fixation. |
| Complex Regional Pain Syndrome (CRPS) | <1% | A rare but severe post-operative pain condition characterized by disproportionate pain, swelling, skin changes, and autonomic dysfunction. | Multidisciplinary approach: Aggressive pain management, physical therapy, sympathetic blocks, psychological support. Early diagnosis and intervention are key. |
| Overcorrection (Flexion deformity) | Rare | Toe fixed in excessive plantarflexion, potentially impinging on adjacent toes or footwear. More common with aggressive flexor tendon transfers or overly aggressive plantar plate reefing. | Physical therapy: Stretching and mobilization. Revision surgery: Lengthening of shortened soft tissues or revision of flexor tendon transfer. |
Post-Operative Rehabilitation Protocols
A structured and progressive rehabilitation protocol is essential for optimizing the long-term success of second MTPJ instability repair, promoting healing, restoring function, and preventing recurrence. The protocol will vary slightly depending on the specific surgical procedures performed (e.g., plantar plate repair alone vs. with Weil osteotomy and K-wire fixation).
Phase 1: Immediate Post-Operative Protection (Weeks 0-2)
- Weight-Bearing: Strictly non-weight-bearing (NWB) on the operative foot.
- Immobilization: Foot protected in a post-operative surgical shoe or CAM walker boot. A soft compressive dressing is applied to minimize swelling.
-
Activity:
- Elevation of the foot above heart level to reduce swelling.
- Ice application (20 minutes on, 20 minutes off) multiple times a day.
- Gentle active range of motion (AROM) exercises of the ankle and non-operative toes to prevent stiffness and reduce DVT risk.
- Avoid any active or passive motion of the operated MTP joint or toe.
- Pain Management: Prescribed analgesics.
- Wound Care: Keep incision clean and dry. Dressing changes as instructed.
Phase 2: Early Mobilization and Protected Weight-Bearing (Weeks 2-6)
- Weight-Bearing: Progress to protected weight-bearing (PWB) in a rigid sole surgical shoe or CAM walker boot, gradually increasing as tolerated. If a Weil osteotomy was performed, a heel-weight-bearing gait is encouraged initially.
- K-wire Removal: If a K-wire was used for temporary fixation, it is typically removed at 4-6 weeks post-operatively, after radiographic confirmation of initial osteotomy healing (if applicable).
-
Activity:
- Begin gentle passive and then active range of motion exercises for the operated MTP joint, focusing on plantarflexion and extension without stressing the repair.
- Gentle toe flexion/extension exercises.
- Scar massage once the incision is well-healed to prevent adhesions.
- Continue ankle range of motion exercises.
- Light stationary cycling (without toe engagement) may be introduced, depending on surgeon preference.
- Footwear: Continue surgical shoe/boot.
Phase 3: Progressive Strengthening & Return to Activity (Weeks 6-12)
- Weight-Bearing: Transition from the surgical shoe/boot to a supportive, wide-toe box athletic shoe or comfortable shoe with a rigid sole. Custom orthotics with a metatarsal pad are often prescribed to offload the second metatarsal head.
-
Activity:
- Strengthening: Introduce progressive strengthening exercises for intrinsic foot muscles (e.g., towel scrunches, marble pickups), calf raises, and balance exercises.
- Range of Motion: Continue MTPJ range of motion exercises, aiming for full, pain-free motion.
- Gait Training: Focus on normal gait mechanics.
- Low-Impact Aerobics: Stationary bike, elliptical, swimming can be resumed.
- Avoid high-impact activities or running.
- Driving: May resume if the operative foot is not the driving foot and pain control is adequate.
Phase 4: Advanced Strengthening & Return to Sport (Months 3-6+)
-
Activity:
- Advanced Strengthening: Progress to more dynamic strengthening, agility drills, and sport-specific training.
- Impact Activities: Gradual reintroduction of higher impact activities, jogging, and running, often starting with short intervals. Close monitoring for pain or recurrence is crucial.
- Footwear: Continue supportive footwear and custom orthotics.
- Full Recovery: Full return to sport or unrestricted activities typically occurs between 3 to 6 months, but can take up to a year for complete resolution of symptoms and full strength restoration. Patient education regarding realistic expectations and the importance of long-term foot care is paramount.
