INTRODUCTION AND BIOMECHANICS
Fractures of the tibial shaft represent the most commonly encountered long bone fractures in orthopaedic traumatology. Due to its anatomical location and lack of robust anterior soft tissue coverage, the tibia is highly susceptible to both low-energy torsional forces and high-energy direct impacts. The management of these fractures cannot be distilled into a simple, universal set of rules; rather, it requires a nuanced understanding of bone biomechanics, soft tissue envelopes, and fracture morphology.
The tibia's unique anatomy dictates its vulnerability and healing potential. Approximately one-third of the tibial surface—specifically the anteromedial face—is subcutaneous throughout its entire length. Consequently, open fractures are more common in the tibia than in any other major long bone. Furthermore, the blood supply to the tibial diaphysis is notoriously precarious compared to bones enveloped by heavy musculature (e.g., the femur). The endosteal blood supply, provided by the nutrient artery, is frequently disrupted in displaced transverse or short oblique fractures, leaving the bone reliant on a tenuous periosteal network.
CLINICAL PEARL: The presence of hinge joints at the knee and the ankle allows for absolutely no compensatory adjustment for rotary deformity after a fracture. Special care is mandatory during reduction to correct any rotational malalignment, as failure to do so will alter the loading characteristics of adjacent joints and accelerate posttraumatic arthrosis.
High-energy tibial fractures are frequently associated with severe complications, including compartment syndrome, neural compromise, and vascular injury. Delayed union, nonunion, and deep infection remain relatively common, particularly in the setting of severe soft tissue compromise.
CLINICAL EVALUATION AND INITIAL MANAGEMENT
The evaluation of a patient with a tibial shaft fracture must begin with Advanced Trauma Life Support (ATLS) protocols, followed by a detailed history and physical examination of the injured extremity.
Physical Examination
The limb must be meticulously inspected for open wounds, soft tissue crush injuries, degloving (Morel-Lavallée lesions), and severe contusions. A thorough neurovascular examination is paramount.
SURGICAL WARNING: A pulse deficit or a neurological deficit (such as decreased sensation in the first web space or weakness in extensor hallucis longus) may be an early sign of compartment syndrome or a major vascular injury. These conditions must be identified and treated emergently with four-compartment fasciotomies or vascular shunting/repair.
The ipsilateral femur, knee, ankle, and foot must also be examined to rule out floating knee injuries or concomitant articular fractures. Once the initial examination is complete, the limb should be gently realigned and placed in a well-padded splint to minimize further soft tissue trauma.
Open Fracture Protocol
If open wounds are present, they must be managed aggressively in the emergency department:
* Wounds are irrigated gently with sterile saline.
* Gross contamination is removed.
* The wound is covered with a sterile, saline-soaked dressing.
* Appropriate tetanus prophylaxis is administered.
* Intravenous antibiotics are initiated immediately (e.g., a first-generation cephalosporin for Gustilo-Anderson Type I and II; addition of an aminoglycoside for Type III; addition of high-dose penicillin for severe agricultural or crush contamination).
Radiographic Evaluation
Standard imaging includes plain anteroposterior (AP) and lateral radiographs orthogonal to the tibial shaft, ensuring that both the knee and ankle joints are fully visualized.
* Oblique Views: Radiographs at 45 degrees are sometimes required to detect nondisplaced spiral fractures or to better delineate butterfly fragments.
* Contralateral Views: Radiographs of the uninjured, contralateral tibia are frequently necessary to evaluate native length and alignment, particularly in fractures with severe comminution or segmental bone loss.
* Cross-Table Views: Useful in the trauma bay for patients who cannot be easily positioned.
PROGNOSTIC FACTORS AND ACCEPTABLE ALIGNMENT
The prognosis of a tibial shaft fracture is heavily influenced by the energy of the injury and the resulting fracture morphology. Hoaglund and States classified tibial fractures based on energy mechanisms, which remains highly relevant for predicting union times:
* High-Energy Trauma: Motor vehicle collisions, crush injuries, and high-velocity gunshot wounds. These account for the majority of total fractures and 90% of open fractures. Average healing time is approximately 6 months.
* Low-Energy Trauma: Falls from standing height, twisting injuries (e.g., skiing). These typically heal in an average of 4 months.
