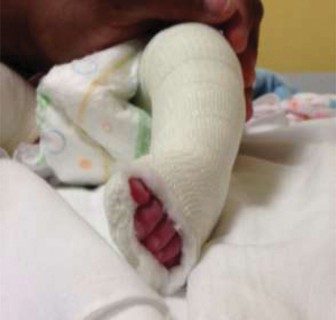
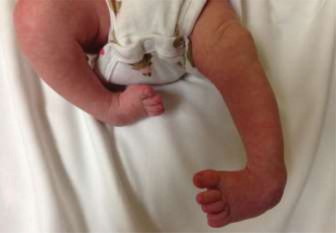
Introduction & Epidemiology
Congenital Talipes Equinovarus (CTEV), commonly known as clubfoot, is a complex three-dimensional deformity of the foot and ankle, presenting as a combination of hindfoot equinus and varus, midfoot cavus, and forefoot adduction. It represents one of the most common musculoskeletal birth defects, with an estimated incidence ranging from 1 to 2 per 1,000 live births globally. A male predominance is observed, with a male-to-female ratio of approximately 2:1. Bilateral involvement occurs in about 30-50% of cases. While idiopathic clubfoot is the most prevalent form, CTEV can also be associated with underlying syndromes such as arthrogryposis, spina bifida, or other neuromuscular conditions. Genetic factors are increasingly recognized, with studies indicating a multifactorial inheritance pattern and highlighting genes like PITX1 .
The pathoanatomy of clubfoot involves a C-shaped deformity characterized by contracted medial and posterior soft tissues. Key structural abnormalities include plantarflexion, internal rotation, and medial displacement of the talus, leading to its head being uncovered by the navicular. The calcaneus is in equinus, varus, and adducted beneath the talus. The navicular and cuboid are medially displaced relative to the talus and calcaneus, respectively, contributing to forefoot adduction and cavus. From a functional perspective, muscle imbalances and altered tendon dynamics play a significant role in maintaining and exacerbating these deformities. Specifically, the anterior tibialis tendon, typically an ankle dorsiflexor and foot invertor, can be abnormally positioned or contracted, contributing to the persistent cavus and forefoot adduction. Its assessment is crucial for both diagnostic and therapeutic decision-making in resistant or recurrent cases.
The Ponseti method, involving serial manipulation and casting followed by percutaneous Achilles tenotomy and foot abduction bracing, is the globally recognized gold standard for idiopathic clubfoot treatment, demonstrating success rates exceeding 90%. However, a subset of patients may present with resistant deformities, non-compliance with bracing, or relapse, necessitating surgical intervention. Understanding the specific anatomical contributions of tendons, especially the anterior tibialis, is paramount in these surgical scenarios.
Surgical Anatomy & Biomechanics
A thorough understanding of the anatomical derangements and their biomechanical consequences is fundamental for effective surgical correction of pediatric clubfoot. The deformity involves all articulations distal to the ankle joint, most notably the talonavicular, talocalcaneal, and calcaneocuboid joints.
Osseous Deformities
- Talus: The talus is universally in a position of plantarflexion and internal rotation within the ankle mortise. Its head is medially and plantarly deviated, often significantly uncovered by the navicular.
- Calcaneus: The calcaneus is held in equinus, varus, and adduction beneath the talus. Its anterior process is plantarflexed.
- Navicular: The navicular is medially displaced and often subluxed on the talar head, contributing to the forefoot adduction.
- Cuboid: The cuboid is also medially displaced relative to the calcaneus.
- Cuneiforms & Metatarsals: The forefoot, including the cuneiforms and metatarsals, is in adduction and supination, compounding the cavus deformity.
Soft Tissue Deformities
The rigidity of the clubfoot is primarily due to contracture of specific soft tissue structures on the medial and posterior aspects of the foot and ankle. These include:
*
Posterior Structures:
*
Achilles tendon:
Contracted, leading to hindfoot equinus.
*
Posterior ankle capsule:
Tight, restricting dorsiflexion.
*
Posterior talofibular ligament:
Contracted.
*
Flexor digitorum longus (FDL), Flexor hallucis longus (FHL), Tibialis posterior (TP) tendons:
These tendons often appear tight, especially their sheaths, and contribute to the equinus and varus.
*
Medial Structures:
*
Tibialis posterior tendon:
Significantly contracted, pulling the foot into inversion and adduction.
