Tibial Eminence Fracture Case Study: Comprehensive Diagnostic & Imaging Insights
Key Takeaway
Tibial eminence fractures are diagnosed via detailed clinical examination, noting acute knee pain, swelling, limited ROM, and positive Lachman/Anterior Drawer tests, especially after sports injury. Confirmatory imaging includes X-rays showing avulsion, CT for fragment morphology and displacement (e.g., Type III), and MRI to assess associated soft tissue injuries like meniscal entrapment.
Patient Presentation and History
Case 36 presents a 24 year old male collegiate football player who sustained an acute high energy left knee injury during a full contact scrimmage. The mechanism of injury involved a forced valgus stress applied to a partially flexed knee, compounded by a significant axial load as the athlete was tackled directly from the lateral aspect. This specific biomechanical vector combination places extraordinary tensile stress on the anterior cruciate ligament and its bony insertions. The patient reported a distinct and audible pop sensation at the exact moment of impact, which was immediately followed by profound functional impotence, severe localized pain, and an absolute inability to bear weight on the affected extremity.
In the context of adult orthopedic trauma, this mechanism typically results in a midsubstance rupture of the anterior cruciate ligament. However, the transmission of forces in this specific patient resulted in a failure at the osteoligamentous junction, leading to an avulsion fracture of the tibial eminence. The epidemiology of tibial eminence fractures is heavily skewed toward the pediatric and adolescent populations, where the unossified tibial physis and relatively weaker cancellous bone fail prior to the robust ligamentous tissue. The occurrence of this injury pattern in a skeletally mature 24 year old athlete indicates a highly specific distribution of kinetic energy, likely involving a rapid deceleration combined with a rotational moment that perfectly isolated the anterior intercondylar area of the tibia.
His past medical history is entirely unremarkable. He has no prior history of knee trauma, previous orthopedic surgeries, or significant medical comorbidities. He is a non smoker, consumes alcohol occasionally, and denies any regular daily medication use or illicit substance use. A thorough review of systems reveals no family history of bleeding diatheses, hypercoagulable states, or connective tissue disorders. As a collegiate athlete, his primary and overriding goal is a full return to high level competitive sport, necessitating an intervention that not only restores structural anatomy but also guarantees the precise kinematic function of the knee joint.
Understanding the precise mechanism of injury is paramount for anticipating concomitant intraarticular pathology. The valgus stress component highly correlates with potential medial collateral ligament sprains or peripheral medial meniscal tears, while the axial loading in partial flexion frequently results in chondral impaction injuries to the lateral femoral condyle or lateral tibial plateau. The rapid onset of swelling reported by the athletic training staff on the field is highly indicative of an acute hemarthrosis, a hallmark sign of intraarticular fracture or major ligamentous disruption.
Clinical Examination Findings
Upon arrival at the orthopedic emergency department, the patient presented in significant acute distress, utilizing a knee immobilizer placed by the field medical staff. The clinical examination was meticulously conducted to differentiate between soft tissue disruption and osteochondral pathology, despite the limitations imposed by the patient's acute pain and involuntary muscle guarding.
Inspection and Palpation
Gross inspection of the left lower extremity revealed a massive, tense hemarthrosis. This was visually manifested as significant suprapatellar fullness, complete obliteration of the normal peripatellar sulci, and loss of the standard topographical contours of the anterior knee. Mild ecchymosis was observed tracking along the lateral joint line and extending inferiorly into the popliteal fossa, suggesting capsular disruption or fascial tracking of the intraarticular hematoma. No gross angular deformities of the mechanical axis were observed, and the overlying skin envelope was completely intact. The absence of open wounds, abrasions, or severe soft tissue degloving precluded the immediate concern for an open fracture or impending compartment syndrome, though vigilance was maintained.
