Introduction & Epidemiology
Thumb mallet finger, characterized by the inability to actively extend the interphalangeal (IP) joint of the thumb, represents a distinct and relatively rare injury compared to its more common counterparts in the lesser digits. Epidemiological data indicates that thumb mallet injuries constitute approximately 2-3% of all mallet finger presentations, making it an infrequent, yet functionally significant, entity for the hand surgeon. This rarity often translates to a less standardized approach in management compared to other mallet injuries.
The etiology of thumb mallet finger is predominantly traumatic, with a notable incidence in athletic populations dueating to high-impact or forceful flexion injuries. While mallet injuries in the lesser digits are frequently closed avulsions of the extensor digitorum communis (EDC) or extensor indicis proprius (EIP) tendons, thumb mallet injuries exhibit a higher propensity for open lacerations or avulsions of the extensor pollicis longus (EPL) tendon. This difference underscores the distinct biomechanical forces at play and the anatomical characteristics of the thumb's extensor mechanism. Closed injuries, though less common, do occur and present unique diagnostic and therapeutic challenges, particularly concerning the extent of tendon retraction. The profound functional importance of the thumb necessitates precise diagnosis and an optimized treatment strategy to restore maximal IP joint extension and overall hand dexterity.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the thumb's extensor mechanism is paramount for the effective management of thumb mallet injuries.
Extensor Pollicis Longus (EPL) Tendon
The EPL tendon is the primary extensor of the IP joint of the thumb, as well as an extensor and abductor of the carpometacarpal (CMC) joint and extensor of the metacarpophalangeal (MCP) joint. Originating from the posterior surface of the ulna and the interosseous membrane, the EPL courses distally, passing through the third dorsal compartment of the wrist, where it hooks around Lister's tubercle. This anatomical arrangement allows it to gain a mechanical advantage for extension and abduction.
Distally, the EPL tendon inserts onto the dorsal base of the distal phalanx of the thumb. Unlike the complex sagittal band and lateral band system of the lesser digits' extensor mechanism, the EPL tendon in the thumb lacks true dedicated lateral bands originating from the EPL itself. Instead, fibers from the intrinsic muscles, specifically the abductor pollicis brevis (APB) and adductor pollicis (AdP), contribute to the extensor mechanism by blending into the dorsal hood and sending fibers that extend distally to insert on the尺侧和桡侧 of the EPL tendon, continuing towards the distal phalanx base. These intrinsic contributions provide supplementary stability and extension force, particularly at the MCP joint, but their direct role in IP joint extension after EPL avulsion is limited.
Key anatomical considerations in thumb mallet finger:
*
Strong Extensor Force:
The EPL is a powerful muscle with a substantial moment arm at the IP joint, contributing to its strong contractile force. This inherent strength contributes to significant tendon retraction upon injury.
*
Long Excursion:
The EPL has a relatively long excursion, meaning that when avulsed, the proximal stump can retract a considerable distance, often proximally to the MCP joint or even further, making retrieval challenging.
*
Thicker Tendon:
Compared to the terminal extensor tendons of the lesser digits, the EPL is a robust and thicker tendon. This characteristic can be advantageous during surgical repair, as it provides more substance for secure suture placement and improved pull-out strength.
*
Unique IP Joint Stability:
A distinguishing feature of thumb mallet finger, as highlighted in existing literature, is the infrequent occurrence of IP joint subluxation or dislocation. This is attributed to the inherent stability provided by the IP joint capsule and collateral ligaments, as well as the unique anatomical insertion of the EPL and the absence of a direct force vector that typically causes dorsal subluxation in lesser digits' mallet injuries. Consequently, joint stability is often preserved despite tendon disruption.
*
Distal Phalanx Anatomy:
The distal phalanx is relatively short, and its dorsal base provides the insertion site for the EPL. Bony avulsions typically involve a portion of this dorsal base, potentially compromising articular congruence if displaced.
Biomechanics of Injury
Thumb mallet finger typically results from a sudden, forceful passive flexion of the IP joint against an actively contracting EPL (e.g., catching a ball awkwardly, falling onto the thumb). This mechanism can lead to:
1.
