Patient Presentation & History
A 12-year-old male presented to the emergency department following a high-energy mechanism of injury. He was an unrestrained passenger in a motor vehicle collision, where the vehicle sustained a direct lateral impact. The patient reported immediate, severe pain localized to his right distal thigh and knee, accompanied by an inability to bear weight. There was no reported loss of consciousness or head injury. No other significant injuries were identified during the initial primary survey by the trauma team. His past medical history was unremarkable, with no known bleeding diatheses, metabolic bone disorders, or prior lower extremity trauma. He was prepubescent, with an estimated remaining growth potential of approximately 4-5 years based on Tanner staging and skeletal age assessment.
Clinical Examination
Upon initial assessment, the patient was alert and oriented, in significant distress dueating to pain.
Inspection
The right distal thigh and knee exhibited marked swelling, ecchymosis, and obvious deformity, specifically an angulatory deformity of the distal femur. The skin overlying the fracture site was intact, without evidence of open injury, tenting, or impending compromise. There was no obvious rotational deformity, but the knee appeared to be in a fixed position of slight flexion.
Palpation
Palpation revealed exquisite tenderness circumferentially around the distal femur, most pronounced over the medial and lateral femoral condyles and the suprapatellar region. A palpable gap or step-off consistent with a fracture was appreciated proximally to the physis. The knee joint was tense with effusion. There was no crepitus on gentle attempted motion.
Range of Motion
Active and passive range of motion of the right knee was severely limited and painful, estimated at 10-20 degrees of flexion and fixed at 5 degrees of flexion. Any attempt to move the joint elicited significant guarding. Ankle and foot range of motion were preserved and pain-free.
Neurological/Vascular Assessment
Distal neurological examination revealed intact sensation to light touch in the saphenous, superficial peroneal, deep peroneal, sural, and tibial nerve distributions. Motor function of the ankle and toes was intact and strong (5/5). The dorsalis pedis and posterior tibial pulses were palpable, strong, and symmetrical compared to the contralateral limb. Capillary refill in the toes was brisk (<2 seconds). However, due to the high-energy mechanism and significant soft tissue swelling, a high index of suspicion for vascular compromise was maintained. Continuous neurovascular monitoring was initiated.
Imaging & Diagnostics
Initial diagnostic imaging consisted of plain radiographs of the right femur and knee.
X-ray Findings
Anteroposterior (AP) and lateral views of the right distal femur clearly demonstrated a Salter-Harris type IV physeal fracture involving the medial femoral condyle. The fracture line extended from the articular surface of the medial femoral condyle, obliquely through the physis, and then proximally into the metaphysis. There was significant displacement of the articular fragment (medial condyle), with approximately 6mm of vertical displacement and 4mm of articular step-off. The epiphysis was displaced posteriorly and medially relative to the metaphysis. There was also a notable valgus angulation of the distal fragment relative to the femoral shaft. No other acute bony abnormalities were identified. The joint space appeared maintained, and there were no loose bodies visible on the plain radiographs.
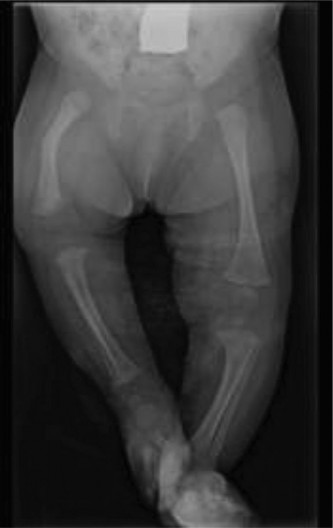
Above: Representative lateral radiograph demonstrating a distal femoral physeal fracture, showing posterior displacement and typical angulation.
