Introduction & Epidemiology
Traumatic spondylolisthesis of C2, colloquially known as a Hangman's fracture, is a historically significant yet anatomically diverse injury pattern of the subaxial cervical spine. Defined by bilateral fractures through the pars interarticularis or pedicles of the axis (C2), this injury results in anterior displacement of the C2 vertebral body relative to C3. The nomenclature stems from the original description of cervical spine injuries sustained during judicial hanging, although the mechanisms encountered in contemporary trauma are significantly broader.
Epidemiologically, Hangman's fractures account for approximately 4-7% of all cervical spine fractures and 15-20% of C2 fractures. They are predominantly observed in high-energy trauma, most commonly motor vehicle accidents (MVAs) and falls, particularly in elderly populations. The injury mechanism in MVAs typically involves sudden deceleration leading to hyperextension and axial loading, often with a flexion component. True distraction-hyperextension, akin to the original hanging mechanism, is less common in modern trauma but results in the most severe fracture types.
A critical consideration in the management of these injuries is the potential for associated trauma. Concomitant cervical spine fractures occur in approximately 30% of cases, necessitating a thorough evaluation of the entire cervical and upper thoracic spine. Beyond osseous injuries, associated neurovascular and craniofacial injuries are not infrequent. This includes potential for cranial nerve deficits, vertebral artery dissection or occlusion, and concurrent facial trauma. Given the intimate relationship of the vertebral artery with the C2 transverse foramen and its course, any significant displacement or angulation of C2 warrants meticulous vascular assessment.
The incidence of spinal cord injury (SCI) with Hangman's fractures varies significantly with the fracture subtype. Type I and Type II fractures, while unstable, are often associated with a low incidence of complete SCI due to the decompression afforded by the displacement of the C2 body anteriorly, effectively enlarging the spinal canal at the C2-C3 level. However, Type III injuries, characterized by severe C2-C3 facet dislocation, carry a significantly higher risk of neurological compromise and complete SCI. Understanding these distinctions is paramount for appropriate triage, diagnostic workup, and definitive management strategies. The initial assessment must therefore extend beyond plain radiographs to include advanced imaging modalities such as computed tomography (CT) and magnetic resonance imaging (MRI) to fully delineate osseous, ligamentous, and neurovascular involvement.
Surgical Anatomy & Biomechanics
The axis (C2) is a transitional vertebra, bridging the highly mobile craniovertebral junction with the more rigid subaxial spine. Its unique anatomy is critical to understanding Hangman's fractures. Key anatomical features include:
- Vertebral Body: The main load-bearing anterior component.
- Dens (Odontoid Process): Articulates with the C1 anterior arch, forming the atlantoaxial joint. While not directly fractured in a Hangman's, its integrity is essential for C1-C2 stability.
- Pedicles: Connect the vertebral body to the posterior elements. The pars interarticularis, a constricted region between the superior and inferior articular facets, is the typical site of fracture in Hangman's injury.
- Laminae: Form the posterior arch, protecting the spinal cord.
- Superior Articular Facets: Large, flat, and superiorly directed, articulating with the inferior facets of C1.
- Inferior Articular Facets: Anteriorly and inferiorly directed, articulating with the superior facets of C3. These facets, along with the C2-C3 intervertebral disc, form a critical load-bearing and motion segment.
- Transverse Processes: Contain the foramen transversarium, through which the vertebral artery ascends. Fractures involving C2 can directly injure the vertebral artery.
Ligamentous structures play a vital role in C2-C3 stability. The anterior longitudinal ligament (ALL) and posterior longitudinal ligament (PLL) provide significant anterior and posterior column support, respectively. The intervertebral disc at C2-C3 is a key component, with its integrity varying significantly across fracture types. The ligamentum flavum, interspinous, and supraspinous ligaments also contribute to posterior element stability.
The biomechanics of Hangman's fractures are complex and involve varying combinations of forces:
- Hyperextension-Axial Loading: The most common mechanism. In hyperextension, the inferior articular facets of C2 impinge on the pars interarticularis of C3, creating a fulcrum. Axial load then causes a buckling failure through the pars of C2.
- Flexion-Axial Loading: Less common for typical Hangman's, but contributes to Type IA and potentially Type II fracture patterns, especially when combined with lateral bending.
- Distraction: Pure distraction, as seen in judicial hanging, causes simultaneous hyperextension and separation of the C2-C3 segment. This typically results in bilateral pedicle fractures and complete disruption of the C2-C3 disc and ligamentous complex, leading to severe instability.