Palpation elicited marked, exquisitely localized tenderness over the anteromedial aspect of the knee joint. The point of maximal tenderness was situated deep to the patellar tendon, directly over the anatomic footprint of the tibial eminence and the anterior intercondylar area. Additional tenderness was noted along the medial joint line, raising the index of suspicion for a concomitant medial meniscal injury. A large, tense effusion was palpable, and a patellar ballotment test was strongly positive, confirming the presence of a substantial fluid wave consistent with acute hemarthrosis. Mild thermal changes, specifically localized warmth, were noted over the affected joint, consistent with the acute inflammatory cascade secondary to trauma.
Range of Motion and Mechanical Block
Active and passive range of motion assessments were severely restricted secondary to pain, effusion, and involuntary hamstring guarding. Active flexion was limited to approximately 40 degrees. Most notably, the patient exhibited a fixed flexion deformity of 15 degrees. Any attempt by the examiner to achieve full passive extension was met with excruciating pain and an abrupt, firm mechanical block.
This mechanical block to extension is a critical clinical finding in the setting of a suspected tibial eminence avulsion. It almost universally signifies that the avulsed bony fragment, along with the attached anterior cruciate ligament, has migrated superiorly and anteriorly, impinging against the roof of the intercondylar notch during extension. Furthermore, this mechanical block frequently indicates the entrapment of adjacent intraarticular structures beneath the avulsed fragment. The transverse intermeniscal ligament or the anterior horn of the medial meniscus are the most commonly incarcerated structures, effectively preventing the anatomic reduction of the fracture fragment and physically blocking terminal knee extension.
Ligamentous Stability Assessment
Ligamentous stability testing in the acute, severely swollen knee is notoriously challenging and requires cautious, gentle manipulation to yield reliable data without exacerbating patient discomfort.
The Lachman test was positive, demonstrating increased anterior tibial translation compared to the contralateral uninjured knee. Crucially, the endpoint was described as soft and ill defined. This finding confirms the functional insufficiency of the anterior cruciate ligament. In the context of an eminence fracture, the ligament itself may be structurally intact, but its functional capacity as the primary restraint to anterior tibial translation is completely lost due to the detachment of its distal anchor. The Anterior Drawer test was also positive, corroborating the Lachman findings.
The Posterior Drawer test was negative, with a firm endpoint, suggesting an intact posterior cruciate ligament. Varus and valgus stress testing performed at both 0 degrees and 30 degrees of flexion demonstrated no significant gapping or asymmetric joint space opening, suggesting that the medial collateral ligament and lateral collateral ligament complexes remained structurally intact despite the valgus mechanism of injury. Standard provocative testing for meniscal pathology, such as the McMurray test and Apley compression test, could not be reliably performed due to the patient's severe pain and the pre existing mechanical block to motion. However, the clinical suspicion for meniscal pathology remained exceptionally high based on the mechanism of injury and the joint line tenderness.
Neurological and Vascular Assessment
A comprehensive neurovascular examination of the distal extremity was performed to rule out any limb threatening vascular compromise or peripheral nerve injury, which can occasionally accompany high energy knee trauma. Distal pulses, including the dorsalis pedis and posterior tibial arteries, were strong, symmetric, and easily palpable bilaterally. Capillary refill was brisk, occurring in under two seconds in all digits of the left foot. There were no signs of pallor, paresthesia, pulselessness, or poikilothermia.
Neurological assessment confirmed intact sensation to light touch and pinprick in the dermatomal distributions of the saphenous, deep peroneal, superficial peroneal, and tibial nerves. Motor function was fully preserved, with the patient demonstrating 5/5 strength in ankle dorsiflexion, plantarflexion, extensor hallucis longus function, and toe flexion. Palpation of the muscular compartments of the lower leg revealed soft, compressible compartments with no clinical evidence suggestive of acute compartment syndrome.
Imaging and Diagnostics
The diagnostic imaging algorithm for suspected tibial eminence fractures requires a multi modality approach to accurately define the osseous architecture, evaluate the degree of fragment displacement, and assess the integrity of the surrounding soft tissue envelope.
