Introduction & Epidemiology
Congenital Vertical Talus (CVT), also known as congenital convex pes valgus (CCPV) or congenital rocker-bottom foot, is a rare and complex congenital foot deformity. It is characterized by an irreducible dorsal dislocation of the navicular bone on the talar head, a fixed equinus deformity of the talus, and a valgus hindfoot with compensatory forefoot abduction and dorsiflexion. This triad results in a rigid, non-reducible "rocker-bottom" appearance, distinguishing it from more benign and flexible flatfoot variants.
The true incidence of CVT is estimated to be approximately 1 in 10,000 live births, though accurate epidemiological data are scarce due to its rarity and potential for misdiagnosis. CVT can occur as an isolated deformity, but it is frequently associated with underlying systemic conditions in up to 50-60% of cases. These include:
* Neurological disorders: Spina bifida, cerebral palsy, myelomeningocele.
* Genetic syndromes: Arthrogryposis multiplex congenita, Marfan syndrome, Ehlers-Danlos syndrome, trisomy 13, 15, and 18.
* Neurofibromatosis.
* Prune Belly syndrome.
Early and accurate diagnosis is paramount to differentiate true CVT from flexible flatfoot, calcaneovalgus foot, or other more common and less severe conditions that do not require aggressive intervention. Clinical examination reveals the characteristic rocker-bottom shape, a prominent talar head palpable in the plantar aspect of the foot, and a stiff, irreducible dorsiflexed forefoot. Radiographic assessment, particularly true lateral weight-bearing (or simulated weight-bearing) views, is essential for confirmation. Key radiographic findings include:
* A vertically oriented talus (equinus).
* Dorsal dislocation of the navicular on the talar head.
* Increased talocalcaneal angle and talo-first metatarsal angle (Meary's angle).
* Hindfoot valgus.
Untreated CVT leads to significant functional impairment, pain, difficulty with shoe wear, and abnormal gait patterns due to the rigid nature of the deformity and inability to adapt to uneven surfaces. Therefore, early intervention, predominantly surgical, is the accepted standard of care.
Surgical Anatomy & Biomechanics
Congenital Vertical Talus involves a profound and rigid disruption of the normal osseous and soft tissue architecture of the foot and ankle. Understanding these specific derangements is critical for effective surgical planning and execution.
Osseous Deformities
- Talus: The talus is fixed in an exaggerated plantarflexed position, appearing "vertical" on lateral radiographs. This position is a primary driver of the deformity. The body of the talus remains within the ankle mortise, but its head and neck are directed plantarly.
- Navicular: The most pathognomonic finding is the irreducible dorsal dislocation of the navicular onto the dorsal aspect of the talar head and neck. This prevents normal midfoot articulation and contributes significantly to the rigidity.
- Calcaneus: The calcaneus is in a position of marked valgus and varying degrees of dorsiflexion relative to the talus. The subtalar joint is often subluxated or dislocated, further contributing to hindfoot instability and valgus.
- Forefoot: The forefoot is abducted and dorsiflexed at the midtarsal joints (talonavicular and calcaneocuboid), creating the "rocker-bottom" appearance, with the plantar prominence of the talar head serving as the primary weight-bearing point.
- Cuboid: The cuboid may be laterally displaced or relatively abducted in relation to the calcaneus.
Soft Tissue Contractures
The osseous deformities are maintained and exacerbated by severe contractures of multiple soft tissue structures, both ligamentous and muscular:
*
Dorsal Talonavicular Capsule:
Thickened and contracted, preventing reduction of the navicular.
*
Spring Ligament (Plantar Calcaneonavicular Ligament):
Often elongated, stretched, and positioned dorsally, but its functional relationship is distorted, contributing to the instability. The medial components of the spring ligament are particularly affected.
*
Deltoid Ligament:
Contracted and tight, contributing to hindfoot valgus.
*
Peroneal Tendons (Peroneus longus and brevis):
Severe contracture and spasm of these tendons are common, leading to active forefoot abduction and hindfoot valgus. They tether the lateral aspect of the foot.
*
Achilles Tendon (Gastrocnemius-soleus complex):
Markedly contracted, maintaining the talus in equinus and preventing ankle dorsiflexion.
*
Posterior Ankle Capsule and Subtalar Joint Capsule:
Contracted, preventing dorsiflexion of the talus and proper subtalar articulation.
