Cracking 11 Pediatric Cases: The Bar with Contralateral Guide
Key Takeaway
Discover the latest medical recommendations for Cracking 11 Pediatric Cases: The Bar with Contralateral Guide. A femur fracture in a 3-month-old nonambulatory child strongly indicates nonaccidental trauma (NAT), with an 80% likelihood. The immediate next step is a thorough full-body examination, including skin assessment, to identify other injuries. Management of such fractures might involve immobilization with a spica cast, potentially incorporating a bar with contralateral leg support for stability and proper alignment.
Detailed Patient Presentation and Mechanism of Injury
Welcome to this Grand Rounds presentation. Today, we are dissecting a highly sensitive, exceptionally critical, and unfortunately common scenario in pediatric orthopedic trauma. The case before us involves a 3-month-old male infant who is brought into the emergency department by his pediatrician following an initial clinic visit. The history provided is notably vague, which should immediately raise your clinical index of suspicion. The child’s grandmother, who is the primary caregiver for the day, reports that she noticed the infant’s left thigh appeared acutely swollen. Furthermore, she observed that the infant was inconsolable and cried forcefully whenever the leg was manipulated, particularly during routine diaper changes.
Crucially, the grandmother noted a phenomenon we refer to as "pseudoparalysis." The infant was observed kicking the contralateral right leg with normal, spontaneous, and symmetric vigor, but the affected left leg remained entirely motionless. There is no reported history of a fall, no motor vehicle collision, and no witnessed traumatic event. The child is non-ambulatory, entirely dependent, and lacks the motor development to generate high-energy forces independently.
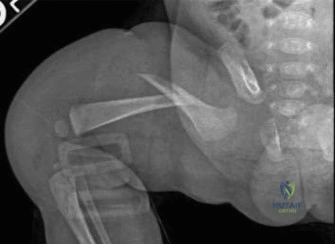
As orthopedic surgeons, we must understand the biomechanical properties of infant bone to appreciate the gravity of this presentation. The pediatric femur, particularly in a 3-month-old, possesses a thick, highly active periosteum and a lower modulus of elasticity compared to adult bone. It is highly porous and requires a substantial, high-energy mechanism—such as a severe axial load, a violent bending moment, or a massive torsional force—to reach the point of catastrophic mechanical failure. When a non-ambulatory infant presents with a diaphyseal or metaphyseal femur fracture in the absence of a verified, high-energy mechanism (like a high-speed motor vehicle accident), the mechanism of injury is incongruent with the clinical findings.
Statistically, up to 80% of femur fractures in children under the age of one year are the direct result of nonaccidental trauma (NAT). While we must systematically rule out metabolic bone diseases, genetic collagenopathies, and birth-related injuries, our foremost duty is to recognize that this fracture pattern in this demographic is pathognomonic for child abuse until definitively proven otherwise. The discrepancy between the innocent history provided by the caregiver and the violent force required to snap an infant's femur is the diagnostic crux of this case.
Pathophysiology of Infant Fractures
To fully grasp the mechanism, we must delve into the microstructural anatomy of the infant skeleton. At three months of age, the bone is predominantly woven rather than lamellar, providing flexibility but lower ultimate tensile strength. However, the energy required to propagate a fracture through the thick pediatric periosteal sleeve is immense. In NAT, the classic mechanism involves a forceful grabbing, twisting, or yanking of the extremity. This generates a spiral or oblique fracture pattern in the diaphysis. Alternatively, violent shaking or pulling can cause shearing forces across the primary spongiosa of the metaphysis, leading to the classic metaphyseal lesion (CML), often described radiographically as a "corner" or "bucket-handle" fracture. Understanding these biomechanics is essential for accurately reconstructing the likely mechanism of injury when consulting with child protection teams.
Comprehensive Clinical Examination Findings
When evaluating a pediatric patient with a suspected femur fracture, particularly in the context of potential NAT, the physical examination must be exhaustive, meticulously documented, and approached with a high degree of clinical objectivity. The initial orthopedic evaluation often begins with the affected extremity, but it absolutely cannot end there.
