INTRODUCTION TO HAND MALIGNANCIES
Primary malignant tumors of the hand are exceedingly rare, representing a small fraction of all musculoskeletal neoplasms. However, their presence poses a profound challenge to the orthopaedic oncologist and hand surgeon. The complex, compact anatomy of the hand—where neurovascular bundles, tendons, and osseous structures are intimately associated with minimal soft-tissue coverage—makes achieving wide oncologic margins difficult without sacrificing significant function.
This comprehensive guide delineates the pathophysiology, clinical presentation, and precise surgical management of the most frequently encountered hand malignancies, including squamous cell carcinoma, various sarcomas, and acro-metastases.
SQUAMOUS CELL CARCINOMA (SCC)
Squamous cell carcinoma is the most prevalent primary malignancy of the hand, accounting for 58% to 90% of all hand malignancies. It frequently exceeds malignant melanoma as the most common malignancy affecting the nail bed.
Epidemiology and Pathophysiology
SCC of the hand typically manifests in individuals in their 50s and exhibits a strong male predominance, occurring four times more frequently in men than in women. The pathogenesis is heavily linked to environmental and occupational exposures.
- Actinic Radiation: SCC has a distinct predilection for sun-exposed areas of the skin (the dorsum of the hand) and is exceptionally uncommon on the volar palm.
- Viral Etiology: High-risk Human Papillomavirus (HPV) strains (particularly HPV 16) are strongly associated with subungual SCC.
- Chronic Inflammation: Marjolin’s ulcers can develop in chronic burn scars, osteomyelitis sinus tracts, or radiation-induced dermatitis.
Clinical Presentation
The clinical appearance of SCC is highly variable. Lesions may initially present as small, desquamating, erythematous plaques (often misdiagnosed as chronic paronychia, verruca vulgaris, or eczema) and can progress to large, fungating, ulcerated masses. Subungual SCC often presents as chronic nail dystrophy, ulceration, or a non-healing periungual mass.
Clinical Pearl: Any chronic, atypical "infection" of the nail bed or paronychia that fails to respond to standard antimicrobial therapy after 4 to 6 weeks mandates a full-thickness tissue biopsy to rule out subungual squamous cell carcinoma.
Surgical Management
The primary goal of surgical intervention is complete tumor extirpation with negative margins, followed by functional reconstruction.
- Wide Local Excision (WLE): For dorsal skin lesions without deep tissue invasion, WLE with 4 to 5 mm margins is standard. Defects are typically reconstructed using full-thickness skin grafts (FTSG) or local rotational flaps.
- Amputation: If the tumor invades the extensor paratenon, joint capsule, or underlying distal phalanx (bone erosion visible on radiographs), amputation is indicated.
- For distal phalangeal involvement, a distal interphalangeal (DIP) joint disarticulation or amputation through the middle phalanx is performed.
- The volar flap should be preserved if oncologically safe to provide durable, sensate coverage over the amputation stump.
- Lymph Node Management: Routine prophylactic axillary or epitrochlear lymph node dissection is not indicated unless clinically palpable adenopathy is present or sentinel lymph node biopsy (SLNB) is positive in high-risk lesions (e.g., >2 cm, deep invasion, poor differentiation).
CHONDROSARCOMA OF THE HAND
While enchondromas are the most common benign bone tumors of the hand, secondary malignant transformation into chondrosarcoma is a recognized, albeit rare, phenomenon.
Clinical and Radiographic Evaluation
Transformation should be suspected when a patient with a known, long-standing enchondroma develops new-onset, progressive pain without antecedent trauma.
Radiographically, benign enchondromas present as well-circumscribed, central lytic lesions with stippled calcifications. Malignant transformation is heralded by endosteal scalloping (exceeding two-thirds of the cortical thickness), cortical breakthrough, soft-tissue extension, and a "fluffy radiopacity."


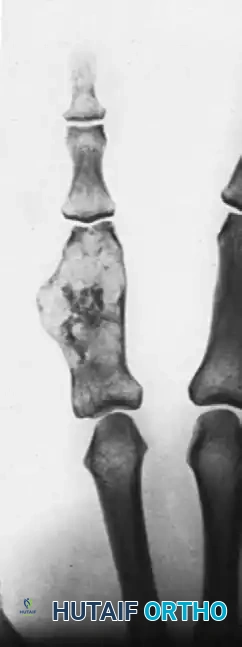
Above: Posteroanterior, lateral, and oblique radiographic views demonstrating a chondrosarcoma arising in a pre-existing enchondroma of 40 years’ duration. Note the greatly expanded proximal phalanx with clearly visible fluffy radiopacity and cortical destruction.
