Introduction & Epidemiology
Foot ulcers represent a significant and debilitating complication of various systemic diseases, most notably diabetes mellitus, peripheral neuropathy, and peripheral arterial disease. Their global prevalence is substantial, affecting approximately 15% of diabetic patients over their lifetime, with an annual incidence ranging from 2% to 5% in this population. The morbidity associated with foot ulcers is profound, encompassing pain, infection, impaired ambulation, reduced quality of life, and a dramatically increased risk of lower extremity amputation. Indeed, foot ulcers precede up to 85% of non-traumatic amputations in diabetic patients, contributing significantly to healthcare expenditure and societal burden.
The etiology of foot ulcers is classically multifactorial, involving a complex interplay of neuropathy (sensory, motor, autonomic), ischemia, structural deformities, repetitive mechanical stress, and impaired wound healing. While neuropathy reduces protective sensation and alters foot mechanics, and ischemia compromises tissue viability, structural deformities and abnormal biomechanics often provide the critical mechanical stress that initiates ulceration. Among these biomechanical factors, isolated gastrocnemius contracture (IGC) has emerged as a frequently overlooked yet potentially significant contributor to increased plantar forefoot pressures and recurrent ulceration.
Gastrocnemius contracture limits ankle dorsiflexion, particularly when the knee is extended. This restriction forces compensatory mechanisms during gait, such as premature heel-off, subtalar pronation, and midfoot collapse, ultimately leading to excessive and sustained plantar pressures beneath the metatarsal heads and toes. In patients with sensory neuropathy, this repetitive, unperceived microtrauma frequently progresses from callus formation to ulceration, and in the presence of ischemia or infection, to deeper tissue destruction and osteomyelitis. Recognizing and addressing IGC as part of a comprehensive management strategy for foot ulcers, particularly those located in the forefoot, is therefore critical for effective treatment and prevention of recurrence. This review aims to delineate the diagnostic considerations, surgical anatomy, indications, technical approaches, and post-operative management pertaining to gastrocnemius recession in the context of foot ulcer prevention and healing.
Surgical Anatomy & Biomechanics
A thorough understanding of the anatomical and biomechanical aspects of the triceps surae complex is paramount for proper diagnosis and surgical planning in patients with gastrocnemius contracture.
Anatomy of the Triceps Surae
The triceps surae muscle group comprises three distinct muscles: the medial gastrocnemius, the lateral gastrocnemius, and the soleus. All three converge to form the Achilles tendon, which inserts onto the calcaneal tuberosity.
- Gastrocnemius: This superficial, biarticular muscle originates from the medial and lateral femoral condyles (medial and lateral heads, respectively), just above the knee joint. It is primarily composed of fast-twitch (Type II) muscle fibers, making it well-suited for powerful, propulsive movements. Due to its origin above the knee, its ability to act on the ankle is dependent on knee position. It is innervated by the tibial nerve (L4-S2).
- Soleus: Lying deep to the gastrocnemius, the soleus is a monoarticular muscle originating from the posterior aspect of the fibular head and proximal tibia. It consists predominantly of slow-twitch (Type I) muscle fibers, crucial for sustained postural control. Its action on the ankle is independent of knee position. It is also innervated by the tibial nerve (L4-S2).
- Plantaris: A small, vestigial muscle with a long tendon, originating from the lateral supracondylar ridge of the femur and inserting into the calcaneus medial to the Achilles. It contributes minimally to plantarflexion but can be a source of pain or used as a graft.
Biomechanics of Ankle Dorsiflexion and Gastrocnemius Contracture
Normal ankle dorsiflexion, with the knee extended, is typically around 10-20 degrees beyond neutral (0 degrees). This range of motion is essential for normal gait progression, particularly during the mid-stance and terminal-stance phases, allowing the tibia to advance over the foot.
- Gastrocnemius Contracture: When the gastrocnemius muscle or its aponeurosis is pathologically shortened, it restricts ankle dorsiflexion specifically when the knee is extended. This is because the gastrocnemius is stretched across both the knee and ankle joints simultaneously. When the knee is flexed, the gastrocnemius slackens, allowing for a greater range of ankle dorsiflexion.
- Soleus Contracture: A contracture of the soleus muscle restricts ankle dorsiflexion regardless of knee position, as it is a monoarticular muscle acting only on the ankle.
-
The Silfverskiöld Test:
This clinical maneuver is the gold standard for differentiating between isolated gastrocnemius contracture and global equinus contracture (involving both gastrocnemius and soleus). The test involves assessing passive ankle dorsiflexion with the knee fully extended and then with the knee flexed to 90 degrees.
- Positive Silfverskiöld Test (Isolated Gastrocnemius Contracture): Ankle dorsiflexion is limited (typically <0 degrees, i.e., in equinus) with the knee extended, but significantly improves (≥10 degrees of dorsiflexion or an improvement of >10 degrees from the extended knee position) when the knee is flexed.