*
Plantar Fascia and Short Plantar Ligaments:
Contracted, especially along the lateral column, contributing to midfoot rigidity.
*
Tibialis Anterior:
Can be contracted, further contributing to forefoot dorsiflexion.
Biomechanics of Deformity
The fixed vertical orientation of the talus acts as a fulcrum, causing the forefoot to dorsiflex and abduct relative to the hindfoot. The navicular's dorsal dislocation onto the talus prevents normal articulation and midfoot collapse, leading to a rigid arch. The hindfoot valgus further destabilizes the subtalar joint. This composite deformity results in:
*
Loss of foot flexibility:
The foot is unable to absorb shock or adapt to uneven surfaces.
*
Abnormal weight-bearing:
The prominent talar head on the plantar aspect becomes a painful weight-bearing area, leading to callus formation and skin breakdown.
*
Inefficient gait:
Without a functional heel strike and push-off mechanism, gait is compensated, leading to increased energy expenditure and potential pain in other joints (e.g., knee, hip, spine).
*
Muscle imbalances:
The contracted peroneal tendons, Achilles, and plantar fascia perpetuate the deformity, while muscles like the tibialis posterior, which normally supports the arch, are often stretched and dysfunctional.
Indications & Contraindications
Treatment for congenital vertical talus is primarily surgical due to the rigid and progressive nature of the deformity and the significant functional impairment it causes if left untreated. Non-operative management typically serves as a pre-surgical adjunct or for misdiagnosed flexible conditions.
Indications for Operative Management
- Confirmed Diagnosis of Congenital Vertical Talus (CVT): This is the primary indication, established through characteristic clinical findings (rigid rocker-bottom foot, palpable plantar talar head, irreducible deformity) and radiographic confirmation (vertical talus, dorsal talonavicular dislocation, hindfoot valgus).
- Failure of Non-Operative Management (if attempted): While true CVT rarely responds to isolated non-operative treatment, some protocols involve an initial period of serial casting (e.g., Dobbs method). Failure to achieve or maintain reduction and correction with casting necessitates surgical intervention.
- Progressive Deformity: Any evidence of worsening clinical or radiographic parameters over time, particularly in untreated or inadequately treated cases.
- Age: Optimal timing for primary surgical correction is generally between 6 to 12 months of age. This allows for sufficient bone ossification for K-wire fixation while soft tissues are still relatively pliable, minimizing the extent of surgical release required. Intervention before ambulation is preferred to prevent secondary compensatory deformities and pain.
- Functional Impairment: Anticipated or existing difficulties with ambulation, shoe wear, and pain are clear indications.
Contraindications for Operative Management
- Misdiagnosis: The most critical "contraindication" is an incorrect diagnosis. Flexible flatfoot, calcaneovalgus foot, or other benign conditions should not be subjected to CVT surgery. These conditions typically respond to observation, stretching, or orthotics.
- Severe Systemic Comorbidities: Patients with severe cardiac, pulmonary, or neurological conditions that preclude safe general anesthesia or have a significantly shortened life expectancy may be considered for palliative non-operative care.
- Active Local Infection: Any active infection in the foot or ankle region should be fully treated and resolved before elective surgery.
- Extreme Prematurity/Low Weight: Surgery is generally delayed until the infant is of appropriate size and maturity to minimize anesthetic risks and allow for better bone quality for fixation.
Summary Table: Operative vs. Non-Operative Indications
| Indication Category | Operative Management | Non-Operative Management (Limited Scope for True CVT) |
|---|---|---|
| Diagnosis | Confirmed Congenital Vertical Talus (CVT) | Flexible Flatfoot, Calcaneovalgus Foot, other benign variants |
| Foot Rigidity | Rigid, irreducible deformity | Flexible, passively correctable deformity |
| Radiographic Findings | Fixed dorsal talonavicular dislocation, vertical talus | Reducible talonavicular joint, flexible talus position |
| Functional Status | Significant or anticipated functional limitations/pain | Asymptomatic, no functional impairment (often for misdiagnosed conditions) |
| Age for Intervention | Typically 6-12 months for primary correction | Initial serial casting (Ponseti-like) for very young infants or as part of a staged approach (e.g., Dobbs method), aiming to improve reducibility. Rarely definitive. |
| Associated Conditions | Often present, requiring comprehensive interdisciplinary care | Isolated deformity (if any non-operative approach is attempted for a mild variant) |
| Prior Treatment Outcome | Failure to correct or maintain correction with non-operative methods | Successful correction and maintenance with casting/orthotics (rare for true CVT) |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential to ensure a successful outcome in CVT correction, considering the complex anatomy and potential for recurrence.
