Intertrochanteric Fracture Fixation Failure: A Deep Dive into Lag Screw Exchange and Cement Augmentation
Introduction & Epidemiology
Intertrochanteric (IT) hip fractures represent a significant global health burden, particularly affecting the elderly population. With an aging demographic, the incidence of these fractures is projected to rise exponentially, imposing immense challenges on healthcare systems worldwide. In the United States alone, an estimated 500,000 adults sustain hip fractures annually, with approximately half being IT fractures. The morbidity and mortality associated with these injuries are substantial, contributing to an inpatient mortality rate of 3-7% and a staggering one-year mortality ranging from 19.4% to 58%. Beyond mortality, these fractures profoundly impact patient quality of life, often leading to chronic pain, loss of independence, and diminished functional status.
Primary treatment for displaced IT fractures almost universally involves internal fixation. The two most commonly employed implants are the cephalomedullary nail (CMN) and the sliding hip screw (SHS). While advancements in implant design and surgical techniques have significantly improved outcomes, fixation failure remains a devastating complication, with recent studies reporting rates as high as 6% even with modern hardware. The consequences of failed fixation, such as implant cutout, nonunion, and malunion, necessitate revision surgery, which carries its own set of complexities and risks.
Revision strategies for failed IT fracture fixation are varied and depend heavily on patient factors, fracture characteristics, and the nature of the failure. Arthroplasty, either hemiarthroplasty or total hip arthroplasty, is often considered the gold standard, particularly in cases of significant femoral head damage, nonunion, or severe malunion. However, arthroplasty in this context is a technically demanding and invasive procedure, frequently associated with increased blood loss, prolonged operative times, heightened risks of intraoperative fracture, and early dislocation, especially in the context of compromised bone stock and altered anatomy. Furthermore, the economic implications of arthroplasty are substantial due to more expensive implants and longer hospital stays. For the frail, elderly patient with multiple comorbidities, these limitations can be prohibitive, underscoring the critical need for alternative, less invasive, yet effective revision treatment modalities.
In response to this clinical imperative, specific institutions have explored and implemented simpler revision techniques. One such approach involves the exchange of the cephalic lag screw with concomitant cement augmentation, a technique reported in small-scale studies primarily from Europe and Asia. This method aims to enhance implant stability and bone-implant interface, offering a potentially less morbid option for select elderly patients with failed IT fracture fixation. This academic review will systematically explore the anatomical, biomechanical, clinical, and technical aspects of intertrochanteric fracture fixation failure and the role of lag screw exchange with cement augmentation as a viable revision strategy.
Surgical Anatomy & Biomechanics
Surgical Anatomy of the Proximal Femur
A thorough understanding of the proximal femoral anatomy is paramount for both primary and revision IT fracture fixation. The proximal femur comprises the femoral head, neck, greater trochanter, lesser trochanter, and the intertrochanteric region.
- Intertrochanteric Region: This area extends from the transcervical line superiorly to a line approximately 5 cm distal to the lesser trochanter. It is characterized by cancellous bone, which, while rich in blood supply, is often osteoporotic in the elderly, contributing to comminution and fixation challenges. The intertrochanteric line anteriorly and the intertrochanteric crest posteriorly connect the greater and lesser trochanters.
- Greater Trochanter: The most lateral prominence, serving as the insertion site for the gluteus medius and minimus, and acting as a critical landmark for CMN insertion.
- Lesser Trochanter: Located posteromedially, it is the insertion point for the iliopsoas muscle and is a key indicator of fracture stability; its displacement signifies an unstable fracture pattern.
- Femoral Neck: Connects the head to the shaft, traversed by the cephalic lag screw. Its integrity and angle (neck-shaft angle, average 125-130°) are crucial for hip mechanics.
- Vascularity: The main blood supply to the femoral head is predominantly from the medial circumflex femoral artery, with contributions from the lateral circumflex femoral artery and the obturator artery. Disruption of this vascularity, especially in fractures extending into the femoral neck, can predispose to avascular necrosis, a critical consideration in any revision setting.
Biomechanics of Intertrochanteric Fractures and Fixation
The biomechanics of the hip joint dictate the forces acting on the proximal femur and, consequently, on implants used for IT fracture fixation.
