Introduction & Epidemiology
Acromioclavicular (AC) joint separations represent a common traumatic injury to the shoulder girdle, particularly prevalent in active populations and contact sports. These injuries result from disruption of the ligamentous stabilizers of the AC joint, leading to varying degrees of displacement of the distal clavicle relative to the acromion. Understanding the etiology, classification, and management spectrum is critical for optimal patient outcomes.
Epidemiologically, AC joint injuries account for approximately 9% to 12% of all shoulder girdle injuries, with a reported incidence ranging from 3 to 10 per 100,000 people per year. They disproportionately affect males aged 20-30 years, often associated with sports such as football, rugby, cycling, and hockey. The typical mechanism involves a direct blow to the superior or superolateral aspect of the acromion with the arm adducted, driving the acromion inferiorly and medially relative to the clavicle. Less commonly, an indirect fall onto an outstretched hand can transmit axial load, leading to injury.
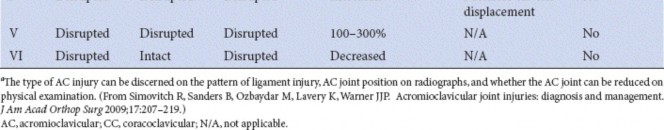
The universally accepted classification system for AC joint separations is the Rockwood classification, which categorizes injuries based on the direction and degree of displacement of the distal clavicle and the extent of ligamentous disruption. This system guides diagnosis and treatment decision-making:
*
Type I:
Sprain of the AC ligaments without significant disruption. The joint is stable.
*
Type II:
Complete tear of the AC ligaments, but the coracoclavicular (CC) ligaments remain intact. Partial superior subluxation of the clavicle, often less than 25% of the clavicular height.
*
Type III:
Complete tears of both AC and CC ligaments. The clavicle is superiorly displaced by 25% to 100% of its height, but typically remains within the sagittal contour of the acromion on an anteroposterior radiograph. The deltoid and trapezius muscle attachments may be intact or minimally disrupted.
*
Type IV:
Complete tears of AC and CC ligaments with posterior displacement of the clavicle into or through the trapezius muscle. This is a severe injury requiring specific reduction techniques.
*
Type V:
Complete tears of AC and CC ligaments, with marked superior displacement of the clavicle (typically >100% of its height). Extensive stripping of the deltoid and trapezius from the distal clavicle occurs.
*
Type VI:
Extremely rare injury involving inferior dislocation of the clavicle beneath the coracoid process or acromion. This often involves significant associated neurovascular injury.
While Rockwood Types I and II are consistently managed non-operatively, the management of Type III injuries remains controversial, with ongoing debate regarding operative versus non-operative approaches. Types IV, V, and VI are generally considered surgical indications due to significant instability, functional impairment, and cosmetic deformity.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and biomechanics of the AC joint is paramount for effective treatment of its separations. The AC joint is a diarthrodial joint formed by the articulation of the distal clavicle and the medial aspect of the acromion. It contains an articular disc or meniscus, which can be partially or completely torn in traumatic injuries.
The primary stabilizers of the AC joint are:
- Acromioclavicular (AC) Ligaments: These are capsular thickenings (superior, inferior, anterior, posterior) that span the joint. The superior AC ligament is the thickest and strongest, providing primary horizontal stability and resisting posterior displacement of the clavicle. The AC ligaments primarily resist anterior and posterior shear forces and superior translation in the initial stages of injury.
-
Coracoclavicular (CC) Ligaments:
These robust extra-articular ligaments are the primary vertical stabilizers of the AC joint. They originate from the coracoid process of the scapula and insert onto the undersurface of the clavicle. They consist of two distinct bundles:
- Conoid Ligament: Medial and conical in shape, originating from the posterior medial aspect of the coracoid and inserting onto the conoid tubercle on the undersurface of the clavicle. It primarily resists superior translation of the clavicle and posterior rotation.
- Trapezoid Ligament: Lateral and quadrilateral, originating from the superior aspect of the coracoid and inserting onto the trapezoid line on the undersurface of the clavicle, just anterior and lateral to the conoid tubercle. It primarily resists superior translation and posterior displacement, and limits horizontal movement.
