Introduction & Epidemiology
Fibular deficiency, often referred to as longitudinal fibular deficiency or fibular hemimelia, represents the most common congenital longitudinal limb deficiency of the lower extremity. It is characterized by partial or complete absence of the fibula, frequently accompanied by an array of associated deformities in the tibia, ankle, and foot. The spectrum of presentation ranges from mild hypoplasia to complete agenesis of the fibula, dictating the severity of limb length discrepancy (LLD), angular deformities, and functional impairment.
The estimated incidence varies, generally reported to be between 1 in 50,000 to 1 in 100,000 live births, with a slight male predominance and often sporadic occurrence. While typically isolated, fibular deficiency can rarely be associated with specific syndromes such as proximal femoral focal deficiency, developmental field defects, and other limb anomalies, necessitating a comprehensive assessment for associated systemic conditions.
Classification systems are crucial for prognostic assessment and treatment planning. The Achilles-Kuts classification, though historically significant, has been largely superseded by more detailed systems. Paley's classification for fibular hemimelia (Type 1A, 1B, 2) provides a framework based on the presence and size of the distal fibular epiphysis and the extent of fibular absence, directly correlating with the severity of limb shortening and ankle instability:
*
Type 1A:
Distal fibular physis is present, allowing for lengthening with moderate LLD. The fibula is significantly shorter than the tibia, but the ankle joint is stable.
*
Type 1B:
A portion of the fibula is present, but the distal physis is absent. The ankle joint is unstable, often with a valgus deformity.
*
Type 2:
Complete absence of the fibula. Severe LLD, profound ankle instability, and marked foot deformities are characteristic.
Pappas's classification, which includes eight grades based on the extent of fibular involvement and associated tibial bowing, also contributes to understanding the variability. Regardless of the classification used, the hallmark features include progressive LLD, anterior-medial bowing of the tibia, ankle valgus with or without a tarsal coalition, and absence or hypoplasia of the lateral rays of the foot (commonly the 4th and 5th toes, or even more profound lateral ray deficiencies). The fundamental challenge lies in restoring functional limb length, mechanical alignment, and a plantigrade, stable foot for ambulation.
Surgical Anatomy & Biomechanics
The absence or hypoplasia of the fibula profoundly alters the anatomical and biomechanical landscape of the lower limb. Understanding these deviations is paramount for effective surgical planning.
Tibial Deformities
The tibia, in the absence of its fibular buttress, often exhibits anterior-medial bowing. This bowing can range from subtle curvature to a severe angulation, sometimes complicated by skin tethering or impending pseudoarthrosis. The growth of the tibia may also be intrinsically affected, contributing to LLD. The distal tibial physis can be irregular, and its intrinsic growth potential may be diminished.
Ankle Joint Anomalies
The ankle joint is perhaps the most severely affected articulation. The fibula normally forms the lateral malleolus, providing critical stability to the talus within the mortise. In fibular deficiency:
*
Ankle Valgus:
This is nearly universal, ranging from mild to severe, due to the lack of lateral support and often accompanied by talar tilt.
*
Talar Hypoplasia/Dysplasia:
The talus can be hypoplastic or abnormally shaped, further contributing to instability and incongruity. The talus may migrate proximally relative to the distal tibia.
*
Absence of Lateral Malleolus:
In Type 2 deficiency, the complete absence of the lateral malleolus leads to profound instability and a widened ankle mortise. In Type 1B, the rudimentary fibula is often non-functional in providing stability.
*
Ligamentous Instability:
The lateral collateral ligaments of the ankle are either absent or severely attenuated.
*
Muscle Imbalance:
Hypoplasia or absence of the lateral compartment muscles (peronei) exacerbates valgus deformity and impacts dynamic stability. The Achilles tendon is often contracted, contributing to equinus.
Foot Deformities
The foot in fibular deficiency is characterized by:
*
Absence of Lateral Rays:
This is a hallmark feature, ranging from hypoplasia or absence of the 4th and 5th toes (often referred to as 'lateral ray deficiency') to a more extensive oligodactyly involving additional rays.
*
Equinovalgus Deformity:
A combination of hindfoot valgus and ankle equinus, making the foot functionally difficult to manage.
*
Tarsal Coalition:
A fibrous, cartilaginous, or bony bridge between two or more tarsal bones, frequently involving the calcaneus and navicular or talus and calcaneus. This can cause rigidity, pain, and contribute to progressive deformity.
*
Forefoot Abduction:
Often present, further compounding gait difficulties.
Biomechanical Consequences
The collective anatomical abnormalities lead to significant biomechanical impairments:
*
Altered Load Bearing:
The absence of the fibula shifts weight-bearing forces primarily through the tibia, which may already be deformed. This can lead to abnormal stress distribution across the ankle and foot.
*
Gait Abnormalities:
LLD, ankle instability, and foot deformities collectively result in a pathologic gait pattern, characterized by circumduction, steppage, or toe-walking, leading to increased energy expenditure and pain.
*
Progressive Deformity:
Without intervention, LLD and angular deformities tend to worsen with growth, due to unequal growth plate contributions and asymmetric loading.
These complex deformities necessitate a multi-faceted surgical approach tailored to the individual child's specific presentation, aimed at restoring length, alignment, and function.
Indications & Contraindications
The decision-making process for intervention in fibular deficiency is complex, weighing the severity of deformity against the potential risks and benefits of various operative and non-operative strategies. The primary goals are to achieve a functional, plantigrade foot, restore limb length equality, correct mechanical axis deviations, and enable pain-free ambulation.
Indications for Intervention
Non-Operative Indications:
*
Mild LLD (<3-5 cm):
Can often be managed with shoe lifts, orthotics, or bracing to improve ambulation and prevent compensatory deformities of the spine and pelvis.
*
Stable Ankle/Foot:
When ankle valgus and foot deformities are minimal, well-compensated, and asymptomatic, observation with regular follow-up may be appropriate.
*
Very Young Age (<2 years):
For certain complex reconstructions, delaying surgery until the child is older may allow for better tissue quality, larger bone stock, and more reliable cooperation with rehabilitation. However, early bracing might be initiated for progressive deformities.
*
Significant Medical Comorbidities:
When the risks of anesthesia and extensive surgery outweigh the potential functional benefits.
*
Patient/Family Preference:
After thorough counseling regarding options, risks, and expected outcomes.
Operative Indications:
*
Significant LLD (>3-5 cm or projected significant LLD):
Particularly when progressive and causing functional impairment or compensatory scoliosis.
*
Severe Ankle Instability/Deformity:
Persistent, painful, or progressive ankle valgus, equinus, or profound instability leading to gait disturbance or difficulty with shoe wear.
*
Progressive Foot Deformity:
Severe equinovalgus, painful tarsal coalitions, or disabling lateral ray deficiencies that preclude functional weight-bearing or footwear.
