Introduction & Epidemiology
Total hip arthroplasty (THA) is one of the most successful surgical interventions in orthopedics, profoundly improving quality of life and restoring function for millions of patients globally. With increasing surgical volume and an aging population, the prevalence of primary and revision THA continues to rise. While the vast majority of patients experience excellent outcomes, a significant subset develops persistent pain following THA, necessitating a comprehensive understanding of its etiology and management. A painful total hip is a complex diagnostic and therapeutic challenge, demanding a systematic approach to differentiate mechanical failure from biological reactions, infection, or other causes. This review aims to outline the causes of painful THA and provide a structured framework for evaluation and treatment, targeting orthopedic surgeons, residents, and medical students.
Epidemiologically, patient satisfaction rates after THA are generally high, often exceeding 90%. However, 10-20% of patients report some degree of dissatisfaction or persistent pain post-operatively, which can be debilitating. The incidence of revision THA is projected to increase substantially, with aseptic loosening and periprosthetic joint infection (PJI) remaining the leading indications for revision. Understanding the underlying reasons for pain is paramount to successful salvage.
Surgical Anatomy & Biomechanics
A thorough understanding of the pertinent surgical anatomy and biomechanics is fundamental to both primary THA success and the differential diagnosis of a painful hip.
Bony Anatomy
- Acetabulum: The hemispherical socket provides articulation for the femoral head. Proper reaming and component placement (inclination 40-45°, anteversion 15-20°) are critical for stability and avoiding impingement.
- Femur: The femoral canal accepts the stem, and the proximal femur dictates offset and leg length. Calcar preservation and appropriate stem sizing are crucial.
Muscular Anatomy
- Abductors: Gluteus medius and minimus are paramount for gait stability. Injury or dysfunction (e.g., abductor tear, avulsion, fatty atrophy) can lead to trendelenburg gait and pain. The superior gluteal nerve innervates these muscles and is vulnerable during posterior or direct lateral approaches.
- Adductors: Adductor longus, brevis, magnus, gracilis, and pectineus. Contribute to medial stability. Psoas impingement on the anterior rim of the acetabular component can cause anterior groin pain.
- External Rotators: Piriformis, gemelli (superior/inferior), obturator internus, quadratus femoris. The piriformis is a key landmark, and its integrity and reattachment are important in posterior approaches. The short external rotators protect the sciatic nerve posteriorly.
- Hip Flexors: Iliopsoas, rectus femoris, sartorius.
- Hip Extensors: Gluteus maximus, hamstrings.
Neurovascular Anatomy
- Sciatic Nerve: Most vulnerable nerve in posterior approaches, typically lying deep to the external rotators. Risk of stretch or direct injury.
- Femoral Nerve: Vulnerable anteriorly, particularly with aggressive retraction during anterior approaches or in revision settings.
- Obturator Nerve: Medial to the psoas, vulnerable during medial acetabular wall reaming or cement extrusion.
- Lateral Femoral Cutaneous Nerve (LFCN): Sensory nerve, highly variable course, prone to injury with direct anterior or modified Hardinge approaches, leading to meralgia paresthetica.
- Superior Gluteal Nerve: Innervates gluteus medius/minimus. Vulnerable superiorly, especially in transtrochanteric or specific direct lateral approaches.
- Vascular Structures: Femoral artery/vein anteriorly, superior/inferior gluteal arteries posterolaterally.
Biomechanical Principles
- Leg Length Discrepancy (LLD): Can lead to gait abnormalities, back pain, and nerve stretch (e.g., sciatic nerve neuropraxia with lengthening). Precise leg length restoration is critical.
- Femoral Offset: The horizontal distance from the center of rotation to the femoral axis. Restoration is vital for abductor muscle tension, hip stability, and preventing impingement. Reduced offset can lead to limp and abductor insufficiency.
- Joint Center of Rotation: Optimizing the center of rotation minimizes joint reaction forces and wear, and aids in soft tissue balancing.
-
Component Positioning:
- Acetabular Inclination & Anteversion: "Safe zone" (Lewinnek: 40±10° inclination, 15±10° anteversion) aims to minimize dislocation and wear. Malposition can lead to impingement, edge loading, and accelerated wear.
- Femoral Anteversion: Combined with acetabular anteversion, determines overall hip stability and range of motion.
