Introduction & Epidemiology
Chronic Achilles tendon rupture represents a significant clinical challenge, distinct from acute ruptures in its pathology, treatment complexity, and often, prognosis. While acute ruptures are generally amenable to direct repair, chronic ruptures, defined typically as those presenting more than 4-6 weeks after injury, are characterized by substantial tendon gap formation, significant scar tissue, tendon retraction, and muscle atrophy. These factors preclude primary end-to-end repair without excessive tension, necessitating reconstructive techniques to bridge the defect and restore the functional integrity of the triceps surae complex.
The incidence of Achilles tendon ruptures has been reported to be increasing, particularly among middle-aged "weekend warriors" participating in recreational sports. While the majority present acutely, a notable percentage of ruptures are either initially misdiagnosed, neglected, or suffer re-rupture after initial treatment, leading to a chronic presentation. Such chronic cases result in persistent pain, weakness in plantarflexion, inability to perform a single heel raise, and significant functional disability.
Reconstructive options for chronic Achilles ruptures range from local tendon transfers (e.g., gastrocnemius-soleus V-Y advancement) to synthetic grafts or allografts. However, for large defects exceeding 3-6 cm, autologous tendon transfer, specifically the Flexor Hallucis Longus (FHL) tendon, has emerged as a gold standard. The FHL offers several advantages: it is a strong, expendable tendon, anatomically proximal to the Achilles insertion, and its harvest typically results in minimal functional deficit due to synergistic action with the Flexor Digitorum Longus (FDL). This extensive review will delve into the surgical considerations, detailed technique, and evidence supporting FHL transfer for the management of chronic Achilles rupture.
Surgical Anatomy & Biomechanics
A thorough understanding of the regional anatomy is paramount for successful FHL transfer.
Achilles Tendon
The Achilles tendon, the strongest and thickest tendon in the human body, is formed by the confluence of the gastrocnemius and soleus muscles (triceps surae). It inserts onto the posterior aspect of the calcaneal tuberosity. The tendon typically undergoes a 90-degree twist, with fibers from the medial gastrocnemius rotating laterally and those from the lateral gastrocnemius rotating medially before insertion. This anatomical twist is important as it influences biomechanics and potential rerupture patterns.
- Blood Supply: The Achilles tendon has a relatively poor blood supply, particularly in its watershed zone (2-6 cm proximal to its insertion), which is considered a common site for rupture. Vascularization is primarily derived from the posterior tibial artery through the paratenon and to a lesser extent from the peroneal artery.
- Innervation: Motor innervation to the gastrocnemius and soleus is provided by the tibial nerve (S1, S2). Sensory innervation around the tendon is predominantly from the sural nerve, which runs superficially along the lateral border of the Achilles tendon. Iatrogenic injury to the sural nerve is a common complication during surgical approaches to the Achilles.
Flexor Hallucis Longus (FHL) Tendon
The FHL muscle originates from the posterior surface of the fibula and interosseous membrane. Its tendon is robust, providing strong plantarflexion of the hallux and contributing to ankle plantarflexion.
- Course: The FHL tendon runs in a groove on the posterior aspect of the talus, then courses beneath the sustentaculum tali (medial to the FDL tendon and neurovascular bundle) before passing into the foot to insert on the plantar aspect of the distal phalanx of the great toe.
- Relationship to Neurovascular Structures: In the posterior compartment of the leg, the FHL lies deep to the FDL and tibialis posterior tendons. It is immediately lateral to the posterior tibial artery and tibial nerve, which travel within the tarsal tunnel. When harvesting the FHL proximally, care must be taken to protect these structures.
-
Knot of Henry (Chiasma Plantare):
This crucial anatomical structure is an tendinous intersection located in the midfoot/hindfoot where the FHL tendon typically passes dorsal to the FDL tendon, exchanging a slip of tendon with the FDL. Distal to this chiasm, the FHL runs deep to the FDL, contributing to toe flexion and arch support.
Surgically, the Knot of Henry is important because it represents the point distal to which the FHL can be harvested without causing significant functional deficit to the lesser toes, as the FDL can compensate for FHL function at this junction.
Harvesting the FHL proximal to the Knot of Henry requires careful dissection to separate it from the FDL, and leaves the great toe dependent on the FDL slip for flexion, potentially leading to a mild, often well-compensated, loss of isolated great toe flexion strength. For Achilles reconstruction, the FHL is typically harvested proximal to the Knot of Henry to obtain maximal tendon length for transfer.