The CC ligaments provide approximately 70-80% of the vertical stability of the AC joint, while the AC ligaments contribute the remaining 20-30% of vertical stability and the majority of horizontal stability. Disruption of both AC and CC ligaments, as seen in Rockwood Type III and higher injuries, leads to significant instability, particularly in the vertical plane, due to the unopposed pull of the trapezius muscle on the distal clavicle.
Other relevant anatomical considerations include:
*
Deltoid and Trapezius Muscles:
These muscles insert directly onto the distal clavicle and acromion. In higher-grade AC separations (Type IV, V), these muscle attachments are extensively torn, contributing to the severe displacement and difficulty in reduction. The trapezius muscle pulls the clavicle superiorly, while the deltoid exerts an inferior and anterior force on the acromion.
*
Neurovascular Structures:
The brachial plexus and subclavian vessels lie inferior and medial to the coracoid process. Extreme caution is required during surgical dissection and drilling around the coracoid to avoid iatrogenic injury.
*
Coracoacromial Ligament:
This ligament forms part of the coracoacromial arch and may be involved in some injury patterns, though it is not a primary stabilizer of the AC joint itself.
Biomechanically, the AC joint allows for scapular rotation, elevation, and protraction, primarily gliding movements. The clavicle acts as a strut, connecting the upper extremity to the axial skeleton. Injury to the AC joint disrupts this kinematic chain, affecting overall shoulder function and stability. Restoration of the anatomical relationship and ligamentous integrity is crucial for re-establishing normal shoulder biomechanics.
Indications & Contraindications
The decision to treat an AC joint separation operatively or non-operatively is based on the Rockwood classification, patient factors (age, activity level, hand dominance, occupation), and the presence of associated injuries or specific symptoms.
Operative Indications
-
Rockwood Type III:
This remains the most controversial indication.
- Acute injuries in young, high-demand individuals (e.g., overhead athletes, manual laborers) where functional demands are high and an earlier return to full activity is desired.
- Patients with persistent pain, weakness, or functional limitations despite a trial of non-operative management.
- Objective evidence of ongoing instability with active motion.
- Hand dominance on the affected side, particularly in throwing athletes.
- Significant cosmetic deformity causing patient distress (though this is often a secondary indication).
- Rockwood Type IV: Undisputed operative indication. Posterior displacement of the clavicle into the trapezius musculature necessitates surgical reduction and stabilization due to irreducibility and high risk of persistent dysfunction.
- Rockwood Type V: Undisputed operative indication. Marked superior displacement with extensive deltoid and trapezius disruption leads to severe instability, pain, and cosmetic deformity.
- Rockwood Type VI: Undisputed operative indication. Inferior dislocation is rare but requires surgical intervention due to neurovascular compromise and extreme instability.
- Chronic AC joint separation: Defined as injuries presenting typically 3 weeks or more after the initial trauma, with persistent pain, instability, and functional deficit (e.g., instability, fatigue, weakness). These often require reconstructive rather than reparative procedures.
- Associated Injuries: Concurrent ipsilateral clavicle fracture, scapular fracture, or brachial plexus injury that may complicate non-operative management or necessitate surgical access.
Non-Operative Indications
- Rockwood Type I: Universal consensus for non-operative management. Sling for comfort, early range of motion (ROM), and rehabilitation.
- Rockwood Type II: Universal consensus for non-operative management. Sling for comfort for 1-2 weeks, followed by progressive ROM and strengthening.
-
Rockwood Type III (Selected Cases):
- Sedentary individuals or those with low functional demands.
- Elderly patients with comorbidities.
- Patients willing to accept potential residual deformity and a potentially longer, albeit successful, recovery period.
- Initial management often involves a sling, pain control, and early rehabilitation. Surgery may be considered if symptoms persist.
Contraindications
-
Absolute Contraindications:
- Active local or systemic infection.