*
Tibial Bowing/Pseudoarthrosis Risk:
Significant anterior-medial bowing that is progressive, causing skin compromise, or deemed at high risk for pseudoarthrosis.
*
Failure of Non-Operative Management:
When conservative measures no longer adequately address symptoms or functional limitations.
*
Anticipated Functional Benefit:
Surgical intervention is indicated when a clear improvement in ambulation, comfort, and independence can be achieved.
Contraindications
Absolute Contraindications:
*
Uncontrolled Systemic Conditions:
Severe cardiac, pulmonary, or neurological conditions that significantly increase surgical risk.
*
Insufficient Bone Stock:
In cases of severe hypoplasia or poor regenerate potential, attempts at limb lengthening may be futile or carry unacceptable risks.
*
Irreversible Neurovascular Damage:
Existing severe compromise that would be exacerbated by surgery.
*
Terminal Illness.
Relative Contraindications:
*
Lack of Patient/Family Compliance:
Successful outcomes from complex limb reconstruction require dedicated adherence to rehabilitation protocols, which can be prolonged and demanding.
*
Unrealistic Expectations:
Failure to fully understand the arduous nature of the treatment, potential complications, and realistic functional outcomes.
*
Severe Scaring/Poor Skin Quality:
Can complicate approaches and increase infection risk.
*
Profound Global Developmental Delay:
In cases where the child's overall developmental trajectory suggests limited ambulation potential, even with limb reconstruction, the utility of extensive surgery must be carefully considered against prosthetic options.
Operative vs. Non-Operative Indications
| Indication Type | Operative Indications ```
Introduction & Epidemiology
Fibular deficiency, also known as congenital longitudinal fibular deficiency or fibular hemimelia, represents the most prevalent congenital longitudinal limb deficiency of the lower extremity. It is characterized by the partial or complete absence of the fibula, frequently associated with a spectrum of anomalies in the tibia, ankle, and foot. The clinical presentation varies from mild hypoplasia to complete agenesis of the fibula, directly correlating with the severity of limb length discrepancy (LLD), angular deformities, and functional impairment.
The estimated incidence ranges from 1 in 50,000 to 1 in 100,000 live births, often presenting as a sporadic event with a slight male predominance. Although typically an isolated finding, fibular deficiency can rarely manifest as part of specific syndromes, such as proximal femoral focal deficiency, or in conjunction with other developmental field defects. A thorough assessment for co-existing systemic anomalies is therefore always warranted.
Classification systems are indispensable for guiding prognosis and treatment strategies. While historical systems like Achilles-Kuts contributed to early understanding, modern approaches largely rely on more granular classifications. Paley's classification for fibular hemimelia is widely utilized, categorizing the deficiency based on the presence and size of the distal fibular epiphysis and the extent of fibular absence, which correlates directly with limb shortening and ankle stability:
*
Type 1A:
Characterized by a shortened but present fibula with a functional distal fibular physis. This type typically presents with moderate LLD, and the ankle joint maintains relative stability, although valgus deformity is common.
*
Type 1B:
A portion of the fibula is present, but the distal fibular physis is absent. This leads to progressive LLD and significant ankle instability due to the lack of a stabilizing lateral malleolus.
*
Type 2:
Denotes complete absence of the fibula. This is the most severe form, associated with profound LLD, severe ankle instability, and marked foot deformities.
Pappas's classification, which delineates eight grades based on the extent of fibular involvement and associated tibial bowing, also provides valuable insights into the variability of this condition. Key pathological features universally observed include progressive LLD, anterior-medial bowing of the tibia, ankle valgus (often with talar hypoplasia or dysplasia), and hypoplasia or agenesis of the lateral rays of the foot, frequently involving the 4th and 5th toes, or more extensive oligodactyly. The overarching therapeutic challenge lies in restoring functional limb length, achieving mechanical alignment, and ensuring a plantigrade, stable foot for independent ambulation.
Surgical Anatomy & Biomechanics
The congenital absence or hypoplasia of the fibula profoundly disrupts the normal anatomical relationships and biomechanical function of the lower limb. A detailed understanding of these alterations is crucial for meticulous surgical planning and execution.
Tibial Deformities
In the absence of its fibular counter-support, the tibia typically develops an anterior-medial procurvatum and varus deformity. This bowing can vary from subtle curvature to severe angulation, which may compromise overlying skin integrity or predispose to pseudoarthrosis. The inherent growth potential of the tibia may also be intrinsically affected, contributing to the progressive LLD. The distal tibial physis often appears irregular or dysplastic, and its growth plate activity can be disproportionately diminished, further exacerbating the LLD and angular deformities with growth.
Ankle Joint Anomalies
The ankle joint is consistently among the most severely affected articulations. The fibula's role as the lateral malleolus is critical for forming the ankle mortise and ensuring talar stability. In fibular deficiency:
*
Ankle Valgus:
This deformity is nearly universal, ranging from mild to severe, directly attributable to the absence of a competent lateral malleolar buttress and often compounded by a lateral tilt of the talus.
*
Talar Hypoplasia/Dysplasia:
The talus itself may be hypoplastic, flattened, or abnormally shaped, further contributing to joint incongruity and instability. Proximal migration of the talus relative to the distal tibia is a common finding, exacerbating the LLD and valgus.
*
Mortise Widening:
In Type 2 deficiency, the complete absence of the fibula results in a widened ankle mortise, allowing for excessive talar translation and severe instability. Even in Type 1B, the rudimentary fibula is often too short or dysplastic to provide functional stability.
*
Ligamentous Insufficiency:
The lateral collateral ligaments of the ankle are typically absent, severely attenuated, or functionally incompetent. The deltoid ligament on the medial side may be hyperplastic or contracted.
*
Muscle Imbalance:
Hypoplasia or agenesis of the lateral compartment muscles (peronei) accentuates the valgus deformity and compromises dynamic ankle stability. The Achilles tendon frequently exhibits contracture, contributing to an equinus component.
Foot Deformities
The foot in fibular deficiency presents with a characteristic constellation of deformities:
*
Lateral Ray Deficiency:
This is a hallmark feature, encompassing hypoplasia, aplasia, or absence of the lateral-most rays, most commonly the 4th and 5th toes. More extensive oligodactyly involving additional rays can also occur. This directly impacts foot width and stability.
*
Equinovalgus Deformity:
A complex three-dimensional deformity comprising hindfoot valgus and varying degrees of ankle equinus. This renders the foot functionally difficult for weight-bearing and shoe accommodation.
*
Tarsal Coalition:
A fibrous, cartilaginous, or bony synostosis between two or more tarsal bones, most frequently affecting the calcaneo-navicular or talo-calcaneal joints. Coalitions can lead to significant foot rigidity, pain, and contribute to progressive deformity, limiting the efficacy of conservative management.
