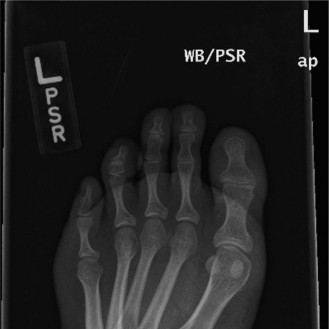
Patient Presentation & History
A 42-year-old male, previously fit and active with no significant medical comorbidities or pertinent past surgical history, presented to the emergency department following a fall from a height of approximately 4 meters. The patient reported landing directly on his feet. He experienced immediate, severe pain and deformity in his right ankle, rendering him unable to bear weight. There was no reported loss of consciousness or other systemic injuries. He denied any neurovascular symptoms distal to the ankle at the scene, though increasing swelling was noted. Smoking history was negative.
Clinical Examination
Upon initial assessment, the patient was hemodynamically stable. Local examination of the right ankle revealed gross deformity with significant swelling and ecchymosis, consistent with a high-energy injury. The skin over the anteromedial aspect of the ankle was severely distended, blanched, and showed impending tenting, with a developing blister laterally. There was no obvious open wound, but the skin appeared compromised (Tscherne C2-C3).
- Inspection: Marked ankle swelling, ecchymosis extending proximally and distally. Anterior skin tension with a tense soft tissue envelope. Absence of a "wrinkle sign" suggesting significant compartment swelling. Palpable bony prominence medially.
- Palpation: Diffuse tenderness throughout the ankle joint and distal tibia. Marked tenderness over the anterior compartment. Crepitus was elicited with gentle manipulation. Peripheral pulses (dorsalis pedis and posterior tibial) were palpable, albeit diminished due to swelling, and capillary refill was brisk (<2 seconds). Sensation to light touch was intact in all major dermatomes (superficial peroneal, deep peroneal, sural, saphenous, plantar nerves).
- Range of Motion (ROM): Actively and passively, ankle dorsiflexion, plantarflexion, inversion, and eversion were severely restricted and exquisitely painful. Due to pain and swelling, a comprehensive assessment of individual muscle strength was challenging, but the patient could weakly attempt dorsiflexion against gravity, indicating some initial function of the anterior tibialis. The strength of the anterior tibialis was estimated at 3/5, with significant guarding. Other muscle groups were similarly affected by pain.
- Neurological/Vascular Assessment: Distal pulses were initially present but required careful monitoring. The deep peroneal nerve function was clinically intact, confirmed by sensory discrimination between the first and second toes and weak, painful active dorsiflexion. Gross examination revealed no signs of acute compartment syndrome, but the tense soft tissue envelope warranted close observation.
Imaging & Diagnostics
Initial radiographic assessment was performed in the emergency department.
-
Plain Radiographs: AP, lateral, and mortise views of the right ankle demonstrated a highly comminuted intra-articular fracture of the distal tibia (pilon fracture), extending into the tibial plafond. Significant articular depression and metaphyseal comminution were evident. There was associated fibular fracture approximately 5 cm proximal to the ankle joint and lateral talar subluxation. The overall pattern was consistent with a high-energy axial load injury. The mortise appeared widened, suggesting syndesmotic disruption.
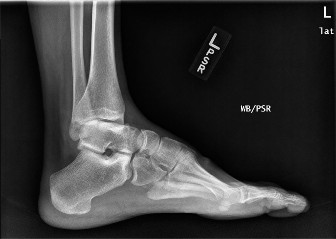
Figure 1: Initial AP radiograph demonstrating a highly comminuted intra-articular fracture of the distal tibia (pilon fracture) with significant articular depression and talar subluxation. -
Computed Tomography (CT) Scan: Following stabilization and preliminary assessment, a CT scan of the ankle was obtained to delineate the extent of articular involvement, fragment displacement, and comminution for pre-operative planning. The CT confirmed an OTA/AO 43-C3 pilon fracture with extensive articular depression and displacement, involving the entire plafond. Significant comminution of the anterior and posterior tibial metaphysis was noted, with distinct posteromedial and anterolateral fragments. The syndesmosis was disrupted, and the fibular fracture was further characterized. The CT provided crucial information regarding the exact number and size of articular fragments, allowing for a detailed reduction strategy.

