Spring Ligament Reconstruction Using Peroneus Longus Autograft
Key Takeaway
Spring ligament reconstruction using a peroneus longus graft is a powerful joint-sparing procedure for advanced adult acquired flatfoot deformity. This technique restores the static medial column restraints when the native calcaneonavicular ligament is irreparably attenuated. By routing the graft through anatomically positioned navicular and calcaneal or tibial tunnels, surgeons can effectively correct plantar sag and forefoot abduction, providing robust support alongside a medializing calcaneal osteotomy.
INTRODUCTION TO SPRING LIGAMENT RECONSTRUCTION
The spring ligament (calcaneonavicular ligament) complex is the primary static stabilizer of the medial longitudinal arch, working synergistically with the posterior tibial tendon (PTT), which acts as the primary dynamic stabilizer. In the pathogenesis of Adult Acquired Flatfoot Deformity (AAFD) or Posterior Tibial Tendon Dysfunction (PTTD), the loss of protective dynamic support from the PTT inevitably leads to the elongation, attenuation, and eventual incompetence of the spring ligament.
When the spring ligament becomes irreparably attenuated, primary repair alone is often insufficient to maintain arch kinematics and prevent recurrent pes planovalgus deformity. In such advanced cases (typically Stage IIb or early Stage III AAFD with a flexible hindfoot), reconstruction of the spring ligament using a peroneus longus autograft or allograft presents a robust, joint-sparing alternative to talonavicular or triple arthrodesis. This comprehensive guide details the indications, biomechanical rationale, and step-by-step surgical execution of spring ligament reconstruction utilizing a peroneus longus graft, combined with a medializing calcaneal osteotomy.
SURGICAL ANATOMY AND BIOMECHANICAL PRINCIPLES
A profound understanding of the medial column anatomy is mandatory for successful reconstruction. The spring ligament complex consists of three distinct bands:
* Superomedial Calcaneonavicular Ligament: The most critical restraint against talar head plantarflexion and medial subluxation. It originates from the anterior margin of the sustentaculum tali and inserts broadly onto the superomedial aspect of the tarsal navicular.
* Medioplantar Oblique Calcaneonavicular Ligament: Originates from the coronoid fossa of the calcaneus and inserts onto the plantar navicular.
* Inferoplantar Longitudinal Calcaneonavicular Ligament: Lies plantar to the medioplantar band, providing additional longitudinal support.
💡 Biomechanical Pearl
The superomedial band is the most frequently torn or attenuated structure in AAFD. Its failure allows the talar head to plantarflex (creating a "plantar sag" at the talonavicular joint) and the navicular to abduct (uncovering the talar head). The choice of reconstructive tunnel trajectory—calcaneal versus tibial—is directly dictated by which of these two multiplanar deformities predominates.
The peroneus longus is selected as a graft source due to its excellent tensile strength, dense collagenous architecture, and adequate length, which allows for multi-tunnel routing without compromising lateral column stability, provided the peroneus brevis remains intact.
INDICATIONS AND PATIENT SELECTION
Spring ligament reconstruction is indicated in patients demonstrating:
* Advanced Stage II AAFD: Flexible hindfoot valgus with significant forefoot abduction (>40% talonavicular uncoverage) and profound medial column collapse.
* Irreparable Spring Ligament: Intraoperative assessment revealing a ligament that is excessively thinned, structurally disorganized, or completely ruptured, rendering primary imbrication impossible or biomechanically futile.
* Failed Previous Soft Tissue Procedures: Patients who have undergone isolated PTT debridement or transfer without addressing the static medial restraints, leading to recurrent deformity.
Contraindications include rigid, fixed hindfoot or midfoot deformities (Stage III/IV AAFD), severe talonavicular osteoarthritis, active infection, or profound peripheral neuropathy (e.g., Charcot neuroarthropathy), where arthrodesis is the definitive standard of care.
PREOPERATIVE PLANNING AND IMAGING
Thorough preoperative imaging is essential to quantify the deformity and plan the osseous and soft tissue corrections.