*
Forefoot Abduction:
Often seen in conjunction with hindfoot valgus, further complicating gait mechanics and footwear.
Biomechanical Consequences
The culmination of these anatomical deviations results in profound biomechanical impairments:
*
Altered Load Bearing:
The absence of the fibula shifts axial weight-bearing stresses predominantly through the tibia, which is already structurally compromised. This leads to abnormal and uneven stress distribution across the ankle and foot, potentially accelerating degenerative changes.
*
Pathologic Gait:
The combination of LLD, ankle instability, and foot deformities gives rise to a compensatory gait pattern, such as circumduction, steppage gait, or excessive toe-walking. This results in increased energy expenditure, poor balance, and often chronic pain.
*
Progressive Deformity:
Without surgical intervention, both LLD and angular deformities tend to worsen with skeletal growth due to continued unequal growth plate contributions, asymmetric muscle pull, and abnormal loading.
Addressing these complex, multi-planar deformities requires a highly individualized, multi-stage surgical strategy, focused on restoring anatomical alignment, functional length, and a stable, plantigrade foot to facilitate pain-free and efficient ambulation.
Indications & Contraindications
The therapeutic decision-making process for children with fibular deficiency is highly nuanced, necessitating a careful evaluation of the severity of the anomaly, the child's functional status, and the potential benefits and risks of various interventions. The overarching objectives are to achieve limb length equality, correct angular and rotational deformities, provide a stable and plantigrade foot, and optimize functional independence for ambulation.
Indications for Intervention
Non-Operative Indications
- Mild Limb Length Discrepancy (LLD): Discrepancies typically less than 3-5 cm, particularly in younger children, can often be effectively managed with shoe lifts, orthoses, or custom bracing. These aids aim to improve gait mechanics, prevent compensatory postural adaptations (e.g., pelvic tilt, secondary scoliosis), and maintain ankle/foot alignment.
- Stable Ankle and Foot: Cases where ankle valgus and foot deformities are mild, non-progressive, asymptomatic, and well-accommodated by conservative measures.
- Very Young Age (<2 years): For certain complex reconstructive procedures, delaying surgery until the child has larger bone stock, better tissue quality, and a greater capacity for rehabilitation adherence may lead to more predictable outcomes. However, early bracing or casting might be initiated to prevent progressive deformity.
- Significant Medical Comorbidities: When the intrinsic risks associated with extensive surgery and prolonged anesthesia are deemed to outweigh the potential functional improvements.
- Patient/Family Preference: Following comprehensive counseling regarding all available options, including their respective risks, benefits, and expected long-term outcomes, some families may elect for a conservative approach or choose early prosthetic fitting.
Operative Indications
- Significant and Progressive LLD: Discrepancies projected to exceed 3-5 cm at skeletal maturity, particularly if causing functional impairment (e.g., pathologic gait, energy expenditure) or secondary spinal deformities.
- Severe Ankle Instability or Deformity: Persistent, painful, or progressive ankle valgus, severe equinus, or profound instability leading to significant gait disturbance, difficulty with footwear, or impending skin breakdown.
- Progressive Foot Deformity: Disabling equinovalgus deformities, painful tarsal coalitions, or severe lateral ray deficiencies that preclude functional weight-bearing, accommodate shoe wear, or are associated with chronic pain.
- Significant Tibial Bowing: Progressive anterior-medial tibial bowing that threatens skin integrity, creates a risk for pseudoarthrosis, or significantly impacts the mechanical axis.
- Failure of Non-Operative Management: When conservative measures no longer adequately control symptoms, prevent progression of deformity, or maintain functional independence.
- Optimizing Functional Outcomes: Surgical intervention is considered when it can demonstrably improve the child's ability to ambulate, participate in age-appropriate activities, reduce pain, and enhance overall quality of life. This often involves a thoughtful discussion comparing reconstruction versus primary amputation, especially in severe Type 2 deficiencies.
Contraindications
Absolute Contraindications
- Uncontrolled Systemic Conditions: Severe, unmanaged cardiac, pulmonary, neurological, or metabolic disorders that confer an unacceptably high anesthetic or surgical risk.
- Insufficient Skeletal Maturation/Bone Stock for Lengthening: In specific scenarios, severe hypoplasia or intrinsically poor bone quality may preclude successful osteogenesis and lengthening.
- Irreversible Neurovascular Compromise: Pre-existing severe neurovascular damage that would predictably be exacerbated by surgical maneuvers, particularly lengthening.
- Terminal Illness: When life expectancy is severely limited.
Relative Contraindications
- Lack of Patient/Family Adherence: Successful outcomes in complex limb reconstruction are highly dependent on dedicated compliance with a rigorous and prolonged rehabilitation program, including pin site care, distraction protocols, and physical therapy. Non-compliance can lead to catastrophic complications and poor results.
- Unrealistic Expectations: Patients and families must possess a clear, realistic understanding of the arduous treatment course, potential complications, the need for multiple staged procedures, and the expected functional rather than cosmetic outcome.
- Severe Local Tissue Conditions: Extensive scarring, poor skin quality, or chronic infection in the surgical field can increase complication rates.
- Profound Global Developmental Delay: In cases where a child's overall developmental trajectory and cognitive function suggest a limited potential for independent ambulation even after extensive limb reconstruction, a primary prosthetic fitting might be a more pragmatic and functionally beneficial option.
Operative vs. Non-Operative Indications Summary
| Indication Type | Operative Indications | Non-Operative Indications |
|---|---|---|
| Leg Length Discrepancy (LLD) | Projected >3-5 cm at skeletal maturity; progressive LLD causing gait abnormalities, pain, or spinal deformity. | Mild LLD (<3-5 cm) at skeletal maturity; manageable with shoe lifts, orthoses, or bracing; stable LLD not significantly impacting function. |
| Ankle Deformity | Severe, progressive, or painful ankle valgus/equinus; profound instability preventing functional weight-bearing or shoe accommodation; irreducibility of deformity. | Mild ankle valgus/equinus; stable ankle joint; asymptomatic or well-managed with bracing/orthotics; minimal impact on ambulation. |
| Foot Deformity | Severe equinovalgus; painful or rigid tarsal coalitions; disabling lateral ray deficiency preventing shoe wear or ambulation; progressive deformity. | Mild lateral ray deficiency without significant functional impact; flexible foot deformities manageable with accommodative footwear or orthotics; asymptomatic tarsal coalitions. |
| Tibial Deformity | Progressive anterior-medial bowing leading to skin compromise or high risk of pseudoarthrosis; significant angular deformity impacting mechanical axis. | Mild, non-progressive tibial bowing; stable bone without risk of pseudoarthrosis; minimal impact on mechanical axis and function. |
| Functional Impairment | Significant limitations in ambulation, participation in activities, or independence due to limb deformity or LLD; chronic pain related to deformity. | Unimpaired or minimally impaired function with conservative management; no significant pain; able to participate in age-appropriate activities with aids. |
| Age of Child | Typically 2-8 years for primary reconstructive procedures (e.g., centralization, osteotomies); adolescence for definitive LLD correction or internal lengthening nails. | Very young children (<2 years) awaiting more mature bone stock for complex reconstructions; patients with skeletal maturity for whom LLD is minor and stable. |
| Associated Factors | Failure of conservative management; realistic patient/family expectations; good local soft tissue quality; absence of major contraindications. | Significant medical comorbidities; lack of patient/family compliance; unrealistic expectations; poor local soft tissue health; patient/family preference for primary amputation in severe cases. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is the cornerstone of successful surgical outcomes in fibular deficiency, a condition characterized by high variability and complexity. A multidisciplinary approach involving orthopedic surgeons, physiatrists, prosthetists, and child life specialists is often beneficial.
