Predictors of Hip Fracture Fixation Failure: Etiology, Biomechanics, & Prevention
Key Takeaway
Fixation failure in hip fractures is predicted by patient factors like osteoporosis, fracture biomechanics (e.g., high Pauwels angle, comminution), surgical technique (e.g., implant placement, load sharing), and vascular disruption. Understanding proximal femoral anatomy, bone quality, and fracture pattern stability is crucial for prevention and optimizing internal fixation outcomes.
Introduction and Epidemiology
Hip fractures represent a significant global health burden, primarily affecting the elderly population and carrying substantial morbidity and mortality. The incidence is projected to rise exponentially with an aging demographic, making their effective management a paramount orthopedic challenge. While internal fixation remains the preferred treatment modality for many hip fracture patterns, particularly in younger patients and specific stable fractures in the elderly, fixation failure remains a critical complication leading to revision surgery, prolonged recovery, and increased healthcare costs.
Fixation failure, encompassing implant cutout, migration, nonunion, malunion, and avascular necrosis, undermines the primary goal of restoring anatomical continuity and functional independence. The one-year mortality rate following a hip fracture in the elderly remains stubbornly high, approaching twenty to thirty percent, and this risk is compounded when revision surgery is required for failed fixation. Understanding and identifying the critical predictors of fixation failure are essential for optimizing patient selection, refining surgical techniques, and guiding post-operative management strategies.
This review consolidates current knowledge regarding the multifactorial nature of these predictors, ranging from patient-specific biological factors to biomechanical aspects of the fracture and technical nuances of surgical fixation. The primary predictors of failure can be broadly categorized into patient factors including severe osteoporosis and medical comorbidities, fracture factors including inherent instability and comminution, and surgeon factors including inadequate reduction and suboptimal implant positioning.
Surgical Anatomy and Biomechanics
Effective internal fixation of hip fractures hinges upon a thorough understanding of the proximal femoral anatomy and its inherent biomechanical properties, particularly in the context of compromised bone quality.
Proximal Femoral Osteology
The proximal femur comprises the femoral head, neck, and trochanteric regions. The femoral head articulates with the acetabulum and relies on a tenuous blood supply. The femoral neck connects the head to the shaft, characterized by a dense cortical shell and an intricate trabecular network. Its anteversion and valgus angulation are critical biomechanical features. Fractures here disrupt the primary weight-bearing trabeculae, specifically the medial compressive and lateral tensile trabecular systems. The intersection of these systems forms a relative void known as Wards triangle, which becomes increasingly prominent and structurally vulnerable in osteoporotic bone.
The trochanteric region serves as the attachment point for the primary hip musculature. The greater trochanter is the insertion site for the abductor complex, while the lesser trochanter serves as the insertion for the iliopsoas. The intertrochanteric region is largely cancellous, making it highly susceptible to comminution. The calcar femorale, a dense vertical plate of bone originating from the posteromedial aspect of the femoral shaft and extending into the posterior femoral neck, is a critical structural landmark. Loss of posteromedial support due to comminution of the calcar is a primary predictor of varus collapse and fixation failure in intertrochanteric fractures.
Vascular Anatomy of the Femoral Head
The vascularity of the femoral head is a critical consideration, especially in femoral neck fractures. The primary supply is derived from the medial circumflex femoral artery and the lateral circumflex femoral artery, which form an extracapsular arterial ring at the base of the femoral neck. The medial circumflex femoral artery is the dominant contributor, giving rise to the lateral epiphyseal artery via the retinacular vessels that ascend along the posterosuperior aspect of the femoral neck within the synovial reflection.
Displacement of femoral neck fractures tears or occludes these retinacular vessels, predisposing the femoral head to avascular necrosis and subsequent subchondral collapse. Intracapsular hematoma may also increase intra-articular pressure, potentially causing a tamponade effect on the remaining intact venous drainage and arterial supply, further compromising perfusion.
Biomechanical Principles of Hip Fixation
The proximal femur is subjected to substantial bending, shear, and compressive forces during weight-bearing and muscular contraction. Joint reaction forces across the hip can exceed three times body weight during normal gait. Internal fixation constructs are designed to counteract these forces, providing stability until biological healing occurs.
Ideal constructs promote load sharing between the implant and the bone, minimizing stress shielding and allowing physiological stress stimulation for callus formation in extracapsular fractures. Osteoporosis significantly reduces bone mineral density and architectural integrity, decreasing the pullout strength of screws and the purchase of intramedullary nails.