- Weight-Bearing Axis and Load: The hip joint experiences significant compressive and shear forces during weight-bearing activities. The resultant force vector from body weight and abductor muscle pull passes through the femoral head, placing considerable stress on the intertrochanteric region.
- Fracture Instability: IT fractures are classified by systems such as AO/OTA or the Evan's classification (modified). Unstable patterns (e.g., reverse obliquity, severe comminution of the posteromedial cortex, subtrochanteric extension) are biomechanically disadvantaged, prone to varus collapse, and carry a higher risk of fixation failure. Loss of the posteromedial buttress is a cardinal sign of instability, leading to uncontrolled medialization and cutout.
-
Implant Biomechanics:
- Sliding Hip Screw (SHS): Relies on controlled collapse at the fracture site, allowing impaction and secondary stability. It functions as a load-sharing device. Proper placement of the lag screw (central or slightly inferior in the femoral head on AP view, central in the superior half on lateral view) is critical.
- Cephalomedullary Nail (CMN): A load-sharing device that provides greater stability in unstable fracture patterns due to its intramedullary position, which resists bending and rotational forces. The lag screw (or blade) through the nail into the femoral head provides proximal fixation.
- Tip-Apex Distance (TAD): This critical parameter, defined as the sum of the distance from the tip of the lag screw to the apex of the femoral head on both AP and lateral radiographs, is a strong predictor of fixation success. A TAD > 25 mm significantly increases the risk of cutout. Optimal TAD ensures the lag screw is centrally located within the femoral head, maximizing bone purchase and preventing eccentric loading.
- Bone Quality: Osteoporosis significantly compromises the ability of bone to hold screws, leading to poor screw purchase, loss of reduction, and subsequent implant cutout. This is a primary driver for fixation failure in the elderly and a key indication for cement augmentation in revision settings.
- Neck-Shaft Angle: A varus neck-shaft angle, either pre-existing or resulting from inadequate reduction, predisposes the implant to increased shear forces and cutout.
Understanding these anatomical and biomechanical principles is essential for identifying risk factors for failure, selecting appropriate implants, performing meticulous surgical technique, and, critically, planning effective revision strategies such as lag screw exchange with cement augmentation.
Indications & Contraindications
The decision to proceed with revision surgery for a failed intertrochanteric fracture fixation, and the choice of revision modality, is complex and multifactorial.
Indications for Revision Internal Fixation (Lag Screw Exchange with Cement Augmentation)
This specific revision technique is most suitable for a carefully selected cohort of patients.
- Painful Fixation Failure with Intact Nail/Plate: The primary indication is persistent or new onset of significant hip pain associated with radiological evidence of implant cutout (e.g., lag screw protrusion into the hip joint), loosening of the lag screw within the femoral head, or signs of impending cutout, while the main implant (CMN or plate) remains well-fixed within the femoral shaft.
- Nonunion with Adequate Reduction and Stable Primary Implant: In cases where a nonunion develops but the primary implant is stable and the fracture reduction is acceptable, enhancing the fixation within the femoral head can promote healing.
- Osteopenia/Osteoporosis-Related Failure: Patients with severe osteopenia or osteoporosis where the initial lag screw failed to achieve sufficient purchase, leading to cutout, are prime candidates for cement augmentation. The cement reinforces the cancellous bone, improving screw purchase and stability.
- Elderly and Frail Patients: This technique offers a less invasive alternative to arthroplasty, minimizing surgical insult, blood loss, and operative time. This makes it particularly attractive for patients with significant comorbidities who may not tolerate the physiological stress of a joint replacement.
- Femoral Head Preservation: For patients where preservation of the native femoral head is desirable (e.g., younger patients, although IT fractures are less common in this group), this technique can be considered if the head itself is not severely damaged or avascular.
- Isolated Lag Screw Malposition/Migration: If the original lag screw was malpositioned (e.g., high TAD) and has migrated, exchanging it for a new, correctly positioned screw, reinforced with cement, can provide improved biomechanical stability.
Contraindications for Lag Screw Exchange with Cement Augmentation
Several factors preclude the use of this technique:
- Gross Malunion or Significant Femoral Deformity: If the primary fracture healed in severe malunion (e.g., excessive varus, rotation), a simple lag screw exchange will not correct the underlying deformity. These cases often require osteotomy or arthroplasty.