Fracture Morphology and Healing
Torsional (spiral) fractures, with or without simple comminution, generally carry a better prognosis than high-energy short oblique or transverse fractures. Torsional forces tend to create a longitudinal tear in the periosteum, often sparing the endosteal vessels. Conversely, transverse fractures usually tear the periosteum circumferentially and completely disrupt the endosteal circulation.
The amount of cortical contact is a critical prognosticator. Fractures maintaining 50% to 90% cortical contact heal significantly faster than those with less contact. Initial displacement exceeding 50% of the tibial width is a known risk factor for delayed union or nonunion.
Parameters for Acceptable Alignment
The limits of acceptable malalignment remain a topic of debate, though distal tibial malalignment is generally more poorly tolerated than proximal malalignment due to its direct effect on ankle joint biomechanics (as demonstrated by Tarr et al. and Puno et al.).
We adhere to Trafton’s stringent recommendations for acceptable reduction:
* Varus/Valgus Angulation: Less than 5 degrees.
* Anteroposterior Angulation (Procurvatum/Recurvatum): Less than 10 degrees.
* Rotation: Less than 10 degrees.
* Shortening: Less than 15 mm.
If repeated attempts at closed reduction fail to achieve these parameters, operative fixation is strictly indicated.
NONOPERATIVE MANAGEMENT
While historically common, nonoperative treatment is now generally reserved for closed, stable, isolated, minimally displaced fractures caused by low-energy trauma, as well as select stable low-velocity gunshot fractures.
Sarmiento, Nicoll, and others pioneered the use of functional bracing, demonstrating that closed treatment can be highly effective while avoiding surgical complications. For closed treatment to succeed:
1. The cast or brace must maintain acceptable fracture alignment.
2. The fracture pattern must possess inherent axial stability to allow for early weight-bearing, which stimulates osteogenesis and prevents nonunion.
3. The patient must be compliant and possess a body habitus that allows for effective brace molding (extreme obesity or severe edema precludes effective bracing).
Repeated attempts at closed manipulation should be avoided to prevent further soft tissue stripping. If alignment is lost, surgical intervention should be pursued.
OPERATIVE MANAGEMENT: INDICATIONS AND MODALITIES
Operative treatment is indicated for the vast majority of tibial fractures caused by high-energy trauma. These fractures are typically unstable, comminuted, and associated with significant soft tissue injury. Surgery allows for early mobilization, provides access for soft tissue management, and mitigates the systemic complications of prolonged immobilization.
The primary goals of operative treatment are:
1. A healed, well-aligned fracture.
2. Pain-free weight-bearing.
3. Functional range of motion of the knee and ankle joints.
Management of Open Tibial Fractures
Soft tissue management is the single most critical factor determining the outcome of open tibial fractures. Aggressive, meticulous, and repeated surgical débridements of all devitalized tissue—including muscle, fascia, and avascular bone fragments—are essential.
CLINICAL PEARL: Gustilo emphasized the importance of leaving open fracture wounds open initially. Our protocol mandates a repeat débridement and irrigation at 48 to 72 hours if there is any evidence of continuing demarcation of the zone of injury. All Gustilo Type III fractures undergo mandatory planned repeat débridements.
Soft tissue coverage (via delayed primary closure, split-thickness skin grafting, or local/free flaps) should ideally be achieved within 5 to 7 days to minimize nosocomial infection rates.
Intramedullary Nailing
For Gustilo Type I, Type II, and Type IIIA open fractures, as well as the majority of unstable closed fractures, locked intramedullary (IM) nailing is the gold standard. IM nailing provides load-sharing biomechanics, preserves the extraosseous blood supply, and allows for early weight-bearing.
- Reamed vs. Unreamed: Studies comparing reamed versus unreamed nailing have demonstrated a reduced risk of reoperation and higher union rates with the reamed technique, even in open fractures, provided the soft tissue envelope is adequately managed.
- Type IIIB and IIIC Fractures: The use of IM nails in Type IIIB fractures remains debated due to higher infection rates, though many traumatologists still prefer unreamed nails combined with immediate flap coverage. Type IIIC fractures, war injuries, and fractures with severe medullary contamination are generally better served with external fixation.