Tendon Avulsion:
The EPL tendon ruptures at its insertion into the distal phalanx. The strong muscle belly then causes significant proximal retraction.
2.
Bony Avulsion:
A fragment of the dorsal distal phalanx is avulsed along with the EPL tendon. The size and displacement of this fragment are critical in determining treatment.
The loss of active IP extension leads to a "mallet" deformity, where the distal phalanx rests in a flexed position. The extensor lag can vary depending on the completeness of the injury and any residual contribution from the intrinsic muscles. The significant retraction capability of the EPL means that approximation of tendon ends can be difficult, even in closed injuries, requiring careful assessment to guide treatment.
Indications & Contraindications
The decision-making process for thumb mallet finger, whether conservative or operative, hinges on a careful assessment of injury type, extent of tendon retraction, joint stability, patient factors, and functional demands. Unlike lesser finger mallet injuries where conservative management is often the default, the thumb's critical role often shifts the paradigm towards earlier operative intervention, especially with significant extensor lag or bony involvement.
Non-Operative Indications
Non-operative management for thumb mallet finger is considered for a select subset of patients, typically involving strict immobilization of the IP joint in full extension.
*
Closed Tendon Avulsions with Minimal Retraction:
Injuries where the tendon ends are in close apposition, confirmed by imaging (e.g., ultrasound, MRI), and the extensor lag is minimal (e.g., <10-15 degrees).
*
Small Bony Avulsions:
Fractures involving less than 30% of the articular surface, with no significant displacement or joint incongruity, and demonstrated stability on clinical and radiographic examination.
*
Patient Preference & Compliance:
For patients who are fully informed of the potential for persistent extensor lag and who are highly committed to a prolonged period of strict splinting (typically 6-8 weeks continuously, followed by nocturnal splinting for several more weeks).
*
High Surgical Risk Comorbidities:
Patients with significant medical comorbidities that preclude safe anesthesia or surgery.
*
Sedentary Lifestyle:
Individuals with low functional demands on their thumb.
Operative Indications
Operative intervention is generally favored for thumb mallet injuries due to the critical function of the thumb and the high propensity for tendon retraction.
*
Open Injuries:
Any open laceration of the EPL tendon requires surgical exploration, debridement, and primary repair to prevent infection and restore tendon integrity.
*
Closed Tendon Avulsions with Significant Retraction:
When MRI or dynamic ultrasound demonstrates significant retraction of the proximal tendon stump, indicating a large gap between tendon ends. The original content highlights that "磁共振检查可以确认肌腱回缩距离,断端之间裂隙较大者,通常无保守治疗机会。" (Magnetic resonance imaging can confirm the distance of tendon retraction; those with a large gap between the tendon ends usually have no opportunity for conservative treatment.)
*
Bony Avulsions with Significant Articular Involvement:
Fractures involving >30-50% of the articular surface of the distal phalanx.
*
Displaced Bony Fragments:
Any bony avulsion fragment that is significantly displaced, leading to joint incongruity or instability.
*
Failed Conservative Management:
Persistent or worsening extensor lag, pain, or functional impairment despite an adequate trial of non-operative treatment.
*
Chronic Mallet Deformity:
Established deformities (>3-6 months post-injury) with significant extensor lag and functional deficit. These often require more complex reconstructive procedures.
*
Young, Active Individuals:
Patients with high functional demands, especially athletes, where optimal functional restoration is paramount.
Contraindications
-
Absolute Contraindications:
- Active local infection at the surgical site (relative contraindication for elective repair; infection must be managed first).
- Uncontrolled systemic infection.
- Severe, unstable medical comorbidities that pose an unacceptably high anesthetic or surgical risk.
-
Relative Contraindications:
- Poor patient compliance with post-operative rehabilitation protocols.
- Severe, pre-existing osteoarthritis of the IP joint (in such cases, IP joint arthrodesis might be a more suitable primary procedure).
- Extremely fragile skin or soft tissues.