Upon inspection of the left lower extremity, you will typically note gross swelling, a potential clinical deformity (such as external rotation and shortening), and exquisite tenderness to palpation. The infant will exhibit pseudoparalysis—a protective mechanism where the child refuses to move the limb to prevent pain. While your immediate orthopedic instinct may be to assess for compartment syndrome, it is critical to recognize that acute compartment syndrome of the thigh following an isolated closed femur fracture in an infant is exceedingly rare. The thigh compartments have a massive volume capacity, and the infant's physiological response rarely leads to the tissue pressures necessary to cause ischemic necrosis in this specific scenario. Nevertheless, a baseline neurovascular examination, documenting distal pulses, capillary refill, and spontaneous movement of the toes, is mandatory.
The Head-to-Toe Naked Baby Examination
The most critical step in your evaluation, once the limb is stabilized and the patient's airway, breathing, and circulation are secured, is the complete removal of the infant's clothing. Fractures are only the second most common physical manifestation of child abuse; cutaneous lesions, including bruises, burns, and abrasions, are the most common. You must perform a meticulous head-to-toe skin survey.
We utilize the TEN-4 FACESp clinical decision rule to identify bruising highly predictive of abuse. Any bruising in the Torso, Ears, or Neck (TEN) in a child under 4 years of age, or ANY bruising whatsoever in an infant under 4 months of age, is a massive red flag. You must examine the frenulum for tears (often caused by forceful feeding), inspect the buttocks and perineum for immersion burns or patterned bruising, and palpate the entire skull for occult step-offs indicating skull fractures.

Furthermore, a formal ophthalmologic consultation is non-negotiable. The presence of multi-layered retinal hemorrhages, particularly extending to the periphery of the retina, is highly correlated with abusive head trauma (formerly known as shaken baby syndrome). The orthopedic surgeon is often the first specialist to evaluate these children; therefore, our physical examination sets the trajectory for the entire multidisciplinary investigation.
Advanced Imaging and Diagnostics
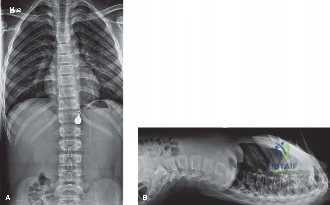
The initial radiographic evaluation of the swollen thigh will confirm the presence of a femur fracture. However, the diagnostic workup for a non-ambulatory infant with a suspicious fracture must immediately pivot to a systemic evaluation for occult injuries. The historical practice of ordering a "babygram"—a single, large-cassette radiograph encompassing the entire infant—is obsolete, medically unacceptable, and medicolegally indefensible. A babygram suffers from severe parallax distortion, inadequate penetration of thicker body parts, and over-penetration of thinner parts, rendering it useless for detecting subtle, high-specificity fractures.
The Skeletal Survey Protocol
The gold standard diagnostic imaging modality is a formal, high-detail Skeletal Survey, performed according to the rigorous guidelines established by the American College of Radiology (ACR) and the American Academy of Pediatrics (AAP). This survey consists of 21 distinct, tightly collimated radiographic views, including bilateral AP and lateral views of the skull, AP and lateral views of the axial skeleton (cervical, thoracic, and lumbar spine), AP views of the bilateral humeri, forearms, femurs, and lower legs, as well as specific views of the hands, feet, and pelvis.
We are specifically hunting for fractures that carry a high specificity for child abuse. These include the Classic Metaphyseal Lesions (CMLs), posterior rib fractures (caused by the clinician's or abuser's hands squeezing the infant's thorax, levering the ribs over the transverse processes), scapular fractures, spinous process fractures, and sternal fractures. Furthermore, the skeletal survey allows us to identify fractures in various stages of healing. Finding a fresh, acute femur fracture alongside a healing posterior rib fracture with robust callus formation proves that the child has been subjected to multiple traumatic events over time, cementing the diagnosis of NAT.
