INTRODUCTION AND BIOMECHANICAL PRINCIPLES
Retrograde femoral nailing has evolved into an indispensable technique in the armamentarium of the orthopedic trauma surgeon. Initially popularized for the management of supracondylar femur fractures, its indications have expanded significantly to include diaphyseal fractures, particularly in the setting of polytrauma, morbid obesity, ipsilateral pelvic or acetabular fractures, and the classic "floating knee" injury.
Biomechanically, intramedullary nailing offers a load-sharing construct that aligns the mechanical axis of the femur more anatomically than laterally based plate constructs. The retrograde approach specifically bypasses the complex anatomy of the hip abductor musculature, thereby eliminating the risk of iatrogenic superior gluteal nerve injury and postoperative abductor weakness—a well-documented complication of antegrade nailing. However, the retrograde trajectory introduces its own unique biomechanical challenges, most notably the "bell-clapper" effect within the wide distal femoral metaphysis, which can lead to coronal and sagittal plane malalignment if not meticulously managed with precise entry point selection and the strategic use of blocking (Poller) screws.
INDICATIONS AND PREOPERATIVE PLANNING
Careful patient selection and preoperative templating are critical for the success of retrograde femoral nailing.
Primary Indications
- Distal Third Femoral Shaft Fractures (OTA/AO 32): Ideal for fractures where antegrade nailing would result in a short distal segment with inadequate fixation.
- Supracondylar Femur Fractures (OTA/AO 33-A and select 33-C): Extra-articular or simple intra-articular fractures that can be anatomically reduced prior to nail insertion.
- Floating Knee Injuries: Ipsilateral femoral and tibial shaft fractures can be addressed through a single knee incision, minimizing operative time and patient repositioning.
- Morbid Obesity: The retrograde approach avoids the massive soft tissue envelope of the proximal thigh and buttock, simplifying the entry portal and reducing operative time.
- Ipsilateral Pelvic/Acetabular Fractures: Allows simultaneous or sequential fixation without compromising the surgical approach to the pelvis.
- Pregnancy: Minimizes radiation exposure to the abdomen and pelvis during fluoroscopy.
Preoperative Templating
Orthogonal radiographs of the entire femur, including the hip and knee joints, are mandatory. Templating must assess the isthmic diameter to determine the appropriate reamer and nail size, and evaluate the anterior bow of the femur. The radius of curvature of the selected nail must closely match the patient's native anatomy to prevent anterior cortical penetration or iatrogenic fracture during insertion.
PATIENT POSITIONING AND SETUP
Optimal positioning is the foundation of a successful retrograde nailing procedure. While a fracture table can be used, the supine position on a radiolucent flattop table is overwhelmingly preferred in modern orthopedic trauma surgery.
The Flattop Radiolucent Table Technique
Place the patient supine on a fully radiolucent operating table. A small bolster is positioned under the ipsilateral hip to prevent external rotation of the proximal femur, bringing the patella to a neutral, anterior-facing position. Surgical preparation and draping must be extensive, encompassing the entire lower extremity from the hip girdle and lower flank down to the toes, allowing for unrestricted manipulation of the limb.
Position the knee over a sterile bump or radiolucent triangle to maintain approximately 30 to 50 degrees of knee flexion. This degree of flexion is critical; it relaxes the deforming force of the gastrocnemius muscle on the distal fragment (which typically causes an apex posterior deformity) and provides a clear trajectory for the instruments to clear the patella.
Clinical Pearl: If manual traction is insufficient for length restoration, a tibial traction pin and traction bow can be inserted into the proximal tibia. This serves as a powerful "joystick" and handle for exacting control of the distal segment during reduction maneuvers.
SURGICAL APPROACH AND ENTRY PORTAL
The Incision and Arthrotomy
Make a 3 to 5 cm incision centered over the knee. The approach can be a lateral parapatellar, medial parapatellar, or transpatellar tendon splitting incision, largely dictated by surgeon preference and the presence of concurrent injuries.
