Introduction & Epidemiology
Distal radius fractures (DRFs) are among the most common fractures encountered in orthopedic practice, representing approximately one-sixth of all fractures treated in emergency departments. Their epidemiology demonstrates a bimodal distribution: high-energy trauma in younger, active individuals and low-energy falls in the osteoporotic elderly population. The global incidence is substantial, with reported rates ranging from 23.6 to 36.1 per 10,000 person-years, and these figures are projected to rise with an aging demographic.
The profound socioeconomic burden of DRFs stems not only from the direct costs of treatment but also from the significant potential for long-term morbidity, including persistent pain, stiffness, loss of function, and the dreaded development of Complex Regional Pain Syndrome (CRPS) and post-traumatic arthritis. While seemingly straightforward, the complexity of managing DRFs lies in restoring intricate wrist anatomy and kinematics to prevent these debilitating complications. A meticulous understanding of fracture morphology, surgical anatomy, biomechanics, and contemporary treatment strategies is paramount to achieving optimal functional outcomes and mitigating the risk of CRPS and late instability. Prevention of CRPS necessitates early recognition of risk factors, gentle tissue handling, adequate pain control, and early mobilization where appropriate. Similarly, identifying and addressing subtle signs of carpal or distal radioulnar joint (DRUJ) instability is critical for long-term wrist function and prevention of progressive degenerative changes.
Surgical Anatomy & Biomechanics
Successful management of distal radius fractures hinges upon a profound understanding of the complex anatomical and biomechanical interrelationships of the distal radius, ulna, and carpus.
Distal Radius Anatomy
The distal radius comprises three key components: the diaphysis, metaphysis, and epiphysis, encompassing the articular surface.
*
Articular Surface:
The distal articular surface articulates with the scaphoid (scaphoid fossa, laterally) and lunate (lunate fossa, medially). These fossae are separated by a subtle osseous ridge, often termed the scaphoid-lunate ridge or water-shed line. The normal articular surface has a characteristic volar tilt (average 11-12° relative to the radial shaft axis in the sagittal plane) and radial inclination (average 22-23° in the coronal plane).
*
Cortical Structures:
The dorsal cortex is relatively straight, while the volar cortex has a sigmoid curve, forming the volar buttress. Lister's tubercle, a dorsal osseous prominence, serves as a pulley for the extensor pollicis longus (EPL) tendon and is a key surgical landmark. The radial styloid provides attachment for the brachioradialis tendon and the stout radioscaphocapitate ligament.
*
Soft Tissues:
*
Pronator Quadratus (PQ):
This quadrangular muscle lies on the volar aspect of the distal radius, acting as a crucial stabilizer of the DRUJ and providing a robust vascularized soft tissue envelope over volar plates. Its preservation or meticulous repair is important for both function and minimizing tendon irritation.
*
Neurovascular Structures:
The median nerve and flexor tendons pass through the carpal tunnel volar to the radius. The radial artery courses dorsoradially. The superficial branch of the radial nerve and dorsal sensory branch of the ulnar nerve are vulnerable to injury during surgical approaches.
Distal Radioulnar Joint (DRUJ)
The DRUJ is a complex trochoid joint critical for forearm rotation. It is formed by the ulnar head articulating with the sigmoid notch of the distal radius. Stability is primarily conferred by the triangular fibrocartilage complex (TFCC), which includes the articular disc, dorsal and volar radioulnar ligaments, and meniscal homologue.
*
TFCC:
The TFCC originates from the distal radius near the sigmoid notch and inserts onto the fovea and styloid process of the ulna. The volar radioulnar ligament is generally considered the stronger and more critical stabilizer against dorsal translation of the ulna relative to the radius.
*
Ulnar Variance:
The relationship between the distal articular surfaces of the radius and ulna in the coronal plane (ulnar variance) is critical. Neutral ulnar variance (ulna and radius at the same level) or slight negative variance (ulna shorter) is typical. Positive ulnar variance (ulna longer) is frequently associated with DRUJ pathology and can lead to ulnar impaction syndrome.
Carpal Anatomy and Ligaments
The carpus consists of two rows of bones, interconnected by a complex network of intrinsic and extrinsic ligaments. DRFs frequently involve these ligamentous structures, leading to carpal instability.
