Tibial Eminence Fracture: Case 36 Diagnosis & Surgical Insights
Patient Presentation & History
Case 36 presents a 24-year-old male, a collegiate football player, who sustained an acute knee injury during a scrimmage. The mechanism of injury involved a forced valgus stress to a partially flexed knee combined with an axial load as he was tackled from the side, resulting in immediate, severe pain and inability to bear weight. He reported a distinct "pop" sensation at the time of injury, followed by rapid onset of swelling.
His past medical history is unremarkable, with no prior knee surgeries or significant comorbidities. He is a non-smoker and denies any regular medication use. There is no family history of bleeding disorders or hypercoagulability. His primary goal is to return to high-level competitive sport.
Clinical Examination
Upon arrival at the emergency department, the patient was in significant distress with a visibly swollen left knee.
Inspection
- Effusion: Gross hemarthrosis was evident, manifesting as significant suprapatellar fullness and obliteration of normal knee contours.
- Ecchymosis: Mild ecchymosis was noted laterally, extending into the popliteal fossa.
- Deformity: No gross deformities were observed.
- Skin Integrity: Intact skin, no open wounds or abrasions were present, precluding an open fracture.
Palpation
- Tenderness: Marked tenderness was elicited over the anteromedial aspect of the knee joint, specifically over the tibial tubercle and the medial joint line.
- Effusion: A large, tense effusion was palpable.
- Patellar Ballotment: Strongly positive.
- Thermal Changes: Mild warmth was noted over the affected joint.
Range of Motion (ROM)
Active and passive ROM were severely limited due to pain and guarding.
*
Flexion:
Limited to approximately 40 degrees.
*
Extension:
A fixed flexion deformity of 15 degrees was present, with attempts at full extension met with excruciating pain and muscle spasm. This mechanical block suggested possible meniscal interposition or fragment impingement.
Ligamentous Stability Assessment
Ligamentous testing was challenging due to pain and guarding, necessitating cautious and gentle manipulation.
*
Lachman Test:
Positive with a soft, ill-defined endpoint, indicating anterior tibial translation and disruption of the primary ACL restraint.
*
Anterior Drawer Test:
Positive, corroborating the Lachman findings, further supporting ACL insufficiency.
*
Posterior Drawer Test:
Negative, suggesting an intact Posterior Cruciate Ligament (PCL).
*
Varus/Valgus Stress Tests:
Performed at 0 and 30 degrees of flexion. No significant gapping or instability was noted on either medial or lateral stress, suggesting intact collateral ligaments.
*
Meniscal Tests:
McMurray's test could not be reliably performed due to pain and limited ROM. Suspicion for meniscal injury remained high given the MOI and mechanical block.
Neurological & Vascular Assessment
- Vascular: Distal pulses (dorsalis pedis and posterior tibial) were strong and palpable bilaterally. Capillary refill was brisk in all digits. No pallor, paresthesia, or poikilothermia were noted.
- Neurological: Intact sensation to light touch in the distributions of the saphenous, peroneal, and tibial nerves. Motor function of ankle dorsiflexion, plantarflexion, and great toe extension was preserved. Compartment pressures were not elevated.
Imaging & Diagnostics
Plain Radiographs
Initial radiographic evaluation included anteroposterior (AP), lateral, and oblique views of the left knee.
*
AP View:
Demonstrated a clear avulsion fracture of the tibial eminence, involving the intercondylar area. The fragment appeared partially displaced laterally and superiorly.
*
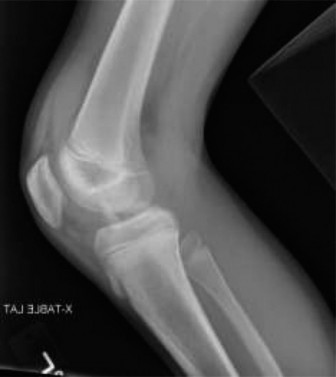
Lateral View:
Provided crucial information regarding the anterior displacement and superior migration of the fragment. A subtle "fleck sign" (osseous fragment from the lateral tibial plateau) was absent, suggesting no associated Segond fracture.
*
Oblique Views:
Further delineated the fracture morphology and confirmed the displacement.
