Introduction & Epidemiology
Hallux rigidus (HR) represents a progressively debilitating degenerative arthritic condition affecting the first metatarsophalangeal (MTP) joint, characterized by progressive stiffness, pain, and restricted range of motion, particularly dorsiflexion. It is the second most common arthritic condition of the foot, surpassed only by ankle osteoarthritis, and the most common disorder of the great toe. The term "rigidus" accurately reflects the cardinal clinical feature of reduced or absent joint motion.
The pathophysiology involves a complex interplay of genetic predisposition, biomechanical factors, and traumatic events. Repetitive microtrauma or a single macrotraumatic event can initiate cartilage degeneration. Biomechanical aberrations such as metatarsus primus elevatus, a long first metatarsal, or hypermobility of the first ray are frequently implicated in altering normal joint kinematics, leading to increased dorsal compressive forces during gait and subsequent cartilage wear. Osteophyte formation, particularly dorsally, is a hallmark of the condition and contributes significantly to the mechanical blockade of dorsiflexion, leading to the characteristic pain with push-off during ambulation.
Epidemiological data indicate a prevalence of HR ranging from 2.5% to 10% in the adult population, with increasing incidence in individuals over 50 years of age. While some studies suggest a slight male predominance, others report equal distribution or a marginal female preponderance, particularly in older age groups. The condition can be bilateral in a significant percentage of patients (up to 70%), underscoring a potential systemic or multifactorial etiology beyond isolated trauma. Early diagnosis and appropriate staging are crucial for guiding treatment decisions and optimizing patient outcomes. The Coughlin and Shurnas classification system, which grades the severity of HR from 0 to 4 based on clinical and radiographic findings (ranging from minimal dorsal osteophytes with preserved joint space to severe pan-articular degenerative changes with complete joint effacement), serves as a widely accepted framework for this purpose. The primary objective of any therapeutic intervention, whether conservative or surgical, is to alleviate pain, restore functional range of motion, and improve the patient's quality of life.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the first MTP joint is paramount for effective treatment of hallux rigidus.
First MTP Joint Anatomy
The first MTP joint is a diarthrodial condyloid joint formed by the articulation of the convex head of the first metatarsal and the concave base of the proximal phalanx. The articular cartilage on these surfaces is typically thicker than in other joints, designed to withstand significant compressive and shear forces during gait.
*
Capsule and Ligaments:
The joint is enveloped by a fibrous capsule, which is reinforced by medial and lateral collateral ligaments. These ligaments provide mediolateral stability.
*
Plantar Plate Complex:
Ventral to the joint lies the fibrocartilaginous plantar plate, a critical structure for stability and load bearing. It originates from the metatarsal neck and inserts into the base of the proximal phalanx. Embedded within the plantar plate are the medial and lateral sesamoid bones, which articulate with two distinct grooves on the plantar aspect of the first metatarsal head. The sesamoids act as fulcrums for the flexor hallucis brevis (FHB) muscle, increasing its mechanical advantage for plantarflexion and protecting the flexor hallucis longus (FHL) tendon. The FHL tendon runs in a groove between the sesamoids.
*
Musculature:
*
Dorsiflexors:
The extensor hallucis longus (EHL) and extensor hallucis brevis (EHB) tendons are located dorsally. EHL originates from the fibula and inserts on the distal phalanx, primarily dorsiflexing the hallux at the MTP and IP joints. EHB originates from the calcaneus and inserts into the base of the proximal phalanx, aiding in MTP dorsiflexion.
*
Plantarflexors:
The FHL, originating from the fibula, inserts on the distal phalanx and is a powerful plantarflexor. The FHB, originating from the cuboid and lateral cuneiform, divides into two heads inserting into the medial and lateral sesamoids and then onto the proximal phalanx base, providing strong MTP plantarflexion.
*
Intrinsic Muscles:
Abductor hallucis (medial, contributes to medial stability), adductor hallucis (oblique and transverse heads, lateral, stabilizes the MTP joint).
*
Neurovascular Structures:
The medial dorsal cutaneous nerve (a branch of the superficial fibular nerve) typically courses dorsomedially, posing a risk during dorsal incisions. The medial plantar nerve provides sensation to the plantar aspect of the great toe. The dorsalis pedis artery and its branches supply the dorsal aspect, while the medial and lateral plantar arteries supply the plantar aspect.
Biomechanics of the First MTP Joint
The first MTP joint plays a pivotal role in the propulsion phase of gait, undergoing significant dorsiflexion.