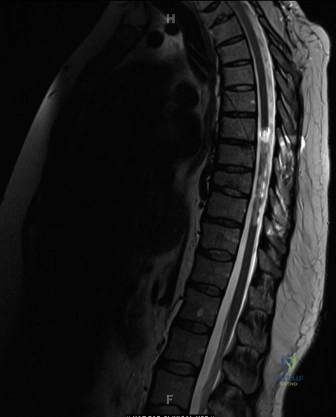
Advanced Neuroimaging and Laboratory Workup
Given the high correlation between abusive skeletal trauma and abusive head trauma, a non-contrast Computed Tomography (CT) scan of the head is mandatory in infants under 6 months of age presenting with high-suspicion fractures, even if they are neurologically intact. We are screening for subdural hematomas, subarachnoid hemorrhage, and cerebral edema.
Simultaneously, a comprehensive laboratory panel must be drawn to rule out metabolic bone disease and bleeding diatheses. This includes serum Calcium, Phosphorus, Alkaline Phosphatase, 25-OH Vitamin D, Parathyroid Hormone (PTH), and a complete coagulation panel (PT, PTT, INR). If Osteogenesis Imperfecta (OI) is suspected based on clinical findings (e.g., blue sclerae, dentinogenesis imperfecta, family history), genetic testing for mutations in the COL1A1 and COL1A2 genes should be initiated, though this should never delay the immediate protection of the child.
Exhaustive Differential Diagnosis
While NAT is the most statistically probable diagnosis for a femur fracture in a 3-month-old, the orthopedic surgeon must maintain extreme academic rigor and systematically exclude other etiologies. Anchoring bias can lead to devastating medicolegal and social consequences. The differential diagnosis must encompass congenital, metabolic, and alternative traumatic etiologies.
Diagnostic Comparison Table
| Condition | Clinical Presentation & Demographics | Radiographic Findings | Key Differentiating Factors |
|---|---|---|---|
| Nonaccidental Trauma (NAT) | Non-ambulatory infant (<1 yr), vague/inconsistent history, delayed presentation, cutaneous bruising. | Diaphyseal spiral/oblique fractures, CMLs, posterior rib fractures, fractures in multiple stages of healing. | Inconsistent mechanism of injury. Normal bone density. Presence of retinal hemorrhages or subdural hematomas. |
| Osteogenesis Imperfecta (OI) | Family history of fragility fractures, blue sclerae, dentinogenesis imperfecta, joint hypermobility. | Osteopenia, thin cortices, bowing deformities, multiple fractures, wormian bones in the skull. | Genetic mutations in COL1A1/COL1A2. Abnormal collagen synthesis. Lack of classic abuse-specific fractures (like CMLs). |
| Birth Trauma | Neonate (usually <2-3 weeks old), history of macrosomia, difficult extraction, breech presentation. | Mid-shaft femur or clavicle fractures. Robust, exuberant callus formation visible by 2-3 weeks of age. | The timeline is critical. A 3-month-old with a fresh fracture cannot be attributed to birth trauma. Birth fractures would be fully healed. |
| Rickets / Metabolic Bone Disease | Nutritional deficiency (lack of Vitamin D), exclusively breastfed without supplementation, premature infants. | Metaphyseal cupping, fraying, and widening. Generalized osteopenia. Looser zones. | Abnormal laboratory values (Low Vit D, elevated Alk Phos, abnormal Ca/Phos). Fractures are typically insufficiency fractures rather than acute traumatic breaks. |
Deep Dive into Osteogenesis Imperfecta
Osteogenesis Imperfecta represents the most common genetic differential diagnosis for NAT. It is a disorder of Type I collagen synthesis. Type I OI is the most common and mildest form, often presenting with blue sclerae and mild to moderate bone fragility. Type II is perinatally lethal. Type III is severe and progressively deforming, while Type IV is intermediate. While a child with OI can certainly suffer from a femur fracture, the radiographic appearance of the bone is rarely normal. We look for profound osteopenia, gracile cortices, and pre-existing bowing deformities. If the skeletal survey reveals normal bone mineralization and cortical thickness, OI becomes exceedingly unlikely, though a genetics consultation remains a prudent step in a comprehensive workup.