* Medial Parapatellar: Often preferred as it provides excellent visualization of the intercondylar notch and avoids the patellar tendon entirely.
* Transpatellar Tendon: Provides a direct, inline trajectory to the medullary canal but carries a theoretical risk of postoperative anterior knee pain or tendon pathology.
Regardless of the approach, the retropatellar fat pad must be incised or retracted, and a formal arthrotomy performed to visualize the articular surface and the intercondylar notch.
Establishing the Entry Point
The accuracy of the entry point dictates the final alignment of the fracture.
1. Insert a 3.2-mm threaded guidewire into the intercondylar notch.
2. Anteroposterior (AP) Imaging: The pin must be directed centrally into the medullary canal, perfectly bisecting the medial and lateral femoral condyles.
3. Lateral Imaging: Confirm the trajectory. The pin placement should be exactly in line with the medullary canal, positioned at the anterior extent of Blumensaat’s line.
Surgical Warning: An entry point that is too anterior will result in a flexion deformity of the distal fragment and potential damage to the patellofemoral articulation. An entry point that is too posterior risks injury to the posterior cruciate ligament (PCL) origin and can cause an extension deformity.
CANAL PREPARATION AND REAMING
Once the guidewire is perfectly positioned, advance it into the distal femoral metaphysis.
- Soft Tissue Protection: It is absolutely mandatory to place a soft tissue protection sleeve over the guidewire. This sleeve protects the articular cartilage of the patella, the trochlear groove, and the patellar tendon from the catastrophic iatrogenic damage that can be caused by the reamer flutes.
- Entry Portal Creation: A multiple-pin "honeycomb" insert can be used over the initial guidewire to fine-tune the entry point if the initial wire is slightly off-center. Once satisfied, remove the honeycomb and pass a cannulated entry reamer (typically 12mm to 13mm) over the guidewire.
- Advancement: Advance the entry reamer into the distal femur, taking special care to maintain the soft tissue protection sleeve firmly against the bone.
Fracture Reduction and Guidewire Passage
Remove the entry reamer and insert a 3-mm bead-tipped (ball-tipped) guidewire.
Reduce the fracture using manual traction, external distractors, or percutaneous joysticks (Schanz pins). Small bumps or bolsters placed along the posterior surface of the thigh can correct sagittal plane malalignment. Once reduced, advance the bead-tipped guidewire across the fracture site and into the proximal segment, terminating at the level of the lesser trochanter.
Pitfall: Ensure the guidewire does not inadvertently enter the femoral neck, which can occur if the wire is advanced too proximally in a femur with a wide proximal metaphysis.
Intramedullary Reaming
Prepare the medullary canal by introducing flexible cannulated reamers over the bead-tipped guidewire. Reaming should be performed sequentially in 0.5-mm increments. The canal should be reamed to a diameter 1.0 to 1.5 mm larger than the anticipated diameter of the selected intramedullary nail. This over-reaming prevents nail incarceration and reduces the hoop stresses generated during nail insertion, which could otherwise propagate iatrogenic fractures.
NAIL INSERTION AND PROXIMAL ADVANCEMENT
After reaming, recheck the position of the guidewire to confirm it remains at the level of the lesser trochanter. Apply axial traction to the leg to ensure proper length is restored.
Measure for the appropriate length of the nail using a radiopaque ruler placed over the guidewire. Ensure the ruler is countersunk to the exact depth you intend to seat the nail (typically 2-3 mm below the articular cartilage). This measurement is most accurately performed on the lateral fluoroscopic image.
Remove the entry portal tool and attach the selected retrograde nail to the targeting guide. Insert the nail over the guidewire. Advance the nail using gentle, controlled mallet strikes until it is seated at the level of the lesser trochanter proximally.