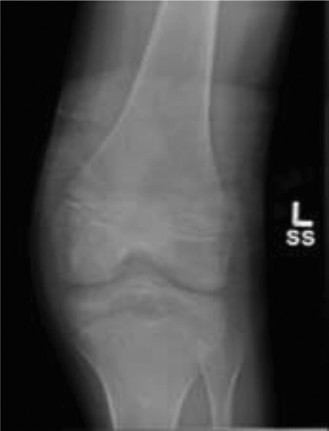
Figure 1: Pre-operative lateral radiograph demonstrating a displaced tibial eminence fracture, with superior and anterior migration of the avulsed fragment.
Computed Tomography (CT) Scan
Given the displacement and suspected intra-articular involvement, a CT scan with 3D reconstructions was obtained to further characterize the fracture and guide surgical planning.
*
Fracture Morphology:
The CT scan confirmed a Type III Tibial Eminence fracture according to the Meyers and McKeever classification, indicating complete avulsion and significant displacement of the intercondylar fragment. It also revealed a small degree of comminution at the posterior aspect of the avulsed fragment.
*
Articular Involvement:
The fracture involved the weight-bearing surface to a limited extent, but the primary concern was the detached ACL insertion and its mechanical implications.
*
Fragment Displacement:
The 3D reconstructions vividly demonstrated the superior and anterior displacement of the fragment, confirming its malposition.
*
Associated Findings:
No obvious depression of the tibial plateau or significant impaction was noted. The CT also helped to rule out large osteochondral fragments elsewhere in the joint. Importantly, it highlighted the potential for meniscal entrapment, as the fragment's displacement suggested a possible "bucket handle" type tear or entrapment of the anterior horn of the medial meniscus beneath the avulsed fragment.
Magnetic Resonance Imaging (MRI)
While not always acutely necessary for primary surgical planning of a displaced tibial eminence fracture, an MRI was obtained due to the high index of suspicion for associated soft tissue injuries and the patient's strong desire for an optimal outcome and return to sport.
*
Fracture Confirmation:
The MRI confirmed the tibial eminence avulsion fracture.
*
Ligamentous Assessment:
It unequivocally demonstrated the integrity of the PCL, MCL, and LCL. The ACL fibers were attached to the avulsed bony fragment.
*
Meniscal Evaluation:
The MRI revealed entrapment of the anterior horn of the medial meniscus, which was incarcerated beneath the displaced bony fragment, explaining the mechanical block to full extension. There was also evidence of edema in the anterior fat pad. No significant meniscal tears were noted apart from the entrapment.
*
Cartilage:
No significant chondral lesions were identified.
Templating
Pre-operative templating involved reviewing the CT images, particularly the 3D reconstructions, to conceptualize the reduction maneuver and select the appropriate fixation method. The size and shape of the avulsed fragment were carefully assessed to determine if screw fixation (e.g., 3.5mm cannulated screws) or suture fixation would be most appropriate. Given the fragment size and patient's athletic demands, screw fixation was deemed feasible and provided rigid fixation.
Differential Diagnosis
A thorough differential diagnosis is crucial in evaluating acute knee trauma with hemarthrosis and instability.
| Feature / Condition | Tibial Eminence Fracture (Case 36) | Isolated ACL Rupture (Intrasubstance) | Tibial Plateau Fracture (e.g., Schatzker II) | Complex Meniscal Tear (Bucket-Handle) |
|---|---|---|---|---|
| Mechanism of Injury | Valgus/varus stress with axial load and rotation, hyperextension | Non-contact deceleration, pivot, direct blow (hyperextension) | High-energy axial load with valgus/varus force, direct trauma | Twisting injury on a flexed, loaded knee, often with pivot |
| Primary Symptom | Acute pain, significant swelling, instability, mechanical block | Acute pain, "pop," rapid swelling, feeling of instability | Severe pain, gross swelling, inability to bear weight, potential deformity | Intermittent pain, locking/catching, effusion, instability |
| Physical Exam Findings | Gross effusion, limited ROM, anterior laxity (Lachman, anterior drawer), potential meniscal signs (e.g., block) | Gross effusion, anterior laxity (Lachman, anterior drawer), joint line tenderness | Gross swelling, ecchymosis, tenderness over plateau, crepitus, potential instability (varus/valgus) | Joint line tenderness, effusion, palpable clicking/locking, positive McMurray's test |
| Radiographs (X-ray) | Visible avulsion fragment from tibial eminence, displaced | Normal plain films (unless associated Segond fracture) | Depression/split of tibial plateau, articular step-off, metaphyseal involvement | Normal plain films (unless degenerative changes or loose body) |
| CT Scan | Confirms fragment size, displacement, comminution, articular involvement, meniscal entrapment | Normal bone; useful for associated osteochondral injuries | Detailed fracture pattern, articular congruence, bone loss, aids pre-op templating | Not primary for diagnosis; may show associated chondral or bony lesions |