Complex Surgical Decision Making and Classifications
The management of an infant femur fracture is a dual-pathway algorithm: we must simultaneously manage the orthopedic injury and navigate the complex psychosocial and medicolegal landscape.
The immediate decision involves hospital admission. Any child with a suspected NAT injury must be admitted to the hospital. This is not merely for pain control or orthopedic intervention; it is a mandatory protective measure. A multidisciplinary child protection team—comprising pediatricians, social workers, orthopedic surgeons, radiologists, and law enforcement—must be activated. Discharging this patient from the emergency department is a catastrophic failure of care that places the child's life in imminent danger.
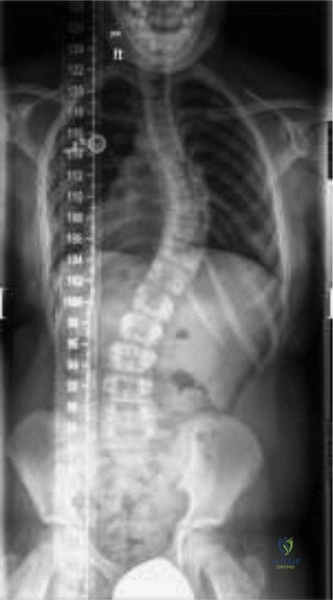
Orthopedic Management Algorithms
From a purely orthopedic standpoint, the treatment of a femur fracture in a 3-month-old is almost exclusively non-operative. The remodeling potential in this age group is nothing short of phenomenal. Infants can correct up to 30 degrees of varus/valgus angulation, 30 degrees of apex anterior/posterior angulation, and up to 1.5 to 2 centimeters of shortening.
The two primary modalities for definitive management are the Pavlik harness and the early application of a hip spica cast.
- The Pavlik Harness: For infants under 6 months of age with a proximal or mid-shaft femur fracture, the Pavlik harness is often the treatment of choice. It is exceptionally well-tolerated, allows for easier diaper changes, and has a lower risk of skin complications compared to a spica cast. The harness holds the hips in flexion and abduction. Biomechanically, this position relaxes the deforming muscle forces (specifically the iliopsoas, which flexes and externally rotates the proximal fragment, and the adductors, which pull the distal fragment medially). By aligning the distal fragment to the flexed and abducted proximal fragment, the harness acts as a dynamic tension-band, utilizing the thick periosteal sleeve to guide reduction.
- The Hip Spica Cast: If the fracture is highly unstable, extremely distal, or if there are concerns about the caregivers' ability to manage a harness (though in NAT cases, the child will likely be placed in foster care), a spica cast is indicated. Spica casting provides rigid immobilization but requires meticulous application technique to prevent skin breakdown, compartment syndrome, and unacceptable malalignment.
Step-by-Step Surgical Technique and Intervention
For the purpose of this Grand Rounds, let us detail the application of a one-and-a-half hip spica cast, which remains a fundamental skill for every orthopedic trauma and pediatric surgeon.
Preparation and Positioning
The procedure is ideally performed in the operating room under general anesthesia to ensure complete muscle relaxation, pain control, and immobility, though it can be performed in the emergency department with deep sedation if necessary. The infant is placed on a specialized pediatric spica table. A well-padded perineal post is utilized.
Padding and Protection
Skin protection is paramount. We begin by applying a Gore-Tex liner or a double layer of specialized stockinette over the torso and bilateral lower extremities. A folded towel is placed over the infant's abdomen before the cast material is applied; this is the "belly space" towel, which will be removed after the cast sets to allow for diaphragmatic expansion and post-prandial abdominal distension. We meticulously pad the bony prominences: the anterior superior iliac spines (ASIS), the sacrum, the greater trochanters, the patellae, and the heels.