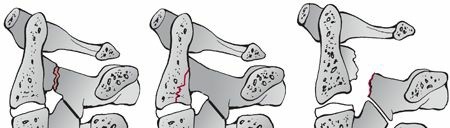
Classification (Levine and Edwards; Effendi)
The Levine and Edwards classification system, building upon Effendi's initial work, remains the most widely accepted for guiding clinical management and prognosis. This system categorizes Hangman's fractures based on displacement, angulation, and the integrity of the C2-C3 disc and associated ligaments.
Type I: Nondisplaced, No Angulation
This type is characterized by bilateral C2 pedicle or pars interarticularis fractures with minimal or no anterior angulation and translation of the C2 body relative to C3, typically less than 3 mm. The C2-C3 intervertebral disc and anterior/posterior longitudinal ligaments are considered intact or minimally disrupted. These injuries are typically caused by hyperextension and axial loading. Despite being a fracture through the pars, Type I fractures are considered relatively stable due to the intact C2-C3 disc-ligament complex, allowing for management with rigid cervical immobilization. They represent approximately 29% of Hangman's fractures. Spinal cord injury is rare with this type.

Type IA: Atypical Unstable Lateral Bending Fractures
This is a more recently recognized subtype, often resulting from axial loading combined with lateral bending. It involves an oblique fracture pattern, typically unilateral or markedly asymmetric, extending anterior to the pars interarticularis into the vertebral body on the contralateral side. These fractures are characterized by significant lateral displacement and angulation but minimal anterior translation. The mechanism often involves lateral flexion and compression. Type IA fractures are considered unstable due to their atypical fracture line and are often irreducible by traction, posing unique challenges for non-operative management.
Type II: Significant Angulation and Translation
Type II fractures represent the most common injury pattern, accounting for approximately 56% of cases. They are characterized by significant anterior translation of the C2 body relative to C3, exceeding 3 mm, and/or significant angulation at the C2-C3 interspace, typically greater than 10-15 degrees. Crucially, the C2-C3 intervertebral disc and its associated ligaments (ALL and PLL) are disrupted, rendering this fracture inherently unstable. The mechanism typically involves initial hyperextension and axial load, followed by a flexion-compression or flexion-distraction component that drives the C2 body forward. These injuries often require reduction and stabilization.
Type IIA: Avulsion of Entire C2-C3 Intervertebral Disc in Flexion
This subtype is characterized by severe angulation at the C2-C3 level with minimal anterior translation, distinguishing it from Type II. The injury occurs via a flexion-distraction mechanism, leading to a complete avulsion or disruption of the entire C2-C3 intervertebral disc. The posterior longitudinal ligament (PLL) often remains intact, while the anterior longitudinal ligament (ALL) is typically avulsed. This allows for significant angulation with a "teeter-totter" effect. Despite minimal translation, this fracture is highly unstable, particularly in flexion, and is notoriously difficult to stabilize with traction due to the intact PLL acting as a fulcrum, potentially exacerbating the angulation. It requires distinct management considerations compared to Type II.

Type III: Bilateral C2 Pedicle Fractures with Severe C2-C3 Facet Dislocation
Type III fractures are the most severe and least common type, resulting from extreme flexion-compression with distraction, typically seen in judicial hanging or severe MVAs. They involve bilateral C2 pedicle fractures in conjunction with a severe C2-C3 facet dislocation, which may be unilateral or bilateral, often resulting in locked facets. The C2-C3 disc and all associated ligaments are completely disrupted. These injuries are profoundly unstable and carry the highest incidence of severe neurological deficit, including complete spinal cord injury, due to direct compression or distraction of the cord. Immediate and meticulous management is essential.

Indications & Contraindications
The decision-making process for managing Hangman's fractures hinges on the Levine and Edwards classification, patient factors, and the overall stability of the C2-C3 motion segment.
Non-Operative Indications
- Levine and Edwards Type I: These fractures are generally considered stable due to intact C2-C3 disc and ligaments. Management involves rigid external immobilization, typically a halo vest, for 8-12 weeks. Close radiographic follow-up is essential to monitor for any delayed displacement or angulation.
- Select Type IIA with minimal displacement (Controversial): In very specific cases, if there is minimal angulation and no significant translation, a trial of halo immobilization may be considered, but this remains highly controversial due to the inherent instability in flexion and the difficulty in maintaining reduction. Close monitoring for loss of reduction is critical, and many surgeons would favor operative intervention for Type IIA.
- Patients with severe comorbidities: In patients who are medically unstable or have a very limited life expectancy, non-operative management might be the only feasible option, even for unstable fracture types, with a focus on comfort and palliation.