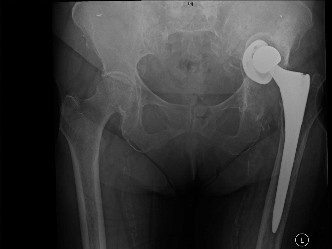
Indications & Contraindications
The decision to proceed with primary total hip arthroplasty, which aims to prevent future pain and improve function, relies on a combination of clinical assessment, radiographic findings, and patient expectations. Indications for revision surgery, on the other hand, directly address the painful total hip.
Operative Indications (Primary THA)
- Severe, debilitating hip pain unresponsive to conservative management.
- Radiographic evidence of end-stage degenerative joint disease (osteoarthritis), avascular necrosis, inflammatory arthritis, or post-traumatic arthritis.
- Functional impairment significantly impacting quality of life (e.g., restricted ambulation, sleep disturbance).
Non-Operative Management (Primary THA)
- Mild to moderate pain.
- Early stages of arthritis.
- Patients with significant medical comorbidities precluding surgery.
- Patients unwilling or unable to participate in post-operative rehabilitation.
Table: Operative vs. Non-Operative Management Indications (Primary THA Context)
| Category | Operative Indications | Non-Operative Management |
|---|---|---|
| Pain | Severe, intractable pain (NRS > 7/10) | Mild to moderate pain (NRS < 5/10) |
| Function | Significant functional limitation, impaired ADLs, limp | Minor functional limitations, good ADL independence |
| Radiographs | End-stage arthritis (Kellgren-Lawrence Grade III-IV), AVN | Early arthritis (Kellgren-Lawrence Grade I-II), joint space narrowing |
| Response to PT/Meds | Failed extensive conservative management (>3-6 months) | Responds to activity modification, NSAIDs, injections, PT |
| Patient Factors | Medically optimized, motivated for rehab | Significant comorbidities, poor surgical candidate, unwilling for surgery |
Pre-Operative Planning & Patient Positioning
Careful pre-operative planning and meticulous patient positioning are crucial steps in mitigating risks and optimizing outcomes for primary THA, thereby preventing many causes of a painful total hip.
Pre-Operative Planning
-
Patient Assessment:
- History & Physical: Document pain characteristics, functional limitations, previous surgeries, comorbidities, allergies. Assess gait, range of motion, neurovascular status, and presence of infection.
- Medical Optimization: Ensure cardiac, pulmonary, renal, and diabetic status are optimized. Anemia correction, DVT prophylaxis strategy (mechanical and/or chemical).
- Infection Screening: Rule out urinary tract infections, dental issues, or skin infections.
-
Imaging:
- Standard Radiographs: AP pelvis, frog-leg lateral, and true lateral views of the affected hip are essential for templating. Assess bone stock, osteophyte formation, deformity, and previous hardware.
- CT Scan: May be indicated for complex deformities, severe acetabular protrusio, or revision cases to assess bone loss and guide component placement using 3D reconstruction.
-
Templating:
- Size and Type: Determine appropriate acetabular cup size and position, femoral stem size and type (cemented/uncemented, standard/high offset), and head diameter/neck length.
- Leg Length & Offset: Critical for restoring biomechanics and stability. Aim for minimal leg length discrepancy (<5mm) and restoration of native offset.
- Surgical Approach: Determine the most appropriate surgical approach based on patient anatomy, surgeon preference, and potential challenges.
- Implant Selection: Choose implants based on patient age, bone quality, activity level, and surgeon experience. Consider bearing surfaces (metal-on-poly, ceramic-on-poly, ceramic-on-ceramic) based on wear characteristics and risk profiles.
- Consent: Comprehensive discussion of risks (infection, dislocation, nerve injury, leg length discrepancy, persistent pain, loosening, fracture), benefits, and alternatives.
Patient Positioning
Proper positioning is paramount for exposure, preventing nerve injury, and accurate component placement.
-
Lateral Decubitus Position (Posterior/Direct Lateral Approaches):
- Position patient on the unaffected side, secured with sacral post, anterior pelvic support, and posterior support.
- Pillows between knees and ankles to prevent nerve compression.
- Ensure proper padding of all pressure points (axilla, malleoli, fibular head).
- The operative leg should be free-draped for manipulation.
