Solving Elbow Cases Adhesive: Capsulitis Stages & Treatment
Patient Presentation & History
A 48-year-old right-hand dominant male presented to the Orthopedic Trauma Clinic with a 9-month history of progressive left elbow pain and stiffness. His medical history is significant for well-controlled Type 2 Diabetes Mellitus and hypothyroidism, managed medically. There was no preceding major trauma identified by the patient; however, he recalled a minor "jarring" injury to his elbow approximately 10 months prior, following which he self-immobilized in a sling for 2 weeks, fearing a fracture. The pain initially presented as a dull ache, particularly worse at night and with attempts at terminal range of motion. Over the subsequent months, he noted a gradual, symmetrical restriction in both active and passive elbow flexion and extension, significantly impacting his activities of daily living, including dressing, personal hygiene, and occupational tasks (clerical work). He denied any acute locking, instability, or neurological symptoms such as paresthesias or weakness. Initial conservative management with oral NSAIDs and a short course of physical therapy focusing on stretching had provided minimal relief, with persistent functional limitations. He reported compliance with his diabetes and thyroid medication regimens.
Clinical Examination
Upon examination, the patient was alert and cooperative.
- Inspection: The left elbow appeared mildly swollen globally, with no erythema or overt deformity. There was no visible skin lesion or scar tissue. Mild disuse atrophy was noted in the forearm musculature compared to the contralateral limb.
- Palpation: Diffuse tenderness was elicited around the anterior and posterior aspects of the elbow joint, particularly over the joint line. No focal tenderness was identified over the epicondyles, olecranon, or radial head. The ulnar nerve groove was non-tender, and the ulnar nerve was not subluxable.
-
Range of Motion (ROM):
-
Left Elbow:
- Flexion: Active 90 degrees, Passive 95 degrees (normal 140-150 degrees). Flexion endpoint was firm and painful.
- Extension: Active -45 degrees, Passive -40 degrees (normal 0-5 degrees hyperextension). Extension endpoint was firm and painful.
- Pronation: Active 70 degrees, Passive 75 degrees (normal 80-90 degrees).
- Supination: Active 60 degrees, Passive 65 degrees (normal 80-90 degrees).
-
Right Elbow (contralateral):
Full, pain-free range of motion.
The global loss of motion, particularly affecting flexion and extension symmetrically in a "capsular pattern," was a key finding.
-
Left Elbow:
-
Neurological Assessment:
- Motor: Intact strength (5/5) in all muscle groups innervated by the radial, median, and ulnar nerves.
- Sensory: Intact light touch and pinprick sensation in all dermatomes distal to the elbow.
- Reflexes: Biceps, brachioradialis, triceps reflexes were 2+ bilaterally and symmetrical.
- Vascular Assessment: Radial and ulnar pulses were 2+ and symmetrical bilaterally. Capillary refill was brisk in all digits. No signs of venous congestion or lymphoedema.
- Ligamentous Stability: Varus and valgus stress testing performed at 30 degrees of flexion and full extension revealed a firm endpoint with no demonstrable laxity, indicating intact medial and lateral collateral ligament complexes.
Overall, the clinical picture was consistent with a progressive, global restriction of elbow motion, characterized by end-range pain and a firm capsular feel, without signs of instability or neurovascular compromise. This presentation, coupled with his predisposing comorbidities, strongly suggested adhesive capsulitis of the elbow.
Imaging & Diagnostics
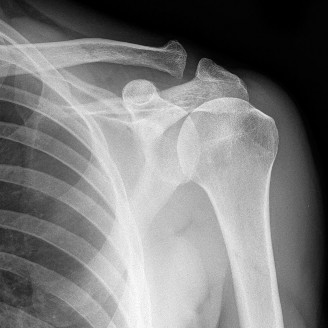
Plain Radiographs:
Standard anteroposterior (AP) and lateral views of the left elbow were obtained. These revealed:
* No evidence of fracture, dislocation, or subluxation.
* Maintained joint space without significant degenerative changes or osteophytes.
* No visible heterotopic ossification (HO).
* Normal alignment of the humeroulnar and radiocapitellar joints.
* Absence of loose bodies.