Complex Distal Extensions and Arthrodesis
In cases of severe distal tibial comminution (AO Type C pilon fractures) extending into the diaphysis, or in patients with preexisting severe posttraumatic arthrosis of the ankle and hindfoot, primary arthrodesis may be indicated as a salvage or definitive procedure.
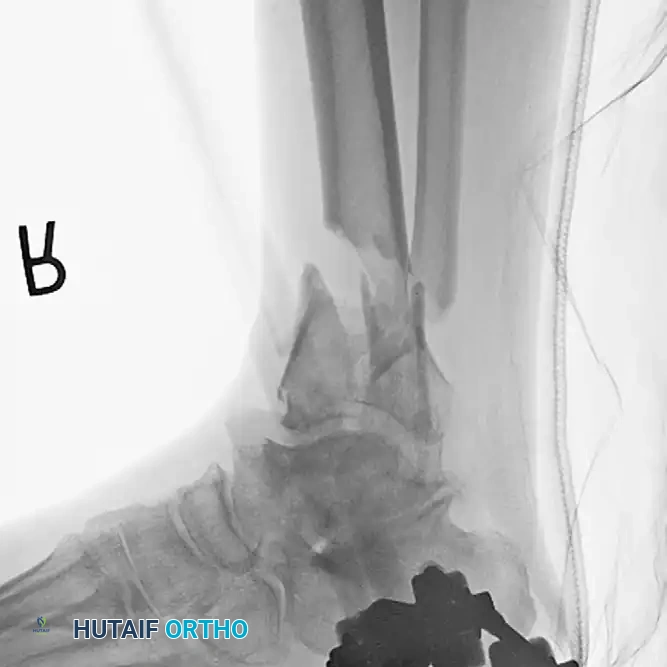
Preoperative radiograph demonstrating a highly comminuted fracture of the tibial pilon following a fall from a height. Note the preexisting posttraumatic arthritis of the tibiotalar and subtalar articulations secondary to a previous talar fracture.
In such complex scenarios, a primary tibiotalocalcaneal (TTC) arthrodesis utilizing a retrograde intramedullary nail provides rigid stabilization of the fracture while simultaneously addressing the arthritic joints, allowing for early mobilization.
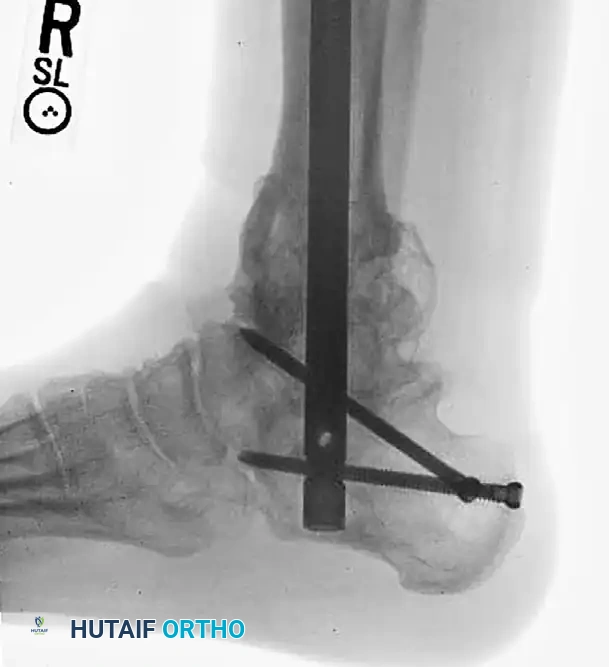
Postoperative radiograph demonstrating definitive management with a primary tibiotalocalcaneal arthrodesis using a retrograde intramedullary implant. This construct bypasses the comminution and provides rigid distal fixation.
SURGICAL TECHNIQUE: CIRCULAR EXTERNAL FIXATION (ILIZAROV METHOD)
For highly comminuted fractures, severe open injuries (Type IIIB/IIIC), or fractures with extensive bone loss, circular ring fixation provides unparalleled versatility. It allows for mechanical axis restoration, bone transport, and soft tissue access without further devascularizing the fracture site.