*
Gait Cycle Requirements:
During normal ambulation, the first MTP joint requires approximately 60-70 degrees of dorsiflexion during terminal stance (the "toe-off" phase) for efficient push-off. Activities of daily living generally require at least 30 degrees of pain-free dorsiflexion. Restriction of this motion leads to compensatory mechanisms, including early heel-off, decreased stride length, increased pressure under the lesser metatarsals (transfer metatarsalgia), and altered kinematics at the ankle, knee, and hip.
*
Windlass Mechanism:
The first MTP joint is integral to the "windlass mechanism" described by Hicks. As the metatarsophalangeal joints dorsiflex during propulsion, the plantar fascia becomes taut, shortening the arch and converting the foot into a rigid lever for propulsion. Restricted dorsiflexion of the hallux inhibits this mechanism, leading to a less efficient and more painful gait.
*
Pathobiomechanics of Hallux Rigidus:
*
Dorsal Impingement:
The most common cause of restricted dorsiflexion is the formation of dorsal osteophytes on both the metatarsal head and the proximal phalanx. These osteophytes abut during dorsiflexion, causing pain and mechanical blockade.
*
Metatarsus Primus Elevatus:
This condition, characterized by a structurally elevated first metatarsal relative to the lesser metatarsals, leads to increased dorsal compression during weight-bearing, predisposing the joint to HR. This effectively reduces the functional arc of dorsiflexion by requiring a greater range of motion to reach the ground during propulsion.
*
Cartilage Degeneration:
Chronic dorsal impingement and altered joint loading patterns lead to progressive articular cartilage degradation, joint space narrowing, and subchondral sclerosis, culminating in end-stage osteoarthritis.
Indications & Contraindications
The decision-making process for managing hallux rigidus involves a careful evaluation of the patient's symptoms, functional limitations, radiographic findings, and expectations. Treatment strategies are generally categorized into non-operative and operative approaches.
Non-Operative Indications
Non-operative management is typically the first-line treatment, especially for early stages of hallux rigidus (Coughlin and Shurnas Grade 0, 1, and often Grade 2).
*
Mild to Moderate Symptoms:
Patients presenting with intermittent pain, minimal functional impairment, or primarily activity-related pain.
*
Early Radiographic Changes:
Cases with minimal dorsal osteophytes and preserved joint space (Grade 0-1), or moderate osteophytes with minimal to moderate joint space narrowing (Grade 2).
*
Patient Preference:
Individuals who are unwilling or medically unfit for surgical intervention.
*
Initial Management:
All patients, regardless of severity, should typically undergo a trial of conservative management unless they present with end-stage disease and intractable pain.
Non-Operative Treatment Modalities:
*
Activity Modification:
Avoiding activities that exacerbate pain, such as running or prolonged standing.
*
Footwear Modification:
Shoes with a stiff sole, rocker-bottom sole, or wide toe box can reduce motion at the MTP joint and alleviate dorsal impingement.
*
Orthoses:
Custom or off-the-shelf orthotics, such as a Morton's extension (a rigid insert under the hallux to limit dorsiflexion), can be effective.
*
Non-Steroidal Anti-Inflammatory Drugs (NSAIDs):
Oral or topical NSAIDs to manage pain and inflammation.
*
Corticosteroid Injections:
Intra-articular corticosteroid injections can provide temporary pain relief, reduce inflammation, and may have diagnostic utility, but are not curative and typically lose efficacy over time. Repeated injections are discouraged due to potential cartilage damage.
*
Physical Therapy:
Modalities focused on improving range of motion, strengthening intrinsic foot muscles, and optimizing gait mechanics.
Operative Indications
Surgical intervention is considered when conservative measures have failed to provide adequate pain relief and functional improvement, or in cases of advanced disease. The choice of surgical procedure is guided by the Coughlin and Shurnas classification, patient age, activity level, and concomitant pathology.
- Failure of Conservative Management: Persistent, debilitating pain and functional limitation despite a comprehensive trial of non-operative treatments (typically 3-6 months).
- Progressive Disease: Radiographic evidence of significant degenerative changes (Coughlin and Shurnas Grade 2-4) that are expected to worsen without intervention.
-
Specific Grade-Based Indications:
- Grade 1-2: Often amenable to motion-preserving procedures such as cheilectomy, with or without an osteotomy (e.g., Moberg osteotomy).
- Grade 2-3: Cheilectomy combined with an osteotomy (e.g., proximal phalangeal or metatarsal osteotomy) may be indicated. Cartilage restoration techniques (e.g., microfracture, OATS) may be considered for focal defects in younger patients.
- Grade 3-4: Patients typically require joint-altering procedures such as interposition arthroplasty, hemiarthroplasty, or arthrodesis.
- Grade 4: Arthrodesis (fusion) of the first MTP joint is often considered the gold standard for end-stage hallux rigidus due to its reliable pain relief and high success rates.
Contraindications
General and relative contraindications to foot surgery apply.