| MRI | Confirms fracture, assesses meniscal entrapment, associated ligament/cartilage injuries (e.g., meniscal impaction) | Confirms ACL tear, assesses concomitant injuries (meniscus, MCL, bone bruise) | Useful for soft tissue injuries (meniscus, ligaments) associated with bone marrow edema | Confirms meniscal tear type, location, and extent, particularly bucket-handle |
| Treatment Considerations | ORIF for displaced fragments (Type II-IV), non-operative for non-displaced (Type I) | ACL reconstruction (often with rehabilitation program) | ORIF (if displaced/unstable/depressed), non-operative (if non-displaced/stable) | Arthroscopic repair or meniscectomy (based on tear type, stability, and patient factors) |
| Prognosis | Good with appropriate treatment, risk of stiffness, secondary OA, residual laxity | Good with reconstruction, risk of OA, re-tear | Variable, high risk of post-traumatic OA, stiffness, malunion, infection | Variable, risk of re-tear, potential for OA after meniscectomy |
Surgical Decision Making & Classification
Classification
Based on the radiographic and CT findings, Case 36 was classified as a
Meyers and McKeever Type III Tibial Eminence Fracture
.
*
Type I:
Non-displaced.
*
Type II:
Partially avulsed, with the anterior portion hinged upwards.
*
Type III:
Completely avulsed and displaced from its bed.
*
Type IV:
Comminuted fracture of the eminence.
This classification is critical in guiding treatment. Type I fractures are typically managed non-operatively with immobilization and protected weight-bearing. However, Type II, III, and IV fractures, especially in an active young patient with significant displacement and a mechanical block, warrant surgical intervention.
Why Operative Intervention?
The decision for operative management in Case 36 was clear due to several factors:
1.
Displacement (Type III fracture):
The completely avulsed and displaced fragment prevents accurate healing of the ACL attachment site, leading to persistent knee instability.
2.
Mechanical Block:
The fixed flexion deformity and inability to achieve full extension indicated mechanical impingement, confirmed by MRI revealing meniscal entrapment beneath the fragment. Non-operative management would not resolve this, leading to functional impairment and potential long-term issues.
3.
Patient Demands:
As a collegiate athlete, restoring full stability, ROM, and function is paramount for a successful return to sport. Non-operative treatment would likely result in chronic instability and inability to meet performance demands.
4.
Risk of Nonunion/Malunion:
Displaced fractures carry a higher risk of fibrous nonunion or malunion, which would compromise ACL function and knee kinematics.
5.
Addressing Associated Injuries:
Operative intervention allows for direct visualization and management of concomitant intra-articular pathologies, such as meniscal entrapment, which was identified on MRI.
Surgical Technique / Intervention
The surgical goal was to achieve anatomic reduction of the tibial eminence fragment and secure rigid internal fixation, facilitating early motion and rehabilitation, and restoring knee stability.
Timing of Surgery
Surgery was performed within 72 hours of injury, after initial swelling had sufficiently subsided to minimize soft tissue complications, yet before significant arthrofibrosis or fibrous healing of the fragment in a malpositioned state could occur.
Patient Positioning & Preparation
- The patient was placed supine on the operating table.
- A thigh tourniquet was applied and inflated to 300 mmHg after limb exsanguination.
- A lateral post was used to allow for controlled knee flexion to 90 degrees or more during the procedure.
- The limb was prepped and draped in a sterile fashion, ensuring access for standard arthroscopic portals and potential medial arthrotomy if conversion was necessary.
Arthroscopic Approach
An arthroscopic approach was chosen due to its advantages: superior visualization of the joint, ability to manage associated intra-articular pathologies, and reduced surgical morbidity compared to an open arthrotomy.
-
Portal Placement:
- Standard anterolateral and anteromedial portals were established. A superomedial portal was also created for inflow.
-
Diagnostic Arthroscopy:
- Initial arthroscopic inspection confirmed the Type III tibial eminence fracture with the ACL attached to the avulsed fragment.
- The anterior horn of the medial meniscus was found to be incarcerated beneath the displaced bony fragment.
- The joint was thoroughly irrigated to remove hemarthrosis and small debris.