Plain Radiographic Evaluation
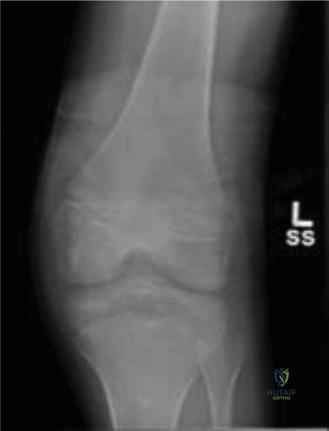
Initial radiographic evaluation in the emergency department included standard non weight bearing anteroposterior, lateral, and oblique views of the left knee.
The anteroposterior radiograph demonstrated a distinct avulsion fracture of the tibial eminence, localizing to the anterior intercondylar area. The primary fracture fragment appeared partially displaced in a lateral and superior direction. The lateral radiograph was paramount in defining the true extent of the pathology. It clearly visualized the anterior displacement and superior hinging of the avulsed fragment, confirming the clinical suspicion of a mechanical block to extension caused by notch impingement.
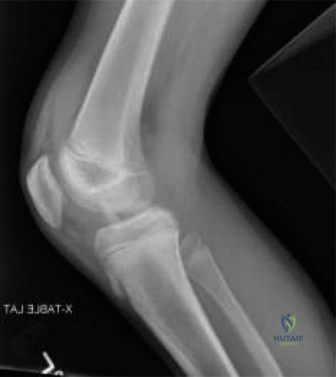
Careful scrutiny of the radiographs is required to differentiate the primary eminence fragment from other potential osseous avulsions. The lateral view must be evaluated for the presence of a Segond fracture, a small vertically oriented avulsion off the anterolateral proximal tibia, which is highly pathognomonic for an anterior cruciate ligament tear and anterolateral complex disruption. In this case, no Segond fracture was identified. The intercondylar notch view, if obtainable, can provide additional perspective on the medial to lateral dimensions of the fracture bed, though it is often difficult to acquire in the acutely injured, painful knee.
Advanced Cross Sectional Imaging
While plain radiographs confirm the diagnosis of a tibial eminence avulsion, advanced cross sectional imaging is absolutely critical for comprehensive preoperative planning, especially in an adult patient where the fracture pattern may be significantly more comminuted than in the pediatric population.
A non contrast Computed Tomography scan of the knee with fine cuts and three dimensional reconstruction capabilities is highly recommended. The CT scan provides precise spatial mapping of the fracture bed, delineates the exact size and morphology of the avulsed fragment, and identifies any occult comminution that may dictate the choice of internal fixation. In adults, the eminence fragment is often composed of dense subchondral bone with minimal cancellous backing, making it prone to fragmentation upon injury or during surgical manipulation. The 3D reconstructions are invaluable for conceptualizing the required vectors for anatomic reduction.
Magnetic Resonance Imaging remains the gold standard for evaluating the intraarticular soft tissues. An MRI of the left knee without contrast was obtained to evaluate the integrity of the anterior cruciate ligament substance, the menisci, and the articular cartilage.

The MRI sequences confirmed the completely displaced avulsion fracture of the anterior tibial eminence. Crucially, the MRI allowed for the assessment of the anterior cruciate ligament fibers themselves. In adult eminence fractures, the ligament frequently undergoes significant interstitial plastic deformation prior to the bony avulsion. Identifying midsubstance attenuation or partial tearing on MRI is vital, as a structurally compromised ligament may fail to restore normal joint kinematics even after rigid anatomic fixation of the bony fragment. Furthermore, the MRI meticulously evaluated the menisci. It confirmed the clinical suspicion of an anterior horn medial meniscal entrapment beneath the displaced bony fragment, explaining the mechanical block to extension. No concomitant peripheral meniscal root tears or high grade collateral ligament sprains were identified.