*
Extrinsic Ligaments:
These connect the radius/ulna to the carpus. Key ligaments include the volar radioscaphocapitate, radiolunotriquetral, and short radiolunate ligaments, which are crucial for maintaining carpal alignment.
*
Intrinsic Ligaments:
These connect carpal bones to each other. The scapholunate (SL) and lunotriquetral (LT) ligaments are paramount for carpal stability. Disruption of these ligaments can lead to dissociative carpal instability (e.g., scapholunate advanced collapse - SLAC wrist).
Biomechanics of DRFs and Instability
The hallmark of a well-reduced DRF is the restoration of normal radiographic parameters:
*
Volar Tilt:
Loss of volar tilt (dorsal angulation) is common in extension-type fractures and increases stress on the volar carpal ligaments, potentially leading to carpal instability and post-traumatic arthrosis.
*
Radial Inclination:
Loss of radial inclination can alter load transfer across the carpus and DRUJ, leading to ulnar-sided wrist pain and DRUJ dysfunction.
*
Radial Length:
Shortening of the radius relative to the ulna (positive ulnar variance) significantly alters DRUJ mechanics, predisposing to TFCC tears, ulnar impaction, and DRUJ instability. A difference of >3-5 mm compared to the contralateral wrist is often considered significant.
*
Articular Congruity:
Intra-articular step-off or gap of >1-2 mm is strongly correlated with the development of post-traumatic arthritis.
Recognizing and correcting these parameters is crucial not only for joint congruity but also for maintaining the intricate balance of forces across the wrist. Failure to restore these relationships can lead to chronic pain, loss of motion, and progressive degenerative changes, directly impacting the risk of CRPS and long-term disability.
Indications & Contraindications
The decision-making process for managing distal radius fractures involves a careful assessment of fracture characteristics, patient factors, and the presence of associated injuries. The goal is to achieve an anatomically and functionally acceptable reduction while minimizing complications.
Non-Operative Indications
Non-operative management, typically involving closed reduction and cast immobilization, is generally reserved for:
*
Stable fractures:
Minimally displaced, extra-articular fractures.
*
Reducible fractures:
Fractures that can be anatomically reduced and held in a stable position.
*
Elderly, low-demand patients:
Particularly those with significant comorbidities where the risks of surgery outweigh the potential benefits, and a functional outcome rather than anatomical perfection is the primary goal.
*
Acceptable parameters post-reduction:
* Radial inclination >15°
* Volar tilt (or neutral, up to 10° dorsal tilt in very elderly)
* Radial shortening <3-5 mm (compared to contralateral wrist)
* Intra-articular step-off/gap <1-2 mm (if present)
* No significant DRUJ instability after reduction.
Operative Indications
Operative intervention aims to achieve and maintain an anatomical reduction in fractures that are inherently unstable or have specific characteristics that preclude successful non-operative management.
*
Unstable fractures:
Fractures prone to re-displacement after closed reduction, including:
* Significant comminution (especially dorsal and volar metaphysis).
* Loss of volar tilt (dorsal angulation >0-5° is a common threshold for operative intervention, especially in active patients).
* Initial radial shortening >3-5 mm.
* Initial radial inclination <15°.
* Age <60 years with any significant displacement.
*
Intra-articular fractures:
* Articular step-off or gap >1-2 mm, particularly involving the scaphoid fossa.
* Displaced die-punch fragments.
*
DRUJ instability:
Irreducible or persistently unstable DRUJ after reduction of the distal radius. This often indicates TFCC disruption or gross incongruity.
*
Open fractures:
Require immediate surgical debridement and stabilization.
*
Associated injuries:
Carpal instability (e.g., scapholunate dissociation), carpal bone fractures, severe soft tissue compromise, neurovascular compromise (though rare, can be an emergency indication).
*
Young, high-demand patients:
A lower threshold for operative intervention is often adopted to optimize long-term function and minimize the risk of post-traumatic arthritis.
Contraindications
Absolute contraindications for operative intervention are rare but include:
*
Active local infection:
Requires resolution before elective fixation.
*
Severe uncontrolled comorbidities:
Where general or regional anesthesia poses an unacceptable risk.
*
Non-compliant patient:
If strict post-operative protocols (e.g., rehabilitation, weight-bearing restrictions) cannot be followed, leading to potential failure.
Relative contraindications may include severe osteopenia where durable fixation is challenging, although modern locking plate technology has significantly expanded the surgical indications in this population.