Step-by-Step Frame Application
- Fibula Reduction and Transfixation: If the fibula is fractured and has not been plated, ensure it is pulled out to its full length and that appropriate rotation is maintained. Reduce the diastasis by passing a transfixation wire from the fibula across the tibia.
- Distal Reference Wire: Place the final transverse reference wire just anterior to the fibula. Pass this wire only through the tibia to ensure it is perfectly parallel to the ankle joint, approximately 1 cm proximal to the joint line.
- Ring Placement: "Clamshell" the distal ring (assemble two half-rings) and place it around the leg, positioning the ring exactly on the reference wire. This guarantees that the knee and ankle joints will remain parallel when the distal and proximal rings are eventually connected.
- Wire Fixation and Build-Ups: Attach the remainder of the wires to the free ring. Because the wires may not lie directly in apposition to the ring surface, build up to the ring using various posts and washers of different heights to prevent wire bending and loss of tension.
- Tensioning: Tension the opposing olive wires symmetrically using two-wire tensioners.
> SURGICAL WARNING: Perform all tensioning under strict fluoroscopic control to prevent asymmetrical compression, which can inadvertently displace the fracture lines. - Connecting the Construct: Attach the distal ring to the proximal rings using threaded rods equipped with conical washers. This allows for multi-planar variability in reducing and maintaining the overall mechanical axis.
- Managing Shaft Comminution: Use an intermediate ring at the level of the proximal shaft extension to reduce comminution. Utilize olive or smooth wires to manipulate and maintain shaft alignment, pulling large butterfly fragments into place. Attach these wires to the mid-distal ring and tension them under fluoroscopy.
Distraction Ligamentotaxis for AO Type C Injuries
For severe injuries with extensive joint involvement and large areas of metaphyseal comminution, preconstructing a four-ring frame with an attached foot frame is highly advantageous.
* Construct Assembly: The distraction construct can range from a simple calcaneal pin attached to a distal half-ring, to a comprehensive foot frame attached to the distal tibial ring.
* Application: Attach the proximal tibial rings first to ensure appropriate soft tissue clearance. Then, attach the foot frame or calcaneal pin.
* Ligamentotaxis: Perform distraction ligamentotaxis across the ankle joint by adjusting the threaded rods. The tension of the intact capsuloligamentous structures will help reduce the articular fragments.
* Open Reduction: If ligamentotaxis reduction is inadequate, a limited open procedure must be performed to anatomically reduce the joint surface.
* Final Fixation: Once reduction is satisfactory, position the distal tibial ring at the level of the fracture. Pass the fixation wires across the fragments, attach them to the ring, and tension them. Because the distal ring is already attached to the frame in this technique, "clamshelling" is not necessary.
POSTOPERATIVE CARE AND REHABILITATION
Postoperative protocols must be tailored to the fracture pattern, the stability of the fixation, and the condition of the soft tissues.
External Fixation and Periarticular Comminution
In fractures with significant periarticular comminution or fragments possessing minimal soft tissue attachment, Watson recommends maintaining distraction across the ankle joint for a full 6 weeks.
* Once tentative healing and early callus formation are observed at the joint line, the foot frame or calcaneal pin is removed in an outpatient setting.
* Aggressive physical therapy is immediately initiated to restore range of motion and general limb strength.
Weight-Bearing Protocols
- Severe Comminution (AO Type C3): Strict non-weight-bearing is maintained initially to prevent construct failure or fracture collapse.
- Shaft Extensions: In fractures with diaphyseal extension, tentative partial weight-bearing is initiated only when early callus and definitive signs of healing are visible on orthogonal radiographs, typically between 8 to 10 weeks.
- Progression: Progressive weight-bearing is advanced based on clinical and radiographic healing. By 12 to 14 weeks, the patient is usually ambulatory with the aid of a single crutch or a cane.
Monitoring for Complications
Patients must be closely monitored for signs of delayed union, nonunion, and infection. In cases of delayed union following IM nailing, dynamization (removal of the static interlocking screws furthest from the fracture) may be performed at 10 to 12 weeks to allow axial compression and stimulate osteogenesis. Pin tract infections in external fixators are common and should be managed aggressively with local pin care and oral antibiotics to prevent deep osteomyelitis.