- Severe medical comorbidities that preclude safe anesthesia or surgery (e.g., uncontrolled cardiac disease, severe coagulopathy).
- Non-displaced or minimally displaced associated fractures of the clavicle or acromion that could be worsened by surgery, unless the surgical plan incorporates addressing these fractures.
-
Relative Contraindications:
- Patient non-compliance with post-operative rehabilitation protocols.
- Significant osteoporosis potentially compromising hardware fixation.
- Severe, non-reconstructible soft tissue damage.
Operative vs. Non-Operative Indications
| Rockwood Type | Operative Indications | Non-Operative Indications |
|---|---|---|
| Type I | N/A (Always non-operative) | Universal consensus: Sling for comfort, early ROM, physical therapy. |
| Type II | N/A (Always non-operative) | Universal consensus: Sling for 1-2 weeks, progressive ROM, physical therapy. |
| Type III | - Young, active, high-demand individuals (athletes, manual laborers) | - Sedentary individuals or those with low functional demands |
| - Persistent pain, instability, or functional deficit after non-operative trial | - Elderly patients with significant comorbidities | |
| - Dominant arm injury in overhead athletes | - Patient preference after informed discussion of pros and cons | |
| - Significant cosmetic deformity causing distress | ||
| Type IV | Universal consensus: Irreducible posterior clavicular displacement. | N/A (Always operative due to irreducibility and high risk of persistent dysfunction). |
| Type V | Universal consensus: Marked superior clavicular displacement (>100%), extensive soft tissue stripping. | N/A (Always operative due to severe instability, pain, and functional impairment). |
| Type VI | Universal consensus: Inferior clavicular dislocation beneath coracoid/acromion, often with neurovascular compromise. | N/A (Always operative due to extreme instability and potential neurovascular compromise). |
| Chronic AC | - Persistent pain, instability, fatigue, or functional deficit despite non-operative treatment, typically presenting >3 weeks post-injury. Often requires reconstructive procedures. | - Asymptomatic or minimally symptomatic chronic cases. |
| Associated | - Concurrent fractures (e.g., ipsilateral clavicle or scapula) that require surgical fixation or complicate non-operative management. | - Minor associated injuries that do not alter the stability or prognosis of the AC joint separation. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential for a successful outcome in AC joint reconstruction. This involves comprehensive patient evaluation, detailed imaging review, and thoughtful selection of surgical technique and implants.
Pre-Operative Assessment
- Clinical Evaluation: A thorough history, focusing on mechanism of injury, symptom duration, previous shoulder injuries, and functional demands. A detailed physical examination should assess active and passive range of motion, strength, neurovascular status, and specific AC joint tenderness and stability. Special tests such as the cross-body adduction test can elicit AC joint pain. The degree of superior, anterior, and posterior displacement should be noted.
-
Imaging:
- Plain Radiographs: Anteroposterior (AP) view of the shoulder, Zanca view (10-15 degrees cephalic tilt, allowing for better visualization of the AC joint without glenoid overlap), axillary lateral view (to assess anterior/posterior displacement), and potentially stress views (bilateral AP with weight-bearing, though their utility is debated for acute injuries).
- MRI: Valuable for assessing the integrity of the AC and CC ligaments, articular disc, and surrounding soft tissues (deltoid/trapezius avulsion). It can also identify occult fractures or other intra-articular pathology.
- CT Scan: Useful for complex injuries, concomitant fractures (e.g., coracoid, clavicle), or in chronic cases to assess degenerative changes or heterotopic ossification. CT with 3D reconstructions can precisely map the displacement and aid in surgical planning.
- Medical Optimization: Ensure the patient is medically optimized for surgery. Address any comorbidities, review medications, and obtain appropriate medical clearances.
- Informed Consent: Discuss the diagnosis, proposed surgical procedure, alternative treatments (including non-operative), potential benefits, risks (including infection, neurovascular injury, hardware failure, loss of reduction, persistent pain, stiffness), and expected recovery course. Manage patient expectations regarding function and cosmetic outcome.