Fracture pattern stability dictates the biomechanical environment. In femoral neck fractures, instability is often related to displacement and comminution of the posterior cortex. The Pauwels classification, based on the angle of the fracture line relative to the horizontal, dictates the ratio of shear to compressive forces. High Pauwels angles inherently have higher shear forces, acting as a strong predictor for nonunion and fixation failure. In intertrochanteric fractures, stability is determined by the integrity of the posteromedial cortex and the lateral wall. A deficient lateral wall precludes the use of a sliding hip screw, as the proximal fragment will slide laterally, leading to massive shortening and construct failure.
Indications and Contraindications
The decision to proceed with operative fixation versus arthroplasty, or non-operative management, requires a careful assessment of patient physiology, chronological and biological age, ambulatory status, and precise fracture morphology. Internal fixation is generally indicated to preserve the native joint when the blood supply to the femoral head is presumed intact or when the patient is young enough that arthroplasty would inevitably lead to multiple future revisions.
In the elderly population with displaced femoral neck fractures, arthroplasty is generally preferred due to the unacceptably high rates of fixation failure, nonunion, and avascular necrosis associated with internal fixation. Conversely, stable intertrochanteric fractures are almost universally managed with internal fixation, utilizing either a sliding hip screw or a cephalomedullary nail.
| Variable | Operative Fixation Indications | Non Operative Management Indications | Arthroplasty Indications |
|---|---|---|---|
| Femoral Neck Fractures | Non-displaced fractures (Garden I and II); Displaced fractures in young patients (typically under 60 years); Basicervical fractures. | Non-ambulatory patients with minimal pain; Patients with unacceptable anesthetic risk (ASA V); Palliative care status. | Displaced fractures (Garden III and IV) in elderly patients; Pre-existing symptomatic hip osteoarthritis; Pathological fractures. |
| Intertrochanteric Fractures | Nearly all patterns (Stable and Unstable); Reverse obliquity patterns; Subtrochanteric extension. | Non-ambulatory, bedbound patients with minimal pain; Terminal illness with very short life expectancy. | Rarely indicated; Severe pre-existing osteoarthritis combined with highly comminuted osteoporotic bone (salvage). |
| Bone Quality | Adequate bone stock for screw purchase; Young patients regardless of density. | Severe osteopenia where surgical risk outweighs mobilization benefits. | Severe osteoporosis in femoral neck fractures where screw purchase is highly likely to fail. |
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is the foundation of successful hip fracture fixation. Failure to anticipate anatomical variations, fracture comminution, or necessary implant dimensions frequently leads to intraoperative compromises that increase the risk of subsequent fixation failure.
Radiographic Templating
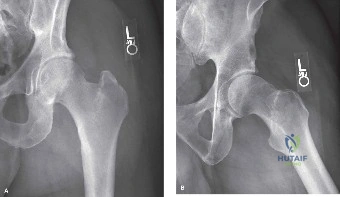
Standard preoperative imaging must include an anteroposterior pelvis radiograph and a cross-table lateral view of the affected hip. Traction-internal rotation views can be utilized to better delineate the fracture pattern and assess reducibility. Radiographic templating is mandatory to determine the native neck-shaft angle, the appropriate implant size, and the required length of the lag screw or cephalomedullary nail.
When templating for a cephalomedullary nail, the surgeon must assess the anterior bow of the femur to avoid anterior cortical impingement or perforation by the distal tip of the nail. The lateral wall thickness must be measured on the anteroposterior radiograph; a thickness of less than twenty point five millimeters is a strong predictor of lateral wall fracture during sliding hip screw insertion, necessitating the use of a cephalomedullary nail.

Operating Room Setup and Positioning
Positioning on a fracture table is the standard approach for most hip fracture fixations. The patient is placed supine with the bilateral lower extremities secured in traction boots. A perineal post is utilized to provide counter-traction. The unaffected leg is typically placed in a hemilithotomy position or scissored posteriorly to allow unobstructed access for the lateral fluoroscopy beam.
Gross reduction is achieved through longitudinal traction, followed by internal rotation to correct the typical external rotation deformity and restore femoral neck anteversion. The reduction must be confirmed on both anteroposterior and lateral fluoroscopic views before any incision is made. An unreduced fracture cannot be salvaged by perfect implant placement. If closed reduction is inadequate, the surgeon must be prepared to transition to an open reduction technique.
Detailed Surgical Approach and Technique
The surgical technique for hip fracture fixation requires precision. The primary objective is to achieve an anatomic or slightly valgus reduction, followed by the placement of a biomechanically sound implant that allows for controlled impaction without cutout.