Reduction and Casting Technique
The fracture is reduced by applying longitudinal traction. In a proximal third fracture, the proximal fragment is flexed, abducted, and externally rotated by the iliopsoas and gluteal muscles. Therefore, we must bring the distal limb into a matching position of 90 degrees of hip flexion, 30-45 degrees of abduction, and mild external rotation. This is the classic "90-90" position.
We apply the cast material (typically a hybrid of plaster for the initial molding layers, followed by fiberglass for structural integrity). The cast extends from the nipple line down to the toes on the affected side, and down to the knee on the contralateral side (hence, a "one-and-a-half" spica).
The Art of Molding
The critical step is the mold. The surgeon must apply a gentle, broad-based supracondylar mold to control rotation and a lateral mold to prevent varus bowing. We must also ensure the cast is molded well around the iliac crests to prevent the cast from pistoning distally. Once the material sets, the abdominal towel is removed. The perineal opening is carefully trimmed and petaled with waterproof tape to allow for hygienic diapering. A post-application radiograph is obtained in the operating room to confirm acceptable alignment.
Strict Post-Operative Protocol and Rehabilitation Stages
The post-intervention protocol for an infant in a spica cast or Pavlik harness requires rigorous follow-up.
Immediate Post-Intervention Care
Before discharge, the child must undergo a formal car seat test. Standard infant car seats cannot accommodate the abducted leg position of a spica cast. A specialized car seat, such as the Wallaby seat, must be procured, and the caregivers (often foster parents in NAT cases) must be trained on its safe use. Detailed instructions on cast hygiene, double-diapering techniques (tucking a smaller diaper inside the cast edges and placing a larger diaper over the outside), and skin inspection are provided.
Radiographic Follow-up and Remodeling
Orthopedic follow-up is scheduled at 1 week, 2 weeks, and 4 weeks post-application. Radiographs are taken at each visit to ensure maintenance of reduction and to monitor callus formation. In infants, robust woven bone callus is typically visible by 10 to 14 days. Clinical union is usually achieved by 3 to 4 weeks, at which point the cast or harness can be safely discontinued.
We rely heavily on the infant's massive remodeling potential. While we strive for perfect anatomic reduction, we accept up to 30 degrees of angulation in any plane. Over the next 12 to 24 months, the bone will undergo intense osteoclastic resorption on the convex side and osteoblastic bone formation on the concave side, governed by Wolff's Law. However, it is vital to remember that while angulation remodels exceptionally well, rotational malalignment does not remodel reliably. Therefore, controlling rotation during the initial casting or harnessing is the surgeon's most critical biomechanical objective.
High-Yield Clinical Pearls and Pitfalls
To conclude this Grand Rounds, I want to leave you with several non-negotiable clinical pearls and potential pitfalls regarding pediatric femur fractures and nonaccidental trauma:
- The Age Threshold: A femur fracture in a child who is not yet cruising or walking independently (<10-12 months) is child abuse until proven otherwise. Do not let a charming family or a plausible-sounding but low-energy story dissuade you from a thorough workup.
- The Pitfall of the "Babygram": Never order or accept a babygram. Insist on a formal, 21-view Skeletal Survey per ACR guidelines. Missing an occult CML or rib fracture because of poor imaging technique is a catastrophic diagnostic error.
- Mandatory Reporting: As physicians, we are mandatory reporters. You do not need absolute proof of abuse to report; you only need a reasonable clinical suspicion. Failing to report suspected NAT can result in the child being returned to an abusive environment, carrying a high risk of subsequent severe injury or fatality.
- Remodeling Rules: Remember what remodels and what does not. Angulation and shortening (up to 2 cm) will remodel beautifully in an infant. Rotational deformities will persist. Mold your casts to control rotation above all else.
- The Multidisciplinary Shield: You are not alone in these cases. Utilize your pediatricians, child abuse specialists, social workers, and radiologists. The orthopedic surgeon stabilizes the bone, but the team stabilizes the child's life.
Thank you for your attention to this complex and critical topic. We will now open the floor for questions regarding the biomechanics of infant bone or the specifics of spica cast application.