Operative Indications
-
Levine and Edwards Type II, Type IIA, and Type III Fractures:
These are inherently unstable injuries requiring surgical stabilization once the patient is medically optimized.
- Type II: Significant angulation (>10-15 degrees) or translation (>3 mm) indicates C2-C3 disc and ligamentous disruption. Surgical stabilization after reduction is usually required.
- Type IIA: While translation may be minimal, the severe angulation and significant ligamentous disruption make this type highly unstable in flexion. It is often irreducible with traction and frequently requires operative stabilization.
- Type III: These are the most unstable injuries with C2-C3 facet dislocation and high neurological risk. Urgent reduction and surgical stabilization are indicated.
- Progressive Neurological Deficit: Any new or worsening neurological deficit mandates emergent surgical decompression and stabilization.
- Irreducible Displacement or Dislocation: If closed reduction via traction is unsuccessful or impossible, surgical intervention is required to achieve anatomical alignment and stability. This is particularly true for locked facets in Type III injuries.
- Failed Non-Operative Treatment: Loss of reduction or persistent instability despite appropriate external immobilization (e.g., halo vest) necessitates surgical stabilization.
- Patient Intolerance to Bracing: Patients who cannot tolerate prolonged halo vest immobilization due to discomfort, skin breakdown, or pulmonary compromise may be candidates for earlier surgical intervention.
- Associated Unstable Cervical Spine Fractures: Concomitant unstable fractures elsewhere in the cervical spine often dictate a surgical approach that can address both pathologies.
- Vertebral Artery Injury with Instability: While not a direct indication for surgery, if vertebral artery injury is present alongside an unstable Hangman's fracture, surgical stabilization may be prioritized to prevent further vascular insult and promote fusion.
Contraindications
Absolute contraindications for operative intervention are rare and generally relate to the patient's overall medical status rather than the fracture itself.
*
Severe Medical Comorbidities:
Patients with uncorrectable coagulopathies, severe cardiac or pulmonary compromise, or overwhelming sepsis may be too high-risk for elective or even urgent surgical intervention. In such cases, non-operative management with maximal support is pursued.
*
Local Infection:
Active infection at the surgical site is a contraindication to immediate instrumentation and fusion.
*
Severe Osteoporosis:
While not a strict contraindication, severe osteoporosis can compromise screw purchase and lead to hardware failure, requiring careful consideration of fixation techniques and potentially extended fusion segments.
*
Stable Fracture in a Reliable Patient:
For true Type I fractures, non-operative management is the standard of care.
Operative vs. Non-Operative Indications Summary
| Feature | Non-Operative Indications | Operative Indications |
|---|---|---|
| Fracture Type | Levine & Edwards Type I | Levine & Edwards Type II, IIA, III |
| Translation | < 3 mm (Type I) | > 3 mm (Type II, III) |
| Angulation | < 10 degrees (Type I) | > 10-15 degrees (Type II, IIA) |
| C2-C3 Disc Integrity | Intact | Disrupted (Type II, IIA, III) |
| Ligamentous Integrity | Intact or minimally disrupted | Disrupted (ALL, PLL, or both) |
| Neurological Status | Intact, no progression | Progressive deficit, new deficit |
| Reducibility | Easily reducible and maintainable with external bracing | Irreducible by closed means, locked facets (Type III) |
| Failure of Bracing | N/A | Loss of reduction in halo, patient intolerance to halo |
| Associated Injuries | None requiring surgical intervention | Concomitant unstable cervical fractures |
| Patient Factors | Medically stable, reliable for bracing | Medically optimized for surgery, unreliable for bracing |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial to optimize outcomes and minimize complications in Hangman's fracture management.
Pre-Operative Planning
-
Comprehensive Imaging Review:
- Plain Radiographs: AP, lateral, and open-mouth odontoid views are initial screening tools. Lateral views are critical for assessing C2-C3 angulation and translation.
- Computed Tomography (CT) Scan: Thin-cut axial CT with sagittal and coronal reconstructions is indispensable. It provides detailed bony anatomy, delineates fracture lines, assesses comminution, and quantifies displacement. 3D reconstructions are invaluable for visualizing fracture morphology, C2 pedicle/pars integrity, and planning screw trajectories.
- CT Angiography (CTA) or Magnetic Resonance Angiography (MRA): Essential in cases of significant C2 displacement, Type IA fractures, or any suspicion of vertebral artery injury. The vertebral arteries traverse the foramen transversarium of C2, making them vulnerable to direct trauma, dissection, or occlusion. Bilateral studies are required.