-
Supine Position (Direct Anterior Approach):
- Patient lies flat on their back, often on a specialized traction table.
- Bony prominences (sacrum, heels, occiput) well-padded.
- Foot of the operative leg secured in a boot for controlled manipulation.
- Consider a small bump under the ipsilateral hip for internal rotation and improved access.
Detailed Surgical Approach / Technique (Posterior Approach)
The posterior approach remains a workhorse for primary THA, offering excellent exposure of both the acetabulum and femur. Meticulous technique is vital to minimize complications that could lead to a painful hip.
Incision & Superficial Dissection
- Incision: A curvilinear incision centered over the greater trochanter, extending 8-10 cm proximally along the iliac crest towards the PSIS, and 8-10 cm distally along the femoral shaft.
- Fascial Layer: Incise the fascia lata in line with the skin incision. Identify the tensor fascia lata anteriorly and gluteus maximus posteriorly.
- Gluteus Maximus Split: The gluteus maximus fibers are split bluntly and retracted. Avoid excessive dissection superiorly to protect the superior gluteal neurovascular bundle.
Deep Dissection & Capsulotomy
- Identification of Short External Rotators: Retract the gluteus maximus and expose the short external rotators (piriformis, gemelli superior/inferior, obturator internus, quadratus femoris) overlying the posterior capsule. The sciatic nerve lies deep to these muscles.
- Release of External Rotators: The short external rotators are sharply released from their insertions on the greater trochanter, often as a single flap, taking a cuff of bone if possible for later repair. Tag sutures are placed for reattachment.
- Capsulotomy: A T-shaped or inverted T-shaped capsulotomy is performed, reflecting the posterior capsule to expose the femoral head and neck. Preserve as much capsule as possible for later repair.
Femoral Osteotomy & Dislocation
- Femoral Neck Osteotomy: With the hip internally rotated and adducted, measure leg length, determine the level of the osteotomy (typically 1-2 cm above the lesser trochanter), and perform the osteotomy.
- Femoral Head Removal: Dislocate the femoral head posteriorly or inferiorly. The head is then removed.
Acetabular Preparation
- Exposure: Retract the femur anteriorly and inferiorly. Use specialized retractors (e.g., Hohmanns) to expose the acetabulum circumferentially. Protect the sciatic nerve.
- Osteophyte Removal: Remove peripheral osteophytes and the labrum.
- Reaming: Sequentially ream the acetabulum starting with a smaller reamer and increasing size until host bone is exposed in all quadrants and a hemispherical socket is created. Aim for bleeding cancellous bone. Avoid over-reaming or eccentric reaming.
- Acetabular Component Insertion: Insert the definitive acetabular component with appropriate inclination (40-45°) and anteversion (15-20°). Ensure secure fixation (press-fit or screw fixation).
- Liner Insertion: Insert the polyethylene or ceramic liner.
Femoral Preparation
- Femoral Canal Reaming/Broaching: Prepare the femoral canal using sequential broaches or reamers, starting with a smaller size and increasing until cortical engagement is achieved proximally, ensuring a snug fit. Confirm appropriate anteversion of the broach.
-
Trial Reduction:
Insert a trial femoral stem and head.
- Reduction: Reduce the hip.
- Stability Assessment: Assess stability in flexion, extension, internal/external rotation, and in adduction/abduction.
- Leg Length & Offset Assessment: Compare leg lengths and assess offset, adjusting trial head and neck length as needed.
- Definitive Femoral Stem Insertion: Remove the trial components. Insert the definitive femoral stem (cemented or uncemented) with correct anteversion.
- Head Insertion: Impact the definitive femoral head onto the taper.
- Final Reduction: Reduce the hip.
Closure
- Final Stability Check: Perform a thorough range of motion assessment to confirm stability through a full range of motion.
- Capsular/Rotator Repair: Reattach the posterior capsule and short external rotators securely to the greater trochanter via drill holes or sutures. This is critical for post-operative stability and preventing soft tissue causes of pain.
- Fascial Closure: Close the fascia lata.
- Subcutaneous & Skin Closure: Close subcutaneous tissue and skin layers. Drain placement is optional.
Complications & Management
A painful total hip is typically a manifestation of a complication. A systematic approach to diagnosis and management is crucial. The differential diagnosis is broad, ranging from mechanical issues to infection and soft tissue problems.