Comprehensive Assessment
-
Clinical Evaluation:
- Detailed History: Birth history, developmental milestones, family history, previous interventions, functional limitations, and pain.
-
Physical Examination:
- Limb Length Discrepancy: Measured clinically (e.g., block test) and compared to expected growth curves.
- Angular and Rotational Deformities: Assess tibial bowing (anterior-medial procurvatum), ankle valgus, hindfoot valgus, and forefoot abduction/adduction. Evaluate range of motion at knee, ankle, and foot joints, identifying contractures (e.g., Achilles tendon).
- Foot Assessment: Note the number and morphology of toes (lateral ray deficiency), presence of skin creases, callosities, and overall foot flexibility/rigidity (e.g., suspicion for tarsal coalition).
- Neurovascular Status: Thorough assessment of sensation, motor function, and peripheral pulses. While major neurovascular anomalies are less common, nerves can be stretched or compressed by severe deformities.
- Gait Analysis: Observe the child's gait pattern for compensatory mechanisms, stability, and efficiency.
- Associated Anomalies: Screen for hip dysplasia, genu valgum, patellar instability, and spinal deformities (e.g., scoliosis).
-
Radiographic Imaging:
- Standing Full-Length AP/Lateral Radiographs (LLDograms): Essential for accurate LLD measurement and assessment of overall mechanical alignment of the lower extremity. These are critical for quantifying angular deformities and planning osteotomies.
- Ankle and Foot AP/Lateral/Oblique Views: To delineate ankle mortise anatomy, talar morphology, and specific foot deformities, including lateral ray deficiencies and potential tarsal coalitions.
- Computed Tomography (CT) Scan: Indicated for detailed 3D assessment of bony anatomy, joint congruity (especially ankle and subtalar), and identification of tarsal coalitions, which are notoriously difficult to fully characterize on plain radiographs. Pre-operative CT planning can precisely define osteotomy levels and angles.
- Magnetic Resonance Imaging (MRI): Useful for evaluating soft tissue structures (muscle hypoplasia, ligamentous integrity), cartilage quality, growth plate status, and neurovascular bundle relationships, particularly if nerve compression or severe soft tissue contractures are suspected.
-
Surgical Goals Formulation:
-
Based on the comprehensive assessment, define realistic and achievable goals:
- Correction of LLD to within functional limits (typically <2 cm).
- Establishment of a stable, plantigrade foot.
- Correction of significant ankle and tibial angular deformities.
- Improvement of ambulation and functional independence.
- A critical discussion regarding limb salvage versus primary amputation (Syme's) for severe Type 2 deficiencies is often necessary, considering expected functional outcomes, number of procedures, and psychological impact.
-
Based on the comprehensive assessment, define realistic and achievable goals:
Surgical Planning and Templating
- Lengthening Calculations: Using growth charts, predict LLD at skeletal maturity. Determine the total length required and the number of lengthening cycles.
- Osteotomy Planning: Precisely define the location, type (e.g., dome, wedge, transverse), and magnitude of osteotomies required for angular correction of the tibia and foot. Software-assisted planning (e.g., using Surgimap, specialized external fixator planning software) can be invaluable for complex multiplanar corrections with circular external fixators (Ilizarov, Taylor Spatial Frame).
- Fixator Configuration: Plan pin/wire placement to avoid vital structures and optimize stability. Determine the optimal frame design (monorail, circular).
- Soft Tissue Management: Anticipate the need for extensive soft tissue releases (e.g., Achilles tendon lengthening, lateral ankle ligament release, peroneal tendon releases) to facilitate correction.
- Grafting: Plan for potential bone graft harvest (e.g., iliac crest) if nonunion risk is high or structural augmentation is required.
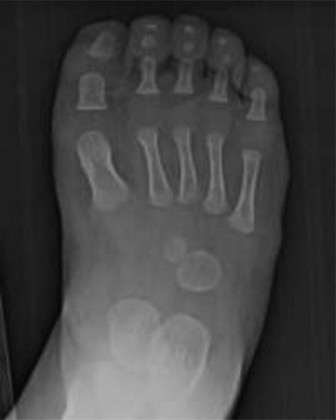
This image, likely depicting pre-operative radiographs or clinical assessment, underscores the importance of thorough initial evaluation in fibular deficiency.
Patient Positioning
- Supine Position: The patient is typically positioned supine on the operating table.
- Ipsilateral Hip Elevation: A bolster or blanket roll beneath the ipsilateral hip can facilitate internal rotation of the limb, providing optimal access to the lateral aspect of the leg and ankle.
- Tourniquet Application: A pneumatic tourniquet applied high on the thigh is essential for a bloodless field, which significantly aids visualization and reduces operative time.
- C-Arm Availability: Intraoperative fluoroscopy (C-arm) is mandatory for confirming osteotomy sites, pin placement, and assessing reduction and alignment throughout the procedure. The C-arm should be draped and positioned to allow for AP and lateral views without contamination of the sterile field.
- Padded Surfaces: All pressure points must be meticulously padded to prevent neuropathies or skin breakdown during prolonged procedures.
- Preparation for Graft Harvest: If bone grafting is anticipated, the ipsilateral iliac crest should be prepared and draped into the sterile field.
Detailed Surgical Approach / Technique
Surgical intervention for fibular deficiency is highly individualized, often involving a combination of procedures staged over several years. The primary goals are to achieve functional limb length, correct multi-planar deformities, and create a stable, plantigrade foot. Common strategies include limb lengthening, ankle stabilization, and foot reconstruction or amputation.
I. Limb Lengthening and Tibial Correction
A. Gradual Lengthening with External Fixators
This is the most common method for LLD correction and simultaneous correction of tibial bowing. Circular external fixators (Ilizarov, Taylor Spatial Frame) are preferred for their ability to correct complex multiplanar deformities.