* Weight-Bearing Radiographs: AP, lateral, and mortise views of the foot and ankle. Assess the talonavicular coverage angle (AP view), the lateral talo-first metatarsal angle (Meary's angle), and the calcaneal pitch.
* Magnetic Resonance Imaging (MRI): Highly sensitive for evaluating the integrity of the PTT and the superomedial band of the spring ligament. Look for increased signal intensity, thickening, or discontinuity of the ligamentous complex.
* Computed Tomography (CT): Useful in assessing joint congruency and ruling out subtle degenerative changes in the subtalar or talonavicular joints that might necessitate arthrodesis.
PATIENT POSITIONING AND ANESTHESIA
- Anesthesia: General anesthesia or regional anesthesia (spinal/popliteal block) is utilized based on patient comorbidities and anesthesiologist preference.
- Positioning: The patient is placed in the supine position. A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the medial aspect of the foot and ankle into direct view.
- Tourniquet: A well-padded pneumatic thigh or calf tourniquet is applied to ensure a bloodless surgical field.
- Preparation: Standard orthopedic prep and drape from the toes to the proximal tibia.
COMPREHENSIVE SURGICAL TECHNIQUE
1. Exposure and Soft Tissue Assessment
- Make a longitudinal medial utility incision extending from the posterior aspect of the medial malleolus, following the course of the PTT, and extending distally to the medial cuneiform.
- Carefully dissect through the subcutaneous tissues, taking meticulous care to identify and protect the saphenous vein and nerve dorsally, and the medial plantar nerve branches plantarly.
- Incise the flexor retinaculum to expose the PTT. Perform a thorough tenosynovectomy and debridement of the PTT.
- Retract the PTT plantarly to expose the underlying spring ligament complex. Locate the superomedial portion of the calcaneonavicular ligament just inferior to the head of the talus, where it attaches to the plantar and plantar-medial aspect of the tarsal navicular.
2. Spring Ligament Wedge Excision and Primary Repair
Before proceeding to the graft reconstruction, the native, redundant tissue must be addressed to restore the anatomic tension of the medial column.
- Adduct the foot and forefoot into a neutral and slightly adducted position.
- Excise a wedge of the attenuated spring ligament and the plantar talonavicular capsule. The excised wedge should typically measure 8 to 10 mm, depending on the magnitude of the preoperative deformity and the degree of redundancy.
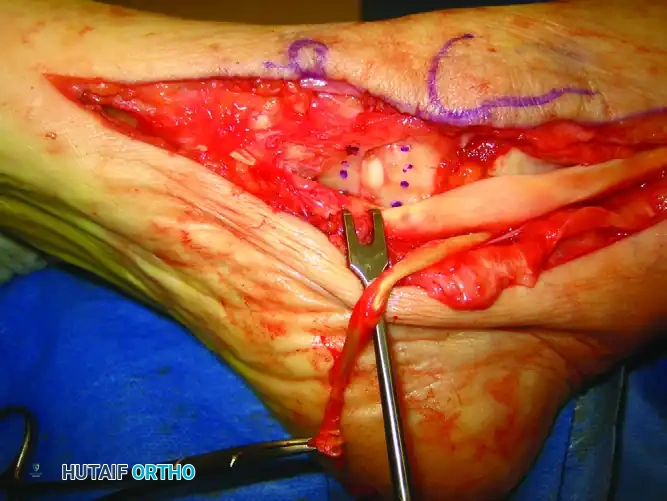
Clinical photograph demonstrating the exposure of the medial column and the precise location for the wedge excision of the redundant spring ligament.
- Following the excision, repair and imbricate the remaining spring ligament using multiple interrupted 2-0 braided, nonabsorbable sutures.