-
Implant Selection:
The choice of fixation device depends on surgeon preference, injury pattern, and chronicity. Options include:
- Suture-button systems (e.g., Dog Bone, TightRope): Increasingly popular for acute and chronic CC ligament reconstruction, offering dynamic stability.
- Coracoclavicular hook plate: Provides rigid fixation but requires a second surgery for removal.
- AC plates (e.g., clavicle hook plate): Less commonly used as primary fixation due to high hardware irritation rates, but may be considered for select patterns or in conjunction with CC fixation.
- Allograft/autograft reconstruction: Often utilized for chronic injuries or revisions, augmenting CC ligament reconstruction.
Patient Positioning
The patient is typically positioned for shoulder surgery, allowing for adequate exposure of the AC joint, distal clavicle, and coracoid process.
1.
Anesthesia:
General endotracheal anesthesia is standard. A regional interscalene block can be co-administered for post-operative pain management.
2.
Positioning Options:
*
Beach Chair Position:
This is a common and versatile position. The patient is semi-recumbent at 30-70 degrees, allowing good access to the superior shoulder and a comfortable working angle for arthroscopic or open approaches. The head is stabilized and often tilted away from the operative side to allow neck extension if needed. The arm is draped free, allowing full manipulation.
*
Lateral Decubitus Position:
Less common for open AC joint reconstruction but may be used if arthroscopy is combined with an open approach, or if other procedures (e.g., rotator cuff repair) are planned. The patient is positioned on the contralateral side, with the operative arm suspended in traction.
3.
Preparation and Draping:
The shoulder girdle, including the entire ipsilateral arm, neck, and chest, is prepped with an antiseptic solution (e.g., chlorhexidine or povidone-iodine). The area should extend from the clavicle anteriorly to the scapular spine posteriorly, and from the base of the neck to the mid-humerus. The limb is often draped free to allow intraoperative manipulation and assessment of reduction. A sterile tourniquet is typically not required unless there is a specific need for bloodless field in the arm.
Detailed Surgical Approach / Technique
The goal of surgical management for AC joint separations is to achieve and maintain anatomical reduction of the distal clavicle to the acromion and/or coracoid, restore ligamentous stability, and promote healing. Modern approaches often combine direct AC joint repair/stabilization with coracoclavicular ligament reconstruction or augmentation. We will detail a common approach utilizing an open reduction and internal fixation with a suture-button construct for CC ligament reconstruction, often augmented with AC joint capsular repair.
Incision and Dissection
- Skin Incision: A curvilinear or saber-shaped incision is made, typically 6-8 cm in length, centered over the AC joint and extending medially along the clavicle and slightly inferiorly towards the coracoid process. A vertical incision over the AC joint may also be used.
- Subcutaneous Dissection: Dissect through the subcutaneous tissue, carefully identifying and preserving the supraclavicular nerves to minimize post-operative dysesthesia.
-
Muscle Exposure:
The deltoid muscle anteriorly and the trapezius muscle posteriorly insert onto the distal clavicle. These muscles are often partially or completely detached in higher-grade injuries (Rockwood Types IV, V). The deltoid fascia is incised longitudinally along the clavicular attachment. The deltoid and trapezius are carefully elevated subperiosteally or subfascially from the superior aspect of the distal clavicle to expose the AC joint and distal 3-4 cm of the clavicle. In Rockwood Type IV injuries, the clavicle may be found buttonholed through the trapezius, requiring specific maneuver for extraction.
Figure 1: Illustration showing the anatomical relationship of the AC joint, clavicle, coracoid process, and the CC ligaments (conoid and trapezoid). - Coracoid Exposure: The key to CC ligament reconstruction is reliable identification and exposure of the coracoid process. This is typically done by dissecting inferiorly and medially from the undersurface of the clavicle. The interval between the deltoid and pectoralis major muscles can be utilized to access the coracoid. Care must be taken to protect the cephalic vein laterally and the neurovascular structures (brachial plexus, subclavian artery/vein) located immediately medial and inferior to the coracoid. The pectoralis minor muscle often attaches to the coracoid and may need to be partially detached or retracted.