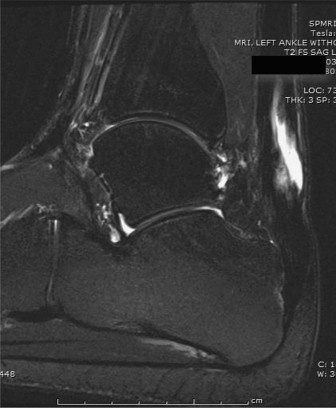
Figure 1: Illustration of the deep posterior compartment, highlighting the FHL tendon's course relative to the neurovascular bundle and its relationship with the FDL.
Biomechanics of FHL Transfer
The FHL muscle-tendon unit contributes significantly to ankle plantarflexion, albeit less than the Achilles. Transferring the FHL to augment a chronic Achilles rupture leverages its synergistic function with the triceps surae. Post-transfer, the FHL assists in plantarflexion, bridging the gap, and providing a durable biological augmentation. The goal is to restore not only strength but also the endurance and dynamic capabilities of the ankle plantarflexors. Studies have shown that while some loss of isolated great toe flexion strength may occur, overall functional outcomes are excellent due to compensation from the FDL and the relatively minor contribution of FHL to isolated great toe motion compared to its role in general foot mechanics.
Indications & Contraindications
The decision for operative versus non-operative management of chronic Achilles ruptures, and specifically the choice of FHL transfer, hinges on several factors including patient activity level, extent of the defect, and overall health.
Indications for Operative Intervention (FHL Transfer)
- Chronic rupture: Defined as presenting >4-6 weeks after injury, particularly with functional deficit.
- Large tendon gap: Defects typically >3 cm that cannot be closed primarily without excessive tension.
- Failed conservative management: Persistent pain, weakness, or functional limitation despite appropriate non-operative treatment.
- Failed primary repair: Re-rupture after initial surgical intervention.
- Active individual: Patients with high functional demands who desire to return to pre-injury activity levels, including sports.
- Significant weakness: Inability to perform a single leg heel rise.
Contraindications for Operative Intervention
- Active infection: Local or systemic.
- Severe peripheral vascular disease: Compromised healing potential.
- Severe peripheral neuropathy: Risk of neurotrophic ulceration and impaired healing.
- Poor skin quality: Significant scarring, ulceration, or previous failed surgery that compromises skin integrity.
- Non-ambulatory or low-demand patient: For whom the risks of surgery may outweigh the benefits. Non-operative management with bracing and rehabilitation might be more appropriate.
- Unrealistic patient expectations.
- Inability to comply with post-operative rehabilitation protocol.
Summary of Operative vs. Non-Operative Indications
| Feature | Non-Operative Management | Operative Management (FHL Transfer) |
|---|---|---|
| Rupture Type | Acute rupture (often small gap), low demand chronic | Chronic rupture (>4-6 weeks), re-rupture |
| Tendon Gap | Small (e.g., <2-3 cm) in acute or low demand chronic | Large (>3-6 cm), inability to approximate ends without tension |
| Patient Activity Level | Sedentary, low-demand, elderly, significant comorbidities | Active, high-demand, desire to return to sports/strenuous activity |
| Functional Impairment | Mild pain, minimal weakness, able to cope functionally | Significant pain, inability to perform single heel rise, marked weakness |
| Comorbidities | Multiple, high surgical risk (diabetes, PVD, smoking) | Few, acceptable surgical risk |
| Compliance | Able to adhere to brace protocol | Able to adhere to rigorous post-operative rehabilitation |
| Skin Conditions | Intact, healthy | Significant skin scarring, poor vascularity (caution, may require flaps) |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial for optimizing outcomes in chronic Achilles rupture reconstruction with FHL transfer.
Pre-Operative Planning
- Clinical Assessment: A thorough history and physical examination are essential. Assess the patient's functional demands, current limitations, and expectations. Palpate the Achilles tendon defect, evaluate plantarflexion strength, and assess the integrity of the great toe flexion to anticipate FHL harvest.
