Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 51-year-old man sustained an open fracture of his tibia in Korea 42 years ago. An infection developed and it was resolved with surgical treatment. For the past 6 months, an ulcer with mild drainage has developed over the medial tibia. The ulcer is small and there is minimal erythema at the ulcer site. A radiograph and MRI scan are shown in Figures 43a and Figure 43b. Initial cultures show Staphylococcus aureus susceptible to the most appropriate antibiotics. Laboratory studies show an erythrocyte sedimentation rate of 70 mm/h. What is the most appropriate surgical treatment at this time?
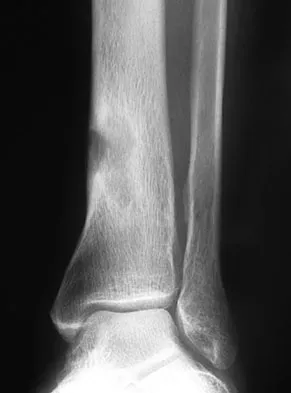
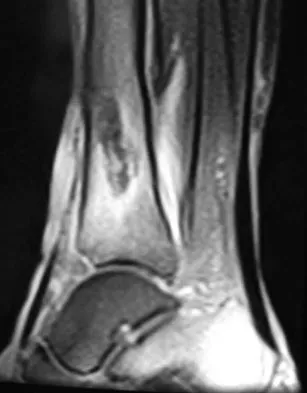
Explanation
The patient has chronic tibial osteomyelitis that is due to low virulent bacteria. The history and studies do not suggest the need for an amputation or a free-flap procedure. This is a localized tibial infection that is in a healed bone; there is no need to resect the entire area of the tibia bone around the infection. The most appropriate treatment is curettage, debridement of nonviable bone, and placement of absorbable antibiotic beads, followed by a course of IV antibiotics from 1 to 4 weeks and a 6-week course of oral antibiotics. Studies have shown that in cases of localized osteomyelitis that are of low virulence, as little as 1 week of IV antibiotics followed by 6 weeks of oral antibiotics is successful. Patzakis MJ, Zalavras CG: Chronic posttraumatic osteomyelitis and infected nonunion of the tibia: Current management concepts. J Am Acad Orthop Surg 2005;13:417-427.
Question 2
Figures 5a and 5b show axial and coronal MRI images of the left ankle of a patient with lateral ankle pain. What is the most likely diagnosis?
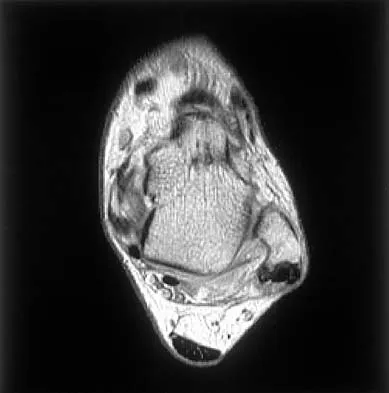
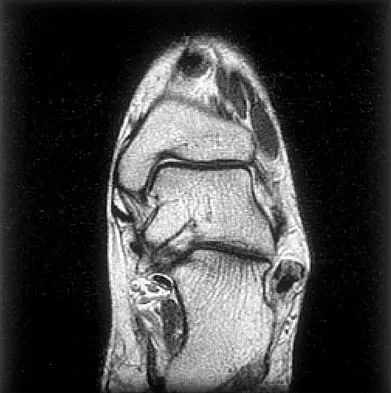
Explanation
The figures show a longitudinal split within the peroneus brevis tendon as it courses posterior to the fibula. The peroneus longus tendon has been driven between the medial and lateral components of the peroneus brevis tendon. Peroneal split syndrome is a cause of lateral ankle pain but may be less asymptomatic in the elderly. It may be associated with tendon subluxation following a tear of the superior peroneal retinaculum.
Question 3
A 25-year-old man is brought to the emergency department following a motor vehicle accident. Extrication time was 2 hours, and in the field he had a systolic blood pressure by palpation of 90 mm Hg. Intravenous therapy was started, and on arrival in the emergency department he has a systolic blood pressure of 90 mm Hg with a pulse rate of 130. Examination reveals a flail chest and a femoral diaphyseal fracture. Ultrasound of the abdomen is positive. The trauma surgeons take him to the operating room for an exploratory laparotomy. At the conclusion of the procedure, he has a systolic pressure of 100 mm Hg with a pulse rate of 110. Oxygen saturation is 90% on 100% oxygen, and he has a temperature of 95.0 degrees F (35 degrees C). What is the recommended treatment of the femoral fracture at this time?
Explanation
This is a "borderline trauma" patient where serious consideration for damage control orthopaedic surgery is required. His prolonged hypotension, abdominal injury, and chest injury put him at higher risk for serious postinjury complications. Further surgery, such as definitive fracture fixation, adds metabolic load and injury to his system. It is prudent to consider femoral fracture stabilization with an external fixator until he is physiologically recovered as evidenced by a normal base excess and/or lactate acid levels, as well as all other parameters of resuscitation. A borderline patient has been described as polytrauma with an ISS > 20 and thoracic trauma (AIS > 2); polytrauma and abdominal/pelvic trauma (Moore > 3) and hemodynamic shock (initial BP < 90 mm Hg); ISS > 40; bilateral lung contusions on radiographs; initial mean pulmonary arterial pressure > 24 mm Hg; pulmonary artery pressure increase during intramedullary nailing > 6 mm Hg. Factors that worsen the situation following surgery include multiple long bones and truncal injury (AIS > 2), estimated surgery time of more than 6 hours, arterial injury and hemodynamic instability, and exaggerated inflammatory response (eg, Il-6 > 800 pg/mL). It is incumbent on the orthopaedic surgeon who is a member of the trauma team to make sure that he or she is aware of these factors and guides the team to the best patient care. Pape HC, Hildebrand F, Pertschy S, et al: Changes in the management of femoral shaft fractures in polytrauma patients: From early total care to damage control orthopaedic surgery. J Trauma 2002;53:452-461.
Question 4
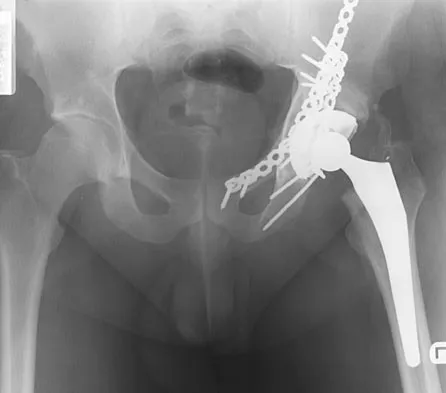
A 32-year-old man has posttraumatic arthritis after undergoing open reduction and internal fixation of a left acetabular fracture. A total hip arthroplasty is performed, and the radiograph is shown in Figure 18. What is the most common mode of failure leading to revision in this group of patients?
Explanation
Acetabular component loosening has been reported as the most common mode of failure following total hip arthroplasty in patients with a previous acetabular fracture. Following acetabular fracture and subsequent open reduction and internal fixation, the bone quality and vascularity are compromised, thus reducing the success rate of acetabular component cementless fixation. Jimenez ML, Tile M, Schenk RS: Total hip replacement after acetabular fracture. Orthop Clin 1997;28:435-446.
Question 5
Examination of a carpenter who hit his thumb with a hammer reveals that the nail plate is broken but in place, and there is a 100% subungual hematoma that covers 100% of the area under the nail plate. Radiographs reveal a comminuted distal phalangeal tuft fracture. Management should consist of
Explanation
This is a classic situation for a distal phalanx tuft fracture with associated nail bed injury and subungual hematoma. In general, when the subungual hematoma is greater than 50% of the surface area under the nail plate, treatment should consist of nail plate removal, nail bed repair, oral antibiotics, and a fingertip splint. Oral antibiotics and fingertip splinting alone do not address the nail bed laceration, which will most likely lead to nail plate deformity if not repaired. Kirschner pin stabilization is not indicated because these fractures are nondisplaced and usually are inherently stable after nail bed repair. The use of IV antibiotics alone does not address the nail bed laceration surgically. Casting, followed by hydrotherapy and topical antibiotics, is not indicated because it does not address the nail bed laceration. Further, a nondisplaced distal phalangeal tuft fracture does not require cast immobilization. Stern PJ: Fractures of the metacarpals and phalanges, in Green DP, Hotchkiss RN, Pederson WC (eds): Green's Operative Hand Surgery, ed 4. Philadelphia, PA, 1999, pp 711-771.
Question 6
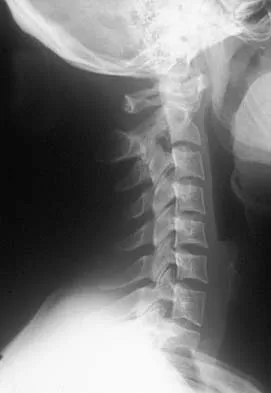
A 62-year-old man with a long history of ankylosing spondylitis has neck pain after lightly bumping his head on the wall. Examination reveals neck pain with any attempted motion; the neurologic examination is normal. Plain radiographs show extensive ankylosis of the cervical spine and kyphosis but no fracture. What is the next most appropriate step in management?
Explanation
A high level of suspicion must be given for a fracture in any patient with ankylosing spondylitis who reports neck pain, even with minimal or no trauma. The neck should be immobilized in its normal position, which is often kyphotic, and plain radiographs should be obtained. If no obvious fracture is seen, CT with reconstruction should be obtained. The placement of in-line traction can have catastrophic effects because it may malalign the spine. Brigham CD: Ankylosing spondylitis and seronegative spondyloarthropathies, in Clark CR (ed): The Cervical Spine, ed 3. Philadelphia, PA, Lippincott Raven, 1998, pp 724-727.
Question 7
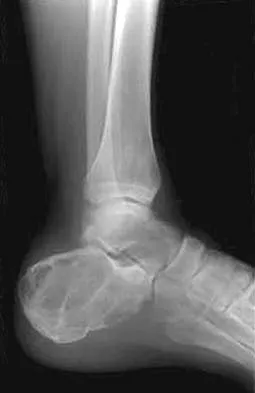
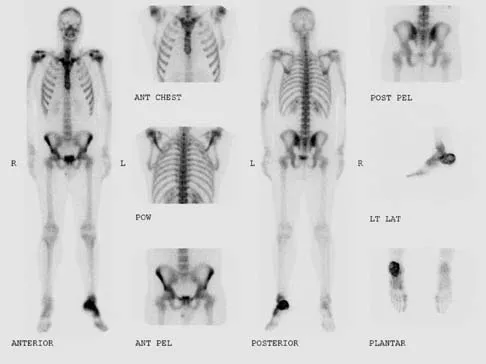
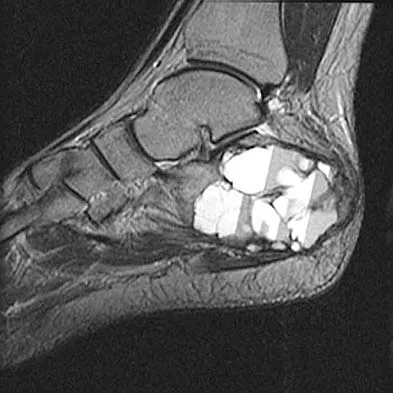
A 23-year-old man has had heel pain and fullness for the past several months. He reports that initially the pain was present only with activity, but more recently the pain has become constant. Figures 53a through 53d show a radiograph, a bone scan, and T2-weighted and gadolinium MRI scans. What is the most likely diagnosis?
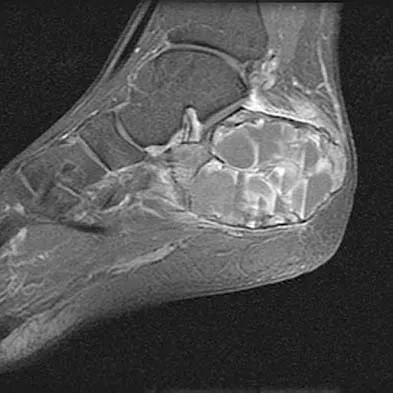
Explanation
The imaging studies reveal an expansile lesion with the classic soap bubble appearance that involves most of the calcaneus. The bone scan reveals a very active lesion with intense uptake, and the MRI scans show the classic, loculated appearance of the lesion with multiple fluid-fluid levels. While it is important to rule out telangiectatic osteosarcoma, the most likely diagnosis is an aneurysmal bone cyst. While giant cell tumor might have a similar appearance, the multiple fluid levels in a expansile lesion strongly favor an aneurysmal bone cyst. Parsons TW: Benign bone tumors, in Fitzgerald RH, Kaufer H, Malkani AL (eds): Orthopaedics. St Louis, MO, Mosby, 2002, pp 1027-1035.
Question 8
A 27-year-old woman has a bilateral C5-C6 facet dislocation and quadriparesis after being involved in a motor vehicle accident. Initial management consisted of reduction with traction, but she remains a Frankel A quadriplegic. To facilitate rehabilitation, surgical stabilization and fusion is planned. From a biomechanical point of view, which of the following techniques is the LEAST stable method of fixation?
Explanation
In two different biomechanical studies performed in both bovine and human cadaveric spines, all posterior techniques of stabilization were found to be superior to anterior plating in flexion-distraction injuries of the cervical spine. These injuries usually have an intact anterior longitudinal ligament that allows posterior fixation to function as a tension band. Anterior plating with grafting destroys this last remaining stabilizing structure and does not allow for a tension band effect because all of the posterior stabilizing structures have been destroyed with the injury. In clinical practice, however, anterior plating can be effective in the treatment of this injury with appropriate postoperative orthotic management. Sutterlin CE III, McAfee PC, Warden KE, et al: A biomechanical evaluation of cervical spine stabilization methods in a bovine model: Static and cyclical loading. Spine 1988;13:795-802.
Question 9
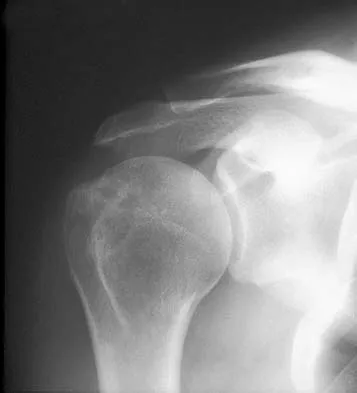
A 65-year-old woman landed on her nondominant left shoulder in a fall. An AP radiograph is shown in Figure 39. Management should consist of
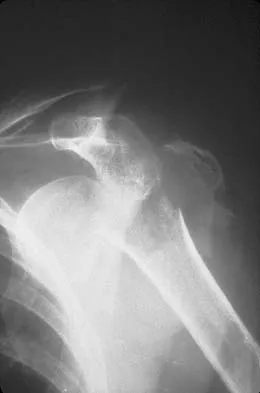
Explanation
The radiograph reveals a four-part fracture-dislocation of the proximal humerus. Humeral hemiarthroplasty and tuberosity repair is the treatment of choice because the risk of osteonecrosis is high after attempted repair of this injury. Glenoid resurfacing is reserved for acute fractures in which there is significant preexisting glenoid arthrosis, such as in patients with rheumatoid arthritis. Neer CS II: Displaced proximal humeral fractures: II. Treatment of three- and four-part displacement. J Bone Joint Surg Am 1970;52:1090-1103.
Question 10
What is the primary intracellular signaling mediator for bone morphogenetic protein (BMP) activity?
Explanation
BMPs signal through the activation of a transmembrane serine/threonine kinase receptor that leads to the activation of intracellular signaling molecules called SMADs. There are currently eight known SMADs, and the activation of different SMADs within a cell leads to different cellular responses. The other mediators are not believed to be directly involved with BMP signaling. Lieberman J, Daluiski A, Einhorn TA: The role of growth factors in the repair of bone: Biology and clinical applications. J Bone Joint Surg Am 2002;84:1032-1044. Li J, Sandell LJ: Transcriptional regulation of cartilage-specific genes, in Rosier RN, Evans C (eds): Molecular Biology in Orthoapedics, Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 21-24.
Question 11
A 29-year-old man reports severe knee instability and popliteal pain. History reveals that he had polio of the left lower extremity as a child and has been brace-free his entire life. Examination reveals that he walks with 40 degrees of knee hyperextension and has a fixed ankle equinus deformity of 30 degrees. He has no active motors about the knee or ankle. Which of the following methods will provide knee stability and pain relief?