CT/MRI Indications
Given the Salter-Harris type IV nature of the injury, which involves the articular surface and physis, a Computed Tomography (CT) scan with 1mm cuts was deemed essential for a comprehensive evaluation of the fracture morphology, particularly the articular involvement, displacement, and comminution. The CT scan confirmed the articular step-off and provided detailed visualization of the fracture lines extending through the physis and into the metaphysis. It further highlighted the extent of displacement of the articular fragment and confirmed the absence of significant comminution that would preclude open reduction internal fixation (ORIF).
Magnetic Resonance Imaging (MRI) was considered but not immediately pursued. While MRI can provide detailed information regarding soft tissue injuries (ligaments, menisci) and physeal integrity, the primary concern was achieving anatomic reduction of the articular surface and physis. The critical information for surgical planning (articular congruence, physeal displacement) was adequately provided by the CT scan. MRI would have been indicated if there were concerns for concomitant ligamentous injuries significantly influencing post-operative rehabilitation, or if persistent pain and instability were noted post-operatively without clear radiographic findings. Pre-operative MRI could also be considered for precise assessment of the growth plate injury, especially in complex cases or if growth arrest was a significant concern post-reduction, but it typically delays urgent operative intervention for displaced physeal fractures.
Templating
Pre-operative templating involved assessing the size and configuration of the distal femoral epiphysis and metaphysis to anticipate appropriate fixation hardware. Given the patient's age and the Salter-Harris IV classification, smooth K-wires for temporary fixation and cannulated screws for definitive fixation were considered. Screw length and diameter were estimated to ensure adequate purchase without violating the physis or articular cartilage unnecessarily. The goal was to achieve stable fixation across the metaphysis and epiphysis, bypassing the physis with smooth wires, or using screws perpendicular to the physis where safe. For Salter-Harris IV fractures, fixation across the physis with screws is often necessary in the epiphyseal-metaphyseal fragment to maintain reduction, but careful planning is crucial to avoid hardware within the critical growth zone, or to use small, smooth pins in areas of epiphyseal extension.
Differential Diagnosis
A comprehensive differential diagnosis for an acute pediatric knee trauma with significant deformity and pain, especially with a history of high-energy mechanism, includes several critical conditions that must be distinguished.
| Feature | Salter-Harris Type IV Distal Femoral Physeal Fracture (Our Case) | Proximal Tibial Physeal Fracture (e.g., S-H Type II) | Distal Femoral Metaphyseal Fracture (Complete) | Patellar Dislocation with Osteochondral Fracture |
|---|---|---|---|---|
| Injury Mechanism | High-energy, valgus/varus stress, axial load, direct impact | High-energy, valgus/varus, axial load | High-energy, axial load, direct impact | Twisting, direct blow, valgus-flexion-external rotation |
| Age Group | Adolescents (10-16 years) | Adolescents (10-16 years) | Children/Adolescents (variable, often younger) | Adolescents, particularly females |
| Clinical Presentation | Significant knee deformity, swelling, pain, inability to bear weight. Tenderness over distal femur. | Knee deformity, swelling, pain, inability to bear weight. Tenderness over proximal tibia. | Thigh deformity/swelling, pain, inability to bear weight. Tenderness proximal to physis. | Acute pain, knee "giving way," patellar displacement (may reduce spontaneously). Effusion, tenderness over patella/medial retinaculum. |
| Radiographic Findings | Fracture line from articular surface, through physis, into metaphysis. Articular step-off, physeal widening/displacement. | Fracture through physis, metaphyseal fragment ("Thurston Holland" sign). Variable displacement. | Fracture through metaphysis, intact physis. Angulation, displacement. | Patella displaced laterally (or reduced). May show osteochondral fragment, often from lateral femoral condyle or medial patella facet. |
| CT/MRI Role | CT critical for articular congruity/displacement. MRI for growth plate and soft tissue. | CT for complex displacement, MRI for soft tissue and growth plate. | CT for complex comminution, surgical planning. | MRI critical for osteochondral fragments and ligamentous injury (MPFL). |