Pre-Operative Assessment
- Clinical Evaluation: Thorough assessment of the foot deformity, flexibility, skin integrity, and neurovascular status. Documentation of the rocker-bottom foot, hindfoot valgus, and forefoot abduction/dorsiflexion. Assessment for associated conditions.
-
Radiographic Imaging:
- AP and Lateral Views: Standard radiographs are crucial. Lateral views should ideally be weight-bearing or simulated weight-bearing (e.g., using a specialized frame or applying pressure to the plantar aspect of the foot with the ankle dorsiflexed to 90 degrees) to demonstrate the fixed equinus of the talus and dorsal dislocation of the navicular.
- Forced Dorsiflexion/Plantaflexion Stress Views: Lateral views with maximal forced ankle dorsiflexion and plantarflexion of the hindfoot can help assess the rigidity of the talus and the reducibility of the talonavicular joint. In true CVT, the talus remains in equinus even with forced dorsiflexion.
- Kite Views (AP view of the foot with ankle dorsiflexed): Useful for assessing hindfoot alignment.
- MRI: Rarely required for routine diagnosis, but may be considered in atypical presentations, for assessing cartilaginous talonavicular joint in very young infants, or to rule out other anomalies.
Anesthetic Considerations
- General anesthesia is typically administered.
- A regional block, such as a caudal epidural or popliteal nerve block, can be used as an adjunct for post-operative pain control.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Hip Roll: A small towel roll or sandbag is placed under the ipsilateral hip to prevent external rotation of the limb, ensuring the foot is positioned anatomically for the surgical approach.
- Tourniquet: A sterile tourniquet is applied to the proximal thigh of the operative limb. Inflation pressure and duration should follow institutional guidelines, typically 250-300 mmHg for infants.
- Prepping and Draping: The foot and ankle are prepped with an antiseptic solution (e.g., chlorhexidine or povidone-iodine) and draped in a sterile fashion to allow complete visualization and manipulation of the foot, ankle, and distal leg. This includes draping above the ankle to allow for Achilles tendon lengthening and full range of motion.
- Image Intensifier: A C-arm fluoroscope is brought into the sterile field and positioned to allow for immediate AP and lateral radiographic views during the procedure to confirm reduction and K-wire placement.
Detailed Surgical Approach / Technique
The goal of surgical correction for CVT is to achieve a plantigrade, flexible, and functional foot. This involves extensive soft tissue releases, reduction of dislocated joints, and temporary K-wire fixation. While various approaches exist, the comprehensive open reduction via a Cincinnati incision remains a well-established method, particularly for rigid deformities. More recently, limited posterior and lateral releases with percutaneous pinning, often combined with serial casting (Dobbs method), has gained popularity.
Comprehensive Open Reduction (e.g., Cincinnati Incision)
This approach provides excellent exposure to all aspects of the foot and ankle, allowing for thorough soft tissue release and accurate joint reduction.
1. Incision
- A single, curved Cincinnati incision is typically employed. This incision starts just posterior to the lateral malleolus, curves transversely across the plantar aspect of the ankle (distal to the malleoli), and ends just posterior to the medial malleolus.
- Alternatively, a dual incision approach (separate medial and lateral incisions) can be used, particularly in cases where minimizing scar burden is prioritized, though exposure may be less comprehensive.
2. Dissection and Soft Tissue Releases
Careful dissection is performed to identify and protect neurovascular structures (superficial peroneal nerve laterally, saphenous nerve and great saphenous vein medially).
-
Lateral Aspect:
- Release the peroneal tendons (peroneus longus and brevis) from their sheaths, allowing them to retract. Z-lengthening of these tendons may be required if severely contracted, though often simply releasing them from their tethering effect is sufficient.
- Capsulotomy of the lateral subtalar joint.
- Release of the calcaneofibular ligament and lateral talocalcaneal ligament.
