Diagnosing Hindfoot Pain: When It's Not Tibial Tendon Dysfunction
Introduction & Epidemiology
Hindfoot pain is a prevalent presenting complaint in orthopedic practice, often leading to significant functional impairment and a reduction in quality of life. While posterior tibial tendon dysfunction (PTTD), manifesting as adult-acquired flatfoot deformity, is a common and extensively studied etiology, a substantial proportion of patients present with hindfoot pain originating from other sources. Misdiagnosis or delayed diagnosis of these alternative pathologies can lead to ineffective treatment, prolonged suffering, and potentially irreversible secondary changes. This review aims to systematically explore the differential diagnoses for hindfoot pain when PTTD is not the primary cause, focusing on the critical anatomical, biomechanical, and diagnostic considerations necessary for the discerning orthopedic surgeon.
Epidemiologically, hindfoot pain is multifactorial and its prevalence varies depending on the specific underlying condition. PTTD affects an estimated 3.3% of women over 40 and 1.9% of the general population, establishing it as a significant contributor. However, conditions such as subtalar arthritis, often post-traumatic, can affect up to 15% of patients with a history of calcaneal fracture. Sinus tarsi syndrome, while debated as a distinct entity or a symptom complex, is frequently encountered. Peroneal tendon pathologies, including tendinopathy and tears, are common in athletes and those with chronic ankle instability, representing 5-10% of all ankle-related complaints. Posterior ankle impingement syndrome is particularly common in dancers and athletes requiring extreme plantarflexion, with an incidence rate as high as 60% in professional ballet dancers. Calcaneal stress fractures are more prevalent in military recruits, runners, and individuals with osteopenia, accounting for up to 20% of all foot stress fractures. Understanding this diverse epidemiology underscores the necessity of a broad differential and a methodical diagnostic approach beyond PTTD.
Surgical Anatomy & Biomechanics
A precise understanding of hindfoot anatomy and biomechanics is paramount for accurate diagnosis and effective treatment of non-PTTD pathologies. The hindfoot comprises the talus and calcaneus, forming the talocrural (ankle) and subtalar (talocalcaneal) joints.
Osseous Structures
- Talus: Crucial link between the leg and foot, transmitting forces. Its lack of muscle attachments makes it susceptible to avascular necrosis following trauma.
- Calcaneus: The largest tarsal bone, forming the heel. It articulates with the talus superiorly (subtalar joint) and the cuboid anteriorly (calcaneocuboid joint, part of the midtarsal joint). Calcaneal fractures are notorious for sequelae such as subtalar arthritis, peroneal impingement, and malunion leading to hindfoot deformity.
- Navicular: Key component of the midfoot, articulating with the talus posteriorly and cuneiforms anteriorly. Its relationship with the posterior tibial tendon insertion is critical.
- Os Trigonum: An accessory ossicle or ununited lateral tubercle of the posterior process of the talus, present in 7-25% of the population. When symptomatic, it contributes to posterior ankle impingement.
- Sinus Tarsi: A canal between the neck of the talus and the calcaneus, bordered by the extensor digitorum brevis, contents include fat, neurovascular structures, and ligaments (cervical and interosseous talocalcaneal ligaments). Inflammation or injury here can lead to "sinus tarsi syndrome."
Ligamentous Structures
- Subtalar Ligaments: The cervical and interosseous talocalcaneal ligaments are vital for subtalar joint stability and proprioception. Injury can lead to subtalar instability or sinus tarsi syndrome.
- Deltoid Ligament Complex: A strong medial stabilizer of the ankle, connecting the medial malleolus to the talus, navicular, and calcaneus. Injuries can cause medial hindfoot pain and valgus instability.
- Lateral Ankle Ligaments: Anterior talofibular (ATFL), calcaneofibular (CFL), and posterior talofibular (PTFL) ligaments are primary stabilizers against inversion. Chronic instability can lead to peroneal pathology and subtalar degenerative changes.
- Spring Ligament (Plantar Calcaneonavicular Ligament): Supports the medial longitudinal arch, connecting the sustentaculum tali to the navicular. Although classically associated with PTTD, isolated injury can also contribute to arch collapse and medial hindfoot pain.