The plain radiographs were largely unremarkable, which is a common finding in primary adhesive capsulitis, where the pathology is predominantly soft tissue. However, they are crucial to rule out bony blocks, malunion from previous subtle trauma, and degenerative arthrosis.
Magnetic Resonance Imaging (MRI):
Given the persistent symptoms and the characteristic clinical presentation, an MRI of the left elbow was performed to further characterize the soft tissue pathology and rule out other internal derangements.
The MRI findings demonstrated:
* Significant thickening and fibrosis of the anterior joint capsule, particularly noticeable at the coronoid fossa.
* Mild thickening of the posterior capsule.
* Increased signal intensity on T2-weighted images within the anterior capsule, suggesting an inflammatory component, consistent with the "freezing" phase of adhesive capsulitis.
* No evidence of osteochondral lesions, loose bodies, or significant articular cartilage loss.
* The medial and lateral collateral ligaments appeared intact, although some peri-ligamentous edema was noted.
* No significant tendinopathy or muscle pathology was identified.
* The ulnar nerve course appeared normal, with no signs of compression or edema within the cubital tunnel.
Other Diagnostics:
*
Laboratory Investigations:
HbA1c was 6.8%, indicating controlled but slightly elevated blood glucose. Thyroid stimulating hormone (TSH) was within normal limits, reflecting well-managed hypothyroidism. These tests were performed to correlate with known risk factors for adhesive capsulitis.
*
CT Scan:
A CT scan was considered but ultimately not deemed necessary in this case due to the clear MRI findings and absence of bony pathology on plain films. It would have been indicated if there was suspicion of subtle malunion, complex heterotopic ossification, or osteochondral defects not fully characterized by MRI.
Summary of Imaging: The imaging studies collectively supported the diagnosis of adhesive capsulitis, demonstrating soft tissue capsular contracture without significant intrinsic joint pathology or mechanical bony blocks. This confirmed the necessity to address the capsular thickening as the primary cause of stiffness.
Differential Diagnosis
The differential diagnosis for elbow stiffness is broad and requires systematic exclusion of various pathologies. For this patient, considering his clinical presentation and imaging findings, the key differentials included:
| Feature | Adhesive Capsulitis (Primary/Secondary) | Post-Traumatic Stiffness (Bony Block/HO) | Elbow Osteoarthritis | Complex Regional Pain Syndrome (CRPS) Type I |
|---|---|---|---|---|
| Pathophysiology | Idiopathic or post-event capsular fibrosis, inflammation, contracture. | Mechanical impediment: Malunion, nonunion, heterotopic ossification (HO). | Degenerative cartilage loss, osteophyte formation, joint space narrowing. | Dysregulation of sensory, motor, autonomic nervous systems post-injury. |
| Onset | Gradual, insidious; often post-minor trauma/immobilization. | Following significant trauma (fracture, dislocation) or surgery. | Gradual, progressive, typically insidious, age-related. | Post-minor or major trauma, often disproportionate pain. |
| Pain Characteristics | Diffuse, achy, worse at end-range, often at night. Associated with stiffness. | Mechanical pain, sharp with attempted motion into block; may be less constant. | Activity-related, worse with weight-bearing, crepitus, mechanical catching. | Severe, burning, throbbing, disproportionate to injury; allodynia, hyperalgesia. |
| ROM Loss | Global, symmetrical loss of active and passive ROM in a capsular pattern (flexion > extension loss). | Specific mechanical block; often non-capsular pattern, hard endpoint. | Primarily extension loss initially, progressive global loss; crepitus. | Global, profound, often with associated skin/trophic changes. |
| Physical Exam | Diffuse tenderness, firm capsular end-feel. No focal bony tenderness. | Focal tenderness over bony block/HO. Hard, abrupt end-feel. | Crepitus, tenderness over osteophytes, often posterior. | Swelling, erythema, hyperhidrosis, allodynia, trophic changes (skin/nails). |
| Plain Radiographs | Usually normal; may show soft tissue thickening. | Evidence of malunion, nonunion, HO, fracture lines. | Joint space narrowing, osteophytes, subchondral sclerosis/cysts. | May show patchy osteopenia in later stages. |
| MRI Findings | Capsular thickening (esp. anterior), increased signal intensity. | Defines bony anatomy, HO extent, soft tissue impingement. | Cartilage defects, subchondral changes, synovitis, loose bodies. | Soft tissue edema, effusions; later stages: bony atrophy. |