Explanation
The ankle equinus allows the patient to keep his weight-bearing line anterior to the axis of the hyperextended knee joint. With time, pain has developed because of continued stretching and now incompetence of the posterior capsule of the knee joint. Several soft-tissue and bony procedures have been designed to provide knee stability in this situation; however, the results have been either short-lived or inconsistent. Tenodeses, capsular plications, and bony blocks have had limited success and generally fail over time. Current orthotic technology makes soft-tissue release and orthotic control the most predictable option. To decrease the hyperextension moment on the knee joint, the ankle deformity also must be corrected. The most predictable method of achieving stability and diminished pain during walking is with soft-tissue release of the ankle and a knee-ankle-foot orthosis with a locked ankle and drop-lock knee joint.
Question 12
The gluteus maximus is innervated by which of the following nerves?
Explanation
The inferior gluteal nerve supplies the gluteus maximus muscle. The superior gluteal nerve supplies the gluteus medius, gluteus minimus, and tensor fascia lata muscles. The femoral nerve supplies the quadriceps, sartorius, and pectineus muscles. The pudendal nerve is primarily a sensory nerve.
Question 13
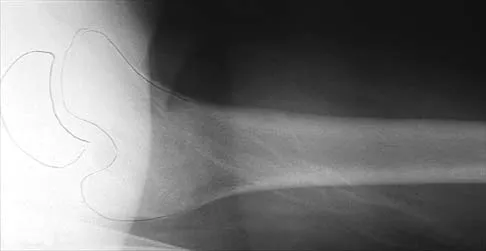
Figures 20a and 20b show the radiographs of an obese 15-year-old boy who has severe left groin pain and is unable to bear weight following a minor injury. Treatment should consist of
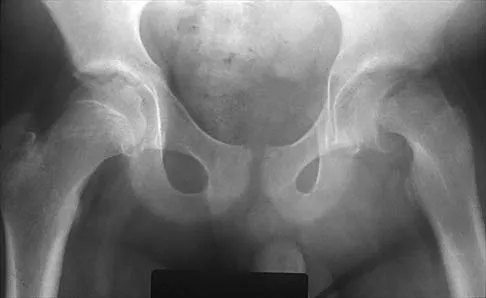
Explanation
The radiographs and history are consistent with an acute unstable slipped capital femoral epiphysis. Aronson and Loder documented an increased rate of osteonecrosis associated with manipulative reduction. They recommended bed rest with skin traction to allow the synovitis to resolve, followed by in situ pinning. They noted, however, that many of these slips reduced with anesthesia and positioning on a fracture table. Biomechanic studies have shown a slight increased resistance to shear stress when two screws are used, but it is unknown if this is significant in the clinical setting. Open epiphyseodesis does not provide postoperative stability; therefore, adjunctive fixation or immobilization is required. Numerous studies have noted the inadvisability of using multiple screws. Casting has a high rate of complications, including chondrolysis and progression of the slip. Aronson DD, Loder RT: Treatment of the unstable (acute) slipped capital femoral epiphysis. Clin Orthop 1996;322:99-110. Karol LA, Doane RM, Cornicelli SF, Zak PA, Haut RC, Manoli A II: Single versus double screw fixation for treatment of slipped capital femoral epiphysis: A biomechanical analysis. J Pediatr Orthop 1992;12:741-745.
Question 14
What is the most common nonanesthetic-related reversible cause of changes in intraoperative neurophysiologic monitoring data?
Explanation
Patient positioning that results in local nerve compression, plexus traction, or improper neck alignment is the most common nonanesthetic-related cause of changes in intraoperative neurophysiologic monitoring data during spinal surgery. Jones SC, Fernau R, Woeltjen BL: Use of somatosensory evoked potentials to detect peripheral ischemia and potential injury resulting from positioning of the surgical patient: Case reports and discussion. Spine J 2004;4:360-362.
Question 15
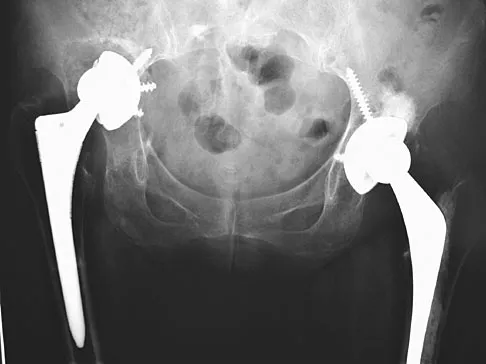
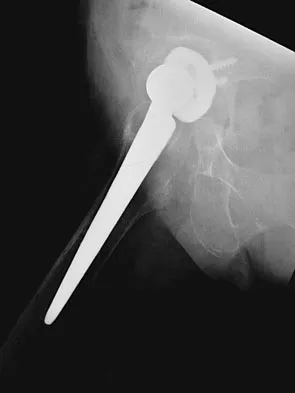
A 72-year-old woman who underwent right total hip arthroplasty 7 years ago now reports right hip pain and limb shortening. Studies for infection are negative. AP and lateral radiographs are shown in Figures 13a and 13b. What is the most appropriate management?
Explanation
Current literature supports the use of reinforcement cages for the reconstruction of failed, loosened acetabular components associated with major bone loss as seen in this patient. Although results of revision using the so-called jumbo cup with screws generally have been good, the amount of bone loss and medial wall penetration shown here and the likelihood of pelvic discontinuity precludes the use of that technique. With either technique, bone grafting of remaining defects is recommended. Sporer SM, O'Rourke M, Paprosky WG: The treatment of pelvic discontinuity during acetablular revision. J Arthroplasty 2005;20:79-84.
Question 16
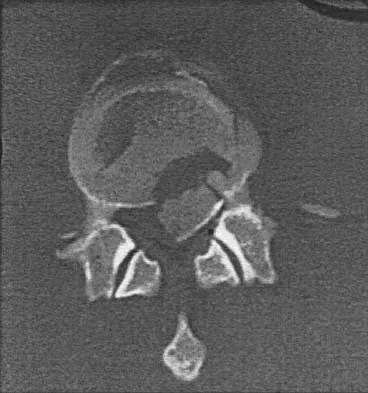
Figure 12 shows the lumbar CT scan of a 24-year-old man who was injured in a snowmobile accident. What is the mechanism of injury?
Explanation
A true compression fracture is a single-column injury that does not create canal compromise. A burst fracture is a two- or three-column injury that disrupts the middle column and thereby narrows the spinal canal. This patient has a burst fracture. The mechanism of injury is usually vertical compression or flexion compression. Garfin SR, Vaccaro AR (eds): Orthopaedic Knowledge Update: Spine. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1997, pp 197-217.
Question 17
Which of the following best characterizes the antigenicity of allograft bone?
Explanation
Cell surface glycoproteins present in the heterogeneous population of the cells within the graft are primarily responsible for the antigenicity. Macromolocules of the matrix have also been implicated. Cryopreserved grafts have less antigenicity than fresh. Freezing, freeze-drying, or chemical sterilization and antigen extraction of the bone allograft have all been shown to reduce the antigenicity of the graft. Freeze-drying of retroviral-infected cortical bone and tendon does not inactivate retrovirus. Immunosuppression has been shown to decrease response. Hematopoietic elements along with osteogenic, chondrogenic, fibrous, and vascular cells have been shown to be antigenic. Crawford MJ, Swenson CL, Arnoczky SP, et al: Lyophilization does not inactivate infectious retrovirus in systemically infected bone and tendon allografts. Am J Sports Med 2004;32:580-586. Stevenson S, Li XQ, Davy DT, et al: Critical biological determinants of incorporation of non-vascularized cortical bone grafts: Quantification of a complex process and structure. J Bone Joint Surg Am 1997;79:1-16.
Question 18
A 55-year-old woman fell and sustained an elbow dislocation with a coronoid fracture and a radial head fracture. The elbow is reduced and splinted. What is the most common early complication?
Explanation
The patient has a dislocation of the elbow with displaced coronoid process and radial head fractures. The elbow is extremely unstable after this injury, and recurrent dislocation in a splint is the most common early complication. Skeletal stabilization of the fractures is required to restore stability of the joint. Characteristics of the fractures will determine the techniques required to restore stability. Ring D, Jupiter JB, Zilberfarb J: Posterior dislocation of the elbow with fractures of the radial head and coronoid. J Bone Joint Surg Am 2002;84:547-551.
Question 19
An 18-month-old boy with obstetric brachial plexus palsy is being evaluated for limited right shoulder motion. Physical therapy for the past 6 months has failed to result in improvement of the contracture. Which of the following studies is necessary prior to any shoulder reconstruction?
Explanation
The child sustained a brachial plexus injury at birth, and internal rotation/adduction contractures frequently develop at the shoulder. Initial treatment should consist of physical therapy to increase the range of motion. If this fails, as in this patient, MRI is used to evaluate the glenohumeral joint. Commonly, there is joint deformity with increased retroversion of the glenoid and even posterior shoulder subluxation. If the deformity is mild, an anterior release, coupled with teres major and latissimus transfers, is very effective. If the deformity is severe and the shoulder is unreconstructable, then humeral derotation osteotomy is the procedure of choice. MRI of the brain, a radiograph of the elbow, and aspiration of the shoulder would not be helpful. Waters PM: Update on management of pediatric brachial plexus palsy. J Pediatr Orthop B 2005;14:233-244. Waters PM, Bae DS: Effect of tendon transfers and extra-articular soft-tissue balancing on glenohumeral development in brachial plexus birth palsy. J Bone Joint Surg Am 2005;87:320-325.
Question 20
A 45-year-old woman awakens with the acute onset of burning left shoulder pain that radiates toward the axilla. She denies any history of trauma. On examination, she is unable to abduct her arm but has full passive shoulder motion. Her sensation is intact. Cervical spine examination reveals full range of motion and a negative Spurling's test. Radiographs and MRI studies are normal for the cervical spine and shoulder. What is the most likely diagnosis?
Explanation
The definition of brachial neuritis or Parsonage-Turner syndrome is a rare disorder of unknown etiology that causes pain or weakness of the shoulder and upper extremity. The loss of active motion excludes cervical C6-7 radiculopathy and impingement. A normal MRI scan and full passive motion exclude a rotator cuff tear and adhesive capsulitis, respectively. Misamore GW, Lehman DE: Parsonage-Turner syndrome (acute brachial neuritis). J Bone Joint Surg Am 1996;78:1405-1408.
Question 21
Wear particles of ultra-high molecular weight polyethylene that are generated by total hip implants are predominantly of what diameter?
Explanation
Multiple studies have shown that the size of an ultra-high molecular weight polyethylene particle generated by total hip implants is typically less than 1 micron. This finding is significant in that particles of that size are readily phagocytized by macrophages. Campbell P, Ma S, Yeom B, McKellop H, Schmalzried TP, Amstutz HC: Isolation of predominantly submicron-sized UHMWPE wear particles from periprosthetic tissues. J Biomed Mater Res 1995;29:127-131. Shanbhag AS, Jacobs JJ, Glant TT, Gilbert JL, Black J, Galante JO: Composition and morphology of wear debris in failed uncemented total hip replacement. J Bone Joint Surg Br 1994;76:60-67.
Question 22
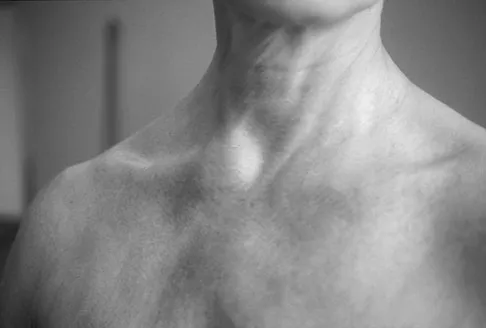
A 57-year-old man with type I diabetes mellitus has had a tender, erythematous right sternoclavicular joint for the past 2 weeks. Radiographs reveal mild osteolysis without arthritic changes, within normal limits. Management should consist of
Explanation
Sternoclavicular joint sepsis is a rare condition that is most often restricted to patients who are immunocompromised, diabetic, or IV drug abusers. Examination commonly reveals a tender, painful, and possibly swollen sternoclavicular joint. If suspicion remains high following a thorough history, physical examination, radiographs, and routine blood tests, joint aspiration should be performed prior to incision and drainage or administration of antibiotics. Bremner RA: Monarticular noninfected subacute arthritis of the sternoclavicular joint. J Bone Joint Surg Br 1959;41:749-753.
Question 23
What does Dual Energy X-ray Absorptiometry (DEXA) testing, as a technique, measure?
Explanation
DEXA can provide data on bone mineral content and soft-tissue composition, and requires cross-sectional dimension for accuracy. DEXA provides a quantitative, not qualitative, measurement of bone mineral content and is incapable of differentiating between trabecular and cortical bone. Osteoarthritis falsely elevates the values, especially in the AP spinal analysis. Genant HK, Faulkner KG, Gluer CC: Measurement of bone mineral density: Current status. Am J Med 1991;91:49S-53S. Genant HK, Engelke K, Fuerst T, et al: Review: Noninvasive assessment of bone mineral density and stature: State of the art. J Bone Miner Res 1996;11:707-730.
Question 24
A 21-year-old college student reports hearing a pop and has acute pain laterally over the ankle after twisting it during a recreational basketball game. Examination 1 hour after the injury reveals minimal swelling and ecchymosis. The anterior drawer sign is positive. Radiographs reveal no evidence of a fracture. What is the best course of action?
Explanation
Even though the patient has a grade 3 ankle ligament injury, studies have shown that 95% of patients with a grade 3 injury that may include a complete tear of the ligaments will heal successfully with conservative functional management. Extensive diagnostic evaluation with stress radiographs, CT, and MRI is not indicated. Surgical reconstruction is not indicated because of the overwhelming success of conservative management; however, in the few patients where late instability develops, surgical reconstruction offers an excellent outcome. Carne P: Nonsurgical treatment of ankle sprains using the modified Sarmiento brace. Am J Sports Med 1989;17:253-257.
Question 25
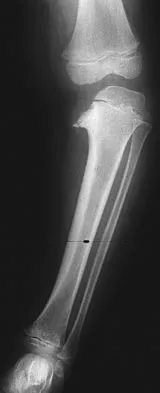
A 2-year-old child has refused to bear weight on his leg for the past 2 days. His parents report that he will crawl, has no fever, and has painless full range of motion of his hip and knee. Examination reveals no deformity or bruising, but there is mild swelling and tenderness over the anterior tibia. C-reactive protein, WBC count, and erythrocyte sedimentation rate studies are normal. Radiographs are negative. What is the best course of action?
Explanation
Despite the negative radiographic findings, the child's age and presentation are most consistent with a toddler's fracture. There is often not a witnessed injury. The differential diagnosis of infection is unlikely given that the child is afebrile and shows no signs of illness. Immobilization will make the child more comfortable and will often allow weight bearing. Repeat radiographs at the end of treatment will show a healing fracture and confirm the diagnosis. Aspiration of the tibial metaphysis would be indicated to obtain material for culture. The bone scan and MRI would show abnormalities, but these studies are nonspecific, costly, and time-consuming. Occasionally, oblique radiographs will show the fracture. Halsey MF, Finzel KC, Carrion WV, Haralabatos SS, et al: Toddler's fracture: Presumptive diagnosis and treatment. J Pediatr Orthop 2001;21:152-156.
Question 26
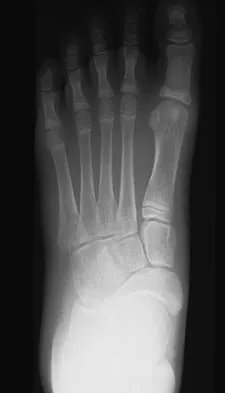
A 52-year-old woman who underwent cheilectomy 1 year ago for hallux rigidus now reports continued pain in the first metatarsophalangeal joint. She did not have any incision healing problems, and has not had any fevers, erythema, or drainage. Which of the following procedures will provide the best combination of pain relief and function?
Explanation
All but the Moberg osteotomy are capable of providing pain relief; however, arthrodesis offers the best long-term results and restores weight bearing and propulsion function to the first ray. Machacek F Jr, Easley ME, Gruber F, et al: Salvage of a failed Keller resection arthroplasty. J Bone Joint Surg Am 2004;86:1131-1138.