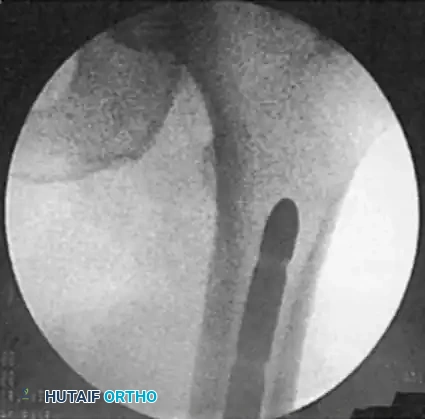
Maintain continuous traction on the leg during insertion to avoid acute shortening of the fracture. Check the lateral fluoroscopic image of the knee to ensure the distal end of the nail is properly countersunk beneath the articular cartilage to prevent patellofemoral impingement. Once the nail is at the proper level, the bead-tipped guidewire is removed.
INTERLOCKING AND FINAL REDUCTION CHECKS
Distal Interlocking
Distal locking is performed first using the targeting guide attached to the nail insertion handle.
1. Insert the drill sleeve and trocar through the targeting guide to dimple the skin.
2. Make a stab incision and enlarge the tract with blunt dissection down to the bone to protect the genicular arteries and articular capsule.
3. Reinsert the drill guide to the bone. Drill through both cortices.
4. Read the measurement directly off the calibrated drill bit to determine screw length.
5. Insert the interlocking screws by hand until fully seated. Confirm length and position with AP and lateral fluoroscopy.
Proximal Interlocking (Perfect Circle Technique)
Before proximal locking, recheck the overall alignment and length of the femur. A Bovie cord can be stretched from the anterior superior iliac crest, over the middle of the patella, to the middle of the tibial plafond to confirm the mechanical axis.
Proximal locking is performed freehand using the "perfect circle" technique.
1. Position the fluoroscope in the true AP plane at the level of the lesser trochanter. Adjust the C-arm until the locking hole in the nail appears as a perfect circle.
2. Make a longitudinal skin incision over the lateral thigh at this level. Sharply divide the fascia lata and bluntly dissect the vastus lateralis to the bone.
3. Using a radiolucent drill drive, align the drill tip precisely in the center of the perfect circle. Drill through the lateral cortex, pass through the nail hole, and penetrate the medial cortex.
4. Measure the depth and place the interlocking screw using a captured screwdriver.
Critical Step: Always image the hip in full fluoroscopic mode with internal/external rotation and push-pull maneuvers to rule out an occult ipsilateral femoral neck fracture, which occurs in up to 5-8% of high-energy femoral shaft fractures.
POSTOPERATIVE CARE AND REHABILITATION
Postoperative rehabilitation is highly individualized, depending heavily on the fracture pattern, the stability of the fixation, and the patient's overall polytrauma status.
- Immobilization: Patients are initially placed in a knee immobilizer to protect the soft tissues and the arthrotomy site.
- Range of Motion: For stable diaphyseal fractures, a continuous passive motion (CPM) program or active-assisted range of motion is initiated within the first 24 to 48 hours to prevent knee stiffness.
- Weight Bearing:
- Stable Diaphyseal Fractures: Often permitted weight-bearing as tolerated (WBAT) immediately postoperatively.
- Comminuted, Intercondylar, or Supracondylar Fractures: Require protected, toe-touch weight bearing (TTWB) until radiographic evidence of callus formation is observed, typically advancing weight bearing between 10 and 12 weeks.
ERRORS, PITFALLS, AND COMPLICATIONS
Despite excellent union rates, retrograde femoral nailing is associated with specific complications that require meticulous surgical technique to avoid.
Knee Pain and Intra-articular Pathology
The most frequently reported complication is postoperative knee pain, occurring in up to 30-40% of patients. This is often multifactorial, stemming from:
* Prominent nail hardware impinging on the patellofemoral joint (failure to countersink).
* Iatrogenic damage to the articular cartilage during reaming (failure to use a soft tissue sleeve).
* Inadequate closure of the arthrotomy or fat pad fibrosis.
Malalignment and the "Bell-Clapper" Effect
In fractures involving the wide distal femoral metaphysis, the intramedullary nail is significantly smaller than the canal diameter. This canal-nail mismatch allows the distal fragment to toggle around the nail (the bell-clapper effect), leading to varus/valgus or flexion/extension malunions.