- Negative Silfverskiöld Test (Global Equinus or Soleus Contracture): Ankle dorsiflexion remains limited regardless of knee position.
Impact of Gastrocnemius Contracture on Foot Biomechanics and Ulceration
The functional consequences of IGC are profound, particularly in the presence of neuropathy:
- Increased Forefoot Plantar Pressures: During the stance phase of gait, restricted ankle dorsiflexion with the knee extended prevents the tibia from advancing normally over the foot. To compensate, the foot is forced into premature heel-off and/or excessive pronation, leading to prolonged and elevated pressure on the plantar aspect of the forefoot, specifically under the metatarsal heads and hallux. This increased pressure, coupled with shear forces, is a primary driver of callus formation and subsequent ulceration, particularly in neuropathic feet that lack protective sensation.
- Midfoot Collapse and Deformity: Chronic compensatory pronation can contribute to the development or progression of acquired adult flatfoot deformity. In the context of Charcot neuroarthropathy, IGC can exacerbate midfoot collapse and rocker-bottom deformity by increasing stress across the midfoot joints.
- Hallux Valgus and Lesser Toe Deformities: Elevated forefoot pressures can also contribute to the development of hallux valgus, hammer toes, and claw toes, which in turn create new areas of pressure and potential ulceration.
- Achilles Tendinopathy: Increased tensile loads on the Achilles tendon due to persistent equinus can contribute to chronic Achilles tendinopathy.
- Impaired Wound Healing: By maintaining high plantar pressures, IGC prevents effective offloading and creates a hostile environment for wound healing, leading to recalcitrant ulcers. Even after initial ulcer closure, unaddressed IGC significantly increases the risk of recurrence.
Therefore, the identification and surgical correction of IGC in patients with chronic or recurrent forefoot ulcers, particularly in the neuropathic population, is a critical component of a comprehensive foot preservation strategy.
Indications & Contraindications
The decision to proceed with gastrocnemius recession for foot ulcer diagnosis and management is nuanced, requiring careful patient selection and consideration of overall clinical status.
Indications for Gastrocnemius Recession
The primary indication for gastrocnemius recession in the context of foot ulcers is the presence of a demonstrable isolated gastrocnemius contracture, confirmed by a positive Silfverskiöld test, in a patient with chronic or recurrent forefoot ulcers that have failed conservative management. Beyond direct ulcer management, gastrocnemius recession may be indicated for various other foot pathologies where increased forefoot pressure or equinus contracture is a significant contributing factor.
Operative Indications for Gastrocnemius Recession
| Condition | Specific Criteria | Rationale for IGC Release |
|---|---|---|
| Recalcitrant Plantar Forefoot Ulcers | Positive Silfverskiöld test; Neuropathic or neuroischemic ulcers (post-revascularization if needed); Ulcers unresponsive to aggressive offloading and wound care for ≥6 weeks; Recurrent ulcers in the same location; No active deep infection. | Reduces peak plantar pressures under metatarsal heads and toes, promoting ulcer healing and preventing recurrence. Improves ankle dorsiflexion, normalizing gait mechanics, and allowing for effective offloading. |
| Diabetic Foot Ulcer Prevention | Positive Silfverskiöld test; History of recurrent ulcers; Pre-ulcerative calluses with underlying erythema or hemorrhage; High-risk neuropathic foot with significant equinus. | Prophylactic measure to prevent initial or recurrent ulceration by addressing the underlying biomechanical stressor. Lowers the risk of limb-threatening complications in high-risk patients. |
| Charcot Neuroarthropathy | Positive Silfverskiöld test; Mild to moderate, stable Charcot foot (Eichenholtz stages I-III) with forefoot or midfoot ulceration; Equinus deformity contributing to rocker-bottom foot; Post-reconstructive stability compromised by equinus. | Decreases stress on reconstructed joints and aids in maintaining reduction/fixation. Reduces forefoot pressures in the presence of rocker-bottom deformity, improving shoe wear and preventing ulceration. May improve ankle stability and gait. |
| Adult Acquired Flatfoot Deformity | Positive Silfverskiöld test; Flexible or semi-rigid flatfoot with equinus contributing to pronation; Persistent pain or progressive deformity despite orthotics. | Addresses the deforming force of gastrocnemius contracture contributing to hindfoot valgus and forefoot abduction. Improves midfoot stability and reduces stress on medial soft tissues. |
| Chronic Metatarsalgia/Hallux Valgus | Positive Silfverskiöld test; Forefoot pain or deformity exacerbated by equinus, unresponsive to conservative care; Increased pressure under the metatarsal heads. | Redistributes forefoot pressure, alleviating metatarsalgia. May reduce the deforming forces contributing to hallux valgus and lesser toe deformities, potentially preventing recurrence after corrective osteotomies. |