Figure 2: Coronal CT reconstruction illustrating the severe articular comminution and depression of the tibial plafond, consistent with an OTA/AO 43-C3 pilon fracture. -
No MRI was indicated acutely given the clear bony pathology and the need for urgent intervention. If chronic ligamentous instability or specific tendon pathology were suspected post-operatively or in a delayed setting, MRI might be considered.
-
Templating: Based on the CT images, a comprehensive templating strategy was formulated. This involved outlining the planned approaches, screw trajectories, and plate positions. Specific attention was given to identifying the main articular fragments, especially the posteromedial (Volkmann's) and anterolateral (Chaput/Tillaux) fragments, which are crucial for anatomical reduction. The integrity of the anterior tibialis tendon and muscle was noted to be grossly intact on CT, with no overt evidence of rupture or significant intramuscular hematoma within the anterior compartment, which was a positive prognostic sign for future dorsiflexion capabilities.
Differential Diagnosis
The acute presentation strongly suggests a pilon fracture, however, other high-energy ankle and foot injuries can present similarly. A careful differential diagnosis is crucial for comprehensive management.
| Feature | Pilon Fracture (e.g., OTA 43-C3) | Complex Ankle Fracture-Dislocation (e.g., Lauge-Hansen SER IV) | Talus Fracture (Body/Neck) |
|---|---|---|---|
| Mechanism of Injury | High-energy axial load (fall from height, MVA with foot on brake). | High-energy rotational or combined rotational/axial forces. | High-energy axial load with forced dorsiflexion/plantarflexion. |
| Clinical Presentation | Severe pain, gross deformity, marked swelling, often severe soft tissue compromise (blanching, tenting, blistering). | Severe pain, marked deformity, significant swelling, potential neurovascular compromise. | Severe pain, deformity, often less severe swelling acutely than pilon, but can progress. |
| Primary Location of Injury | Distal tibial metaphysis and intra-articular plafond. | Tibia, fibula, and talus (malleoli, syndesmosis, talar subluxation/dislocation). | Talus (body, neck, head), often associated with subtalar or ankle joint dislocation. |
| X-ray Findings | Tibial plafond comminution, articular depression, metaphyseal extension. Often associated fibular fracture, talar subluxation. | Fractures of medial/lateral malleoli, posterior malleolus, syndesmotic disruption. Talar shift/dislocation. | Fracture line through talar body or neck, often associated with subtalar or ankle dislocation. Avulsion fractures possible. |
| CT Scan Findings | Detailed articular mapping, fragment analysis (Volkmann's, Chaput), extent of comminution, syndesmosis, fibula fracture. | Precise definition of malleolar fractures, syndesmosis, associated ligamentous injuries, talar position. | Exact fracture configuration, displacement, subtalar involvement, osteochondral lesions. |
| Relevance of Anterior Tibialis | Crucial. Assessed for integrity post-trauma; essential for functional dorsiflexion and preventing equinus post-op. Its preservation is a major positive prognostic indicator. | Important for dorsiflexion function; may be compromised by severe displacement or compartment syndrome in anterior compartment. | Its integrity is less directly threatened than in pilon fractures, but function is impaired by pain and swelling. |
| Surgical Management | Often staged (external fixator -> ORIF). Focus on articular reduction, restoration of mechanical axis, stable fixation. | ORIF of malleoli, syndesmotic fixation. Focus on anatomical reduction and stability. | ORIF if displaced, often complex due to vascularity of talus and multiple facets. |
| Key Complications | Post-traumatic arthritis, non-union/malunion, infection, soft tissue necrosis, equinus deformity. | Post-traumatic arthritis, instability, non-union, infection. | Avascular necrosis of talus, post-traumatic arthritis, non-union, malunion. |
Surgical Decision Making & Classification
Given the high-energy nature of the injury, the severe comminution, and critically, the compromised soft tissue envelope (Tscherne C2-C3), a staged surgical approach was deemed essential. Immediate open reduction and internal fixation (ORIF) would significantly increase the risk of wound complications, including necrosis and infection, due to the acute swelling and tissue damage.
Decision for Operative Management:
The intra-articular nature, significant displacement, and instability of the pilon fracture (OTA/AO 43-C3) necessitated surgical intervention to restore articular congruity, alignment, and stability. Non-operative management would inevitably lead to severe post-traumatic arthritis, malunion, and functional disability.