* Solution: The use of blocking screws (Poller screws) placed adjacent to the nail in the wide metaphysis effectively narrows the canal, creating an artificial cortex that forces the nail into the center of the fragment, ensuring anatomic alignment.
Neurologic Complications
While retrograde nailing avoids the superior gluteal nerve, patient positioning can lead to other nerve palsies. If a fracture table is utilized and excessive traction is applied against a perineal post, pudendal nerve palsy can occur. Similarly, prolonged traction in a well-leg holder can result in compartment syndrome or peroneal nerve palsy of the uninjured leg. The flattop table technique with manual traction largely mitigates these risks.
Bent or Broken Nails
Intramedullary nails are load-sharing devices designed to withstand physiologic stresses until bone union occurs. However, delayed union, nonunion, or premature weight-bearing in highly comminuted fractures can subject the nail to fatigue failure.
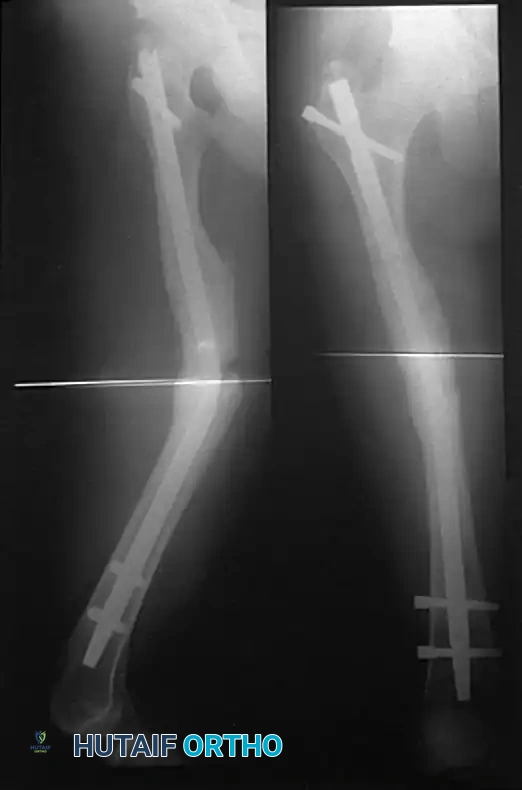
A bent nail usually indicates an injudicious act on the part of the patient (e.g., early unprotected weight-bearing) or the selection of an undersized nail.
* Management: A bent nail is not an indication for closed manipulation, as this will only further weaken the metal and lead to catastrophic breakage. The bent nail must be extracted and exchanged for a larger, stiffer nail.
* Broken Nail Extraction: If the nail breaks, the distal half is easily removed via the knee arthrotomy. The proximal half requires a separate lateral thigh incision. A ball-tipped guidewire is passed through the cannulation of the retained proximal segment, and specialized extraction hooks or jammed guidewires are used to back the broken segment out of the canal.
Nail Incarceration
A nail that is larger than the prepared medullary canal may become firmly incarcerated during insertion, resisting all efforts to drive it further or extract it. This is a severe complication resulting from inadequate preoperative templating or insufficient reaming.
* Prevention: Always ream 1.0 to 1.5 mm larger than the selected nail diameter.
* Rescue Technique: If incarceration occurs, a small incision is made laterally at the level of the jam. Two 5- to 6-mm holes are drilled in the lateral cortex 3 to 4 cm apart and connected with an osteotome to relieve the cortical tension, allowing the nail to be withdrawn.
By adhering to strict biomechanical principles, meticulous entry point localization, and proactive complication management, retrograde femoral nailing provides a robust, reliable, and highly successful method for the stabilization of complex femoral fractures.
📚 Medical References
- retrograde femoral nailing and unreamed tibial nailing, J Orthop Trauma 10:309, 1996.