Summary of Operative vs. Non-Operative Indications
| Feature / Condition | Non-Operative Treatment | Operative Treatment |
|---|---|---|
| Tendon Injury | Closed, minimal retraction, good apposition (e.g., <5mm gap) | Open injuries, significant retraction (e.g., >5mm gap on MRI) |
| Bony Avulsion | Small fragment (<30% articular surface), no joint incongruity, stable | Large fragment (>30-50% articular surface), joint incongruity, displaced fragment |
| Joint Stability | Stable IP joint | Unstable IP joint (rare for thumb mallet, but a definitive indication) |
| Patient Factors | Compliant patient, high surgical risk, low functional demands | Active individual, good compliance expected, high functional demands |
| Chronic Deformity | Mild extensor lag, minimal functional impact | Significant extensor lag (>30 degrees), functional impairment, established deformity |
| Failed Conservative Trial | No improvement after 6-8 weeks of strict splinting | Persistent or worsening deformity after adequate trial |
Pre-Operative Planning & Patient Positioning
Careful pre-operative planning is essential to anticipate surgical challenges and optimize outcomes for thumb mallet finger repair.
Pre-Operative Assessment
- Detailed History and Physical Examination: Document mechanism of injury, time since injury, previous treatments, and patient's functional demands. Assess IP joint extensor lag, passive range of motion, and any associated injuries. Note any skin compromise or pre-existing conditions.
-
Imaging Studies:
- Standard Radiographs: Anteroposterior (AP) and true lateral views of the thumb are crucial for identifying bony avulsions, assessing fragment size, displacement, and articular involvement. Lateral views are critical for confirming joint congruity. Oblique views may provide additional information.
-
Magnetic Resonance Imaging (MRI):
As emphasized in the seed content, MRI is invaluable, especially for closed tendon injuries. It provides detailed visualization of the soft tissues, allowing for precise assessment of EPL tendon integrity, the extent of retraction of the proximal stump, and the presence of any intervening hematoma or scar tissue. This information directly influences the decision for surgery and helps plan the extent of surgical exploration.
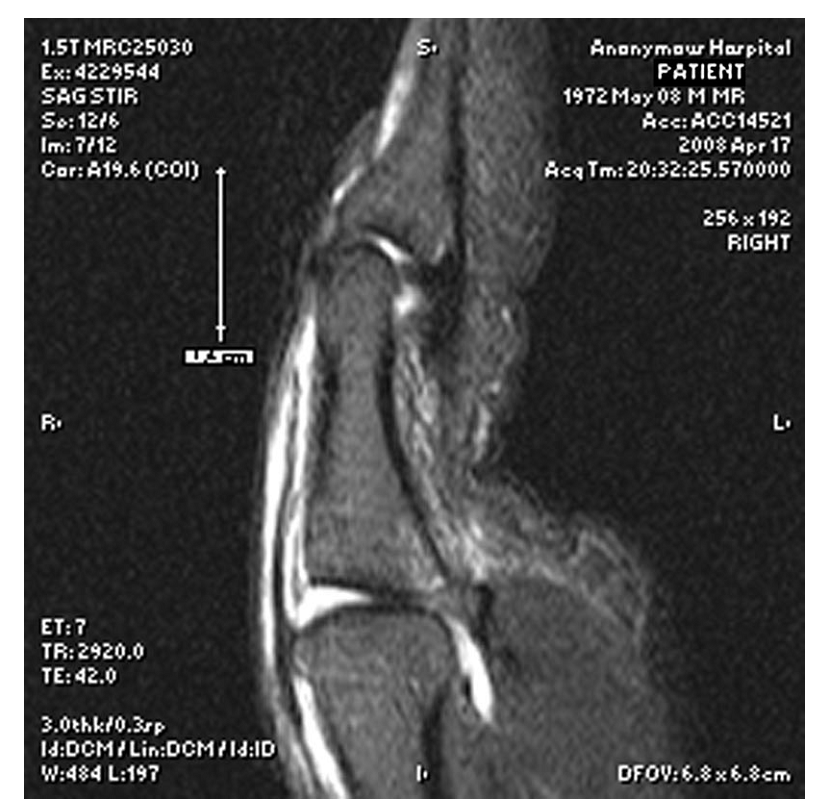
The image above depicts a sagittal MRI view demonstrating significant EPL tendon retraction (white arrow) from its insertion, indicating a large gap between tendon ends. Such findings strongly advocate for surgical intervention due to the low probability of successful conservative management. - Ultrasound: Dynamic ultrasound can also be used to assess tendon retraction in real-time, although it is highly operator-dependent. It can differentiate between complete and partial tears and assess tendon excursion.