Differential Diagnosis
The acute presentation of a traumatic hemarthrosis with an inability to bear weight and a positive Lachman test requires a rigorous differential diagnosis. While the plain radiographs rapidly isolate the osseous pathology in this specific case, the initial clinical presentation overlaps significantly with several other severe intraarticular knee injuries.
| Diagnosis | Clinical Presentation | Imaging Findings | Differentiating Factors |
|---|---|---|---|
| Midsubstance Anterior Cruciate Ligament Rupture | Acute pop, massive hemarthrosis, profound instability, positive Lachman and pivot shift tests. | MRI shows discontinuity of ACL fibers, bone bruising on lateral femoral condyle and posterolateral tibia. Normal AP/Lateral X-rays (unless Segond present). | Lack of osseous avulsion fragment on plain radiographs. The mechanical block to extension is less common unless a large bucket handle meniscal tear is present. |
| Tibial Eminence Avulsion Fracture | Acute pop, hemarthrosis, positive Lachman (soft endpoint), severe mechanical block to extension. | Plain radiographs show osseous fragment in the intercondylar notch. MRI confirms bony avulsion with intact midsubstance ACL fibers. | Clear radiographic evidence of the intercondylar fracture. High incidence of meniscal or intermeniscal ligament entrapment causing the fixed flexion deformity. |
| Acute Patellar Dislocation with Osteochondral Fracture | Sensation of the knee "giving way," medial sided pain, positive patellar apprehension test. | X-rays may show lateral patellar tilt or subluxation. Skyline view may reveal osteochondral fragments. MRI shows MPFL disruption and lateral femoral condyle bone bruising. | Mechanism usually involves twisting rather than direct valgus/axial load. Tenderness is distinctly localized to the medial patellofemoral ligament and medial retinaculum, not the deep intercondylar area. |
| Meniscal Root Avulsion Tear | Posterior knee pain, pop sensation during deep flexion or squatting, joint line tenderness. | Plain films generally normal. MRI shows fluid cleft at the meniscal root attachment, extrusion of the meniscus on coronal sequences, and the "ghost sign" on sagittal sequences. | The Lachman test is typically negative or demonstrates a firm endpoint. The instability is less profound than an ACL or eminence injury. |
| Tibial Plateau Fracture (Schatzker I or II) | High energy valgus load, severe pain, inability to bear weight, lateral joint line tenderness. | Plain radiographs demonstrate lateral plateau depression or split. CT scan precisely defines the articular step off and metaphyseal extension. | Ligamentous exam may be stable if the fracture is isolated, though collateral injuries are common. The pathology is localized to the weight bearing articular surface rather than the non weight bearing intercondylar eminence. |
Surgical Decision Making and Classification
The management of tibial eminence fractures is dictated by the degree of fragment displacement, the presence of a mechanical block to motion, the patient's physiological age, and their functional demands. To standardize communication and guide treatment algorithms, these fractures are universally categorized using the Meyers and McKeever classification system, which was later modified by Zaricznyj to include comminuted patterns.
Classification Systems
The Meyers and McKeever classification is based primarily on the lateral radiographic appearance of the fracture fragment:
- Type I: Non displaced or minimally displaced fracture. The anterior margin of the fragment may be slightly elevated, but the fragment remains firmly seated within its anatomical bed.
- Type II: Partially displaced fracture. The anterior portion of the fragment is elevated, creating a "beak" appearance, but the posterior hinge remains intact, maintaining cortical contact with the fracture bed.
- Type III: Completely displaced fracture. The fragment is entirely lifted from the fracture bed, with no cortical contact. This is further subdivided into IIIA (involving only the ACL footprint) and IIIB (involving the entire eminence and potentially extending into the articular surface).
- Type IV (Zaricznyj Modification): A completely displaced and comminuted fracture of the tibial eminence.
Based on the comprehensive radiographic and MRI evaluation, the patient in Case 36 presents with a Meyers and McKeever Type III fracture. The fragment is completely displaced, migrated superiorly, and lacks any posterior cortical hinge. The MRI confirmed that the fragment is acting as a mechanical block in the intercondylar notch.
Indications for Operative Intervention
The decision to proceed with operative intervention in this 24 year old high level athlete is absolute and unambiguous. Non operative management, consisting of closed reduction and cast immobilization in extension, is strictly reserved for true Type I fractures or select Type II fractures where anatomic reduction can be unequivocally achieved and maintained in extension without soft tissue interposition.