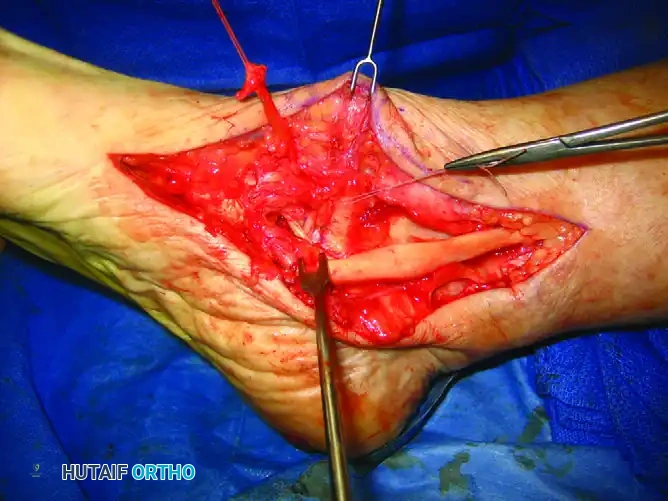
Clinical photograph showing the completed primary repair of the spring ligament with robust, nonabsorbable sutures, restoring the static tension of the medial arch.
🚨 Surgical Warning
Elongation and incompetence of the spring ligament from the loss of protective support of the posterior tibial tendon contribute significantly to the pes planovalgus deformity. Repair of the spring ligament should be done routinely as part of the medial soft tissue procedure. However, if the tissue is so attenuated that it cannot hold suture tension, reconstruction with a peroneus longus graft is strictly required as an alternative to arthrodesis.
3. Decision Making: Tunnel Trajectory
The routing of the peroneus longus graft is dictated by the specific plane of deformity present at the talonavicular joint:
* Plantar Sag Predominance: If the primary deformity is a plantar sag at the talonavicular joint (loss of the longitudinal arch), a calcaneal tunnel is created.
* Abduction Predominance: If the primary deformity is forefoot abduction through the talonavicular joint (uncovering of the talar head), a tibial tunnel is created.
4. Tunnel Preparation
The Navicular Tunnel (Common to Both Techniques)
- Identify the center of the tarsal navicular.
- Under fluoroscopic guidance, place a guidewire from dorsal to plantar through the body of the navicular.
- Overdrill the guidewire with an 8 to 9 mm cannulated drill bit, ensuring the cortical bridges remain intact to prevent iatrogenic fracture.
The Calcaneal Tunnel (For Plantar Sag)
- Place a Kirschner wire (K-wire) in the calcaneus immediately inferior to the sustentaculum tali.
- Crucial Anatomy Check: Take extreme care not to violate or damage the flexor hallucis longus (FHL) tendon, which runs in the groove beneath the sustentaculum.
- Advance the K-wire posteriorly and laterally across the body of the calcaneus. The wire should exit above the planned (or completed) medializing calcaneal osteotomy incision on the lateral side of the foot.
- Confirm fluoroscopically that the subtalar joint has not been violated.
- Replace the K-wire with a guidewire and overdrill with an 8 to 9 mm cannulated drill.
The Tibial Tunnel (For Forefoot Abduction)
- Identify a starting point between the anterior and posterior colliculi of the medial malleolus.
- Make a small lateral fibular incision. Use a small Bennett retractor through this incision to gain access to the lateral tibia, just anterior to the fibula.
- Under strict fluoroscopic guidance, place a K-wire from the medial malleolus directed proximally and laterally toward the prepared lateral exposure.
- Crucial Anatomy Check: Ensure the trajectory remains entirely extra-articular, avoiding the ankle joint plafond.
- Replace the K-wire with a guidewire and overdrill with an 8 to 9 mm cannulated drill.
5. Graft Passage and Tensioning
- Harvest and prepare the peroneus longus autograft (or thaw and prepare an allograft) using standard techniques, ensuring the ends are whipstitched with high-strength nonabsorbable suture.
- Pass the graft from dorsal to plantar through the navicular tunnel.
- Subsequently, route the graft through either the calcaneal tunnel or the tibial tunnel, depending on the prepared trajectory.
- Tensioning Protocol: Tensioning must occur after the fixation of any concurrent osteotomies (e.g., Medial Displacement Calcaneal Osteotomy).
- Place the foot in slight inversion, plantar flexion, and 5 to 10 degrees of adduction through the talonavicular joint, simulating a corrected weight-bearing posture.
- Pretension the graft: Apply sustained, firm tension to the graft ends for several minutes to remove inherent viscoelastic creep before final fixation.
6. Graft Fixation
- Fixation is achieved using solid screws acting as posts to tie down the graft sutures, or via interference screws, depending on surgeon preference.