Anesthesia and Tourniquet
- Anesthesia: Regional anesthesia (e.g., axillary block, supraclavicular block) is often preferred, providing excellent intraoperative analgesia and prolonged post-operative pain control, reducing the need for systemic opioids. General anesthesia is an alternative depending on patient preference and surgeon judgment.
- Tourniquet: A pneumatic tourniquet on the upper arm is routinely used to provide a bloodless field, which is critical for identifying delicate structures and performing precise tendon or bone repair. Standard inflation pressures are typically 250-300 mmHg.
Patient Positioning and Preparation
- Positioning: The patient is positioned supine on the operating table. The affected arm is abducted and placed on a specialized hand table, ensuring comfortable access for the surgeon and assistant. The entire arm should be prepped and draped to allow for potential extension of the incision or harvesting of graft material if necessary.
- Sterile Prep and Drape: The hand and forearm are prepped with an antiseptic solution (e.g., chlorhexidine or povidone-iodine) and draped using sterile technique, isolating the surgical field.
- Instrumentation: Ensure availability of fine hand instruments, microsurgical instruments (if tendon grafting or complex repair is anticipated), K-wires (0.035" or 0.045"), mini-screws/plates, suture anchors, and appropriate suture material (e.g., 3-0 or 4-0 non-absorbable core sutures, 5-0 or 6-0 absorbable epitendinous sutures). Fluoroscopy should be readily available for bony avulsion repairs.
Detailed Surgical Approach / Technique
Surgical repair of thumb mallet finger aims to restore anatomical tendon continuity or bony alignment, allowing for active IP joint extension and minimizing extensor lag. The specific technique depends on the type of injury (tendon avulsion vs. bony avulsion, acute vs. chronic).
Incision and Exposure
- Incision Design: A dorsal longitudinal or slightly curvilinear incision centered over the IP joint and distal phalanx is typically employed. This provides direct access to the extensor mechanism. For chronic injuries or those requiring extensive exploration, a lazy-S or modified Z-plasty incision may be considered to prevent scar contracture and improve exposure.
- Skin Incision: Meticulous skin incision is crucial to avoid injury to the superficial dorsal sensory nerves and veins.
- Subcutaneous Dissection: Careful blunt and sharp dissection proceeds through the subcutaneous tissue. Identify and protect any dorsal veins, retracting them judiciously. Identify the dorsal hood mechanism.
-
Identification of Tendon Ends:
- For tendon avulsions , the distal stump may be very small or absent, with the EPL tendon having avulsed directly from the bone. The proximal stump of the EPL tendon will often be significantly retracted, sometimes even proximal to the MCP joint. The strong retracting force of the EPL makes its retrieval a primary step. This may require gently milking the forearm musculature or extending the incision proximally.
- For bony avulsions , the avulsed fragment will be located dorsally at the base of the distal phalanx, often tethered by the avulsed EPL tendon.
Internervous Planes
The dorsal aspect of the thumb IP joint does not involve distinct internervous planes in the manner of deeper limb compartments. The dissection is superficial, focusing on longitudinal separation of tissues to access the extensor mechanism while protecting the small dorsal sensory branches of the radial nerve and superficial veins.
Tendon Repair (Acute Tendon Laceration/Avulsion)
- Debridement: Trim any frayed or unhealthy tissue from the tendon ends to ensure a clean, viable surface for repair.
- Retrieval and Mobilization: Retrieve the retracted proximal EPL tendon stump. If significant retraction makes direct repair difficult, gentle proximal dissection or even a small counter-incision proximally may be required to mobilize the tendon. The IP joint is kept in full extension to reduce tension.
-
Repair Technique:
- Core Suture: A strong, non-absorbable core suture technique is paramount. Modified Kessler, modified Bunnell, or four-strand repairs (e.g., Savage, Lim-Tsai) are commonly used. Typically, 3-0 or 4-0 braided polyester or similar non-absorbable suture is preferred. The core sutures should be placed to achieve maximum purchase within the tendon substance without constricting the tendon.