Summary Table: Operative vs. Non-Operative Indications
| Feature | Non-Operative Management | Operative Management |
|---|---|---|
| Fracture Type | Minimally displaced, stable, extra-articular | Displaced, unstable, intra-articular, comminuted |
| Articular Step-off/Gap | <1-2 mm | >1-2 mm |
| Radial Shortening | <3-5 mm | >3-5 mm |
| Radial Inclination | >15° | <15° |
| Volar Tilt (Sagittal) | Normal to neutral (up to 10° dorsal in elderly) | Dorsal angulation >0-5° (loss of volar tilt) |
| DRUJ Stability | Stable after reduction | Unstable or irreducible after reduction of radius |
| Patient Factors | Elderly, low functional demand, significant comorbidities | Young, active, high functional demand, minimal comorbidities |
| Open Fracture | Never | Always |
| Associated Injuries | None or minor | Carpal instability, neurovascular compromise, other fractures |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial for optimizing outcomes, preventing complications, and addressing potential instability.
Pre-Operative Planning
-
Clinical Assessment:
- Neurovascular Status: Thorough assessment of median, ulnar, and radial nerve function (sensory and motor) and vascular integrity. Evaluate for signs of acute carpal tunnel syndrome.
- Soft Tissue Envelope: Inspect for open wounds, severe swelling, blistering, or impending compartment syndrome.
- Contralateral Wrist: Always assess the contralateral wrist for baseline range of motion, strength, and importantly, radiographic parameters (ulnar variance, radial inclination, volar tilt) for comparison.
-
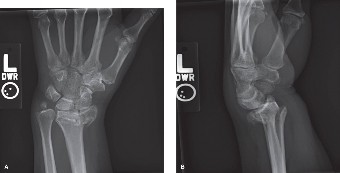
Radiographic Evaluation:
- Standard Views: High-quality posteroanterior (PA), lateral, and oblique views are essential. The PA view assesses radial inclination and length, while the lateral view is crucial for volar tilt and dorsal/volar comminution.
- Computed Tomography (CT) Scan: Highly recommended for all displaced intra-articular fractures. A CT scan provides invaluable detail regarding articular step-off/gap, the extent of comminution, specific fragment anatomy, and assessment of the sigmoid notch and DRUJ. This information directly informs plate selection, surgical approach, and reduction strategy to restore articular congruence and prevent instability.
- Contralateral CT: In complex cases, a CT of the uninjured wrist can serve as a template for anatomical restoration.
- Fracture Classification: Utilize a consistent classification system (e.g., AO/OTA) to guide treatment and communication.
- Implant Selection: Based on fracture pattern, determine the appropriate volar locking plate system (standard, wide, variable angle, fragment specific). Consider the need for dorsal plates, K-wires, or external fixation.
- Tourniquet Time & Blood Loss: Anticipate these parameters.
- CRPS Prevention: Discuss pre-operative Vitamin C supplementation (500mg daily for 50 days) with the patient, as some studies suggest a prophylactic benefit, particularly in higher-risk individuals. Ensure aggressive pain management strategies are in place.
Patient Positioning
The most common position for distal radius fracture fixation is supine on the operating table, with the affected arm extended on a specialized hand table or a stable arm board. This setup allows for unimpeded fluoroscopic imaging in both AP and lateral planes.
-
Preparation:
- Tourniquet: A pneumatic tourniquet is applied to the upper arm, allowing for a bloodless field, which is critical for meticulous soft tissue dissection and accurate reduction.
- Padding: All pressure points are meticulously padded to prevent iatrogenic nerve compression.
- Fluoroscopy: The C-arm is positioned to allow unobstructed AP and lateral views of the distal radius and carpus without repositioning the patient or the arm during the case. This is paramount for confirming reduction and implant placement.
- Traction (Optional): For significantly comminuted or shortened fractures, a finger trap traction setup (suspended from an IV pole or specialized tower) can be invaluable for ligamentotaxis and initial indirect reduction. This can also help distinguish true intra-articular fragments from soft tissue interposition.
Detailed Surgical Approach / Technique
The goal of surgical fixation is to achieve anatomical reduction, stable fixation, and facilitate early mobilization while minimizing iatrogenic injury and preventing long-term complications like CRPS and instability. The volar approach using a locking plate is the most common technique for unstable distal radius fractures.