- Release of the calcaneocuboid joint capsule, if contracted.
-
Medial Aspect:
- Release of the deltoid ligament (superficial and deep portions).
- If severely contracted, the posterior tibial tendon can be Z-lengthened.
- Capsulotomy of the medial talonavicular joint.
- Release of the deep fascia and soft tissues surrounding the talonavicular joint.
-
Posterior Aspect:
- A formal Z-lengthening of the Achilles tendon (gastrocnemius-soleus complex) is performed to correct the talar equinus.
- Posterior ankle capsulotomy and posterior subtalar capsulotomy are performed to further mobilize the talus and calcaneus.
- The flexor hallucis longus and flexor digitorum longus tendons may require percutaneous or open lengthening if found to be tight after initial releases.
-
Plantar Aspect:
- Release of the plantar fascia and abductor hallucis origin if contributing to the rigidity. The short plantar ligaments (calcaneocuboid ligament) may also require release.
3. Reduction Sequence
This is the most critical phase, focusing on correcting the multiplanar deformities in a specific order:
- Talus Dorsiflexion: After posterior soft tissue releases (Achilles lengthening, posterior capsule releases), apply gentle anterior and superior force to the calcaneus while stabilizing the tibia, aiming to dorsiflex the talus within the ankle mortise. This brings the talus out of its fixed equinus.
-
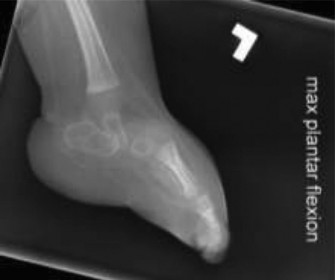
Navicular Reduction onto the Talus:
This is often the most challenging step. The dorsal talonavicular capsule is incised. With counterpressure on the talar head, the navicular is manually manipulated from its dorsal position onto the plantar aspect of the talar head. This usually requires significant force and persistent stretching of the surrounding soft tissues, especially the spring ligament complex, which may be elongated but still distorted. Ensure the entire talar head is seated within the navicular. This image highlights the severe dislocation and structural derangement often seen preoperatively.
- Calcaneus Valgus Correction and Subtalar Joint Reduction: Once the talonavicular joint is reduced, the calcaneus is manipulated to correct the valgus deformity and properly articulate with the talus in the subtalar joint.
- Forefoot Abduction/Dorsiflexion Correction: The forefoot is then adducted and plantarflexed to align with the hindfoot, creating a plantigrade foot. The calcaneocuboid joint may need further manipulation or release.
4. Fixation
Temporary K-wire fixation is essential to maintain the achieved correction while soft tissues heal.
- Talonavicular Joint: A K-wire (typically 1.6mm or 2.0mm) is drilled from the dorsal-medial aspect of the navicular, across the reduced talonavicular joint, and into the talus. Ensure the wire provides stable fixation without impinging on the articular surfaces. Confirm reduction and K-wire position with fluoroscopy.
- Subtalar Joint: A second K-wire is usually placed from the plantar-lateral aspect of the calcaneus, across the subtalar joint, and into the talus, providing hindfoot stability and correcting valgus.
- Calcaneocuboid Joint: If significant instability remains at the calcaneocuboid joint, a third K-wire may be placed across this joint.
5. Final Assessment and Closure
- Before closing, clinically assess the foot for full range of motion, plantigrade alignment, and stability.
-
Obtain AP and lateral fluoroscopic images to confirm proper alignment of all joints and satisfactory K-wire placement. Ensure the talonavicular reduction is concentric and the talus is no longer in equinus. This image demonstrates a successfully reduced foot with K-wire fixation.
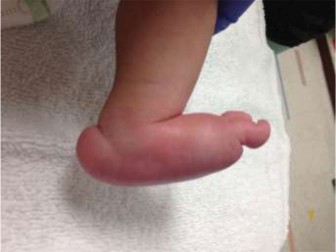
- Close the soft tissues in layers, ensuring meticulous hemostasis. The skin is closed with absorbable sutures.
- Apply a well-padded, above-knee cast with the knee flexed to 30-45 degrees to prevent cast rotation and maintain foot position (neutral dorsiflexion, slight hindfoot varus, forefoot adduction).