-
Meniscal Release & Fragment Debridement:
- The incarcerated anterior horn of the medial meniscus was carefully released from beneath the fragment using an arthroscopic probe and shaver. This maneuver was crucial for achieving full reduction and preventing future impingement.
- Any fibrous tissue or hematoma from the fracture bed was debrided to expose fresh bone, promoting bony healing.
-
Reduction of the Fragment:
- Reduction was performed by placing the knee in near full extension, which tensed the PCL, pushing the fragment posteriorly.
- An arthroscopic probe or meniscal hook was used to manipulate the fragment anteriorly and inferiorly back into its anatomic bed. This required precise triangulation of instruments.
- Maintaining the knee in extension with valgus stress (if medial eminence) or varus stress (if lateral eminence) often aided in reduction. Once reduced, stability was assessed.
-
Fixation Technique (Screw Fixation):
- Given the size and integrity of the avulsed fragment, two 3.5mm cannulated cortical screws with washers were selected for fixation. This provided robust compression and resistance to pull-out.
- A guidewire was passed from the anteromedial tibia, approximately 1-2 cm distal to the joint line, under fluoroscopic guidance, aiming centrally through the reduced fragment. It's critical to ensure the guidewire does not enter the joint space prematurely or violate the growth plate if pediatric.
- The position of the guidewire and subsequent screw path were confirmed arthroscopically and fluoroscopically in both AP and lateral views to ensure accurate placement, avoidance of posterior cortex penetration, and optimal compression.
- The cannulated drill was used over the guidewire, followed by tapping, and then screw insertion. The first screw provided initial stability, and the second screw added rotational control and further compression.
- A second guidewire and screw were placed in a similar fashion, ensuring parallel or slightly divergent trajectories for optimal purchase.
- The screws were countersunk to prevent soft tissue irritation.
- Alternative: Suture Fixation: For highly comminuted fragments or pediatric cases where physeal sparing is crucial, suture fixation via transtibial tunnels is an excellent alternative. Non-absorbable sutures (e.g., FiberWire) are passed through the ACL substance or directly into the bony fragment, then retrieved through tibial drill tunnels and tied over a button or post on the anterior tibial cortex.

Figure 2: Post-operative AP radiograph showing anatomic reduction and stable internal fixation of the tibial eminence fracture with two cannulated screws.
Post-Fixation Assessment
- The knee was brought through a full range of motion under arthroscopic visualization to confirm stable fixation and anatomic reduction.
- Lachman and anterior drawer tests were re-performed to verify restoration of anterior stability. A firm endpoint was now achieved.
- No further mechanical block was observed with full extension.
- The tourniquet was deflated, hemostasis achieved, and portals closed with simple sutures. A sterile dressing was applied.
Post-Operative Protocol & Rehabilitation
The post-operative protocol is critical for preventing complications such as arthrofibrosis while protecting the repair.
Phase 1: Immediate Post-Operative (Weeks 0-2)
- Immobilization: Knee immobilizer or hinged knee brace locked in full extension for ambulation, worn continuously for the first week to protect the repair site.
- Weight-Bearing (WB): Non-weight bearing (NWB) with crutches for 0-2 weeks.
- ROM: Gentle passive ROM within a protected range (0-30 degrees flexion initially) is initiated immediately. Continuous Passive Motion (CPM) machine may be used. Avoid active hamstring contraction.
- Exercises: Quadriceps sets, gentle ankle pumps. Cryotherapy and elevation for swelling control.
Phase 2: Early Rehabilitation (Weeks 2-6)
- Immobilization: Hinged knee brace is unlocked to allow for progressive ROM.
- Weight-Bearing: Progress to partial weight bearing (PWB) with crutches (25-50% body weight) at 2-3 weeks, advancing to full weight bearing (FWB) by week 6, as tolerated and based on radiographic evidence of healing.
- ROM: Gradually increase active and passive flexion, aiming for 90 degrees by week 4 and full flexion by week 6. Continue to protect full extension.
- Exercises: Gentle closed-chain quadriceps strengthening (e.g., mini-squats with limited depth), hamstring curls (non-resistive initially), straight leg raises, core strengthening. Focus on regaining proprioception.
Phase 3: Intermediate Rehabilitation (Weeks 6-12)
- Weight-Bearing: Full weight bearing without assistive devices.
- ROM: Full, pain-free range of motion should be achieved.
- Strengthening: Advance closed-chain exercises (e.g., leg press, wall sits), introduce open-chain exercises (e.g., knee extension machine with light resistance, leg curls). Focus on eccentric control and single-leg balance.
