INTRODUCTION TO METACARPAL NONUNION
The management of metacarpal nonunion, particularly when complicated by segmental bone loss, represents a formidable challenge in hand reconstruction. Unlike simple fractures that typically heal with conservative management or standard internal fixation, metacarpal defects usually result from high-energy trauma, severe crush injuries, gunshot wounds, or post-infectious debridement. These etiologies leave behind a hostile local environment characterized by compromised vascularity, dense cicatrix formation, and significant structural voids.
The ultimate success of bone grafting in metacarpal defects is predicated upon two non-negotiable pillars: the vitality of the soft tissue envelope and the biomechanical precision of the osseous reconstruction. Sterling Bunnell aptly coined the term "bone carpentry" to describe the exacting tolerances required in hand surgery. A structurally sound graft placed into a poorly vascularized bed will inevitably resorb or succumb to infection; conversely, a robust soft tissue envelope cannot compensate for a poorly fashioned, mechanically unstable graft.
This comprehensive guide details the surgical correction of metacarpal nonunions utilizing the classic Littler technique, providing orthopedic surgeons with an evidence-based framework for restoring digital length, alignment, and function.
PREOPERATIVE EVALUATION AND SOFT TISSUE MANAGEMENT
Before any osseous reconstruction is attempted, the surgeon must critically evaluate the soft tissue bed. The dorsum of the hand possesses a naturally thin subcutaneous layer, making it highly susceptible to breakdown over prominent hardware or bulky bone grafts.
Soft Tissue Prerequisites
First and foremost, the dorsum of the hand must be well covered by pliable, well-vascularized skin and subcutaneous tissue. If the native tissue has been lost to trauma or multiple previous surgeries, soft tissue reconstruction must precede or accompany the bone grafting procedure.
Surgical Pearl: The Reconstructive Elevator
Never attempt structural bone grafting under a split-thickness skin graft or severely scarred, adherent skin. If local tissue is inadequate, the surgeon must employ local rotational flaps, pedicled flaps (such as a groin or abdominal pedicle flap), or free tissue transfer (e.g., anterolateral thigh or lateral arm free flap) to establish a robust biological bed prior to osseous reconstruction.
Infection Eradication
Because the injury producing the bone defect is frequently open, the region remains potentially infected even though the original wound may have healed. A thorough preoperative workup, including inflammatory markers (ESR, CRP) and potentially a tagged white blood cell scan or preoperative aspiration, is mandatory if latent infection is suspected. Prophylactic antibiotics must be administered just before surgery and continued for several days postoperatively to mitigate the risk of acute flare-ups from disturbed dormant bacteria.
BIOMECHANICS AND PATHOANATOMY OF METACARPAL DEFECTS
Understanding the deforming forces acting upon a metacarpal nonunion is critical for executing a durable reconstruction.

As illustrated above, a metacarpal defect inevitably leads to a predictable pattern of deformity:
* Shortening: The intrinsic muscles (interossei and lumbricals) and extrinsic flexors exert a constant longitudinal compressive force, causing the distal fragment to migrate proximally. This shortens the ray, leading to an extensor lag at the metacarpophalangeal (MCP) joint and weakening grip strength.
* Dorsal Apex Angulation: The volar location of the intrinsic muscles creates a flexion moment on the distal fragment. Without the structural strut of the intact metacarpal diaphysis, the bone collapses into dorsal apex angulation.
* Rotational Malalignment: The lack of continuity allows the distal fragment to rotate, which manifests clinically as digital scissoring or overlapping during active flexion.
THE LITTLER TECHNIQUE: STEP-BY-STEP SURGICAL EXECUTION
The Littler technique is a masterclass in structural autografting. It relies on precise geometric cuts to maximize bone-to-bone contact, resist deforming forces, and utilize the hand's natural longitudinal compression to stabilize the construct.
1. Approach and Soft Tissue Dissection
- Incision: Expose the defective metacarpal utilizing a longitudinal or gently curved dorsal incision. The exact placement should be dictated by the location of existing scars to avoid creating narrow, ischemic skin bridges.
- Tendon Management: Meticulously dissect all scar tissue away from the extensor tendons.
Surgical Warning: It is absolutely critical to preserve the paratenon intact during this dissection. Stripping the paratenon will result in severe postoperative tendon adhesions, tethering the extensor mechanism to the new bone graft and severely limiting digital flexion.
- Fibrous Resection: Dissect the fibrous nonunion tissue en bloc from between the osseous fragments. Complete excision of this pseudarthrosis tissue is necessary to mobilize the distal fragment so that longitudinal traction can restore normal finger length.
2. Preparation of the Host Bone
The host bone must be prepared to receive the graft with exacting geometric precision.
* Proximal Fragment: Usually, the proximal fragment is sclerotic and must be sacrificed as far as its base to reach bleeding, healthy bone. Resect the proximal fragment with a sharp osteotome at an angle of exactly 30 degrees, creating a dorsal-facing recess in the bone. This 30-degree angle is biomechanically designed to resist the dorsal apex angulation forces exerted by the intrinsic muscles.
* Distal Fragment: Cut the end of the distal fragment transversely with an oscillating saw or a sharp rongeur. Use a burr or awl to open the medullary canal, preparing it to receive the doweled end of the graft.
3. Graft Harvesting and Fashioning
A structural autograft is required. While the iliac crest provides excellent cancellous bone, the tibial crest or medial tibial face is often preferred for the Littler technique due to its dense cortical structure, which can be precisely machined.
- Measurement: Apply longitudinal traction to the finger to restore its anatomical length. Measure the resulting defect between the prepared fragments.