*
Absolute Contraindications:
* Active infection (local or systemic).
* Severe peripheral vascular disease with compromised tissue perfusion.
* Uncontrolled diabetes mellitus with high risk of wound complications or neuropathy.
* Acute Charcot neuroarthropathy.
* Poor skin integrity or active dermatological conditions in the operative field.
*
Relative Contraindications:
* Unrealistic patient expectations regarding surgical outcomes or recovery.
* Significant osteopenia or osteoporosis (may affect fixation strength for osteotomies or fusions).
* Severe generalized rheumatoid arthritis with systemic involvement (increases risk of complications).
* Severe obesity (increased risk of wound healing issues, DVT/PE).
* Neuropathic foot (increased risk of recurrence, delayed healing, or complications, particularly for motion-sparing procedures).
Table 1: Operative vs. Non-Operative Indications for Hallux Rigidus
| Feature/Treatment | Non-Operative Indications | Operative Indications |
|---|---|---|
| Coughlin & Shurnas Grade | Grade 0, 1, early 2 | Grade 2, 3, 4 (and failure of conservative care for Grade 2) |
| Pain Level | Mild to moderate, intermittent, activity-related | Persistent, debilitating, functional limitation despite conservative care |
| Functional Limitation | Minimal | Significant impairment of daily activities, gait disturbance |
| Radiographic Findings | Minimal dorsal osteophytes, preserved joint space | Moderate to severe osteophytes, joint space narrowing, subchondral sclerosis, cyst formation, effacement |
| Response to Conservative Treatment | Initial trial or good response to modalities | Failure of an adequate trial of conservative measures |
| Patient Age/Activity Level | Any age, particularly lower demand patients | Any age, particularly active patients with significant impairment |
| Surgical Goal | Pain relief, improved ROM, restore function | Pain relief, improved ROM, restore function (with consideration for joint preservation vs. fusion) |
| General Health | Good candidates for non-operative care | Medically fit for surgery; comorbidities optimized |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential for achieving optimal outcomes in first MTP joint surgery. This process encompasses comprehensive patient evaluation, appropriate imaging, and detailed surgical strategy.
Clinical Assessment
- History: Obtain a detailed history focusing on pain characteristics (location, intensity, aggravating/alleviating factors, duration, nocturnal pain), functional limitations (difficulty with shoe wear, walking, recreational activities), and previous treatments (injections, orthotics, physical therapy) and their efficacy. Enquire about any history of trauma, other foot conditions (e.g., hallux valgus, lesser metatarsal pain), systemic diseases (e.g., rheumatoid arthritis, diabetes), and neurovascular comorbidities.
-
Physical Examination:
- Inspection: Assess for swelling, erythema, skin lesions, callosities, and any associated foot deformities (e.g., hallux valgus, hammer toes, pes planus).
- Palpation: Identify areas of tenderness, particularly around the dorsal aspect of the first MTP joint and the metatarsal head. Assess for osteophytes.
- Range of Motion (ROM): Actively and passively assess dorsiflexion and plantarflexion of the first MTP joint. Perform the "dorsiflexion grind test" (axial compression with dorsiflexion) to elicit pain, indicating articular degeneration. Compare with the contralateral foot. Normal dorsiflexion is typically 60-90 degrees.
- Gait Analysis: Observe the patient's gait for any compensatory mechanisms, such as premature heel-off or pronation, which may indicate restricted MTP motion.
- Neurovascular Status: Assess light touch sensation in the webspaces, particularly the first, to evaluate for nerve impingement, and palpate pedal pulses.
Imaging
-
Weight-Bearing Plain Radiographs:
These are the cornerstone of imaging for hallux rigidus. Standard views include:
- Anteroposterior (AP): Evaluate joint space narrowing, hallux valgus angle, intermetatarsal angle, and metatarsal head morphology.
- Lateral: Crucial for assessing dorsal osteophyte size, joint space, subchondral sclerosis, and the presence of metatarsus primus elevatus. This view is essential for determining the extent of dorsal impingement.
- Oblique: Provides additional views of the joint space and osteophytes, particularly medially and laterally.
- Contralateral views: Useful for comparison, especially if the disease is unilateral or for evaluating pre-existing asymptomatic pathology.
-
Advanced Imaging (Rarely Indicated):
- CT Scan: May be considered in complex cases, for pre-operative planning of arthrodesis (to assess bone stock), or to evaluate for occult fractures or non-union after previous surgery.
- MRI Scan: Rarely necessary for hallux rigidus, but can be useful to assess soft tissue pathology (e.g., synovitis, plantar plate tears) or differentiate osteochondral lesions.