Tendinous Structures
- Peroneal Tendons (Fibularis Longus & Brevis): Course posterolateral to the lateral malleolus, crucial for ankle eversion and lateral hindfoot stability. Pathology includes tendinopathy, tears, subluxation/dislocation, and impingement (e.g., against a calcaneal malunion or peroneal tubercle hypertrophy). The fibularis brevis inserts on the fifth metatarsal base, while the fibularis longus courses under the cuboid to insert on the first metatarsal and medial cuneiform.
- Flexor Hallucis Longus (FHL) Tendon: Originates from the posterior fibula, courses through a groove on the posterior talus and sustentaculum tali, deep to the posterior tibial tendon, to insert on the hallux distal phalanx. It can be a source of posterior ankle pain due to tenosynovitis, stenosing tenosynovitis, or impingement, particularly with os trigonum pathology.
- Flexor Digitorum Longus (FDL) Tendon: Courses medially, parallel to the PTT, but more posterior. Rarely a primary source of isolated hindfoot pain, but can be involved in multi-tendon pathologies.
- Achilles Tendon: Inserts into the posterior calcaneus. While primarily an ankle dorsiflexor, its pathology (tendinopathy, rupture, insertional calcification) can be perceived as diffuse posterior hindfoot pain.
Neurovascular Structures
- Tibial Nerve (Tarsal Tunnel): Courses posterior to the medial malleolus, deep to the flexor retinaculum, with its branches (medial and lateral plantar nerves, medial calcaneal nerve). Compression (tarsal tunnel syndrome) causes burning pain, numbness, and tingling, classically radiating into the arch and toes, but can present as diffuse hindfoot pain.
- Sural Nerve: Arises from the tibial and common peroneal nerves, runs posterolateral to the ankle. Susceptible to injury during lateral hindfoot approaches or direct trauma, causing neuropathic pain or numbness in its distribution.
- Medial Calcaneal Nerve: A branch of the tibial nerve, supplying sensation to the medial heel. Compression or entrapment can mimic plantar fasciitis.
Biomechanics
The hindfoot complex functions to adapt to varied terrain and propel the body.
*
Subtalar Joint:
Primarily allows pronation and supination, critical for shock absorption and converting the foot from a flexible adapter to a rigid lever. Dysfunctional subtalar motion, whether due to arthritis, instability, or coalition, directly impairs gait and causes pain.
*
Peroneal Tendon Function:
Essential for dynamic lateral stability, resisting inversion, and assisting in first ray plantarflexion (fibularis longus). Weakness or pathology leads to inversion sprains and altered foot mechanics.
*
FHL Function:
Crucial for toe-off during gait. Its posterior course makes it vulnerable to impingement with repetitive plantarflexion.
A comprehensive clinical assessment, integrating a detailed history and physical examination, is indispensable for narrowing the differential. Pain localization, aggravating factors, associated symptoms (e.g., clicking, instability, numbness), and patient demographics guide the diagnostic process. Palpation of specific anatomical landmarks, provocative maneuvers (e.g., forced dorsiflexion for posterior impingement, eversion against resistance for peroneal pathology, Tinel's sign for tarsal tunnel), and gait analysis are key.
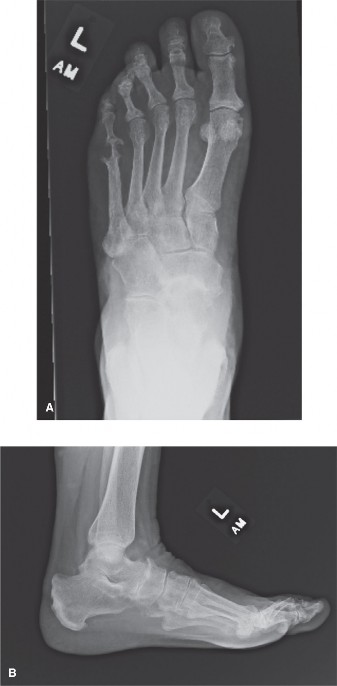
Figure 1: Illustration depicting key anatomical structures of the hindfoot, highlighting common sites of non-PTTD pathology.
Indications & Contraindications
When hindfoot pain is determined not to be originating from the posterior tibial tendon, the indications and contraindications for intervention depend heavily on the specific alternative diagnosis. Non-operative management is the initial approach for most conditions, often involving activity modification, orthoses, physical therapy, and anti-inflammatory medications. Surgical intervention is typically reserved for cases that fail comprehensive non-operative treatment, or for acute conditions requiring immediate stabilization or decompression.
