Patient Presentation & History
Mr. P.C. is a 58-year-old male presenting to the emergency department following a low-energy fall at home. He reportedly tripped over a rug, landing directly on his left hip. He experienced immediate, severe pain in his left thigh and was unable to bear weight.
His medical history is significant for several previous fractures: a right distal radius fracture 5 years prior after a similar low-energy fall, and a left fifth metatarsal stress fracture 3 years ago, which was initially managed conservatively but progressed to non-union requiring surgical fixation. He also reports a history of premature loss of deciduous teeth as a child and subsequent early loss of permanent dentition, requiring dentures by age 45. He describes intermittent, generalized musculoskeletal pain for several years, often worse with activity, which he attributed to "getting older." He denies any history of bisphosphonate use or other anti-resorptive medications. He has no known family history of metabolic bone disease. His other comorbidities include well-controlled hypertension and dyslipidemia. He is a non-smoker and consumes alcohol socially.
Clinical Examination
Upon arrival, Mr. P.C. was alert and oriented.
Inspection
The left lower extremity exhibited noticeable deformity, with external rotation and shortening consistent with a femoral shaft fracture. Significant swelling and ecchymosis were observed over the lateral aspect of the mid-to-distal thigh. No open wounds were present.
Palpation
Palpation revealed exquisite tenderness along the mid-diaphysis of the left femur. Gross crepitus was elicited with gentle manipulation.
Range of Motion
Active and passive range of motion of the left hip, knee, and ankle were severely restricted and painful due to the obvious femoral fracture.
Neurological Assessment
Distal neurological examination revealed intact sensation to light touch in the L2-S1 dermatomes. Motor function was limited due to pain, but gross ankle dorsiflexion and plantarflexion were possible. No evidence of sciatic or femoral nerve compromise.
Vascular Assessment
The left dorsalis pedis and posterior tibial pulses were palpable, strong, and symmetric with the contralateral limb. Capillary refill was brisk in the toes (<2 seconds). Ankle-brachial index (ABI) was not assessed acutely but would be part of a complete workup if concerns existed.
Imaging & Diagnostics
Initial Radiographs
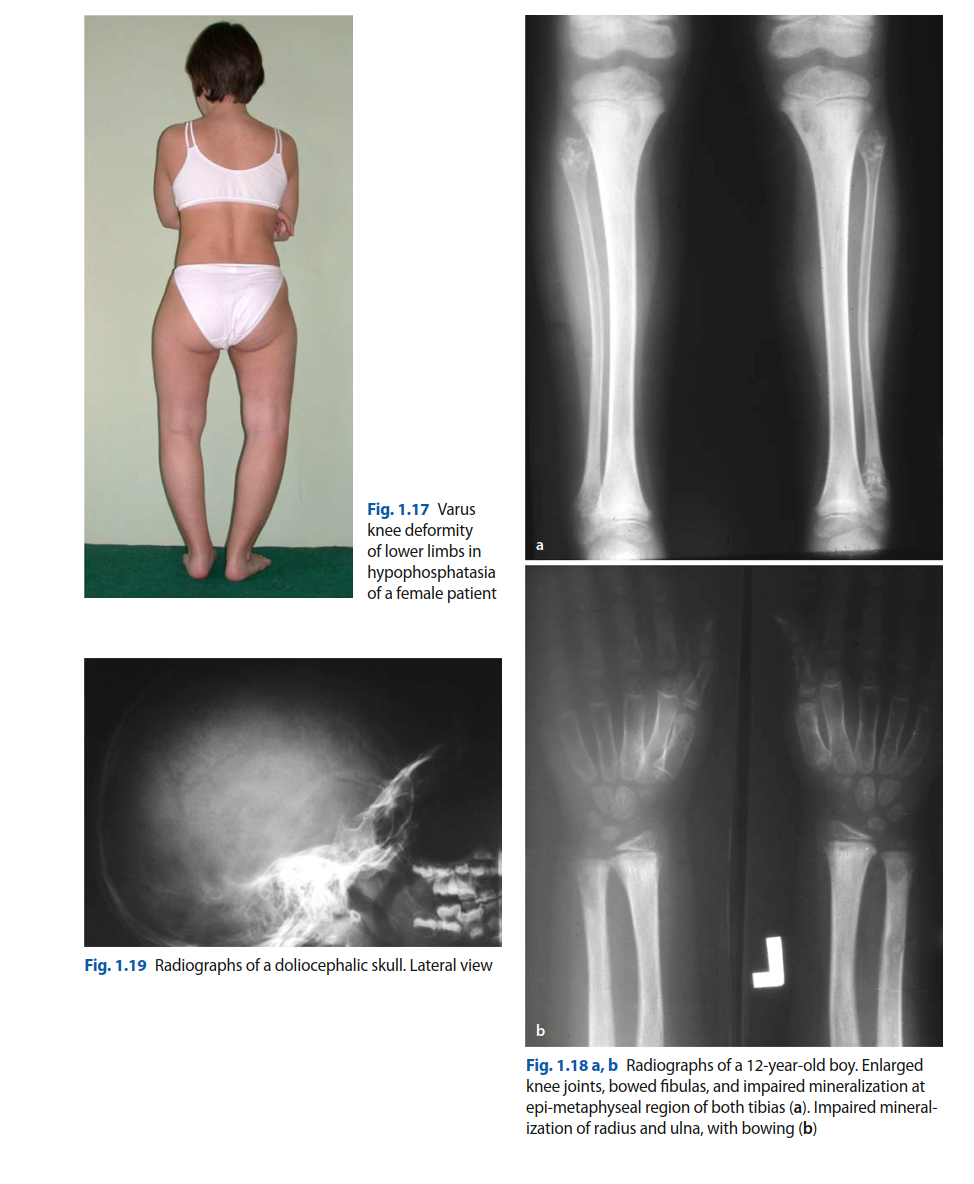