| Vascular Injury Risk | High (especially popliteal artery due to distal displacement) | High (especially popliteal artery) | Moderate | Low |
| Nerve Injury Risk | Low (peroneal nerve possible with extreme displacement) | High (peroneal nerve due to proximal tibial displacement) | Low | Low (may have transient sensory deficits) |
| Growth Arrest Risk | High (type IV, involves germinal cells and articular cartilage) | Moderate-High (type II/III, partial or complete) | Low (physis intact) | None (physeal injury not involved) |
| Management Principle | Anatomic articular and physeal reduction (ORIF). Preserve growth plate. | Anatomic physeal reduction (closed vs. ORIF). | Non-operative (casting) or ORIF for unstable/displaced. | Closed reduction, rehabilitation. ORIF for large osteochondral fragments or MPFL repair. |
| Long-Term Complications | Growth arrest, angular deformity, arthritis. | Growth arrest, angular deformity. | Malunion, leg length discrepancy (rare). | Recurrent dislocation, patellofemoral pain/arthritis. |
Surgical Decision Making & Classification
The decision for operative management was paramount for this Salter-Harris type IV distal femoral physeal fracture. Non-operative management is typically reserved for non-displaced or minimally displaced (less than 2mm) physeal fractures without articular involvement (e.g., Salter-Harris type I or II) or for certain metaphyseal fractures in very young children. Given the significant displacement (>2mm) of both the physeal and articular components, as well as the inherent instability of a Salter-Harris type IV injury, operative intervention was the only viable option to achieve anatomic reduction and stable fixation, critical for optimizing long-term outcomes.
Classification:
The injury was classified using the
Salter-Harris classification system
, specifically as a
Salter-Harris Type IV fracture
. This classification denotes a fracture that extends from the articular surface, across the physis, and into the metaphysis.
*
Significance:
Salter-Harris type IV fractures carry a high risk of premature physeal closure and angular deformity because the fracture line crosses the physis, potentially damaging both the proliferative and germinal zones of the growth plate, and involves the articular cartilage, increasing the risk of post-traumatic arthritis if not anatomically reduced.
Surgical Goals:
- Anatomic Reduction: Achieve perfect restoration of the articular surface. This is critical to prevent post-traumatic arthritis.
- Anatomic Physeal Reduction: Restore alignment of the growth plate to minimize the risk of growth arrest or angular deformity.
- Stable Fixation: Provide sufficient stability to allow for early motion (where appropriate) and maintain reduction until fracture union, while minimizing damage to the growth plate.
- Growth Plate Preservation: Avoid placing hardware across the physis unless absolutely necessary for fixation, and if so, use smooth, small-diameter Kirschner wires (K-wires) that are subsequently removed.
Operative vs. Non-Operative Justification:
- Displaced Articular Fragment: Any articular step-off exceeding 1-2mm is a strong indication for ORIF to prevent future degenerative arthritis. The 6mm displacement observed here mandated operative correction.
- Physeal Displacement: Significant physeal displacement carries a high risk of growth arrest and angular deformity, especially with Salter-Harris type III and IV injuries. Accurate reduction is essential.
- Inherent Instability: Salter-Harris type IV fractures are inherently unstable due to the fragmented nature involving both the epiphysis and metaphysis. Closed reduction attempts are often unsuccessful in achieving and maintaining anatomic alignment, and repeated attempts carry risks of further soft tissue and physeal damage.
- High Energy Mechanism: High-energy injuries are often associated with more severe displacement and soft tissue injury, making non-operative treatment less predictable and often unsuccessful.
- Age and Growth Potential: The patient's remaining growth potential (4-5 years) makes accurate reduction of the physis paramount, as any malunion or growth arrest will have significant long-term consequences on limb length and alignment.
Surgical Technique / Intervention
The patient was taken to the operating theater urgently for open reduction and internal fixation (ORIF) once the trauma workup was completed and the patient was hemodynamically stable.