Anesthesia
Regional anesthesia (e.g., axillary block) often combined with general anesthesia is preferred. Regional blocks provide excellent intra-operative analgesia and can contribute to post-operative pain control, potentially reducing the risk of CRPS.
Surgical Approaches
-
Volar Henry Approach (Modified):
- This is the workhorse approach for most distal radius fractures, allowing direct access to the volar surface of the radius and the pronator quadratus.
- Incision: A longitudinal incision, typically 6-8 cm, centered over the FCR tendon, extending from just proximal to the wrist crease to approximately 6-8 cm proximally.
-
Dissection:
- Skin and Subcutaneous Tissue: Careful dissection, protecting the palmar cutaneous branch of the median nerve (which courses radially to the FCR tendon in the distal forearm) and the superficial radial artery branch.
- Fascia: Incise the forearm fascia in line with the FCR tendon.
- Internervous Plane: The most common interval utilizes the plane between the flexor carpi radialis (FCR) tendon (retracted ulnarly) and the radial artery (retracted radially). Alternatively, some prefer a more ulnar interval between the FCR tendon and the flexor pollicis longus (FPL), retracting the FCR radially. The radial artery must be protected as it courses obliquely towards the snuffbox. The median nerve lies ulnar to the FPL, deeper in the carpal tunnel.
-
Pronator Quadratus:
This muscle lies directly on the volar aspect of the distal radius. It is incised in an L-shape fashion, with the horizontal limb along its distal border and the vertical limb extending proximally from its radial attachment. This allows the pronator quadratus to be elevated from radial to ulnar, creating a vascularized flap that can be repaired over the plate at closure. This careful elevation protects the nutrient vessels to the distal radius and is thought to reduce tendon irritation from the plate.
- Fracture Exposure: The fracture site is now exposed. Debride any hematoma, loose bone fragments, or soft tissue interposition.
-
Dorsal Approach (Limited Indications):
- Less common due to higher risk of tendon irritation and poorer bone quality dorsally. Reserved for specific fracture patterns with significant dorsal comminution or displacement that cannot be adequately reduced volarly (e.g., Barton's fracture with dorsal displacement, some shear fractures, or extremely comminuted fractures requiring dorsal buttressing).
- Incision: Typically longitudinal, between the third and fourth extensor compartments (between EPL and EDC).
- Dissection: Retraction of tendons (EPL radially, EDC ulnarly). Careful handling of the dorsal sensory branch of the radial nerve. Risk of extensor tendonitis or rupture is higher with dorsal plating.
Reduction Techniques & Fixation
Regardless of the approach, the principles of reduction remain constant: restore radial length, radial inclination, volar tilt, and articular congruity.
-
Indirect Reduction (Ligamentotaxis):
- Application of longitudinal traction (manual or using a finger trap setup) can help distract the fracture fragments and indirectly reduce them by tensioning the intact carpal ligaments. This is particularly useful for comminuted fractures.
- Wrist is often held in slight flexion and ulnar deviation initially to help disimpact fragments.
-
Direct Reduction:
- After exposing the fracture, direct manipulation of fragments using periosteal elevators, K-wires (as joysticks), or small pointed reduction clamps.
- Restoration of Volar Tilt: Often achieved by pushing the dorsal aspect of the distal fragment volarly while maintaining axial traction.
- Restoration of Radial Length & Inclination: Achieved by distraction and correction of angulation.
- Articular Reduction: Crucial for intra-articular fractures. Direct visualization (if possible) or fluoroscopic guidance (in multiple planes) is used to ensure an anatomical reduction of the articular surface. Small fragments can be manipulated with K-wires. Bone graft (autograft or allograft) may be used to fill metaphyseal defects, especially in comminuted fractures or osteoporotic bone, providing structural support and preventing collapse.
-
Provisional Fixation:
- K-wires are often used to provisionally hold the reduction while the plate is applied. They can be inserted from the radial styloid into the scaphoid fossa (to restore radial inclination and length) or across articular fragments.
- Ensure K-wires do not interfere with plate placement.