- Gregory P, Sanders R: The treatment of supracondylar-intracondylar fractures of the femur using the dynamic condylar screw, Tech Orthop 9:195, 1995.
- Grosse A: Manual for osteosynthesis for femoral and tibial shaft fractures, Kiel, Germany, 1981, Howmedica International. Grosse A, Kempf I, Lafforgued D: Le traitement des fracas, pertes de substance osseuse et pseudoarthroses du fémur et du tibia par l’enclouage verrouillé (a propos de 40 case), Rev Chir Orthop 64(suppl 2):33, 1978.
- Grover J, Wiss DA: A prospective study of fractures of the femoral shaft treated with a static, intramedullary, interlocking nail comparing one versus two distal screws, Orthop Clin North Am 26:139, 1995.
- Grundy M: Fractures of the femur in Paget’s disease of bone: their etiology and treatment, J Bone Joint Surg 52B:252, 1970.
- Gustilo RB, Anderson JT: Prevention of infection in the treatment of one thousand and twenty-fi ve open fractures of long bones, J Bone Joint Surg 58A:453, 1976.
- Gynning JB, Hansen D: Treatment of distal femoral fractures with intramedullary supracondylar nails in elderly patients, Injury 30:43, 1999.
- Hall RM: Freehand technique, Smith & Nephew technique manual for Russell-Taylor Nail System, 1997, Smith & Nephew, Memphis, Tenn. Halpenny J, Rorabeck CH: Supracondylar fractures of the femur: results of treatment of 61 patients, Can J Surg 27:606, 1984.
- Hammacher ER, van Meeteren MC, van der Werken C: Improved results in treatment of femoral shaft fractures with the unreamed femoral nail? A multicenter experience, J Trauma 45:517, 1998.
- Hanks GA, Foster WC, Cardea JA: Treatment of femoral shaft fractures with the Brooker-Wills interlocking intramedullary nail, Clin Orthop Relat Res 226:206, 1988.
- Hansen ST, Winquist RA: Closed intramedullary nailing of fractures of the femoral shaft, II: technical considerations, Instr Course Lect 27:90, 1978.
- Hansen ST, Winquist RA: Closed intramedullary nailing of the femur: Küntscher technique with reaming, Clin Orthop Relat Res 138:56, 1979.
- Hansson LI, Cedar L, Svensson K, et al: Incidence of fractures of the distal radius and proximal femur: comparison of patients in a mental hospital and the general population, Acta Orthop Scand 53:721, 1982.
- Harder Y, Martinet O, Barraud GE, et al: The mechanics of internal fi xation of fractures of the distal femur: a comparison of the condylar screw (CS) with the condylar plate (CP), Injury 30:A31, 1999.
- Hardy AE: The treatment of femoral fractures by cast-brace application and early ambulation, J Bone Joint Surg 65A:56, 1983.
- Harris LJ: Condylocephalic nailing of proximal femoral fractures, Instr Course Lect 32:292, 1983.
- Harryman DT II, Kurth LA, Davis CM: Ipsilateral femoral neck and shaft fractures: report of two cases using an alternate technique, Clin Orthop Relat Res 213:183, 1986.
- Healy WL, Brooker AF Jr: Distal femoral fractures: comparison of open and closed methods of treatment, Clin Orthop 174:166, 1983.
- Helal B, Skevis X: Unrecognized dislocation of the hip in fractures of the femoral shaft, J Bone Joint Surg 49B:293, 1967.
- Hemple D: Interlocking nail osteosynthesis. In Hemple D: Intramedullary nailing, New York, 1982, Thieme, Stratton. Henry SL, Booth RE Jr: Management of supracondylar fractures above total knee prostheses, Tech Orthop 9:243, 1994.
- Henry SL, Seligson D: Management of supracondylar fractures of the femur with the GHS supracondylar nail: the percutaneous technique, Tech Orthop 9:189, 1995.
- Herscovici D, Whiteman KW: Retrograde nailing of the femur using an intercondylar approach, Clin Orthop Relat Res 332:98, 1996.