- Failed or Broken Primary Implant: If the CMN itself has broken, backed out, or the side plate of an SHS has fractured, a simple lag screw exchange is insufficient. The entire construct needs revision, often involving implant removal and replacement or conversion to arthroplasty.
- Septic Nonunion or Periprosthetic Joint Infection: Any evidence of infection (elevated inflammatory markers, sinus tract, purulence) is an absolute contraindication to cement augmentation without prior infection eradication.
- Severe Femoral Head Avascular Necrosis (AVN): If the femoral head is severely necrotic, it cannot support a new screw or benefit from cement augmentation. Arthroplasty is indicated.
- Extensive Femoral Head Comminution/Damage: If the femoral head itself is severely comminuted, fractured, or has extensive bone loss from multiple cutouts, there may not be enough bone stock to hold cement or a new screw effectively.
- Patient Inability to Tolerate Any Surgery: In extremely frail patients, palliative care or non-operative management may be the only option if revision surgery of any type is deemed too risky.
- Hardware Breakage Preventing Removal: If the original lag screw or its locking mechanism is broken and cannot be safely removed, the exchange technique cannot be performed.
- Lack of Surgeon Experience: This is a specialized revision technique; it should only be performed by surgeons experienced in complex hip fracture management and bone cement handling.
Table: Revision Strategy Selection for Failed Intertrochanteric Fractures
| Revision Strategy | Primary Indication(s) | Key Considerations/Contraindications It is the most common reason for emergency surgery in patients over 65 years.
Fixation failure in IT fractures leads to significant morbidity and mortality, making revision strategies crucial.
Factors contributing to fixation failure are multifactorial:
*
Patient-related:
Advanced age, osteoporosis, poor nutritional status, comorbidities (e.g., diabetes, dementia).
*
Fracture-related:
Unstable fracture patterns (AO/OTA 31-A2, A3), severe comminution, particularly of the posteromedial cortex.
*
Surgeon-related:
Inadequate reduction (especially varus angulation), suboptimal implant placement (high Tip-Apex Distance [TAD] > 25mm, eccentric screw position), choice of implant for a given fracture pattern.
*
Implant-related:
While modern implants are robust, mechanical failure can occur with excessive stress or poor bone-implant interface.
Revision surgery aims to address these failures, alleviate pain, improve function, and allow for weight-bearing mobilization.
Surgical Anatomy & Biomechanics
Surgical Anatomy of the Proximal Femur
The proximal femur encompasses the femoral head, neck, and the trochanteric region. The intertrochanteric area, specifically, is bounded superiorly by the base of the femoral neck and inferiorly by the subtrochanteric region, extending approximately 5 cm distal to the lesser trochanter. This region is primarily composed of cancellous bone, which is a critical consideration in both primary fixation and revision, especially in osteoporotic bone.
- Greater Trochanter: This large, quadrangular prominence serves as the primary insertion point for the gluteus medius and minimus muscles. It is a key landmark for the entry portal of cephalomedullary nails. The trochanteric fossa lies on its medial aspect.
- Lesser Trochanter: Located posteromedially, it is the insertion site for the iliopsoas tendon. Its integrity or displacement is often indicative of fracture stability; a comminuted or detached lesser trochanter usually signifies an unstable IT fracture pattern (e.g., AO/OTA 31-A2.2 or A2.3).
- Intertrochanteric Line/Crest: The intertrochanteric line runs obliquely across the anterior surface of the proximal femur, connecting the two trochanters, and marks the distal capsular attachment. Posteriorly, the more prominent intertrochanteric crest connects the greater and lesser trochanters, often featuring the quadrate tubercle.
- Femoral Neck: Connects the femoral head to the shaft, characterized by both cortical and cancellous bone. The caliber and density of the cancellous bone within the femoral head and neck are critical for lag screw purchase.
- Vascularity: The main blood supply to the femoral head is predominantly from the medial circumflex femoral artery, particularly its retinacular branches ascending along the femoral neck. Preservation of this blood supply is paramount to prevent avascular necrosis (AVN), a feared complication that can exacerbate fixation failure or complicate revision.