Question 27
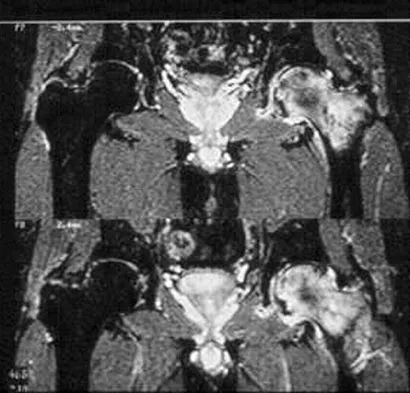
A 52-year-old man has had groin and deep buttock pain for the past 2 months. Examination reveals that hip range of motion is mildly restricted, and he has pain with both weight bearing and at rest. An MRI scan is shown in Figure 28. Management should consist of
Explanation
The MRI findings show highly increased signal through the entire femoral head and neck that is diagnostic of transient osteoporosis of the femoral head. This recently described entity is often seen in middle-aged men and should be treated nonsurgically with protected weight bearing and anti-inflammatory drugs. The natural history is that of self-resolution. Guerra JJ, Steinberg ME: Distinguishing transient osteoporosis from avascular necrosis of the hip. J Bone Joint Surg Am 1995;77:616-624.
Question 28
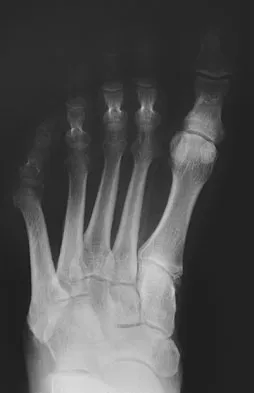
A 61-year-old man has a symptomatic bunionette that is refractory to nonsurgical management. A radiograph is shown in Figure 6. What is the optimal surgical correction?
Explanation
The patient has a bunionette with a large 4-5 intermetatarsal angle. This requires not only ostectomy of the lateral prominence but metatarsal osteotomy to decrease the intermetatarsal angle. Excising the head results in a flail joint and creates the possibility of a transfer lesion. Condylectomy can reduce plantar pressures but does not address the bunionette. The joint surface is well maintained, thus there are no indications for resection. Coughlin MJ: Treatment of bunionette deformity with longitudinal diaphyseal osteotomy with distal soft tissue repair. Foot Ankle 1991;11:195-203.
Question 29
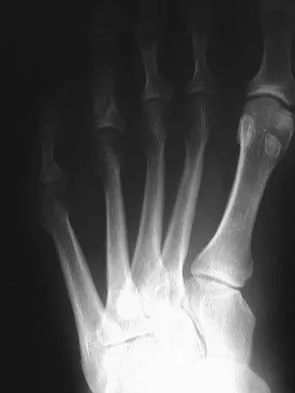
Figure 30 shows the radiograph of a 38-year-old man who reports persistent pain laterally and plantarly about the fifth metatarsal head. Examination reveals calluses dorsolaterally and plantarly about the fifth metatarsal head. Nonsurgical management has failed to provide relief. Surgical treatment should include
Explanation
The patient has painful lateral and plantar keratoses with metatarsus quintus valgus deformity. This combination of problems is best addressed with an oblique mid-diaphyseal osteotomy that allows the distal metatarsal to be displaced medially and dorsally. Lateral eminence resection alone will not address the painful plantar keratosis. A distal chevron osteotomy has a more limited ability to address the plantar keratosis (if translated medially and slight dorsally). Proximal diaphyseal osteotomies of the fifth metatarsal are associated with an increased risk of delayed union or nonunion secondary to the relative hypovascularity in the proximal diaphysis. Excision of the fifth metatarsal head can result in a floppy fifth toe and transfer metatarsalgia. Coughlin MJ: Treatment of bunionette deformity with longitudinal diaphyseal osteotomy with distal soft tissue repair. Foot Ankle 1991;11:195-203.
Question 30
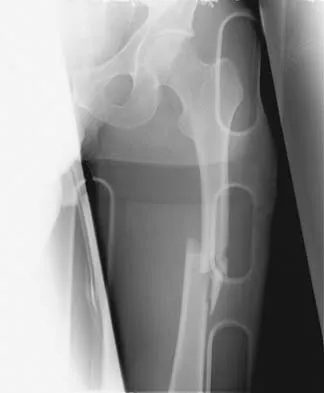
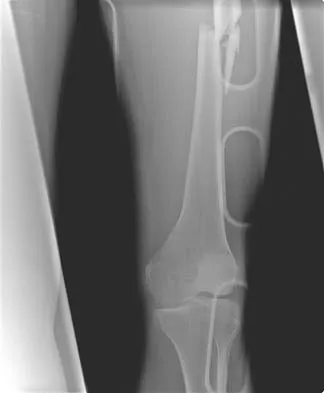
A 25-year-old man sustained the closed injury shown in Figures 22a and 22b. Examination reveals that this is an isolated injury, and he is hemodynamically stable. Treatment should consist of
Explanation
The treatment of choice for closed diaphyseal femoral fractures in adults is reamed intramedullary nailing with static interlocking. Reaming allows placement of a larger, stronger implant and offers better healing rates than unreamed nailing. Static interlocking ensures that there is no loss of reduction because of underappreciated fracture lines or comminution. Brumback RJ, Virkus WW: Intramedullary nailing of the femur: Reamed versus nonreamed. J Am Acad Orthop Surg 2000;8:83-90.
Question 31
A 24-year-old man sustained a grade IIIb open tibial fracture and an ipsilateral grade IIIa femoral fracture in a motorcycle accident. He is unresponsive, intubated, and has a Glasgow Coma Scale score of 8. He is resuscitated and taken to the operating room for definitive orthopaedic care. Which of the following intraoperative problems will most likely adversely affect his long-term outcome?
Explanation
Traumatic brain injury is considered to be either primary or secondary. Primary injury is direct or impact damage to the brain, and secondary injury can have intracranial or systemic causes. While treatment has little impact on primary brain injury, secondary brain injury can be avoided. There are also many causes of intracranial secondary brain injury, including intracranial hypertension or cerebral edema. There are many causes of systemic secondary brain injury, but none has a greater impact on outcome than hypotension or hypoxia. In fact, the occurrence of hypotension postinjury causes a 10- to 15-fold increase in mortality. In a series by Pietropaoli and associates, the mortality rate for head-injured patients that were normotensive during surgery was 25%, but if they were hypotensive the mortality rate was 82%. In the same series, the number of patients with a Glasgow Coma Scale score of either 4 or 5 dropped from 58% in those patients that were normotensive during surgery to 6% in those patients that became hypotensive during surgery. Efforts to avoid hypotension postinjury and especially during surgery should be of primary importance. Chesnut RM, Marshall LF, Klauber MR, et al: The role of secondary brain injury in determining outcome from severe head injury. J Trauma 1993;34:216-222. Pietropaoli JA, Rogers FB, Shackford SR, Wald SL, Schmoker JD, Zhuang J: The deleterious effects of intraoperative hypotension on outcome in patients with severe head injury. J Trauma 1992;33:403-407. Schmeling GJ, Schwab JP: Polytrauma care: The effect of head injuries and timing of skeletal fixation. Clin Orthop 1995;318:106-116.
Question 32
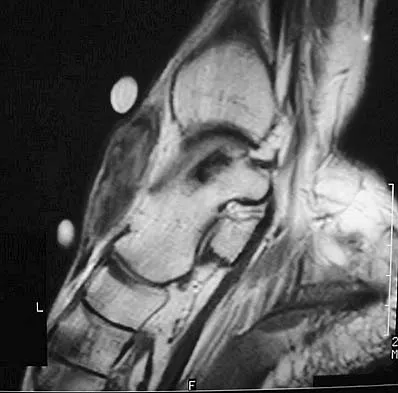
A 40-year-old man has a palpable mass over the dorsum of the ankle. He reports no history of direct trauma but notes that he sustained a laceration to the middle of his leg 6 weeks ago. Examination reveals a 4-cm x 1-cm mass. T1- and T2-weighted MRI scans are shown in Figures 12a and 12b. An intraoperative photograph and biopsy specimen are shown in Figures 12c and 12d. What is the most likely diagnosis?
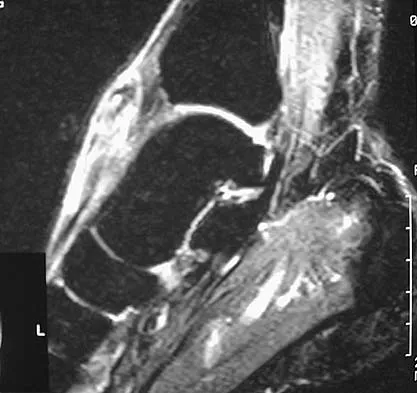
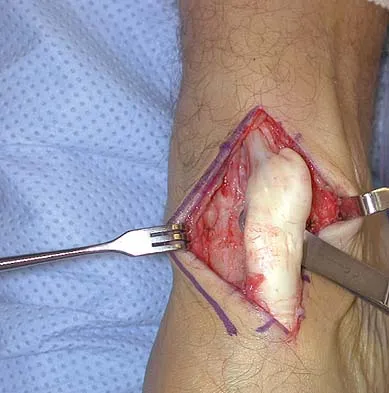
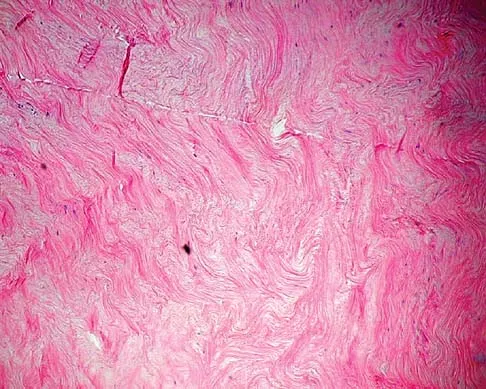
Explanation
The findings are most consistent with a rupture of the anterior tibial tendon. The damaged area of tendon should be resected, followed by tendon reconstruction or tenodesis. The histology is not consistent with giant cell tumor of the tendon sheath, gout, or synovial sarcoma. Fibromatosis is characterized by a large number of spindle cells within the collagen background. Otte S, Klinger HM, Loreaz F, Haerer T: Operative treatment in case of closed rupture of the anterior tibial tendon. Arch Orthop Traum Surg 2002;122:188-190.
Question 33
Figures 32a and 32b show the radiographs of a 13-year-old right hand-dominant boy who sustained a closed Salter-Harris type II fracture of the proximal humerus during a hockey game. The shoulder has significant swelling, but is neurovascularly intact. What treatment offers the best chance of reestablishing normal shoulder motion?
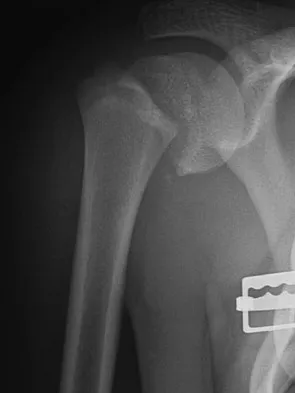
Explanation
The patient has a significantly angulated proximal humerus fracture with a high degree of varus angulation, and rotational malalignment is likely. Failure to correct the varus angulation will result in permanent loss of shoulder abduction because the patient's age limits bony remodeling. These fractures are inherently unstable due to the inability to control the proximal fracture alignment. Shoulder spica casts have a high rate of redisplacement after treatment. Adequate open or closed reduction and pin fixation in the operating room optimizes alignment and all but eliminates the chance of redisplacement. Dobbs MB, Luhmann SJ, Gordon JE, et al: Severely displaced proximal humerus epiphyseal fractures. J Pediatr Orthop 2003;23:208-215. Vaccaro AR (ed): Orthopaedic Knowledge Update 8. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2005, p 701.
Question 34
A healthy 70-year-old man has a swollen knee after undergoing a knee replacement 10 years ago. Aspiration of the knee reveals cloudy, viscous synovial fluid. Laboratory studies show an erythrocyte sedimentation rate of 10 mm/h and a C-reactive protein level of less than 0.5. What is the most likely diagnosis?
Explanation
Polyethylene wear debris can result in significant synovitis and subsequent cloudy appearing synovial fluid. Typically, laboratory studies show a WBC of less than 30,000/mm3 no left shift. Cytologic examination can reveal intra-articular polyethylene particles. Infected total knee arthroplasty is extremely uncommon in a healthy, immune-competent patient who has a normal preoperative erythrocyte sedimentation rate and C-reactive protein level.
Question 35
When considering a flexor digitorum longus tendon transfer as part of the surgical treatment in patients with symptomatic flatfoot deformity caused by posterior tibial tendon insufficiency, which of the following patients is the most appropriate candidate?
Explanation
Transfer of the flexor digitorum longus tendon is a common technique combined with other procedures to treat patients with posterior tibial tendon insufficiency. However, it is contraindicated in patients with a fixed hindfoot deformity, hypermobility, or neuromuscular compromise. It is relatively contraindicated in patients who are obese, and those older than age 60 to 70 years. Pedowitz WJ, Kovatis P: Flatfoot in the adult. J Am Acad Orthop Surg 1995;3:293-302.
Question 36
A 29-year-old woman reports shoulder pain after sustaining a minor fall 6 weeks ago. She has a history of celiac sprue. Radiographs of the forearm and shoulder are shown in Figures 53a and 53b. Which of the following serum abnormalities would be expected?
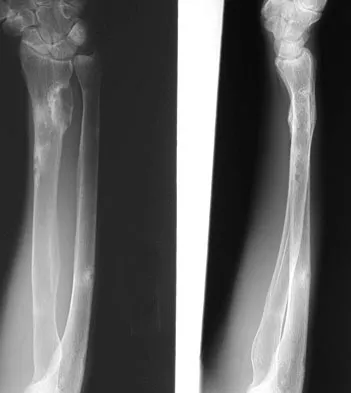
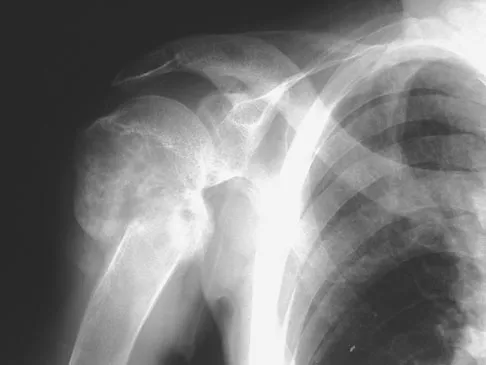
Explanation
Celiac sprue results in rapid gastrointestinal transit and fatty stools that impair the absorption of calcium and vitamin D and result in nutritional-deficiency osteomalacia with secondary hyperparathyroidism. The radiographs show marked osteopenia with brown tumors. A pathologic fracture is seen in the proximal humerus through a large brown tumor. Serum findings include low or normal calcium, low phosphate, elevated alkaline phosphatase, low 1,25(OH)2D, and increased PTH levels. Secondary hyperparathyroidism is associated with a variety of conditions including malabsorption syndromes. Potts JT: Parathyroid hormone: Past and present. J Endocrinol 2005;187:311-325. Corazza GR, Di Stefano M, Maurino E, et al: Bones in coeliac disease: Diagnosis and treatment. Best Pract Res Clin Gastroenterol 2005;19:453-465.
Question 37
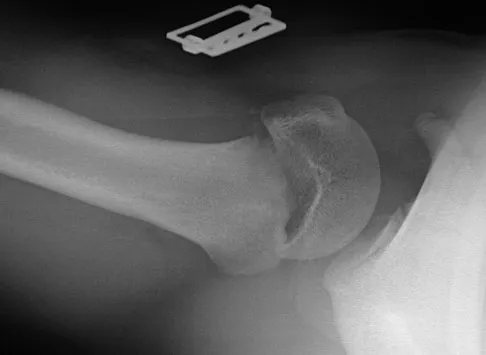
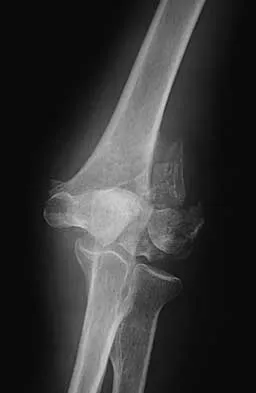
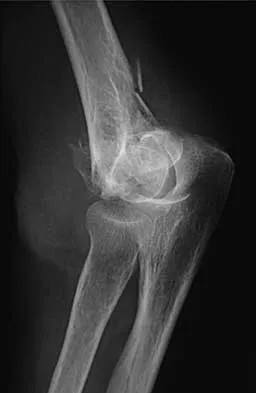
Figures 20a through 20c show the radiographs of a 69-year-old woman who has severe pain in her dominant right arm after falling on the ice. History includes arthritis, hypertension, and heart disease. She is neurovascularly intact. Management should consist of
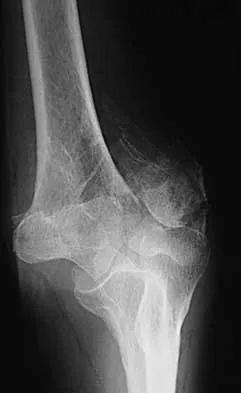
Explanation
The radiographs reveal a severely comminuted distal humerus fracture. A long arm cast, functional bracing, and closed reduction and percutaneous pin fixation all have a poor outcome and could result in a nonunion that will be very difficult to treat. Open reduction and internal fixation is indicated in most supracondylar humerus fractures, but total elbow arthroplasty is a good alternative in elderly patients who have multiple medical problems and when the fracture pattern may preclude stable enough internal fixation to allow postoperative motion. Cobb TK, Morrey BF: Total elbow arthroplasty as primary treatment for distal humeral fractures in elderly patients. J Bone Joint Surg Am 1997;79:826-832.