-
Imaging:
- MRI (Magnetic Resonance Imaging): This is the gold standard for evaluating chronic Achilles ruptures. MRI accurately depicts the extent of the gap, the quality of the remaining tendon stumps (e.g., degenerative changes, scarring), and the degree of muscle retraction and atrophy within the gastrocnemius-soleus complex. Crucially, MRI also allows for assessment of the FHL tendon itself, ensuring its integrity and ruling out pre-existing pathology.
- Ultrasound: Can provide dynamic assessment of the tendon gap and retraction, but is operator-dependent.
- X-rays: Primarily used to rule out calcaneal avulsion fractures or other osseous pathology, but do not directly visualize soft tissue.
- Surgical Approach Selection: Determine the primary incision for Achilles exposure (typically posterior) and the secondary incision for FHL harvest (often medial longitudinal or through the primary posterior incision if extended).
- Informed Consent: Discuss the risks and benefits of FHL transfer, including potential donor site morbidity (e.g., great toe weakness, stiffness), sural nerve injury, infection, and re-rupture.
Patient Positioning
- Prone Position: The patient is typically positioned prone on the operating table. This allows excellent access to the posterior aspect of the leg and ankle for both Achilles exposure and FHL harvest.
- Bolsters: Place bolsters or a specialized leg roll under the ankles to allow the feet to hang free in slight plantarflexion. This helps relax the gastrocnemius-soleus complex, reducing tension on the Achilles tendon.
- Tourniquet: A thigh tourniquet is applied and inflated after exsanguination of the limb to provide a bloodless field, which is critical for meticulous dissection and identification of neurovascular structures.
- Padding: Ensure all pressure points are adequately padded to prevent nerve palsies (e.g., peroneal nerve at the fibular head) or skin breakdown.
- Preparation and Draping: The limb is prepped and draped from the knee to the toes in a sterile fashion, allowing for visualization and manipulation of both the hindfoot and great toe.
Detailed Surgical Approach / Technique
The surgical technique for FHL transfer for chronic Achilles rupture involves several precise steps, focusing on adequate exposure, meticulous debridement, careful FHL harvest, and robust reconstruction.
1. Incision and Exposure of the Achilles Tendon
-
Incision:
A longitudinal incision is typically made along the medial border of the Achilles tendon, extending from approximately 10-15 cm proximal to the calcaneal insertion down to the calcaneus. A medial incision is preferred over a central posterior incision to minimize the risk of damage to the sural nerve, which lies laterally, and to improve soft tissue coverage over the repair. Some surgeons advocate for an extensile posterior incision if significant exposure for FHL harvest is also anticipated through the same wound.
- Alternative: A more posterior midline incision can also be used, but necessitates careful identification and protection of the sural nerve.
-
Dissection:
Dissect sharply through the skin and subcutaneous tissue. Identify and carefully protect the sural nerve and lesser saphenous vein, which typically lie superficially along the lateral aspect of the incision. The paratenon is incised longitudinally to expose the ruptured Achilles tendon.

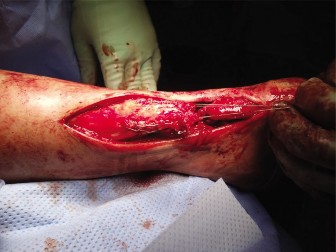
Figure 2: Intraoperative view showing exposure of a chronic Achilles rupture, with identification of the retracted tendon ends and surrounding scar tissue. - Debridement: Excise all non-viable, scarred, and degenerate tissue from the proximal and distal tendon stumps. This is crucial for promoting healing of the repair. The remaining viable tendon ends are identified, which often reveal a significant gap. The plantaris tendon, if present, can be excised or used as an adjunct for repair.
2. Preparation of the Achilles Tendon Bed and Calcaneal Tunnels
- Tendon Gap Assessment: Once debrided, the actual defect size is measured. Attempt to gently bring the tendon ends together to assess the residual tension. For chronic ruptures with significant retraction, this often highlights the need for augmentation.
- Calcaneal Tunnel Creation: Two or three parallel bone tunnels (e.g., 3.2-4.5 mm diameter) are drilled from posterior to anterior through the calcaneus, exiting on the plantar aspect. These tunnels should be positioned approximately 1.5-2 cm proximal to the Achilles insertion, maintaining a robust bone bridge between them. A curved awl or suture passer is then used to pass heavy non-absorbable sutures (e.g., FiberWire, Ethibond) from the plantar foot, through the calcaneal tunnels, and exiting posteriorly. These will be used to secure the transferred FHL tendon.