Debridement and Reduction
- Joint Debridement: If the AC joint capsule and meniscoid are severely damaged or incarcerated, debridement or partial meniscectomy may be performed. In chronic cases, any hypertrophic tissue, osteophytes, or degenerative changes at the AC joint should be addressed.
- Anatomical Reduction: The distal clavicle is anatomically reduced to the acromion. This often requires gentle superior and posterior pressure on the acromion while simultaneously applying inferior and anterior pressure to the clavicle, restoring the correct vertical and horizontal alignment. In Type IV injuries, the clavicle must be disengaged from the trapezius first. A temporary reduction clamp (e.g., Verbrugge or speed clamp) or K-wires may be used to hold the reduction while fixation is applied.
Coracoclavicular Ligament Reconstruction (Suture-Button Technique)
This is a commonly employed technique for its biological approach and avoidance of rigid hardware.
- Clavicular Tunnels: Under fluoroscopic guidance, two drill holes are created in the clavicle, approximately 2-3 cm medial to the AC joint, corresponding to the anatomical footprint of the conoid and trapezoid ligaments. The holes should be spaced 1-1.5 cm apart in the anteroposterior plane, roughly centered over the CC ligament insertions. The holes are drilled from superior to inferior. Ensure the drill path avoids comminuting the inferior cortex.
-
Coracoid Tunnels:
Using a specific drill guide, a single tunnel or two separate tunnels are drilled through the base of the coracoid process, carefully avoiding the medial aspect where neurovascular structures lie. The drill path should be directed from superior to inferior, exiting the coracoid at its base. The ideal drill trajectory is often oblique, aiming for the inferomedial aspect of the coracoid base, about 1-1.5 cm from its tip. Confirm proper positioning with fluoroscopy to ensure the drill does not plunge or exit laterally or medially near neurovascular structures.
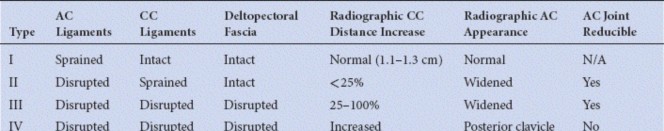

Figure 2: Intraoperative view depicting the drilling of tunnels through the clavicle and coracoid process for suture-button fixation. - Suture-Button Passage: Suture tapes (e.g., FiberTape) attached to cortical buttons are then passed through the drilled tunnels. One button is placed on the inferior aspect of the coracoid, and another on the superior aspect of the clavicle. For a double-button system, four suture limbs (two from each button) pass through the tunnels.
-
Tensioning and Fixation:
With the clavicle anatomically reduced, the sutures are sequentially tensioned and tied (or secured with adjustable loops) over the superior clavicular button(s). This compresses the clavicle towards the coracoid, reconstituting the CC space and providing vertical stability. The reduction should be assessed fluoroscopically and visually for anatomical alignment.

Figure 3: Post-operative radiograph showing anatomical reduction of the AC joint and stabilization with a suture-button construct for coracoclavicular ligament reconstruction.
AC Joint Stabilization (Optional Augmentation)
- Capsular Repair: The remnants of the AC joint capsule and torn AC ligaments (especially the superior AC ligament) are repaired with non-absorbable sutures to further enhance horizontal stability. This may involve drilling small tunnels through the clavicle and acromion or using suture anchors.
- Muscle Repair: The deltoid and trapezius muscles are meticulously reapproximated and repaired to their respective attachments on the clavicle and acromion. This is crucial for both functional recovery and to prevent loss of reduction.
Wound Closure
- Layered Closure: The muscle fascia is closed with absorbable sutures. Subcutaneous layers are reapproximated. The skin is closed with staples or absorbable sutures.
- Sterile Dressing: A sterile dressing is applied, and the arm is placed in a sling or shoulder immobilizer.
Complications & Management
Despite advancements in surgical techniques, AC joint reconstruction is not without potential complications. Recognizing these and implementing appropriate management strategies is crucial for long-term success.