Biomechanics of Intertrochanteric Fractures and Fixation
The proximal femur is subjected to substantial biomechanical forces during daily activities. Understanding these forces and how they interact with implants is crucial for preventing and managing fixation failure.
- Weight-Bearing Load: The hip joint bears loads equivalent to 2.5 to 3 times body weight during single-limb stance, and significantly higher forces during activities such as stair climbing or running. These forces generate compressive, shear, and bending stresses across the intertrochanteric region.
- Fracture Stability: The stability of an IT fracture largely depends on the integrity of the posteromedial cortex. Loss of this crucial buttress (e.g., in AO/OTA 31-A2 and A3 patterns) leads to an unstable construct prone to varus collapse and medial migration of the femoral shaft relative to the femoral head.
-
Implant Design Principles:
- Sliding Hip Screw (SHS): This extramedullary device allows for controlled collapse and impaction at the fracture site, theoretically promoting secondary bone healing and reducing the risk of screw cutout. It functions as a load-sharing device.
- Cephalomedullary Nail (CMN): An intramedullary device that provides enhanced biomechanical stability, particularly for unstable fracture patterns, by acting as a load-sharing device and resisting bending and rotational forces within the medullary canal. The cephalic screw (lag screw or blade) component is crucial for proximal fixation within the femoral head.
- Tip-Apex Distance (TAD): This is the most widely recognized radiographic predictor of cephalic implant cutout. It is the sum of the distance from the tip of the lag screw/blade to the apex of the femoral head on both anteroposterior (AP) and lateral radiographs. A TAD exceeding 25 mm significantly correlates with an increased risk of cutout. Optimal placement aims for a TAD of <25 mm, ideally within the "safe zone" of 10-20 mm, ensuring the screw is centrally positioned in the femoral head (especially in the inferior-central quadrant on AP and central in the superior half on lateral views). This maximizes bone purchase and distributes stresses effectively.
- Bone Quality: Osteoporosis, prevalent in the elderly, is a primary biomechanical challenge. Reduced bone mineral density directly compromises screw purchase, leading to screw toggle, loss of reduction, and subsequent cutout. Cement augmentation directly addresses this by reinforcing the weakened cancellous bone, thus improving the bone-implant interface.
- Varus Collapse: Inadequate reduction, particularly resulting in varus angulation, or progressive collapse due to an unstable fracture pattern, increases shear forces on the lag screw, predisposing it to cutout and fixation failure.
Indications & Contraindications
The decision to revise a failed intertrochanteric fracture fixation is complex and hinges on several factors, including the patient's functional status, comorbidities, the nature of the fixation failure, and the condition of the bone and joint. The choice of revision strategy must be meticulously tailored to each individual case.
Indications for Revision: Lag Screw Exchange with Cement Augmentation
This specific revision technique is a less invasive option best suited for a carefully selected patient population.
-
Symptomatic Lag Screw Cutout/Migration:
The primary indication is significant hip pain and functional impairment due to documented lag screw migration, perforation of the femoral head into the joint, or progressive cutout, provided the main implant (cephalomedullary nail or sliding hip screw side plate) remains acceptably positioned and stable within the femoral shaft.