*
Deltoid ligament:
Medial collateral ankle ligament, contracted, contributing to talar internal rotation and medial displacement.
*
Spring ligament (plantar calcaneonavicular ligament):
Contracted, exacerbating cavus and medial arch collapse in relation to the navicular.
*
Talonavicular and subtalar joint capsules:
Thickened and contracted medially.
*
Abductor hallucis:
Often hypertrophied and displaced plantar-medially, contributing to cavus and forefoot adduction.
*
Plantar fascia:
Contracted, contributing to cavus.
The Anterior Tibialis Tendon (ATT)
The anterior tibialis tendon (ATT) plays a critical role in the biomechanics of both the normal and clubfoot, particularly in the context of forefoot deformities and potential recurrence.
*
Normal Anatomy & Function:
The ATT originates from the lateral condyle of the tibia and the upper half of the lateral surface of the tibia, inserting primarily onto the medial cuneiform and the base of the first metatarsal. Its primary actions are dorsiflexion of the ankle and inversion of the foot.
*
Role in Clubfoot Deformity:
In clubfoot, the ATT is often displaced medially relative to its normal anatomical course. Due to the overall adducted and inverted position of the forefoot, the ATT's line of pull is altered. Its continued contraction can:
*
Exacerbate Forefoot Adduction and Supination:
While a primary dorsiflexor, its insertion on the medial border of the foot, coupled with the existing deformity, can make it a powerful invertor and adductor, contributing to residual or recurrent forefoot supination and cavus.
*
Maintain Cavus:
Its strong pull on the medial column can deepen the cavus deformity by plantarflexing the first ray.
*
Clinical Significance:
The prominence, tension, and excursion of the ATT are important clinical indicators. A persistently prominent or contracted ATT, particularly if it actively contributes to dynamic forefoot supination during attempted dorsiflexion, signals its involvement in the uncorrected or recurrent deformity. This dynamic action is often observed when the child attempts to walk, leading to a "tripod" gait with weight-bearing on the lateral border of the foot.
Relevant Neurovascular Structures
During surgical correction, meticulous attention must be paid to protecting key neurovascular structures:
*
Posterior Tibial Neurovascular Bundle:
Located posterior to the medial malleolus, superficial to the flexor retinaculum. It supplies the intrinsic muscles of the sole of the foot and provides sensation to the plantar aspect.
*
Saphenous Nerve and Vein:
Found anterior to the medial malleolus. The nerve provides sensation to the medial aspect of the ankle and foot.
*
Superficial Peroneal Nerve:
Courses laterally in the distal leg, providing sensation to the dorsum of the foot.
*
Deep Peroneal Nerve:
Located in the anterior compartment, crucial for dorsiflexion and sensation in the first web space.
Indications & Contraindications
The management of pediatric clubfoot primarily follows the Ponseti method. Surgical intervention is typically reserved for cases that are resistant to conservative management, exhibit significant residual deformity, or experience recurrence despite adequate non-operative treatment.
Indications for Operative Management
Surgical correction is considered for children, typically beyond 1-2 years of age, or in complex syndromic cases, when:
*
Failure of Non-Operative Treatment:
The most common indication. This includes:
* Failure to achieve full correction (specifically dorsiflexion to 15-20 degrees, heel valgus, and forefoot abduction) after an adequate trial of the Ponseti method (typically 5-7 casts followed by bracing).
* Inability to maintain correction due to rigid deformity despite consistent Ponseti treatment.
*
Rigid Residual Deformity:
Persistent, rigid components after initial non-operative treatment, even with good compliance. This includes:
* Residual hindfoot equinus (less than 10 degrees dorsiflexion) or varus.
* Persistent forefoot adduction and supination/cavus (often dynamic, where the foot pronates with weight-bearing but supinates during swing phase, indicating muscular imbalance).
* Uncorrected talonavicular subluxation or other significant osseous malalignment visible on imaging.
*
Relapse/Recurrence:
Recurrence of the clubfoot deformity despite a well-executed Ponseti protocol and subsequent brace compliance. The pattern of relapse often dictates the specific surgical approach. Recurrence presenting as dynamic supination of the forefoot or pes cavus strongly implicates the anterior tibialis tendon.
*
Syndromic Clubfoot:
Clubfoot associated with conditions such as arthrogryposis, myelomeningocele, or other neuromuscular disorders. These often present with more rigid soft tissue contractures and muscle imbalances, frequently requiring primary surgical release at an earlier age compared to idiopathic cases.