- Magnetic Resonance Imaging (MRI): Indicated for assessing soft tissue injuries, including the C2-C3 intervertebral disc, anterior and posterior longitudinal ligaments, ligamentum flavum, and the integrity of the spinal cord. It helps differentiate between Type II and IIA based on ALL/PLL disruption patterns and identifies any epidural hematoma or spinal cord edema/contusion.
-
Neurological Assessment: A thorough baseline neurological examination is mandatory. Intraoperative neurophysiological monitoring (IONM) with somatosensory evoked potentials (SSEPs) and motor evoked potentials (MEPs) is strongly recommended for all surgical cases to monitor spinal cord integrity during reduction maneuvers and instrumentation.
-
Anesthesia Considerations: Airway management is paramount. Awake fiberoptic intubation is often the safest approach, especially in patients with significant instability, to avoid inadvertent extension or flexion that could compromise the spinal cord. The anesthesia team should be prepared for potential massive blood loss, particularly with anterior approaches or if major vessel injury is encountered.
-
Surgical Approach Selection: The choice between anterior, posterior, or combined approaches depends on the fracture type, reducibility, and desired fusion length.
- Posterior Approach: Generally preferred for Type II, IIA, and III fractures, especially if reduction can be achieved or if C2 pedicle/pars/lamina fixation is planned. It allows for direct reduction, decompression if needed, and robust posterior instrumentation.
- Anterior Approach: Primarily considered for Type II and IIA fractures requiring C2-C3 discectomy and fusion, particularly if there is significant anterior column instability or a need for direct C2-C3 disc space restoration. It is often combined with posterior fixation for maximal stability.
- Combined Approach: May be necessary for highly unstable Type III fractures, failed anterior or posterior attempts, or significant multi-column injuries.
Patient Positioning
Patient positioning must be meticulously performed to maintain cervical alignment and prevent further neurological injury.
- Traction: Gardner-Wells tongs are often applied pre-operatively with axial traction (typically 5-10 lbs initially, increasing cautiously under fluoroscopic guidance) to achieve or maintain reduction. This is especially important during turning.
-
Prone Position (for Posterior Approach):
- The patient is carefully log-rolled from the stretcher to the operating table while maintaining axial traction and cervical spine immobilization (e.g., with tongs or a rigid collar).
- The head is secured in a Mayfield skull clamp or a similar head-holding device, allowing for intraoperative adjustability for reduction maneuvers and fluoroscopic access. Ensure the head is free-floating to permit appropriate positioning for surgical access and imaging.
- Padding is applied generously at all pressure points (cheeks, eyes, shoulders, iliac crests, knees, ankles) to prevent nerve palsies or skin breakdown.
- A chest roll or frame (e.g., Jackson table) is used to support the chest and pelvis, allowing the abdomen to hang free. This reduces intra-abdominal pressure, minimizing epidural venous bleeding.
- The neck is gently positioned in a neutral or slightly flexed/extended position, depending on the fracture reduction requirements. Lateral fluoroscopy is used throughout positioning to confirm alignment.
- Arms are tucked at the sides or outstretched on arm boards, ensuring no brachial plexus compression.
-
Supine Position (for Anterior Approach):
- Patient is positioned supine, usually with a small shoulder roll to facilitate neck extension and expose the anterior neck.
- The head is placed on a padded head ring or held securely with tape. Gardner-Wells tongs may still be used for gentle traction if needed for reduction.
- Arms are tucked at the sides.
- Fluoroscopy access to the C2-C3 region must be confirmed.
Throughout positioning, careful attention must be paid to maintaining a stable cervical spine, minimizing movement, and continuously monitoring neurophysiological signals if IONM is active.
Detailed Surgical Approach / Technique
The surgical management of Hangman's fractures primarily focuses on achieving stable reduction and fusion. The choice of approach (anterior, posterior, or combined) is dictated by fracture morphology, associated ligamentous injury, reducibility, and surgeon preference.
Anterior C2-C3 Discectomy and Fusion
This approach is less common for isolated Hangman's fractures but may be necessary for Type II or IIA fractures with significant C2-C3 disc disruption and persistent anterior angulation or translation, especially when a primary C2-C3 fusion is indicated. It can provide direct decompression of the neural elements anteriorly and robust anterior column support.
-
Incision and Dissection:
- A transverse skin incision at the C2-C3 level or a longitudinal incision along the anterior border of the sternocleidomastoid (SCM) muscle is made, typically on the right side to avoid the recurrent laryngeal nerve.
- The platysma muscle is incised, and subplatysmal flaps are raised.
- The deep cervical fascia is incised anterior to the SCM.