- Harvest: Harvest a cortico-cancellous graft from the tibia (or other suitable site) that is at least 1.3 cm longer than the measured defect. This extra length is required for the dowel and the angled overlap.
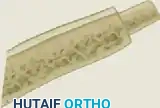

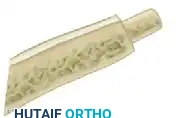
- Fashioning the Graft: As seen in the detailed graft images above, the "bone carpentry" must be exact:
- Distal End: Fashion a cylindrical dowel (peg) at one end of the graft. This dowel must match the inner diameter of the prepared distal metacarpal medullary canal.
- Proximal End: Cut the opposite end of the graft obliquely at a 30-degree angle to perfectly mate with the recess created in the proximal metacarpal base or carpus.
4. Graft Insertion and Fixation
- Insertion: Insert the doweled end of the graft into the medullary canal of the distal fragment. Next, apply longitudinal traction to the digit, distract the fragments, and press the 30-degree proximal end of the graft into the prepared proximal recess.
- Biomechanical Stability: Once traction is released, the natural resting tension of the intrinsic and extrinsic muscles compresses the graft between the two fragments, holding it firmly in place.
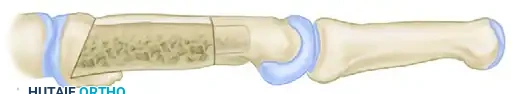
- Supplemental Fixation: While the geometric press-fit provides excellent inherent stability, supplemental fixation is often prudent to prevent rotational displacement. If necessary, stabilize the graft by passing one or more smooth Kirschner wires (K-wires) obliquely through the graft and into the adjacent, uninvolved metacarpals.
- Closure: If a periosteal sheath is present, close it over the graft to provide a vascularized cambium layer. Close the soft tissues and skin with fine, non-reactive sutures.
MANAGEMENT OF SECONDARY CONTRACTURES
Prolonged metacarpal shortening and nonunion frequently lead to secondary contractures of the adjacent joints, most notably the MCP joint.
Collateral Ligament Contracture
The MCP joint collateral ligaments are eccentric; they are lax in extension and taut in flexion. When a metacarpal is shortened or immobilized in extension for a prolonged period, these ligaments rapidly contract and fibrose.
* Capsulotomy: If intraoperative assessment reveals that MCP joint flexion is severely limited due to secondary collateral ligament contracture, a dorsal capsulotomy and collateral ligament release may be indicated concurrently with the bone grafting procedure.
* Technique: Carefully elevate the extensor mechanism, incise the dorsal capsule, and selectively release the dorsal fibers of the collateral ligaments until 70 to 90 degrees of passive MCP flexion is achieved.
POSTOPERATIVE CARE AND REHABILITATION PROTOCOL
The postoperative protocol must balance the need for rigid immobilization to allow osseous integration with the need to prevent irreversible joint stiffness.
Phase I: Immediate Postoperative Immobilization (Days 0-12)
- Positioning: The hand is placed in the classic "position of function" (intrinsic-plus position): the wrist extended 20-30 degrees, the MCP joints flexed 70-90 degrees, and the interphalangeal (IP) joints fully extended.
- Splinting: A bulky plaster cast or rigid splint is applied, extending to the proximal interphalangeal (PIP) joints.
Surgical Warning: Postoperative swelling following structural bone grafting in the hand can be severe. The cast or splint must be immediately split in the operating room to accommodate this swelling and prevent compartment syndrome or soft tissue necrosis.
- Pharmacology: Administration of prophylactic intravenous antibiotics during surgery is mandatory. Given the history of open trauma, oral antibiotics should be continued for several days postoperatively.
Phase II: Focused Immobilization (Day 12 to 2 Months)
- Cast Change: On approximately the 12th postoperative day, the initial bulky dressings and split cast are removed. Sutures are assessed and removed if the wound is adequately healed.
- Targeted Casting: A new, well-molded cast or custom thermoplastic splint is applied. This secondary orthosis is designed to immobilize only the grafted metacarpal and its corresponding proximal phalanx, leaving the adjacent uninvolved digits free to begin active range of motion (ROM) exercises.
- Duration: This targeted immobilization is left in place for a total of 2 months, or until radiographic evidence of bridging trabecular bone is confirmed at both the proximal and distal graft-host interfaces.
Phase III: Rehabilitation and Strengthening (Month 2 Onwards)
- Once clinical and radiographic union is achieved, immobilization is discontinued.
- Aggressive hand therapy is initiated, focusing on active and passive ROM of the MCP and IP joints, tendon gliding exercises, and progressive grip strengthening.
- If K-wires were utilized for supplemental fixation, they are typically removed in the clinic between 6 to 8 weeks postoperatively, prior to the initiation of aggressive mobilization.
COMPLICATIONS AND PITFALLS
Surgeons undertaking the Littler technique must be prepared to manage several potential complications:
- Graft Resorption or Nonunion: Usually the result of inadequate soft tissue coverage, thermal necrosis during bone preparation, or failure to completely resect the fibrous pseudarthrosis. Revision requires a fresh cortico-cancellous graft and potentially rigid plate fixation.
- Infection: A catastrophic complication that requires immediate hardware/graft removal, aggressive serial debridement, placement of an antibiotic spacer, and eventual staged reconstruction once the infection is definitively cleared.
- Extensor Tendon Adhesions: Preventable by meticulous preservation of the paratenon and early mobilization of uninvolved digits. If severe, a secondary tenolysis may be required 6-12 months after bone healing is complete.
- Malunion: Rotational malalignment is the most common error. It must be assessed intraoperatively by observing the cascade of the flexed digits; all fingertips should point toward the scaphoid tubercle. Supplemental K-wire fixation helps prevent postoperative shifting.