Surgical Planning
- Procedure Selection: Based on the clinical assessment, radiographic staging (Coughlin and Shurnas), patient's age, activity level, and expectations. Discuss the advantages and disadvantages of motion-preserving procedures versus fusion.
- Templating: For procedures involving osteotomies, implant placement (e.g., hemiarthroplasty), or arthrodesis, pre-operative templating on radiographs can aid in selecting appropriate hardware size and optimizing joint positioning.
- Patient Counseling: A thorough discussion of the chosen procedure, expected outcomes, potential complications, rehabilitation protocol, and alternatives is critical. Address patient concerns regarding pain, return to activity, and limitations.
Anesthesia
- General Anesthesia: Provides complete patient immobility and is often chosen for longer or more complex procedures.
- Regional Anesthesia: Spinal or epidural anesthesia offers excellent post-operative pain control and reduced systemic side effects.
- Ankle Block: Can be used as a primary anesthetic for shorter procedures or as an adjunct to general anesthesia for prolonged post-operative analgesia. Often combined with monitored anesthesia care (MAC).
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Tourniquet: A pneumatic tourniquet is typically applied to the proximal thigh or ankle to ensure a bloodless surgical field, enhancing visibility and precision. Tourniquet time must be monitored.
- Leg Holder: A leg holder or sandbag may be used to elevate the operative limb, facilitating access and comfort for the surgeon.
- Padding: Meticulous padding of all pressure points is crucial to prevent nerve compression or skin breakdown.
- Sterile Prep and Drape: The entire lower extremity, from above the knee to the toes, is meticulously prepped with an antiseptic solution and draped in a sterile fashion. A sterile stockinette or U-drape is typically utilized.
Detailed Surgical Approach / Technique
The goal of surgical intervention for hallux rigidus is to alleviate pain, improve or restore functional range of motion, and prevent disease progression. The specific technique employed is dictated by the stage of the disease, patient factors, and surgeon preference. The general principles of aseptic technique, gentle tissue handling, and meticulous hemostasis apply to all procedures.
Dorsomedial Approach
This is the most common approach for accessing the first MTP joint for procedures such as cheilectomy, osteotomies, and arthrodesis.
1.
Incision:
A longitudinal skin incision, approximately 4-6 cm in length, is made over the dorsomedial aspect of the first MTP joint. It is typically centered over the joint, slightly medial to the extensor hallucis longus (EHL) tendon. Care is taken to avoid crossing skin creases perpendicularly to minimize scar contracture.
2.
Skin and Subcutaneous Dissection:
The incision is carried through the skin and subcutaneous tissue. Meticulous dissection is required to identify and protect the branches of the medial dorsal cutaneous nerve, which typically courses dorsomedially over the first MTP joint. Retraction of these nerve branches, often using self-retaining retractors, is critical to prevent iatrogenic injury, which can lead to post-operative numbness or painful neuroma formation. Hemostasis is achieved with bipolar cautery.
3.
Deep Dissection:
The EHL tendon is identified and retracted laterally, away from the operative field. The extensor hallucis brevis (EHB) may also be encountered and can be retracted or carefully incised if necessary. The dorsal capsule of the MTP joint is then exposed.
4.
Capsulotomy:
A longitudinal capsulotomy is performed along the dorsomedial aspect of the joint, extending proximally and distally as needed for adequate exposure.
5.
Exposure:
The capsular flaps are carefully retracted, exposing the dorsal aspect of the first metatarsal head and the base of the proximal phalanx. Dorsal osteophytes are typically immediately visible.
Specific Procedures to "Unlock Motion"
1. Cheilectomy (Dorsal Decompression)
- Indication: Coughlin and Shurnas Grade 1, 2, and occasionally early Grade 3 hallux rigidus, primarily to remove dorsal osteophytes and improve dorsiflexion.
-
Technique:
- After exposure, the dorsal and dorsomedial/dorsolateral osteophytes are identified on both the metatarsal head and the proximal phalanx base.
- Using a small osteotome, rongeur, or a high-speed burr, these osteophytes are systematically resected. The goal is to remove sufficient bone to achieve at least 70-80 degrees of pain-free dorsiflexion intraoperatively.
- Historically, a resection of approximately 20-30% of the dorsal metatarsal head articular surface was advocated to ensure adequate decompression. However, excessive resection can lead to joint instability or shortening. The focus is on clearing the impingement and achieving adequate motion.
- The resected surfaces should be smoothed to prevent further irritation. Any frayed or degenerated synovium is debrided.
- The joint is thoroughly irrigated to remove bone debris.
- The range of motion is meticulously assessed to confirm satisfactory dorsiflexion without impingement.
- Capsular repair is optional; some surgeons prefer not to repair the dorsal capsule tightly to avoid restricting the newly gained dorsiflexion.