Patient Positioning
The patient was positioned supine on a radiolucent operating table. A high thigh tourniquet was applied to the right lower extremity, inflated to 300 mmHg after limb exsanguination. A bolster was placed under the ipsilateral hip to achieve neutral rotation of the limb. Intraoperative fluoroscopy was available and draped into the sterile field for real-time visualization of reduction and hardware placement.
Approach
A standard medial parapatellar arthrotomy approach was chosen. This allowed direct visualization and access to the fractured medial femoral condyle and the articular surface. The skin incision extended from the proximal patella, curving medially around the patella, and distally to the level of the joint line. The subcutaneous tissues were dissected, and the medial retinaculum was incised longitudinally. The vastus medialis obliquus was reflected anteriorly or split longitudinally, and a capsular incision was made to expose the fracture site. Care was taken to preserve the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) insertions.
Reduction Techniques
- Hemarthrosis Evacuation: The joint was irrigated to remove any hematoma and small bony fragments that might impede reduction.
- Visualization of Articular Surface: The fracture was meticulously cleaned, and the articular surface of the medial femoral condyle fragment was directly visualized.
- Provisional Reduction: Gentle traction and manipulation of the knee joint, combined with direct manipulation of the fracture fragments, were employed to achieve provisional reduction. The key was to align the articular surface first, using the contralateral intact articular cartilage as a guide. Reduction clamps (e.g., small pointed reduction clamps, Verbrugge clamps) were used to hold the articular fragment temporarily.
- Verification: Intraoperative fluoroscopy (AP and lateral views) was used to confirm preliminary reduction of the articular surface and the physis. A probe was used to run across the articular surface to ensure anatomical congruity without any step-off.
Fixation Construct
- Temporary Fixation: Once anatomic reduction was achieved and confirmed fluoroscopically, the articular fragment was temporarily secured with two smooth, 1.6 mm Kirschner wires (K-wires) inserted from the medial aspect of the condyle, across the fracture, and into the metaphyseal bone, aiming to avoid the central physeal plate. These were placed perpendicular to the fracture plane. These smooth wires are typically placed where they can provide stability without causing further damage to the growth plate and are removed during the definitive fixation or post-operatively.
-
Definitive Fixation:
Due to the Salter-Harris Type IV nature, involving the physis and metaphysis, and the need for robust stability, definitive fixation involved cannulated screws. Two partially threaded 4.0 mm cannulated cancellous screws were strategically placed.
- First Screw: Inserted from the non-articular surface of the medial femoral condyle, obliquely across the reduced fracture line, to engage the metaphyseal bone of the distal femur. This screw was placed carefully to avoid the main weight-bearing articular surface and the primary physeal plate, crossing the epiphyseal extension of the fracture into the metaphysis. A specific trajectory was chosen to provide compression across the fracture.
- Second Screw: A second partially threaded 4.0 mm cannulated cancellous screw was placed similarly, diverging slightly from the first, to enhance rotational stability and compression.
- Physeal Avoidance: Crucially, these screws were carefully planned to be either entirely within the epiphysis (if the fragment was large enough), or to cross the physis in areas where growth plate damage would be minimal (e.g., through the metaphyseal bone proximal to the physis and into the epiphysis in the area of the fracture extension, but not through the active growth zone if possible). In this Salter-Harris type IV case, where the fracture crosses the physis, screws often traverse the physis. When this occurs, partially threaded screws are preferred, and they must be positioned so that the threads do not cross the physis, allowing for potential growth. Alternatively, if crossing the physis is unavoidable, smooth K-wires are the preferred method for definitive fixation, and screws are placed metaphyseal-to-metaphyseal or epiphyseal-to-epiphyseal. In this specific Salter-Harris IV case with a large articular-physeal-metaphyseal fragment, screws could be placed from the articular fragment (epiphyseal component) across the fracture line into the metaphysis, perpendicular to the physis, to provide interfragmentary compression. The specific location and direction of these screws were chosen to maximize stability while minimizing disruption to the growth plate, particularly the central germinal cells. The smooth K-wires initially used for provisional fixation were then either removed or left in place if they provided additional necessary stability without crossing the growth plate.