*
Older Child Presenting for First Time:
While rare in developed countries, older children (e.g., >3 years) presenting with untreated or undertreated clubfoot may require more extensive primary surgical release due to established bony deformities and severe soft tissue contractures.
Contraindications for Operative Management
- Successful Correction by Ponseti Method: If the deformity is fully corrected and maintained with bracing, surgery is not indicated.
- Ongoing Non-Operative Treatment: Surgery should generally not precede an adequate trial of the Ponseti method for idiopathic clubfoot, unless there are compelling reasons related to syndromic presentation or severe rigidity.
- Active Local Infection: Any active infection in the operative field should be treated and resolved prior to surgery to minimize the risk of wound complications and deep infection.
- Severe Vascular Compromise: Patients with compromised vascular status (e.g., severe peripheral vascular disease, although rare in infants) should be carefully assessed, as surgery could further jeopardize circulation.
Operative vs. Non-Operative Indications
| Indication Category | Operative Management | Non-Operative Management (Ponseti First Line) |
|---|---|---|
| Primary Deformity | Typically reserved for older children (>2-3 years) with severe, rigid clubfoot refractory to comprehensive Ponseti attempts, or as initial treatment for severe syndromic clubfoot (e.g., arthrogryposis). Primary extensive soft tissue release is rare for idiopathic cases. | All infants with idiopathic clubfoot, regardless of severity (Pirani score 0-6). Initiation within the first few weeks of life is ideal. |
| Residual Deformity | Persistent rigid hindfoot equinus, varus, or forefoot adduction/cavus after comprehensive Ponseti treatment and Achilles tenotomy. Uncorrected talonavicular subluxation. | Minor residual deformities, particularly flexible components, managed with extended bracing, orthoses, stretching exercises, or shoe modifications. |
| Recurrent Deformity | Recurrence of rigid components (equinus, varus, cavus, forefoot adduction) despite documented good compliance with bracing. Particularly, dynamic forefoot supination or cavus often suggests the need for anterior tibialis tendon transfer. | Mild, flexible recurrence usually managed with repeat serial casting and intensified bracing protocols. Re-evaluation of brace compliance and parental education. |
| Associated Conditions | Clubfoot secondary to arthrogryposis, myelomeningocele, or other conditions with significant muscle imbalance or tissue rigidity often requires earlier or more extensive surgical release. | Many syndromic clubfeet can still benefit from initial Ponseti casting to gain some correction, but often have higher rates of requiring surgical intervention and more complex issues. |
| Specific Tendon Involvement | Significant contracture or malposition of the anterior tibialis tendon contributing to residual cavus or dynamic forefoot supination/adduction, warranting tenotomy, lengthening, or transfer. | (Addressed by Ponseti manipulation, stretching, and specific casting techniques aimed at correcting forefoot adduction and cavus, which indirectly addresses the effects of the anterior tibialis tendon). Minor imbalances may be managed with orthotics. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical to optimize surgical outcomes and minimize complications in pediatric clubfoot correction.
Clinical Assessment
A comprehensive evaluation begins with a detailed history, including the child's age, previous treatments (number of casts, Achilles tenotomy, brace compliance), and any associated medical conditions or syndromes. The physical examination should systematically assess:
*
Deformity components:
Quantify the rigidity of equinus, varus, adduction, and cavus.
*
Range of Motion:
Both passive and active range of motion of the ankle and foot.
*
Skin integrity:
Note any skin creases, scars, or areas of potential compromise, particularly relevant for incision planning.
*
Neurovascular status:
Assessment of distal pulses and neurological function.
*
Specific Tendon Assessment (Anterior Tibialis Tendon):
*
Palpation:
Identify the course of the anterior tibialis tendon. In clubfoot, it may feel taut or prominent, especially medially.
*
Dynamic Assessment:
Observe the foot during attempted active dorsiflexion. Does the forefoot actively supinate or adduct, demonstrating a dynamic imbalance where the ATT acts predominantly as an invertor/adductor rather than a pure dorsiflexor? This is a key indicator for potential ATT transfer.
*
Flexibility:
Assess the flexibility of the forefoot and its relation to the hindfoot. Can the cavus be passively corrected?