Classification Utilized:
*
AO/OTA Classification:
43-C3. This signifies a complex articular and metaphyseal fracture of the distal tibia, representing the highest severity.
*
Ruedi-Allgower Classification:
Type III (highly comminuted with impaction and joint surface destruction). This classification further emphasizes the severity of the articular injury.
*
Tscherne Classification:
C2-C3 for soft tissue injury. This guided the decision for staged management, prioritizing soft tissue recovery before definitive fixation.
Rationale for Staged Approach:
1.
Soft Tissue Optimization:
The primary goal of the initial stage was to stabilize the fracture and allow the soft tissue envelope to recover. This involves reducing swelling, resolving fracture blisters, and improving skin viability, thereby minimizing the risk of wound complications.
2.
External Fixation:
An ankle-spanning external fixator was applied acutely in the emergency department. This provided immediate provisional stability, indirectly reduced the fracture (ligamentotaxis), and helped to restore ankle length and alignment. This decompressed the compromised soft tissues and facilitated nursing care.
3.
Timing of Definitive ORIF:
The definitive ORIF was planned after a period of 7-10 days, or when the "wrinkle sign" returned and the soft tissues were deemed amenable to surgery.
Consideration of a Strong Anterior Tibialis:
The assessment of the anterior tibialis muscle function was paramount throughout this decision-making process. While acutely compromised by pain and swelling, the initial presence of weak active dorsiflexion was a positive indicator. A strong anterior tibialis provides:
*
Dynamic Stability:
Helps stabilize the ankle joint and prevent equinus deformity.
*
Gait Improvement:
Essential for a normal heel-to-toe gait pattern.
*
Rehabilitation Potential:
Its intactness allows for earlier and more effective active dorsiflexion exercises, crucial for preventing arthrofibrosis and promoting functional recovery.
*
Reduced Need for Future Procedures:
If the anterior tibialis were non-functional or severely compromised, complex tendon transfers or even ankle fusion might be considered in the long term, especially if significant equinus developed. The initial assessment confirmed its general structural integrity and potential for recovery.
Surgical Technique / Intervention
Stage 1: Acute External Fixation
Within hours of presentation, the patient underwent application of an ankle-spanning external fixator under regional anesthesia.
*
Patient Positioning:
Supine on a radiolucent table.
*
Approach:
Standard external fixator pin placement. Two pins were placed in the anterior shaft of the tibia, approximately 10-15 cm proximal to the ankle joint, avoiding neurovascular structures. Two additional pins were placed in the talar neck/body or calcaneus, ensuring clear passage through bone.
*
Reduction:
Gentle traction was applied to the foot to achieve initial reduction of the talar subluxation and restoration of ankle length via ligamentotaxis. The ankle was held in a neutral position.
*
Construct:
A sturdy uniplanar or delta frame was assembled and secured.
*
Post-op:
The ankle was dressed, and continuous elevation with regular ice application was initiated.
Stage 2: Definitive Open Reduction Internal Fixation (ORIF)
Seven days later, with the soft tissues significantly improved (return of the wrinkle sign, resolution of most blistering), the patient underwent definitive ORIF.
- Patient Positioning: Supine on a radiolucent table, with a bump under the ipsilateral hip. A high thigh tourniquet was applied.
-
Approaches:
- Lateral Fibula Approach: A longitudinal incision was made over the distal fibula. The fibula was anatomically reduced and fixed with a one-third tubular plate and cortical screws. This step restores the lateral column length and rotation, providing a guide for subsequent tibial reduction.
- Anterolateral Approach: A second incision, longitudinal, was made between the anterior tibialis tendon and the superficial peroneal nerve. This incision allowed access to the lateral aspect of the tibial plafond, the Chaput fragment (anterolateral fragment), and the syndesmosis. The anterior tibialis tendon was gently retracted medially. This approach also facilitated visualization of the anterior portion of the joint.
- Anteromedial Approach: A third longitudinal incision was made between the anterior tibialis tendon and the medial malleolus, often more medial, to access the medial plafond and provide working space for articular reduction. Care was taken to protect the saphenous nerve and vein. The anterior tibialis tendon was again retracted laterally from this approach. The intactness and resilience of the anterior tibialis muscle-tendon unit were crucial here; careful retraction without excessive tension minimized risk of iatrogenic injury.