Question 38
Spontaneous entrapment of the posterior interosseous nerve most commonly occurs in which of the following locations?
Explanation
The extensor carpi radialis brevis, supinator muscle, arcade of Frohse, and leash of Henry are potential sites of compression for the posterior interosseous nerve. The most common location of spontaneous entrapment is the arcade of Frohse. The lateral intermuscular septum is a site of compression for the radial nerve.
Question 39
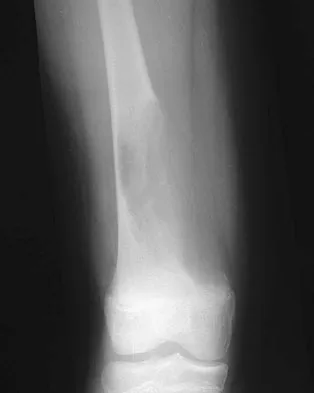
Compared to postoperative radiation therapy, preoperative radiation therapy has a higher rate of what complication?
Explanation
Radiation therapy is commonly used as an adjuvant in the treatment of soft-tissue sarcomas, but a controversy exists whether it should be preoperative or postoperative. Radiation therapy can be given prior to or following resection of the tumor. Postoperative radiation is usually given in a higher dose to a larger treatment field. This commonly results in a higher incidence of fibrosis and lymphedema. There is no statistical difference in local recurrence rate between the two radiation treatment plans. Neuropathy is more commonly a complication of chemotherapy. Preoperative radiation therapy has been shown to have a higher wound complication rate than postoperative radiation. Vaccaro AR (ed): Orthopaedic Knowledge Update 8. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2005, pp 197-215.
Question 40
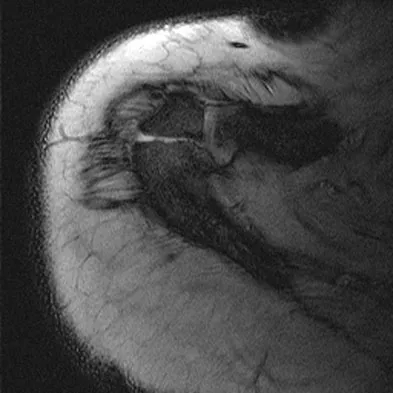
A 23-year-old man reports pain on the superior aspect of his right shoulder with repetitive overhead activities and when lying on his right side. Figure 29 shows an axial MRI scan. What is the most likely diagnosis based on the MRI findings?
Explanation
Os acromiale represents a failure of fusion of the anterior acromial apophysis and has been reported in approximately 8% of the population. Patients with a symptomatic os acromiale often report impingement-type symptoms with pain over the superior acromion, especially with overhead activities or sleeping. When nonsurgical management is unsuccessful, surgical options include excision, open reduction and internal fixation, and arthroscopic decompression. Kurtz CA, Humble BJ, Rodosky MW, et al: Symptomatic os acromiale. J Am Acad Orthop Surg 2006;14:12-19.
Question 41
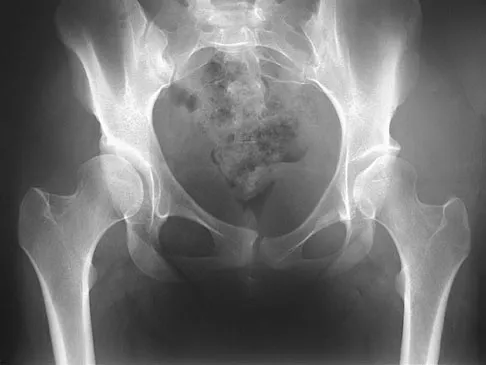
Figure 21 shows the radiograph of a 32-year-old patient with right hip pain that has failed to respond to nonsurgical management. What is the most appropriate surgical treatment at this time?
Explanation
The radiograph reveals developmental dysplasia of both hips. The patient has classic anterolateral undercoverage of the femoral head on the right side as demonstrated by a high acetabular index (measured at 27 degrees). Anterior undercoverage can be determined by drawing the marking for the anterior wall that fails to overlap the femoral head in this patient. Currently in North America, the most accepted surgical management for symptomatic dysplasia of the hip with good joint space is a Bernese (Ganz) periacetabular osteotomy. Surgical dislocation of the hip and femoroacetabular osteoplasty may be considered for patients with symptomatic femoroacetabular impingement of the hip. Ganz R, Klaue K, Vinh TS, et al: A new periacetabular osteotomy for the treatment of hip dysplasias: Technique and preliminary results. Clin Orthop 1988;232:26-36.
Question 42
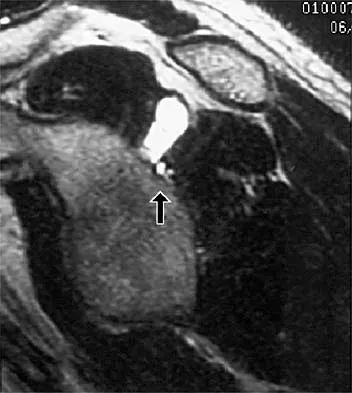
Figure 13 shows the MRI scan of a 29-year-old rock climber who reports increasing shoulder pain and weakness. Based on these findings, atrophy will most likely occur in which of the following muscles?
Explanation
The MRI scan shows a cyst at the spinoglenoid notch. These cysts are often associated with a labral injury, such as a superior labrum anterior and posterior (SLAP) lesion. The suprascapular nerve passes through the suprascapular notch and sends motor branches to the supraspinatus and sensory branches to the capsule. At the spinoglenoid notch, the infraspinatus branch of the suprascapular nerve is compressed by the cyst, leading to isolated infraspinatus atrophy. The teres minor and the deltoid are innervated by the axillary nerve. Fehrman DA, Orwin JF, Jennings RM: Suprascapular nerve entrapment by ganglion cysts: A report of six cases with arthroscopic findings and review of the literature. Arthroscopy 1995;11:727-734. Ianotti JP, Ramsey ML: Arthroscopic decompression of a ganglion cyst causing suprascapular nerve compression. Arthroscopy 1996;12:739-745.
Question 43
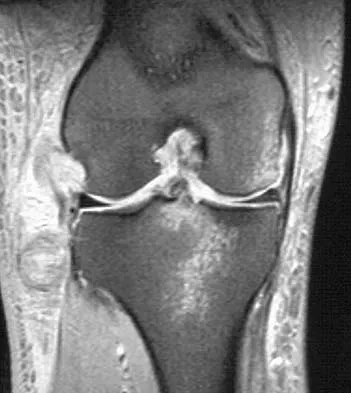
The brachialis muscle is innervated by what two nerves?
Explanation
The brachialis is innervated by two nerves: medially, the musculocutaneous nerve; laterally, the radial nerve. The muscle is split longitudinally to approach the humerus anteriorly. Henry AK: The distal part of the humerus and front of the forearm, in Henry AK (ed): Extensile Exposure, ed 2. Edinburgh, UK, Churchill Livingstone, 1973, pp 90-115.
Question 44
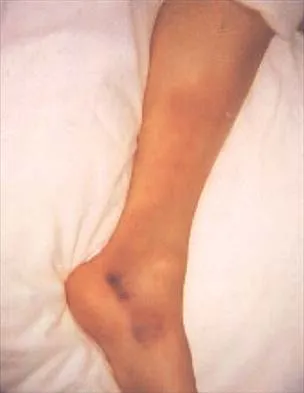
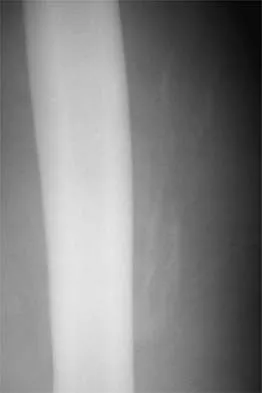
An 18-year-old high school football player sustains a thigh injury that results in the findings shown in Figure 1. Initial management should consist of
Explanation
The radiograph shows myositis ossificans within the quadriceps muscle. This condition occurs as a complication of muscle injury. Initial treatment should include rest, ice, compression, and elevation. While gentle active range of motion is encouraged in the functional recovery from this injury, passive stretching is contraindicated as it can enhance hemorrhage and accentuate the development of myositis ossificans. Ultrasound is similarly contraindicated because it can enhance the development of myositis ossificans and has no proven efficacy in this patient; electrical stimulation also has no proven benefits. Massage is contraindicated in the initial management of this injury because of its influence on increasing local blood flow. Anderson JE (ed): Grant's Atlas of Anatomy. Baltimore, MD, Williams & Wilkins, 1978, pp 4.39-4.49. Brumet ME, Hontas RB: The thigh, in DeLee JC, Drez D Jr (eds): Orthopaedic Sports Medicine. Philadelphia, PA, WB Saunders, 1994, pp 1086-1112. Antao NA: Myositis of the hip in a professional soccer player: A case report. Am J Sports Med 1988;16:82-83.
Question 45
What mechanism contributes to strength gains during conditioning of the preadolescent athlete?
Explanation
Prepubescent athletes gain strength through neurogenic adaptations, including recruitment of motor units, reduced inhibition, and learned motor skills. Myogenic adaptations (muscle hypertrophy) occur after puberty and include increased contractile proteins, thickening of the connective tissue, and increased short-term energy sources such as creatine phosphate. Grana WA: Strength training, in Stanitski CL, DeLee JC, Drez D Jr (eds): Pediatric and Adolescent Sports Medicine. Philadelphia, PA, WB Saunders, 1994, pp 520-526.
Question 46
A 7-year-old boy sustained an acute puncture wound of the foot after stepping barefoot on a piece of glass 1 day ago. His mother states that she is not sure if she got the piece of glass out; however, she reports that his immunizations are up-to-date. Examination reveals that the wound is slightly erythematous, less than 1 mm in length on the heel, and is not currently draining. What is the next most appropriate step im management?
Explanation
The child has an up-to-date tetanus; therefore, a booster is not recommended. Pseudomonas coverage is most likely not needed because the child was barefoot. It is too early to evaluate for abscess or osteomyelitis with MRI, and a formal debridement is rarely indicated without signs of an abscess or a retained foreign body. Radiographs with soft-tissue penetration should be obtained to check for a retained foreign body. Richardson EG (ed): Orthopaedic Knowledge Update: Foot and Ankle 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2004, pp 199-205.
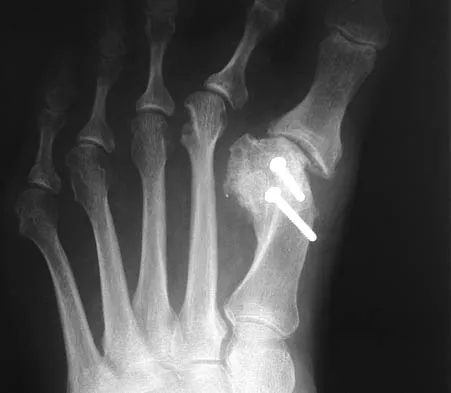
Question 47
A 21-year-old patient has had pain and a marked decrease in active and passive shoulder motion after having had a seizure 2 months ago as the result of alcohol abuse. Current AP and axillary radiographs and a CT scan are shown in Figures 26a through 26c. Management should consist of
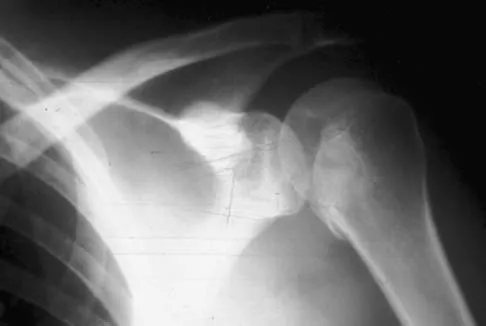
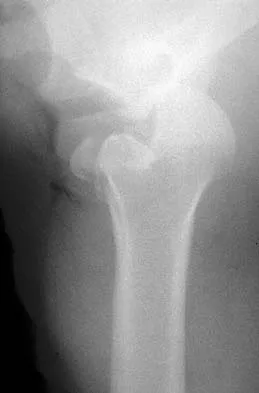
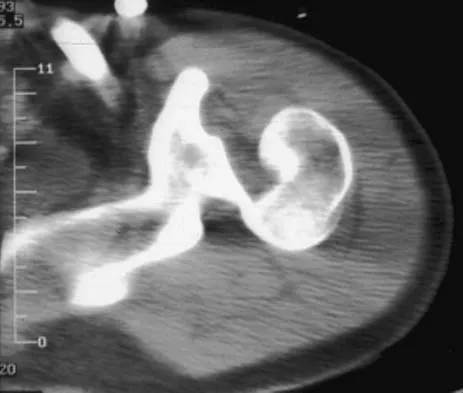
Explanation
Open reduction and subscapularis and lesser tuberosity transfer into the defect is the treatment of choice in young individuals who have defects that involve between 20% to 45% of the head. Disimpaction and bone grafting is an option in injuries that are less than 3 weeks old. Closed reduction 2 to 3 months after injury usually is unsuccessful and increases the risk of fracture or neurovascular injury. Total shoulder arthroplasty is reserved for defects of greater than 50% or with associated glenoid surface damage. Hemiarthroplasty should be avoided in young individuals unless 50% or more of the head is involved. Gerber C: Chronic locked anterior and posterior dislocations, in Warner JJ, Iannotti JP, Gerber C (eds): Complex and Revision Problems in Shoulder Surgery. Philadelphia, PA, Lippincott-Raven, 1997, pp 99-113.
Question 48
The parents of a 3-year-old girl who has had pain and swelling in the right ankle for the past 3 months now report that she has a limp and that the right knee and both ankles are painful and swollen. The limp and difficulty walking are most severe in the morning when the child first gets out of bed and are also more severe after extended walking. The parents deny fever, chills, weight loss, or night pain. Examination shows mild swelling and slightly restricted motion of the right knee and both ankles but is otherwise normal. In addition to initiation of treatment, the child should be referred to which of the following specialists?
Explanation
Pauciarticular juvenile rheumatoid arthritis (JRA) is the most common subgroup of JRA. It typically presents between the ages of 2 to 4 years with a mild swelling of one to four joints. Girls are affected four times more often than boys. The ankle and knee are commonly involved, and limping is typically worse in the morning and after extended activity. The diagnosis of pauciarticular JRA is typically one of exclusion because laboratory studies, including erythrocyte sedimentation rate and rheumatoid factor, are usually within normal limits. Pauciarticular JRA has the highest incidence of chronic uveitis, and in the subgroup with elevated antinuclear antibody (ANA) titers, the incidence is 75%. In JRA, uveitis usually occurs after the onset of synovitis but may precede the joint symptoms. At the early stage of uveitis, the patient is asymptomatic. If the eye condition is not detected and treated, progressive loss of vision may occur. Orthopaedic surgeons may be instrumental in making the diagnosis of pauciarticular JRA. Pauciarticular JRA is not associated with conditions that require input from the other specialists. Carey TP: Inflammatory arthritides: Juvenile rheumatoid arthritis, seronegative spondyloarthropathies, transient synovitis, hemophilic arthropathy, in Fitzgerald RH, Kaufer H, Malkani AL (eds): Orthopaedics. St Louis, MO, Mosby, 2002, pp 1315-1321.