- Hershman EB, Lombardo J, Bergfeld JA: Femoral shaft stress fractures in athletes, Clin Sports Med 9:111, 1990.
- Hossam E, Morsey A, Eid E: Ipsilateral fracture of the femoral neck and shaft, treated by reconstruction interlocking nail, Arch Orthop Trauma Surg 121:71, 2001.
- Hutson JJ Jr: Reconstruction of distal intercondylar femoral fractures with limited internal fi xation and Ilizarov tensioned-wire external fi xation, Tech Orthop 11:182, 1996.
- Hutson JJ Jr, Zych GA: Treatment of comminuted intraarticular distal femur fractures with limited internal and external tensioned wire fi xation, J Orthop Trauma 14:405, 2000.
- Iannacone WM, Bennett FS, DeLong WG Jr, et al: Initial experience with treatment of supracondylar femoral fractures using the supracondylar intramedullary nail: a preliminary report, J Orthop Trauma 8:322, 1994.
- Ingram AJ, Turner TC: Bilateral traumatic posterior dislocation of the hip complicated by bilateral fracture of the femoral shaft: report of a case, J Bone Joint Surg 36A:1249, 1954.
- Ito K, Grass R, Zwipp H: Internal fi xation of supracondylar femoral fractures: comparative biomechanical performance of the 95-degree blade plate and two retrograde nails, J Orthop Trauma 12:259, 1998.
- Jaarsma RL, Pakvis DFM, Verdonschot N, et al: Rotational malalignment after intramedullary nailing of femoral fractures, J Orthop Trauma 18:403, 2004.
- Jakobsen J, Christensen KS, Rasmussen OS: Patellectomy—a 20-year follow-up, Acta Orthop Scand 56:430, 1985.
- Janzing HM, Vaes F, Van Damme G, et al: Treatment of distal femoral fractures in the elderly: results with the retrograde intramedullary supracondylar nail, Unfallchir 24:55, 1998.
- Jazrawi LM, Kummer FJ, Simon JA, et al: New technique for treatment of unstable distal femur fractures by locked doubleplating: case report and biomechanical evaluation, J Trauma 48:87, 2000.
- Johnson KD, Johnston DWC, Parker B: Comminuted femoralshaft fractures: treatment by roller traction, cerclage wires and an intramedullary nail, or an interlocking intramedullary nail, J Bone Joint Surg 66A:1222, 1984.
- Kääb MJ, Frenk A, Schmeling A, et al: Locked internal fi xator: sensitivity of screw/plate stability to the correct insertion angle of the screw, J Orthop Trauma 18:483, 2004.
- Kao JT, Burton D, Cornstock C, et al: Pudendal nerve palsy after femoral intramedullary nailing, J Orthop Trauma 7:58, 1993.
- Karlström G, Olerud S: Ipsilateral fracture of the femur and tibia, J Bone Joint Surg 59A:240, 1977.
- Karpos PAG, McFerran MA, Johnson KD: Intramedullary nailing of acute femoral shaft fractures using manual traction without a fracture table, Orthop Trauma 9:57, 1995.
- Kellam JF: Early results of the Sunnybrook experience with locked intramedullary nailing, Orthopedics 8:1387, 1985.
- Kempf I, Grosse A, Lafforgued L: L’enclouage avec blocage de la rotation on “clou blogue” principles, technique, indications et premiers resultants, Communication a la journee d’hiver, Sofcot, 1976.
- Ker MB, Maempel FZ, Paton DF: Bone cement as an adjunct to medullary nailing in fractures of the distal third of the femur in elderly patients, Injury 16:102, 1984.
- Khan FA, Ikram MS, Badr AA, al-Khawashki H: Femoral neck fracture: a complication of femoral nailing, Injury 26:319, 1995.
- Kimbrough EE: Concomitant unilateral hip and femoral-shaft fractures—a too frequently unrecognized syndrome: report of fi ve cases, J Bone Joint Surg 43A:443, 1961.