-
Preparation and Incision:
- Patient positioned supine, tourniquet applied. The entire limb is prepped and draped from hip to toes.
- Identify proposed osteotomy site, typically in the metadiaphyseal region of the tibia, away from growth plates and major neurovascular structures. Mark the tibial crest and other anatomical landmarks.
- Small longitudinal incisions (2-3 cm) are made over the proposed osteotomy site.
-
Dissection and Internervous Plane:
- The incision is deepened carefully through subcutaneous tissue. The internervous plane for the tibia is generally straightforward, accessing bone directly over the anterior or anteromedial cortex.
- Care is taken to protect the superficial peroneal nerve laterally, the deep peroneal nerve anteriorly (distally), and the saphenous nerve and vein medially.
- Subperiosteal dissection is minimized to preserve periosteal blood supply for osteogenesis.
-
Corticotomy/Osteotomy:
- A percutaneous corticotomy is often favored to minimize soft tissue stripping. Multiple small drill holes are made around the tibial cortex (anteromedial or lateral) to weaken it, followed by an osteotome or Gigli saw passed percutaneously to complete the corticotomy, leaving the periosteum intact on the posterior aspect. This preserves the medullary blood supply.
- For significant angular correction, a wedge osteotomy might be necessary, though this typically involves more open exposure.
-
External Fixator Application:
- Proximal Ring/Half-Pin Placement: Two or more rings or half-pins are typically placed in the proximal tibia, ensuring stable fixation. Pins are inserted using drill guides, aiming for bicortical purchase, avoiding neurovascular structures and the proximal tibial physis.
- Distal Ring/Half-Pin Placement: Similar fixation is achieved in the distal tibia, ensuring adequate space for the desired lengthening and deformity correction. For ankle instability, rings can extend to the foot to provide stabilization.
- Frame Assembly: The chosen frame (e.g., Taylor Spatial Frame) is assembled according to pre-operative planning, connecting the proximal and distal bone segments. The foot component, if used, is meticulously attached to the foot frame.
- Intraoperative Fluoroscopy: Essential to confirm accurate pin/wire placement and verify immediate post-osteotomy alignment.
-
Distraction Protocol:
- Typically, distraction begins 5-7 days post-operatively (latency period) at a rate of 1 mm per day, divided into four equal increments (0.25 mm every 6 hours). This rate aims to optimize regenerate bone formation.
- The frame is adjusted according to the pre-programmed correction parameters if a TSF is used, or manually for an Ilizarov.
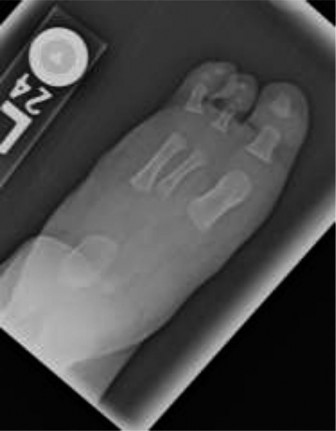
This image, likely showcasing an external fixator on a limb, illustrates the apparatus used for gradual lengthening and deformity correction.
B. Contralateral Epiphysiodesis
In specific cases of less severe LLD or when maximal lengthening of the affected limb is contraindicated or undesired, a contralateral epiphysiodesis (e.g., distal femur, proximal tibia) may be performed at the appropriate age to equalize limb lengths at skeletal maturity. This requires precise timing based on remaining growth and predicted LLD.
II. Ankle and Foot Reconstruction
These procedures are often performed concurrent with or subsequent to initial lengthening, depending on the severity and specific goals.
A. Supramalleolar Osteotomy and Ankle Stabilization
For ankle valgus deformity, particularly in Paley Type 1A/1B where some fibular remnant exists, or for improving ankle mortise congruity.
- Incision: Longitudinal incision over the medial or lateral aspect of the distal tibia and ankle, guided by the deformity.
- Dissection: Careful identification of the anterior tibial neurovascular bundle, deep peroneal nerve, and superficial peroneal nerve. Dissect to the distal tibial metaphysis.
- Osteotomy: A distal tibial dome or wedge osteotomy is performed to correct the valgus and often the procurvatum. The osteotomy is typically fixed with plates and screws, or can be incorporated into the external fixator.
- Soft Tissue Releases: Achilles tendon lengthening (Z-plasty) is often required for equinus. Lateral ankle ligament reconstruction or peroneal tendon transfer might be considered for residual instability if sufficient tissue exists.
- Centralization of the Talus: In cases where the talus has migrated proximally or laterally, soft tissue releases and occasionally osteotomies of the talus or calcaneus may be performed to achieve better alignment within the distal tibia. This often involves medial capsular release and careful reduction.
B. Foot Reconstruction for Lateral Ray Deficiency and Equinovalgus
-
Ray Resection:
For absent or severely hypoplastic lateral rays (4th/5th toes),
ray resection
is often performed to create a narrower, more functional foot, especially if associated with significant forefoot abduction or making shoe wear difficult. The goal is to create a well-aligned, stable tripod foot.
- Incision directly over the involved metatarsal and phalanx.
- Dissection down to the metatarsal, careful protection of neurovascular bundles to adjacent digits.
- Resection of the metatarsal and associated phalanges. The metatarsal is often resected at its base to minimize impact on the midfoot.
- Smooth edges and careful wound closure.
-
Calcaneal Osteotomy:
For hindfoot valgus, a
medializing calcaneal osteotomy
(e.g., Dwyer or modified Grice procedure) is often performed.
- Lateral incision over the calcaneus.
- Subperiosteal dissection to expose the lateral calcaneal wall.
- Osteotomy performed, typically a laterally based wedge, and fixed with K-wires or screws.
- Tarsal Coalition Resection: If symptomatic, the coalition is resected, and interposition material (fat graft, muscle) is used to prevent recurrence. This can improve foot flexibility and pain.
C. Syme's Amputation
In severe Type 2 fibular deficiency, particularly when associated with significant LLD, profound ankle instability, a non-functional foot, or when multiple complex reconstructive surgeries are anticipated with uncertain outcomes, a primary Syme's amputation (ankle disarticulation) is often a preferred option.
- Rationale: Creates an end-bearing stump, preserves growth potential of the distal tibia, and allows for excellent prosthetic fitting. This often results in superior functional outcomes and requires fewer surgeries than complex limb salvage.
-
Technique:
- Transverse incision made across the plantar aspect of the heel, extending dorsally to meet just distal to the malleoli.
- Dissection preserves the heel pad, crucial for end-bearing.
- Disarticulation of the talus and calcaneus.
- Trimming of the distal tibia and fibular remnants (if any) to create a smooth, bulbous end for prosthetic fit.