| Achilles Tendinopathy | Positive Silfverskiöld test; Non-insertional or insertional Achilles tendinopathy refractory to conservative management; Mid-substance tendinosis with associated equinus. | Reduces chronic tension on the Achilles tendon unit, promoting healing and preventing recurrence of tendinopathy symptoms. |
Non-Operative Management Indications for Gastrocnemius Contracture
| Condition | Specific Criteria | Rationale for Non-Operative Management |
|---|---|---|
| Mild/Asymptomatic Contracture | Positive Silfverskiöld test, but ankle dorsiflexion is ≥0 degrees with knee extended; No current ulcers or significant pre-ulcerative lesions; Minimal or no pain/deformity; Contracture identified incidentally. | Initial management focuses on observation and preventive measures if symptoms are mild or absent. Surgical risks outweigh potential benefits in asymptomatic or mildly symptomatic patients. |
| Early Stage Ulcer/Callus | Initial presentation of a non-infected forefoot ulcer or significant callus, with or without IGC; Limited duration of symptoms; Patient compliant with offloading. | Aggressive non-operative offloading (total contact cast, specialized boot), meticulous wound care, and physical therapy (stretching, strengthening) are the first-line treatments. Surgery is reserved for failed conservative treatment. |
| Compromised Medical Status | Uncontrolled diabetes (HbA1c >8-9%); Severe cardiac, pulmonary, or renal disease; Active systemic infection; Unmanaged coagulopathy. | High surgical risk. Medical optimization is paramount. Address life-threatening conditions or optimize systemic health before considering elective or semi-elective procedures. |
| Inadequate Vascularity | Ankle-Brachial Index (ABI) <0.6, Toe-Brachial Index (TBI) <0.4, or Transcutaneous Oxygen Pressure (TcPO2) <30 mmHg; Clinical signs of severe peripheral arterial disease (rest pain, non-healing wounds); Without prior successful revascularization. | Surgical intervention in the presence of severe ischemia significantly increases the risk of wound healing complications and amputation. Revascularization must be prioritized and successfully achieved before any elective lower extremity surgery. |
| Patient Preference/Compliance | Patient unwilling to undergo surgery; Patient unable to comply with post-operative rehabilitation protocols (e.g., non-weight bearing, physical therapy); Cognitive impairment precluding adherence to post-operative instructions. | Patient autonomy and ability to comply with treatment are crucial for successful outcomes. Alternative non-surgical offloading and accommodative measures should be pursued. |
Contraindications for Gastrocnemius Recession
Absolute and relative contraindications must be carefully considered:
- Global Equinus Contracture: If the Silfverskiöld test is negative (i.e., dorsiflexion is restricted with both knee extended and flexed), an isolated gastrocnemius recession will be insufficient. A more extensive Achilles tendon lengthening or Z-plasty may be required, depending on the severity and specific structures involved.
- Severe Peripheral Arterial Disease (PAD): Uncorrected, severe PAD (e.g., ABI <0.6, TcPO2 <30 mmHg) is a contraindication due to significantly increased risk of wound dehiscence, infection, and limb loss. Revascularization must precede any elective or semi-elective foot surgery.
- Active Infection: Active osteomyelitis or deep soft tissue infection must be thoroughly debrided and controlled with appropriate antibiotics before performing gastrocnemius recession. This is typically addressed as a staged procedure.
- Uncontrolled Diabetes: Poor glycemic control (HbA1c consistently >8-9%) significantly impairs wound healing and increases infection risk. Optimization is essential.
- Fixed Deformity: If the equinus deformity is fixed and irreducible even with the knee flexed, suggesting chronic contracture involving all posterior structures (capsule, ligaments), then gastrocnemius recession alone may not achieve the desired correction, and more extensive arthroplasty or fusion may be needed.
- Acute Charcot Neuroarthropathy: While IGC release can be beneficial in stable Charcot, performing it during the acute, inflammatory phase (Eichenholtz Stage I) can destabilize the foot and exacerbate bone destruction.
- Severe Calf Muscle Weakness: In patients with pre-existing significant calf weakness, gastrocnemius recession could further compromise push-off strength and gait.
- Non-Ambulatory Patients: If the patient is non-ambulatory and increased ankle dorsiflexion will not improve function, reduce pressure, or aid in bracing/orthosis fitting, the risks of surgery may outweigh the benefits.
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential to ensure a safe and successful outcome, particularly in patients with complex medical comorbidities commonly associated with foot ulcers.
Clinical Evaluation
-
Comprehensive History:
- Medical Comorbidities: Diabetes (type, duration, control, complications like neuropathy, nephropathy, retinopathy), peripheral vascular disease, cardiac disease, autoimmune disorders.