| Response to PT/Injections | Limited initial response; progress can be slow but possible. Often requires prolonged therapy. | Poor response to non-operative methods if mechanical block is significant. | Variable; some relief with injections/PT, but structural issues persist. | Often poor response; may worsen with aggressive PT; requires specific CRPS management. |
| Key Differentiating Features | Capsular pattern of loss, firm end-feel, lack of bony blocks/arthrosis on imaging, systemic comorbidities. | Clear bony pathology on imaging, hard mechanical end-feel, history of significant trauma. | Radiographic evidence of degenerative changes, crepitus, specific ROM patterns. | Disproportionate pain, autonomic dysfunction, trophic changes. |
In our patient's case, the insidious onset, global and symmetrical loss of both active and passive ROM in a capsular pattern, the presence of predisposing comorbidities (diabetes, hypothyroidism), the firm but yielding end-feel on examination, and the characteristic MRI findings of capsular thickening with absence of bony blocks or significant arthrosis, strongly favored the diagnosis of secondary adhesive capsulitis of the elbow. The lack of neurovascular compromise or autonomic dysfunction effectively ruled out CRPS.
Surgical Decision Making & Classification
Despite a supervised course of intensive physical therapy for 3 months post-diagnosis, which included Mulligan mobilizations, static progressive splinting, and home exercises, the patient demonstrated only marginal improvement in his range of motion (flexion to 100 degrees, extension to -35 degrees) and persistent pain, particularly at the end ranges. His functional limitations remained significant. This failure of conservative management, typically defined as 6-9 months of dedicated, supervised therapy without satisfactory functional improvement, served as the primary indication for surgical intervention.
The patient was approaching the "thawing" phase of adhesive capsulitis, where inflammation starts to subside, and the stiffness becomes more predominant. Performing a surgical release in this phase is generally preferred over the acute "freezing" phase, where inflammation is high, potentially leading to increased pain and re-stiffening post-operatively.
Surgical Indications for Elbow Stiffness:
* Failure of prolonged, aggressive non-operative treatment (typically 6-12 months).
* Persistent significant functional limitation (e.g., inability to perform ADLs, work-related tasks).
* Documented significant loss of motion (e.g., flexion contracture >30 degrees, flexion <100 degrees).
* Specific mechanical blocks identified on imaging or exam that are amenable to surgical excision (e.g., heterotopic ossification, loose bodies, osteophytes). In this case, it was primarily capsular contracture.
Classification of Elbow Stiffness:
Elbow stiffness can be broadly classified based on its etiology and location of the pathology.
*
Intrinsic Stiffness:
Refers to intra-articular pathology (e.g., articular surface damage, loose bodies, intra-articular adhesions, malunited intra-articular fractures).
*
Extrinsic Stiffness:
Refers to extra-articular pathology (e.g., capsular contracture, heterotopic ossification, skin contractures, muscle contractures, ligamentous contracture).
*
Mixed Stiffness:
A combination of both intrinsic and extrinsic factors.
This patient primarily presented with extrinsic stiffness secondary to capsular contracture , predominantly anterior, confirmed by MRI. There were no significant intrinsic factors.
Maneuver and Morrey Classification:
Morrey et al. described a classification based on the predominant loss of motion:
*
Flexion contracture:
Loss of extension (e.g., -40 degrees).
*
Loss of flexion:
Inability to achieve full flexion (e.g., 90 degrees).
*
Loss of pronation/supination:
Less common as a primary component in adhesive capsulitis, but can occur.
Our patient demonstrated a significant flexion contracture (-40 degrees extension) and loss of terminal flexion (to 95 degrees), classifying him with a combined flexion-extension restriction.
The decision was made for an arthroscopic elbow capsular release. Arthroscopy was chosen over an open approach due to its minimally invasive nature, reduced soft tissue dissection, potentially faster recovery, and excellent visualization for capsular release, especially in the absence of large bony blocks or complex HO.
Surgical Technique / Intervention
Procedure: Arthroscopic Elbow Capsular Release and Debridement.