*
Scoring Systems:
Utilize validated scoring systems such as the Pirani score or Dimeglio score to objectively quantify deformity severity and track progress or recurrence. The Pirani score components related to forefoot adduction and cavus are particularly relevant for ATT assessment.
Imaging
-
Weight-bearing Radiographs:
For older children (typically >1 year), weight-bearing anteroposterior (AP) and lateral radiographs are invaluable. Non-weight-bearing films may be necessary for younger infants.
- AP View: Assess the talonavicular coverage angle and the talus-first metatarsal angle (often referred to as Kite's angle, though this term is also used for the talocalcaneal angle). Medial subluxation of the navicular on the talus is characteristic.
- Lateral View: Assess the talocalcaneal angle (decreased in equinus and varus) and the talus-first metatarsal angle (plantarflexed first ray indicates cavus).
- Stress Views: Forced dorsiflexion and eversion views can help assess the flexibility of the deformity and identify the most rigid components.
Surgical Planning
- Procedure Selection: Based on the clinical and radiographic assessment, decide on the extent of soft tissue release, potential osteotomies, and whether tendon transfers (e.g., anterior tibialis tendon transfer) are indicated. For recurrence with dynamic supination, ATT transfer is often the procedure of choice.
- Incision Planning: The Cincinnati incision (transverse) is widely favored for extensive soft tissue releases due to excellent exposure and minimal scar contracture.
- Resource Management: Ensure availability of appropriate instrumentation, implants (K-wires), and image intensifier.
- Patient and Parent Counseling: Thoroughly discuss the surgical plan, potential risks (infection, recurrence, stiffness, neurovascular injury), expected outcomes, and the need for post-operative casting and bracing. Manage expectations regarding the potential for further procedures.
Patient Positioning
- Supine Position: The patient is placed supine on a radiolucent operating table.
- Tourniquet: A pneumatic tourniquet is applied to the proximal thigh of the operative limb to provide a bloodless field, typically inflated to 250 mmHg or 100 mmHg above systolic blood pressure.
- Hip Roll: A small roll or bump is placed under the ipsilateral hip to allow for internal rotation of the leg, bringing the foot into a neutral or slightly abducted position for optimal exposure.
- Sterile Prep and Drape: The entire limb, from mid-thigh to toes, is prepped with an antiseptic solution and sterilely draped to ensure a wide sterile field for surgical access and manipulation, as well as potential K-wire insertion.
- Fluoroscopy: An image intensifier is positioned for intraoperative fluoroscopy to confirm osseous alignment and K-wire placement.
Detailed Surgical Approach / Technique
The primary goal of surgical correction for clubfoot is to achieve a plantigrade, flexible foot by restoring normal osseous alignment, releasing contracted soft tissues, and balancing muscle forces. The most common approach for a comprehensive release is the posteromedial release (PMR), often performed through a Cincinnati incision. In cases of recurrence or dynamic forefoot supination, an anterior tibialis tendon transfer may be concurrently or subsequently performed.
General Steps for a Posteromedial Release (PMR)
-
Skin Incision:
- A Cincinnati incision is typically employed. This transverse, curvilinear incision extends from the anterior aspect of the medial malleolus, crosses the ankle joint posteriorly, to the posterior aspect of the lateral malleolus. This incision provides excellent exposure to all medial and posterior structures while minimizing the risk of longitudinal scar contracture and skin complications.
-
 - Consideration: For isolated forefoot or hindfoot issues, more limited incisions may be used (e.g., medial incision for talonavicular release, posterior for Achilles lengthening).
-
Soft Tissue Dissection & Neurovascular Protection:
- Careful dissection through subcutaneous tissues. Identify and protect the saphenous nerve and vein anteriorly along the medial aspect.
- Posterior to the medial malleolus, meticulously identify and protect the posterior tibial neurovascular bundle (artery, veins, nerve). These structures are often displaced more anteriorly and inferiorly in clubfoot and must be retracted gently but firmly.
-
Posterior Release (Correction of Equinus):
- The Achilles tendon is identified. A Z-plasty lengthening is performed. The tendon is incised distally on one side and proximally on the opposite side, allowing for controlled lengthening.
- The deep fascia, posterior ankle capsule, and posterior subtalar capsule are then released. The posterior talofibular ligament is often sectioned.
- This step aims to fully correct the hindfoot equinus, allowing the ankle to be passively dorsiflexed to at least 15-20 degrees.