- Ulcer History: Location, duration, previous treatments (offloading, wound care), recurrence rate, history of infection or osteomyelitis.
- Functional Limitations: Pain, difficulty with ambulation, shoe wear issues.
- Social History: Smoking, alcohol use, social support for post-operative care.
- Medications: Anticoagulants, steroids, immunosuppressants.
-
Thorough Physical Examination:
- Vascular Assessment: Palpation of pedal pulses (dorsalis pedis, posterior tibial), capillary refill time, skin temperature, presence of rubor. Ankle-Brachial Index (ABI) and Toe-Brachial Index (TBI) are crucial. Transcutaneous Oxygen Pressure (TcPO2) measurement is highly recommended, especially in diabetic patients, to assess microcirculatory status. If vascular compromise is suspected, referral for vascular surgery consultation and imaging (angiography) is mandatory.
- Neurological Assessment: Semmes-Weinstein monofilament testing for protective sensation, vibratory sense (128-Hz tuning fork), pinprick, light touch, proprioception. Motor function assessment (foot intrinsics, ankle dorsi- and plantarflexors).
-
Musculoskeletal Examination:
- Silfverskiöld Test: Essential to confirm isolated gastrocnemius contracture.
- Range of motion of the ankle, subtalar, and midfoot joints.
- Foot alignment and deformities (e.g., pes planus, pes cavus, hallux valgus, hammer toes, Charcot changes).
- Assessment of plantar calluses, their location, and correlation with ulcer sites.
- Gait analysis to identify compensatory mechanisms.
- Wound Assessment: Size, depth, location, presence of granulation tissue, signs of infection, surrounding erythema, induration, drainage. Probing to bone to rule out osteomyelitis.
Imaging Studies
-
Weight-Bearing Radiographs:
AP, lateral, and oblique views of the foot and ankle are essential to assess:
- Bony alignment, joint spaces.
- Presence of Charcot neuroarthropathy (fragmentation, dislocation, osteolysis).
- Signs of osteomyelitis (cortical erosion, periosteal reaction, sequestrum).
- Degenerative changes.
- Magnetic Resonance Imaging (MRI): Indicated if osteomyelitis, deep abscess, or extensive soft tissue infection is suspected. It provides excellent soft tissue contrast.
- Computed Tomography (CT) Scan: Useful for complex bony deformities, detailed assessment of joint destruction, or pre-operative planning for Charcot reconstruction.
Patient Optimization
- Glycemic Control: Optimize blood glucose levels (HbA1c <7%) to reduce infection risk and improve wound healing.
- Nutritional Status: Ensure adequate protein and micronutrient intake, as malnutrition impairs healing.
- Infection Control: Any active soft tissue infection must be treated with appropriate antibiotics, and osteomyelitis debrided, prior to elective recession.
- Wound Management: The ulcer should be debrided, free of necrotic tissue, and ideally showing signs of granulation. Advanced wound care techniques may be employed pre-operatively.
- Vascular Optimization: If PAD is identified, revascularization must be performed and successful before proceeding with gastrocnemius recession.
Informed Consent
A comprehensive discussion with the patient is crucial, covering:
* The nature of the contracture and its role in ulceration.
* The surgical procedure, expected outcomes, and potential benefits (ulcer healing, recurrence prevention).
* Potential risks: nerve injury (sural nerve), bleeding, infection, wound healing problems, overcorrection (weakness), undercorrection (recurrence), DVT, CRPS, persistent pain, need for further surgery.
* Alternatives to surgery: continued offloading, bracing, physical therapy.
* The importance of post-operative adherence to rehabilitation and offloading protocols.
Patient Positioning and Anesthesia
- Anesthesia: A combination of regional anesthesia (e.g., popliteal block) and general anesthesia is often preferred. Regional blocks provide excellent post-operative pain control and reduce systemic analgesic requirements.
-
Patient Positioning:
- Prone Position: This is the most common position, offering excellent exposure to the posterior calf. The knee can be easily flexed to assess the degree of dorsiflexion.
- Supine Position: Less common for open techniques but may be used for endoscopic approaches or if prone positioning is contraindicated due to other medical conditions. Requires meticulous positioning and draping to access the posterior calf.
- Tourniquet: A thigh tourniquet is routinely used to provide a bloodless field, typically inflated to 250-300 mmHg or 100 mmHg above systolic blood pressure.
- Preparation and Draping: Standard sterile preparation from above the knee to the toes. Draping should allow for knee flexion and ankle manipulation for intraoperative assessment of dorsiflexion. The unaffected leg should be padded and positioned to prevent pressure injuries.
Detailed Surgical Approach / Technique
Several techniques exist for gastrocnemius recession, broadly categorized as proximal (e.g., Strayer) or distal (e.g., Vulpius, Baker, endoscopic). The choice often depends on surgeon preference, specific patient factors, and desired extent of lengthening. The goal is to lengthen the gastrocnemius aponeurosis while preserving the soleus and avoiding over-lengthening.