-
Closure is performed in layers: subcutaneous tissue, then skin.
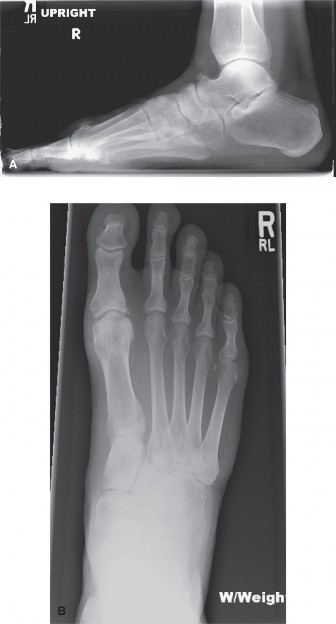
(This image, if depicting osteophyte removal or post-cheilectomy radiograph, would illustrate the primary mechanism of motion restoration in this procedure.)
2. Moberg Osteotomy (Dorsal Wedge Osteotomy of Proximal Phalanx)
- Indication: Often combined with cheilectomy for Grade 1-3 hallux rigidus, particularly when functional hallux limitus persists despite adequate cheilectomy or when a metatarsus primus elevatus is present. It functionally increases dorsiflexion of the hallux by reorienting the proximal phalanx.
-
Technique:
- Performed through the same dorsomedial incision after cheilectomy.
- A transverse or oblique dorsal closing wedge osteotomy is created at the base of the proximal phalanx, approximately 5-7 mm distal to the articular surface. The wedge is typically 2-3 mm wide at its dorsal aspect, with the apex directed plantarly, effectively dorsiflexing the hallux relative to the metatarsal.
- Care is taken to avoid violating the plantar cortex to maintain stability.
- Fixation is typically achieved with a single small K-wire, a headless compression screw (e.g., Acutrak or equivalent), or a small staple, ensuring stable compression of the osteotomy.
- Range of motion is again checked.
- Layered closure.
3. Watermann Osteotomy (Dorsal Wedge Osteotomy of Distal Metatarsal)
- Indication: Less common, but can be considered for patients with metatarsus primus elevatus and mild to moderate hallux rigidus. It shortens and plantarflexes the metatarsal head.
-
Technique:
- A dorsal closing wedge osteotomy is made through the distal first metatarsal shaft, just proximal to the articular cartilage.
- The wedge is removed dorsally, and the metatarsal head is then translated proximally and plantarflexed.
- Fixation is crucial and usually achieved with two small screws or a small plate, providing stable osteosynthesis.
4. Cartilage Restoration Techniques (e.g., Microfracture, OATS, MACI)
- Indication: For younger patients with focal cartilage defects (e.g., osteochondral lesions) associated with early hallux rigidus, where the surrounding cartilage is relatively healthy. Not suitable for diffuse, end-stage arthritis.
- Technique: Involves debridement of the unstable cartilage, followed by microfracture (drilling small holes into the subchondral bone to stimulate fibrocartilage formation) or osteochondral autograft/allograft transplantation (OATS), or autologous matrix-induced chondrogenesis (MACI). Outcomes are variable and depend heavily on patient selection and defect size.
5. Interposition Arthroplasty
- Indication: Coughlin and Shurnas Grade 3-4 hallux rigidus in older, lower-demand patients who wish to preserve some motion and avoid fusion.
-
Technique:
- Resection of diseased articular cartilage and a small amount of subchondral bone from both the metatarsal head and proximal phalanx base.
- The joint surfaces are shaped to accommodate the interposition material.
- A soft tissue interposition graft (e.g., fascia lata autograft, Achilles tendon allograft, fat graft) or a synthetic spacer (e.g., polyetheretherketone (PEEK)) is inserted into the joint space and secured.
- The goal is to maintain motion by preventing bone-on-bone articulation.
- Results are variable, with concerns regarding graft incorporation, spacer migration, and long-term durability.
6. Hemiarthroplasty
- Indication: Similar to interposition arthroplasty, for Grade 3-4 HR, especially in older, less active individuals seeking motion preservation. Replaces one side of the joint.
-
Technique:
- Resection of the diseased articular surface, typically the base of the proximal phalanx, less commonly the metatarsal head.
- A metallic or synthetic implant (e.g., cobalt-chrome, titanium) is then inserted into the prepared bone bed.
- Concerns exist regarding implant loosening, wear of the contralateral cartilage, osteolysis, and long-term implant survival.
7. Arthrodesis (Fusion)
- Indication: The gold standard for Coughlin and Shurnas Grade 4 hallux rigidus, severe painful end-stage arthritis, failed previous motion-preserving procedures, neuropathic joints, or in high-demand patients where predictable pain relief and stability are paramount. It sacrifices motion but provides reliable pain relief.