Indications for Intervention (Non-PTTD Hindfoot Pain)
-
Subtalar Arthritis:
- Non-Operative: Mild to moderate pain, early degenerative changes, no significant deformity, failure to improve with conservative measures (NSAIDs, activity modification, bracing, injections).
- Operative: Persistent severe pain despite non-operative treatment, significant functional limitation, progressive joint destruction, symptomatic hindfoot deformity (e.g., varus or valgus malalignment).
-
Peroneal Tendinopathy/Tears/Subluxation:
- Non-Operative: Mild tendinopathy, intact retinaculum, acute tendinitis, no mechanical symptoms.
- Operative: Chronic symptomatic tendinopathy unresponsive to conservative care, longitudinal tears (>50% thickness), complete ruptures, recurrent subluxation/dislocation of tendons, associated ankle instability or osseous impingement (e.g., enlarged peroneal tubercle).
-
Posterior Ankle Impingement Syndrome (Os Trigonum Syndrome, FHL Tenosynovitis):
- Non-Operative: Mild, intermittent pain, acute presentation, no mechanical block.
- Operative: Persistent pain or mechanical symptoms (catching, stiffness) despite non-operative treatment, symptomatic os trigonum, stenosing FHL tenosynovitis, cartilage lesions amenable to debridement.
-
Tarsal Tunnel Syndrome:
- Non-Operative: Mild to moderate intermittent symptoms, acute onset, no significant motor deficit.
- Operative: Persistent or progressive neuropathic pain, motor weakness, intractable symptoms despite conservative measures, identified space-occupying lesion (e.g., ganglion, varicosity).
-
Sinus Tarsi Syndrome:
- Non-Operative: Initial management with rest, NSAIDs, orthoses, corticosteroid injection.
- Operative: Chronic pain and instability unresponsive to comprehensive non-operative treatment, often when associated with subtalar instability.
-
Calcaneal Stress Fracture:
- Non-Operative: Most cases managed with protected weight-bearing (boot/crutches) for 6-12 weeks, activity modification, bone health optimization.
- Operative: Rarely indicated; may be considered for displaced fractures in specific circumstances, but typically treated non-operatively.
Contraindications for Surgical Intervention
General contraindications apply to most elective hindfoot surgeries:
* Active local or systemic infection.
* Severe uncontrolled systemic comorbidities (e.g., uncontrolled diabetes, severe peripheral vascular disease, significant cardiac or pulmonary compromise) that significantly increase anesthetic and surgical risk.
* Severe neuropathy affecting the foot that could compromise wound healing or sensation post-operatively.
* Poor soft tissue envelope or compromised skin integrity in the operative field.
* Non-compliance with post-operative protocols (e.g., weight-bearing restrictions, rehabilitation).
* Unrealistic patient expectations regarding outcome.
Table: Operative vs. Non-Operative Indications for Non-PTTD Hindfoot Conditions
| Condition | Primary Non-Operative Indications | Primary Operative Indications |
|---|---|---|
| Subtalar Arthritis | Mild pain, early changes, no significant deformity | Severe pain, functional limitation, progressive deformity, failed non-op |
| Peroneal Tendinopathy/Tears | Mild tendinopathy, intact retinaculum, acute inflammation | Chronic tendinopathy, tears (>50%), recurrent subluxation, osseous impingement |
| Posterior Ankle Impingement | Intermittent pain, acute onset, no mechanical block | Persistent pain/mechanical symptoms, symptomatic os trigonum/FHL tenosynovitis |
| Tarsal Tunnel Syndrome | Mild/intermittent symptoms, acute onset, no motor deficit | Progressive neuropathic pain/weakness, failed conservative, mass effect |
| Sinus Tarsi Syndrome | Acute pain, respond to injection/brace, no gross instability | Chronic pain & instability refractory to conservative measures |
| Calcaneal Stress Fracture | All cases (unless severely displaced, extremely rare) | (Rarely indicated) |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is essential for successful hindfoot surgery. This involves a meticulous review of patient history, physical examination findings, and comprehensive imaging.
Pre-Operative Planning
- Clinical Assessment: Reconfirm the diagnosis. Evaluate for comorbidities (e.g., diabetes, smoking, peripheral neuropathy) that may affect wound healing, infection risk, or non-union rates. Assess overall functional status and patient expectations.