Open Gastrocnemius Recession (Modified Strayer Technique)
This technique involves a proximal release of the gastrocnemius aponeurosis, maintaining the integrity of the gastrocnemius muscle belly and the soleus. It is a reliable and widely adopted method.
-
Incision: A longitudinal incision, typically 6-8 cm in length, is made over the posteromedial aspect of the calf, approximately 2-3 cm medial to the midline of the calf and distal to the popliteal crease. The incision should be centered over the junction of the gastrocnemius and Achilles tendon, usually about 10-15 cm proximal to the calcaneal insertion of the Achilles. This location minimizes the risk to the sural nerve (which is more lateral) and small saphenous vein (variable course but often more medial).
-
- Surgical planning often includes marking anatomical landmarks and proposed incision lines pre-operatively to ensure optimal exposure and avoid neurovascular structures.
-
-
Superficial Dissection:
- The skin and subcutaneous tissues are incised.
- Care is taken to identify and ligate or coagulate any superficial veins.
- The fascia of the superficial posterior compartment is identified. The sural nerve typically courses more laterally in the calf, away from this incision. The small saphenous vein, if present in the field, should be identified and protected or ligated if necessary.
-
Identification of Gastrocnemius Aponeurosis and Soleus:
- The deep fascia is incised longitudinally. This exposes the triceps surae complex.
- The surgeon palpates the transition zone from the muscular belly of the gastrocnemius to its broad aponeurosis.
- The gastrocnemius aponeurosis is then carefully separated from the underlying soleus muscle fascia. This can be achieved by blunt dissection using a finger or a blunt instrument. The cleavage plane is usually evident. It is crucial to ensure the soleus muscle fibers are visualized underneath the gastrocnemius aponeurosis to confirm correct identification. The soleus fascia must remain intact.
-
Gastrocnemius Aponeurosis Release:
- With the knee extended, the ankle is brought into maximum dorsiflexion, placing tension on the gastrocnemius aponeurosis.
- A transverse incision is made through the gastrocnemius aponeurosis. This incision should be complete, extending from medial to lateral across the width of the aponeurosis.
- Crucially, the underlying soleus fascia must be meticulously preserved . This prevents over-lengthening and protects the neurovascular structures that lie deep to the soleus. A Metzenbaum scissors or scalpel can be used, with the tip elevated to avoid the soleus.
- Once the aponeurosis is fully divided, a visible gap (typically 1-3 cm) will appear as the gastrocnemius muscle retracts proximally, and the ankle is gently dorsiflexed. This gap indicates successful lengthening.
-
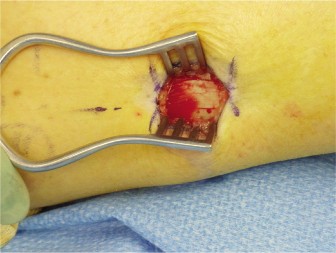
- Intraoperative view demonstrating the completed transverse tenotomy of the gastrocnemius aponeurosis, revealing the underlying intact soleus fascia and the created gap that allows for increased ankle dorsiflexion.
-
Intraoperative Assessment:
- After the release, the knee is again extended, and passive ankle dorsiflexion is re-assessed. The goal is to achieve 5-10 degrees of neutral dorsiflexion with the knee extended. Overcorrection (excessive dorsiflexion) should be avoided as it can lead to calcaneal gait and weakness.
-
Closure:
- Adequate hemostasis is achieved.
- The deep fascia is typically not closed, or only loosely approximated if under no tension, to prevent compartment syndrome.
- Subcutaneous tissues are closed with absorbable sutures.
- Skin is closed with non-absorbable sutures or staples.
- A sterile dressing is applied, followed by a short-leg splint or cast in slight dorsiflexion.
Endoscopic Gastrocnemius Recession
This minimally invasive technique offers advantages such as smaller incisions, potentially less pain, and faster recovery. It typically involves two small portals and endoscopic visualization. While gaining popularity, it requires specific equipment and expertise.
Other Open Techniques (Vulpius, Baker, Baumann)
These techniques typically involve a V-Y lengthening or a tongue-in-groove release of the distal gastrocnemius aponeurosis or a portion of the Achilles tendon itself (for combined gastrocnemius and soleus lengthening). While effective, they may carry a slightly higher risk of over-lengthening if not performed precisely. For isolated gastrocnemius contracture, the Strayer technique or its modifications are generally preferred.
Key Surgical Principles:
- Protect Neurovascular Structures: The sural nerve and small saphenous vein are the primary structures at risk. Careful blunt dissection and anatomical awareness are paramount.
- Avoid Over-Lengthening: Always preserve the soleus fascia. Over-lengthening can result in significant weakness of plantarflexion, calcaneal gait, and functional impairment.