3. Harvest of the Flexor Hallucis Longus (FHL) Tendon
- Approach: The FHL tendon can be harvested through the primary Achilles incision by dissecting deeper and medially, or through a separate small medial longitudinal incision in the hindfoot/midfoot. The posterior approach through the Achilles incision offers direct access.
- Identification: Retract the medial skin and fat. Identify the FHL tendon lying deep to the FDL tendon, adjacent to the posterior tibial artery and tibial nerve. The FHL is typically the largest and most lateral of the three deep posterior compartment tendons (Tibialis Posterior, FDL, FHL) at the ankle level. It has a distinctive robust, somewhat flattened appearance.
- Tenotomy: Carefully dissect the FHL tendon free from its surrounding sheath and any adhesions. Isolate the tendon for a sufficient length (typically 10-15 cm or more, depending on the defect size). Using a small incision over the great toe MTP joint, the FHL tendon can be identified and secured distally. It is then released as far distally as possible, taking care to preserve the integrity of the Knot of Henry (Chiasma plantare) if possible, to minimize great toe flexion weakness. However, for maximum length, the FHL is often harvested proximal to the Knot of Henry. The released distal end of the FHL is then retrieved proximally into the Achilles wound.
- Mobilization: Mobilize the FHL tendon proximally, ensuring it is free from adhesions and has adequate length to reach the proximal Achilles stump. Care must be taken to avoid injury to the neurovascular bundle (tibial nerve and posterior tibial artery) lying medial to the FHL.
4. FHL Transfer and Fixation
- Passage: The harvested FHL tendon is then passed through the previously created calcaneal tunnels from posterior to anterior. The sutures passed earlier are used to shuttle the FHL tendon through the tunnels. The tendon should exit the plantar aspect of the foot and then be rerouted back superiorly for fixation.
- Securing to Calcaneus: The FHL is typically secured to the calcaneus under appropriate tension. One technique involves passing the FHL through a single calcaneal tunnel, looping it and suturing it back onto itself (tendon-to-tendon repair) with strong non-absorbable sutures (e.g., Krackow stitch). Another common method, particularly for larger defects, involves passing the FHL through two or three parallel calcaneal tunnels and securing the limbs of the FHL directly into the Achilles stump or to the calcaneal periosteum.
-
Proximal Fixation to Achilles Stump:
The primary goal is to bridge the Achilles defect and augment the remaining tendon. The FHL tendon is brought proximally and integrated into the Achilles tendon stump using a variety of robust suturing techniques.
- Side-to-Side Anastomosis: The FHL can be woven through the proximal Achilles stump in a Pulvertaft fashion.
- End-to-Side Anastomosis: The FHL can be sutured directly into the proximal Achilles stump with multiple non-absorbable sutures (e.g., Krackow, modified Bunnell). The FHL can also be split longitudinally to create two limbs for broader integration.
- Tensioning: Tensioning is critical. The foot should be positioned in 10-20 degrees of plantarflexion during FHL fixation to minimize tension on the repair, yet allow for a functional range of motion post-operatively. Over-tensioning can lead to stiffness, while under-tensioning can result in persistent weakness.
- Direct Repair (if possible): If any portion of the Achilles tendon stumps can be approximated without excessive tension after FHL transfer, a primary repair of the remaining Achilles tissue can be performed over the FHL, further reinforcing the construct.
5. Wound Closure
- Paratenon: The paratenon, if preserved, can be loosely reapproximated to provide a gliding surface.
- Subcutaneous Tissue: Close the subcutaneous layers with absorbable sutures.
- Skin: Close the skin with non-absorbable sutures or staples.
- Dressing: Apply a sterile dressing.
- Splint/Cast: Apply a well-padded posterior splint or cast with the ankle in approximately 15-20 degrees of plantarflexion. This minimizes tension on the repair.
Complications & Management
Despite meticulous technique, FHL transfer for chronic Achilles rupture carries potential complications. Understanding these and having a management strategy is crucial.