-
Imaging Review:
- Weight-bearing Radiographs: Essential for evaluating alignment, joint space narrowing, and osseous deformities (AP, lateral, oblique foot; AP and lateral ankle). Saltzman view for hindfoot alignment.
- MRI: Gold standard for soft tissue evaluation (tendons, ligaments, nerve pathology), marrow edema (stress fractures), cartilage status, and identifying space-occupying lesions in the tarsal tunnel or sinus tarsi.
- CT Scan: Superior for complex osseous pathology, particularly post-traumatic arthritis, coalitions, or subtle fractures. Useful for surgical planning of fusions or osteotomies.
- SPECT-CT: Can be valuable for localizing metabolic activity in ambiguous pain presentations, differentiating between active arthritis, tendinopathy, or stress reactions.
-
Surgical Planning:
- Approach Selection: Based on the specific pathology (e.g., lateral for subtalar fusion, posterolateral/posteromedial for posterior impingement, medial for tarsal tunnel release).
- Hardware Selection: For fusions, determine screw length and diameter, plate choice. For tendon repairs/transfers, appropriate suture and anchor selection.
- Instrumentation: Ensure all necessary instruments for bone work (osteotomes, burrs, reamers), soft tissue dissection, and fixation are available.
- Contingency Planning: Prepare for potential intraoperative findings not fully appreciated pre-operatively (e.g., more severe arthritis, occult fracture).
Patient Positioning
Patient positioning is critical for optimal exposure and minimizing complications.
1.
General Considerations:
*
Tourniquet:
Typically applied to the proximal thigh, inflated to 250-300 mmHg for exsanguination and a bloodless field, crucial for visualization.
*
Anesthesia:
General anesthesia is common, sometimes supplemented with regional blocks (e.g., popliteal block) for post-operative pain control.
*
C-arm:
Readily available and draped for intraoperative fluoroscopic imaging, especially for fusions or hardware placement.
2.
Specific Positions:
*
Supine with Bump:
For medial approaches (e.g., tarsal tunnel release, FHL tenolysis via posteromedial approach). A bump under the ipsilateral hip rotates the foot internally, presenting the medial aspect.
*
Lateral Decubitus:
Primarily for lateral approaches (e.g., subtalar fusion via sinus tarsi approach, peroneal tendon repair/reconstruction). The affected limb is prepped free, allowing easy access to the lateral aspect. Consider a beanbag positioner for stability.
*
Prone:
Less common for hindfoot-specific procedures, but can be used for extensive posterior approaches or combined Achilles/posterior ankle pathology. Care must be taken to pad pressure points. For posterior ankle arthroscopy, prone or supine with significant ankle hyperflexion are options.
Detailed Surgical Approach / Technique
Given the breadth of non-PTTD hindfoot pathologies, detailing every surgical approach is beyond the scope of this review. Instead, we will focus on the principles of two representative and commonly performed procedures for non-PTTD hindfoot pain: Subtalar Arthrodesis (for subtalar arthritis) and Posterior Ankle Arthroscopy / Open Posterior Debridement (for posterior ankle impingement).
Subtalar Arthrodesis (Lateral Sinus Tarsi Approach)
Subtalar arthrodesis is a common procedure for debilitating subtalar arthritis or instability refractory to conservative management. The lateral sinus tarsi approach provides excellent access to the subtalar joint while preserving the peroneal tendons and neurovascular structures.
- Incision: A curvilinear incision approximately 6-8 cm long is made, centered over the sinus tarsi. It typically starts just distal to the tip of the fibula, extending distally and slightly obliquely towards the cuboid. This avoids direct incision over the sural nerve, which often courses more posteriorly.
-
Dissection & Internervous Plane:
- Careful dissection through subcutaneous tissues. Identify and protect the sural nerve , typically located subcutaneously, posterior and lateral to the incision. Branches may need to be retracted.
- The superficial fascia is incised. The extensor digitorum brevis (EDB) muscle belly often lies immediately deep. This muscle can be split longitudinally or reflected plantarly to expose the sinus tarsi.
- The internervous plane for this approach involves retracting the EDB, which is innervated by the deep peroneal nerve, and accessing the deeper structures which are in proximity to the sural nerve (sensory, lateral side).