- Achieve Adequate Correction: The goal is to normalize ankle biomechanics, which means achieving 5-10 degrees of passive ankle dorsiflexion with the knee extended.
- Meticulous Hemostasis: Especially important in diabetic and vascularly compromised patients, to minimize hematoma formation and wound complications.
Complications & Management
While gastrocnemius recession is generally considered a safe procedure, like any surgical intervention, it carries potential risks and complications. These can be categorized into general surgical complications and those specific to gastrocnemius lengthening.
General Surgical Complications
-
Infection (0.5-5%):
Risk factors include diabetes, immunosuppression, poor vascularity, and prolonged surgical time.
- Management: Superficial infections may respond to oral antibiotics and local wound care. Deep infections (e.g., fasciitis, osteomyelitis) require surgical debridement, intravenous antibiotics, and potentially flap coverage.
-
Bleeding/Hematoma (1-3%):
More common in patients on anticoagulants or with underlying coagulopathies.
- Management: Meticulous hemostasis intraoperatively. Post-operative compression dressings. Large or expanding hematomas may require surgical evacuation.
-
Wound Dehiscence (2-8%):
Higher risk in diabetic patients, those with poor vascularity, or excessive tension on the wound.
- Management: Local wound care, offloading, serial debridement, vacuum-assisted closure (VAC), or reconstructive surgery (e.g., skin grafting or local flap) for large defects.
- Pain: Post-operative pain is expected but should be well-controlled with analgesia. Persistent or disproportionate pain may indicate a complication.
-
Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE) (0.5-2%):
Risk factors include immobilization, obesity, history of DVT, and hypercoagulable states.
- Management: Prophylactic anticoagulation (LMWH, fondaparinux) and mechanical prophylaxis (compression stockings, pneumatic compression devices). Treatment involves therapeutic anticoagulation.
Specific Complications of Gastrocnemius Recession
| Complication | Incidence | Management / Salvage Strategies |
|---|---|---|
| Sural Nerve Injury | Neurapraxia: 5-15% (transient paresthesia/dysesthesia) | Neurapraxia: Expectant management, neuropathic pain medications (gabapentin, pregabalin). Sensory recovery often occurs within weeks to months. |
| Transection/Neuroma: <1% (permanent sensory loss, painful neuroma) | Neuroma: Surgical excision of neuroma, nerve repair (if deficit immediately recognized), or nerve capping. Chronic pain management strategies. Careful dissection and anatomical awareness are key to prevention. | |
| Undercorrection / Recurrence | 5-10% | Management: Persistent equinus deformity and/or recurrent forefoot ulcers. Non-operative: repeat stretching, orthotics, bracing. Operative: revision gastrocnemius recession or more extensive Achilles lengthening (e.g., Z-plasty) if residual contracture involves soleus or other posterior structures. |
| Overcorrection / Weakness | 1-5% | Symptoms: Calcaneal gait, difficulty with push-off, weakness in plantarflexion, pain in the heel/hindfoot. Less common with isolated gastrocnemius recession if soleus is preserved. |
| Management: Physical therapy to strengthen remaining plantarflexors. Orthotics (heel lift). In severe cases, surgical reconstruction (e.g., tendon transfer) to augment plantarflexion, although this is rare for IGC release. Prevention is paramount by preserving soleus and avoiding excessive lengthening. | ||
| Wound Healing Problems | 5-10% (especially in diabetics with poor vascularity) | Management: Debridement, negative pressure wound therapy (NPWT), careful glucose control, vascular optimization, offloading. May require skin grafting or local flap coverage. Early recognition and aggressive management are crucial to prevent progression to deeper infection or amputation. |
| Complex Regional Pain Syndrome (CRPS) | <1% | Symptoms: Disproportionate pain, swelling, skin changes, allodynia. |
| Management: Multidisciplinary approach involving pain management specialists. Physical therapy, sympathetic nerve blocks, neuromodulation, pharmacotherapy (NSAIDs, gabapentinoids, tricyclic antidepressants). Early diagnosis and aggressive treatment improve prognosis. | ||
| Achilles Tendon Rupture | Rare | Mechanism: Possible if soleus fascia is inadvertently incised or weakened during a proximal gastrocnemius release, or if the Achilles tendon itself is compromised. |
| Management: Surgical repair of the Achilles tendon, followed by structured rehabilitation. |
Careful patient selection, meticulous surgical technique, and vigilant post-operative monitoring are essential to minimize the risk of these complications. Comprehensive patient education regarding potential risks and expected recovery is also vital.
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is critical for maximizing the benefits of gastrocnemius recession, achieving functional outcomes, and preventing recurrence of contracture and ulceration. The protocol must be individualized based on the patient's comorbidities, baseline functional status, and wound healing potential.