- The dissection proceeds between the carotid sheath (laterally) and the strap muscles, trachea, and esophagus (medially). The omohyoid muscle may need to be retracted or divided.
- The prevertebral fascia is identified and incised to expose the anterior aspect of the C2 and C3 vertebral bodies and the C2-C3 disc space.
- Fluoroscopy is used to confirm the correct level.
-
Reduction:
- Gentle axial traction through Gardner-Wells tongs, possibly combined with careful intraoperative manipulation (e.g., leverage with a Cobb elevator), is used to reduce the C2 spondylolisthesis.
- Once reduced, slight extension or flexion may be required to maintain alignment.
-
Discectomy and Decompression:
- A complete C2-C3 discectomy is performed under microscopic or loupe magnification. This involves removing the annulus fibrosus, nucleus pulposus, and any osteophytes.
- Care is taken to preserve the posterior longitudinal ligament unless direct decompression is required. If neural compression exists from posterior osteophytes or disc material, a posterior longitudinal ligamentotomy and decompression may be performed.
-
Fusion and Fixation:
- The C2 and C3 endplates are prepared by decortication.
- A structural interbody graft (e.g., autologous tricortical iliac crest, allograft, or PEEK cage filled with bone graft) is inserted into the disc space to restore height and lordosis.
- An anterior cervical plate is applied spanning C2 and C3.
- Screw Placement: Two screws are typically placed into the C2 vertebral body and two into the C3 vertebral body. Angulation and depth must be carefully controlled to avoid vertebral artery, esophageal, or spinal canal violation. For C2, screws should be directed slightly medially and superiorly to engage the dens and strong bone in the C2 body.
- Final fluoroscopic images confirm hardware placement and alignment.

Posterior C2-C3 or C1-C3 Fusion
The posterior approach is the workhorse for most unstable Hangman's fractures (Type II, IIA, and III) as it allows for strong posterior fixation, excellent reduction maneuvers, and access to the posterior elements for fusion.
-
Incision and Dissection:
- A midline longitudinal incision is made from the occiput to C4/C5, depending on the planned fusion length.
- The subcutaneous tissue is incised, and the nuchal ligament is sharply divided in the midline.
- A subperiosteal dissection is performed bilaterally, carefully elevating the paraspinal muscles (semispinalis cervicis, multifidus, and rotatores) from the spinous processes, laminae, and lateral masses of C1 to C3/C4.
- Care is taken to minimize muscle stripping to preserve vascularity. The C2-C3 facet capsules are exposed.
-
Identification of Anatomy and Reduction:
- The C1 posterior arch, C2 spinous process, and C3 spinous process are key landmarks. Lateral fluoroscopy helps confirm levels.
- The C2 nerve root exits inferior to the C1 posterior arch and superior to the C2 pedicle/lamina, supplying sensation to the posterior scalp (greater occipital nerve). It is at risk during screw placement.
- The vertebral artery exits the C2 transverse foramen, traversing laterally to the C2 pars/pedicle region, and enters C1 through its transverse foramen. Extreme caution is needed.
- Reduction: Gentle axial traction (Gardner-Wells) is maintained. Intraoperative reduction can be achieved by applying posterior pressure on the C2 spinous process, slight extension, or using specialized reduction instrumentation. For locked facets (Type III), gentle distraction, flexion, and then extension with posterior manipulation may be required.
-
Fixation Options:
The goal is rigid internal fixation to stabilize the C2-C3 segment and promote fusion. Instrumentation often involves pedicle or pars screws.-
C2 Pedicle Screws: These provide the strongest fixation in C2, engaging all three columns.
- Technique: The entry point is typically at the intersection of the midpoint of the C2 lateral mass and the midpoint of the superior border of the C2 lamina, or just medial to the C2-C3 facet joint. The trajectory is medial (15-30 degrees) and slightly rostral (15-20 degrees). Meticulous technique with blunt probing, fluoroscopic guidance (AP and lateral), and neuromonitoring is essential due to the proximity of the vertebral artery and spinal cord. A drill guide can be used.
- Considerations: Fracture patterns that extend into the pedicle or significant comminution may preclude pedicle screw placement.
-
C2 Pars Interarticularis Screws: Provide good fixation but are biomechanically inferior to pedicle screws.
- Technique: Entry point typically at the inferomedial aspect of the C2 superior articular facet. Trajectory is directed anteriorly and medially, aiming towards the C2 body. Similar risks to pedicle screws.