- Anchoring to Bone: If the tendon has avulsed from bone without a significant bony fragment, the tendon end must be securely reattached to the dorsal base of the distal phalanx. This can be achieved using transosseous pull-out sutures through drill holes in the distal phalanx or via a suture anchor system inserted into the dorsal distal phalanx.
- Epitendinous Suture: After securing the core repair, a running epitendinous suture (e.g., 5-0 or 6-0 absorbable monofilament) is performed circumferentially to smooth the repair site, improve tendon gliding, and increase the strength of the repair by coapting the peripheral fibers.
- Tension Assessment: With the IP joint fully extended (0 degrees), the repair should be tension-free. Excessive tension can lead to repair failure or compromise vascularity, while insufficient tension will result in persistent extensor lag.
Bony Avulsion Repair (Acute Fractures)
- Reduction: Gently manipulate the avulsed bony fragment back into its anatomical position, ensuring a congruent articular surface. Fluoroscopy is invaluable at this stage to confirm accurate reduction.
-
Fixation Methods:
The choice of fixation depends on the size and morphology of the bony fragment.

The image above illustrates various fixation methods for bony avulsion mallet fingers, demonstrating pre-operative, post-operative, and final follow-up radiographic views. These techniques range from K-wire fixation to mini-screw applications.-
K-wire Fixation:
- Transarticular K-wire: A 0.035" or 0.045" K-wire can be inserted from the tip of the distal phalanx, across the IP joint, and into the proximal phalanx, immobilizing the joint in full extension. This provides stable immobilization during healing. For bony fragments, a second K-wire can be inserted across the fracture fragment into the distal phalanx.
- Fragment-to-fragment K-wire: For larger fragments, one or two fine K-wires can be used to directly fix the fragment back to the distal phalanx.
- Pull-Out Wire Technique: For small, comminuted fragments or when direct fixation is challenging, a pull-out wire can be passed through the tendon and fragment, exiting volarly through the distal phalanx, and tied over a button or bolster on the volar skin. This provides compressive force to hold the fragment in place.
- Mini-Screws/Suture Anchors: For larger bony fragments providing adequate bone stock, a mini-screw (e.g., 1.0mm or 1.3mm cortical screw) can provide rigid fixation. Alternatively, a small suture anchor can be placed into the distal phalanx, and sutures passed through the avulsed tendon and fragment, providing secure reattachment and compression.
- Tension Band Wiring: Less commonly used for thumb mallet, but may be considered for larger fragments with sufficient bone for wire tunnels, to convert distractive forces into compressive forces.
-
K-wire Fixation:
- Confirmation: Once fixed, confirm stable anatomical reduction with fluoroscopy.
Chronic Mallet Deformity
Management of chronic thumb mallet involves addressing established scar tissue and often necessitates reconstructive techniques due to tendon shortening and joint contracture.
*
Scar Excision and Release:
Extensive debridement of scar tissue around the tendon ends and IP joint capsule is required to mobilize the tendon and allow for IP joint extension.
*
Tendon Lengthening or Grafting:
* If a significant tendon gap exists after mobilization, a local V-Y plasty or Z-plasty lengthening of the EPL may be attempted.
* If the gap is too large for direct repair or local lengthening, an interposition tendon graft (e.g., palmaris longus, plantaris, or a segment of an extensor indicis proprius) may be required.
*
Arthrodesis:
In cases of severe, painful, or functionally debilitating chronic mallet deformity with irreparable tendon damage or significant joint destruction/arthrosis, IP joint arthrodesis in a functional position (e.g., 15-20 degrees of flexion) may be the most reliable salvage procedure to provide a stable, painless, and functional thumb.
IP Joint Stabilization (Optional but Recommended)
For most thumb mallet repairs, particularly bony avulsions or extensively retracted tendon repairs, temporary transarticular K-wire fixation of the IP joint in full extension (0 degrees) is highly recommended. A 0.035" or 0.045" K-wire is typically inserted from the dorsal aspect of the distal phalanx, across the IP joint, and into the proximal phalanx, ensuring it is parallel to the dorsal cortex and avoids the articular cartilage if possible. This protects the repair site from early stress and allows for healing in the correct position for 4-6 weeks.