Immediate Post-Operative Phase (Day 0 - Week 2-4)
-
Immobilization:
- Short-leg posterior splint or cast: Applied immediately post-surgery, holding the ankle in slight dorsiflexion (typically 0-5 degrees) and the knee slightly flexed if possible (for optimal gastrocnemius stretch). This position helps maintain the surgical lengthening and protects the repair site.
- Duration: Typically maintained for 2-4 weeks.
-
Weight-Bearing:
- Non-weight bearing (NWB): Usually strictly non-weight bearing on the operative limb for the initial 2-4 weeks to protect the wound and allow for initial healing. Crutches, walker, or knee scooter are used.
-
Pain Management:
- Administer appropriate analgesics (NSAIDs, acetaminophen, opioids as needed). Regional blocks significantly aid early pain control.
-
Wound Care:
- Keep the surgical site clean and dry. Monitor for signs of infection (erythema, swelling, discharge, fever).
- First dressing change usually occurs at 1-2 weeks. Sutures/staples are typically removed at 2-3 weeks, provided the wound is healing well.
-
Edema Control:
- Elevation of the limb above heart level.
- Intermittent cryotherapy (ice packs over the cast/splint).
-
Early Motion (Non-operative joints):
- Gentle, active range of motion (ROM) exercises for the toes and knee (if not restricted by splint) to prevent stiffness and improve circulation.
Early Mobilization Phase (Weeks 2-4 to Week 6-8)
-
Transition from Immobilization:
- Once the surgical wound is well-healed and pain is controlled, the splint/cast is removed.
- Transition to a removable controlled ankle motion (CAM) boot (walker boot) set at neutral or slight dorsiflexion.
-
Progressive Weight-Bearing:
- Initiate gradual, protected weight-bearing in the CAM boot, starting with partial weight-bearing (PWB) and progressing to full weight-bearing (FWB) over 2-4 weeks, as tolerated.
-
Physical Therapy (Focus on ROM and gentle stretching):
- Ankle ROM: Gentle active and passive ankle dorsiflexion and plantarflexion within the pain-free range. The goal is to regain functional dorsiflexion.
- Gastrocnemius Stretching: Begin gentle gastrocnemius stretching, focusing on exercises with the knee extended (e.g., wall stretches, stair stretches).
- Soleus Stretching: Incorporate soleus stretches (knee flexed).
- Joint Mobilization: Gentle mobilization of the ankle and subtalar joints if stiffness is present.
- Initiate Strengthening (Isometric): Isometric plantarflexion exercises to activate the triceps surae without full load.
Intermediate Rehabilitation Phase (Weeks 6-8 to Week 12)
-
Transition to Footwear:
- Once sufficient strength and ROM are achieved, transition from the CAM boot to supportive, well-cushioned, and spacious athletic shoes. Custom orthotics may be prescribed to optimize foot mechanics and offload high-pressure areas, especially in neuropathic feet.
-
Progressive Strengthening:
- Isotonic Exercises: Heel raises (initially bilateral, then unilateral), resistance band exercises for plantarflexion, dorsiflexion, inversion, and eversion.
- Proprioception and Balance: Single-leg stance, balance board exercises to improve neuromuscular control.
-
Gait Training:
- Focus on normalizing gait pattern, emphasizing full stance phase and avoiding premature heel-off. Address any compensatory movements.
-
Continued Stretching:
- Maintain an aggressive home stretching program for gastrocnemius and soleus.
Advanced Rehabilitation Phase (Beyond Week 12)
-
Return to Activity:
- Gradual return to pre-injury or desired activities, avoiding high-impact activities initially.
- Progress to sport-specific drills if applicable.
-
Maintenance Program:
- Long-term adherence to a stretching and strengthening program is crucial to prevent recurrence of contracture.
- Lifelong Offloading: For patients with neuropathy or a history of ulcers, continuous vigilance regarding foot care, appropriate footwear, and custom orthotics or accommodative devices is mandatory to prevent recurrent ulceration.
-
Regular Follow-up:
- Periodic clinical assessment by the orthopedic surgeon and wound care specialist to monitor for recurrent contracture, assess gait, and screen for new or recurrent ulcers.
Throughout the rehabilitation process, close collaboration between the surgeon, physical therapist, and wound care team is paramount. Patients with neuropathy and diabetes require particular attention to skin integrity and careful progression to avoid new ulcer formation during activity. The primary goal is not just to lengthen the gastrocnemius but to restore functional ankle mechanics and prevent future limb-threatening complications.
Summary of Key Literature / Guidelines
The role of isolated gastrocnemius contracture in various foot and ankle pathologies, including foot ulceration, has gained increasing recognition in orthopedic literature over the past two decades. While historically a procedure primarily for pediatric deformities, its application in adult reconstructive foot and ankle surgery is now well-established.