-
Technique:
- Joint Preparation: The articular cartilage and subchondral bone from both the metatarsal head and the base of the proximal phalanx are completely resected. Various techniques exist, including flat cuts, dome-and-cup reaming, or angled cuts to optimize contact area.
- Positioning: The joint is meticulously positioned. The ideal position for fusion is typically 10-20 degrees of dorsiflexion relative to the plantar aspect of the foot (or 5-10 degrees relative to the first metatarsal shaft), 10-15 degrees of valgus, and slight external rotation. This position facilitates comfortable shoe wear and optimizes the push-off phase of gait despite the loss of motion.
-
Fixation:
Stable, rigid internal fixation is critical to achieve high fusion rates. Common methods include:
- A dorsal locking or non-locking plate with compression screws.
- Two or more crossing compression screws (e.g., 3.0 mm or 3.5 mm).
- Combinations of plates and screws.
- K-wires are sometimes used as temporary fixation or as primary fixation in non-compliant patients or poor bone quality (though less rigid).
- Bone Graft: If there are significant bone defects or poor bone quality, autologous bone graft (from the distal metatarsal, calcaneus, or tibia) or allograft may be used to enhance fusion rates.
- Closure: Layered closure is performed after achieving hemostasis.
Complications & Management
Despite meticulous surgical technique, complications can arise following surgery for hallux rigidus. A thorough understanding of these potential issues and their management is crucial for all orthopedic surgeons.
General Surgical Complications
- Infection: Superficial or deep. Managed with antibiotics, wound debridement, and potentially hardware removal.
- Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE): Prophylaxis protocols are critical. Management involves anticoagulation.
- Nerve Injury: Most commonly the medial dorsal cutaneous nerve, leading to numbness, paresthesias, or painful neuroma. Prevention involves careful dissection and retraction. Management ranges from observation to neuromodulators or surgical neurectomy for persistent painful neuromas.
- Wound Healing Issues: Delayed healing, dehiscence, or skin necrosis, particularly in patients with diabetes, peripheral vascular disease, or those who smoke. Meticulous skin handling and tension-free closure are important.
Specific Complications to First MTP Surgery
Table 2: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (approx.) | Management & Salvage Strategies |
|---|---|---|
| Persistent/Recurrent Pain | 10-20% |
Cheilectomy/Osteotomy:
Inadequate resection, progression of arthritis, avascular necrosis, hardware irritation. Re-evaluate with imaging. Management: revision cheilectomy, conversion to arthroplasty or arthrodesis.
Arthrodesis: Nonunion, malunion, transfer metatarsalgia. Management: revision arthrodesis, orthotics. |
| Stiffness/Limited ROM | 10-15% | Cheilectomy/Arthroplasty: Inadequate bone resection, capsular scarring, aggressive post-op immobilization. Management: early aggressive physical therapy, manipulation under anesthesia, revision cheilectomy/capsular release. |
| Nonunion (Arthrodesis) | 5-10% | Arthrodesis: Inadequate fixation, poor bone quality, infection, early weight-bearing. Management: revision arthrodesis with bone graft (autograft/allograft), stronger internal fixation, extended immobilization. |
| Malunion (Arthrodesis) | 10-15% | Incorrect positioning of fusion (too much/little dorsiflexion, valgus/varus). Management: if symptomatic (e.g., shoe wear problems, transfer metatarsalgia), corrective osteotomy or revision arthrodesis. |
| Hardware Issues | 5-10% | Prominent, symptomatic hardware (screws, plates), hardware failure (breakage, loosening). Management: hardware removal after healing is complete, revision fixation if integrity is compromised. |
| Overcorrection/Undercorrection | <5% | Osteotomies: Incorrect cut, inadequate or excessive correction. Management: revision osteotomy, or conversion to arthrodesis in severe cases. |
| Transfer Metatarsalgia | 5-15% | Altered weight-bearing mechanics leading to pain under lesser metatarsals (often after cheilectomy due to shortening or arthrodesis). Management: accommodative orthotics, shoe modifications, metatarsal pads. Rarely, lesser metatarsal osteotomies. |
| Implant Failure (Arthroplasty) | Up to 20-30% | Loosening, subsidence, fracture, osteolysis, silicon synovitis (for older silastic implants). Management: implant removal, revision to arthrodesis, or another form of arthroplasty. |
| Avascular Necrosis (AVN) | <1% | Rare, typically affecting the metatarsal head. Can lead to joint collapse and accelerated arthritis. Management: conservative management initially, then debridement or conversion to arthrodesis for severe cases. |
| Recurrence of Deformity/Symptoms | Variable | Most common with motion-preserving procedures in advanced stages or if primary problem not fully addressed (e.g., inadequate cheilectomy). Management: revision surgery, conversion to arthrodesis. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical component of successful surgical management for hallux rigidus, aiming to optimize functional recovery and prevent complications. Protocols vary significantly based on the specific surgical procedure performed.
