INTRODUCTION TO RHEUMATOID UPPER EXTREMITY SURGERY
Rheumatoid arthritis (RA) is a systemic, autoimmune, inflammatory polyarthritis characterized by chronic synovitis that leads to progressive joint destruction, tendon rupture, and severe biomechanical deformity. While the advent of disease-modifying antirheumatic drugs (DMARDs) and biologic therapies has drastically altered the natural history of the disease, surgical intervention remains a critical component in the management of structural failures, intractable pain, and functional deficits.
Operating on the rheumatoid patient requires a holistic, multidisciplinary approach. The surgeon must look beyond the isolated deformity and evaluate the entire kinematic chain, the patient’s systemic medical status, and their functional demands. This masterclass details the surgical management of rheumatoid nodules and the complex, hierarchical decision-making process required for staging multiple operations in the rheumatoid patient.
RHEUMATOID NODULES
Rheumatoid subcutaneous nodules are pathognomonic extra-articular manifestations of rheumatoid arthritis, occurring in approximately 20% to 30% of seropositive patients. Histologically, they are characterized by a central zone of fibrinoid necrosis surrounded by a palisading layer of histiocytes and an outer zone of chronic inflammatory cells.
Clinical Presentation and Anatomic Distribution
Nodules predominantly develop in areas subjected to repeated mechanical pressure or friction. In the upper extremity, the most common locations include:
* The olecranon bursa and the extensor surface of the elbow.
* The subcutaneous border of the proximal ulna.
* The dorsum of the hand and metacarpophalangeal (MCP) joints.
* The palmar surface of the fingers (often intimately associated with the flexor tendon sheath).
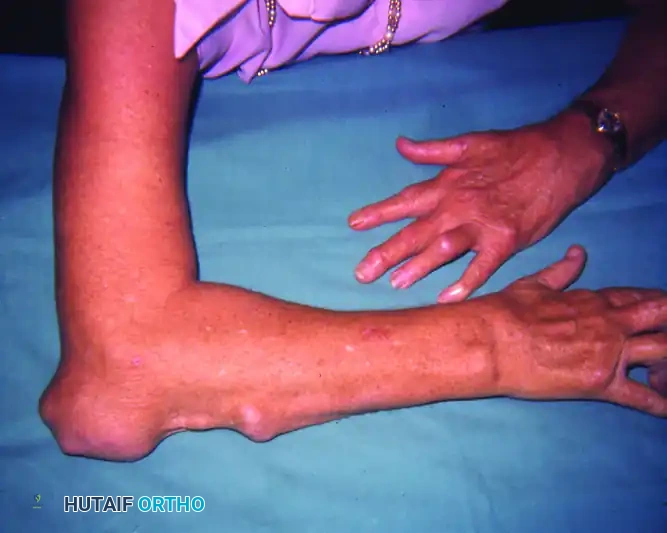
While many nodules remain asymptomatic, they can grow to a substantial size, leading to significant clinical challenges. Large nodules on the palmar aspect of the digits can cause mechanical blocks to finger flexion. Nodules over the olecranon or ulnar border can become exquisitely tender, cosmetically unacceptable, or, most concerningly, undergo skin breakdown leading to chronic ulceration and secondary bacterial infection.
Indications for Surgical Excision
Surgical excision of rheumatoid nodules is not indicated for purely cosmetic reasons in the asymptomatic patient, as recurrence rates are notoriously high. However, operative intervention is strongly indicated in the following scenarios:
1. Impending or Frank Ulceration: To prevent deep space infections or septic bursitis.
2. Mechanical Impingement: When palmar nodules restrict digital range of motion or grip.
3. Intractable Pain: Particularly over pressure points like the olecranon during activities of daily living (ADLs).
4. Neurological Compression: When nodules compress adjacent peripheral nerves (e.g., ulnar nerve at the cubital tunnel).
Clinical Pearl: Always evaluate the skin integrity overlying a rheumatoid nodule. The skin is often atrophic, tethered, and poorly vascularized. Aggressive excision without a plan for soft tissue reconstruction can lead to disastrous wound healing complications.
Surgical Technique and Considerations
The excision of rheumatoid nodules requires meticulous surgical technique, respecting the fragile soft tissue envelope characteristic of the rheumatoid patient.
1. Preoperative Planning and Positioning:
* The procedure is typically performed under regional anesthesia (e.g., axillary or supraclavicular block) with a proximal pneumatic tourniquet.
* For olecranon nodules, the patient may be positioned supine with the arm draped across the chest, or in the lateral decubitus position.
2. Incision and Dissection:
* Incision Placement: Avoid placing incisions directly over the apex of the nodule or the point of maximal pressure. For olecranon nodules, a lateral or medial curvilinear incision is preferred to keep the scar off the weight-bearing surface of the elbow.