- Deep to the EDB, the cervical and interosseous talocalcaneal ligaments are encountered, forming the roof and floor of the sinus tarsi. These are sharply divided and excised to expose the subtalar joint.
-
Joint Preparation:
- The articular cartilage from the middle and posterior facets of the subtalar joint is meticulously removed. A combination of osteotomes, curettes, and burrs can be used. Care must be taken to avoid damaging the underlying subchondral bone, which is vital for fusion, but sclerotic bone may need to be decorticated.
- Ensure complete removal of all cartilage remnants and eburnated bone to expose bleeding cancellous surfaces.
- Correct any existing hindfoot deformity (e.g., varus or valgus) by carefully resecting wedges of bone as needed. The goal is to achieve a neutral or slightly valgus alignment (typically 0-5 degrees).
- Bone Grafting: Autologous bone graft (e.g., from the calcaneus via the same incision or from the distal tibia) or allograft can be packed into the denuded joint space to promote fusion.
-
Fixation:
- Typically, two or three large-diameter cannulated screws (e.g., 6.5mm or 7.0mm) are used for compression.
-
Screw Trajectory:
- One screw is usually placed from the posterior-lateral aspect of the calcaneal tuberosity, aiming anteromedially across the subtalar joint into the talar neck.
- A second screw is placed more anteriorly in the lateral calcaneus, aiming superior-medially into the talar body.
- Some surgeons use a third screw or a plate for enhanced stability.
- Reduction & Compression: The hindfoot is manually reduced into the desired alignment (often neutral to 5 degrees valgus), and provisional fixation (K-wires) may be used. Guide wires for cannulated screws are then placed under fluoroscopic guidance, ensuring proper trajectory and preventing intra-articular placement or neurovascular injury. Screws are inserted, achieving lag compression across the fusion site.
- Closure: The wound is copiously irrigated. The EDB muscle is allowed to fall back into place. The subcutaneous layers and skin are closed anatomically.
Posterior Ankle Arthroscopy / Open Posterior Debridement (for Impingement)
Posterior ankle impingement syndrome, often involving os trigonum or FHL tenosynovitis, can be addressed arthroscopically or with an open approach. Arthroscopy offers advantages of minimal invasiveness but requires significant skill.
Posterior Ankle Arthroscopy (Posterolateral & Posteromedial Portals)
- Patient Positioning: Prone position with a pillow under the distal tibia and the foot hanging free, or supine with the ankle hyperflexed over a support. A distraction device may be helpful.
-
Portal Placement:
- Posterolateral Portal: Located approximately 1-1.5 cm proximal and 1 cm lateral to the Achilles tendon insertion, just lateral to the Achilles. Avoid the sural nerve.
- Posteromedial Portal: Located approximately 1-1.5 cm proximal and 1 cm medial to the Achilles tendon insertion, just medial to the Achilles. Avoid the neurovascular bundle (tibial nerve, posterior tibial artery, posterior tibial tendon, FDL, FHL).
- Establish the posterolateral portal first. After skin incision, a blunt trocar is used to enter the posterior compartment, aiming towards the anteromedial malleolus.
- Once the cannula is in, fluid distension and the arthroscope are introduced.
-
Anatomy & Debridement:
- The flexor hallucis longus (FHL) tendon groove on the posterior talus is a key landmark. The tendon runs through the posterior compartment.
- Identify the os trigonum (if present) or the prominent lateral tubercle of the posterior talus.
- Identify inflamed synovium, fibrous bands, or impinging soft tissue.
- Using shavers and burrs, debride hypertrophic synovium, fibrous scar tissue, and excise the os trigonum. Care must be taken not to injure the FHL tendon.
- If FHL tenosynovitis is present, the tendon sheath can be released, and debridement of inflammatory tissue around the tendon performed.
- Confirm free range of motion of the ankle and FHL tendon after debridement.
- Closure: Remove instruments, allow fluid to drain. Close skin incisions with simple sutures or steri-strips.
Open Posterior Debridement (Posteromedial Approach)
For larger resections, extensive FHL tenolysis, or in cases where arthroscopy is contraindicated/unsuccessful, an open approach may be preferred. The posteromedial approach is often used to address the os trigonum and FHL.