Question 49
Figures 32a and 32b show the radiographs of a 13-year-old boy who sustained a fracture while playing football 1 week ago. Management at the time of injury included application of a cast and the use of crutches. A follow-up office visit reveals a normal neurologic examination, and the patient reports no discomfort with the cast and crutches. Management should now include
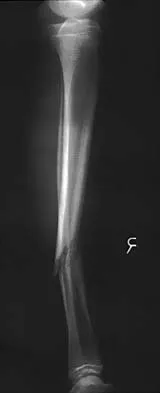
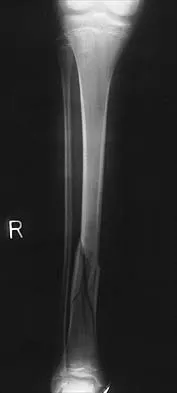
Explanation
Stable fractures and minimally displaced fractures in children can and should be treated by closed methods. Because loss of reduction is common, alignment of tibia fractures must be monitored closely for the first 3 weeks after cast application. This is most easily handled in a cooperative patient by cast wedging. Some children require application of a second cast under general anesthesia 2 to 3 weeks after injury, particularly if the subsidence of swelling has caused the cast to loosen. Surgical indications include the presence of soft-tissue injuries, unstable fracture patterns, fractures associated with compartment syndrome, and the child with multiple injuries. Surgical options in children include percutaneous pins, external fixation, plates and screws, and intramedullary nails. Heinrich SD: Fractures of the shaft of the tibia and fibula, in Rockwood CA, Wilkins KE, Beaty JH (eds): Fractures in Children, ed 4. Philadelphia, Pa, Lippincott-Raven, 1996, pp 1340-1346.
Question 50
When elevating the arm, the ratio of scapulothoracic to glenohumeral motion over the total range of motion is best described as
Explanation
The ratio of scapulothoracic to glenohumeral motion with elevation has been shown to vary depending on what portion of elevation is examined, how much load is on the arm, and the technique used to measure increments of elevation. However, almost every study shows that the ratio of scapulothoracic to glenohumeral motion is 1:2 for the contributions over a full range of elevation to 170 degrees. In the first 30 degrees of elevation, there is significant variability in the ratio, and there may be significant variability up to around 60 degrees. Inman VT, Saunders JR, Abbott LC: Observations of the function of the shoulder joint. Clin Orthop 1996;330:3-12.
Question 51
At the level of the midcalf, the plantaris tendon is found at which of the following locations?
Explanation
The plantaris tendon is often harvested to augment a tendon reconstruction. The origin of the plantaris muscle is on the posterolateral aspect of the distal femur, and the muscle lies lateral to the tibial nerve and the posterior tibial artery. The tendon then courses posteriorly between the soleus and the medial head of the gastrocnemius. Clement CD: Anatomy: A Regional Atlas of Human Anatomy, ed 3. Baltimore, MD, Munich, Germany, Urban and Schwarzberg, 1987, Figure 475.
Question 52
Evaluation of the percent of necrosis in the resected specimen after preoperative chemotherapy is of prognostic value for what type of sarcoma?
Explanation
To date, only the percent of necrosis after induction chemotherapy in high-grade osteosarcomas seems to be of prognostic value. The value in soft-tissue sarcoma and rhabdomyosarcoma is being evaluated but has not been substantiated. Chondrosarcomas and parosteal osteosarcomas are not treated with chemotherapy. Rosen G, Marcove RC, Caparros B, Nirenberg A, Kosloff C, Huvos AG: Primary osteogenic sarcoma: The rationale for pre-operative chemotherapy and delayed surgery. Cancer 1979,43:2163-2177. Davis AM, Bell RS, Goodwin PJ: Prognostic factors in osteosarcoma: A critical review. J Clin Oncol 1994;12:423-431.
Question 53
What is the most common complaint in patients with a developmental radial head dislocation?
Explanation
Developmental dislocation of the radial head most frequently presents as a painless mass over the posterior aspect of the elbow. Patients do not have feelings of elbow subluxation but may report pain or clicking. Limitation of motion is most frequently found in the pronation and supination arc rather than in flexion and extension. Lloyd-Roberts GC, Bucknill TM: Anterior dislocation of the radial head in children-etiology: Natural history and management. J Bone Joint Surg Am 1977;58:402.
Question 54
Which of the following design features of a femoral component used in a total knee arthroplasty best minimizes the patellar component contact stresses?
Explanation
Several studies have shown that design of the femoral component, especially the trochlear groove portion, largely influences patellar tracking and patellofemoral contact stresses. A deep, curved anatomic femoral trochlear groove has been shown to have the lowest contact stresses. Petersilge WJ, Oishi CS, Kaufman KR, Irby SE, Colwell CW Jr: The effect of trochlear design on patellofemoral shear and compressive forces in total knee arthroplasty. Clin Orthop 1994;309:124-130. Theiss SM, Kitziger KJ, Lotke PS, Lotke PA: Component design affecting patellofemoral complications after total knee arthroplasty. Clin Orthop 1996;326:183-187.
Question 55
A 32-year-old woman has left second toe dactylitis (sausage toe). Radiographs show a "pencil in cup" distal interphalangeal joint deformity. Examination reveals that subtalar motion is markedly reduced. What is the most likely diagnosis?
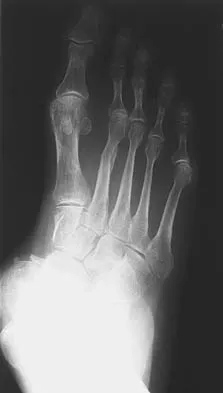
Explanation
The patient's clinical picture is considered the classic presentation for psoriatic arthritis. The other answers are not applicable for the constellation of findings. Jahss MH: Disorders of the Foot and Ankle, ed 2. Philadelphia, PA, WB Saunders, 1991, pp 1691-1693.
Question 56
The arrow in the axial T1-weighted MRI scan shown in Figure 18 is pointing to which of the following structures?
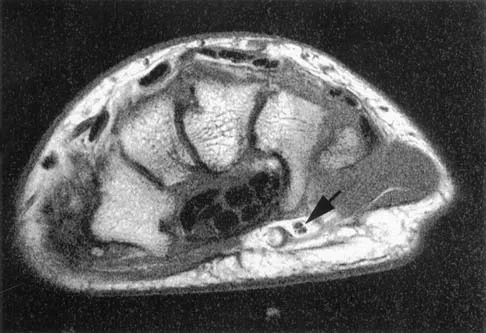
Explanation
The arrow is pointing to the ulnar nerve within Guyon's canal. Guyon's canal is approximately 4 cm long, beginning at the proximal extent of the transverse carpal ligament and ending at the aponeurotic arch of the hypothenar muscles. Many structures comprise the boundaries of Guyon's canal. The floor, for example, consists of the transverse carpal ligament, the pisohamate and pisometacarpal ligaments, and the opponens digiti minimi. Within Guyon's canal, the ulnar nerve bifurcates into the superficial and deep branches, with the deep branch of the ulnar nerve persisting distal to the canal. The ulnar artery is immediately adjacent and radial to the ulnar nerve. The median nerve is visualized within the carpal tunnel. The radial artery is on the radial side of the wrist. The hook of the hamate is clearly seen in the figure, orienting the observer to the ulnar side of the wrist. Goss MS, Gelberman RH: The anatomy of the distal ulnar tunnel. Clin Orthop 1985;196:238-247.
Question 57
A 5-year-old boy has had pain in the right foot for the past month. Examination reveals tenderness and mild swelling in the region of the tarsal navicular. Radiographs are shown in Figure 30. Management should consist of
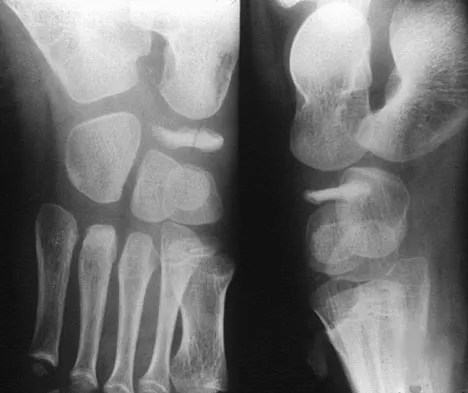
Explanation
The child has the classic findings of Kohler's disease or osteochondrosis of the tarsal navicular. The cause of this condition is not known, but osteonecrosis and mechanical compression have been proposed. Children generally report midfoot pain over the tarsal navicular and limping. Physical findings include tenderness, swelling, and occasionally redness in the region of the tarsal navicular. Radiographs show sclerosis and narrowing of the tarsal navicular. The natural history of the condition is spontaneous resolution and reconstitution of the navicular. Symptomatic treatment with restriction of weight bearing or casting is recommended. Karp M: Kohler's disease of the tarsal scaphoid. J Bone Joint Surg 1937;19:84-96.
Question 58
Figure 3 shows the AP radiograph of a patient with diabetes mellitus who has knee pain. A semiconstrained knee prosthesis was used in this patient to prevent which of the following complications?
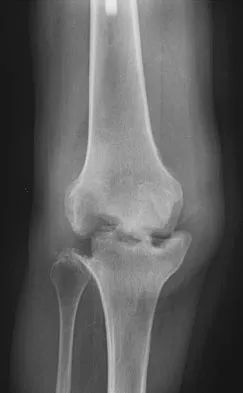
Explanation
The radiographic appearance of the joint is highly suspicious for neuropathic joint (Charcot's joint). Evidence of bone loss on both the tibial and the femoral sides may necessitate the use of metal and/or bone augments. Patients with a neuropathic joint often have excellent range of motion, and postoperative stiffness is not a problem. The main problem with these patients is instability that occurs secondary to ligamentous laxity. Use of a semiconstrained prosthesis prevents the latter complication. Parvizi J, Marrs J, Morrey BF: Total knee arthroplasty for neuropathic (Charcot) joints. Clin Orthop 2003;416:145-150.
Question 59
Which of the following definitions best describes Batson's vertebral vein system?
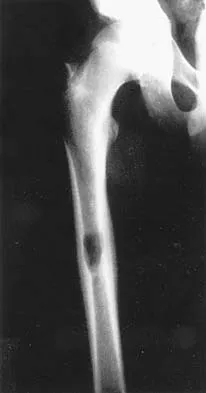
Explanation
The venous plexus was described by Batson and helps to explain the common distribution of metastatic cells to the vertebrae, skull, ribs, and proximal long bones. Batson studied the vertebral vein system extensively by using contrast agents in human cadavers and live monkeys. Batson's plexus is a valveless system that allows retrograde embolism from the major organs such as the breast, prostate, lung, kidney, and thyroid. It is located within the thoracoabdominal cavity and has connections to the proximal long bones and an intercommunicating network of thin-walled veins with a low intraluminal pressure. Batson OV: Function of vertebral veins and their role in spread of metastases. Ann Surg 1940;112:138-149.
Question 60
Figures 3a and 3b show the current radiographs of a 59-year-old woman who has pain and deformity after undergoing bunion surgery 1 year ago. Nonsurgical management has failed to provide relief. Treatment should now consist of
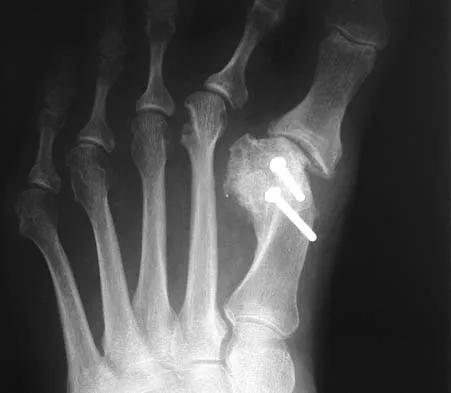
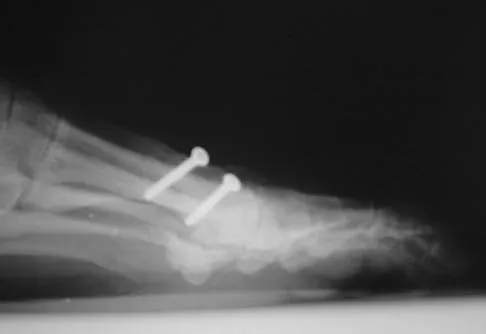
Explanation
The hallux varus seen in this patient is most likely the result of a combination of causes. Based on the degenerative changes and the significant shortening of the first metatarsal relative to the second metatarsal, a metatarsophalangeal arthrodesis is the treatment of choice. The other surgical approaches are not expected to provide a satisfactory result. Coughlin MJ, Mann RA: Adult hallux valgus, in Coughlin MJ, Mann RA (eds): Surgery of the Foot and Ankle, ed 7. St Louis, MO, Mosby-Year Book, 2000, pp 150-269.
Question 61
A 7-year-old girl has pain and swelling of the right elbow after falling off her bicycle. Radiographs are shown in Figure 31. What is the most appropriate initial step in management?
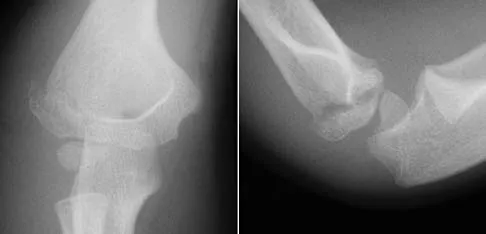
Explanation
Lateral condylar fractures are challenging to treat because of late displacement and development of a nonunion that may lead to valgus instability, pain, or tardy ulnar nerve palsy. Fractures such as this one with more than 2 mm of displacement on any radiographic view are prone to nonunion and should be stabilized. Fractures with less than 2 mm of displacement usually are stable and may be treated nonsurgically. In these patients, careful follow-up is recommended within several days of casting to check for fracture displacement. Arthrography or MRI may be helpful in these minimally displaced fractures. Fractures with an intact articular cartilage surface, such as noted on these studies, are unlikely to displace further. Finnbogason T, Karlsson G, Lindberg L, et al: Nondisplaced and minimally displaced fractures of the lateral humeral condyle in children: A prospective radiographic investigation of fracture stability. J Pediatr Orthop 1995;15:422-425. Attarian DE: Lateral condyle fractures: Missed diagnoses in pediatric elbow injuries. Mil Med 1990;155:433-434. Flynn JC: Nonunion of slightly displaced fractures of the lateral humeral condyle in children: An update. J Pediatr Orthop 1989;9:691-696.
Question 62
A 17-year-old man sustained a 5-mm laceration on the lateral aspect of the hindfoot while working on a farm. Examination in the emergency department revealed no fractures. Twenty-four hours later, he returns to the emergency department with increasing foot pain. Thin brown drainage is seen emanating from the wound. He has a temperature of 102.0 degrees F (38.9 degrees C), a pulse rate of 120, and a blood pressure of 80/40 mm Hg. Examination of the foot reveals diffuse swelling, ecchymosis, tenderness, and crepitus with palpation. Current radiographs are shown in Figures 40a and 40b. Management should now consist of
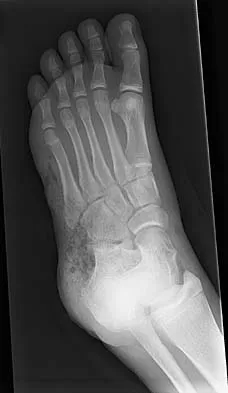
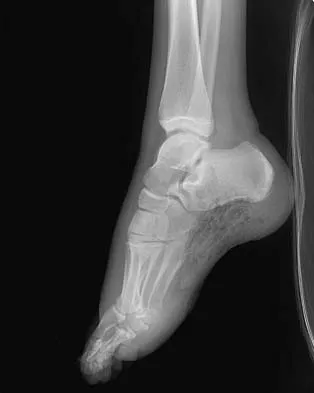
Explanation
The mechanism and environment in which the injury occurred, the clinical picture, and the radiographic findings of gas in the tissues suggest an anaerobic Gram-positive bacterial infection. This can be a life- and limb-threatening infection. Treatment should consist of wide debridement of all devitalized tissue, and intravenous antibiotics should be started. Wounds should be left open to allow bacterial effluent and increase oxygen tension in the wound. Hyperbaric oxygen may be used as an adjuvant but is no substitute for debridement. Pellegrini VD, Reid JS, Evarts CM: Complications, in Rockwood CA, Green DP, Bucholz RW, et al (eds): Rockwood and Green's Fractures in Adults, ed 4. Philadelphia, PA, Lippincott-Raven, 1996, vol 1, pp 458-463.
Question 63
A 12-year-old child with spina bifida paraplegia requires brace management for ankle stability. Which of the following principles applies to brace management in this individual?
Explanation
Bracing for spina bifida paraplegia provides both support and improved function of the movable limb. An orthosis has value in controlling unstable joints. The three-point pressure effect applies a force above and below the joint to prevent it from buckling. A four-point pressure effect is only required for a two-joint system (this patient has problems only at the ankle). A longer lever arm brace and a brace with a greater area of support provide better stability. Finally, a straighter limb, without contracture, applies less pressure to the brace and lessens overload to the skin. Gage JR: An overview of normal walking. Instr Course Lect 1990;39:291-303. Bleck EE: Current concepts review: Management of the lower extremities in children who have cerebral palsy. J Bone Joint Surg Am 1990;72:140-144.