-
Medial Release (Correction of Varus, Adduction, Cavus):
-
Starting from posterior to anterior along the medial aspect:
- The tendons of the Tibialis Posterior, Flexor Digitorum Longus, and Flexor Hallucis Longus are identified. These are typically lengthened via Z-plasty or tenotomized depending on rigidity and expected recovery. Their sheaths are also opened.
- The deltoid ligament is released, typically from the medial malleolus or talus.
- The talonavicular joint capsule and spring ligament (plantar calcaneonavicular) are released. The spring ligament is often the key structure maintaining the cavus and medial arch deformity.
- The abductor hallucis muscle is released from its origin on the medial tubercle of the calcaneus and its deep fascia sectioned to decompress the medial compartment and allow hindfoot correction.
- The plantar fascia may be released if a significant cavus deformity persists.
-
Starting from posterior to anterior along the medial aspect:
-
Osseous Realignment:
- After soft tissue releases, the foot components are sequentially reduced.
- Hindfoot: The calcaneus is brought into dorsiflexion and valgus under the talus, correcting the equinus and varus.
- Midfoot: The navicular is concentrically reduced onto the head of the talus, correcting the medial subluxation. This is a critical step, as failure to reduce the talonavicular joint will inevitably lead to recurrence.
- Forefoot: The forefoot adduction and supination are corrected by abducting and pronating the forefoot relative to the midfoot.
- Fluoroscopy is used to confirm concentric reduction of the talonavicular joint and restoration of normal talocalcaneal and talus-first metatarsal angles.
-
 - Note: In older children with established bony deformities, adjunctive osteotomies (e.g., calcaneal osteotomy, cuboid osteotomy, dorsal closing wedge osteotomy of the first cuneiform for resistant cavus) may be necessary.
-
Addressing the Anterior Tibialis Tendon (ATT):
This step is particularly relevant when the anterior tibialis tendon contributes to residual or recurrent forefoot adduction, supination, or cavus.- Pre-reduction Assessment: Before full correction and pinning, reassess the forefoot. If there is significant active pull of the ATT exacerbating adduction or supination, particularly if the child is older or has a history of relapse, a specific intervention may be necessary.
-
Options for ATT Management:
- Tenotomy/Lengthening: If the ATT is simply tight and contributing to a static cavus or adduction after maximal soft tissue release, a simple percutaneous or open tenotomy, or Z-lengthening, can be performed. This is less common in primary releases and more often considered for isolated issues.
-
Transfer (Anterior Tibialis Tendon Transfer - ATTT):
This is indicated for dynamic forefoot supination or adduction, especially in recurrent clubfoot after Ponseti or prior surgery, and typically in children older than 3-4 years. The goal is to convert the ATT from an invertor/supinator to an evertor/dorsiflexor, balancing the foot.
-
Technique for ATTT:
- A small incision is made over the insertion of the ATT at the medial cuneiform and base of the first metatarsal. The tendon is sharply detached from its insertion.
- A second incision is made more proximally in the anterior compartment. The ATT is retrieved from the original insertion site and pulled out through this proximal incision.
- A drill hole or osseous tunnel is created in the cuboid or, less commonly, the third cuneiform (lateral aspect of the midfoot). The choice depends on the desired vector of pull.
- The tendon is passed subcutaneously or through an intermuscular plane to the lateral midfoot incision.
- The tendon is threaded through the prepared drill hole/tunnel and secured under appropriate tension (typically with the foot held in slight dorsiflexion and eversion) using non-absorbable sutures, a button, or interference screw. The goal is to achieve balance without overcorrection or weakening dorsiflexion significantly.
- Rationale for ATTT: By moving its insertion laterally, the ATT's line of pull is altered, providing an eversion moment that counteracts the supinating forces of the tibialis posterior and intrinsic muscles, thereby preventing recurrence of dynamic forefoot supination and often aiding in cavus correction.
-
Technique for ATTT:
-
Pin Fixation:
-
Once full correction is achieved and confirmed by fluoroscopy, K-wires are typically inserted to maintain the correction. Common pinning sites include:
- Talonavicular joint: One or two K-wires passing from the dorsal aspect of the navicular into the talar head.
- Calcaneocuboid joint: Less common but may be used to stabilize midfoot.
- Talo-calcaneal joint: A wire from the calcaneus into the talus, especially for hindfoot stability.