Minimally Invasive Approaches (Dobbs Method)
The Dobbs method combines initial serial casting, similar to the Ponseti method for clubfoot, with a limited surgical release.
*
Serial Casting:
Weekly manipulation and casting aim to stretch contracted soft tissues and gradually reduce deformities, particularly focusing on the midfoot and hindfoot.
*
Limited Surgical Release:
After a period of casting (typically 6-12 weeks), if full reduction is not achieved, a limited surgical release is performed. This often includes:
* Percutaneous Achilles tendon lengthening.
* Limited posterior ankle and subtalar capsulotomy (often percutaneously or through a small incision).
* Percutaneous pinning of the talonavicular and subtalar joints.
*
Advantages:
Potentially less extensive scarring, fewer wound complications, and faster recovery.
*
Disadvantages:
May not be suitable for all rigid deformities, requires consistent casting and compliance, and the long-term recurrence rates compared to extensive open reduction are still being studied.
The choice of surgical technique depends on the surgeon's experience, the rigidity of the deformity, and the age of the patient. Regardless of the approach, the fundamental principles of achieving accurate anatomical reduction and stable fixation remain paramount.
Complications & Management
Despite meticulous surgical technique, complications are not uncommon in the treatment of congenital vertical talus due to the complexity of the deformity and the inherent propensity for recurrence. Vigilant post-operative monitoring and aggressive management are crucial for optimal outcomes.
Common Complications and Management Strategies
| Complication | Incidence | Management / Salvage Strategy |
|---|---|---|
| Recurrence of Deformity | High (20-50%), especially with growth | Initial: Serial casting, bracing, orthotics. Persistent/Severe: Re-operation (further soft tissue releases, osteotomies e.g., calcaneal lengthening osteotomy, cuboid osteotomy), external fixation. In older children, subtalar or triple arthrodesis may be considered. |
| Residual Deformity (e.g., Pes Planovalgus) | Common (variable) | Orthotics, bracing (AFO). Secondary procedures such as calcaneal osteotomy, cuboid osteotomy, or subtalar fusion if symptomatic and severe. |
| Stiffness / Limited Range of Motion | Common | Aggressive physical therapy, stretching, bracing. Persistent stiffness may necessitate further releases or arthrodesis in adulthood. |
| Wound Complications | 5-15% | Local wound care, antibiotics for superficial infection, debridement for dehiscence. For severe cases, plastic surgery consultation for flap coverage. |
| Superficial Infection (K-wire sites) | 1-5% | Oral antibiotics, local wound care. K-wire removal if infection persists or deepens. |
| Deep Infection | <1% | Intravenous antibiotics, surgical irrigation and debridement, K-wire removal. May require hardware removal and re-fixation after infection control. |
| Neurovascular Injury | Rare (<1%) | Careful dissection. If identified intraoperatively, primary repair. Post-operatively, supportive care; may require nerve grafting if severe deficit. |
| K-wire Migration / Breakage | <5% | K-wire removal. Re-insertion if stability compromised, or cast management if appropriate. |
| Avascular Necrosis (AVN) of Talus | Rare (<1%) | Protective weight-bearing, bracing. May lead to talar collapse and eventually require tibiotalocalcaneal arthrodesis. |
| Overcorrection / Undercorrection | Variable | Undercorrection: Most common, often leads to recurrence; requires re-operation. Overcorrection (e.g., severe clubfoot-like deformity): Rare, may require reverse serial casting, orthotics, or corrective osteotomies. |
| Growth Disturbances | Rare, long-term | Regular follow-up, monitoring limb length discrepancy or angular deformities. May require epiphysiodesis or lengthening procedures in severe cases. |
General Management Principles
- Early Recognition: Prompt identification of complications is crucial. Regular clinical examinations and radiographic follow-ups are essential.
- Conservative Measures First: For recurrence or residual deformities, an initial trial of non-operative measures (serial casting, bracing, orthotics) may be attempted, especially in younger children.
- Revision Surgery: Many complications, particularly recurrence, often necessitate revision surgery. This can involve repeat soft tissue releases, tendon transfers, or osseous procedures (e.g., calcaneal lengthening osteotomy, cuboid shortening osteotomy, or in older children, triple arthrodesis).
- Multidisciplinary Approach: Management of CVT and its complications often benefits from a team approach involving orthopedic surgeons, physical therapists, orthotists, and possibly geneticists or neurologists if underlying conditions are present.