Question 64
Which of the following statements best describes the anatomic considerations of the popliteal artery posterior to the knee joint?
Explanation
Popliteal artery injury during total knee arthroplasty is relatively rare. Knee flexion, the position that occurs during most of the arthroplasty procedure, allows the popliteal vessels to fall posteriorly, further away from harm. Anatomically, the popliteal artery lies anterior to the popliteal vein and 9 mm posterior to the posterior aspect of the tibial plateau in 90 degrees of flexion. Barrack RL, Booth RE Jr, Lonner JH, et al (eds): Orthopaedic Knowledge Update: Hip and Knee Reconstruction 3. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2006, p 151.
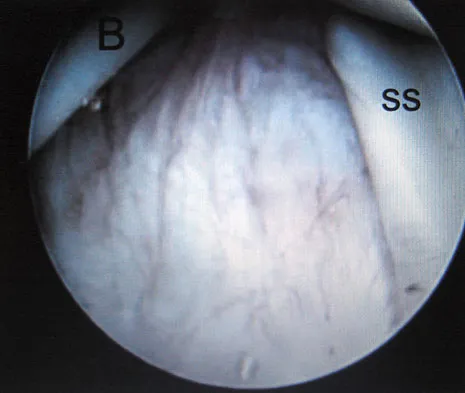
Question 65
What is the function of the rotator cuff during throwing?
Explanation
The coupled action of the rotator cuff prevents superior migration and controls anterior and posterior translation by depressing the humeral head. Poppen NK, Walker PS: Normal and abnormal motion of the shoulder. J Bone Joint Surg Am 1976;58:195-201.
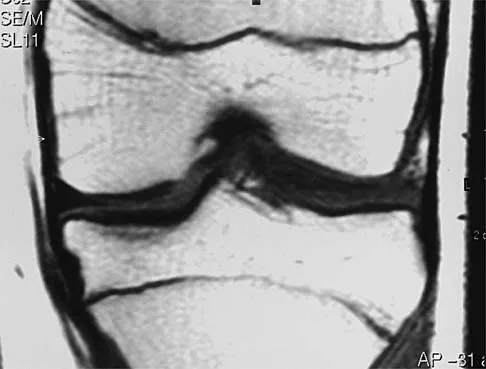
Question 66
A 12-year-old girl has had increasing left knee pain for the past 3 months. A radiograph is shown in Figure 75a, and low- and high-power photomicrographs are shown in Figures 75b and 75c. What is the most appropriate treatment?
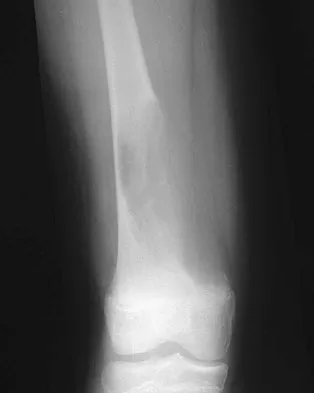
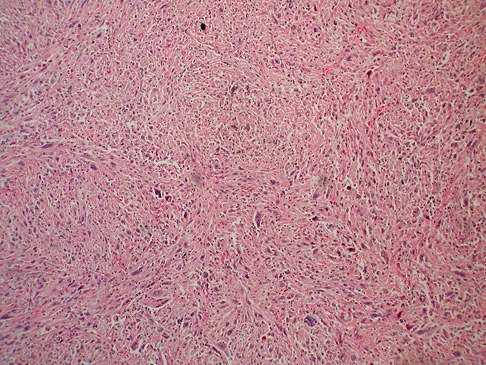
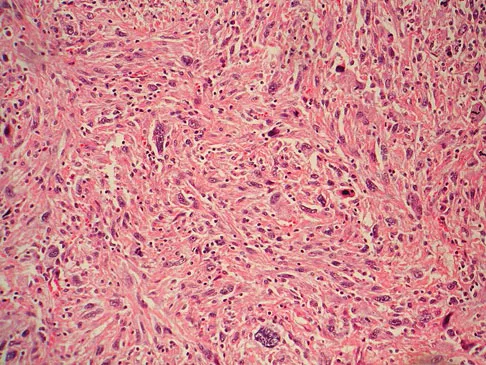
Explanation
The radiograph reveals an aggressive purely lytic lesion of the distal femoral metaphysis. There is no apparent matrix mineralization or periosteal reaction. The photomicrographs show a malignant spindle cell neoplasm in a storiform pattern. Based on these findings, the diagnosis is malignant fibrous histiocytoma of bone. At most institutions, patients with this tumor are treated similar to patients with osteosarcoma with multi-agent chemotherapy and surgery with wide margins (resection or amputation). Menendez LR (ed): Orthopaedic Knowledge Update: Musculoskeletal Tumors. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 203-209.
Question 67
What is the most common benign bone tumor in childhood?
Explanation
The most common benign bone tumor in childhood is a nonossifying fibroma. It is estimated that 30% of children have a nonossifying fibroma. In most patients, the lesion is not identified until a radiograph is obtained for unrelated reasons. Similarly, most identified cases of fibrous cortical defect are not biopsied because the radiographic and clinical presentations are diagnostic. Aboulafia AJ, Kennon RE, Jelinek JS: Benign bone tumors of childhood. J Am Acad Orthop Surg 1999;7:377-388.
Question 68
Figure 16 shows the clinical photograph of a 3-month-old infant with a foot deformity that has been nonprogressive since birth. Examination reveals that the deformity corrects actively and with passive manipulation. There is no associated equinus. Management should consist of
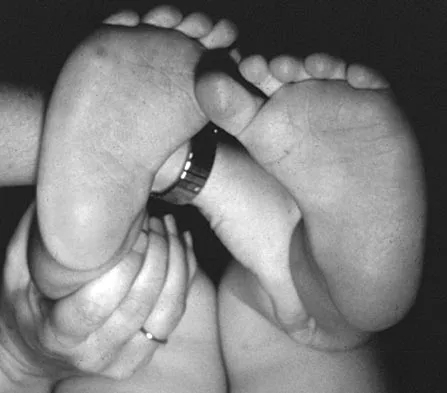
Explanation
The patient has bilateral metatarsus adductus deformities. In a long-term follow-up study by Farsetti and associates, deformities that were passively correctable spontaneously resolved and no treatment was required. More rigid deformities were successfully treated with serial manipulation, with good results in 90%. There were no poor results. Therefore, observation is the management of choice for passively correctable deformities. In feet that are more rigid, serial manipulation and casting is the management of choice.
Question 69
Figure 23 shows the postoperative radiograph of a patient who underwent an anterior cruciate ligament (ACL) reconstruction (with bone-patella tendon-bone autograft) that failed. He initially had loss of flexion postoperatively. What is the most likely cause of this failure?
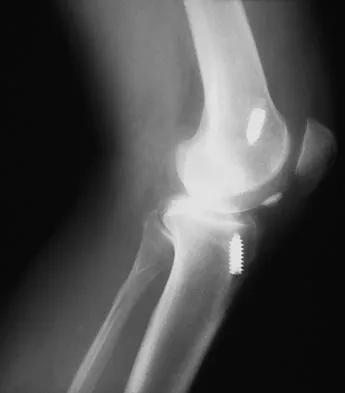
Explanation
The key to this question is the fact that the patient initially lost flexion postoperatively and this relates to anterior placement of the femoral tunnel, thus capturing the knee. The bone plug seen on the radiograph is actually from the tibial tunnel, but this occurred as the patient forced flexion until failure of the ACL graft and pullout of the plug from the tunnel. Although it could be argued that better tibial fixation would have prevented this failure, poor placement of the femoral tunnel led to the failure of this ACL reconstruction. Fu FH, Bennett CH, Latterman C, et al: Current trends in anterior cruciate ligament reconstruction: Part 1. Biology and biomechanics of reconstruction. Am J Sports Med 1999;27:821-830.
Question 70
In addition to the radiographic features seen in Figures 49a and 49b, this patient will most likely have which of the following findings?
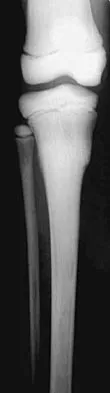
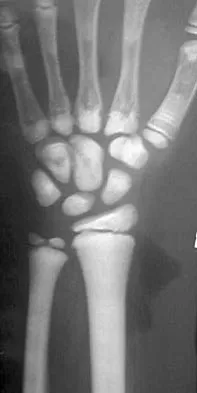
Explanation
The radiographs show the characteristic features of osteopetrosis. The condition results from defective resorption of immature bone by osteoclasts. There are three distinct clinical forms: (1) infantile-malignant, which is autosomal recessive and fatal in the first few years of life if untreated; (2) intermediate autosomal recessive; and (3) autosomal dominant. These conditions do not follow a malignant course, and patients have normal life expectancy with orthopaedic problems and anemia. In the malignant form, the clinical features include frequent fractures, macrocephaly, progressive deafness and blindness, hepatosplenomegaly, and severe anemia beginning in early infancy or in utero. Deafness and blindness are generally thought to represent effects of pressure on nerves and usually occur later in life. The anemia is caused by encroachment of bone on marrow, resulting in obliteration, and the hepatosplenomegaly is caused by compensatory extramedullary hematopoiesis. Dental caries and abscesses, as well as osteomyelitis of the mandible, are also seen. Most patients have normal intelligence. Treatment of the malignant form includes high dose 1,25 dihydroxy vitamin D with a low-calcium diet to stimulate bone resorption, not because there are vitamin deficiencies. Bone marrow transplant has also been successful. Herring JA: Tachdjian's Pediatric Orthopedics, ed 4. Philadelphia, PA, WB Saunders, 2002, p 1550. Zaleske DJ: Metabolic and endocrine abnormalities, in Morrissy RT, Weinstein SL (eds): Lovell and Winter's Pediatric Orthopaedics, ed 5. Philadelphia, PA, Lippincott Williams and Wilkins, 2001, pp 212-214.
Question 71
A 30-year-old elite marathon runner reports chronic pain over the lateral aspect of the distal right leg and dysesthesia over the dorsum of the foot with active plantar flexion and inversion of the foot. Examination reveals a tender soft-tissue fullness approximately 10 cm proximal to the lateral malleolus. The pain is exacerbated by passive plantar flexion and inversion of the ankle. There is also a positive Tinel's sign over the site of maximal tenderness. There is no motor weakness, and deep tendon reflexes are normal. Radiographs and MRI of the leg are normal. What is the next most appropriate step in management?
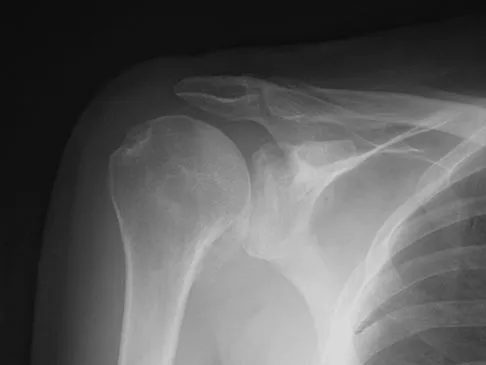
Explanation
The patient has entrapment of the superficial peroneal nerve against its fascial opening in the distal leg. It is typically exacerbated by passive or active plantar flexion and inversion of the foot, which leads to traction of the nerve as it exits this opening. Treatment involves release of the fascial opening to reduce this traction phenomenon. Closure of the defect will only aggravate the condition and potentially result in an exertional compartment syndrome. A four-compartment fasciotomy is only indicated for an established compartment syndrome of the leg. Styf J: Diagnosis of exercise-induced pain in the anterior aspect of the lower leg. Am J Sports Med 1988;16:165-169. Sridhara CR, Izzo KL: Terminal sensory branches of the superficial peroneal nerve: An entrapment syndrome. Arch Phys Med Rehabil 1985;66:789-791.
Question 72
Figure 39 shows the AP radiograph of a 62-year-old man with degenerative osteoarthritis secondary to trauma. History reveals that he underwent total elbow arthroplasty 3 years ago. He continues to report instability and constant pain. A complete work-up, including aspiration and cultures, is negative. Treatment should consist of removal of the components and
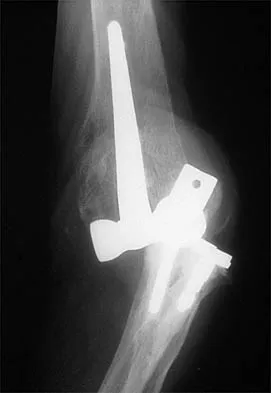
Explanation
An unconstrained prosthesis dislocation is a disconcerting problem that is not easily resolved; however, revision to a semiconstrained prosthesis would best achieve both pain relief and stability. Removal of the components and distraction arthroplasty or conversion to a resection arthroplasty are options, but the results would be unpredictable with regards to pain relief, postoperative motion, or elbow stability. Arthrodesis is poorly tolerated. With revision to another unconstrained prosthesis, there is the risk of continued redislocation because of chronic ligamentous insufficiency. Linscheid RL: Resurfacing elbow replacement arthroplasty: Rationale, technique and results, in Morrey BF (ed): The Elbow and Its Disorders, ed 3. Philadelphia, PA, WB Saunders, 2000, pp 602-610.
Question 73
Which of the following is considered the treatment of choice for a 3-cm chondroblastoma of the distal femoral epiphysis with no intra-articular extension?
Explanation
Curettage and bone grafting typically are the preferred treatment of chondroblastoma, yielding acceptable local recurrence rates of less than 10%. Some surgeons advocate adjuvant therapies such as phenol, liquid nitrogen, or argon beam coagulation. Untreated, these lesions can destroy bone and invade the joint to a significant degree. Large intra-articular lesions may require major joint reconstruction. Wide local excision is rarely required to control the tumor. Radiation therapy is indicated only in unresectable lesions. Springfield DS, Capanna R, Gherlinzoni F, et al: Chondroblastoma: A review of seventy cases. J Bone Joint Surg Am 1985;67:748.
Question 74
Which of the following substances makes up the majority by weight of the extracellular matrix for articular cartilage?
Explanation
The extracellular matrix consists of water, proteoglycans, and collagen. Water makes up the majority (approximately 65% to 80%) of wet weight; 95% of the collage is type II with much smaller amounts of other collagens, including types IV, VI, IX, X, and XI. The exact functions of these other collagens are unknown, but they are believed to be important in matrix attachment and stabilization of the diameter of collagen fibrils. Buckwalter JA, Einhorn TA, Simon SR (eds): Orthopaedic Basic Science: Biology and Biomechanics of the Musculoskeletal System, ed 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2000, pp 444-445.
Question 75
What is the most likely consequence of a vertebral compression fracture associated with osteoporosis?
Explanation
After an osteoporotic vertebral compression fracture, the risk of subsequent fractures at adjacent levels increases. This is felt to be the result of a shifting of the sagittal alignment more anteriorly, putting more stress on the osteopenic vertebral bodies and their anterior cortices. Pain generally resolves with rest, but this may take weeks or months. It has been demonstrated experimentally that osteoporotic vertebral bodies are actually less stiff and weaker after a compression fracture; therefore, deformity predisposes to further deformity. The extensor musculature often fatigues over time and usually does not hypertrophy. Frontal plane deformity is a rare development. Heaney RP: The natural history of vertebral osteoporosis: Is low bone mass an epiphenomenon? Bone 1992;13:S23-S26.
Question 76
A 42-year-old patient has had a fever and low back pain for several days. Laboratory studies show an elevated erythrocyte sedimentation rate and a WBC count of 9,500 mm3 with 75% neutrophils. A CT scan is shown in Figure 15. Examination will most likely reveal what other findings?
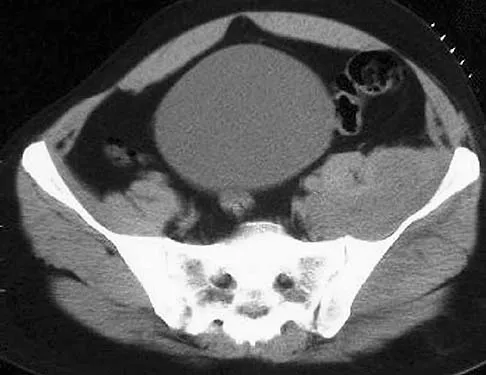
Explanation
The CT scan reveals a left-sided psoas abscess. Irritation of the saphenous division of the femoral nerve can cause paresthesias along the medial aspect of the knee. Pain is usually improved with hip flexion. Cellier C, Gendre JP, Cosnes J, et al: Psoas abscess complication Crohn's disease. Gastroenterol Clin Biol 1992;16:235-238.