- Final Checks: Final fluoroscopic images in multiple planes confirmed anatomic reduction and appropriate hardware placement. The stability of the construct was tested gently by moving the knee through a limited range of motion.
Wound Closure
The joint capsule, retinaculum, and vastus medialis were repaired layer by layer with absorbable sutures. The subcutaneous tissue was closed, and the skin was closed with staples or non-absorbable sutures. A sterile dressing was applied, and the limb was placed in a knee immobilizer.
Post-Operative Protocol & Rehabilitation
The post-operative protocol for a pediatric distal femoral physeal fracture is critical to prevent complications and optimize functional recovery, balancing the need for stability with the imperative for early motion to prevent stiffness and promote cartilage healing.
Immediate Post-Operative (Day 0-1)
- Pain Management: Multimodal analgesia, including epidural catheter (if placed), oral opioids, and NSAIDs.
- Neurovascular Monitoring: Hourly checks for the first 24-48 hours due to the risk of compartment syndrome or vascular injury from swelling.
- Immobilization: Knee immobilizer or hinged knee brace locked in extension for initial stability and comfort.
- Elevation: Continuous limb elevation to reduce swelling.
- Weight Bearing: Non-weight bearing (NWB) on the operative leg.
Early Post-Operative (Week 1-6)
- Immobilization: The knee immobilizer or locked hinged brace is maintained.
- Weight Bearing: Strictly NWB for 4-6 weeks to allow for initial fracture healing and prevent hardware failure or loss of reduction.
-
Range of Motion (ROM):
- Passive ROM: Gentle passive ROM may be initiated at 2-3 weeks post-op, limited to 0-30 or 0-45 degrees of flexion initially, gradually progressing as pain allows and radiographic healing progresses. This is initiated under guidance from a physical therapist.
- Active ROM: Gentle active ankle and toe movements are encouraged from day one to prevent stiffness and promote circulation. Active knee flexion is typically delayed until radiographic signs of union are present, often at 6-8 weeks.
- Physical Therapy: Focus on quadriceps isometric exercises, hamstring sets, and gluteal strengthening in the immobilized position.
- Wound Care: Daily dressing changes as per protocol, staple/suture removal at 2-3 weeks.
- Radiographic Follow-up: AP and lateral radiographs at 2 and 6 weeks to assess for maintenance of reduction and early signs of union.
Intermediate Post-Operative (Week 6-12)
- Radiographic Assessment: Evaluate for bridging callus and signs of early union. Once union is evident, gradual progression of activity is initiated.
- Weight Bearing: Progressive weight bearing (PWB) is started, typically with crutches or a walker. This progresses from partial to full weight bearing over 2-4 weeks.
- Range of Motion: Increase active and passive ROM. Goal to achieve full knee extension and greater than 90 degrees of flexion. Patellar mobilization exercises are crucial to prevent patellofemoral stiffness.
- Strengthening: Progressive strengthening exercises for quadriceps, hamstrings, and calf muscles. Closed-chain exercises (e.g., mini-squats, leg presses) introduced as weight bearing progresses.
- Brace: The hinged knee brace may be unlocked or removed for therapy sessions and then used for ambulation initially.
Late Post-Operative (Month 3-6+)
- Full Weight Bearing: Full weight bearing should be achieved.
- Full ROM: Aim for full, pain-free knee ROM.
- Return to Activity: Gradual return to activities of daily living. Low-impact activities (swimming, cycling) introduced first.
- Sport-Specific Training: For athletes, sport-specific drills and plyometric exercises are gradually incorporated under the guidance of a physical therapist.