- Patient/Family Education: Thoroughly educate parents about the high potential for recurrence and the need for long-term follow-up and bracing to maintain correction.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following congenital vertical talus correction is a critical component for maintaining surgical correction, promoting soft tissue healing, preventing recurrence, and ultimately achieving a functional, plantigrade foot. The protocol typically involves distinct phases of immobilization, protection, and activity progression.
Phase 1: Initial Immobilization (0-6/8 weeks post-op)
- Casting: Immediately post-operatively, an above-knee plaster cast is applied. The knee is typically flexed to 30-45 degrees to prevent rotation of the cast and to relax the gastrocnemius muscle. The foot is maintained in neutral dorsiflexion, slight hindfoot varus, and forefoot adduction.
- K-wires: K-wires remain in situ for the entire duration of this phase, providing internal stability.
- Cast Changes: The cast is typically changed at regular intervals (e.g., 2-3 weeks) to inspect the wound, check for skin irritation, and ensure the foot position is maintained. This also allows for serial radiographs to confirm alignment.
- Weight-Bearing: Strict non-weight-bearing is maintained on the operative foot. Crutches or a wheelchair are used for mobility, depending on the child's age and ability.
- Monitoring: Vigilant monitoring for signs of infection (especially at K-wire sites), neurovascular compromise, or cast complications (e.g., pressure sores).
Phase 2: K-wire Removal and Transition to Partial Weight-Bearing (6/8-12 weeks post-op)
- K-wire Removal: K-wires are typically removed at 6 to 8 weeks post-surgery in the clinic or operating room, under local anesthesia or light sedation.
- Casting: Following K-wire removal, the patient is transitioned to a below-knee walking cast or a controlled ankle motion (CAM) boot.
- Weight-Bearing Progression: Partial weight-bearing is initiated, gradually progressing to full weight-bearing as tolerated. Physical therapy may begin with gentle range of motion exercises for the ankle and foot, focusing on dorsiflexion and inversion.
- Orthotics/Bracing: Preparation for custom ankle-foot orthoses (AFOs) or dynamic foot orthoses (DFOs) is initiated. These are crucial for long-term maintenance of correction.
Phase 3: Orthotic Management and Active Rehabilitation (12 weeks to Skeletal Maturity)
- Orthotic Use: Custom-molded AFOs (or similar rigid braces) are essential and worn for extended periods, typically full-time (day and night) for the first 6-12 months, then transitioning to night-time wear and during high-impact activities for several years until skeletal maturity. The orthosis helps to maintain the correction of the talonavicular joint, prevent hindfoot valgus, and support the longitudinal arch.
-
Physical Therapy:
- Range of Motion: Continue active and passive range of motion exercises for the ankle and foot, emphasizing dorsiflexion and inversion to counteract the deforming forces.
- Strengthening: Strengthen intrinsic foot muscles, as well as extrinsic muscles (e.g., tibialis posterior, tibialis anterior) to improve dynamic arch support and muscle balance.
- Balance and Proprioception: Exercises to improve balance, coordination, and proprioception.
- Gait Training: Address any compensatory gait patterns, encouraging a normal heel-toe gait.
- Stretching: Ongoing stretching of any tight soft tissues (e.g., Achilles tendon, peroneal muscles).
- Activity Progression: Gradual return to age-appropriate activities and sports. High-impact sports may require continued orthotic use.
- Parental Education: Crucial to educate parents on the importance of consistent orthotic wear, home stretching programs, and the need for long-term follow-up due to the high risk of recurrence.
Long-Term Follow-up
- Regular follow-up appointments (e.g., every 6-12 months) are necessary until skeletal maturity.
- Clinical examination and standing radiographs are performed at each visit to monitor for signs of recurrence, residual deformity, or compensatory changes.
- Adjustments to orthotics or physical therapy programs are made as needed.
- Secondary procedures (e.g., osteotomies, further soft tissue releases) may be considered if recurrence or significant residual deformity develops despite non-operative management.
The success of CVT correction relies not only on meticulous surgery but also on a diligent and sustained post-operative rehabilitation program, emphasizing orthotic use and regular follow-up to guide growth and maintain the corrected anatomy.