- The K-wires are cut short and bent to lie beneath the skin or left protruding through the skin, depending on surgeon preference and planned duration.
-
Once full correction is achieved and confirmed by fluoroscopy, K-wires are typically inserted to maintain the correction. Common pinning sites include:
-
Wound Closure:
- The tourniquet is deflated, and hemostasis is achieved.
- The wound is closed in layers. Meticulous skin closure is essential to minimize scar formation and improve aesthetic outcome.
-
Casting:
- A well-padded, long-leg cast is applied with the foot maintained in the corrected position of slight dorsiflexion, eversion, and abduction. The cast extends above the knee to control rotation.
Complications & Management
Despite meticulous surgical technique, complications can arise in the management of pediatric clubfoot. Awareness of these potential issues and strategies for their management is crucial for all orthopedic surgeons.
Common Complications
| Complication | Incidence (Variable, often higher in syndromic cases or extensive releases) | Management Strategy |
|---|---|---|
| Recurrence | 10-30% after extensive surgery; higher with non-compliance or syndromic forms. | The most common and challenging complication. Initially, assess compliance with bracing. For flexible recurrence, repeat serial casting may be attempted. For rigid recurrence, further surgical intervention is indicated. This may involve repeat soft tissue release, targeted osteotomies (e.g., calcaneal or cuboid osteotomy), or crucially, anterior tibialis tendon transfer (ATTT) for dynamic forefoot supination. Early identification and intervention are key. |
| Residual Deformity | Variable, depending on initial severity and surgical technique. |
This refers to incomplete correction of one or more components post-surgery.
- Residual Cavus: Often requires dorsal closing wedge osteotomy of the first cuneiform and/or metatarsal, or plantar fascia release. ATTT can also help balance forces. - Residual Adduction: May necessitate repeat talonavicular joint reduction, or in older children, a lateral column shortening (e.g., cuboid ostectomy) or medial column lengthening. - Residual Equinus: Implies inadequate Achilles lengthening or contracture. May require repeat Achilles lengthening. - Residual Varus: Often addressed with calcaneal osteotomy (lateral closing wedge). |
| Stiffness | Common to varying degrees after extensive soft tissue releases. | Early mobilization after cast removal, aggressive physiotherapy, active and passive range of motion exercises, dynamic splinting, or bracing. Rarely, surgical arthrolysis may be considered for severe cases. |
| Wound Healing Issues / Infection | 1-5% for superficial, <1% for deep. Higher risk in revision surgery or compromised skin. | Careful soft tissue handling, meticulous closure, and strict aseptic technique are paramount. For superficial infections, local wound care and oral antibiotics. For deep infections, surgical debridement, intravenous antibiotics, and removal of any hardware (K-wires) may be necessary. Skin grafting is rare but can be required for large defects. |
| Neurovascular Injury | Rare (<1%), but potentially devastating. | Most commonly involves the posterior tibial neurovascular bundle. Prevention is key through careful dissection and identification of structures. If injured, prompt repair is necessary, with potential for long-term deficits despite repair. |
| Overcorrection / Rocker-bottom Deformity | Rare, but can result from aggressive dorsiflexion in casting or excessive plantar release. | A rocker-bottom foot results from excessive dorsiflexion and an anterior break in the longitudinal arch. Management involves corrective casting (plantarflexion), orthotics, and, in severe cases, plantar fascia release or dorsal closing wedge osteotomy to recreate the arch. |
| K-wire Complications | 5-10% (e.g., pin tract infection, breakage, migration). | Pin tract infections are managed with local wound care, oral antibiotics, and early pin removal if severe. Broken or migrating pins may require surgical removal. |
| Growth Disturbance | Very rare, but possible with direct damage to physeal plates during osteotomies or extensive capsular stripping. | Avoidance through careful surgical technique and awareness of physeal locations. If it occurs, it may lead to angular deformities or limb length discrepancy requiring future corrective osteotomies. |
| Anterior Tibialis Tendon Weakness | Variable after transfer, or if over-lengthened. | If ATT transfer is performed incorrectly or if the tendon is excessively lengthened, it can result in dorsiflexion weakness. Management includes targeted physiotherapy, muscle strengthening, and possibly orthotic support. In rare cases of significant dysfunction, revision surgery or alternative tendon transfers might be considered. |
General Management Principles
- Early Detection: Regular and thorough follow-up is essential to detect complications early.