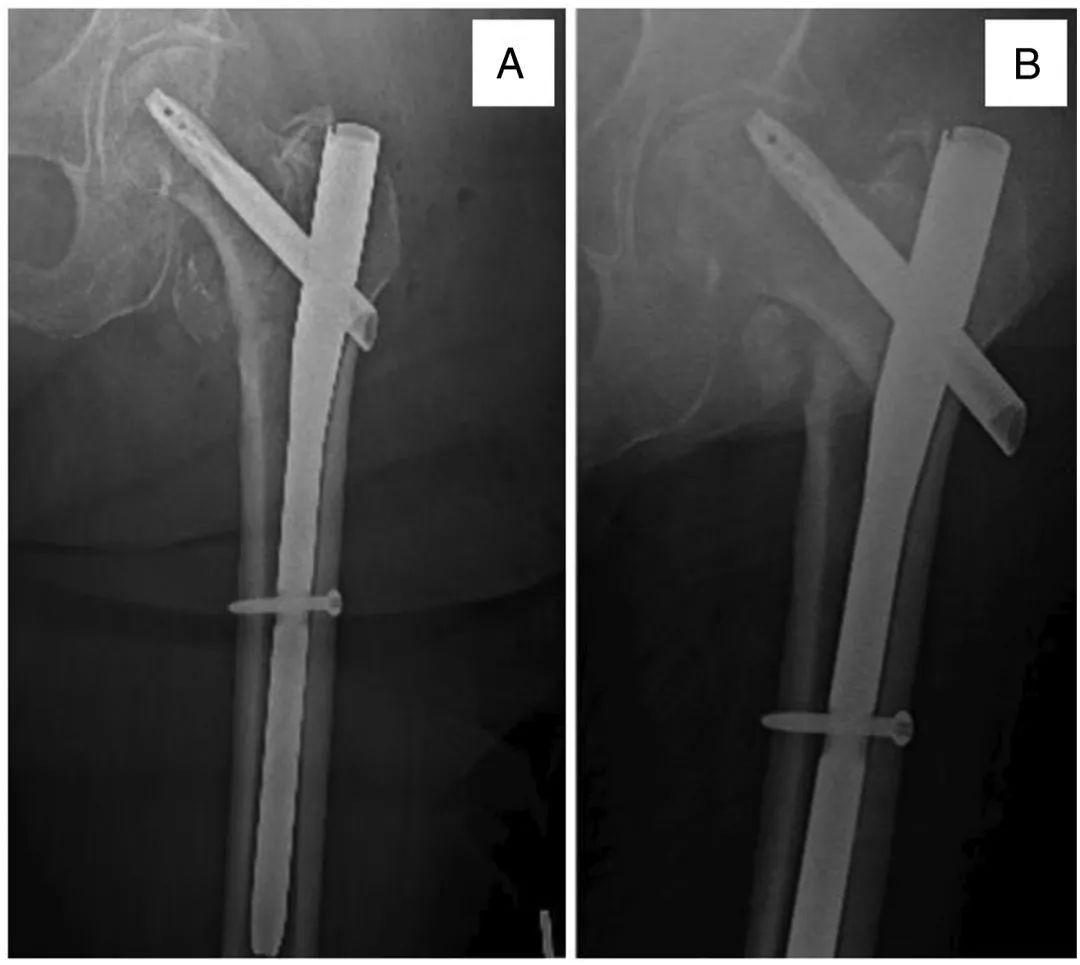
Figure 1: A 76-year-old female initially treated with a CMN for an intertrochanteric fracture (A). Two months post-operatively, she experienced persistent hip pain due to implant cutout into the femoral head (B), indicating failure amenable to revision. - Osteoporosis-Related Failure: In elderly patients with severe osteopenia or osteoporosis where the original lag screw failed to achieve adequate purchase, leading to loss of fixation without significant malunion. Cement augmentation reinforces the compromised cancellous bone, significantly improving screw purchase and stability.
- Impending Cutout/Early Loosening: Radiographic evidence of early lag screw loosening or migration without overt cutout but with clinical symptoms suggestive of fixation instability.
- Nonunion with Preserved Femoral Head: In cases of painful nonunion where the primary implant is stable, reduction is adequate, and the femoral head has good viability and structural integrity, improving the stability of the cephalic fixation may promote healing.
- Frail, Elderly Patients with Multiple Comorbidities: This technique is a less physiologically demanding alternative to arthroplasty, minimizing operative time, blood loss, and the risks associated with major reconstructive surgery. It is particularly valuable for patients who are high-risk for hip arthroplasty.
- Salvage of Initial Reduction: When the overall fracture reduction (e.g., neck-shaft angle, fracture fragment alignment) is acceptable, but only the cephalic fixation has failed, this technique offers a chance to salvage the existing reduction and avoid more extensive reconstructive procedures.
Contraindications for Lag Screw Exchange with Cement Augmentation
Absolute or strong relative contraindications for this revision strategy include:
- Gross Malunion: If the initial fracture healed in a severely malaligned position (e.g., unacceptable varus, rotational deformity, leg length discrepancy), merely replacing the lag screw will not correct the underlying deformity. These cases often require osteotomy or conversion to arthroplasty.
- Gross Failure of Primary Implant: If the main implant (e.g., CMN itself fractured or backed out, SHS side plate broken or extensively loosened) has failed, merely exchanging the lag screw is insufficient. The entire construct needs revision.