Summary of Key Literature / Guidelines
The understanding and management of Congenital Vertical Talus (CVT) have evolved significantly over the past century. Early approaches were often limited, leading to poor outcomes. Modern literature emphasizes early diagnosis, comprehensive surgical correction, and prolonged post-operative management.
Historical Context and Evolution of Treatment
Historically, CVT was treated with various non-operative methods, including prolonged casting, with universally poor results due to the rigid nature of the deformity. Early surgical attempts were often piecemeal, addressing only parts of the deformity, and also had high rates of recurrence.
The concept of comprehensive one-stage open reduction, involving extensive soft tissue releases, talonavicular reduction, and fixation, gained prominence in the mid-20th century. Key contributions by surgeons like Coleman, Osmond-Clarke, and Eyre-Brook established the principles of releasing contracted structures and achieving anatomical alignment. The Cincinnati incision became a favored approach due to its extensive exposure.
Current Paradigms: Open Reduction vs. Minimally Invasive Techniques
The current literature presents two primary surgical paradigms:
-
Comprehensive One-Stage Open Reduction:
- Proponents: Advocates for this approach (e.g., Coleman, Osmond-Clarke, and many traditional pediatric orthopedic surgeons) argue that it provides the most complete release of contracted structures and ensures precise anatomical reduction of the talonavicular and subtalar joints under direct visualization.
- Evidence: Studies on comprehensive open reduction consistently report good to excellent outcomes in a significant majority of patients, with the caveat of a substantial complication rate, primarily recurrence and stiffness, necessitating long-term follow-up and bracing. The potential for wound complications and extensive scarring is also noted.
- Considerations: This remains a robust option, particularly for older children, very rigid deformities, or cases of recurrence after less invasive attempts.
-
Minimally Invasive (Dobbs Method) / Limited Open Release with Serial Casting:
- Proponents: Dr. Matthew Dobbs introduced a less invasive approach in the early 2000s, inspired by the success of the Ponseti method for clubfoot. This method involves initial serial casting to stretch soft tissues, followed by a limited posterior and lateral release (Achilles lengthening, posterior capsulotomy, subtalar release), and percutaneous talonavicular pinning.
- Evidence: Early and mid-term results from Dobbs and other groups suggest comparable success rates to extensive open reduction, with potentially lower rates of wound complications and less scarring. Recurrence rates, however, remain a concern, emphasizing the need for diligent bracing. The appeal lies in its less aggressive surgical footprint.
- Considerations: This method requires significant experience with manipulative techniques and precise percutaneous pinning. It may not be suitable for all cases, especially those with severe, unyielding rigidity or older children where soft tissues are less amenable to stretching.
Key Literature Highlights and Consensus Points
- Early Intervention: There is a broad consensus that CVT should be treated early, ideally between 6 to 12 months of age. Early intervention minimizes the development of secondary deformities, prevents the formation of resistant contractures, and utilizes the pliability of infant tissues.
- Importance of Talonavicular Reduction: All effective treatment methods, whether open or minimally invasive, prioritize the anatomical reduction and stable fixation of the talonavicular joint. This is considered the cornerstone of correcting the entire deformity.
- Long-term Follow-up and Bracing: The literature consistently emphasizes the high potential for recurrence of the deformity (ranging from 20% to 50% or even higher in some series). Therefore, long-term clinical and radiographic follow-up until skeletal maturity, coupled with consistent use of custom orthoses (AFOs), is paramount to maintain correction and address any evolving deformities.
- Associated Conditions: The high incidence of associated neurological or genetic syndromes means a multidisciplinary approach is often beneficial for overall patient care. The presence of these conditions can also influence surgical outcomes and recurrence rates.
- Functional Outcomes: While cosmetic and radiographic correction are important, the primary goal is to achieve a functional, plantigrade foot that allows for pain-free ambulation and shoe wear. Most studies report good functional outcomes with both open and minimally invasive techniques, provided recurrence is managed.
Future Directions
Ongoing research aims to further refine surgical techniques, improve long-term recurrence rates, and better understand the genetic and developmental causes of CVT. The debate between extensive open vs. minimally invasive approaches continues, with both having their place depending on the specific patient presentation and surgeon experience. Regardless of the chosen path, successful management hinges on a thorough understanding of the pathology, meticulous surgical correction, and dedicated post-operative care.