Summary of Key Literature / Guidelines
The understanding and management of second MTPJ instability have evolved significantly, particularly with the recognition of the plantar plate's critical role. A review of the literature highlights several key principles and evidence-based practices.
1. Etiology and Diagnosis:
Early literature often focused on MTPJ synovitis or capsulitis, but advancements in imaging, especially
MRI
, have confirmed the high prevalence of
plantar plate tears
as the primary pathology. Studies by investigators such as Coughlin and Shurnas (2003) were instrumental in characterizing the clinical presentation and diagnostic utility of the vertical stress test (Lachman test). The strong correlation between clinical instability, radiographic dorsal subluxation, and MRI-confirmed plantar plate pathology is well-established. Weight-bearing radiographs remain essential for assessing metatarsal length discrepancies and overall forefoot alignment, which are often predisposing factors.
2. Non-Operative Management:
The initial treatment for second MTPJ instability is universally conservative. Guidelines typically recommend a trial of non-operative management for at least 3-6 months. This includes activity modification, shoe wear modifications (e.g., rigid sole shoes, rocker bottom soles), custom orthotics with metatarsal pads or digital strapping, and anti-inflammatory medications. While non-operative measures can alleviate symptoms in early stages or mild cases, they often fail to address the underlying structural instability in advanced cases.
3. Surgical Techniques and Outcomes:
*
Plantar Plate Repair:
The literature strongly supports direct repair of the plantar plate for symptomatic instability. The
dorsal approach
is the most common, offering good visualization of the joint and allowing for concomitant procedures. While technically challenging for plantar plate access, methods involving metatarsal head distraction or temporary dorsal dislocation of the MTPJ have improved success rates. Studies by investigators like Deland (2005) and Doty et al. (2014) have described various dorsal repair techniques, often utilizing drill holes in the metatarsal head or suture anchors.
*
Weil Osteotomy:
Concomitant
Weil osteotomy
of the second metatarsal is frequently performed, especially in cases with a long second metatarsal or significant dorsal subluxation. It serves to shorten the metatarsal, decompress the MTPJ, and facilitate plantar plate repair. Numerous studies have shown that combining a Weil osteotomy with plantar plate repair improves outcomes, reduces recurrence rates, and addresses metatarsalgia. However, careful consideration of the amount of shortening is necessary to avoid transfer metatarsalgia to adjacent rays.
*
Other Adjunct Procedures:
Lengthening of the extensor digitorum longus tendon or PIP joint fusion/arthroplasty for rigid hammer/claw toe deformities are also well-documented adjuncts that contribute to overall toe alignment and functional improvement.
*
Comparative Studies:
While head-to-head comparisons of different plantar plate repair techniques (e.g., direct vs. suture anchor) are limited, current consensus favors robust fixation that allows for early, protected motion. The long-term outcomes of successful plantar plate repair combined with appropriate adjunct procedures show high patient satisfaction, significant pain reduction, and functional improvement, with recurrence rates ranging from 10-20%.
4. Complications:
The literature consistently reports persistent metatarsalgia (often transfer metatarsalgia from over-shortening), stiffness, and recurrence of deformity as the most common complications. Careful pre-operative planning, precise surgical technique (particularly regarding metatarsal shortening), and adherence to post-operative rehabilitation protocols are highlighted as critical factors in minimizing these risks.
5. Future Directions:
Ongoing research focuses on refining minimally invasive techniques for plantar plate repair, investigating the use of biologic augmentation (e.g., PRP), and developing improved methods for objective functional assessment. However, current evidence continues to emphasize the importance of comprehensive open repair with concomitant osteotomy when indicated.
In summary, current academic guidelines for second MTPJ instability advocate for a systematic approach: conservative management for initial presentations, followed by surgical intervention for failed conservative care, particularly when characterized by persistent pain, irreducible subluxation, progressive deformity, and confirmed plantar plate pathology. The most common and successful surgical strategy involves direct plantar plate repair, often augmented by a Weil osteotomy to address metatarsal length and offload the joint.