- Activities: Stationary cycling, swimming (kickboard initially). Light impact activities only if cleared by surgeon.
Phase 4: Advanced Rehabilitation (Months 3-6)
- Strengthening: Progressive resistance training, plyometrics, agility drills, sport-specific exercises. Emphasis on dynamic stability and neuromuscular control.
- Functional Training: Gradual return to running and cutting activities, under supervision.
- Return to Sport: Typically not before 6-9 months post-operatively, after achieving symmetric strength (isokinetic testing >90% contralateral limb), full ROM, and passing functional performance tests (e.g., hop tests). Clearance is based on clinical and functional assessment.
Potential Complications
- Arthrofibrosis/Stiffness: Most common complication, hence the emphasis on early controlled motion.
- Loss of Reduction/Fixation Failure: Rare with appropriate surgical technique and post-operative protocol.
- Nonunion/Malunion: Can lead to persistent instability or impingement.
- Residual Laxity: Due to inadequate reduction or healing.
- Hardware Complications: Screw irritation requiring removal.
- Post-traumatic Osteoarthritis: Long-term risk, especially with significant chondral damage or persistent instability.
- Infection: Low risk with arthroscopic surgery.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- High Index of Suspicion: Always suspect a tibial eminence fracture in young, active patients presenting with acute knee pain, effusion, and anterior instability following a relevant mechanism (e.g., hyperextension, valgus/varus stress with axial load).
-
Imaging Essentials:
- Plain Radiographs: Often diagnostic, especially lateral view for displacement.
- CT Scan (with 3D recons): Absolutely essential for precise characterization of fragment size, displacement, comminution, and articular involvement. Invaluable for pre-operative planning.
- MRI: Crucial for identifying associated soft tissue injuries, particularly meniscal entrapment (which causes a mechanical block) and concomitant ligamentous injuries.
- Arthroscopic Advantage: The arthroscopic approach is generally preferred. It offers superior intra-articular visualization, allows for concurrent treatment of meniscal tears or entrapment, facilitates thorough debridement, and minimizes soft tissue dissection compared to open approaches.
- Anatomic Reduction is Key: Achieving true anatomic reduction of the fragment is paramount for restoring ACL function and knee stability. The knee extension maneuver (tensing the PCL) can aid in reduction of anteriorly displaced fragments.
- Rigid Fixation: Secure and stable fixation is vital to allow for early, controlled range of motion and prevent arthrofibrosis. Cannulated screws offer excellent compression and stability for suitable fragments. Suture fixation is a viable alternative, especially for comminuted fragments or when physeal sparing is necessary in skeletally immature patients.
- Early Controlled Motion: Initiate passive and controlled active range of motion as soon as possible post-operatively to prevent arthrofibrosis, which is a significant complication. However, respect the repair and avoid excessive stress, particularly anterior tibial translation.
Pitfalls
- Missing Concomitant Injuries: Failing to identify or adequately address associated meniscal tears (especially entrapped menisci), collateral ligament injuries, or osteochondral lesions can lead to persistent pain, instability, or mechanical symptoms. MRI is key here.
- Inadequate Reduction: A suboptimally reduced fragment can result in residual anterior laxity, persistent mechanical impingement, or early post-traumatic osteoarthritis due to altered kinematics.
- Aggressive Post-operative Rehabilitation: Overly aggressive weight-bearing or range of motion exercises in the initial phases can jeopardize the repair, leading to loss of reduction or fixation failure. Conversely, prolonged immobilization leads to stiffness.
- Inappropriate Fixation Choice: Selecting a fixation method unsuitable for the fracture type (e.g., absorbable pins for a large fragment in a high-demand athlete) or fragment size/quality can lead to failure.
- Neurovascular Compromise: Although rare, failing to recognize and manage acute compartment syndrome or neurovascular injury (e.g., common peroneal nerve palsy in lateral eminence fractures) can have devastating consequences. Regular assessment is critical.
- Fixation Placement Errors: Malpositioned screws (e.g., too long, into the joint, through the growth plate) or inadequate tunnels for sutures can cause iatrogenic injury or lead to fixation failure. Fluoroscopy and arthroscopic visualization are essential during placement.
- Ignoring a Mechanical Block: Persistent inability to achieve full extension post-injury should immediately raise suspicion of meniscal entrapment and mandates further investigation (MRI) and surgical release.
Clinical & Radiographic Imaging