- Incision: A longitudinal incision approximately 6-8 cm long is made posterior to the medial malleolus, parallel to the Achilles tendon.
-
Dissection & Internervous Plane:
- Carefully dissect through the subcutaneous tissue. Identify and protect the sural nerve (often more lateral) and the tibial nerve/vascular bundle (more medial, deep to the flexor retinaculum).
- Retract the Achilles tendon laterally.
- The internervous plane involves separating the Achilles tendon complex (sural nerve, musculocutaneous, sensory) from the deeper structures (tibial nerve, motor/sensory).
- Incise the deep fascia. The flexor retinaculum will be encountered. Incise it carefully.
- Deep to the retinaculum, the tendons of tibialis posterior, FDL, and FHL , along with the tibial nerve and posterior tibial artery/veins are encountered (from anterior to posterior, medial to lateral).
- Carefully retract the neurovascular bundle and the FDL/PTT tendons medially. The FHL tendon lies deepest, running in its groove on the posterior talus.
-
Debridement:
- Expose the posterior aspect of the talus. The os trigonum or lateral talar tubercle is identified.
- Using osteotomes or a small burr, excise the os trigonum and debride any impinging bone.
- If FHL tenosynovitis is present, perform a tenolysis by incising the FHL tendon sheath longitudinally, debriding any inflammatory tissue around the tendon. Ensure the tendon glides freely.
- Closure: Irrigate the wound. The flexor retinaculum may or may not be repaired, depending on tension. Close subcutaneous tissues and skin layers.
Complications & Management
Complications following hindfoot surgery, particularly for non-PTTD pathologies, can be diverse and may vary depending on the specific procedure. Vigilant post-operative care and timely recognition are crucial for effective management.
General Complications
-
Infection:
Superficial wound infection (cellulitis) or deep surgical site infection (osteomyelitis, septic arthritis).
- Incidence: 1-5%. Higher in diabetics, immunocompromised, or smokers.
- Management: Superficial infections may respond to oral antibiotics. Deep infections require surgical debridement, intravenous antibiotics, and potentially hardware removal (if fusion is solid) or staged reconstruction.
-
Wound Healing Issues:
Delayed healing, dehiscence, necrosis, particularly problematic with limited soft tissue coverage in the ankle/hindfoot.
- Incidence: 5-15%, especially in patients with diabetes, PVD, or who smoke.
- Management: Local wound care, débridement, negative pressure wound therapy. May require skin grafting or flap coverage for severe cases.
-
Nerve Injury:
Transection, stretch, or compression of local nerves (e.g., sural nerve with lateral approaches, tibial nerve with medial approaches, saphenous nerve with medial malleolar hardware).
- Incidence: 5-20% for sensory nerves (often transient neuropraxia), <1% for motor nerves.
- Management: Most neuropraxias resolve spontaneously. Neuropathic pain may be managed with gabapentin/pregabalin. Persistent pain or motor deficit may warrant nerve exploration and neurolysis, or repair for transection.
-
DVT/PE:
Deep vein thrombosis and pulmonary embolism are risks with any lower extremity surgery.
- Incidence: DVT 1-5%, PE <1%.
- Management: Prophylaxis (chemical, mechanical) is standard. Treatment involves anticoagulation.
-
Complex Regional Pain Syndrome (CRPS):
A rare but debilitating pain condition.
- Incidence: <1%.
- Management: Multimodal approach including physical therapy, pharmacotherapy (gabapentinoids, TCAs), nerve blocks, and psychological support. Early diagnosis is key.
Specific Complications for Subtalar Arthrodesis
-
Non-Union / Delayed Union:
Failure of the bones to fuse.
- Incidence: 5-15%. Higher in smokers, NSAID users, revision surgery, poor bone quality.
- Management: Prolonged immobilization, bone stimulator. For established non-union: revision surgery with debridement, fresh bone graft (autograft is preferred), and rigid internal fixation.
-
Malunion:
Fusion in an undesirable position (e.g., excessive varus/valgus).
- Incidence: 2-5%.
- Management: For symptomatic malunion, corrective osteotomy or revision arthrodesis may be required.
-
Hardware Complications:
Screw prominence, breakage, or loosening.
- Incidence: 5-10%.
- Management: Symptomatic hardware may require removal after fusion is complete.
-
Adjacent Joint Arthritis:
Increased stress on the ankle or midtarsal joints.