- Patient and Parent Education: Reinforce the importance of brace compliance and the long-term nature of clubfoot management, even after surgery.
- Multidisciplinary Approach: Involve physical therapists, orthotists, and other specialists as needed for comprehensive management.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgical procedure itself in achieving and maintaining the correction of pediatric clubfoot. The protocols aim to protect the corrected alignment, facilitate healing, restore function, and prevent recurrence.
Immediate Post-Operative Period (0-6 Weeks)
-
Casting:
A well-padded, long-leg cast is applied in the operating room, maintaining the foot in the corrected position (slight dorsiflexion, eversion, and abduction). The cast should extend above the knee with the knee flexed to prevent rotation and maintain the ankle position.
- Duration: The initial cast is typically kept for 4-6 weeks. K-wires, if used, remain embedded within the cast during this period.
- Monitoring: Close monitoring for neurovascular compromise (color, temperature, capillary refill, sensation) and cast complications (pressure sores, excessive swelling) is paramount, especially in the first 24-48 hours.
- Non-Weight-Bearing: The child is kept strictly non-weight-bearing on the operative limb during this phase to protect the surgical repair and K-wire fixation.
- Pain Management: Appropriate analgesia should be provided.
After Cast and K-wire Removal (6 Weeks onwards)
- K-wire Removal: K-wires are typically removed in an outpatient setting or minor procedure room after 4-6 weeks, once initial soft tissue healing is sufficient to hold the correction.
-
Transition to Brace/Orthosis:
Immediately following cast and K-wire removal, the foot is typically transitioned into a specialized foot abduction brace (FAB), similar to the Ponseti brace (e.g., high-top shoes attached to a bar).
- Brace Schedule: The brace is worn full-time (23 hours/day) for the first 3 months, similar to the initial Ponseti phase. This is then gradually transitioned to night-time and nap-time wear.
-
Physiotherapy Initiation:
A structured physiotherapy program is initiated to restore range of motion, strengthen muscles, and facilitate normal gait development.
- Range of Motion (ROM): Passive and active ROM exercises focusing on dorsiflexion and eversion are crucial to counteract the tendency for recurrence of equinus and varus. Parents are educated on gentle stretching exercises.
- Strengthening: Exercises to strengthen the dorsiflexors (especially if an anterior tibialis tendon transfer was performed) and evertors are emphasized.
- Weight-Bearing: Gradual progression to full weight-bearing as tolerated.
- Gait Training: Once comfortable, gait training is initiated, focusing on a heel-strike to toe-off pattern and promoting an outwardly rotated foot progression angle.
Long-Term Management (Months to Years)
- Continued Bracing: Bracing remains a cornerstone of long-term management to prevent recurrence. Night-time and nap-time wear of the foot abduction brace is typically recommended until 4-5 years of age, and sometimes longer in cases of syndromic clubfoot or high risk of recurrence. Non-compliance with bracing is a leading cause of relapse.
-
Regular Follow-up:
Ongoing clinical follow-up is essential, typically every 6-12 months, to monitor for:
- Maintenance of correction.
- Foot growth and development.
- Muscle balance and function.
- Potential for recurrence.
- Assessment of brace fit and compliance.
- Orthotics/Shoe Modifications: For some children, custom orthotics or specific shoe modifications may be beneficial to support the arch, prevent supination, or accommodate any residual foot shape.
- Activity: Encourage normal participation in age-appropriate physical activities. The goal is to achieve a functional, pain-free foot that allows full participation in life.
Specific Considerations for Anterior Tibialis Tendon Transfer (ATTT)
- Immobilization: If an ATTT is performed, the cast protocol may be slightly modified. The foot is typically immobilized in the cast in a position that minimizes tension on the transferred tendon while maintaining initial correction (e.g., neutral dorsiflexion, slight eversion/abduction).
- Strengthening: Post-cast removal, specific strengthening exercises for the newly transferred anterior tibialis tendon are critical. The aim is to "retrain" the muscle to function as an evertor and dorsiflexor, promoting active foot balance. Electrical stimulation or biofeedback may be used in selected cases.
- Bracing: Rigorous bracing with the foot abducted and slightly everted is crucial to protect the ATTT and allow for healing in the new position.
The success of clubfoot surgery is highly dependent on dedicated and consistent post-operative rehabilitation. It is a long-term commitment for both the medical team and the family.