Common Complications and Management
| Complication | Incidence (%) | Salvage Strategy / Management |
|---|---|---|
| Loss of Reduction / Re-dislocation | 5-20% |
- Revision surgery with stronger fixation (e.g., additional suture-buttons, allograft augmentation, AC plate).
- Address technical errors (e.g., inadequate tensioning, improper tunnel placement, premature mobilization). - For chronic cases, more robust reconstruction with graft. |
| Hardware Failure / Migration |
Suture-buttons: 2-10%
Hook plates: 10-30% |
- Suture-button breakage: Revision with new construct.
- Coracoid fracture (from button pull-through): Revision with larger coracoid washer, bone graft, or different fixation method. - Hook plate irritation/migration: Early removal if symptomatic, revision if loss of reduction. |
| Infection | 1-5% |
- Superficial: Oral antibiotics, local wound care.
- Deep: Surgical debridement, intravenous antibiotics, hardware removal (if necessary and stable joint). - Prophylactic antibiotics are standard. |
| Neurovascular Injury | <1% (but severe) |
- Brachial plexus injury: Careful dissection around coracoid, proper drill guide use, intraoperative nerve monitoring.
- Subclavian artery/vein injury: Immediate vascular surgery consultation, repair. - Supraclavicular nerve injury: Meticulous dissection in superficial layers, often sensory loss is permanent. |
| Persistent Pain | 5-25% |
- Rule out hardware irritation, loss of reduction, infection, degenerative AC joint changes.
- AC joint arthritis: Distal clavicle excision (Mumford procedure), typically after 6-12 months. - Nerve entrapment/irritation: Diagnostic injections, neurolysis. |
| Stiffness / Arthrofibrosis | 5-15% |
- Early and aggressive physical therapy.
- Manipulation under anesthesia. - Arthroscopic capsular release if conservative measures fail. |
| Heterotopic Ossification (HO) | 10-20% (radiographic), <5% (symptomatic) |
- Prophylaxis (NSAIDs, radiation therapy) for high-risk patients.
- Observation for asymptomatic HO. - Surgical excision if symptomatic and mature. |
| Coracoid Fracture | <1% (iatrogenic) |
- Prevention: Accurate drill guide usage, avoid overtightening sutures.
- If acute, often requires open reduction and internal fixation of coracoid, or revision to a different AC joint stabilization technique (e.g., AC plate) if CC fixation is compromised. |
| Distal Clavicle Osteolysis | Rare, but possible |
- Etiology debated (microtrauma, inflammatory response).
- Non-operative management with activity modification, NSAIDs. - If refractory symptoms, consider Mumford procedure (distal clavicle excision). |
Specific Considerations
- Chronic Injuries: In chronic AC joint separations, soft tissue scarring, contracture, and degenerative changes can make reduction difficult and increase the risk of re-dislocation. Augmentation with allograft (e.g., semitendinosus, gracilis) or autograft (e.g., coracoacromial ligament transfer - Weaver-Dunn modification) is often considered in conjunction with suture-button fixation to provide biological scaffolding and enhance long-term stability. The Mumford procedure (distal clavicle excision) may also be performed concurrently if significant AC joint arthritis is present.
- Hardware-Related Issues: Coracoclavicular hook plates, while providing rigid fixation, have a high incidence of local irritation, necessitating routine removal (usually at 3-6 months). Suture-button systems generally have lower rates of symptomatic hardware, but complications like suture breakage or coracoid tunnel enlargement can occur.
- Residual Deformity: Despite successful stabilization, some degree of residual superior clavicular prominence can persist, particularly in Type III injuries. Patients should be counseled on this pre-operatively.
Post-Operative Rehabilitation Protocols
A structured and progressive rehabilitation protocol is crucial for optimizing outcomes after AC joint reconstruction, facilitating ligament healing, restoring range of motion, and regaining strength and function while protecting the surgical repair. The protocol is typically divided into three phases.
Phase I: Protection & Early Motion (Weeks 0-6)
Goals:
* Protect the healing repair.
* Control pain and inflammation.