- Significant Femoral Head Damage or Avascular Necrosis (AVN): If the femoral head is severely comminuted, osteonecrotic, or has sustained extensive bone loss from multiple prior cutouts, there may be insufficient viable bone stock to effectively augment with cement or hold a new lag screw.
- Active Infection: Any signs of active periprosthetic infection (elevated inflammatory markers, sinus tract, purulence) are an absolute contraindication to the immediate placement of cement. Infection must be thoroughly addressed first, often with a two-stage procedure.
- Unreconstructible Bone Loss: If there is extensive bone loss around the lag screw track that cannot be adequately filled or stabilized by cement, conversion to arthroplasty may be necessary.
- Hardware Breakage Preventing Removal: If the original lag screw or its locking mechanism is broken in a manner that prevents safe and complete removal, the exchange technique cannot be performed.
- Patient Unsuitable for Any Operative Intervention: In rare cases of extreme frailty, a non-operative approach with palliative care may be the only option.
Table: Revision Strategy Comparison for Failed Intertrochanteric Fractures
| Revision Strategy | Ideal Patient Profile | Primary Advantages | Primary Disadvantages |
|---------------------------------------|----------------------------------------------------------|-------------------------------------------------------------------------------------------------------------------|------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------ Will during surgery the physician or another qualified professional use imaging to confirm proper placement of the implant? The patient will be appropriately draped and prepped in the usual sterile fashion to perform a hip hemiarthroplasty. The patient will be positioned supine on the operating table, and a standard anteroposterior (AP) pelvis X-ray will be obtained to confirm appropriate patient alignment and rotation. The affected leg will be draped free for full manipulation during the procedure. An incision will be made in the lateral aspect of the hip, centered over the greater trochanter, extending proximally and distally. The incision will be deepened through the subcutaneous tissue and fascia lata. The vastus lateralis muscle will be incised or elevated off the greater trochanter to expose the hip joint capsule. A capsulotomy will be performed to gain access to the femoral head and neck. The femoral head will be dislocated and carefully removed. The femoral canal will be prepared using reamers and rasps to achieve the appropriate size and fit for the femoral stem. The prosthetic femoral head will be selected, and trial components will be inserted to assess leg length, offset, and stability. Once optimal parameters are confirmed, the definitive femoral stem and head will be impacted. The hip will be reduced, and the range of motion and stability will be assessed. The wound will be irrigated and closed in layers. A sterile dressing will be applied. The patient will be transferred to recovery in stable condition.
What else should be included in the operative report to clearly convey to a third-party payer the need for a total hip arthroplasty (THA) or hemiarthroplasty (HHA) revision instead of a simple cephalomedullary nail (CMN) lag screw exchange, given the provided clinical scenario?
Considering the provided clinical scenario, where the initial surgery was for an intertrochanteric fracture that presumably failed, and the proposed procedure is a hip hemiarthroplasty (HHA), the operative report needs to explicitly justify why HHA (or THA, if applicable) is necessary over a less extensive revision like a lag screw exchange. The current operative report template is generic for a primary HHA and lacks specific details regarding the failure of the previous fixation.
Here's what should be included in the operative report to clearly convey the need for HHA/THA revision to a third-party payer:
Additional Critical Elements for a Revision Hemiarthroplasty/Total Hip Arthroplasty Operative Report:
1. Preoperative Diagnosis & History of Present Illness (HPI) -
Expanded
*
Failed Intertrochanteric Fracture Fixation (e.g., with specific details like nonunion, malunion, implant cutout, periprosthetic fracture, implant breakage).
*
Previous Surgical Procedure(s):
Explicitly state the date and type of the initial surgery (e.g., "Status post open reduction internal fixation (ORIF) of left intertrochanteric hip fracture with cephalomedullary nail (CMN) on [Date of original surgery]").
*
Reason for Failure:
Clearly describe the presenting problem leading to revision. For example:
* "Persistent intractable hip pain and inability to bear weight due to [specify e.g., femoral head cutout of lag screw, radiographic evidence of nonunion, severe varus malunion, periprosthetic fracture around the stem, breakage of the cephalomedullary nail]."