General Principles
- Individualized Care: Protocols should be tailored to the individual patient, considering bone quality, surgical stability, and adherence.
- Pain Management: Adequate analgesia is essential to facilitate early mobilization and patient compliance.
- Edema Control: Elevation and cryotherapy are crucial in the immediate post-operative period to minimize swelling and pain.
- Weight-Bearing Progression: Gradual progression of weight-bearing is based on the stability of internal fixation and tissue healing.
Procedure-Specific Protocols
1. Cheilectomy and Moberg Osteotomy
These procedures aim to restore and maintain motion, so early mobilization is typically encouraged.
*
Immediately Post-operative (Day 0 - 2 weeks):
*
Dressing/Immobilization:
Soft compression dressing, surgical shoe (e.g., post-operative shoe with a stiff sole or rocker bottom).
*
Weight-Bearing:
Weight-bearing as tolerated (WBAT) in the surgical shoe. Crutches or a walker may be used for initial balance and comfort.
*
Activity:
Elevation of the foot above the heart to minimize swelling. Ice application for 15-20 minutes, several times a day.
*
Range of Motion (ROM):
Crucial. Initiate immediate, gentle active and passive ROM exercises for the first MTP joint, focusing on dorsiflexion and plantarflexion. Patients are instructed to perform these exercises frequently throughout the day to prevent stiffness and scar tissue formation.
*
Early Phase (2 - 6 weeks):
*
Dressing/Footwear:
Transition from surgical shoe to a stiff-soled, wide-toe box athletic shoe or comfortable walking shoe once sutures are removed and wound healing is satisfactory.
*
ROM/Strengthening:
Continue and progressively increase MTP joint ROM exercises. Begin gentle strengthening exercises for the intrinsic foot muscles and ankle musculature (e.g., toe curls, towel scrunches, heel raises).
*
Gait Training:
Focus on restoring a normal gait pattern, emphasizing full push-off with the great toe.
*
Late Phase (6 - 12+ weeks):
*
Activity:
Gradual return to full activities, including sports, based on pain and achieved ROM.
*
Therapy:
Continue with home exercise program focusing on strength, flexibility, proprioception, and functional activities specific to the patient's goals.
*
Expected Outcome:
Full functional range of motion, typically 60-70 degrees of dorsiflexion, with minimal pain.
2. Arthrodesis (Fusion)
The primary goal is rigid immobilization to achieve bony union. Motion is intentionally sacrificed.
*
Immediately Post-operative (Day 0 - 6 weeks):
*
Dressing/Immobilization:
Non-weight-bearing (NWB) in a short leg cast or a non-removable CAM (Controlled Ankle Motion) boot.
*
Weight-Bearing:
Strict non-weight-bearing on the operative foot. Crutches or a knee scooter are typically used.
*
Activity:
Elevation and ice.
*
ROM:
No active or passive ROM exercises for the fused first MTP joint. Maintain ROM for other joints of the foot and ankle.
*
Fusion Confirmation Phase (6 - 12 weeks):
*
Radiographic Assessment:
Serial weight-bearing radiographs are obtained at 6-8 weeks to assess for signs of bony union.
*
Weight-Bearing Progression:
Once radiographic evidence of early union is confirmed, gradual progression to weight-bearing in a removable CAM boot or stiff-soled shoe is initiated. If union is not evident, NWB may be extended.
*
Therapy:
No direct therapy for the fused joint. Focus on improving gait mechanics with the fused joint and addressing any compensatory issues.
*
Late Phase (3 - 6+ months):
*
Footwear:
Transition to comfortable, stiff-soled shoes with adequate toe box space. Patients need to understand the implications of the fused joint for footwear selection.
*
Activity:
Gradual return to full activities. High-impact sports may be modified or limited based on the patient's individual adaptation.
*
Expected Outcome:
Pain-free, solidly fused joint. Patients adapt well to the loss of motion, with high satisfaction rates once fusion is achieved.
3. Interposition Arthroplasty / Hemiarthroplasty
These protocols combine elements of both motion-preserving and joint-altering procedures, with a focus on protected early motion.
*
Immediately Post-operative (Day 0 - 2 weeks):
*
Dressing/Immobilization:
Soft compression dressing, surgical shoe.
*
Weight-Bearing:
Partial weight-bearing (PWB) in the surgical shoe or CAM boot, gradually progressing to WBAT as comfort allows.