Differential Diagnosis of Painful Total Hip
-
Aseptic Loosening:
- Mechanism: Failure of implant fixation to bone (uncemented) or cement mantle (cemented). Can be due to wear particle osteolysis, stress shielding, or mechanical mismatch.
- Presentation: Gradual onset groin or thigh pain, pain with activity, relieved by rest.
- Diagnosis: Radiographs (periprosthetic lucency >2mm, subsidence, cement mantle fracture), bone scan (diffuse uptake), advanced imaging (CT for osteolysis, PET/SPECT for inflammation).
- Management: Revision arthroplasty.
-
Periprosthetic Joint Infection (PJI):
- Mechanism: Bacterial colonization of the implant and surrounding tissues. Highly morbid complication.
- Presentation: Acute (within 3 months): fever, warmth, redness, swelling, acute severe pain. Chronic (>3 months): persistent pain, mild systemic symptoms, sinus tract.
-
Diagnosis:
- Labs: Elevated ESR, CRP. Leukocytosis. Synovial fluid aspiration (WBC count >3000 cells/uL, PMN% >80%, positive culture, alpha-defensin).
- Imaging: Radiographs (rarely diagnostic), bone scan, PET scan, MRI with metal artifact reduction.
- Intraoperative: Multiple tissue cultures, gram stain, frozen section histology (neutrophil count >10 PMN/HPF in 5 HPFs).
-
Management:
- Debridement and implant retention (DAIR): Early, acute infection, stable implant.
- One-stage exchange: Selected cases with known organism, good soft tissues.
- Two-stage exchange: Gold standard for chronic PJI (explant, antibiotic spacer, prolonged antibiotics, reimplantation).
- Suppression: For medically frail patients.
- Amputation/Arthrodesis: Salvage for failed exchanges.
-
Instability (Dislocation):
- Mechanism: Recurrent or chronic subluxation/dislocation. Can be due to component malposition, soft tissue imbalance, impingement, or patient factors.
- Presentation: Recurrent "giving way," apprehension, acute dislocation.
- Diagnosis: Clinical history, radiographs confirming dislocation or subluxation, CT to assess component position.
-
Management:
- Conservative: Activity modification, bracing for first-time dislocations.
- Operative: Component revision (repositioning or exchange), constrained liners, dual mobility implants, soft tissue repair.
-
Component Malposition:
- Mechanism: Improper inclination or anteversion of acetabular or femoral components.
- Presentation: Impingement, dislocation, accelerated wear, leg length discrepancy.
- Diagnosis: Radiographs, CT scan.
- Management: Revision arthroplasty.
-
Periprosthetic Fracture:
- Mechanism: Fracture around the implant, often intraoperative or post-operative due to trauma, stress risers, or osteolysis.
- Presentation: Acute pain, inability to bear weight.
- Diagnosis: Radiographs (often sufficient), CT for complex patterns.
- Management: Open reduction internal fixation (ORIF), revision arthroplasty with extended trochanteric osteotomy, or stem exchange, depending on fracture type (Vancouver classification).
-
Soft Tissue Impingement:
-
Iliopsoas Impingement:
Anterior groin pain, worse with hip flexion, external rotation. Caused by an anteriorly proud acetabular component or retained cement.
- Diagnosis: Clinical exam, MRI, diagnostic injection into psoas bursa.
- Management: Activity modification, NSAIDs, physical therapy, corticosteroid injection, arthroscopic psoas release, or revision of acetabular component.
-
Trochanteric Bursitis:
Lateral hip pain over greater trochanter, worse with activity, direct pressure.
- Diagnosis: Clinical exam, tenderness.
- Management: NSAIDs, physical therapy, corticosteroid injection, bursectomy (rare).
-
Gluteal Tendinopathy/Tear:
Lateral hip pain, weakness, Trendelenburg gait. Can be post-surgical (posterior approach) or related to implant design/offset.
- Diagnosis: Clinical exam, MRI.
- Management: Physical therapy, injection, surgical repair/reconstruction (e.g., gluteus maximus flap, allograft).
-
Iliopsoas Impingement:
Anterior groin pain, worse with hip flexion, external rotation. Caused by an anteriorly proud acetabular component or retained cement.