- Incidence: Long-term, progressive.
- Management: Non-operative initially (NSAIDs, orthotics), potentially fusion of the adjacent joint if severe.
Specific Complications for Posterior Ankle Arthroscopy / Debridement
-
Incomplete Debridement / Persistent Impingement:
Residual pathology causing continued pain.
- Incidence: 5-10%.
- Management: Re-evaluation, potentially repeat arthroscopy or open revision.
-
FHL Tendon Injury:
Laceration or damage during debridement.
- Incidence: <1% but reported.
- Management: Repair of the tendon if significant. Post-operative immobilization.
-
Ankle Stiffness:
Restricted dorsiflexion/plantarflexion.
- Incidence: 5-15%.
- Management: Intensive physical therapy, stretching, possibly manipulation under anesthesia.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Approx.) | Salvage Strategies |
|---|---|---|
| Infection (Deep) | 1-5% | Debridement, IV antibiotics, hardware removal (if applicable) |
| Wound Dehiscence | 5-15% | Local wound care, NPWT, débridement, skin grafting/flaps |
| Sural Nerve Neuropraxia | 10-20% | Observation, pain medication, nerve blocks, neurolysis |
| Non-Union (Fusion) | 5-15% | Revision surgery with grafting & rigid fixation, bone stimulator |
| Malunion (Fusion) | 2-5% | Corrective osteotomy, revision arthrodesis |
| Hardware Prominence | 5-10% | Hardware removal (after fusion) |
| Persistent Impingement | 5-10% | Re-evaluation, repeat debridement (arthroscopic or open) |
| FHL Tendon Injury | <1% | Tendon repair, immobilization |
| Adjacent Joint Arthritis | Long-term | Non-operative, eventually fusion of adjacent joint |
| Complex Regional Pain Syndrome | <1% | Multimodal pain management, PT, nerve blocks |
Post-Operative Rehabilitation Protocols
Rehabilitation protocols for hindfoot surgery are tailored to the specific procedure performed, the stability of fixation, and the individual patient's healing capacity. The overarching goals are to protect the surgical repair/fusion, restore range of motion (where appropriate), regain strength, and facilitate a safe return to functional activities.
General Principles
- Pain Management: Crucial for early mobilization and compliance. Multimodal approach including NSAIDs, acetaminophen, opioids (short-term), and nerve blocks.
- Wound Care: Meticulous care to prevent infection and promote healing.
- Edema Control: Elevation, compression stockings, cryotherapy.
- Early Motion (When Permitted): Prevents stiffness and promotes circulation.
- Gradual Weight-Bearing Progression: Essential to allow tissue healing and bone consolidation.
- Neuromuscular Re-education: Focus on proprioception, balance, and gait training.
Subtalar Arthrodesis Rehabilitation Protocol
-
Phase I: Protection (Weeks 0-6)
- Immobilization: Non-weight-bearing (NWB) in a short leg splint or cast.
- Activity: Strict elevation, toe wiggles, gentle hip/knee exercises.
- Goal: Protect fusion, control pain and swelling.
-
Phase II: Controlled Mobilization (Weeks 6-12)
- Immobilization: Transition to a removable short leg walking boot or CAM walker.
- Weight-Bearing: Gradual progression from NWB to partial weight-bearing (PWB) with crutches, as tolerated and confirmed by radiographs showing early signs of fusion.
- Motion: Gentle ankle dorsiflexion/plantarflexion. Avoid subtalar motion.
- Goal: Increase weight-bearing, maintain adjacent joint mobility.
-
Phase III: Strengthening & Proprioception (Weeks 12-24)
- Weight-Bearing: Progress to full weight-bearing (FWB) in boot, then transition to supportive shoe.
- Motion: Continue ankle ROM, begin gentle midfoot ROM if allowed.
- Strengthening: Progressive resistive exercises for ankle dorsiflexors, plantarflexors, evertors, invertors (sparing subtalar motion). Calf raises (bilateral then unilateral).
- Proprioception: Balance exercises (single leg stance, wobble board).
- Goal: Restore strength, balance, and gait mechanics.
-
Phase IV: Advanced Activity & Return to Sport (Months 6-12+):
- Activity: Progressive return to higher impact activities, sport-specific drills.
- Considerations: Full fusion may take 6-12 months. Long-term use of supportive footwear or orthotics may be recommended.