-
Reduction Techniques:
- Fibula Fixation: As described above, restoring length and rotation.
- Articular Reduction: This was the most challenging step. The external fixator was removed. Initial reduction of the main articular fragments was achieved using a combination of direct manipulation, small fragment clamps, and impaction grafting (if necessary) for subchondral defects. A critical step involved identifying and reducing the posteromedial and anterolateral fragments, often using joy-sticking K-wires. The intra-articular fragments were reduced under direct visualization and image intensification.
- Metaphyseal Reconstruction: Once the articular surface was restored, the metaphyseal bone was reduced to the articular block. This often involved indirect reduction techniques via traction and carefully placed periarticular clamps.
-
Fixation Construct:
- Articular Screws: Small fragment lag screws (2.7mm or 3.5mm) were placed across the articular fragments to achieve absolute stability. These screws were countersunk and their trajectories carefully planned to avoid impingement in the joint.
- Periarticular Plates: Low-profile periarticular plates (e.g., locking anterolateral and anteromedial plates) were applied to buttress the articular fragments and provide stable fixation to the tibial metaphysis and diaphysis. The plates were contoured to the complex anatomy of the distal tibia. Bi-cortical screws were used in the diaphyseal segment, and locking screws in the metaphyseal/epiphyseal regions.
-
Syndesmotic Fixation:
Given the fibular fracture and confirmed syndesmotic disruption on pre-op imaging and intra-op stress testing, a 3.5mm tricortical syndesmotic screw was placed approximately 2 cm proximal to the plafond, after ensuring anatomical reduction of the syndesmosis.
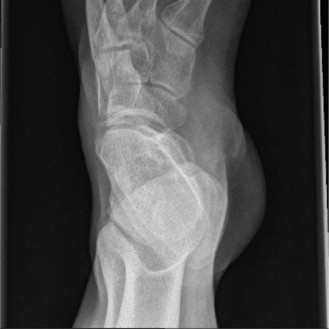
Figure 3: Post-operative AP radiograph showing stable open reduction and internal fixation of the pilon fracture with a lateral fibula plate and periarticular plating of the distal tibia, along with syndesmotic fixation. Note the restored articular congruity and overall alignment.
-
Wound Closure: Meticulous layered closure was performed, paying careful attention to avoiding tension on the skin edges. A sterile dressing was applied.
Post-Operative Protocol & Rehabilitation
The post-operative protocol was designed to protect the reduction and fixation, promote soft tissue healing, and gradually restore function, with particular emphasis on leveraging the function of the anterior tibialis.
-
Initial Post-Operative Period (Weeks 0-2):
- Immobilization: Short leg splint or controlled ankle motion (CAM) boot, non-weight bearing (NWB) for the first 6-8 weeks.
- Elevation: Strict elevation of the limb to minimize swelling.
- Pain Management: Multimodal analgesia.
- Wound Care: Daily dressing changes; monitor for signs of infection or skin necrosis.
- Early ROM: Gentle active range of motion (AROM) of the toes and knee. Avoid active ankle ROM initially to protect fixation.
-
Early Rehabilitation (Weeks 2-6):
- Mobilization: Transition to a removable CAM boot.
- Non-Weight Bearing: Continue NWB.
- Active Ankle Dorsiflexion: Begin gentle, active ankle dorsiflexion exercises, specifically engaging the anterior tibialis. The goal is to prevent equinus contracture and promote muscle activation without stressing the fracture site.
- Active Plantarflexion/Inversion/Eversion: Begin gentle active ROM as pain allows.
- Soft Tissue Mobilization: Gentle massage around incision sites once wounds are healed to prevent scar adherence and improve tissue pliability.
-
Progressive Rehabilitation (Weeks 6-12):
- Radiographic Assessment: Obtain follow-up radiographs to assess fracture healing.
- Weight Bearing: If radiographs show adequate signs of union and fixation remains stable, initiate protected partial weight-bearing (PWB) in the CAM boot, gradually progressing to full weight-bearing (FWB) over several weeks, guided by pain and tolerance.
- Intensified Physiotherapy: Focus on strengthening of the anterior tibialis and other ankle musculature, improving ankle proprioception, and regaining full range of motion.
- Gait Training: Progression from assistive devices (crutches/walker) to independent ambulation.