-
Nerve Injury:
- Mechanism: Stretch, compression, or direct laceration. Sciatic, femoral, obturator, LFCN.
- Presentation: Numbness, paresthesias, motor weakness in nerve distribution.
- Diagnosis: Clinical exam, EMG/NCS.
- Management: Observation (most neuropraxias resolve), physical therapy, nerve decompression, rarely nerve repair/graft.
-
Heterotopic Ossification (HO):
- Mechanism: Aberrant bone formation in soft tissues around the hip.
- Presentation: Stiffness, pain, restricted range of motion.
- Diagnosis: Radiographs (mature HO evident).
- Management: Prophylaxis (NSAIDs, radiation post-op for high-risk patients). Excision only for mature, symptomatic HO.
-
Hardware Impingement/Prominence:
- Mechanism: Prominent screws, cement, or implant edges causing soft tissue irritation.
- Presentation: Localized pain, especially with certain movements.
- Diagnosis: Radiographs, CT.
- Management: Hardware removal or revision if causing significant symptoms.
-
Referred Pain:
- Mechanism: Pain originating from spine, sacroiliac joint, knee, or abdominal/pelvic pathology.
- Presentation: Non-specific hip pain, often atypical for THA complications.
- Diagnosis: Thorough musculoskeletal and systemic workup. Diagnostic injections.
- Management: Address primary source of pain.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (approx.) | Salvage Strategies |
|---|---|---|
| Aseptic Loosening | 5-10% (10 yrs) | Revision arthroplasty (component exchange) |
| Periprosthetic Joint Infection | 0.5-2% | DAIR, 1-stage exchange, 2-stage exchange, suppression |
| Instability/Dislocation | 1-5% | Closed reduction, activity mod, component revision, constrained/dual mobility liners |
| Periprosthetic Fracture | 0.1-1.5% (intraop) | ORIF, stem revision, extended trochanteric osteotomy |
| Leg Length Discrepancy | 10-20% (>1cm) | Shoe lift, rarely revision for severe functional deficit |
| Nerve Injury (e.g., Sciatic) | 0.1-2% | Observation, physical therapy, nerve decompression (rarely) |
| Vascular Injury | <0.1% | Vascular repair (emergent) |
| Heterotopic Ossification | 5-10% (clinically) | Prophylaxis (NSAIDs/XRT), excision for mature HO |
| Soft Tissue Impingement | Varied | Injections, PT, arthroscopic release, component revision |
| Deep Vein Thrombosis (DVT) | 0.5-2% (symptomatic) | Anticoagulation, vena cava filter (rarely) |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing recovery, restoring function, and minimizing pain after THA. Protocols vary based on surgical approach, patient factors, and surgeon preference, but generally follow a phased progression.
General Principles
- Early Mobilization: Essential for preventing DVT, improving circulation, and promoting joint motion.
- Pain Management: Multimodal approach including NSAIDs, acetaminophen, nerve blocks, regional anesthesia, and opioids as needed. Aggressive pain control facilitates participation in therapy.
-
Weight-Bearing:
- Cemented implants: Typically weight-bearing as tolerated (WBAT) immediately.
- Uncemented implants: Often WBAT, but may be protected weight-bearing (PWB) or touch-down weight-bearing (TDWB) for specific press-fit or revision cases with compromised bone stock.
-
Precautions:
Specific hip precautions are typically maintained for 6-12 weeks, depending on the approach and surgeon.
- Posterior approach: Avoid hip flexion >90°, internal rotation, and adduction past midline.
- Anterior approach: Avoid hip hyperextension, excessive external rotation, and combined abduction/external rotation.
- Patient Education: Crucial for adherence to precautions, exercise programs, and recognition of warning signs.
Phased Rehabilitation
-
Phase I: Hospital Stay (Days 0-3)
- Goals: Pain control, bed mobility, transfers, independent ambulation with assistive device, initiate range of motion.
- Activities: Ankle pumps, quad sets, gluteal sets. Gentle active-assisted hip flexion (within precautions), abduction. Standing and ambulating short distances with walker/crutches. Stairs training.
- Focus: Safety, independent living skills, discharge planning.
-
Phase II: Early Home/Outpatient (Weeks 1-6)
- Goals: Wean from assistive devices, improve gait pattern, increase hip ROM and strength, manage swelling.