Anteroposterior (AP) and lateral radiographs of the left femur were obtained in the emergency department. These revealed a complete, transverse, atypical subtrochanteric femoral fracture, approximately 5 cm distal to the lesser trochanter. Characteristic features of an atypical femoral fracture (AFF) were present, including a non-comminuted transverse fracture pattern, localized periosteal thickening (beaking) of the lateral cortex at the fracture site, and generalized cortical thickening along the femoral shaft. There was no evidence of comminution or spiral extension. Generalized osteopenia was noted throughout the skeletal survey, and previous hardware from the fifth metatarsal fixation was visible.
Advanced Imaging
- Computed Tomography (CT) Scan: A CT scan of the left femur was performed for detailed fracture characterization and pre-operative planning. It confirmed the transverse, non-comminuted nature of the fracture and provided a precise understanding of the cortical thickening and the medullary canal dimensions. It also ruled out any underlying neoplastic process, which can mimic AFF. Importantly, the CT demonstrated diffuse osteopenia and thin cortices in other areas, despite the localized thickening at the fracture site.
- Magnetic Resonance Imaging (MRI): An MRI was not routinely indicated for acute, displaced femoral shaft fractures unless there was suspicion of significant soft tissue injury, pathological fracture not evident on CT, or occult contralateral injury. In this case, given the clear traumatic etiology and characteristic radiographic findings, MRI was deferred.
Laboratory Investigations
Given the patient's history of recurrent low-energy fractures, generalized bone pain, dental issues, and the atypical nature of the current fracture, a comprehensive metabolic bone workup was initiated.
*
Serum Alkaline Phosphatase (ALP):
Markedly reduced at 25 U/L (reference range 40-129 U/L). This finding was highly suggestive of hypophosphatasia.
*
Pyridoxal 5'-Phosphate (PLP):
Elevated at 180 nmol/L (reference range 20-100 nmol/L). This is a substrate for tissue-nonspecific alkaline phosphatase (TNSALP) and accumulates when TNSALP activity is low.
*
Phosphoethanolamine (PEA):
Elevated in urine at 450 µmol/24hr (reference range <200 µmol/24hr). Another TNSALP substrate, its elevation further supported the diagnosis.
*
Serum Calcium:
Normal (9.2 mg/dL).
*
Serum Phosphate:
Normal (3.5 mg/dL).
*
Parathyroid Hormone (PTH):
Normal (38 pg/mL).
*
25-hydroxyvitamin D:
Within normal limits (35 ng/mL).
*
Creatinine and eGFR:
Within normal limits.
*
Complete Blood Count (CBC) and Inflammatory Markers:
Unremarkable.
Genetic Testing
Following the biochemical findings, genetic testing for mutations in the ALPL gene was ordered, which subsequently confirmed a heterozygous mutation, consistent with the diagnosis of Adult Hypophosphatasia.
Bone Densitometry (DXA Scan)
A Dual-energy X-ray Absorptiometry (DXA) scan was performed once the patient was stable, revealing osteopenia (T-score -1.8 at the lumbar spine, -2.1 at the non-fractured right hip), which is often observed but not diagnostic for hypophosphatasia.