-
Advanced Rehabilitation (Weeks 12+):
- Transition to Shoe: Progress from CAM boot to supportive shoe.
- Functional Training: Return to sport-specific or activity-specific training. Continued strengthening, balance, and proprioception exercises.
- Addressing Residual Deficits: Any residual stiffness or weakness, particularly in dorsiflexion, will be rigorously addressed. The preserved strength of the anterior tibialis is crucial here, as it provides the primary engine for dorsiflexion, mitigating the risk of a persistent equinus deformity common after severe pilon fractures.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Soft Tissue Management is Paramount: For high-energy ankle fractures, especially pilon fractures, the soft tissue envelope dictates the timing and success of surgery. A staged approach (external fixation followed by delayed ORIF) is often the safest and most effective strategy, reducing wound complications significantly. The "wrinkle sign" is your best friend.
- Anatomical Articular Reduction: This is the cornerstone of pilon fracture management. Prioritize restoring the articular surface congruity, even at the expense of perfect metaphyseal alignment initially. Use small fragments, joystick K-wires, and often a direct approach to reduce the main articular fragments (e.g., posteromedial, anterolateral).
- Restore Fibular Length and Rotation First: Fixing the fibula provides a critical template for restoring the overall length and rotation of the lower limb, aiding in subsequent tibial reduction.
-
Leverage a Strong Anterior Tibialis:
A well-functioning anterior tibialis is a significant asset in these complex ankle injuries.
- Assessment: Always meticulously assess its function pre- and intra-operatively. Its strength and intactness post-trauma are positive prognostic indicators.
- Rehabilitation: Actively engage the anterior tibialis early in rehabilitation (when safe) to prevent equinus contracture, improve dorsiflexion range, and facilitate gait mechanics. Its strength allows for better functional outcomes and reduces the likelihood of requiring future tendon balancing procedures.
- Surgical Planning: When planning anterior approaches, be mindful of the anterior tibialis tendon. Gentle retraction, rather than aggressive pulling, is key to preserving its integrity and function.
- Stable Fixation: Use a combination of lag screws for articular fragments and buttress/locking plates for metaphyseal support. Ensure absolute stability for articular fragments and relative stability for metaphyseal comminution if indirect reduction is employed.
- Syndesmotic Assessment: Always assess the syndesmosis intra-operatively after fibular and tibial fixation. Fix if unstable.
- Early Mobilization of Uninvolved Joints: Keep the knee, hip, and toes moving to prevent stiffness and deep vein thrombosis.
Pitfalls
- Rushing to ORIF: Operating on a "hot" ankle with severe soft tissue swelling and impending skin necrosis is a recipe for disaster (infection, wound dehiscis, skin loss). Adhere strictly to the staged approach.
- Inadequate Articular Reduction: Failure to achieve anatomical reduction of the articular surface will almost inevitably lead to symptomatic post-traumatic osteoarthritis, even with stable fixation. This is the primary long-term complication.
- Ignoring the Fibula: Failure to restore fibular length and rotation can lead to malreduction of the tibia, malunion, and chronic ankle instability or impingement.
- Compartment Syndrome: The anterior compartment, where the anterior tibialis resides, is particularly susceptible to compartment syndrome in high-energy ankle and pilon fractures. Maintain a high index of suspicion, especially with increasing pain, sensory deficits (deep peroneal nerve), and pain on passive dorsiflexion. Prompt fasciotomy is critical if suspected.
- Nerve and Vascular Injury: Be vigilant for iatrogenic injury to neurovascular structures, especially the superficial peroneal nerve with lateral approaches and the saphenous nerve/vein with medial approaches. The anterior tibial artery and deep peroneal nerve are at risk with anterior approaches if not carefully identified and protected.
- Non-Union/Malunion: Inadequate fixation or premature weight-bearing can lead to non-union or malunion, necessitating revision surgery. Malunion, particularly rotational, can be debilitating.
- Post-Traumatic Arthritis: Despite optimal surgical management, the high-energy nature and intra-articular damage frequently lead to some degree of post-traumatic arthritis. Patient counseling regarding this potential outcome is crucial.
- Chronic Equinus Deformity: If the anterior tibialis muscle function is compromised or not adequately rehabilitated, patients can develop a fixed equinus deformity, severely impacting gait and function. This underscores the importance of the "strong anterior tibialis" theme.
Clinical & Radiographic Imaging