For a completely displaced Type III fracture, non operative management is contraindicated. The primary indications for surgical intervention in this case include:
- Restoration of Joint Kinematics: The anterior cruciate ligament is the primary restraint to anterior tibial translation and a critical secondary restraint to internal rotation. Failure to anatomically reduce and rigidly fix the eminence fragment results in a functionally elongated and incompetent ACL, leading to chronic anterior and rotational instability. This instability precludes a return to cutting and pivoting sports and accelerates the onset of post traumatic osteoarthritis.
- Resolution of Mechanical Block: The superiorly migrated fragment, along with the entrapped anterior horn of the medial meniscus, creates an absolute mechanical block to terminal extension. Left untreated, this will rapidly progress to a debilitating flexion contracture and severe arthrofibrosis, permanently compromising the functional outcome of the knee.
- Prevention of Nonunion or Malunion: The synovial fluid environment of the knee joint is inherently hostile to bone healing due to the presence of fibrinolytic enzymes. A completely displaced, unreduced fragment bathed in synovial fluid is at a significantly elevated risk for nonunion. Malunion in an elevated position will result in chronic impingement against the roof of the intercondylar notch (Guillier's impingement) during extension, causing chronic pain and secondary chondral damage.
- Meniscal Preservation: The MRI confirmed entrapment of the medial meniscus. Surgical intervention is required to meticulously extricate the meniscal tissue from the fracture bed without causing iatrogenic damage, thereby preserving the critical load sharing and shock absorbing functions of the meniscus.
Given the patient's athletic profile, the completely displaced nature of the fracture, and the soft tissue entrapment, an arthroscopic assisted anatomic reduction and rigid internal fixation is the definitive standard of care.
Surgical Technique and Intervention
The surgical management of tibial eminence fractures has evolved significantly from traditional open arthrotomies to sophisticated arthroscopic techniques. Arthroscopy offers the distinct advantages of minimizing surgical morbidity, allowing for a comprehensive evaluation of the entire joint space, facilitating the precise management of concomitant intraarticular pathology, and reducing the risk of postoperative arthrofibrosis.
Patient Positioning and Portal Placement
The patient is taken to the operating room and placed in the supine position on the operating table. Following the induction of general anesthesia, a thorough examination under anesthesia is performed to re evaluate ligamentous stability without the confounding factors of pain and muscle guarding. A high thigh tourniquet is applied, and the non operative leg is secured in a well padded leg holder. The operative left leg is prepped and draped in standard sterile orthopedic fashion.
Standard anterolateral and anteromedial arthroscopic portals are established. The anterolateral portal is created adjacent to the lateral border of the patellar tendon, slightly superior to the joint line, serving as the primary viewing portal. The anteromedial portal is established under direct intraarticular visualization to ensure optimal trajectory toward the tibial eminence. In many cases, an accessory anteromedial portal or a transpatellar tendon portal may be required to achieve the precise angles necessary for drilling and hardware placement without causing iatrogenic damage to the articular cartilage of the medial femoral condyle.
Arthroscopic Evaluation and Debridement
Upon entering the joint, a massive hemarthrosis is typically encountered. Thorough joint lavage using an arthroscopic shaver is performed to evacuate the hematoma, clear the visual field, and remove any loose fibrinous debris. A systematic diagnostic arthroscopy is then conducted, examining the suprapatellar pouch, the medial and lateral gutters, the articular surfaces of the patellofemoral joint, and the medial and lateral compartments.
Attention is then directed to the intercondylar notch. The completely displaced tibial eminence fragment is visualized, suspended by the intact fibers of the anterior cruciate ligament. The fracture bed on the proximal tibia is carefully inspected. The bed is meticulously debrided of hematoma, organized clot, and any small, non viable osseous fragments using a combination of a motorized shaver and arthroscopic curettes. It is imperative to expose healthy, bleeding cancellous bone in the crater to optimize the biological environment for fracture healing.