-
C2 Laminar Screws (Magerl Technique): A valuable alternative, particularly in Type IIA fractures (where pars is intact but highly unstable in flexion) or when pedicle screws are contraindicated (e.g., fracture extension, malformation).
- Technique: A small laminotomy is performed at the caudal aspect of the C2 lamina. The screw is inserted at the C2 spinous process base, aiming through the lamina into the C2 body. Two laminar screws (criss-crossing or parallel) provide robust fixation. Careful measurement and trajectory are crucial to avoid spinal canal violation.
-
C3 Lateral Mass Screws: The standard fixation point for C3.
- Technique: Entry point typically 1 mm medial to the midpoint of the lateral mass, directed 10-20 degrees laterally and 30-45 degrees superiorly to avoid the vertebral artery and C3 nerve root.
-
C1-C2 Fixation (Harms or Goel-Harms Construct): In cases where the C2 fracture extends proximally, or C2 pedicle fixation is inadequate, fusion of C1 to C2 might be necessary.
- Technique: C1 lateral mass screws are inserted, and C2 pedicle/pars screws are used. Rods connect C1 lateral masses to C2 pedicles. This provides strong fixation but sacrifices C1-C2 rotation.
-
Rods and Connectors: After screw insertion, appropriately contoured rods are placed and secured. Cross-links may be used to enhance construct rigidity.
-
-
Bone Grafting:
- Decortication of the C2 and C3 laminae and lateral masses is performed.
- Autologous bone graft (e.g., local bone from spinous processes, iliac crest) or allograft is placed over the decorticated surfaces to promote arthrodesis.
- For C2-C3 facet fusion, the C2-C3 facet capsules are denuded, and cancellous bone graft is packed into the joints.
-
Wound Closure:
- The wound is irrigated thoroughly.
- A drain may be placed.
- Muscles are reapproximated in layers, followed by fascial, subcutaneous, and skin closure.

Complications & Management
Despite advancements in surgical techniques, the management of Hangman's fractures is associated with a range of potential complications, some of which can be severe. Proactive recognition and appropriate management are critical for optimizing patient outcomes.
| Complication | Incidence (%) | Salvage / Management Strategies |
|---|---|---|
| Neurological Injury | Low (Type I, II); High (Type III); <5% post-op iatrogenic | New Deficit: Immediate post-op imaging (CT/MRI) to rule out hematoma, cord compression, or malpositioned hardware. Surgical revision for decompression or hardware adjustment. Steroids if indicated. Worsening Deficit: Same as new deficit. C2 Nerve Root Palsy: Typically sensory, often resolves. Surgical decompression if motor. |
| Vertebral Artery Injury (VAI) | ~1-5% (iatrogenic); Higher with Type IA, III, significant displacement | Pre-op: Meticulous vascular imaging (CTA/MRA). Intra-op: Direct pressure, packing, angiographic embolization. Anticoagulation if dissection/thrombosis. Close neurological monitoring for stroke. |
| Infection | Superficial: 2-5%; Deep: <1-2% | Superficial: Oral antibiotics, wound care. Deep: Surgical debridement, IV antibiotics, wound vac. May require hardware removal in chronic cases, but usually after fusion achieved. |
| Pseudarthrosis / Nonunion | 5-15% (C2-C3 fusion); Higher with poor bone quality, smoking, inadequate fixation | Asymptomatic: Monitor. Symptomatic/Progressive Deformity: Revision surgery with further decortication, stronger instrumentation, interbody grafting, and potentially biologics (e.g., BMP). May require longer fusion segments. |
| Hardware Failure | 2-10% (screw pullout, breakage, prominent hardware) | Screw Malposition: Immediate revision. Pullout/Breakage: Revision surgery, stronger fixation (e.g., C1-C3 fusion), alternative screw trajectories (laminar). Prominent Hardware: May require removal after fusion, or revision if symptomatic before fusion. |
| Dysphagia / Dysphonia | Transient (anterior approach): 10-30%; Permanent: <1% | Transient: Soft diet, speech therapy. Permanent: Refer to ENT/speech pathology. May be due to recurrent laryngeal nerve injury (dysphonia) or esophageal injury/swelling (dysphagia). |
| Hemorrhage / Hematoma | <5% | Meticulous hemostasis intra-operatively. Post-operative drain. Urgent surgical evacuation for expanding hematoma causing airway compromise or neurological deficit. |
| Airway Compromise | <1% (usually post-op hematoma/edema, anterior approach) | Close observation in PACU/ICU. Urgent intubation, tracheostomy in extreme cases. Immediate surgical evacuation of hematoma. |
| Spinal Deformity / Kyphosis | <5% | Careful intraoperative reduction and maintenance of lordosis. Revision surgery for significant post-fusion kyphosis or progressive deformity. |
Specific Management Considerations:
- Neurological Deterioration: Any post-operative neurological change mandates immediate clinical reassessment, stat imaging (CT to rule out hardware malposition or hematoma; MRI for cord edema/contusion), and readiness for surgical exploration and revision.