Surgical Approach: Ray Amputation
Due to the cartilaginous nature of the tumor and its resistance to chemotherapy and radiation, aggressive surgical resection is the mainstay of treatment. Intralesional curettage is contraindicated.
- Incision Planning: A racquet-shaped incision is designed around the base of the involved digit, ensuring the biopsy tract is excised en bloc with the specimen.
- Osteotomy: For a proximal phalangeal lesion, a ray amputation (excision of the digit and its corresponding metacarpal) is often required to achieve wide margins. The osteotomy is performed at the proximal metaphyseal-diaphyseal junction of the metacarpal.
- Soft Tissue Reconstruction: The deep transverse metacarpal ligament is reconstructed to prevent splaying of the adjacent digits, and the intrinsic muscles are transferred to optimize grip strength.
EPITHELIAL SARCOMA
Epithelial sarcoma is a rare, high-grade soft tissue sarcoma that frequently affects the distal extremities of young adults. It has a notorious propensity for proximal lymphatic spread and local recurrence.
Presentation and Biomechanics
It often presents as a firm, slow-growing, painless nodule in the deep dermis or subcutaneous tissue, frequently involving the volar aspect of the hand or the web spaces. Because it spreads along fascial planes and tendon sheaths, wide en bloc resection is mandatory.
Surgical Warning: Epithelial sarcoma is frequently misdiagnosed as a benign fibroma, ganglion cyst, or necrotizing granuloma. Inadequate marginal excision ("shelling out") leads to rapid local recurrence and increases the risk of metastasis.
Surgical Technique: Wide Double-Ray Excision
When an epithelial sarcoma involves a web space, a single ray amputation is often insufficient to achieve negative margins. A double-ray excision is indicated.
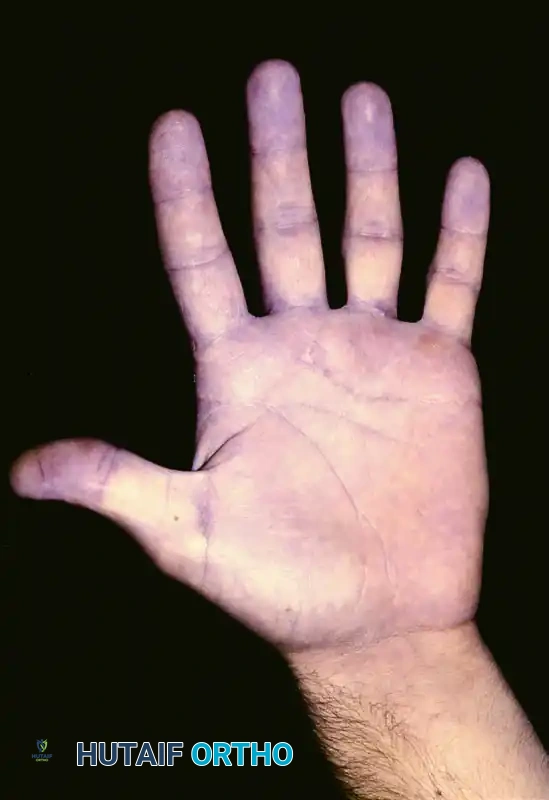
Above: Preoperative clinical presentation of a small epithelial sarcoma involving the distal second web space.
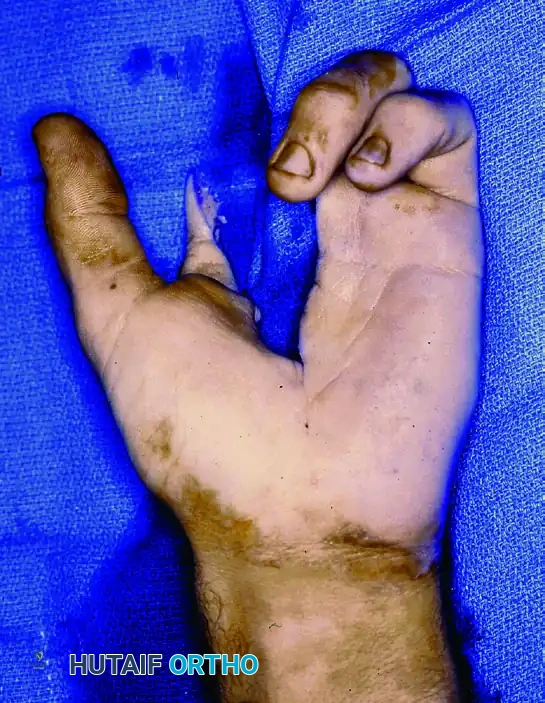
Above: Intraoperative marking and planning for a wide double-ray excision to ensure adequate oncologic margins.