Wound Closure
- Irrigate the wound thoroughly.
- Perform layered closure, reapproximating the subcutaneous tissues with fine absorbable sutures.
- Close the skin with fine non-absorbable sutures (e.g., 5-0 or 6-0 nylon), ensuring tension-free closure.
- Apply a sterile dressing.
Complications & Management
Despite meticulous surgical technique, complications can arise following thumb mallet finger repair. Awareness of these potential issues and strategies for their management is critical for optimal patient outcomes.
Common Complications and Management Strategies
| Complication | Incidence | Management / Salvage Strategy |
|---|---|---|
| Extensor Lag / Re-rupture | 5-15% |
Early:
Re-exploration, revision repair.
Late: Tenolysis, tendon graft, tenodesis, IP fusion. |
| Stiffness / Loss of Motion | 10-20% | Intensive physiotherapy, dynamic splinting (extension/flexion), tenolysis, capsulotomy. |
| Infection | <5% | Antibiotics (IV/oral), wound debridement, hardware removal (if applicable), irrigation. |
| Pain / Tenderness | Variable | Analgesics, therapy, address underlying causes (e.g., hardware prominence, nerve irritation, CRPS). |
| Pin Track Infection | 5-10% (with K-wires) | Local wound care, oral antibiotics. Pin removal if persistent or severe. |
| Nail Deformity | 5-10% | Primarily cosmetic. Nail bed repair if directly injured during trauma/surgery. |
| Nonunion / Malunion (Bony) | <5% |
Nonunion:
Revision fixation with bone grafting, IP fusion.
Malunion: Corrective osteotomy, IP fusion. |
| Complex Regional Pain Syndrome (CRPS) | Rare | Early recognition, multidisciplinary pain management, physical and occupational therapy, sympathetic blocks. |
| Neurovascular Injury | Rare | Intraoperative repair if recognized. Post-operative surveillance. |
| Hardware-Related Issues | Variable | Pain from prominent K-wires or screws, breakage. Removal of symptomatic hardware. |
Discussion of Complications
- Extensor Lag / Re-rupture: This is the most common and often functionally significant complication. It can result from insufficient repair strength, excessive tension, premature mobilization, or poor patient compliance. Early recognition of significant extensor lag post-splint removal warrants aggressive hand therapy. Persistent significant lag or re-rupture may necessitate revision surgery, potentially involving tendon grafting (e.g., palmaris longus, EIP slip) if a large defect exists, or a tenodesis procedure. In chronic, failed cases with severe deformity and loss of function, IP joint arthrodesis can provide a stable, painless thumb.
- Stiffness / Loss of Motion: While the IP joint is immobilized in extension, other joints (MCP, CMC) must be actively moved to prevent global thumb stiffness. Excessive or prolonged immobilization can lead to capsular contracture and loss of both flexion and extension. Aggressive hand therapy with active and passive range of motion exercises, and dynamic splinting, is crucial. In refractory cases, surgical tenolysis or capsulotomy may be considered.
- Infection: Superficial wound infections can usually be managed with antibiotics and local wound care. Deep infections are more serious and require surgical debridement, intravenous antibiotics, and potentially removal of hardware. Pin track infections around K-wires are relatively common but usually resolve with local care and oral antibiotics; persistent infection necessitates pin removal.
- Nail Deformity: Injury to the nail bed during trauma or surgery can lead to cosmetic nail deformities (e.g., ridging, splitting, onycholysis). Direct repair of the nail bed during initial surgery can mitigate this risk.
- Nonunion / Malunion of Bony Fragments: Inadequate reduction, unstable fixation, or biological factors can lead to nonunion or malunion. Nonunion of a bony fragment may result in chronic pain, instability, or persistent deformity and may require revision fixation with bone grafting. Malunion may necessitate corrective osteotomy or, in severe cases, IP joint arthrodesis.