- Vertebral Artery Injury (VAI): Pre-operative CTA/MRA is essential to identify pre-existing VAI or anatomical variants. Intraoperatively, VAI can manifest as pulsatile bleeding. Immediate direct pressure, packing, and consultation with vascular surgery or interventional radiology for angiography and embolization are critical. Post-operatively, antiplatelet or anticoagulation therapy may be considered depending on the extent and type of injury (dissection vs. occlusion) and the risk of stroke.
- Pseudarthrosis: This complication is higher in patients with poor bone quality, smokers, and those with inadequate initial fixation. Nonunion can lead to persistent pain, instability, and hardware failure. Management typically involves revision surgery with further decortication, robust bone grafting (autograft preferred), potentially biologics (e.g., BMP-2 off-label), and often more extensive or stronger instrumentation (e.g., extending fusion to C1 or C4).
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following surgical stabilization of Hangman's fractures aims to protect the surgical construct, facilitate fusion, restore range of motion, and enhance functional recovery. Protocols are tailored based on the stability of the fixation, the extent of fusion, patient factors, and the presence of any neurological deficits.
Phase 1: Acute Post-Operative (Days 0-6 Weeks)
Goals: Protect surgical site, control pain, prevent complications, initiate early mobilization.
-
Immobilization:
- Typically, a rigid cervical collar (e.g., Miami J, Philadelphia collar) is prescribed for 6-12 weeks, depending on the stability of the surgical construct and the surgeon's preference.
- For cases with less rigid constructs, persistent instability concerns, or in non-operative Type I fractures, a halo vest may be used for 8-12 weeks.
- Pain Management: Multimodal analgesia including opioids, NSAIDs/acetaminophen, and muscle relaxants.
- Wound Care: Daily inspection of incision site for signs of infection.
-
Mobilization:
- Out-of-bed activity begins on post-operative day 1, with assistance as needed.
- Log-roll technique for bed mobility.
- Avoidance of cervical spine rotation, flexion, or extension beyond the limits of the brace.
- Neurological Monitoring: Continuous assessment for any new or worsening neurological deficits.
- Deep Vein Thrombosis (DVT) Prophylaxis: Mechanical (SCDs) and/or pharmacological prophylaxis as per institutional protocols.
-
Early Physical Therapy (PT) / Occupational Therapy (OT):
- Focus on functional mobility (transfers, ambulation).
- Instruction on proper brace wear and care.
- Gentle range of motion for extremities.
- Diaphragmatic breathing exercises to optimize pulmonary function.
- Education on activity restrictions (no lifting > 5-10 lbs, no driving).
- Radiographic Follow-up: Initial post-operative radiographs (AP and lateral) to confirm hardware position. Subsequent imaging at 2-4 weeks to assess early healing and maintenance of alignment.
Phase 2: Intermediate (6-12 Weeks Post-Operative)
Goals: Gradual increase in cervical spine motion, initiation of gentle strengthening, radiographic evidence of fusion.
- Immobilization: Weaning from the rigid cervical collar, often to a softer collar or no collar, based on radiographic signs of fusion and clinical stability.
-
Physical Therapy:
- Gentle Cervical Range of Motion (ROM): Active-assisted or active ROM exercises are initiated, avoiding pain or end-range forces. Focus on flexion, extension, lateral bending, and rotation, within tolerance.
- Isometrics: Gentle isometric strengthening of cervical musculature, gradually increasing intensity.
- Scapular Stabilization: Exercises for periscapular muscles to improve posture and reduce compensatory neck strain.
- Core Strengthening: Lumbar and abdominal core stability exercises to indirectly support cervical posture.
- Activity Restrictions: Continue to avoid heavy lifting, strenuous activities, and high-impact sports. No driving until cleared by the surgeon and physical therapist.
- Radiographic Follow-up: Repeat radiographs (AP, lateral, flexion/extension views if cleared by surgeon) at 3 months post-op to assess evidence of fusion. CT scan may be performed if fusion is unclear on plain films.
Phase 3: Advanced Rehabilitation (3-6+ Months Post-Operative)
Goals: Progressive strengthening, restoration of full functional capacity, return to desired activities.
- Cervical Mobility: Progress to full active cervical ROM.