* Maintain passive range of motion (PROM) of glenohumeral joint.
* Prevent stiffness of elbow, wrist, hand.
Guidelines:
*
Immobilization:
Arm is kept in a sling or shoulder immobilizer for 4-6 weeks, with removal only for hygiene and exercises.
*
Elbow, Wrist, Hand ROM:
Active range of motion exercises for the elbow, wrist, and hand should begin immediately.
*
Pendulum Exercises:
Gentle pendulum exercises for the shoulder, without active muscle contraction, can be initiated around 1-2 weeks post-op, staying below shoulder height.
*
Passive Shoulder ROM:
Gentle passive external rotation (0-30 degrees), flexion (0-90 degrees), and abduction (0-90 degrees) may be initiated under therapist guidance around 2-3 weeks, with strict avoidance of cross-body adduction or AC joint compression. No resisted motion.
*
Scapular Mobilization:
Gentle scapular retraction and protraction exercises (non-weight bearing) to maintain scapulothoracic mobility.
*
Activity Restrictions:
No lifting, pushing, pulling, or active shoulder movements against resistance. Avoid sleeping on the operative side.
Phase II: Progressive Motion & Early Strengthening (Weeks 6-12)
Goals:
* Restore full passive and active range of motion.
* Initiate gentle strengthening.
* Improve neuromuscular control.
Guidelines:
*
Sling Discontinuation:
Gradual weaning from the sling at 6 weeks, as tolerated, with full discontinuation typically by 8 weeks.
*
Active Shoulder ROM:
Begin active-assisted range of motion (AAROM) and then active range of motion (AROM) exercises for all planes, gradually progressing towards full motion. Avoid pain.
*
Isometrics:
Initiate isometric strengthening for rotator cuff (internal/external rotation) and deltoid, with the arm at the side. Progress to isometric scapular stabilization exercises.
*
Light Resistance:
Begin light resistance exercises using elastic bands for internal/external rotation, scapular stabilizers (e.g., rows, scaption with light weight). Ensure proper form and controlled movements.
*
Cardiovascular:
Return to light cardiovascular activity (e.g., stationary bike, walking).
*
Activity Restrictions:
Continue to avoid heavy lifting, overhead activities, and activities that stress the AC joint (e.g., push-ups, dips). No contact sports.
Phase III: Advanced Strengthening & Return to Activity (Weeks 12+)
Goals:
* Maximize strength, power, and endurance.
* Restore functional capacity for sport and daily activities.
* Gradual and safe return to sport.
Guidelines:
*
Progressive Resistance:
Continue to advance resistance exercises for all major shoulder muscle groups (rotator cuff, deltoid, pectoralis, trapezius, serratus anterior). Incorporate eccentric strengthening.
*
Functional Training:
Begin sport-specific or occupation-specific exercises, focusing on movement patterns relevant to the patient's activities. This includes throwing mechanics, overhead reaching, carrying, pushing, and pulling.
*
Plyometrics:
For athletes, initiate plyometric exercises (e.g., medicine ball throws, catching drills) to improve power and dynamic stability, typically around 4-5 months post-op.
*
Return to Overhead Activities:
Gradual return to overhead activities and weighted lifting, provided the patient has achieved full, pain-free ROM and adequate strength.
*
Return to Contact Sports:
Full return to contact sports or heavy manual labor is typically allowed no earlier than 6 months post-operatively, often closer to 9-12 months, depending on the individual's recovery, strength, and confidence, and after clinical and functional assessment confirms adequate healing and stability.
*
Long-Term Maintenance:
Encourage ongoing home exercise program to maintain strength and flexibility.
Key Precautions Throughout Rehabilitation:
* Avoid direct pressure on the AC joint.
* Listen to pain: Pain is a guide; exercises should be pain-free.
* Avoid overstretching or aggressive manipulation.
* Strict adherence to the prescribed activity restrictions is critical to prevent hardware failure or loss of reduction.
Summary of Key Literature / Guidelines
The management of AC joint separations has evolved significantly, particularly with regard to Type III injuries and advanced fixation techniques. Current literature provides a foundation for evidence-based decision-making.