Crucially, the soft tissues surrounding the fracture bed are evaluated. As predicted by the preoperative MRI, the anterior horn of the medial meniscus and the transverse intermeniscal ligament are frequently found to be prolapsed and incarcerated within the fracture crater. Using an arthroscopic probe, these structures are gently teased out of the defect and retracted anteriorly. Failure to recognize and clear this soft tissue interposition is the single most common cause of non anatomic reduction and persistent postoperative mechanical blocks.
Fracture Reduction and Fixation Construct
Once the fracture bed is prepared and all soft tissue impingement is cleared, the fracture is reduced. An arthroscopic probe or a specialized elevator is introduced through the anteromedial portal. Downward pressure is applied to the superior aspect of the bony fragment, while simultaneously extending the knee to utilize the tension of the ACL to guide the fragment into its anatomical footprint.
The choice of fixation construct depends on the size, integrity, and comminution of the osseous fragment. In adult patients, the fragment may be large enough to accommodate cannulated screws. However, screw fixation carries the risk of fragment fragmentation during drilling, and the screw heads may cause impingement in the intercondylar notch, frequently necessitating a second surgery for hardware removal.
Given the high energy nature of this injury in an adult athlete, the fragment often exhibits subtle comminution. Therefore, a heavy non absorbable suture pull out technique is often preferred. This technique provides excellent biomechanical stability, distributes the compressive forces evenly across the fragment, and eliminates the need for subsequent hardware removal.

Using a specialized arthroscopic suture passing device (such as a suture lasso or a sharp penetrating grasper), two strands of #2 high strength, non absorbable ultra high molecular weight polyethylene suture are passed through the substance of the anterior cruciate ligament, immediately adjacent to its bony insertion on the avulsed fragment. Care is taken to capture the robust ligamentous tissue without compromising the structural integrity of the ACL bundles.
A highly precise tibial anterior cruciate ligament drill guide is then introduced through the anteromedial portal. The tip of the guide is positioned precisely at the medial margin of the fracture bed. A small incision is made over the anteromedial proximal tibia, approximately 2 centimeters distal to the joint line. A guide pin is drilled from the anteromedial tibial cortex into the medial aspect of the fracture crater. The guide is then repositioned, and a second parallel guide pin is drilled into the lateral aspect of the fracture crater.
The guide pins are overdrilled with a 4.5 millimeter cannulated reamer to create two parallel osseous tunnels. Suture passing loops are introduced through these tunnels into the joint space. The free ends of the high strength sutures previously passed through the ACL are retrieved and shuttled down through the tibial tunnels.
The knee is then placed in approximately 10 to 15 degrees of flexion to approximate the native tension of the anterior cruciate ligament. The sutures are pulled distally, firmly seating the bony fragment into the debrided crater. The reduction is visually confirmed via arthroscopy to ensure it is perfectly flush with the surrounding articular surface and that no soft tissue remains interposed. While maintaining strict tension on the sutures, they are tied securely over a cortical bone bridge on the anteromedial tibia, or alternatively, secured using a low profile biocomposite suture anchor or cortical button.
A final arthroscopic inspection is performed. The knee is cycled through a full range of motion to confirm the stability of the fixation, ensure the absence of notch impingement in full extension, and verify that normal anterior cruciate ligament tension has been restored. The arthroscopic portals and the tibial incision are closed in a standard layered fashion.
Post Operative Protocol and Rehabilitation
The postoperative rehabilitation following surgical fixation of a tibial eminence fracture is a delicate balance between protecting the osseous healing environment and preventing the devastating complication of arthrofibrosis. The protocol must be strictly adhered to and closely monitored by both the surgical team and the physical therapy staff.
Acute Recovery Phase
The acute phase, encompassing postoperative weeks 0 to 2, prioritizes wound healing, edema control, and the initiation of early, protected range of motion. The patient is placed in a hinged knee brace locked in full extension immediately postoperatively. Weight bearing is strictly restricted to touch down weight bearing or non weight bearing using crutches to prevent axial loading and shear forces across the fracture site.
Cryotherapy and elevation are utilized aggressively to manage hemarthrosis and swelling. During this phase, the brace may be unlocked to allow passive and active assisted range of motion from 0 to 90 degrees, strictly under the supervision of a physical therapist.