Summary of Key Literature / Guidelines
The landscape of clubfoot management has been profoundly shaped by evidence-based medicine, moving from predominantly extensive surgical releases to the highly successful Ponseti method. However, surgery retains a crucial role for resistant or recurrent cases.
The Ponseti Method: The Gold Standard
- Foundational Work: Ignacio Ponseti's seminal work in the 1950s and 60s, culminating in his detailed methodology published in Congenital Clubfoot: Fundamentals of Treatment (1996), revolutionized treatment. His method demonstrated superior long-term outcomes, with a plantigrade, flexible, and functional foot, compared to traditional extensive surgical releases.
- Efficacy: Numerous studies and meta-analyses consistently report success rates of 90-95% for idiopathic clubfoot with the Ponseti method (serial casting, percutaneous Achilles tenotomy, and foot abduction bracing).
- Recommendation: Current international guidelines, including those from the American Academy of Orthopaedic Surgeons (AAOS), strongly recommend the Ponseti method as the primary treatment for idiopathic clubfoot.
The Role of Surgical Intervention: Evolving Paradigms
- Shift from Primary Release: Extensive primary posteromedial releases are now rarely indicated for idiopathic clubfoot due to high rates of complications such as stiffness, pain, recurrence, and overcorrection, which often manifest in adolescence or adulthood.
- Targeted Surgery for Resistant/Recurrent Cases: Current surgical philosophy emphasizes limited, targeted releases or procedures for specific residual deformities that persist after adequate Ponseti treatment or for severe relapses.
- Evidence for Recurrence: Studies show that despite high initial success, recurrence rates after Ponseti range from 10-30%, often due to non-compliance with bracing.
The Anterior Tibialis Tendon Transfer (ATTT)
-
Key Literature:
ATTT has emerged as a well-established and evidence-supported procedure for preventing recurrence of dynamic forefoot supination, a common pattern of relapse after Ponseti treatment.
- McKay (1983): Pioneering work on comprehensive clubfoot releases, though his approach was more extensive.
- Herzenberg et al. (2009) and Chu et al. (2014): Studies demonstrating the effectiveness of ATTT in reducing relapse rates, particularly dynamic supination, after initial Ponseti correction. They often recommend ATTT for children over 3 years of age with persistent dynamic forefoot supination, or a Pirani score of >1.5 in the forefoot components.
- Bor et al. (2006): Emphasized the importance of addressing the dynamic component of forefoot supination with ATTT.
-
Indications for ATTT:
Generally considered in children >3-4 years of age presenting with:
- Recurrent forefoot adduction/supination after successful Ponseti treatment.
- Persistent dynamic forefoot supination during gait, even after initial soft tissue release.
- Residual cavus secondary to an unopposed or actively contracted anterior tibialis tendon.
- Outcomes of ATTT: Studies indicate that ATTT significantly reduces the need for further surgery and improves long-term functional outcomes by balancing the muscular forces across the foot. The transfer converts the invertor/supinator action of the ATT into a dorsiflexor/evertor force.
Complications and Long-Term Outcomes
- Comparison of Outcomes: While primary surgical releases had higher rates of stiffness, arthritis, and revision surgery in adulthood, the Ponseti method (and targeted surgery for resistant cases) yields much better long-term function, pain scores, and shoe wear.
- Recurrence: Despite surgical correction, recurrence remains a concern, with rates varying depending on the severity of the initial deformity, patient age, surgical technique, and post-operative compliance.
- Stiffness: A common sequela of extensive surgical releases, underscoring the shift towards less invasive approaches.
Current Guidelines and Recommendations
- Ponseti First: The overwhelming consensus is that the Ponseti method is the initial and preferred treatment for idiopathic clubfoot.
- Surgery as Salvage/Revision: Surgical intervention, often involving soft tissue releases and increasingly targeted procedures like ATTT or osteotomies, is reserved for those who fail Ponseti treatment or experience recurrence.
- Age Considerations: The decision for specific surgical procedures, particularly ATTT or osseous procedures, is often influenced by the child's age, as bone maturity affects the stability and feasibility of osteotomies and the biomechanical impact of tendon transfers.
- Comprehensive Care: Long-term follow-up and adherence to bracing protocols are crucial, regardless of the treatment method, to prevent relapse and ensure optimal foot function throughout growth.
Clinical & Radiographic Imaging