- King KF, Rush J: Closed intramedullary nailing of femoral shaft fractures: a review of one hundred and twelve cases treated by the Küntscher technique, J Bone Joint Surg 63A:1319, 1981.
- Klemm K, Schellmann WD: Dynamische und statische Verrigelung des Marknagels, Mschr Unfallheilk 75:568, 1972.
- Kohlhaas AR, Howard R: Radiation protection during interlocking Küntscher nailing, Orthop Rev 11:83, 1982.
- Koldenhoven GA, Burke JS, Pierron R: Ipsilateral femoral neck and shaft fractures, South Med J 90:288, 1997.
- Kolmert L, Persson BM, Romanus B: An experimental study of device for internal fi xation of distal femoral fractures, Clin Orthop Relat Res 171:290, 1982.
- Koval KJ, Kummar FJ, Bharan S, et al: Distal femoral fi xation: a laboratory comparison of the 95 degrees plate, antegrade and retrograde inserted reamed intramedullary nail, J Orthop Trauma 10:378, 1996.
- Krettek C, Rudolf J, Schandelmaier P, et al: Unreamed intramedullary nailing of femoral shaft fractures: operative technique and early clinical experience with the standard locking option, Injury 27:233, 1996.
- Kröpfl A, Berger U, Neureiter H, et al: Intramedullary pressure and bone marrow fat intravasation in unreamed femoral nailing, J Trauma 42:946, 1997.
- Kröpfl A, Naglik H, Primavesi C, et al: Unreamed intramedullary nailing of femoral fractures, J Trauma 38:717, 1995.
- Krupp RJ, Malkani AL, Goodin RA, et al: Optimal entry point for retrograde femoral nailing, J Orthop Trauma 17:100, 2003.
- Kumar A, Jasani V, Butt MS: Management of distal femoral fractures in elderly patients using retrograde titanium supracondylar nails, Injury 31:169, 2000.
- Küntscher G: Die Marknagelung von Knochenbrüchen: Tierexperimenteller Teil, Klin Wochenschr 19:6, 1940.
- Küntscher G: The Küntscher method of intramedullary fi xation, J Bone Joint Surg 40A:17, 1958.
- Küntscher G: Intramedullary surgical technique and its place in orthopaedic surgery: my present concept, J Bone Joint Surg 47A:809, 1965.
- Lam SJ: The place of delayed internal fi xation in the treatment of fractures of the long bones, J Bone Joint Surg 46B:393, 1964.
- Lanfranco G, Alberton G, Gnemmi G, et al: The use of the computer in a long-term review of 315 fractures of the proximal end of the femur, Ital J Orthop Traumatol 16:103, 1990.
- Laros GS: Supracondylar fractures of the femur: editorial comment and comparative results, Clin Orthop Relat Res 138:9, 1979.
- Laros GS, Spiegel PG: Rigid internal fi xation of fractures, Clin Orthop Relat Res 138:2, 1979 (editorial). Leggon RE, Feldman DD: Retrograde femoral nailing: a focus on the knee, Am J Knee Surg 14:109, 2001.
- Less Invasive Stabilization System (LISS): technique guide, Paoli, Penn, 2000, Synthes. Leung KS, Shen WY, So WS, et al: Interlocking intramedullary nailing for supracondylar and intercondylar fractures of the distal part of the femur, J Bone Joint Surg 73A:332, 1991.
- Leung PC, Mak KH, Lee SY: Percutaneous tension band wiring: a new method of internal fi xation for mildly displaced patella fracture, J Trauma 23:62, 1983.
- Lewert AH, Modny MT: Transfi xion rod in condylar and intercondylar fractures of femur, Orthop Rev 16:310, 1987.
- Lhowe DW, Hansen ST Jr: Immediate nailing of open fractures of the femoral shaft, J Bone Joint Surg 70A:812, 1988.
- Lindsey RW, Blair SR: Closed tibial shaft fractures: which ones benefi t from surgical treatment? J Am Assoc Orthop Surg 4:35, 1996.