Question 77
What radiographic measurement is best used to assess the adequacy of deformity correction for the patient shown in Figure 22?
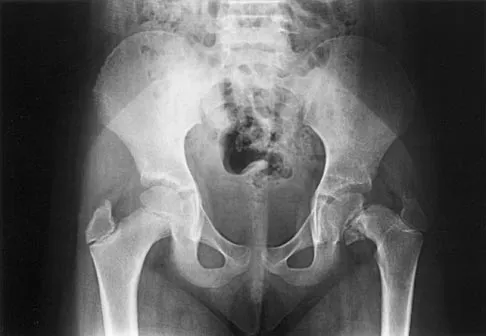
Explanation
Developmental coxa vara develops in early childhood and results in a progressive decrease in the proximal femoral neck-shaft angle with growth. The characteristic radiographic features are seen in this patient and include a decreased neck-shaft angle, a more vertical position of the physeal plate, and a triangular metaphyseal fragment in the inferior femoral neck, surrounded by an inverted radiolucent Y pattern. The main goal of surgery is to correct the varus angulation into a more normal range. Valgus overcorrection is preferred. A recent study emphasized the importance of adequately correcting the Hilgenreiner physeal angle to less than 38 degrees to minimize the risk of recurrent angulation. No study has documented the use of any of the other listed radiographic measurements to the outcome of treating developmental coxa vara. Carroll K, Coleman S, Stevens PM: Coxa vara: Surgical outcomes of valgus osteotomies. J Pediatr Orthop 1997;17:220-224.
Question 78
When harvesting iliac crest bone graft during a posterior spinal decompression and fusion, injury to which of the following nerves may result in painful neuromas or numbness over the skin of the buttocks?
Explanation
The superior cluneal nerves (L1, L2, and L3) are at greatest risk when harvesting iliac crest bone graft during a posterior decompression and fusion. The nerves pierce the lumbodorsal fascia and cross the posterior iliac crest beginning at 8 cm lateral to the posterior superior iliac spine. The ilioinguinal and iliohypogastric nerves innervate anterior structures, and the lateral femoral cutaneous nerve lies in proximity to the anterior superior iliac spine and is at risk with anterior iliac crest bone graft harvesting. The superior gluteal nerve courses through the sciatic notch and supplies motor branches to the gluteus medius, minimus, and tensor fascia lata muscles. An HS: Principles and Techniques of Spine Surgery. Baltimore, MD, Williams and Wilkins, 1998, pp 770-773.
Question 79
What is the most common mechanism of injury that produces turf toe?
Explanation
The most common mechanism of injury for turf toe is a hyperextension injury to the MTP joint. The foot is typically in a dorsiflexed position with the heel raised when an external force drives the MTP joint into further dorsiflexion. The joint capsule usually tears at the metatarsal neck because its attachment is weaker there than at the proximal phalanx. Some compression injuries to the dorsal articular surface of the metatarsal head can result from extension or hyperextension. Clanton TO, Ford JJ: Turf toe injury. Clin Sports Med 1994;13:731-741.
Question 80
Which of the following bearing surface combinations has shown the lowest in vivo wear rates in total hip arthroplasty?
Explanation
Ceramic bearings, made of alumina, have the lowest in vivo wear rates of any bearing combination, 0.5 to 2.5 Mm per component per year. Laboratory wear rates for metal-on-metal are lower than those for metal-on-polyethylene bearings, ranging from 2.5 to 5.0 Mm per year. Titanium used for bearing surfaces has a high failure rate because of a poor resistance to wear and notch sensitivity. Wear rates for ceramic-on-polyethylene bearings have varied, ranging from 0 to 150 Mm. Beaty JH (ed): Orthopaedic Knowledge Update 6. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1999, pp 47-53.
Question 81
What is the known manner in which the growth hormone-insulin-like growth factor-I (GH-IGF-I) system functions to stimulate bone growth?
Explanation
IGF-I, formerly known as somatomedin-C, possibly acts by both paracrine and endocrine hormone pathways. The products of the GH-IGF-I system induce proliferation without maturation of the growth plate and thus induce linear skeletal growth. The action of the thyroid hormone axis is via an active metabolite that enters target cells and signals a nuclear receptor to stimulate both proliferation and maturation of the growth plate. Increased amounts of the active steroid hormone metabolite promote proliferation and maturation of the growth plate. Calcitonin inhibits bone resorption. Binder G, Grauer ML, Wehner AV, et al: Outcome in tall stature: Final height and psychological aspects in 220 patients with and without treatment. Eur J Pediatr 1997;156:905-910. Wang J, Zhou J, Cheng CM, et al: Evidence supporting dual, IGF-I-independent and IGF-I-dependent, roles for GH in promoting longitudinal bone growth. Endocrinol 2004;180:247-255.
Question 82
Figure 20 shows the radiograph of a 21-year-old college basketball player who jammed his left index finger on the rim. He reports pain and tenderness over the dorsum of the distal interphalangeal (DIP) joint. Examination reveals that he is unable to actively extend the DIP joint; however, the skin is intact. Management should consist of
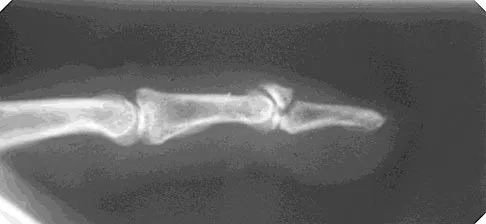
Explanation
Mallet fingers without DIP joint subluxation can be treated with extension splinting. Surgical fixation may be necessary in bony mallet injuries when the joint is subluxated. Size of the bony fragment, while often correlating with stability, is not always an indication for fixation. Buddy taping allows motion; therefore, the fragment will not heal in the appropriate position. Intermittent splinting with range-of-motion exercises also will not allow the fragment to heal in the appropriate position. Crawford GP: The molded polyethylene splint for mallet finger deformities. J Hand Surg Am 1984;9:231-237.
Question 83
A 65-year-old man has a painful mass of the middle finger. A clinical photograph, lateral radiograph, coronal MRI scan, and biopsy specimen are seen in Figures 20a through 20d. What is the most likely diagnosis?
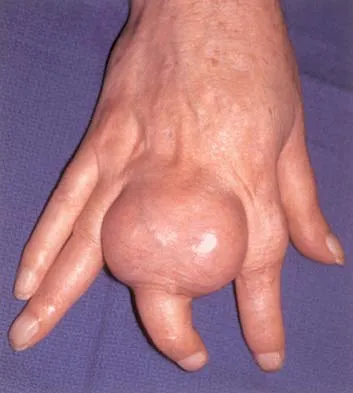
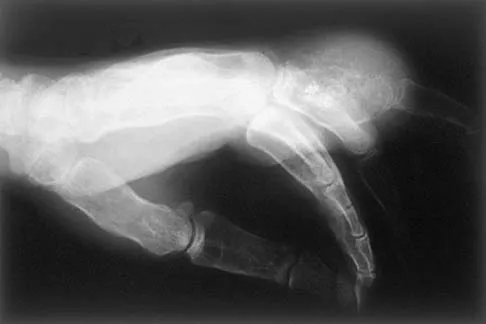
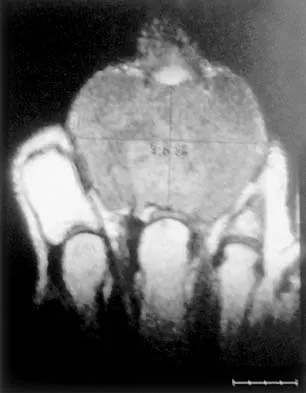
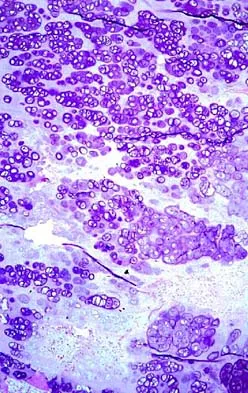
Explanation
Although the degeneration of an isolated benign cartilaginous lesion into a chondrosarcoma is rare, it occurs in roughly 10% of patients with Ollier's disease. Pain is the most common symptom of chondrosarcoma. The treatment of low-grade chondrosarcoma ranges from intralesional excision to wide amputation. The intent of the surgery is to remove all the disease to decrease the chance of local recurrence. Lee FY, Mankin HJ, Fondren G, et al: Chondrosarcoma of bone: An assessment of outcome. J Bone Joint Surg Am 1999;81:326-338.
Question 84
An active 55-year-old man who felt a sudden pop in the left heel while playing tennis 6 months ago was diagnosed with an ankle sprain around the time of injury. He now reports calf atrophy and severe weakness with running. Examination reveals a palpable defect in the Achilles tendon and only trace passive ankle flexion when the calf is squeezed. At the time of surgery, an Achilles tendon defect of 6 cm cannot be approximated. Surgical management of the Achilles tendon should include
Explanation
Chronic or neglected Achilles tendon ruptures can present a surgical problem. Ideally, end-to-end apposition of tendon should be attempted, but this should be accomplished without placing the foot in marked equinus. A defect of greater than 5 cm requires the use of a tendon transfer either alone or in combination with a V-Y advancement of the gastrocnemius. Because of its proximity to the Achilles tendon and its strength as a plantar flexor, the flexor hallucis longus is an ideal choice for this task. Studies have shown that early active range-of-motion exercises after an Achilles tendon repair is beneficial for tendon healing and improved clinical outcomes. Myerson M: Achilles tendon ruptures. Instr Course Lect 1999;48:219-230.
Question 85
Which of the following structures is the most important restraint to posterior subluxation of the glenohumeral joint when positioned in 90 degrees of flexion and internal rotation?
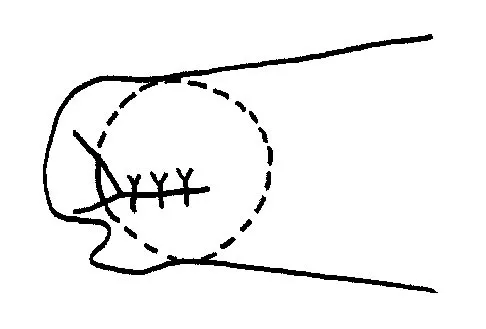
Explanation
The posterior band of the inferior glenohumeral ligament is the most important restraint to posterior subluxation of the glenohumeral ligament with the shoulder in 90 degrees of flexion and internal rotation. With the shoulder in external rotation, the subscapularis is an important stabilizer to posterior subluxation. When the shoulder is in neutral rotation, the coracohumeral ligament is the primary stabilizer. The middle glenohumeral ligament functions primarily to resist anterior translation of the shoulder in the midrange of abduction. The supraspinatus muscle and tendon have relatively little contribution to anterior and posterior translation of the glenohumeral joint. Blasier RB, Soslowsky LJ, Malicky DM, Palmer ML: Posterior glenohumeral subluxation: Active and passive stabilization in a biomechanical model. J Bone Joint Surg Am 1997;79:433-440.
Question 86
What percent of patients initially diagnosed with classic, high-grade osteosarcoma of the extremity have visible evidence of pulmonary metastasis on CT of the chest?
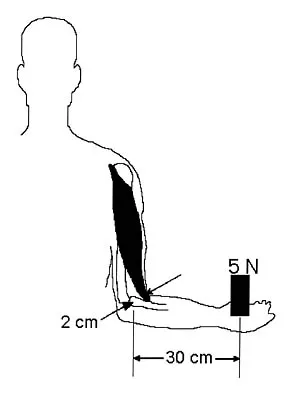
Explanation
CT studies show that approximately 10% to 20% of patients with high-grade osteosarcoma have pulmonary metastases at diagnosis. Although not visible on current staging studies, it is believed that up to 80% of patients have micrometastatic disease that requires systemic chemotherapy. Because it is not possible to identify those patients who do not have disseminated micrometastatic disease, most patients are treated presumptively with chemotherapy. Kaste SC, Pratt CB, Cain AM, et al: Metastases detected at the time of diagnosis of primary pediatric extremity osteosarcoma at diagnosis: Imaging features. Cancer 1999;86:1602-1608.
Question 87
A 5-year-old boy has had right hip pain and a limp for the past 3 months. Examination of the right hip reveals irritability and restricted abduction and internal rotation. AP and lateral radiographs of the hips are shown in Figures 31a and 31b. Initial management should consist of
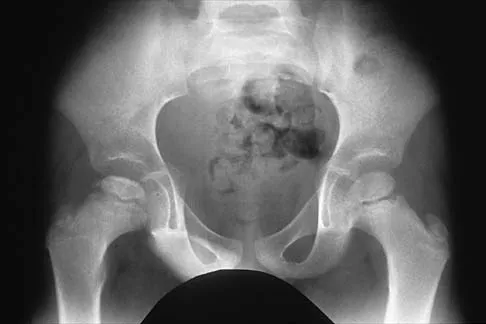
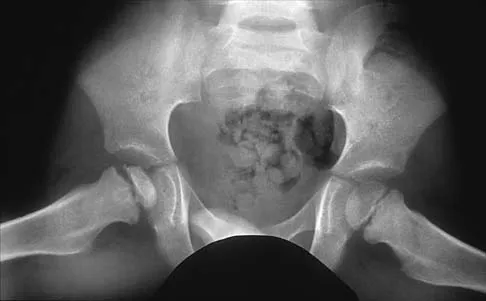
Explanation
A favorable prognosis can be expected in up to 70% of children with Legg-Calve-Perthes disease who are younger than age 6 years. Containment treatment has not been shown to alter the outcome in this age group. The goals of treatment in this patient are to reduce pain (synovitis), restore motion, and improve function. Symptomatic treatment modalities include bed rest, traction, crutches, activity modification, and nonsteroidal anti-inflammatory drugs. Herring JA: The treatment of Legg-Calve-Perthes disease: A critical review of the literature. J Bone Joint Surg Am 1994;76:448-458.
Question 88
A 24-year-old man who was involved in a high speed motor vehicle accident is transferred for definitive care after having been diagnosed with an acute spinal cord injury from a fracture-dislocation at C6-7. He has a complete C6 neurologic level and it is now approximately 10 hours from his injury. What is the most appropriate pharmacologic treatment at this time?
Explanation
The standard practice in the pharmacologic treatment of a spinal cord injury in the United States has been the administration of methylprednisolone with an initial bolus of 30 mg/kg followed by 5.4 mg/kg for 24 hours, in accordance with the findings of the second and third National Acute Spinal Cord Injury Studies (NASCIS). Although the studies have subsequently drawn criticism for their methodology and outcomes, it has been generally accepted that beneficial neurologic outcomes were anticipated in patients who were able to start the protocol within 8 hours of their initial injury. Further improvement was noted in patients receiving the methylprednisolone within 3 hours of their injury and continuing an infusion for 48 hours. In this patient, who is outside the 8-hour treatment window, no studies have supported starting the methylprednisolone protocol at this time. Braken MB, Shepard MJ, Holford TR, et al: Administration of methylprednisolone for 24 or 48 hours or tirilazad mesylate for 48 hours in the treatment of acute spinal cord injury: Results of the third National Acute Spinal Cord Injury Randomized Controlled Trial. National Acute Spinal Cord Injury Study. JAMA 1997;277:1597-1604.
Question 89
In the management of an open tibia fracture, what factor is considered most important in preventing deep infection?
Explanation
The most important aspect of management of any open fracture, and in particular the tibia, is the degree and the completeness of the debridement of the soft tissue and most importantly, the muscle. The ultimate function is determined by the amount of muscle left, as well as the ability to heal. The amount of necrotic muscle left in the wound also determines the predisposition to infection. The method of fixation, the size of the wound, and the amount of contamination are controlled by the surgeon or the injury and have little to do with the long-term outcome. Initial wound cultures have little predictive value. Clifford P: Open fractures, in Ruedi TP, Murphy WM (eds): AO Principles of Fracture Management. Stuttgart, Thieme, 2000, pp 617-638.
Question 90
A 62-year-old man with a long history of right shoulder pain and weakness is scheduled to undergo hemiarthroplasty. Based on the radiographs shown in Figures 6a through 6c, what preoperative factor will most affect postoperative functional outcome?