* Reference specific preoperative imaging findings (X-rays, CT scans, MRI) that demonstrate the failure: "Preoperative imaging demonstrated [e.g., lag screw penetration into the acetabulum, substantial destruction of the femoral head, nonunion with significant bone loss, varus collapse and malalignment of the proximal femur, implant breakage within the femoral shaft]."
*
Patient's Functional Impairment:
Document the impact on the patient's daily life, e.g., "Patient unable to ambulate even with assistive devices, requiring full-time care, significant decline in quality of life."
2. Intraoperative Findings -
Crucially Expanded
This is the most critical section for justifying the choice of revision surgery. Describe the condition of the tissues and prior hardware upon exposure.
- Prior Incision: "Prior lateral incision was utilized and extended..."
-
Condition of Previous Hardware:
- "Upon exposure, the previously placed cephalomedullary nail (CMN) was identified."
- "Examination of the femoral head revealed [e.g., significant destruction/fragmentation of the femoral head secondary to lag screw cutout, large defect in the superior femoral head where the lag screw had migrated, extensive chondral damage to the femoral head and/or acetabulum resulting from implant penetration]."
- "The lag screw was found to be [e.g., completely migrated through the femoral head and into the acetabulum, grossly loose within the osteopenic femoral head, broken at the neck-shaft junction]."
- "The femoral neck was noted to be [e.g., nonunited with fibrous tissue and sclerotic margins, severely comminuted, malunited in significant varus/rotation]."
- "Assessment of the primary implant (CMN): The intramedullary component of the CMN was [e.g., well-seated but the lag screw mechanism had failed, noted to have micromotion within the femoral canal, found to be fractured at the proximal locking screw site, difficult to extract due to bone ingrowth/fracture]."
- "Bone quality: The cancellous bone of the proximal femur and femoral head was noted to be severely osteoporotic and attenuated, further compounding the challenge of achieving stable fixation with an internal fixation device alone."
-
Rationale for Abandoning Internal Fixation Revision (Lag Screw Exchange):
- "Due to the extensive destruction of the femoral head and/or femoral neck, the profound osteopenia, and the inability to achieve adequate purchase or stability for a revised lag screw, a simple lag screw exchange was deemed biomechanically unsound and highly unlikely to succeed."
- "The extent of femoral head destruction precluded a reconstructive approach aimed at preserving the native femoral head."
- "The severe malunion of the femoral neck/intertrochanteric region would not be addressed by lag screw exchange and required prosthetic replacement to restore anatomical alignment and function."
- "Given the patient's age, comorbidities, and the catastrophic nature of the previous fixation failure, a definitive solution offering predictable weight-bearing and pain relief was prioritized over another attempt at internal fixation revision."
3. Hardware Removal -
Detailed
* "The existing cephalomedullary nail and lag screw were carefully removed. [Describe any difficulties encountered, e.g., stripped screw heads, bone overgrowth, the need for specialized extraction tools, potential for iatrogenic fracture during removal]."
* "Upon removal, further assessment confirmed the inadequacy of the remaining bone stock for any form of internal fixation revision."
4. Implant Selection Justification -
Expanded
* "Given the extent of proximal femoral bone loss, the severe osteopenia, and the patient's functional demands, a cemented/uncemented femoral stem was selected to ensure maximal stability and allow for immediate weight-bearing." (Justify cemented vs. uncemented based on bone quality).
* "A bipolar/unipolar femoral head prosthesis was chosen for hemiarthroplasty to articulate with the native acetabulum. [If converting to THA, explicitly state reasons for acetabular component placement, e.g., 'pre-existing acetabular degeneration, extensive acetabular cartilage damage observed intraoperatively, or to minimize risk of acetabular erosion in active patients']."
5. Postoperative Plan -
Expanded
* "Patient will be allowed [specify weight-bearing status, e.g., immediate full weight-bearing as tolerated, protected weight-bearing for 6 weeks, etc.] based on prosthetic stability and bone quality." This is often a significant advantage over another internal fixation, which might require protected weight-bearing.
By including these specific details, the operative report moves beyond a generic description of an HHA to a comprehensive justification for a complex revision procedure, clearly delineating why a simpler, less costly alternative (like lag screw exchange) was inappropriate given the extensive nature of the failure. This provides the third-party payer with a robust clinical and surgical rationale for the chosen procedure.
Clinical & Radiographic Imaging