-
Rockwood Type III Management: The ongoing debate surrounding operative versus non-operative treatment for Type III AC joint separations is a prominent theme in the literature.
- Meta-analyses and Systematic Reviews: Several reviews have generally shown no significant long-term difference in functional outcomes (e.g., ASES, Constant scores) between operative and non-operative management for Type III injuries. However, operative treatment often leads to better cosmetic outcomes and potentially earlier return to demanding activities, albeit with higher complication rates. Non-operative management typically involves initial immobilization followed by progressive rehabilitation, with good results reported for a majority of patients.
- Patient Selection: The trend in recent guidelines emphasizes individualized treatment for Type III injuries, considering patient age, activity level, occupation, hand dominance, and subjective symptoms. High-demand overhead athletes or manual laborers may benefit from early surgical intervention, while sedentary individuals may fare well with conservative management.
- Chronic Type III: For chronic Type III separations with persistent symptoms, surgical reconstruction is generally favored over conservative treatment.
-
Surgical Techniques:
-
Coracoclavicular (CC) Ligament Reconstruction:
This has become the cornerstone of most surgical approaches for higher-grade AC joint separations (Types III-VI).
- Suture-Button Systems: Meta-analyses indicate that modern suture-button constructs (e.g., using FiberTape and cortical buttons) for CC ligament reconstruction offer comparable or superior clinical outcomes and lower hardware-related complications compared to traditional methods like hook plates or K-wires, especially regarding hardware removal rates. They provide dynamic stabilization, allowing for micromotion conducive to biological healing.
- Hook Plates: While providing rigid fixation, hook plates are associated with higher rates of hardware irritation, requiring secondary removal. They are still an option for certain complex fractures or as temporary stabilization.
- Allograft/Autograft Augmentation: For chronic AC separations, revision cases, or when primary ligamentous tissue is severely compromised, augmentation with autograft (e.g., semitendinosus) or allograft is often recommended to provide biological stability and improve long-term outcomes. The Weaver-Dunn procedure (coracoacromial ligament transfer) is a historical example of a biological augmentation technique, often modified with CC fixation.
- AC Joint Fixation: Direct AC joint stabilization (capsular repair, AC plates) is often performed in conjunction with CC ligament reconstruction, especially for acute injuries, to restore horizontal stability. However, rigid AC fixation alone has largely been abandoned due to high failure and complication rates.
-
Coracoclavicular (CC) Ligament Reconstruction:
This has become the cornerstone of most surgical approaches for higher-grade AC joint separations (Types III-VI).
-
Complications: Surgical fixation carries a notable risk of complications, including loss of reduction, hardware failure/migration, infection, and persistent pain. Recent studies highlight that while surgical outcomes are often favorable, the rate of re-operation or complications can be substantial. Thorough pre-operative counseling regarding these risks is critical.
-
Rehabilitation: Evidence-based rehabilitation protocols emphasize early passive motion, followed by progressive active motion and strengthening, while protecting the repair. Gradual return to activity, with specific attention to overhead and contact sports, is paramount. Outcomes are highly dependent on patient adherence to these protocols.
-
Long-Term Outcomes: Long-term studies indicate that many patients achieve satisfactory functional outcomes after both operative and non-operative treatment of AC joint injuries. However, there is a risk of developing AC joint arthrosis in the long term, regardless of the initial treatment, particularly in Type II and III injuries. Distal clavicle excision (Mumford procedure) may be necessary for symptomatic arthrosis.
In summary, the literature supports a nuanced, patient-centered approach to AC joint separation management, with Rockwood Type I/II favoring non-operative care, Type IV/V/VI necessitating surgery, and Type III management guided by patient-specific factors. Modern suture-button techniques for CC ligament reconstruction have emerged as a preferred surgical option due to favorable outcomes and reduced hardware-related complications. Continued research is focused on refining surgical techniques, optimizing graft integration, and improving long-term outcomes while minimizing complications.
Clinical & Radiographic Imaging