* Neurovascular Protection: Large nodules are frequently adherent to underlying neurovascular structures. In the elbow, the ulnar nerve must be identified and protected, as it may be displaced or tethered by the inflammatory mass. In the digits, the neurovascular bundles must be carefully dissected free from palmar nodules using loupe magnification.
* Bursal Excision: For olecranon nodules, a complete bursectomy is often required. The deep margin must be excised down to healthy triceps fascia or periosteum.
3. Soft Tissue Management and Closure:
* Skin Excision: Elliptical excision of the thinned, non-viable skin directly overlying the nodule is often necessary.
* Dead Space Management: Meticulous hemostasis is critical. Obliterate dead space using deep dermal sutures to prevent postoperative hematoma, which serves as a nidus for infection and delayed healing.
* Grafting and Flaps: If primary closure cannot be achieved without excessive tension, local rotational flaps or skin grafting (split-thickness or full-thickness) must be utilized. A tension-free closure is paramount in the rheumatoid patient.
4. Postoperative Protocol:
* The extremity is immobilized in a bulky, well-padded splint for 10 to 14 days to allow for primary wound healing and to prevent hematoma formation.
* Sutures are left in place longer than usual (typically 14-21 days) due to the delayed wound healing associated with RA and systemic corticosteroid use.
STAGING OF OPERATIONS IN RHEUMATOID ARTHRITIS
The surgical management of the rheumatoid patient is rarely a single-event endeavor. Patients frequently present with polyarticular involvement, requiring a strategic, staged approach to reconstruction. The overarching goal is to maximize functional independence, alleviate pain, and prevent irreversible structural damage.
Global Surgical Priorities
When evaluating a patient with widespread rheumatoid disease, the surgeon must prioritize interventions based on a strict hierarchy. The extent to which pain limits function is given the highest priority. However, biomechanical dependencies dictate the sequence of operations.
The globally accepted descending order of surgical priority is:
1. Cervical Spine
2. Foot and Ankle
3. Hip
4. Knee
5. Wrist
6. Shoulder
7. Thumb
8. Elbow
9. Fingers
Surgical Warning: The cervical spine must be evaluated in EVERY rheumatoid patient prior to any surgical intervention. Atlantoaxial subluxation or basilar invagination can lead to catastrophic spinal cord injury during endotracheal intubation. Flexion-extension cervical radiographs are mandatory. If instability is present, cervical spine stabilization takes absolute precedence over all other orthopedic procedures.
The Rationale for Proximal-to-Distal and Lower-to-Upper Staging
Lower Extremity Before Upper Extremity:
Patients with severe RA often require ambulatory aids (canes, walkers, or crutches) during the rehabilitation phase of lower extremity surgery. If the hands and wrists are reconstructed first, the subsequent weight-bearing demands placed on these newly reconstructed small joints during lower extremity rehabilitation can lead to catastrophic failure of the upper extremity arthroplasties or fusions. Therefore, the lower extremities (hips, knees, feet) should generally be reconstructed to provide a stable, pain-free base of support before addressing the upper extremities.
Note: If upper extremity surgery is performed first, platform or forearm crutches must be provided to bypass the hands and wrists during weight-bearing.
Proximal Before Distal (Upper Extremity):
Within the upper extremity, the shoulder and elbow serve to position the hand in space. Correcting significant disease and deformity in the shoulder and elbow must precede hand and wrist reconstruction. A perfectly reconstructed hand is functionally useless if a stiff, painful shoulder or elbow prevents the patient from bringing the hand to their mouth or perineum.
PRIORITIZATION WITHIN THE HAND AND WRIST
When multiple operations are indicated on a single hand, the order of priority is dictated by the risk of irreversible damage and the biomechanical foundation of the hand.
High-Priority Soft Tissue Procedures
Prophylactic soft tissue procedures take precedence over reconstructive joint procedures because they prevent catastrophic loss of function.
* Persistent Tenosynovitis: Chronic dorsal tenosynovitis can invade and rupture extensor tendons (Vaughan-Jackson syndrome). Early extensor tenosynovectomy is highly effective and prevents tendon rupture.
* Tendon Rupture: Acute tendon ruptures require immediate surgical attention (tendon transfers or grafts) before muscle contracture and joint stiffness occur.
* Nerve Compression: Severe carpal tunnel syndrome or cubital tunnel syndrome secondary to proliferative synovitis requires urgent decompression to prevent irreversible neuropathy and intrinsic muscle wasting.