Evidence Supporting Gastrocnemius Recession for Foot Ulcers
Several landmark studies and systematic reviews have demonstrated the efficacy of gastrocnemius recession, particularly in the diabetic neuropathic foot with recalcitrant plantar forefoot ulcers.
-
Diabetic Foot Ulcer Healing and Prevention:
- Lin et al. (2009, 2010): Early studies by Lin and colleagues highlighted the significant role of gastrocnemius contracture in diabetic forefoot ulceration and demonstrated that gastrocnemius recession effectively reduces plantar pressures, leading to improved ulcer healing rates and decreased recurrence. Their prospective studies showed a significant reduction in peak plantar pressures post-operatively, correlating with ulcer closure and prevention of new ulcers.
- Systematic Reviews and Meta-analyses: Numerous systematic reviews, such as those by Cychosz et al. (2018) and others, have compiled evidence, largely supporting the effectiveness of gastrocnemius recession in reducing forefoot pressures, improving ulcer healing, and lowering recurrence rates in diabetic patients with equinus deformity. These studies consistently report high rates of ulcer closure (often >80-90%) and low recurrence rates (below 20-30%) at medium-term follow-up.
- Mechanism Confirmation: Pressure-sensing studies (e.g., using F-Scan systems) consistently show a measurable and significant reduction in peak plantar pressures under the metatarsal heads following gastrocnemius recession, directly substantiating the biomechanical rationale for the procedure.
-
Charcot Neuroarthropathy:
- Gastrocnemius contracture is a common co-morbidity in Charcot neuroarthropathy and contributes to the progression of deformity, especially rocker-bottom foot, and ulceration.
- Pinzur et al. (2009): Studies by Pinzur and others have advocated for gastrocnemius recession as an adjunct to Charcot foot reconstruction or as a standalone procedure for stable Charcot deformities with equinus, demonstrating its utility in offloading the forefoot and midfoot and preventing ulceration. It improves the ability to fit custom footwear and orthotics.
-
Other Foot Pathologies:
- The literature also supports the use of gastrocnemius recession for chronic metatarsalgia, hallux valgus, and adult acquired flatfoot deformity where gastrocnemius contracture contributes to pathology by increasing forefoot load or pronation. While not directly related to ulcer healing, these applications underscore the broad biomechanical impact of IGC.
Current Guidelines and Recommendations
- Multidisciplinary Approach: Consensus guidelines from organizations like the American Diabetes Association (ADA), the International Working Group on the Diabetic Foot (IWGDF), and the Wound Healing Society consistently emphasize a multidisciplinary approach to diabetic foot care. This includes vascular assessment, glycemic control, aggressive wound debridement, infection management, and meticulous offloading.
- Surgical Correction of Deformity: Surgical correction of foot deformities, including equinus contracture, is recommended for recalcitrant ulcers or for prevention in high-risk patients who have failed conservative measures. Gastrocnemius recession is explicitly mentioned as an effective strategy for correcting isolated gastrocnemius contracture.
- Evidence Level: While many studies on gastrocnemius recession are prospective cohort studies or case series, the consistency of positive outcomes and the clear biomechanical rationale provide strong support for its use (often considered Level III or IV evidence, trending towards Level II with larger cohort studies). Randomized controlled trials directly comparing gastrocnemius recession to non-operative management for ulcer healing are more challenging due to ethical considerations and patient heterogeneity, but existing evidence is compelling.
Areas of Ongoing Research and Debate
- Optimal Technique: While open Strayer is well-established, endoscopic techniques are gaining favor due to perceived lower morbidity. Comparative studies are ongoing to definitively establish superior outcomes or specific indications for each.
- Patient Selection Criteria: Refinement of precise patient selection criteria, beyond the Silfverskiöld test, could further optimize outcomes. For instance, quantitative plantar pressure analysis pre-operatively may help identify optimal candidates.
- Long-Term Outcomes: More long-term follow-up studies (beyond 5 years) are needed to assess the durability of correction, ulcer recurrence rates, and functional outcomes, particularly in the context of progressive neuropathy.
- Cost-Effectiveness: Research into the cost-effectiveness of prophylactic gastrocnemius recession versus long-term conservative management and repeated ulcer treatments would be valuable for healthcare policy.
- Pediatric vs. Adult Contracture: While the principles are similar, differences in tissue properties and growth potential between pediatric and adult gastrocnemius contractures necessitate distinct considerations and outcomes assessment.
In conclusion, the academic literature robustly supports the diagnostic importance of identifying isolated gastrocnemius contracture in patients with plantar forefoot ulcers, especially those with diabetes and neuropathy. Gastrocnemius recession is an effective and safe surgical intervention that significantly reduces plantar pressures, promotes ulcer healing, and prevents recurrence, thereby playing a vital role in limb preservation strategies. Continued research will further refine techniques, patient selection, and long-term management strategies.