Common Complications & Salvage Strategies
| Complication | Incidence | Management / Salvage Strategy |
|---|---|---|
| Wound Infection | 5-15% (superficial), 1-3% (deep) | Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, intravenous antibiotics, wound irrigation, potentially negative pressure wound therapy. In severe cases, hardware removal, or reconstructive flap surgery may be necessary. |
| Sural Nerve Injury | 5-10% (paresthesia), <1% (neuroma) | Careful intraoperative identification and protection. Post-op: Conservative management for paresthesia (neurontin, observation). Persistent symptoms or painful neuroma may require surgical neurolysis or neurectomy. |
| Re-rupture | 2-5% | Early (<3 months): Often surgical revision with further augmentation (e.g., allograft, gastrocnemius flap) or repeat FHL transfer if available and viable. Late (>3 months): Depends on functional deficit, may require revision surgery, or further conservative management if minor. |
| Donor Site Morbidity (Great Toe) | 10-20% (mild weakness/stiffness), <5% (functional deficit) | Patients generally adapt well. Pre-operative counseling is essential. Management: Physiotherapy focusing on FDL strengthening and toe exercises. Persistent pain or significant functional impairment is rare but may require orthopedic consultation. |
| Adhesions/Stiffness | Variable, often mild | Early controlled mobilization within protocol. Intensive physical therapy with focus on range of motion and manual therapy. Surgical adhesiolysis in recalcitrant cases. |
| Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE) | <1% with prophylaxis | Pharmacological prophylaxis (LMWH, aspirin) and mechanical prophylaxis (compression stockings, early mobilization). Symptomatic DVT: Anticoagulation. PE: Emergency medical management. |
| Skin Necrosis/Dehiscence | 1-5% | Meticulous soft tissue handling, careful incision placement, tension-free closure. Management: Local wound care, serial debridement. May require skin grafting or local flap coverage for larger defects. |
| Pain | Variable | Multimodal analgesia. Physiotherapy, addressing muscle imbalances, joint stiffness. Chronic pain may require pain management consultation. |
| Calcaneal Tunnel Fracture | Rare | Avoid by ensuring adequate bone bridge and careful drilling. Management: Cast immobilization, potentially revise tunnels, or use different fixation methods. |
General Management Principles
- Prophylaxis: Routine antibiotic prophylaxis before incision and thromboprophylaxis post-operatively are standard.
- Patient Education: Comprehensive education about expected recovery, potential complications, and adherence to rehabilitation protocols is crucial for managing expectations and improving outcomes.
- Early Recognition: Prompt identification and management of complications can prevent escalation and improve salvage rates.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical component of successful FHL transfer for chronic Achilles rupture, aimed at protecting the repair while gradually restoring strength, flexibility, and function. Protocols vary, but typically follow a phased approach.
Phase 1: Immobilization and Protected Weight-Bearing (Weeks 0-6)
- Goal: Protect the repair, minimize swelling, and promote initial healing.
-
Weeks 0-2:
- Non-weight-bearing (NWB) in a short-leg cast or controlled ankle motion (CAM) boot with the ankle in 15-20 degrees of plantarflexion.
- Elevation, ice, and pain management.
- Gentle, active range of motion (ROM) for the knee and hip. Great toe flexion should be avoided if the FHL was harvested through a distal incision or if the Knot of Henry was significantly disturbed.
-
Weeks 2-4:
- Maintain NWB in CAM boot, gradually reducing plantarflexion angle (e.g., 10 degrees).
- Initiate gentle, pain-free active ankle ROM within a protected range (e.g., 15 degrees plantarflexion to neutral) as tolerated, emphasizing dorsiflexion limits.
- Isometrics for gastrocnemius/soleus without resistance.
-
Weeks 4-6:
- Partial weight-bearing (PWB) in CAM boot as tolerated, gradually progressing to full weight-bearing (FWB) by week 6.
- Continue ROM exercises, striving for neutral dorsiflexion.
- Initiate gentle resistance exercises for hip and knee.
Phase 2: Progressive Mobilization and Strengthening (Weeks 6-12)
- Goal: Restore full ankle ROM, begin strengthening the plantarflexors, and improve gait mechanics.
-
Weeks 6-8:
- Transition out of CAM boot for ambulation, using supportive footwear (e.g., shoe with heel lift) as tolerated. Continue boot for longer distances or unstable surfaces.
- Progress ankle ROM to achieve full dorsiflexion.
- Initiate light resistance band exercises for all ankle movements (plantarflexion, dorsiflexion, inversion, eversion).
- Initiate seated calf raises with minimal resistance.
- Focus on normal gait pattern and balance training.
-
Weeks 8-12:
- Discontinue CAM boot.