*
Activity:
Elevation, ice.
*
ROM:
Gentle active and passive ROM exercises initiated early, but with caution to avoid excessive stress on the implant or graft.
*
Early Phase (2 - 6 weeks):
*
Footwear:
Transition to a stiff-soled athletic shoe.
*
ROM/Strengthening:
Continue progressive ROM and gentle strengthening.
*
Late Phase (6 - 12+ weeks):
*
Activity:
Gradual return to activities. Specific limitations may exist based on implant type and surgeon preference (e.g., avoiding high-impact loading for some implants).
*
Expected Outcome:
Maintained motion with pain relief. Long-term durability and motion preservation can be variable.
Summary of Key Literature / Guidelines
The body of literature on hallux rigidus management is extensive, with increasing evidence guiding surgical decision-making. Consensus exists for the staged approach to treatment, correlating surgical procedures with the severity of degenerative changes.
- Cheilectomy: For Coughlin and Shurnas Grade 1 and 2 hallux rigidus, cheilectomy remains the most frequently performed and successful motion-preserving procedure. Studies consistently report good to excellent outcomes in 70-90% of patients, with significant pain relief and improved dorsiflexion, particularly when adequate resection of the dorsal metatarsal head (up to 20-30% of the articular surface) is achieved. However, its effectiveness significantly diminishes in advanced stages (Grade 3 and 4), where rates of recurrent pain and progression of arthritis are higher. The technique's efficacy hinges on patient selection, ensuring minimal joint space narrowing and preservation of articular cartilage.
- Osteotomies (Moberg, Watermann): Dorsal wedge osteotomies of the proximal phalanx (Moberg) or distal metatarsal (Watermann) are valuable adjuncts to cheilectomy, especially in patients with persistent functional hallux limitus or metatarsus primus elevatus. Moberg osteotomy has been shown to significantly increase the effective dorsiflexion of the hallux by changing its angular relationship with the metatarsal, improving push-off mechanics. When combined with cheilectomy, these osteotomies demonstrate superior long-term outcomes compared to cheilectomy alone in select patient populations.
- Arthrodesis: Fusion of the first MTP joint is widely considered the "gold standard" for end-stage hallux rigidus (Coughlin and Shurnas Grade 4), providing the most reliable and durable pain relief. Fusion rates typically range from 90% to 98%, with high patient satisfaction despite the sacrifice of motion. While loss of motion is inherent, studies indicate that patients adapt well, and functional limitations are often minimal in the context of effective pain resolution. Careful attention to appropriate joint positioning (10-20 degrees dorsiflexion, 10-15 degrees valgus) is critical for optimal functional outcomes and shoe wear.
-
Arthroplasty (Interposition, Hemiarthroplasty):
The role of motion-preserving arthroplasty remains controversial. While these procedures offer an alternative to fusion for patients unwilling to sacrifice motion, their long-term outcomes are less predictable compared to arthrodesis.
- Silicone implants: Largely abandoned due to concerns regarding particulate synovitis and implant failure.
- Metallic hemiarthroplasty (e.g., titanium, cobalt-chrome implants): Show promising short-to-mid-term results in selected, often lower-demand patients. However, concerns persist regarding implant loosening, erosion of the contralateral articular cartilage, osteolysis, and revision rates. Long-term comparative studies against arthrodesis often show superior pain relief and durability for fusion in severe cases.
- Interposition arthroplasty (using autograft or allograft): While attempting to preserve motion and avoid implant-related complications, these procedures generally have less predictable outcomes than fusion, with variable rates of pain relief and maintenance of motion. They may be considered for younger, active individuals with significant cartilage loss but who are not candidates for fusion due to professional or lifestyle demands.
- Cartilage Restoration: For focal chondral lesions in younger patients, techniques like microfracture, OATS, or MACI hold promise, but their application in diffuse, advanced hallux rigidus is limited, and long-term data specific to the first MTP joint is still evolving.
- Outcome Measures: The American Orthopaedic Foot & Ankle Society (AOFAS) Hallux MTP-IP Scale is a widely used, albeit criticized for subjectivity, outcome measure for assessing pain, function, and alignment in hallux rigidus patients. More patient-reported outcome measures (PROMs) such as the Foot and Ankle Ability Measure (FAAM) or SF-36 are increasingly employed to capture broader health-related quality of life.
In conclusion, current literature strongly supports a tiered approach to hallux rigidus treatment. Cheilectomy and adjunct osteotomies are effective for early to moderate disease. For end-stage disease, arthrodesis provides the most reliable and durable solution, while arthroplasty options offer a compromise for motion preservation with potentially less predictable long-term results. The decision should always be individualized, integrating the patient's specific presentation, expectations, and the surgeon's expertise.