- CRPS (Complex Regional Pain Syndrome): Though rare in the thumb, CRPS is a debilitating pain condition that can follow hand trauma or surgery. Early diagnosis and aggressive multidisciplinary treatment, including physical therapy, pain management, and pharmacotherapy, are essential.
Post-Operative Rehabilitation Protocols
A structured and disciplined post-operative rehabilitation program is paramount for achieving optimal functional outcomes following surgical repair of thumb mallet finger. Patient compliance is a critical determinant of success.
Phase I: Immobilization and Protection (Weeks 0-4 or 0-6)
The primary goal of this phase is to protect the repair site and allow for initial tendon-bone or tendon-tendon healing, while preventing stiffness in uninvolved joints.
*
IP Joint Immobilization:
* If a transarticular K-wire was used, the IP joint is internally splinted in full extension (0 degrees).
* If no K-wire was used, a custom-molded thermoplastic splint (e.g., stack splint, dorsal block splint) or casting is applied, maintaining the IP joint in full extension at all times. The splint should allow full range of motion at the MCP and CMC joints.
*
Mobility of Uninvolved Joints:
*
Active Range of Motion (AROM):
Patients are instructed to actively move their MCP and CMC joints of the thumb, as well as all joints of the lesser digits, several times a day.
*
Passive Range of Motion (PROM):
Gentle passive motion of the MCP and CMC joints can also be performed.
*
Edema Control:
Elevation of the hand, gentle compression dressings, and active motion of uninvolved joints are encouraged to minimize swelling.
*
Wound Care:
Regular dressing changes and monitoring for signs of infection. Suture removal typically occurs at 10-14 days.
Phase II: Early Controlled Mobilization (Weeks 4-6 to Weeks 8-10)
This phase introduces controlled motion to the IP joint, gradually increasing stress on the healing repair.
*
K-wire Removal (if applicable):
Typically performed at 4-6 weeks post-operatively.
*
Protective Splinting:
The IP joint continues to be protected in full extension, often with a custom-fabricated dorsal blocking splint (stack splint or similar) that allows for active IP flexion to a pre-determined limit (e.g., 20-30 degrees) but blocks IP extension past neutral. This splint is worn continuously, only removed for exercises and hygiene.
*
Initiation of IP Joint Motion:
*
Active IP Flexion:
Gentle active flexion of the IP joint is initiated, carefully monitoring for signs of discomfort or increased extensor lag. The goal is to gradually increase the flexion range while avoiding any active extension beyond neutral.
*
Passive IP Flexion:
Very gentle passive IP flexion within the active range, and controlled by the therapist.
*
Tendon Gliding Exercises:
Active MCP and CMC motion helps promote EPL tendon gliding.
*
Scar Management:
Gentle scar massage and desensitization if needed.
Phase III: Progressive Strengthening and Full ROM (Weeks 8-10 to Weeks 12-16)
The goal of this phase is to restore full range of motion and gradually introduce strengthening exercises.
*
Gradual Weaning from Splint:
The extension protection splint is gradually weaned during the day, with continued use during sleep or during activities at risk for re-injury.
*
Progressive ROM:
Active and passive IP joint flexion is progressively increased. The goal is to achieve full pain-free range of motion.
*
Gentle Strengthening:
* Light resistance exercises for IP joint extension and flexion are introduced. This might include therapeutic putty, rubber bands, or light weights.
* Intrinsic muscle strengthening to improve overall hand function.
*
Functional Activities:
Begin incorporating the thumb into light daily activities.
Phase IV: Return to Activity (Weeks 16+)
This final phase focuses on maximizing strength, endurance, and preparing for a full return to work, sports, or demanding activities.
*
Advanced Strengthening:
Progressive resistive exercises are advanced for all thumb and hand movements.
*
Proprioceptive and Dexterity Training:
Focus on fine motor skills and coordination specific to the patient's occupational or recreational demands.
*
Activity Modification:
Continue to advise on activity modification and protective measures.
*
Return to Sport/Work:
Gradual return to strenuous activities, often with continued protective splinting during high-risk activities for up to 6 months post-operatively.
Key Principles of Rehabilitation
- Patient Education and Compliance: The patient must understand the injury, the surgical repair, and the importance of strict adherence to the rehabilitation protocol.