- Hardware Removal: Consideration for hardware removal, especially if symptoms develop or if there is concern for future growth disturbance, typically 6-12 months post-op after complete union. Smooth K-wires, if used as definitive fixation across the physis, are often removed earlier (3-6 weeks).
- Long-term Follow-up: Regular follow-up for 1-2 years post-injury, then annually until skeletal maturity, to monitor for potential growth arrest, angular deformity, or limb length discrepancy. This includes periodic assessment with standing AP radiographs of the lower extremities with a scanogram to measure leg length.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- High Index of Suspicion for Vascular Injury: Distal femoral physeal fractures, especially those with significant displacement (e.g., posterior displacement), are notoriously associated with popliteal artery injury. Always perform a thorough neurovascular assessment, document pulses and perfusion carefully, and consider an Ankle-Brachial Index (ABI) or even angiography/CT angiography if pulses are diminished or equivocal.
- Salter-Harris IV Specifics: These are intra-articular and physeal. Anatomic reduction of both the articular surface and the physis is paramount. Failure to achieve anatomic reduction is a direct predictor of poor outcomes, including growth arrest and post-traumatic arthritis.
- Imaging for Planning: CT is almost mandatory for Salter-Harris type III and IV fractures to delineate articular involvement and displacement precisely. MRI provides detailed growth plate information but often delays urgent surgery.
- Growth Plate Protection: When placing hardware, always use smooth K-wires across the physis for temporary or definitive fixation (especially if spanning the physis for extended periods). If cannulated screws are used for metaphyseal-epiphyseal fixation, ensure threads do not cross the physis or are placed in a trajectory that minimizes growth plate damage, typically perpendicular to the physis in the metaphyseal bone to capture the epiphyseal fragment. Hardware removal after union is often considered.
- Stability of Fixation: Distal femoral fractures in children can be challenging to stabilize. The fixation needs to be robust enough to withstand early weight bearing (once indicated) and motion without sacrificing growth plate integrity.
- Soft Tissue Interposition: Ensure no soft tissue (periosteum, capsule, menisci) is interposed at the fracture site, as this will prevent anatomic reduction. Open reduction allows direct visualization and removal of any interposed tissue.
- Long-Term Monitoring: These injuries require long-term follow-up until skeletal maturity to detect and address potential complications like growth arrest, angular deformity, and leg length discrepancy. Serial scanograms are essential.
Pitfalls:
- Inadequate Reduction: Accepting even minimal articular step-off (>1-2mm) or physeal malalignment will almost certainly lead to long-term sequelae (arthritis, growth arrest, angular deformity). Strive for anatomical perfection.
- Neglecting Vascular Injury: Missing a popliteal artery injury can lead to limb ischemia and loss. A normal initial pulse may become compromised with swelling or reduction.
- Growth Plate Violation with Threaded Hardware: Using threaded screws across the physis (particularly the central, active growth zone) will cause growth arrest. Smooth K-wires are safer if physeal crossing is unavoidable.
- Insufficient Fixation: An unstable construct can lead to loss of reduction, delayed union, or non-union. The fixation must be appropriate for the fracture pattern and patient age.
- Premature Weight Bearing: Introducing weight bearing too early can lead to loss of reduction, hardware failure, or delayed union. Adherence to a strict NWB protocol initially is crucial.
- Delayed Presentation: Delayed presentation or diagnosis can make reduction more difficult due to early callus formation and soft tissue contracture.
- Compartment Syndrome: Although less common in distal femoral fractures than in tibia fractures, significant soft tissue swelling and hematoma in the thigh warrant vigilance for compartment syndrome.
- Failure to Plan Hardware Removal: In skeletally immature patients, hardware that crosses or impinges on the physis should generally be removed once union is achieved to prevent late growth arrest or irritation, unless removal carries higher risks.
- Ignoring Concomitant Injuries: High-energy mechanisms can cause other injuries, including ligamentous damage to the knee. While primary focus is on the fracture, a comprehensive assessment is vital.