Principles of Anatomic Reduction
Reduction is the single most important surgeon-controlled variable in preventing fixation failure. For femoral neck fractures, a varus malreduction increases shear forces across the fracture site and shifts the weight-bearing axis medially, drastically increasing the risk of cutout and nonunion. An anatomic or slight valgus reduction is required.
For intertrochanteric fractures, the medial and anterior cortices must be intimately opposed. Extramedullary reduction techniques, such as the use of a bone hook, percutaneous elevators, or collinear reduction clamps, should be employed if closed traction fails. Sagittal plane alignment is equally critical; posterior sag of the greater trochanteric fragment must be corrected to prevent apex anterior angulation, which restricts lag screw placement and leads to eccentric loading.
Surgical Approaches for Open Reduction
When closed or percutaneous reduction methods fail, open reduction is mandated. For femoral neck fractures, a Watson Jones approach utilizes the internervous plane between the tensor fasciae latae (superior gluteal nerve) and the gluteus medius (superior gluteal nerve). This approach provides excellent visualization of the anterior femoral neck. Capsulotomy allows for direct manipulation of the fracture fragments and evacuation of the fracture hematoma, which theoretically reduces intracapsular pressure and preserves residual blood supply.
For intertrochanteric fractures requiring open reduction, a direct lateral approach is utilized. The vastus lateralis is elevated from the lateral intermuscular septum or split longitudinally. This provides direct access to the lateral cortex for implant insertion and allows for the application of reduction forceps directly across the fracture site.
Implant Specific Fixation Techniques
For younger patients with femoral neck fractures, cannulated cancellous screws are frequently utilized. Three screws are typically placed in an inverted triangle configuration to maximize biomechanical stability. The inferior screw must be placed adjacent to the calcar to provide inferior cortical support, while the posterior screw should rest on the dense posterior cortex.
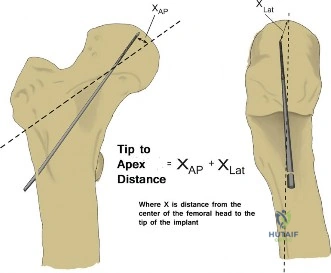
For stable intertrochanteric fractures, the sliding hip screw remains a gold standard. A guide pin is inserted into the femoral head, aiming for a center-center position on both anteroposterior and lateral fluoroscopic views. The concept of Tip Apex Distance, defined as the sum of the distance from the tip of the lag screw to the apex of the femoral head on both views, is critical. A Tip Apex Distance of less than twenty five millimeters has been definitively shown to minimize the risk of lag screw cutout.
For unstable intertrochanteric fractures, reverse obliquity patterns, or fractures with a deficient lateral wall, a cephalomedullary nail is indicated. The entry point is critical and varies based on the specific implant design, typically located at the tip of the greater trochanter or slightly medial. Eccentric reaming or an improper entry point can lead to varus malalignment or iatrogenic fracture of the lateral wall. The lag screw must again be placed perfectly in the center-center position, strictly adhering to the Tip Apex Distance principles.
Complications and Management
Despite meticulous technique, fixation failure and complications occur. Recognizing the early radiographic and clinical signs of failure is essential for timely intervention and salvage.
Etiology of Fixation Failure
Implant cutout is the most common mode of mechanical failure, characterized by the migration of the lag screw through the superior articular surface of the femoral head. Predictors of cutout include a Tip Apex Distance greater than twenty five millimeters, varus malreduction, superior placement of the lag screw, and severe osteoporosis. Once cutout occurs, the joint is rapidly destroyed, and revision surgery is mandatory.
Nonunion occurs when the fracture fails to consolidate, often presenting with persistent groin or thigh pain and progressive hardware failure, such as screw breakage or complete telescoping of the sliding mechanism. Predictors of nonunion include inadequate initial reduction, high Pauwels angle shear forces, and disruption of the vascular supply.
Avascular necrosis is a devastating complication primarily associated with femoral neck fractures. It results from the disruption of the retinacular vessels at the time of injury or due to elevated intracapsular pressure. It typically presents months to years after the index procedure with subchondral collapse and secondary osteoarthritis.

Salvage Arthroplasty Considerations
When internal fixation fails, salvage typically involves conversion to a total hip arthroplasty. This is a technically demanding procedure with complication rates significantly higher than primary arthroplasty.