- Activities: Progress walking distance and duration. Gentle strengthening (isometric, isotonic) of hip abductors, extensors, and flexors (e.g., straight leg raises, sidelying abduction). Stationary cycling (low resistance). Water exercises. Scar massage.
- Focus: Restoring normal movement patterns and independent ambulation. Continue hip precautions.
-
Phase III: Intermediate Strengthening (Weeks 7-12)
- Goals: Discontinue hip precautions (if appropriate), advanced strengthening, improve balance and proprioception, functional return to light activities.
- Activities: Progress resistance exercises. Single-leg stance, balance training. Stair master, elliptical. Gradual return to driving and light recreational activities.
- Focus: Building endurance and functional strength, preparing for return to higher demand activities.
-
Phase IV: Advanced Activities & Maintenance (Months 3+)
- Goals: Full return to desired activities, long-term maintenance.
- Activities: Continue strengthening, flexibility, and cardiovascular conditioning. Gradual return to sports or higher-impact activities (surgeon and patient-dependent; low-impact generally preferred).
- Focus: Lifetime activity modification, monitoring for pain or symptoms.
Summary of Key Literature / Guidelines
The landscape of THA continues to evolve, supported by extensive clinical research and evidence-based guidelines. For the painful total hip, critical literature focuses on diagnostic algorithms, management of periprosthetic joint infection, and outcomes of revision surgery.
Periprosthetic Joint Infection (PJI) Guidelines
- International Consensus Meeting (ICM) on PJI: A landmark effort providing standardized definitions and diagnostic criteria for PJI, significantly improving consistency in diagnosis. The criteria often involve a combination of serological markers (ESR, CRP), synovial fluid analysis (cell count, PMN%, alpha-defensin), and microbiological cultures. Elevated synovial fluid alpha-defensin is a highly specific and sensitive marker for PJI.
- Musculoskeletal Infection Society (MSIS) Criteria: Widely adopted diagnostic criteria for PJI, including major criteria (e.g., sinus tract, positive cultures) and minor criteria (e.g., elevated ESR/CRP, elevated synovial WBC/PMN, positive histology).
- Management Strategies: The literature strongly supports two-stage exchange arthroplasty as the gold standard for chronic PJI, with reported success rates of 85-95%. One-stage exchange is gaining traction in selected cases with susceptible organisms and good soft tissue envelopes, particularly in Europe. DAIR is reserved for early, acute infections with a stable implant.
Implant Survivorship & Patient-Reported Outcomes (PROMs)
- National Joint Registries: Data from national registries (e.g., Swedish, Australian, NJR England & Wales) provide invaluable insights into long-term implant survivorship, identifying well-performing implants and identifying trends in failure mechanisms. Overall 10-year implant survivorship for primary THA typically exceeds 90-95%.
- PROMs: Patient-Reported Outcome Measures (PROMs) like the Hip disability and Osteoarthritis Outcome Score (HOOS) or Oxford Hip Score are increasingly used to assess the patient's perspective on pain, function, and quality of life. These measures are crucial for identifying patients with persistent pain despite technically successful surgery, prompting investigation into non-mechanical causes or patient-specific factors.
Revision Arthroplasty Outcomes
- Indications for Revision: Aseptic loosening and PJI remain the leading indications for revision THA. Instability, osteolysis, and periprosthetic fracture are also common.
- Outcomes: While revision THA can effectively alleviate pain and restore function, outcomes are generally not as favorable as primary THA. Revision surgery carries higher risks of complications (e.g., infection, dislocation, blood loss, nerve injury) and lower implant survivorship compared to primary procedures.
- Bone Loss Management: Significant literature addresses classification and management of periprosthetic bone loss (e.g., Paprosky classification for femoral and acetabular defects), emphasizing the importance of bone grafting, modular components, and impaction grafting techniques for successful reconstruction.
Conclusion
A painful total hip is a diagnostic challenge requiring meticulous evaluation. The systematic application of clinical assessment, laboratory testing, and advanced imaging, guided by established literature and consensus guidelines, is essential for identifying the precise etiology. Treatment strategies range from conservative measures and targeted injections to complex revision arthroplasty, with the ultimate goal of restoring a pain-free, functional hip. Continual professional development and adherence to evidence-based practices are paramount for navigating these complex cases successfully.