-
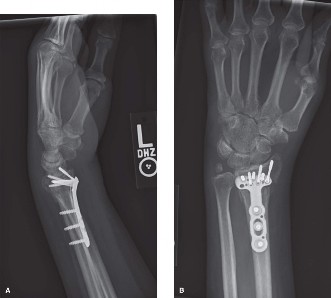
Volar Locking Plate Application:
- The plate is contoured and positioned on the volar aspect of the radius. The distal edge of the plate should be placed just proximal to the critical watershed line (or volar rim) of the articular surface to maximize subchondral screw support without impinging on the flexor tendons in the carpal tunnel.
- Distal Screws: Multi-directional or fixed-angle locking screws are inserted into the subchondral bone of the distal fragment, aiming to buttress the articular surface. Fluoroscopy in both AP and lateral views is crucial to confirm optimal screw length and trajectory, ensuring screws do not violate the joint space or protrude dorsally. Avoid long screws that might impinge on flexor tendons.
- Proximal Screws: Cortical or locking screws are then inserted into the radial shaft, providing stable fixation to the diaphysis.
- Final Assessment: After plate and screw insertion, re-evaluate reduction with fluoroscopy in AP and true lateral views. Check radial inclination, radial length, volar tilt, and articular congruity. Ensure no screw prominence or intra-articular violation.
Intraoperative Assessment for Instability
After plate fixation, meticulous assessment of potential DRUJ and carpal instability is paramount.
*
DRUJ Stability:
Perform a stress test by pronating and supinating the forearm while directly assessing the stability of the ulnar head relative to the sigmoid notch. If unstable, consider intraoperative TFCC repair (via arthroscopy or open approach), or K-wire stabilization of the DRUJ (typically 2 K-wires across the DRUJ, with the forearm in neutral rotation).
*
Carpal Stability:
While less common after an adequate distal radius reduction, gross carpal instability should be re-evaluated on fluoroscopy. Persistent widening of the scapholunate interval (>3mm) or a dorsal intercalated segmental instability (DISI) deformity warrants further investigation (e.g., arthroscopy) and potential ligament repair.
Wound Closure
- Pronator Quadratus Repair: Meticulously reattach the pronator quadratus over the volar plate. This covers the hardware, reduces tendon irritation, provides a vascularized soft tissue layer, and helps restore DRUJ stability.
- Fascia and Subcutaneous Tissue: Close in layers.
- Skin: Close with standard skin sutures.
- Dressing: Apply a sterile dressing and a well-padded sugar tong or volar splint for comfort and initial immobilization, allowing for early finger motion.
Preventing CRPS Intraoperatively
- Gentle Tissue Handling: Minimize retraction and blunt dissection to reduce tissue trauma.
- Adequate Pain Control: Ensure excellent regional block and systemic analgesia.
- Hemostasis: Meticulous hemostasis to prevent large hematoma formation.
- Minimize Tourniquet Time: Keep tourniquet time as short as possible.
Complications & Management
Distal radius fracture fixation, while generally successful, is not without potential complications. A comprehensive understanding of these and their management strategies is essential for all orthopedic surgeons. CRPS prevention must be a continuous focus throughout the management continuum.
Common Complications and Salvage Strategies
| Complication | Incidence | Etiology | Management / Salvage Strategy | CRPS Prevention Relevance |
|---|---|---|---|---|
| Complex Regional Pain Syndrome (CRPS) | 2-35% (variable by definition) | Multifactorial; prolonged immobilization, nerve injury, severe pain, psychological factors, genetics, inflammation. | Proactive: Vitamin C (500mg daily for 50 days), meticulous surgical technique, aggressive pain control (regional blocks), early gentle mobilization, psychological support. Management: Multimodal pain regimen (NSAIDs, gabapentinoids, TCAs), physical/occupational therapy, stellate ganglion blocks, nerve blocks, sympathetic blocks, psychological counseling. | Primary focus of management. Early diagnosis, prompt intervention, gentle surgical technique, adequate analgesia, and early mobilization are paramount. Vitamin C prophylaxis may reduce incidence. |
| Malunion | 5-25% | Inadequate reduction, loss of reduction post-fixation, implant failure, osteoporosis. | Mild/Asymptomatic: Observation. Symptomatic (pain, limited ROM, DRUJ issues): Corrective osteotomy (opening/closing wedge), bone grafting, possible hardware removal, DRUJ procedures (e.g., Darrach, Sauve-Kapandji, wafer resection). | Malunion can lead to chronic pain and stiffness, increasing CRPS risk. Anatomical reduction and stable fixation are critical. |