Anesthesia:
The patient underwent general endotracheal anesthesia combined with a regional supraclavicular brachial plexus block. This multimodal approach provides excellent intraoperative and postoperative analgesia, facilitating early rehabilitation.
Patient Positioning:
The patient was positioned in the lateral decubitus position on a standard operating table. The affected (left) arm was draped free and suspended in a traction tower, with the shoulder abducted to 90 degrees and the elbow flexed to 90 degrees. This provides optimal visualization and manipulation of the elbow joint through traction and allows for dynamic assessment of ROM intraoperatively. A tourniquet was applied to the upper arm but not inflated initially.
Surgical Approach and Portals:
Standard arthroscopic portals were used, with careful attention to neurovascular structures. The elbow joint was first insufflated with normal saline via a needle to distend the joint capsule.
-
Proximal Anteromedial (PAM) Portal: This was the initial working portal. It is established approximately 2 cm proximal and 2 cm anterior to the medial epicondyle. Great care was taken to avoid the median nerve (anterior and medial) and brachial artery.
- Utility: Used for initial diagnostic arthroscopy, anterior capsule release.
-
Proximal Anterolateral (PAL) Portal: Established approximately 2 cm proximal and 2 cm anterior to the lateral epicondyle, avoiding the radial nerve (anterior to the capitellum) and cephalic vein.
- Utility: Used as a viewing portal or for instrumentation for anterior capsule release.
-
Direct Lateral (DL) Portal: Created directly over the capitellum, approximately 1 cm distal to the lateral epicondyle. This portal is useful for instrument access to the posterior compartment if the proximal portals are insufficient. It is less frequently used in primary capsular release but can be an accessory viewing portal.
- Utility: Secondary viewing/working portal, particularly for posterior work.
-
Posterolateral Portal: Located approximately 2 cm proximal to the olecranon tip, just lateral to the triceps tendon. Careful entry is crucial to avoid the ulnar nerve medially.
- Utility: Primarily for posterior compartment viewing and release.
Surgical Steps:
-
Diagnostic Arthroscopy:
- The arthroscope was introduced via the PAM portal. The joint was systematically inspected for synovitis, loose bodies, articular cartilage lesions, and osteophytes. In this case, diffuse synovial hypertrophy and significant anterior capsular thickening were noted, confirming the MRI findings.
- The radiocapitellar joint and the trochlea-olecranon articulation were assessed for integrity. No significant pathology was noted in these areas.
-
Anterior Capsular Release:
- This is often the most critical step for improving elbow flexion and extension. Using a full-radius shaver and a radiofrequency ablator (e.g., VAPR), the thickened and contracted anterior capsule was systematically released.
- The release extended from medial to lateral, working carefully near the neurovascular bundle anteriorly. The capsule was removed from its attachments to the coronoid fossa and the anterior aspect of the humerus.
- The extent of release was visually guided and confirmed by intraoperative passive range of motion. The capsule was resected until the deep fibers of the brachialis muscle were visible.
-
Posterior Capsular Release:
- After the anterior release, the arthroscope was moved to a posterior portal (e.g., posterolateral), and working instruments were used via another posterior portal (e.g., direct lateral or a separate posteromedial).
- The posterior capsule was released from the olecranon fossa and the posterior aspect of the humerus. Care was taken to avoid over-resection, which could lead to posterior instability.
- Any posterior osteophytes or loose bodies (none in this case) would be addressed at this stage.
-
Medial and Lateral Gutter Debridement / Collateral Ligament Management:
- While usually not fully released in adhesive capsulitis without significant post-traumatic deformity, scar tissue in the medial and lateral gutters can contribute to stiffness.
- Careful debridement of hypertrophic synovium and scar tissue in these areas was performed.
- The integrity of the medial (MCL) and lateral (LCL) collateral ligaments was preserved. If significant lateral column contracture was present contributing to fixed varus or valgus, a selective partial release of the appropriate collateral ligament might be considered, but only with extreme caution and intraoperative stress testing to ensure stability. This was not required in this patient.
-
Assessment of Range of Motion:
- Following the capsular release, the tourniquet was deflated.