Pre-operative Templating
Pre-operative templating based on orthogonal radiographs and CT scans was crucial. This involved:
* Determining optimal nail length, diameter, and curvature.
* Assessing the entry point to avoid iatrogenic fracture or malreduction.
* Planning the number and trajectory of locking screws, considering the compromised bone quality associated with hypophosphatasia and the specific cortical thickening at the fracture site. A long cephalomedullary nail was templated to span the entire length of the femur and provide maximum stability, especially given the increased risk of non-union and propagation in HPP patients.
Differential Diagnosis
The presentation of an atypical femoral fracture in a patient with a history of recurrent low-energy fractures and dental issues necessitates a broad differential diagnosis for underlying metabolic bone disease.
| Feature | Hypophosphatasia (HPP) | Osteomalacia | Bisphosphonate-Related Atypical Femoral Fracture (BR-AFF) | Osteoporosis (Severe) |
|---|---|---|---|---|
| Pathophysiology | Deficient tissue-nonspecific alkaline phosphatase (TNSALP) activity due to ALPL gene mutation, leading to accumulation of mineralization inhibitors (PLP, PEA). | Defective mineralization of osteoid due to prolonged vitamin D deficiency or phosphate wasting. | Suppressed bone remodeling by bisphosphonates, leading to accumulation of micro-damage. | Reduced bone mass and microarchitectural deterioration leading to increased fragility. |
| Typical Presentation | Childhood: rickets, craniosynostosis. Adult: premature tooth loss, recurrent fractures (often atypical), generalized bone pain, chondrocalcinosis. | Generalized bone pain, muscle weakness, pathological fractures (vertebral compression, pseudo-fractures/Looser zones). | Unilateral prodromal thigh pain, often followed by a transverse or short oblique fracture of the subtrochanteric or femoral shaft region. | Fragility fractures, particularly vertebral, hip, wrist, after low-energy trauma. |
| Fracture Pattern | Often atypical femoral fractures (transverse, cortical thickening), stress fractures, delayed union/non-union. | Pseudo-fractures (Looser zones), vertebral compression, long bone fractures. | Transverse or short oblique, non-comminuted, localized lateral cortical thickening ("beaking"). | Vertebral compression fractures, hip fractures (intertrochanteric, femoral neck), distal radius. |
| Biochemical Markers | Low/undetectable serum ALP , elevated plasma PLP, elevated urine PEA. Normal Ca, P, PTH, Vit D (unless co-existing deficiency). | Low serum Ca (often), low P (often), elevated PTH, low 25(OH)D . ALP may be normal or slightly elevated. | Normal serum ALP, Ca, P, PTH, Vit D (unless co-existing deficiency). | Normal serum Ca, P, PTH, Vit D (unless co-existing deficiency); normal ALP. |
| Radiographic Features | Generalized osteopenia, metaphyseal changes (rickets in children), premature tooth loss, chondrocalcinosis, atypical fractures. | Generalized osteopenia, cortical thinning, pseudo-fractures (bilateral, symmetric lucencies perpendicular to cortex), bowing deformities. | Localized lateral cortical thickening ("beaking"), transverse or short oblique fracture, often incomplete. | Generalized osteopenia, vertebral compression fractures, loss of cortical thickness, prominent trabecular pattern. |
| Management Implications | Enzyme replacement therapy (asfotase alfa) is indicated. Surgical fixation for fractures with careful consideration of bone quality. Multidisciplinary approach. | Vitamin D and calcium supplementation. Address underlying cause of deficiency. Surgical fixation for fractures. | Discontinue bisphosphonates. Consider teriparatide for delayed healing. Prophylactic nailing for incomplete AFF. | Anti-resorptive or anabolic agents. Calcium and Vitamin D. Fall prevention. Surgical fixation for fractures. |
Surgical Decision Making & Classification
Given the complete, displaced, atypical subtrochanteric femoral fracture, operative management was unequivocally indicated. Non-operative management of complete femoral shaft fractures carries an unacceptably high risk of malunion, non-union, and significant morbidity, especially in a patient with compromised bone quality.