Step-by-Step Approach:
1. Positioning and Tourniquet: The patient is positioned supine with the arm on a hand table. An upper arm tourniquet is applied but not exsanguinated with an Esmarch bandage to prevent proximal tumor embolization; instead, the arm is elevated for 3 minutes prior to inflation.
2. Incision: Dorsal and volar V-shaped incisions are made, encompassing the involved web space and extending proximally over the metacarpals of the involved rays.
3. Neurovascular Dissection: The common digital arteries and nerves supplying the involved rays are identified proximally, ligated, and transected well away from the tumor bed.
4. Bone Resection: The metacarpals of the involved rays are exposed subperiosteally (only outside the tumor zone). Osteotomies are performed at the metacarpal bases using an oscillating saw.
5. Closure and Transposition: If the central rays (e.g., 2nd and 3rd) are removed, the remaining marginal rays may be transposed to close the cleft and improve the biomechanical transverse arch of the hand.
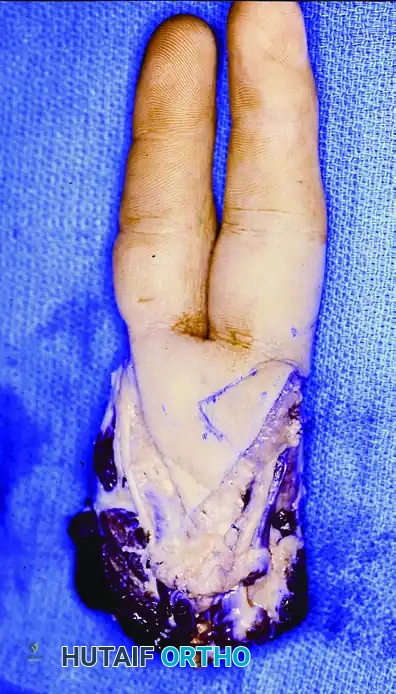
Above: Postoperative volar view demonstrating the healed double-ray excision.
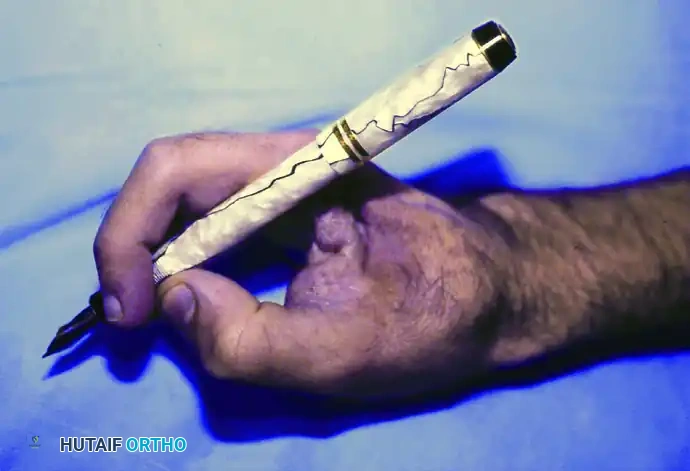
Above: Acceptable functional outcome. The patient retains the ability to perform a modified pinch and grasp, demonstrating the biomechanical viability of the residual hand.
FIBROSARCOMA
Fibrosarcomas are malignant tumors of mesothelial origin characterized by the proliferation of malignant fibroblasts.
Etiology and Presentation
While they can arise de novo, fibrosarcomas have a known association with prior tissue trauma. They can occur years after radiation exposure or arise within the dense scar tissue of severe burn injuries. Congenital and infantile fibrosarcomas can occur in the extremities but are exceedingly rare.
Patients typically present with an enlarging mass on the hand. While often painless, the mass may cause secondary symptoms due to mass effect, such as pressure on peripheral nerves (e.g., median or ulnar nerve compression) leading to paresthesias or motor weakness.
Management
Wide surgical excision or amputation is the definitive treatment. Because fibrosarcomas are relatively radioresistant, achieving R0 (microscopically negative) surgical margins is the most critical prognostic factor for local control.
RHABDOMYOSARCOMA
Rhabdomyosarcoma is a high-grade malignancy of skeletal muscle origin. Three primary histologic subtypes exist: alveolar, embryonal, and pleomorphic.
Clinical Behavior in the Extremity
The alveolar form is the most common subtype encountered in the limbs. Most extremity rhabdomyosarcomas are deeply situated, intimately associated with striated muscle (such as the intrinsic muscles of the hand), and remain painless despite rapid, aggressive growth.
Bone erosion is a common radiographic finding when these tumors affect the hands and feet. Historically, the location of these tumors in the distal extremities accounted for an unfavorable prognosis due to the difficulty of achieving wide margins without amputation.
Multidisciplinary Management
Survival rates have increased significantly with the advent of modern multidisciplinary protocols.