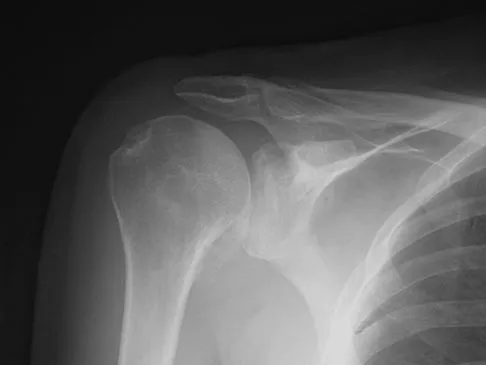
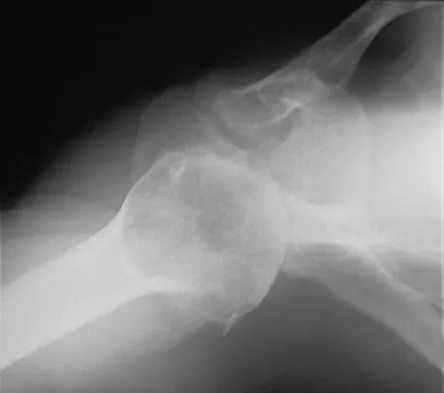
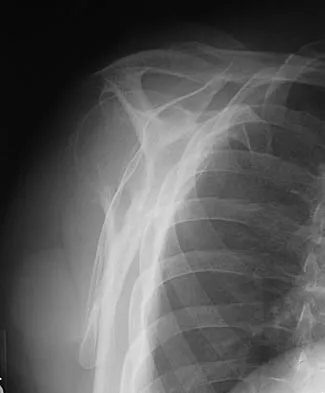
Explanation
The radiographs reveal osteoarthritis and proximal humeral head migration. Integrity of the rotator cuff must be questioned based on these radiographic changes. The status of the rotator cuff is the most influential factor affecting postoperative function in shoulder hemiarthroplasty. The coracoacromial ligament provides a barrier to humeral head proximal migration in the face of a rotator cuff tear. The radiographs do not indicate significant humeral head or glenoid erosion. Acromioclavicular arthritis is often asymptomatic. Iannotti JP, Norris TR: Influence of preoperative factors on outcome of shoulder arthroplasty for glenohumeral osteoarthritis. J Bone Joint Surg Am 2003;85:251-258.
Question 91
The vascularity of the digital flexor tendons is significantly richer in what cross-sectional region?
Explanation
The vascularity of the dorsal portion of the digital flexor tendons is considerably richer than the volar portion. The other regions are not preferentially more vascular. Hunter JM, Scheider LH, Makin EJ (eds): Tendon Surgery in the Hand. St Louis, MO, Mosby, 1987, pp 91-99.
Question 92
Injury to which of the following structures has been reported following iliac crest bone graft harvest?
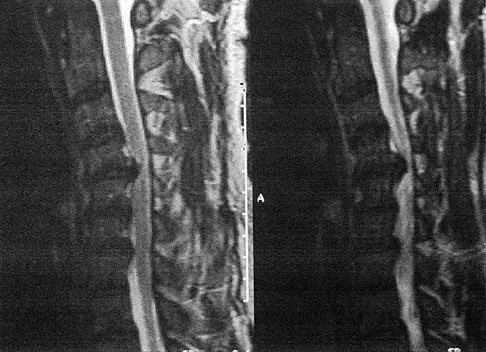
Explanation
Injury to the lateral femoral cutaneous nerve and the ilioinguinal nerve have both been described with an anterior iliac crest bone graft harvest. The lateral femoral cutaneous nerve may be injured from retraction after elevating the iliacus muscle or from direct injury when the nerve actually courses over the crest. A posterior crest harvest can injure the superior gluteal artery if a surgical instrument violates the sciatic notch. Injury to the inferior gluteal artery has not been described; it leaves the pelvis below the piriformis muscle belly and should not be at risk even with a violation of the sciatic notch. Injury to the ilioinguinal nerve has been reported from vigorous retraction of the iliacus muscle after exposing the inner table of the anterior ilium. Cluneal nerve injury may occur with posterior crest harvest, particularly if the skin incision is horizontal or extends more than 8 cm superolateral from the posterior superior iliac spine. Kurz LT, Garfin SR, Booth RE Jr: Iliac bone grafting: Techniques and complications of harvesting, in Garfin SR (ed): Complications of Spine Surgery. Baltimore, MD, Williams and Wilkins, 1989, pp 323-341.
Question 93
Collagen orientation is parallel to the joint surface in what articular cartilage zone?
Explanation
The collagen orientation changes from parallel in the superficial zone to a more random pattern in the middle zone and finally to perpendicular in the calcified zone. Koval KJ (ed): Orthopaedic Knowledge Update 7. Rosemont, IL, American Academy of Orthopaedic Surgeons, 2002, pp 498-499.
Question 94
Which of the following tumors have characteristic chromosomal translocations?
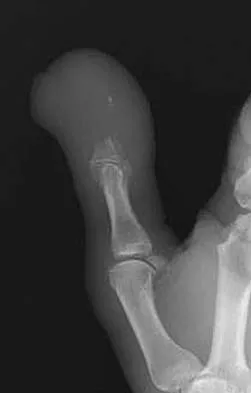
Explanation
Ewing's sarcoma has an 11;22 translocation that creates the EWS/FLI1 fusion gene, and synovial sarcoma has an X;18 translocation that creates the STT/SSX fusion gene. The other tumors do not have consistent translocations. Sandberg AA: Cytogenetics and molecular genetics of bone and soft-tissue tumors. Am J Med Genet 2002;115:189-193.
Question 95
An 18-year-old football player sustains a contact injury to his right lower leg, and radiographs show a closed transverse fracture of the middle third of the tibia. Based on the clinical examination, a compartment syndrome is suspected. When measuring compartment pressures, the highest tissue pressure is recorded how many centimeters proximal or distal to the fracture site?
Explanation
Measurements of compartment pressures in patients with tibial fractures and compartment syndrome reveal that the highest tissue pressures are recorded at the level of the fracture or within 5 cm of the fracture. Tissue pressures show a statistically significant decrease when they are recorded at increasing distances proximal and distal to the site of the highest pressure recorded. To reliably determine the location of the highest tissue pressure in patients with tibial fractures, measurements should be obtained, at a minimum, in both the anterior and deep posterior compartments at the level of the fracture, as well as at locations proximal and distal. The highest tissue pressure recorded should serve as a basis for determining the need for fasciotomy. Heckman MM, Whitesides TE Jr, Grewe SR, Rooks MD: Compartment pressure in association with closed tibial fractures: The relationship between tissue pressure, compartment, and the distance from the site of the fracture. J Bone Joint Surg Am 1994;76:1285-1292.
Question 96
A patient with rheumatoid arthritis has a rupture of the extensor digitorum communis to 4 and 5. You are planning to perform an extensor indicis proprius (EIP) tendon transfer. What effect will this have on index finger extension?
Explanation
EIP transfer results in no functional deficit. If the tendon is cut proximal to the sagittal band, there will be no extensor deficit. Browne EX, Teague MA, Snyder CC: Prevention of extensor lag after indicis proprius transfer. J Hand Surg Am 1979;4:168-172.
Question 97
A 19-year-old man was struck by a car and is seen in the emergency department with a grade IIIC open distal tibia and fibula fracture. Examination reveals that the toes are cool and dusky with a sluggish capillary refill. Angiography reveals a lesion in the posterior tibial artery amenable to repair. There is no sensation on the plantar aspect of the foot, and he is unable to flex his toes. A clinical photograph and radiograph are shown in Figures 2a and 2b. What is the next most appropriate step in management?
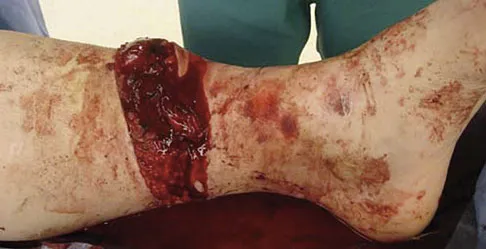
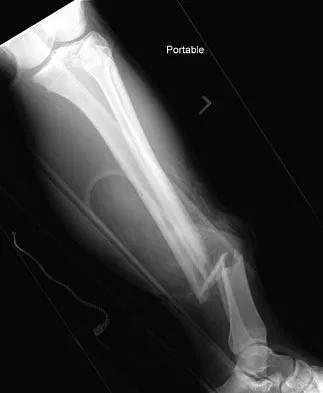
Explanation
In the past, loss of plantar sensation in this grade IIIC tibial fracture would have been an indication for below-knee amputation regardless of the potential for vascular repair. However the 2002 LEAP study divided 55 patients with loss of plantar sensation into two groups, the insensate amputation group and the insensate limb salvage group, with 55% of patients in the insensate salvage group regaining normal sensation 2 years after injury. Furthermore, those in the salvage group who remained insensate after 2 years had equivalent outcomes to those in the amputation group. Because of these findings, limb salvage with vascular repair and external stabilization with delayed closure is deemed appropriate treatment. Immediate intramedullary fixation is not indicated. Because ischemia, contusion, and stretch can adversely affect the tibial nerve, the additional insult of exploration of the nerve is also not advisable given the soft-tissue compromise. Bosse MJ, McCarthy ML, Jones AL, et al: The insensate foot following severe lower extremity trauma: An indication for amputation? J Bone Joint Surg Am 2005;87:2601-2608. Lange RH, Bach AW, Hansen ST Jr, et al: Open tibial fractures with associated vascular injuries: Prognosis for limb salvage. J Trauma 1985;25:203-208. Mackenzie EJ, Bosse MJ, Kellam JF, et al: Factors influencing the decision to amputate or reconstruct after high-energy lower extremity trauma. J Trauma 2002;52:641-649.
Question 98
What is the most common malignant tumor of the foot?
Explanation
Whereas chondrosarcoma is the most frequently occurring malignant bone tumor of the foot and synovial sarcoma is the most common soft-tissue foot malignancy, the most common malignant tumor overall is melanoma. It constitutes approximately 25% of lesions found on the lower extremity. Furthermore, 31% of all melanomas arise in the foot. Mizel MS, Miller RA, Scioli MW (eds): Orthopaedic Knowledge Update: Foot and Ankle 2. Rosemont, IL, American Academy of Orthopaedic Surgeons, 1998, pp 11-26.
Question 99
A 16-year-old girl has had painless swelling in her posterior left arm for the past 4 months. A radiograph, MRI scans, and an incisional biopsy specimen are shown in Figures 43a through 43d. What is the cytogenetic translocation most commonly associated with this tumor?
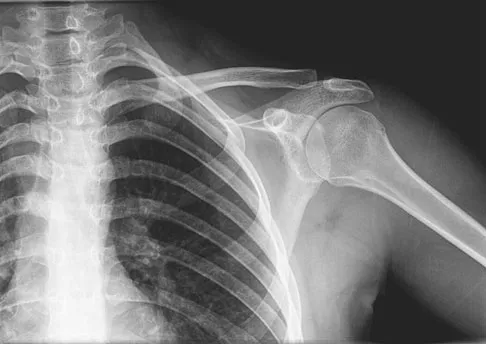
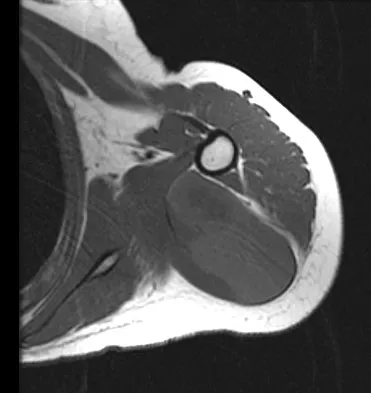
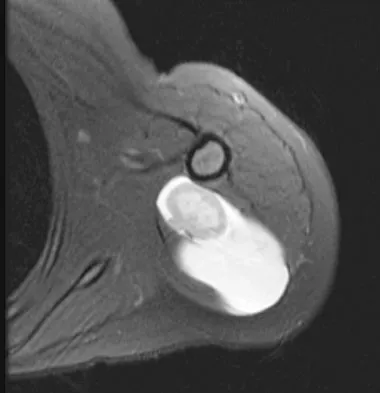
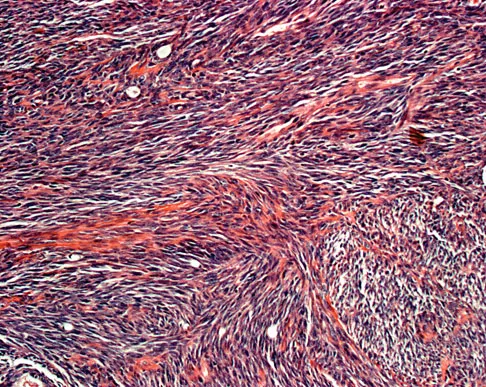
Explanation
This is a case of synovial sarcoma. The radiograph shows some soft-tissue swelling in the upper arm. The MRI scans show a lesion that has increased signal on T2-weighted images and low signal on T1-weighted images. There is a suggestion of a large cystic component to this lesion. The pathology shows a biphasic population of cells, a spindle cell component, and an epithelioid component. Up to 20% of synovial cell sarcomas have areas of cyst formation. The most common cytogenetic translocation with synovial cell sarcoma is X; 18. The 11; 22 translocation is most commonly associated with Ewing's sarcomas; the 12; 22 translocation is most commonly associated with clear cell sarcomas; the 2; 13 translocation is most commonly associated with alveolar rhabdomyosarcomas, and the 12; 16 translocation is most commonly associated with myxoid liposarcomas. Kawai A, Woodruff J, Healey JH, et al: SYT-SSX gene fusion as a determinant of morphology and prognosis in synovial sarcoma. New Engl J Med 1998;338:153-160.
Question 100
A 6-year-old boy has leg pain. A radiograph, MRI, CT, and bone scans, and a biopsy specimen are shown in Figures 14a through 14e. What is the most likely diagnosis?
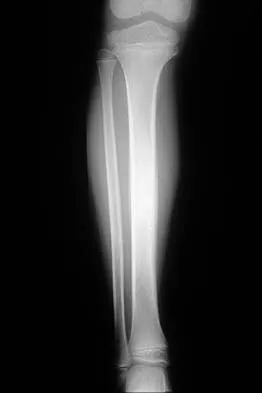
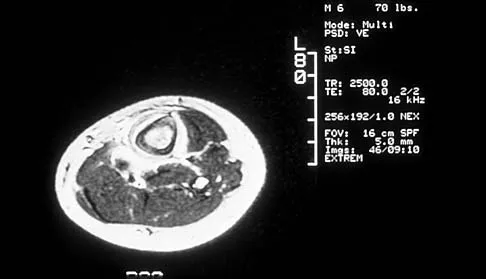
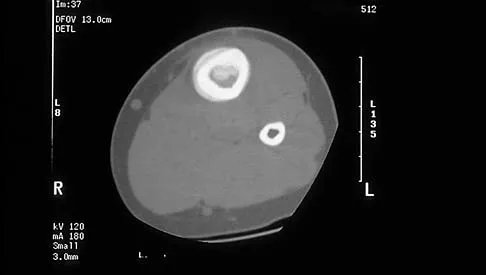
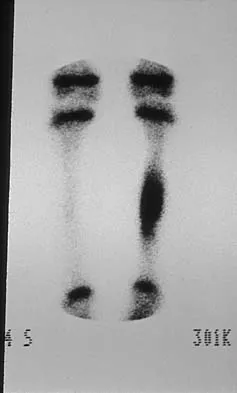
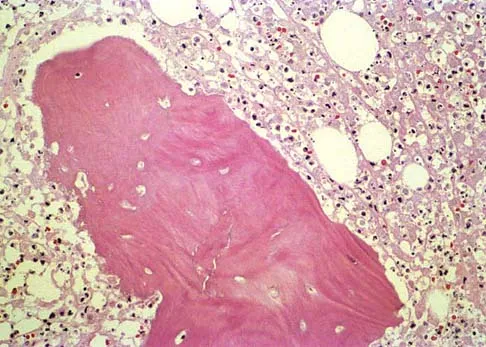
Explanation
From an imaging point of view, all of the diagnoses are possible. Biopsy results and cultures are necessary to make the diagnosis. The biopsy specimen shows inflammatory cells and necrotic bone, consistent with osteomyelitis. Fletcher BD, Hanna SL: Pediatric musculoskeletal lesions simulating neoplasms. Magn Reson Imaging Clin N Am 1996;4:721-747.