- For a Calcaneal Tunnel: Place a 3.5-mm cortical screw anterior to the lateral exit of the calcaneal tunnel. Tie the graft sutures securely around this post.
- For a Tibial Tunnel: Place a 3.5-mm screw laterally on the fibula, several centimeters proximal to the exit of the tibial tunnel, to serve as the fixation post.
- Use two sets of high-strength sutures to secure the graft while an assistant maintains the foot in the corrected, adducted, and plantarflexed position.
- Biological Augmentation: Harvest local cancellous bone graft from the medializing heel slide osteotomy and pack it meticulously into the navicular, calcaneal, or tibial tunnels around the graft to promote osteointegration.
ADJUNCTIVE PROCEDURES
Spring ligament reconstruction is rarely performed in isolation. To protect the soft tissue reconstruction from failing under the immense biomechanical loads of weight-bearing, osseous realignment is mandatory.
* Medial Displacement Calcaneal Osteotomy (MDCO): Almost universally performed concurrently. It shifts the mechanical axis of the hindfoot medially, reducing the valgus thrust on the medial column and protecting the reconstructed spring ligament.
* Flexor Digitorum Longus (FDL) Transfer: Often performed to replace the dysfunctional PTT, providing dynamic support to the newly reconstructed static arch.
* Gastrocnemius Recession or Tendo-Achilles Lengthening (TAL): Essential if equinus contracture is present, as a tight Achilles tendon will exert a destructive midfoot breaching force, jeopardizing the reconstruction.
POSTOPERATIVE REHABILITATION PROTOCOL
Strict adherence to a phased rehabilitation protocol is critical to allow for graft incorporation and soft tissue healing.
- Phase I (Weeks 0-2): The patient is placed in a well-padded, short-leg splint in slight inversion and equinus. Strict non-weight-bearing (NWB) status is enforced. Elevation is prioritized to minimize edema.
- Phase II (Weeks 2-6): Sutures are removed. The patient is transitioned to a short-leg fiberglass cast or a locked controlled ankle motion (CAM) boot. The foot remains immobilized in a neutral to slightly inverted position. Strict NWB status continues.
- Phase III (Weeks 6-10): Radiographic evaluation of the osteotomies is performed. If healing is evident, the patient begins progressive partial weight-bearing in the CAM boot. Gentle active range of motion (AROM) exercises for the ankle and subtalar joints are initiated.
- Phase IV (Weeks 10-16): Transition to full weight-bearing in supportive athletic footwear with a custom medial longitudinal arch orthotic. Physical therapy focuses on strengthening the FDL transfer, peroneal balancing, and proprioceptive training.
- Return to Activity: High-impact activities and sports are generally restricted until 6 to 9 months postoperatively, contingent upon the return of dynamic strength and radiographic consolidation of all osteotomies.
COMPLICATIONS AND AVOIDANCE STRATEGIES
While highly effective, spring ligament reconstruction carries specific risks that the orthopedic surgeon must meticulously mitigate:
- Nerve Injury:
- Sural Nerve: At risk during the lateral exit of the calcaneal tunnel and the lateral fixation of the graft. Careful blunt dissection to the bone is required.
- Medial Plantar Nerve: At risk during the plantar dissection of the navicular and the excision of the spring ligament wedge. Maintain dissection strictly within the subperiosteal/subcapsular plane.
- Iatrogenic Fracture: The tarsal navicular is susceptible to fracture during the creation of the 8-9 mm tunnel. Ensure the guidewire is perfectly centered and avoid eccentric drilling that compromises the dorsal or plantar cortical bridges.
- Graft Failure or Elongation: Failure to pretension the peroneus longus graft will result in postoperative creep, leading to recurrent plantar sag and forefoot abduction. Always pretension the graft and ensure the foot is held in 5-10 degrees of adduction during final fixation.
- Hardware Prominence: The 3.5-mm post screws on the lateral calcaneus or fibula may become symptomatic, particularly in patients with minimal subcutaneous fat, occasionally necessitating delayed hardware removal after complete graft incorporation.
You Might Also Like