- The heel pad is carefully brought anteriorly and secured to the distal tibia, ensuring stable coverage.
- Careful hemostasis and wound closure.
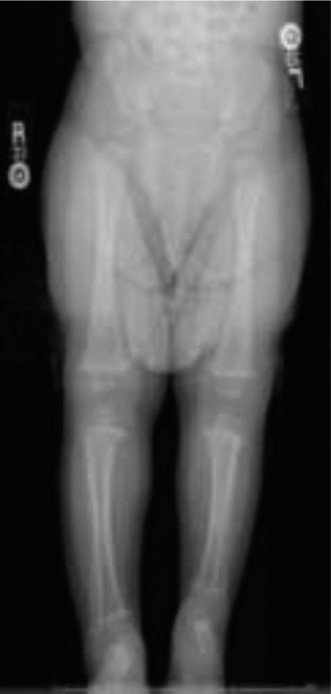
This image, potentially showing a post-operative limb or a specific foot deformity, would be contextually placed when discussing foot reconstruction or the end-result of treatment like Syme's amputation, emphasizing functional outcomes.
III. Fixation and Wound Closure
- Internal Fixation: Plates and screws may be used for osteotomies if not integrated with an external fixator. K-wires are frequently used for temporary fixation in foot procedures.
- External Fixation: Meticulous application and connection of the external frame as per planning.
- Wound Closure: Layered closure of all soft tissues. Careful attention to skin tension, especially over osteotomy sites and reconstructed foot areas. Sterile dressing application.
Complications & Management
Given the complexity and multi-staged nature of interventions for fibular deficiency, a high incidence of complications is anticipated. Proactive monitoring, early recognition, and appropriate management are critical for optimizing outcomes.
| Complication | Incidence (Approx.) | Management / Salvage Strategy B. Epiphysiodesis: To achieve ultimate limb length equality by arresting growth of the longer contralateral limb at the appropriate skeletal age. Requires careful growth plate analysis.
II. Ankle and Foot Reconstruction
These procedures are frequently performed in conjunction with or subsequent to initial lengthening, depending on the individual patient's severity and functional objectives.
A. Supramalleolar Osteotomy and Ankle Stabilization
For significant ankle valgus deformity, particularly in Paley Type 1A/1B where a fibular remnant exists, or to optimize ankle mortise congruity with a centralized talus.
- Surgical Incision: A longitudinal incision is made over the medial or lateral aspect of the distal tibia and ankle, based on the apex of the deformity and planned correction.
- Dissection and Internervous Planes: Careful dissection is performed, identifying and protecting critical neurovascular structures including the anterior tibial neurovascular bundle, deep peroneal nerve, superficial peroneal nerve laterally, and the saphenous nerve and great saphenous vein medially. Dissection proceeds to the distal tibial metaphysis, with minimal subperiosteal stripping.
- Osteotomy: A distal tibial dome or wedge osteotomy is meticulously performed to correct the valgus component and any associated procurvatum. The osteotomy can be fixed internally with plates and screws, or externally integrated into the existing external fixator frame for gradual correction.
- Soft Tissue Releases: An Achilles tendon lengthening (Z-plasty) is almost always required to address associated equinus contracture. In cases of residual instability, lateral ankle ligament reconstruction or transfer of redundant peroneal tendons (if present and functional) may be considered, although this is challenging due to inherent muscle hypoplasia.
- Centralization of the Talus: In instances where the talus is significantly proximally migrated or laterally subluxed, extensive soft tissue releases, often including medial capsular release and careful reduction, are performed to centralize the talus beneath the distal tibia. This improves joint congruity and distributes weight-bearing forces more evenly.
B. Foot Reconstruction for Lateral Ray Deficiency and Equinovalgus
-
Ray Resection for Lateral Ray Deficiency:
For absent, rudimentary, or severely hypoplastic lateral rays (typically the 4th and 5th toes),
ray resection
is often indicated to create a narrower, more functional, and cosmetically acceptable foot that can be easily accommodated by standard footwear. This is particularly relevant if there is significant forefoot abduction or splaying.
- Incision: Longitudinal incision directly over the involved metatarsal and phalanges.
- Dissection: Careful dissection is performed down to the metatarsal, meticulously identifying and protecting the common digital neurovascular bundles to adjacent digits.
- Resection: The metatarsal and associated phalanges are resected, often at the base of the metatarsal, to ensure a smooth contour and minimize impact on the midfoot joint.
- Closure: Meticulous hemostasis and layered wound closure are performed.
-
Calcaneal Osteotomy:
To correct significant hindfoot valgus, a
medializing calcaneal osteotomy
(e.g., Dwyer or modified Grice procedure) is frequently performed.
- Incision: A lateral incision is made over the calcaneus.
- Dissection: Subperiosteal dissection exposes the lateral calcaneal wall.
- Osteotomy: A laterally based wedge osteotomy is created, and the calcaneus is translated medially. Fixation is typically achieved with K-wires, screws, or staples.
-
Tarsal Coalition Resection:
If a tarsal coalition is symptomatic, causing pain, rigidity, or contributing to progressive deformity,
resection of the coalition
is performed.
- Approach: Determined by the location of the coalition (e.g., lateral for calcaneonavicular, medial for talocalcaneal).
- Resection: The fibrous, cartilaginous, or bony bridge is carefully excised.
- Interposition: To prevent recurrence, interpositional material such as a fat graft, muscle flap, or synthetic spacer is often placed into the resection gap.
C. Syme's Amputation
In cases of severe Type 2 fibular deficiency, particularly when accompanied by profound LLD (often greater than 8-10 cm), severe ankle instability that is not amenable to reconstruction, a non-functional or painful foot, or when multiple complex reconstructive surgeries with uncertain long-term outcomes are anticipated, primary Syme's amputation (ankle disarticulation) is often considered the most pragmatic and functionally superior option.
- Rationale: This procedure creates a robust, end-bearing stump that preserves the distal tibial epiphysis, allowing for continued growth and often resulting in superior prosthetic fitting and long-term functional outcomes compared to extensive limb salvage efforts. It minimizes the number of surgical interventions and prolonged rehabilitation periods.
-
Technique:
- Incision: A transverse incision is made across the plantar aspect of the heel, extending dorsally to meet just distal to the malleoli.
- Dissection: Meticulous dissection is performed to preserve the full heel pad and its blood supply, which is critical for creating an end-bearing stump.
- Disarticulation: The talus and calcaneus are disarticulated from the tibia and fibular remnants.
- Bone Preparation: The distal tibia and any fibular remnants are carefully trimmed and contoured to create a smooth, slightly bulbous end, optimizing it for prosthetic fit.
- Heel Pad Advancement: The preserved heel pad is meticulously advanced anteriorly and secured to the distal tibia, ensuring stable and well-vascularized soft tissue coverage for end-bearing.