| Nonunion | <1% | Severe comminution, open fracture, infection, inadequate fixation, biological factors (smoking, NSAIDs). | Debridement, stable internal fixation, bone grafting (autograft/allograft), electrical stimulation. | Prolonged pain and stiffness from nonunion are risk factors for CRPS. |
| Tendon Rupture | 1-5% (FPL most common) | Plate prominence (especially if too distal or proud), sharp plate edges, rough screw heads, chronic irritation, initial tendon injury. | FPL: Tendon transfer (e.g., FDS to FPL). EPL: Tendon transfer (e.g., EIP to EPL), direct repair (rare). Often requires plate removal. | Constant irritation or rupture leads to pain, inflammation, and functional deficits, which can precipitate CRPS. Careful plate placement and pronator quadratus repair are key. |
| Nerve Injury | 5-20% (Radial sensory, median) | Radial Sensory: Direct injury during dorsal/volar approaches, traction injury, entrapment in scar. Median: Acute carpal tunnel syndrome (pre-op), iatrogenic during volar approach, plate prominence, scar. | Radial Sensory: Observation (most recover), neurolysis if persistent neuroma/severe symptoms. Median: Carpal tunnel release (if acute or chronic compression), neurolysis if direct injury. Plate removal if causing compression. | Nerve injury, especially median nerve compression, is a direct predisposing factor for CRPS. Early recognition and decompression/management are crucial. |
| Infection | 1-3% | Contamination during surgery, immunocompromised patient, poor wound care, open fracture. | Superficial: Oral antibiotics, wound care. Deep: Surgical debridement, IV antibiotics, irrigation, possible hardware removal (after fracture healing or staged). | Infection causes significant pain and inflammation, increasing CRPS risk. |
| DRUJ Instability / Arthritis | 5-15% | Inadequate reduction of radial length, unaddressed TFCC injury, persistent positive ulnar variance, poor anatomical restoration of sigmoid notch. | Acute: TFCC repair (arthroscopic or open), DRUJ stabilization with K-wires. Chronic Instability/Arthritis: Ulnar shortening osteotomy, Darrach procedure, Sauve-Kapandji procedure, wafer resection, DRUJ arthroplasty (less common). | Unresolved DRUJ pathology results in chronic pain and restricted motion, both of which are risk factors for CRPS. Thorough intraoperative assessment and appropriate intervention for DRUJ stability are vital. |
| Plate Impingement / Prominence | 5-10% | Plate placed too distally, too prominent, inadequate contouring, hardware loosening, persistent dorsal angulation. | Hardware removal after fracture healing (if symptomatic). Revision surgery with a lower profile plate or repositioning if causing significant issues before healing. | Persistent irritation and pain from prominent hardware can contribute to CRPS symptoms. |
| Post-Traumatic Arthritis | 10-30% | Inadequate articular reduction (step-off/gap >1-2mm), malunion, associated ligamentous injuries (e.g., SLAC wrist), DRUJ incongruity. | Symptomatic: Activity modification, NSAIDs, corticosteroid injections. Progressive: Salvage procedures like partial carpal fusion, proximal row carpectomy, total wrist arthrodesis, or wrist arthroplasty. | Chronic pain and stiffness from arthritis are risk factors for CRPS. Anatomical restoration is the best preventative measure. |
Preventing CRPS: A Proactive Approach
Beyond the generalized measures mentioned above, specific attention should be paid to CRPS prevention throughout all phases of care:
*
Pre-operatively:
Identify high-risk patients (pre-existing chronic pain, anxiety, prior CRPS). Offer Vitamin C.
*
Intra-operatively:
Minimize tourniquet time, meticulous soft tissue handling, precise fracture reduction, stable fixation, generous regional anesthesia.
*
Post-operatively:
Aggressive pain management, early mobilization of fingers/shoulder/elbow, elevation to reduce edema, early referral to occupational/physical therapy, education on CRPS signs and symptoms.
*
Psychological Support:
Address patient anxiety and fear, as psychological factors can play a role in CRPS development.
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is critical for maximizing functional recovery, preventing stiffness, and minimizing the risk of complications, especially CRPS and long-term instability. The protocol is typically tailored to the fracture stability, patient compliance, and surgical findings (e.g., DRUJ stability, associated soft tissue repairs).