The Wrist: The Keystone of Hand Function
In general, when wrist arthroplasty or arthrodesis is indicated, it must be performed first. The wrist is the foundational joint of the hand; its position determines the resting tension and balance of the extrinsic digital flexor and extensor tendons.
A classic rheumatoid deformity involves carpal ulnar translocation and radial deviation of the metacarpals. This radial deviation of the wrist creates a secondary, zigzag biomechanical force that drives the MCP joints into ulnar drift. Attempting to correct MCP ulnar drift with arthroplasty while leaving a radially deviated wrist uncorrected will result in rapid recurrence of the MCP deformity.
Clinical Pearl: Never perform an MCP joint arthroplasty in the presence of an unstable, radially deviated wrist. The wrist must be stabilized (via partial/total arthrodesis or arthroplasty) to provide a neutral, stable foundation before addressing the digits.
At the time of wrist surgery, an additional procedure, such as arthrodesis of the MCP joint of the thumb, may be performed safely. However, more extensive, multi-level surgery is usually best delayed to prevent excessive surgical trauma and prolonged tourniquet times.
Souter's Grading of Surgical Procedures
W.A. Souter developed a highly regarded classification system that groups rheumatoid hand and wrist procedures based on their predictability, effectiveness, and likelihood of long-term success. Souter recommended starting with a procedure that is highly likely to succeed (Group I) to build patient confidence, often beginning with the least involved hand.
GROUP I: Most Effective and Predictable
* Fusion of the Thumb MCP Joint: Provides a stable post for pinch and grip. Highly predictable with excellent patient satisfaction.
* Extensor Synovectomy and Darrach Procedure: Excision of the distal ulna (Darrach) combined with dorsal tenosynovectomy eliminates pain from the distal radioulnar joint (DRUJ), restores forearm rotation, and prevents extensor tendon rupture (caput ulnae syndrome).
GROUP II: Highly Effective
* Flexor Synovectomy: Relieves trigger digits, improves active flexion, and prevents flexor tendon rupture within the fibro-osseous canals.
* MCP Joint Arthroplasty: Silicone implant arthroplasty (e.g., Swanson implants) at the MCP level reliably relieves pain, corrects ulnar drift, and improves the cosmetic appearance and function of the hand.
GROUP III: Moderately Effective
* PIP Joint Fusion: Arthrodesis of the proximal interphalangeal (PIP) joint in a functional position is a reliable salvage procedure for severe fixed deformities, providing stability at the expense of motion.
* Wrist Stabilization: Total wrist arthrodesis provides absolute pain relief and a stable foundation, though it sacrifices all radiocarpal motion.
GROUP IV: Less Predictable Outcomes
* Swan-Neck Correction: Soft tissue reconstructions for swan-neck deformities (PIP hyperextension, DIP flexion) are technically demanding and prone to stretching out over time.
* MCP and PIP Joint Synovectomy: While effective for pain relief in early disease, isolated synovectomy without joint reconstruction in the presence of cartilage damage has a high rate of recurrence.
* Thumb IP Joint Fusion: Effective for instability, but loss of terminal thumb flexion can hinder fine motor tasks.
GROUP V: Least Effective / Highest Failure Rate
* PIP Joint Arthroplasty: Surface replacement or silicone arthroplasty at the PIP level has a high complication rate, including implant fracture, subsidence, and recurrent deformity, due to the complex biomechanical forces across the joint.
* Boutonnière Correction: Reconstructing the central slip and lateral bands in a chronic rheumatoid boutonnière deformity is notoriously difficult, with a high rate of recurrent stiffness or deformity.
PERIOPERATIVE MANAGEMENT AND REHABILITATION
Bilateral vs. Unilateral Surgery
Frequently, a patient with rheumatoid arthritis requires surgery on both hands. Usually, surgery is performed on only one hand at a given time. Operating on both hands simultaneously severely compromises the patient's ability to perform independent activities of daily living (ADLs), personal hygiene, and feeding. Staging the contralateral hand 3 to 6 months later allows the first hand to rehabilitate and serve as the "helper" hand during the second recovery phase.
Medical Management (DMARDs and Biologics)
The perioperative management of systemic medications requires close coordination with the patient's rheumatologist.
* Methotrexate: Current evidence suggests that continuing Methotrexate perioperatively is safe and does not increase infection rates, while preventing disease flare-ups.
* Biologic Agents (e.g., TNF-α inhibitors): These agents significantly impair the immune response. Standard protocol dictates withholding biologic therapy for 1 to 2 dosing cycles prior to surgery, and resuming them 10 to 14 days postoperatively, provided the wound is healing well and there is no evidence of infection.
* Corticosteroids: Patients on chronic systemic corticosteroids may require perioperative stress-dose steroids to prevent adrenal crisis.