Challenges include the removal of integrated or broken hardware, management of cavitary bone defects in the femoral head and neck, and addressing poor proximal femoral bone stock. The abductor musculature is often compromised from the initial trauma, previous incisions, and altered biomechanics, increasing the risk of postoperative dislocation. Surgeons must often utilize diaphyseal fitting stems, modular revision stems, or calcar replacing implants to achieve stable distal fixation bypassing the compromised proximal bone.
| Complication | Estimated Incidence | Primary Predictors and Etiology | Management and Salvage Strategy |
|---|---|---|---|
| Implant Cutout | 2 to 8 percent | TAD > 25mm; Varus malreduction; Superior screw placement; Osteoporosis. | Conversion to Total Hip Arthroplasty; Hemiarthroplasty if low demand. |
| Nonunion | 5 to 15 percent (Femoral Neck) | High shear forces (Pauwels III); Poor reduction; Inadequate fixation stability. | Valgus producing osteotomy (young patients); Conversion Arthroplasty (elderly). |
| Avascular Necrosis | 10 to 30 percent (Femoral Neck) | Initial fracture displacement; Disruption of retinacular vessels; Delayed fixation. | Core decompression (early stage); Conversion Total Hip Arthroplasty (late stage with collapse). |
| Surgical Site Infection | 1 to 3 percent | Medical comorbidities (Diabetes, Malnutrition); Prolonged operative time. | Aggressive irrigation and debridement; Hardware retention if fracture healing; Suppressive antibiotics. |
| Venous Thromboembolism | 1 to 5 percent | Immobility; Hypercoagulable state of trauma; Inadequate chemoprophylaxis. | Therapeutic anticoagulation; IVC filter if anticoagulation is strictly contraindicated. |
Post Operative Rehabilitation Protocols
The postoperative phase is critical for functional recovery and the prevention of medical complications. The overarching goal is early, safe mobilization to mitigate the risks of deep vein thrombosis, pulmonary embolism, pneumonia, decubitus ulcers, and postoperative delirium.
In the vast majority of cases, patients should be allowed weight-bearing as tolerated immediately following surgery. Biomechanical studies and clinical trials have demonstrated that modern fixation constructs in appropriately selected patients can withstand immediate physiological loading. Restricting weight-bearing in the elderly is often impractical, leads to deconditioning, and does not significantly decrease the rate of mechanical failure. Exceptions to immediate weight-bearing may include highly comminuted subtrochanteric extensions or cases where intraoperative fixation was deemed tenuous due to extreme osteoporosis.
Venous thromboembolism prophylaxis is mandatory, typically utilizing low molecular weight heparin or direct oral anticoagulants for a minimum of four weeks postoperatively, tailored to the patients specific bleeding risk profile.
Furthermore, a hip fracture is a sentinel event for severe osteoporosis. Secondary fracture prevention must be initiated prior to discharge. This includes a comprehensive endocrinology evaluation, dual energy x-ray absorptiometry scanning, and the initiation of appropriate pharmacological interventions, such as bisphosphonates or anabolic agents, to improve systemic bone mineral density and reduce the risk of contralateral hip fractures or vertebral compression fractures.
Summary of Key Literature and Guidelines
Evidence based practice in hip fracture management is guided by several landmark trials and established clinical guidelines. The FAITH (Fixation using Alternative Implants for the Treatment of Hip fractures) trial investigated the use of sliding hip screws versus cancellous screws for femoral neck fractures. It demonstrated that while overall revision rates were similar, the sliding hip screw provided a slight advantage in preventing avascular necrosis and revision in displaced fractures and basicervical patterns.
The HEALTH (Hip Fracture Evaluation with Alternatives of Total Hip Arthroplasty versus Hemiarthroplasty) trial, while focused on arthroplasty, highlighted the importance of proper patient selection for fixation versus replacement, noting that total hip arthroplasty provides superior functional outcomes but carries a higher risk of dislocation compared to hemiarthroplasty in the elderly.
The concept of Tip Apex Distance, originally described by Baumgaertner et al., remains one of the most highly cited and clinically relevant predictors of fixation failure. Their work unequivocally established that a Tip Apex Distance of less than twenty five millimeters is the most important surgeon controlled variable in preventing lag screw cutout.
The American Academy of Orthopaedic Surgeons clinical practice guidelines strongly recommend early surgery, ideally within twenty four to forty eight hours of admission, to reduce mortality and complication rates. The guidelines also emphasize the necessity of co-management with geriatric or internal medicine services to optimize preoperative medical status and manage postoperative medical complications, reflecting the multidisciplinary approach required to successfully treat this fragile patient population.