- Closure: Meticulous hemostasis and layered wound closure are performed.
IV. Fixation and Wound Closure
- Internal Fixation: If not utilizing an external fixator, osteotomies may be stabilized with anatomically contoured plates and screws. K-wires are frequently employed for temporary or definitive fixation in foot reconstructions.
- External Fixation: The external frame is meticulously applied and tensioned as per the pre-operative plan, ensuring stability and correct alignment.
- Wound Closure: All incisions are closed in layers with careful attention to skin tension, particularly over osteotomy sites and areas of extensive soft tissue release or reconstruction. Sterile dressings are applied.
Complications & Management
Given the inherent complexity of fibular deficiency and the extensive nature of reconstructive procedures, a high incidence of complications is unfortunately anticipated. Proactive monitoring, early recognition, and aggressive management are paramount for mitigating adverse outcomes and achieving functional success.
| Complication | Incidence (Approx.) | Management / Salvage Strategy
|
Limb Length Discrepancy (LLD)
| Significant variability depending on severity (Type 1A: 2-8 cm; Type 1B: 6-15 cm; Type 2: 10-30 cm at maturity) | Limb lengthening (external fixator, internal lengthening nail), contralateral epiphysiodesis, shoe lifts (if residual LLD is minor). For severe cases not amenable to reconstruction, prosthetic fitting after Syme's amputation. |
|
Nonunion / Delayed Union
| 5-30% in lengthening procedures; higher in re-operations or poor regenerate quality. | Revision osteotomy with decortication, bone grafting (autograft or allograft), adjunctive stimulation (pulsed electromagnetic fields, low-intensity pulsed ultrasound), prolonged fixation, or conversion to internal fixation if appropriate. |
|
Pin Site Infection
| High (20-80% for superficial; 1-5% for deep osteomyelitis) | Meticulous pin site care, oral antibiotics for superficial infection, IV antibiotics for deep infection, pin exchange/removal, debridement and surgical washout for osteomyelitis. |
|
Nerve Injury (Neuropraxia)
| Low (1-5%, typically peroneal or sural nerve) | Observation, neurolysis if persistent or severe deficit, electrodiagnostic studies. Rarely, tendon transfers for functional deficits. Prevention through careful pin placement and gradual distraction. |
|
Vascular Impairment
| Rare (<1%) but limb-threatening | Immediate release of constricting elements (fasciotomy, removal of tension), surgical exploration, vascular repair/grafting. |
|
Joint Stiffness/Contracture
| Common (Knee/Ankle) | Aggressive physiotherapy, serial casting, dynamic splinting, botulinum toxin injections for spasticity, surgical release (e.g., knee arthrolysis, Achilles lengthening). Prevention with early ROM. |
|
Premature Consolidation
| Variable (during distraction) | Acute distraction under anesthesia, revision corticotomy/osteotomy, increasing distraction rate temporarily. |
|
Malunion / Angular Deformity
| Variable (recurrent bowing, valgus) | Corrective osteotomy (acute or gradual via external fixator), further lengthening. Prevention through precise pre-operative planning and meticulous intraoperative execution. |
|
Refracture After Frame Removal
| 5-10% (after tibial lengthening) | Internal fixation (plate/nail), re-application of external fixator, casting/bracing for stable fractures. Prevention with adequate consolidation time and protected weight-bearing. |
|
Residual Ankle Instability
| Common (even after reconstruction) | Long-term bracing (AFO), repeated soft tissue procedures, lateral ankle ligament reconstruction (if suitable tissue), or ankle arthrodesis for severe, painful instability. |
|
Foot Deformity Recurrence
| Common (equinovalgus, tarsal coalition) | Repeat osteotomies (calcaneal, midfoot), additional soft tissue releases, tarsal coalition resection, or ultimately, Syme's amputation if functionally compromised. |
|
Growth Arrest / Physeal Damage
| Low (if pins placed carefully) | Growth modulation (epiphysiodesis) of contralateral limb, further lengthening, or consideration for future internal lengthening nail. |
|
Psychosocial Issues
| Significant and underappreciated | Psychological counseling, patient support groups, realistic goal setting, involving child life specialists. Long-term support is crucial. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is an intensive and protracted process, integral to the success of surgical interventions for fibular deficiency. It requires a dedicated multidisciplinary team approach involving orthopedic surgeons, physical therapists, occupational therapists, and orthotists. Protocols must be tailored to the specific procedure, patient age, and individual response.
I. Acute Phase (Days 0-7, or during latency period if external fixation)
- Pain Management: Aggressive pain control with a multimodal approach (regional blocks, opioids, NSAIDs, acetaminophen) to facilitate early mobilization and patient comfort.
- Pin Site Care (for external fixators): Meticulous daily pin site cleaning with antiseptic solution (e.g., chlorhexidine) to prevent infection. Observe for redness, swelling, drainage.
-
Weight-Bearing:
- Internal Fixation/Foot Reconstruction: Non-weight-bearing initially (e.g., in a cast or splint) for 4-6 weeks, progressing to protected weight-bearing as per bone healing.
- External Fixation (Lengthening): Touch-down or partial weight-bearing as tolerated. Early loading encourages osteogenesis.
-
Range of Motion (ROM):
- Adjacent Joints: Active and passive ROM exercises for the knee, hip, and unaffected foot/toes to prevent stiffness and contractures.
- Affected Ankle/Foot: Gentle, protected ROM exercises may be initiated if compatible with surgical stability, particularly to prevent equinus contracture.
- Edema Control: Elevation of the limb, gentle compression (if no external fixator), and cryotherapy to minimize swelling.
II. Distraction Phase (Weeks 1-3 post-latency until desired length achieved)
- Distraction Protocol: Daily adjustments by the patient/family according to surgeon's prescription (typically 1 mm/day in 4 increments). Regular clinic visits (weekly-biweekly) for clinical and radiographic assessment.
- Pain Management: Continual optimization of pain regimen, considering nerve irritation from distraction.
- Pin Site Care: Continued meticulous daily care. Report any signs of infection promptly.
- Weight-Bearing: Continue partial weight-bearing as tolerated to stimulate regenerate bone formation. Encourage ambulation with crutches or a walker.
-
Physical Therapy (Intensive):
- Joint ROM: Crucial to prevent contractures, especially at the knee (flexion contracture) and ankle (equinus contracture). Daily stretching exercises, often with passive assistance, are essential.
- Muscle Strengthening: Isometric and isotonic exercises for the quadriceps, hamstrings, and hip musculature. Specific exercises for foot and ankle intrinsic muscles.
- Gait Training: Focus on proper gait mechanics, balance, and coordination with the external fixator.