- The arm was brought off traction, and a comprehensive intraoperative passive range of motion was assessed. The goal was to achieve at least 0-5 degrees of extension and 130-140 degrees of flexion, ensuring stability throughout the arc.
- In this patient, we achieved 0 degrees of extension and 135 degrees of flexion with a soft, physiologic end-feel, and no instability on varus or valgus stress testing.
-
Ulnar Nerve Assessment and Release (if indicated):
- Although no preoperative signs of ulnar neuropathy were present, the ulnar nerve was carefully palpated and its course verified, especially if extensive medial release had been performed. A prophylactic ulnar nerve decompression or transposition might be considered if the nerve was found to be tight or subluxing with the new range of motion, but this was not necessary in this case.
-
Closure:
- Portals were closed with simple sutures (e.g., 4-0 nylon).
- A sterile dressing was applied. A bulky soft dressing was applied, and a posterior splint was used for comfort in the first few hours, primarily to protect the portals, before immediate mobilization.
Post-Operative Protocol & Rehabilitation
The success of surgical release for elbow adhesive capsulitis is highly dependent on an aggressive and well-structured post-operative rehabilitation protocol. The goal is to maintain the newly gained range of motion and prevent recurrence of contracture.
Phase 1: Immediate Post-operative (Day 0 - Week 2)
- Pain Management: Aggressive multimodal analgesia including regional nerve block, oral NSAIDs, paracetamol, and opioid analgesics as needed. Adequate pain control is paramount for patient compliance with therapy.
- Continuous Passive Motion (CPM) Machine: Initiated immediately in the recovery room. The patient used the CPM machine for 4-6 hours daily, cycling through the full permissible arc of motion achieved intraoperatively (e.g., 0-135 degrees).
-
Early Mobilization:
- Day 1: Gentle active-assisted and passive range of motion (AAROM/PROM) exercises initiated under the guidance of a dedicated elbow therapist. Focus on maintaining full extension and achieving maximum flexion.
- Exercises: Elbow flexion/extension, pronation/supination.
- Frequency: Exercises performed frequently throughout the day (e.g., 10-15 repetitions every 1-2 hours while awake).
-
Splinting:
- Static Progressive or Dynamic Splints: A dynamic splint (e.g., Dynasplint, JAS splint) set to progressively increase extension was often initiated within the first 24-48 hours. This is worn for several hours daily, particularly at night, to overcome residual capsular tightness and creep.
- A flexion splint may be utilized if flexion remains limited.
- Weight Bearing/Strengthening: None during this phase.
- Wound Care: Standard wound care for portal sites.
Phase 2: Intermediate (Week 2 - Week 6)
- Progressive ROM: Continuation of AAROM and PROM exercises. The therapist gradually increases the intensity and duration of stretching.
- Manual Therapy: Gentle joint mobilizations (e.g., Grade I-II distraction and glides) to improve capsular extensibility.
-
Initiate Light Strengthening:
- Isometric exercises for elbow flexors, extensors, pronators, and supinators.
- Very light resistance with elastic bands or low-weight dumbbells as tolerated.
- Continue Splinting: Ongoing use of dynamic or static progressive splints.
- Activity Modification: Avoid heavy lifting, pushing, or pulling. Educate on ergonomic modifications for daily activities.
Phase 3: Advanced (Week 6 - Month 3)
- Progressive Strengthening: Increase resistance for isotonic exercises. Focus on functional strengthening for all elbow muscle groups.
- Endurance Training: Incorporate light, repetitive activities.
- Functional Training: Gradually integrate occupational and activity-specific tasks.
- Dynamic Splint Weaning: Gradually decrease the use of dynamic splints as functional ROM goals are achieved and maintained.
- Proprioception and Neuromuscular Control: Exercises to improve joint awareness and stability.
Phase 4: Return to Activity (Month 3 onwards)
- Sport-Specific/Work-Specific Training: Tailored exercises to prepare for full return to pre-injury activities.
- Maintenance Program: Lifelong commitment to regular stretching and strengthening exercises to prevent recurrence, especially given the patient's underlying comorbidities.
- Follow-up: Regular clinical follow-ups to monitor progress, assess ROM, and address any concerns. Radiographs may be obtained to rule out heterotopic ossification recurrence.