Phase I: Protective Phase (0-2 Weeks Post-Op)
Goals: Protect surgical repair, minimize pain and swelling, prevent joint stiffness in uninvolved joints, initiate CRPS prevention.
-
Immobilization:
- Initially, a well-padded volar or sugar-tong splint is applied in a neutral position for comfort and protection.
- If DRUJ was stabilized with K-wires, the forearm is immobilized in neutral rotation.
- Pain Management: Continue aggressive pain management (analgesics, anti-inflammatories). Regional blocks from surgery may still be active.
- Edema Control: Elevate the hand above the heart, gentle compression gloves/stockings.
-
Early Active Motion:
- Fingers: Active range of motion (AROM) exercises for metacarpophalangeal (MCP) and interphalangeal (IP) joints (full flexion and extension) several times daily. Encourage "full fisting."
- Elbow & Shoulder: AROM exercises for the elbow and shoulder to prevent stiffness.
- NO active or passive wrist motion, forearm rotation.
- Wound Care: Keep incision clean and dry. Monitor for signs of infection.
- CRPS Prevention: Emphasize elevation, pain control, active finger/shoulder/elbow ROM. Continue Vitamin C if initiated pre-operatively.
Phase II: Early Motion / Mobilization Phase (2-6 Weeks Post-Op)
Goals: Gradually restore active wrist range of motion, improve scar mobility, continue edema control.
- Immobilization: Splint is typically removed, and a removable wrist brace (often worn for comfort/protection between exercises) may be prescribed, depending on fracture stability and surgeon preference. If DRUJ wires were used, they are typically removed around 4-6 weeks, and then gradual rotation initiated.
-
Active Range of Motion (AROM):
- Wrist: Gentle active wrist flexion, extension, radial and ulnar deviation. Start with gravity-assisted exercises. Progress as tolerated, avoiding pain.
- Forearm Rotation: Gentle active pronation and supination (if DRUJ is stable and not wired).
- Fingers, Elbow, Shoulder: Continue AROM.
- Scar Management: Gentle massage and desensitization of the incision site once sutures are removed and the wound is fully healed.
- Edema Control: Continue elevation, compression.
- Sensory Re-education: For any nerve deficits.
- Light ADLs: Encourage use for light activities of daily living (e.g., eating, dressing) within pain limits.
Phase III: Strengthening & Advanced Mobility Phase (6-12 Weeks Post-Op)
Goals: Improve strength, restore full range of motion, enhance proprioception, prepare for return to functional activities.
- Progression: Discontinue wrist brace for most activities, as fracture healing is typically advanced.
-
Strengthening:
- Isometric: Begin with gentle isometric exercises for wrist and forearm.
- Progressive Resistive Exercises (PREs): Gradually introduce light weights, therapy putty, rubber bands for wrist flexion/extension, radial/ulnar deviation, pronation/supination.
- Grip Strength: Squeeze soft ball/putty.
- Proprioception and Coordination: Exercises like ball rolling, picking up small objects, dynamic balance activities for the wrist.
- Functional Activities: Progress to more demanding activities of daily living.
- CRPS Awareness: Monitor for any signs of CRPS progression. If suspected, initiate appropriate interventions promptly.
Phase IV: Return to Activity / Maintenance Phase (12+ Weeks Post-Op)
Goals: Gradual return to work, sport, and recreational activities. Continue strength and endurance training.
- Gradual Return: Based on pain levels, strength, and range of motion, patients can gradually return to more strenuous activities.
- Sport-Specific Training: If applicable, incorporate sport-specific drills.
- Continue Home Exercise Program: Emphasize the importance of long-term maintenance exercises.
- Follow-up: Regular clinical and radiographic follow-up to assess healing, monitor for late complications (e.g., post-traumatic arthritis, DRUJ issues), and address any persistent symptoms.
Throughout all phases, physical and occupational therapists play a critical role in guiding patients, assessing progress, and adapting the protocol as needed. Patient education on proper exercise technique, pain management, and early recognition of concerning symptoms (e.g., disproportionate pain, swelling, color changes indicative of CRPS) is paramount.
Summary of Key Literature / Guidelines
The management of distal radius fractures has evolved significantly, driven by advancements in surgical techniques, implant technology, and a deeper understanding of wrist biomechanics. Current evidence-based practices emphasize anatomical restoration to optimize functional outcomes and minimize long-term complications, particularly CRPS and instability.