- Stretching of Soft Tissues: Emphasize regular stretching of muscles and soft tissues that become tight with distraction (e.g., gastrocnemius-soleus complex, hamstrings).
- Neurovascular Monitoring: Regular assessment for signs of nerve irritation (paresthesias, weakness) or vascular compromise. Adjust distraction rate if symptoms arise.
- Radiographic Monitoring: Weekly or bi-weekly radiographs to assess regenerate bone quality, new bone formation, and monitor for early consolidation, bone deformity, or pin loosening.
III. Consolidation Phase (After distraction ends, until regenerate fully matured)
- Weight-Bearing: Progressive increase to full weight-bearing as tolerated. Continue to monitor for pain and alignment.
-
Physical Therapy:
- Aggressive ROM: Focus on regaining full range of motion in all joints, especially knee and ankle. Manual therapy and stretching are intensified.
- Strengthening: Progressive resistive exercises for all lower extremity muscles.
- Balance and Proprioception: Incorporate exercises to improve balance and coordination.
- Functional Training: Work towards activities of daily living and sport-specific training.
- Regenerate Assessment: Radiographs every 3-4 weeks to monitor bone mineralization and corticalization. The external fixator remains in place until there is adequate corticalization of the regenerate.
- Psychosocial Support: This phase can be prolonged. Continued psychological support and encouragement are vital.
IV. Post-Frame Removal / Post-Cast Phase
- Frame Removal: Performed when regenerate bone is adequately consolidated (typically corticalization of 3 out of 4 cortices). Often followed by a period of protected weight-bearing in a brace or cast.
-
Bracing/Orthotics:
- Protective Brace: A custom-molded orthosis (e.g., an AFO) may be worn for 3-6 months post-frame removal to protect the regenerate from refracture and to support the ankle/foot.
- Functional Orthotics/Shoe Lifts: Custom orthotics may be required long-term to manage residual foot deformities or LLD. Shoe lifts for any remaining LLD.
-
Intensive Physical Therapy:
The most critical period for regaining strength, flexibility, and normal gait.
- Full ROM Restoration: Manual stretching, joint mobilizations, and aggressive exercises to overcome stiffness.
- Strength Training: High-level strengthening to restore muscle power and endurance.
- Gait Retraining: Re-education to achieve a symmetrical, efficient, and pain-free gait pattern without external support.
- Scar Management: Massage, silicone sheeting, or other modalities to prevent hypertrophic scarring and improve skin pliability.
- Long-Term Follow-up: Regular clinical and radiographic follow-up is essential until skeletal maturity to monitor for recurrence of deformity, LLD, and degenerative changes. Further procedures may be necessary.
For patients undergoing Syme's amputation, rehabilitation focuses on stump care, desensitization, strengthening of hip/knee muscles, and early prosthetic fitting and gait training. This usually allows for a much faster return to functional ambulation.
Summary of Key Literature / Guidelines
Fibular deficiency has been a subject of extensive orthopedic literature, reflecting the evolving understanding and management strategies for this complex condition. The foundational work in classification by Paley, Pappas, and Achterman-Kuts has been instrumental in standardizing assessment and guiding treatment algorithms.
Limb Salvage vs. Amputation Debate:
One of the most significant and persistent debates in the management of severe fibular deficiency, particularly Type 2, centers on whether to pursue extensive limb salvage or primary Syme's amputation.
*
Limb Salvage Advocates
emphasize preserving the native limb, believing it can achieve a good functional outcome, potentially avoiding the psychological implications and maintenance challenges associated with a prosthesis. Multi-staged reconstructions, involving multiple lengthenings, angular corrections, and foot reconstructions, are the hallmark of this approach. Studies by investigators such as Paley and Herzenberg have demonstrated that aggressive limb lengthening and deformity correction with modern external fixation techniques (e.g., Ilizarov, Taylor Spatial Frame) can achieve functional limb length equality and a plantigrade foot, albeit requiring multiple surgeries and prolonged treatment times. However, residual deformities, stiffness, and the need for bracing are common.
*
Primary Amputation Advocates
(e.g., Syme's amputation) argue that for severe Type 2 deficiencies, this option often leads to a superior functional outcome with fewer surgical procedures, less pain, and a more predictable rehabilitation course. The creation of an end-bearing stump facilitates excellent prosthetic fitting and allows for a rapid return to ambulation. Studies by Kruger and others have highlighted that children with Syme's amputation for fibular hemimelia often outperform those with complex limb salvage in terms of gait efficiency, energy expenditure, and participation in high-impact activities, with potentially fewer long-term complications or need for revision surgeries. Psychosocial factors are critical in this decision, with some literature suggesting better overall psychosocial adaptation in amputees with well-fitting prostheses.
Current Trends and Techniques:
1.
Gradual Lengthening:
Ilizarov and Taylor Spatial Frame techniques remain the gold standard for LLD correction and simultaneous multi-planar deformity correction in pediatric patients, leveraging the principles of distraction osteogenesis. These frames allow for highly precise adjustments and can address complex angular and rotational deformities.
2.
Internal Lengthening Nails (e.g., PRECICE):
For older children nearing skeletal maturity or adolescents, internal lengthening nails offer the advantage of less external hardware, reduced infection risk, and improved patient comfort. However, their use in very young children or those with significant angular deformity is limited, and they are not typically used across open physes.
3.
Ankle and Foot Reconstruction:
Advances in understanding biomechanics have led to more precise osteotomies (e.g., distal tibial dome osteotomies for valgus, calcaneal osteotomies for hindfoot valgus) and soft tissue releases. The concept of "fibular centralization" or "neo-malleolus creation" aims to improve ankle stability, though long-term results of ankle reconstruction for severe Type 2 deficiencies remain challenging.
4.
Multidisciplinary Care:
The consensus strongly favors a multidisciplinary team approach, including orthopedic surgeons (with expertise in limb reconstruction), physiatrists, physical and occupational therapists, orthotists, prosthetists, and child psychologists. This collaborative model ensures comprehensive care addressing not only the physical but also the functional and psychosocial aspects of the condition.
5.
Long-Term Outcomes:
Key literature underscores that fibular deficiency often requires multiple staged procedures until skeletal maturity and beyond. Patients should be counseled that "cure" is not realistic; rather, the goal is optimal functional adaptation. Long-term follow-up studies emphasize the persistence of LLD, angular deformities, and joint stiffness, often necessitating further interventions or lifelong orthotic use. The focus has shifted from purely radiographic perfection to functional outcomes, patient satisfaction, and quality of life measures.
In summary, the management of fibular deficiency remains a challenging yet rewarding subspecialty of pediatric orthopedic surgery. While significant advancements have improved outcomes, the decision-making process for each child must be highly individualized, transparently discussing the pros and cons of complex reconstructions versus amputation to achieve the best possible functional and psychosocial adaptation.