Posterior Ankle Arthroscopy / Open Debridement Rehabilitation Protocol
-
Phase I: Early Protection & Motion (Weeks 0-2)
- Immobilization: Initial bulky dressing/splint for comfort, then transition to a walking boot or supportive shoe for protection.
- Weight-Bearing: Partial to full weight-bearing as tolerated.
- Motion: Early, gentle active and passive ankle range of motion (dorsiflexion, plantarflexion, inversion, eversion). Start FHL gliding exercises if tenolysis was performed.
- Goal: Minimize stiffness, control swelling, promote wound healing.
-
Phase II: Strengthening & Restoration of Function (Weeks 2-6)
- Weight-Bearing: Full weight-bearing without support as tolerated.
- Strengthening: Begin progressive resistive exercises for all ankle muscle groups. Calf raises, theraband exercises.
- Proprioception: Balance and stability exercises.
- Goal: Restore full, pain-free ROM and initial strength.
-
Phase III: Advanced Activity & Return to Sport (Weeks 6-12+)
- Activity: Gradual return to activity, including running, jumping, and sport-specific drills.
- Focus: Agility, plyometrics, high-level balance training.
- Goal: Full return to desired functional level.
Close communication between the surgeon, physical therapist, and patient is paramount throughout the rehabilitation process to optimize outcomes and prevent complications.
Summary of Key Literature / Guidelines
The diagnostic and management strategies for non-PTTD hindfoot pain are guided by a growing body of literature, though high-level evidence for some specific conditions can be limited.
- Diagnostic Algorithms: Current guidelines emphasize a systematic approach, starting with a thorough history and physical examination, followed by sequential imaging. Weight-bearing radiographs remain the first-line imaging. MRI is invaluable for soft tissue assessment (tendons, ligaments, nerves) and subtle bone pathology (stress fractures, early arthritis). CT scans are preferred for complex bony anatomy and pre-surgical planning for fusions.
- Subtalar Arthritis: Multiple studies support subtalar arthrodesis as a reliable procedure for end-stage subtalar arthritis, with reported fusion rates exceeding 90% and significant pain relief. Long-term follow-up indicates a risk of adjacent joint arthritis, particularly in the ankle joint, but its clinical significance varies. Guidelines from the American Academy of Orthopaedic Surgeons (AAOS) generally support surgical intervention for failed conservative management.
- Peroneal Tendon Pathology: Consensus points towards conservative management for tendinopathy, while tears and recurrent subluxation often require surgical intervention. Studies show favorable outcomes for peroneal tendon repair or reconstruction, with or without groove deepening for subluxation. MRI is the most sensitive imaging modality for tendon tears.
- Posterior Ankle Impingement: Both arthroscopic and open techniques for os trigonum excision and FHL tenolysis demonstrate good to excellent outcomes, particularly in athletic populations. Arthroscopy offers advantages of smaller incisions and potentially faster recovery. The diagnosis is primarily clinical, supported by imaging to confirm pathology.
- Tarsal Tunnel Syndrome: Diagnosis remains challenging, relying heavily on clinical suspicion and electrodiagnostic studies (nerve conduction studies/EMG) to confirm nerve entrapment. MRI is useful to identify compressive lesions. Surgical release, when indicated, can provide significant relief in carefully selected patients, but outcomes can be variable.
- Sinus Tarsi Syndrome: Often a diagnosis of exclusion. While controversial, current literature suggests a combination of ligamentous laxity/inflammation within the sinus tarsi. Non-operative management is typically pursued first, and surgery (arthroscopic debridement or fusion if associated with instability/arthritis) is reserved for refractory cases.
- Calcaneal Stress Fractures: Management is overwhelmingly non-operative. Literature emphasizes rest, protected weight-bearing, and evaluation for underlying metabolic bone disease. Surgical intervention is rarely reported and typically reserved for highly unusual circumstances like persistent non-union with significant pain.
Ongoing research continues to refine diagnostic criteria and optimize treatment protocols for these complex hindfoot conditions, emphasizing a multidisciplinary approach involving orthopedic surgeons, physical therapists, and pain management specialists. The key remains a high index of suspicion and a thorough, systematic diagnostic workup to differentiate these diverse pathologies from the more commonly recognized posterior tibial tendon dysfunction.