Volar Locking Plate Technology
The advent of volar locking plates has revolutionized the treatment of unstable distal radius fractures, becoming the standard of care for many patterns.
*
Advantages:
These plates provide angular stable fixation, allowing for earlier mobilization compared to traditional non-locking plates or cast immobilization alone. Multiple studies, including systematic reviews and meta-analyses, have demonstrated superior radiographic outcomes (restoration of volar tilt, radial inclination, and length) and often improved functional scores (e.g., DASH scores) in the short to medium term compared to non-operative management or K-wire fixation for unstable fractures.
*
Literature:
The superiority of volar locking plates over non-operative treatment for displaced, unstable DRFs in terms of functional outcomes (e.g., DASH scores) at 1-2 years has been demonstrated in several Level I randomized controlled trials (e.g., Arora et al., Orbay et al.). While some studies show limited difference in long-term functional outcomes compared to K-wire fixation for less complex patterns, the robust stability provided by locking plates in comminuted or osteoporotic fractures remains a significant advantage.
Importance of Anatomical Restoration
A consistent theme in the literature is the correlation between anatomical reduction and improved long-term outcomes, directly impacting the prevention of post-traumatic arthritis and CRPS.
*
Articular Congruity:
Intra-articular step-off or gap exceeding 1-2 mm is widely recognized as a predictor of post-traumatic arthritis. CT scans are increasingly recommended pre-operatively to precisely identify these articular defects and guide surgical reduction.
*
Radiographic Parameters:
Restoration of normal radial length, radial inclination, and volar tilt is crucial. Persistent dorsal angulation (loss of volar tilt) is associated with worse functional outcomes and increased risk of pain and instability.
*
DRUJ Stability:
The significance of maintaining or restoring DRUJ congruity and stability is increasingly appreciated. Unaddressed DRUJ instability leads to chronic pain, restricted forearm rotation, and early degenerative changes. Intraoperative assessment of DRUJ stability after radial fixation is therefore a critical step, and if unstable, concurrent TFCC repair or temporary DRUJ stabilization with K-wires should be considered.
Complex Regional Pain Syndrome (CRPS) Prevention
The evidence supporting prophylactic measures for CRPS is growing:
*
Vitamin C:
A meta-analysis by Zollinger et al. (2007) and subsequent studies have suggested that prophylactic oral Vitamin C (e.g., 500mg daily for 50 days) can significantly reduce the incidence of CRPS type I after distal radius fractures. This is a simple, cost-effective intervention with minimal side effects, and its use is increasingly integrated into pre-operative protocols.
*
Early Mobilization and Pain Control:
Early, pain-free active range of motion, coupled with effective perioperative pain management (including regional blocks), is consistently emphasized in guidelines as a cornerstone of CRPS prevention. This reduces stiffness, swelling, and the nociceptive input believed to contribute to CRPS development.
Literature on Instability Signs
- Carpal Instability: While less common than DRUJ instability following DRF, persistent carpal instability (e.g., scapholunate dissociation) due to associated ligamentous injuries requires high suspicion. Careful assessment of radiographic parameters (scapholunate interval, carpal alignment) on standard views and CT scans, and sometimes wrist arthroscopy, is warranted. Failure to address these can lead to progressive carpal collapse (e.g., SLAC wrist).
- DRUJ Instability: Clinical and fluoroscopic assessment of DRUJ stability intraoperatively after distal radius fixation is now a standard recommendation. The "trampoline test" or direct ballotment of the ulnar head are valuable clinical maneuvers. Radiographically, assessing the congruity of the ulna head in the sigmoid notch on lateral fluoroscopic views (in pronation, supination, and neutral) can reveal subluxation.
- AAOS Clinical Practice Guidelines: The American Academy of Orthopaedic Surgeons (AAOS) provides evidence-based guidelines for the treatment of distal radius fractures, reinforcing many of these principles regarding operative indications, anatomical reduction, and considerations for associated injuries.
In summary, current literature and guidelines for distal radius fractures advocate for a comprehensive approach that prioritizes accurate diagnosis (often with CT), anatomical restoration of all critical parameters (length, inclination, tilt, articular congruity, DRUJ stability) using stable fixation (primarily volar locking plates), and a proactive, multimodal strategy for pain control and rehabilitation to prevent debilitating complications such as CRPS and progressive instability.