Specific Considerations for Patients with Diabetes:
* Increased risk of re-stiffening due to impaired collagen synthesis and increased inflammation.
* More aggressive and prolonged rehabilitation may be required.
* Strict glycemic control is crucial for optimal healing and outcome.
* Closer monitoring for wound healing and potential infection.
The patient was discharged with a home exercise program and a dynamic extension splint, with daily outpatient physical therapy scheduled for the first 8 weeks, then tapering frequency based on progress. Close communication between the surgeon and the therapist was maintained to ensure optimal progression and address any setbacks promptly.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls for Adhesive Capsulitis of the Elbow:
- Diagnosis is Clinical: The diagnosis is primarily based on a thorough history and physical examination, particularly the capsular pattern of global ROM loss with a firm end-feel. Imaging is crucial to rule out other pathologies rather than confirm adhesive capsulitis.
- Identify Predisposing Factors: Always screen for comorbidities such as Diabetes Mellitus and thyroid disorders, as these significantly influence prognosis and rehabilitation.
- Exhaustive Conservative Trial: A minimum of 6-9 months of dedicated, supervised physical therapy is generally required before considering surgical intervention. This includes a multimodal approach (NSAIDs, steroid injections, manual therapy, progressive splinting).
- Timing of Surgery: Optimal timing for surgical release is typically in the "thawing" phase or when non-operative treatment has plateaued. Operating during the acute inflammatory "freezing" phase may lead to greater post-operative pain and re-stiffening.
- Comprehensive Release: Arthroscopic release should be comprehensive, addressing the anterior and posterior capsules thoroughly. If present, scar tissue in the medial and lateral gutters also needs debridement. The brachialis muscle often requires partial release from the anterior capsule.
- Intraoperative ROM Assessment: Crucial for confirming adequate release. Aim for at least 0 degrees extension and 130-140 degrees flexion with a soft end-feel and demonstrated stability.
- Aggressive Post-operative Rehabilitation: This is paramount. Immediate active and passive ROM, continuous passive motion (CPM), and dynamic or static progressive splinting are non-negotiable for maintaining the achieved motion.
- Multimodal Pain Management: Essential for allowing patients to participate in the aggressive rehabilitation program. Regional blocks, oral analgesics, and local anesthetic infusions should be considered.
- Patient Education and Compliance: Patients must understand the prolonged nature of rehabilitation and their active role in achieving a successful outcome.
Pitfalls to Avoid:
- Misdiagnosis: Failing to differentiate adhesive capsulitis from other causes of elbow stiffness such as bony blocks (HO, malunion), loose bodies, or early osteoarthritis. This leads to inappropriate management.
- Inadequate Conservative Trial: Rushing to surgery without a sufficiently long and intense course of non-operative treatment.
- Incomplete Surgical Release: The most common technical error. Failure to adequately release the contracted capsule, especially the anterior capsule, will result in persistent stiffness and poor outcomes.
- Over-Aggressive Manipulation Under Anesthesia (MUA) without Release: While MUA can be part of the surgical regimen, it should always be followed by thorough arthroscopic or open capsular release. Isolated MUA carries a high risk of iatrogenic fracture, ligamentous rupture, or neurovascular injury, without adequately addressing the underlying pathology.
- Neglecting Coexisting Pathology: Failing to address concomitant issues like ulnar nerve compression (especially if medial release is extensive) or significant heterotopic ossification.
- Poor Post-operative Pain Control: Leads to patient apprehension and inability to comply with the demanding rehabilitation protocol, ultimately resulting in re-stiffening.
- Lack of Adherence to Rehabilitation: The most common cause of suboptimal results. Patients must be highly motivated and compliant with their therapy.
- Early Weight-Bearing/Loading: Can exacerbate inflammation and potentially lead to recurrence of stiffness or heterotopic ossification, especially if bone formation inhibitors are not used.
- Ignoring Systemic Factors: Failing to recognize and optimize control of systemic conditions like diabetes, which are known to negatively impact surgical outcomes and increase the risk of re-contracture.
- Heterotopic Ossification Recurrence: A concern in post-traumatic cases and after aggressive release, especially in high-risk patients. Consider NSAID prophylaxis (e.g., Indomethacin) or radiation therapy in selected cases.