-
Strengthening:
- Progressive resistive exercises for cervical extensors, flexors, and rotators.
- Focus on endurance and functional strength.
- Incorporate proprioceptive and balance exercises.
-
Functional Training:
- Return to activities of daily living (ADLs) and work-related tasks.
- Sport-specific training and gradual return to recreational activities as tolerated and approved by the surgeon. Contact sports are generally discouraged after cervical fusion.
- Education: Emphasis on proper body mechanics, posture, and strategies for protecting the cervical spine during activities.
- Radiographic Follow-up: Final radiographic assessment of fusion typically at 6-12 months post-op.
Throughout all phases, patient education regarding expected recovery, limitations, and adherence to activity restrictions is paramount for successful outcomes. Smoking cessation is strongly encouraged as it significantly impairs bone healing and increases pseudarthrosis rates.
Summary of Key Literature / Guidelines
The management of traumatic spondylolisthesis of C2 has evolved significantly, with key literature establishing classification systems and guiding treatment algorithms.
The foundational work by Effendi et al. (1976) initially characterized the fracture patterns and proposed a classification system based on displacement. This was subsequently refined by Levine and Edwards (1985) into the widely adopted four-type system (Type I, II, IIA, III) that correlates fracture morphology with mechanism, stability, and prognosis. This classification remains the cornerstone for surgical decision-making.
Early treatment of Hangman's fractures, particularly Type I and Type II, heavily relied on halo vest immobilization . Studies from the 1980s and 1990s, such as those by Aebi et al. (1986) and Kim et al. (1995) , demonstrated high fusion rates (80-90%) with halo vests for Type I and II fractures. However, halo vest complications, including pin site infections, skin breakdown, neurovascular compromise, and patient intolerance, were significant. For Type IIA fractures, the literature highlights challenges with halo immobilization due to the inherent instability in flexion and difficulty maintaining reduction, often leading to nonunion or kyphosis, thereby shifting the preference towards surgical intervention for these specific cases.
The shift towards surgical stabilization for unstable Hangman's fractures gained momentum with advancements in spinal instrumentation. Judas et al. (1988) provided early insights into the biomechanics and the rationale for surgical stabilization. The development and refinement of posterior cervical screw techniques, particularly C2 pedicle screws (originally described for other C2 pathologies), and C2 laminar screws (Magerl technique) , have provided robust alternatives to halo vests for Type II, IIA, and III fractures. Studies by Harkey et al. (2000) and Yeom et al. (2008) demonstrated excellent fusion rates and favorable outcomes with posterior C2 pedicle or laminar screw fixation for unstable Hangman's fractures.
Anterior C2-C3 discectomy and fusion with plating, though less common as a primary approach for isolated Hangman's fractures, has also been successfully employed, particularly for fractures with significant C2-C3 disc disruption and persistent kyphotic deformity. However, anterior approaches alone may not always provide adequate stability in highly unstable posterior element injuries and are often supplemented with posterior fixation (a combined approach).
Controversies
persist regarding the optimal management of certain types:
*
Type IIA Fractures:
While often managed surgically due to their instability, some authors advocate for halo vest immobilization if a perfect reduction can be achieved and maintained. However, the high rate of kyphosis and loss of reduction in flexion makes surgical intervention often preferred.
*
Elderly Patients:
The management of Hangman's fractures in elderly patients, often with osteoporotic bone, poses unique challenges. Non-operative management carries risks of prolonged immobilization and complications, while surgical fixation may be complicated by poor bone quality. Careful risk-benefit analysis is essential.
*
Fusion Length:
The extent of fusion (C1-C2, C2-C3, or C1-C3) depends on the exact fracture pattern, stability, and integrity of adjacent segments. While C2-C3 fusion is the goal for most Hangman's, C1-C2 fusion may be required if C1 is involved or C2 fixation points are compromised, though this sacrifices atlantoaxial rotation.
Current Guidelines and Consensus:
Current consensus generally favors non-operative management with a rigid orthosis (halo vest or rigid cervical collar) for stable Type I fractures. For unstable Type II, IIA, and Type III fractures, surgical stabilization is the preferred approach, often via a posterior technique utilizing C2 pedicle, pars, or laminar screws connected to C3 lateral mass screws, followed by posterolateral fusion. The choice between anterior, posterior, or combined approaches is individualized based on specific fracture characteristics, patient factors, and surgeon expertise, always aiming for anatomical reduction, solid arthrodesis, and minimal neurological risk. Detailed pre-operative planning, including CT angiography for vertebral artery assessment, is critical for all operative cases.
Clinical & Radiographic Imaging