* Neoadjuvant Therapy: Systemic chemotherapy is almost universally employed to address micrometastatic disease and shrink the primary tumor.
* Surgical Resection: Total excision of the extremity tumor is required. Depending on the response to neoadjuvant therapy, this may involve a compartmental resection or, more commonly in the hand, a ray or partial hand amputation.
EWING SARCOMA
Ewing sarcoma is a highly aggressive, small round blue cell tumor. Similar to other primary malignant bone tumors, it rarely involves the hand, but when it does, it presents a significant diagnostic challenge.
Demographics and Clinical Mimicry
It occurs most frequently in males and typically manifests during the second decade of life.
Diagnostic Pitfall: Clinically, Ewing sarcoma of the hand is frequently mistaken for a local infection (osteomyelitis or septic arthritis). The patient often reports localized pain, swelling, erythema, fever, and general malaise. Laboratory studies commonly reveal leukocytosis and an elevation in the erythrocyte sedimentation rate (ESR).
Radiographic Findings and Differential Diagnosis
Radiographs of the hand typically show osteolytic lesions that destroy the adjacent cortical bone. The classic "onion-skin" periosteal reaction seen in long bones is often absent in the small tubular bones of the hand. The phalanges and metacarpals are affected with equal frequency.
The differential diagnosis includes:
* Infection (Osteomyelitis)
* Gouty arthropathy
* Giant cell tumor of bone
* Enchondroma
* Epidermoid inclusion cyst
* Aneurysmal bone cyst (ABC)
Surgical Management
A definitive tissue diagnosis via incisional or core needle biopsy is imperative before any definitive surgical intervention.
The patient’s general oncologic condition dictates the treatment. If a phalangeal lesion is painful and localized, an amputation through the joint proximal to the level of involvement (e.g., MCP joint disarticulation for a proximal phalanx lesion) is indicated. This relieves pain, removes the local disease burden, and provides rapid soft-tissue healing, allowing the patient to resume systemic chemotherapy without delay.
The presence of a metastatic Ewing sarcoma lesion in the hand carries an ominous prognosis, with a median patient survival of only 5 to 6 months.
METASTATIC TUMORS TO THE HAND (ACRO-METASTASES)
Metastatic lesions occurring in the hand (acro-metastases) are exceptionally rare, representing approximately 0.1% of all metastatic skeletal lesions.
Pathophysiology and Primary Sources
Acro-metastases occur via hematogenous dissemination. It is hypothesized that minor, unnoticed trauma to the hands causes local vasodilation and the release of chemotactic factors, creating a favorable microenvironment for circulating tumor cells to arrest and proliferate.
The most frequent primary source is bronchogenic (lung) carcinoma, accounting for nearly half of all cases. Other reported primary sources include:
* Carcinoma of the kidney (Renal Cell Carcinoma)
* Prostate gland
* Breast
* Uterus
* Colon
Clinical Presentation
Metastatic lesions in the hand typically present as rapidly enlarging, painful, erythematous, and swollen digits, often mimicking an acute paronychia, felon, or gout flare. Cutaneous metastases may present with irregular borders, uneven colors, and diameters larger than 6 mm. Awareness of these distinguishing characteristics is essential for early detection.
Management Protocol
The appearance of an acro-metastasis usually signifies widespread, end-stage systemic disease. Therefore, the primary goal of treatment is palliation.
- Multidisciplinary Care: An oncologist and a surgical oncologist should manage lesions that are thicker than 1 mm, as chemotherapy regimens are constantly evolving, and lymph node biopsy/dissection may be integral to systemic management.
- Palliative Surgery: For painful osseous metastases in the digits, a simple amputation (e.g., ray amputation or digit disarticulation) is often the most effective palliative measure. It provides immediate pain relief, removes the fungating or necrotic burden, and allows for rapid wound healing compared to complex resections or radiation therapy, thereby maximizing the patient's remaining quality of life.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
Following the surgical extirpation of any hand malignancy, a rigorous, customized postoperative rehabilitation protocol is essential to maximize residual function.
- Immobilization: The hand is typically immobilized in a bulky, non-compressive dressing with a volar orthosis in the intrinsic-plus position (wrist extended 20-30 degrees, MCP joints flexed 70-90 degrees, IP joints fully extended) to prevent collateral ligament contracture.
- Edema Control: Strict elevation is maintained for the first 48 to 72 hours.
- Early Mobilization: Once the surgical incisions are stable (typically 10-14 days postoperatively), active range of motion (AROM) of the uninvolved digits is initiated under the guidance of a certified hand therapist (CHT).
- Desensitization: For amputation stumps, a structured desensitization program utilizing varied textures, tapping, and fluidotherapy is critical to prevent neuroma-related hypersensitivity and encourage functional use of the residual limb.