- Progress resistance exercises for plantarflexion (standing calf raises, heel raises, seated calf raises with increasing weight).
- Proprioceptive training (balance board).
- Light cardiovascular exercise (e.g., stationary bike, elliptical).
- Address any remaining great toe weakness/stiffness with specific exercises if necessary.
Phase 3: Advanced Strengthening and Return to Activity (Months 3-6+)
- Goal: Maximize strength, power, endurance, and agility; prepare for return to sport/high-level activities.
-
Months 3-4:
- Advance strengthening: weighted calf raises, eccentric calf exercises, plyometric drills (e.g., double-leg hopping, jumping).
- Sport-specific drills, agility training.
- Gradual introduction of jogging/running.
- Continue stretching to maintain full ROM.
-
Months 4-6+:
- Progress to single-leg calf raises and hopping drills.
- Increase intensity and duration of running and sport-specific activities.
- Gradual return to full activity/sport based on functional testing (e.g., single leg heel raise endurance, hop tests, power assessments) and physician clearance. This typically takes 6-12 months.
Key Considerations
- Individualized Approach: Protocols should be tailored to the individual patient's healing, pain tolerance, and functional progress.
- Close Monitoring: Regular follow-up with the surgeon and physical therapist is essential to monitor progress and adjust the protocol as needed.
- Pain as a Guide: Activities should not elicit significant pain.
- Gradual Progression: Avoid premature advancement of activities to prevent re-injury.
Summary of Key Literature / Guidelines
The literature strongly supports FHL tendon transfer as a reliable and effective reconstructive option for chronic Achilles tendon ruptures with large defects.
-
Evidence for Efficacy:
Multiple studies, including systematic reviews and meta-analyses, have demonstrated favorable outcomes with FHL transfer. Patients typically achieve significant improvement in plantarflexion strength, functional scores (e.g., American Orthopaedic Foot & Ankle Society (AOFAS) Ankle-Hindfoot Scale, Achilles Tendon Rupture Score (ATRS)), and return to pre-injury activity levels.
- Maffulli et al. (2010): A comprehensive review highlighted FHL transfer as an excellent option for chronic ruptures, emphasizing good functional recovery and low re-rupture rates.
- Den Hartog (2006): Demonstrated that FHL transfer significantly improved plantarflexion strength and allowed a high percentage of patients to return to recreational sports.
- Wapner et al. (2009): Found excellent results in a large series of FHL transfers, with most patients achieving good to excellent functional outcomes and acceptable donor site morbidity.
- Comparison to Other Techniques: FHL transfer generally outperforms local flaps (e.g., gastrocnemius V-Y advancement) for larger defects (>6 cm) by providing a more robust biological augmentation. While allografts can bridge defects, they carry risks of disease transmission, immunogenicity, and are generally more expensive, with potentially inferior integration compared to autograft. Synthetic grafts have largely fallen out of favor due to high complication rates.
-
Donor Site Morbidity:
The consensus is that great toe flexion weakness after FHL harvest is typically mild and well-compensated by the FDL and intrinsic foot muscles. Most patients do not report significant functional deficit from the donor site.
- Rezaei et al. (2014): A study specifically on donor site morbidity found that while objective weakness in great toe flexion could be measured, subjective functional impairment was rare.
- Long-Term Outcomes: Studies suggest that the favorable outcomes of FHL transfer are maintained in the long term, with sustained improvements in strength and function.
- Guidelines: While no single universally accepted guideline exists, the general consensus among orthopedic foot and ankle surgeons is that FHL transfer is the preferred technique for chronic Achilles ruptures with significant gaps that preclude primary repair. The emphasis is on early surgical intervention for chronic cases once identified, as prolonged delay can lead to more extensive muscle atrophy and tendon retraction, complicating reconstruction.
- Future Directions: Research continues to refine surgical techniques, optimize rehabilitation protocols, and explore advanced imaging modalities for pre-operative assessment and post-operative monitoring. The role of biologics (e.g., PRP) as adjuncts to FHL transfer remains an area of ongoing investigation.
In summary, FHL transfer offers a predictable and durable solution for a challenging clinical problem, allowing patients with chronic Achilles ruptures to regain significant function and improve their quality of life. The meticulous execution of the surgical technique coupled with a structured, progressive rehabilitation protocol is paramount for achieving optimal patient outcomes.
Clinical & Radiographic Imaging