- Protection of the Repair: The most critical aspect is protecting the healing tendon from excessive stress, especially during the early phases.
- Controlled Progression: Rehabilitation should be carefully monitored by a hand therapist, with gradual increases in range of motion and strength based on individual healing and progress.
- Early Motion of Uninvolved Joints: To prevent generalized stiffness.
- Pain and Edema Management: Crucial throughout all phases.
Summary of Key Literature / Guidelines
The existing literature on thumb mallet finger, while less extensive than for other digits, provides important insights into its diagnosis and management. The rarity of the injury often leads to treatment protocols extrapolated from general mallet finger principles, with crucial adaptations for the unique thumb anatomy and function.
- Epidemiology and Diagnosis: Studies consistently highlight the low incidence of thumb mallet injuries (2-3% of all mallet fingers) and the prevalence of open injuries or significant retraction in closed cases. The diagnostic utility of MRI in visualizing tendon retraction, as noted in the original content, is a recurring theme in contemporary hand surgery literature. MRI offers superior soft-tissue contrast compared to ultrasound, especially for quantifying the gap between retracted tendon ends, which is a strong indicator for surgical intervention. Plain radiographs remain essential for identifying bony avulsions and assessing articular involvement.
- Anatomical Distinctions: Academic discussions frequently emphasize the unique anatomy of the EPL tendon, particularly its powerful nature, long excursion, and the contributing fibers from APB and AdP, which differentiate it from the extensor mechanism of the lesser digits. The observation that thumb mallet injuries rarely result in IP joint subluxation or dislocation, due to inherent capsular and ligamentous stability, is a critical distinguishing factor influencing treatment strategies. This stability implies that the primary focus of repair is tendon continuity, rather than joint reduction and stabilization of a frankly dislocated joint.
-
Treatment Paradigm:
While conservative management (splinting in extension) is often the first line for uncomplicated closed mallet fingers in lesser digits, the literature suggests a higher threshold for operative intervention in the thumb. This is primarily driven by:
- The significant retraction potential of the powerful EPL, leading to large tendon gaps that are unlikely to heal conservatively.
- The critical functional importance of the thumb, demanding optimal restoration of IP joint extension.
-
The higher incidence of open injuries.
For bony avulsions, surgical fixation is generally recommended for fragments involving >30-50% of the articular surface or those causing joint incongruity, aligning with principles for other intra-articular fractures. Various fixation techniques, including K-wires, mini-screws, and pull-out sutures, are described, with outcomes often dependent on fragment size and surgeon preference, as illustrated in the provided examples.
- Surgical Techniques and Outcomes: Direct tendon repair using robust core sutures (e.g., modified Kessler, 4-strand techniques) augmented by epitendinous repair is the gold standard for acute tendon ruptures. For reattachment to bone, transosseous sutures or suture anchors are commonly employed. In chronic cases or those with significant tendon loss, tendon grafting (e.g., palmaris longus) or tenodesis procedures are discussed as reconstructive options, with arthrodesis serving as a reliable salvage procedure for irreversible damage or severe chronic deformity. Outcomes generally report good to excellent functional results with surgical repair, although residual extensor lag remains a common complication.
- Rehabilitation Protocols: The literature consistently stresses the importance of structured post-operative rehabilitation, characterized by initial strict immobilization of the IP joint in full extension (typically 4-6 weeks), followed by gradual, controlled mobilization. Patient compliance with splinting and therapeutic exercises is highlighted as a critical factor for success. The duration of immobilization and the precise timing of active motion initiation are areas of ongoing discussion, with some advocating for slightly earlier controlled motion in selected stable repairs.
In summary, the academic consensus emphasizes that thumb mallet finger, despite its rarity, warrants a distinct and often more aggressive management approach compared to lesser digit mallet injuries. The unique anatomical and biomechanical features, combined with the thumb's paramount functional role, necessitate precise diagnostic evaluation (with MRI being particularly useful for tendon retraction assessment) and tailored surgical strategies to achieve optimal long-term outcomes. Continued research focusing on optimal fixation methods, rehabilitation protocols, and long-term comparative studies for different injury types would further refine treatment guidelines.