Classification
The fracture was classified as an
Atypical Femoral Fracture (AFF)
based on the American Society for Bone and Mineral Research (ASBMR) criteria:
1. Location: Subtrochanteric region.
2. Pattern: Transverse, non-comminuted.
3. Appearance: Localized periosteal thickening of the lateral cortex ("beaking") at the fracture site.
4. Absence of severe comminution or spiral component.
5. Absence of high-energy trauma.
6. Absence of osteoporosis or other metabolic bone disease that fully explains the fracture, although HPP is an underlying metabolic disease, AFF is a descriptive term for this fracture pattern often seen in HPP or with bisphosphonate use.
The specific characteristics of the fracture (complete, displaced) necessitated urgent surgical stabilization.
While AO/OTA classification could be applied (e.g., 32-A3 for subtrochanteric), the "atypical" designation takes precedence due to the underlying pathophysiology and implications for healing.
Pre-operative Considerations for Hypophosphatasia
The diagnosis of Hypophosphatasia significantly influenced pre-operative planning:
1.
Impaired Bone Healing:
Patients with HPP have impaired mineralization, leading to a high risk of delayed union or non-union. This mandated a fixation construct that provided maximum stability and consideration for adjunctive bone grafting.
2.
Bone Quality:
The generalized osteopenia and altered cortical structure meant bone might be more fragile during reaming and screw insertion.
3.
Anesthesia:
Standard protocols, but careful positioning to prevent iatrogenic fractures in other osteopenic areas.
4.
Enzyme Replacement Therapy (ERT):
Discussion with the patient and endocrinology regarding the initiation of asfotase alfa. While ERT primarily improves mineralization long-term, initiating it pre-operatively or early post-operatively could potentially aid fracture healing by improving local bone quality. However, acute fracture fixation generally proceeds without delay for ERT initiation. For this patient, a plan was made to initiate ERT with asfotase alfa in the immediate post-operative period after consulting with endocrinology.
Surgical Technique / Intervention
The definitive treatment chosen was intramedullary nailing, which is the gold standard for femoral shaft and subtrochanteric fractures, offering biomechanical advantages in load sharing and stability.
Patient Positioning
The patient was carefully positioned supine on a fracture table. The contralateral limb was abducted and flexed to allow for fluoroscopic imaging access. The ipsilateral limb was placed in traction to achieve preliminary length restoration and facilitate reduction. Proper padding was used to prevent pressure sores and iatrogenic injury to nerves or skin.
Surgical Approach
A standard antegrade approach was utilized for intramedullary nailing.
1.
Incision:
A curvilinear skin incision (approximately 5-7 cm) was made proximal to the greater trochanter, centered over its tip.
2.
Muscle Dissection:
The fascia lata was incised, and the abductor muscles (gluteus medius and minimus) were split in line with their fibers to expose the greater trochanter.
3.
Entry Portal:
The optimal entry portal was identified as the tip of the greater trochanter, slightly medial to its apex and in line with the femoral shaft axis. A guidewire was inserted, and an awl or cannulated drill was used to create an entry portal. Fluoroscopic guidance in both AP and lateral planes was critical to ensure correct entry point and prevent varus or valgus malalignment.
Reduction Techniques
Achieving and maintaining reduction for an atypical subtrochanteric fracture in HPP can be challenging due to cortical thickening and potential difficulties with standard reduction maneuvers.
1.
Traction:
Initial traction on the fracture table was applied to restore length.
2.
Rotation:
The limb was carefully rotated to correct any rotational deformity.
3.
Manual Reduction:
Gentle manual manipulation of the fracture fragments was performed.
4.
Blocking Screws:
Given the transverse nature and tendency for varus malalignment in subtrochanteric fractures, the use of blocking screws (Poller screws) was considered to guide the nail centrally and maintain reduction. These screws are placed eccentrically in the metaphysis to effectively narrow the canal and prevent eccentric nail placement. For this specific case, two Poller screws were placed anteriorly and posteriorly in the distal fragment, just proximal to the fracture site, to ensure optimal nail trajectory and maintain alignment.
5.
Direct Reduction:
In some instances, a limited open approach with reduction clamps may be necessary if closed reduction fails, but every effort was made to achieve closed reduction to minimize soft tissue stripping. Closed reduction was successful in this case.
Fixation Construct
A long, large-diameter cephalomedullary nail (e.g., Synthes PFNA II or similar) was chosen due to the subtrochanteric location, the atypical nature of the fracture, and the systemic bone disease.
1.
Reaming:
Progressive reaming of the medullary canal was performed. Care was taken during reaming due to the potentially altered bone density and cortical thickening. The reamer size was advanced incrementally, and the canal was over-reamed by 1.0-1.5 mm relative to the chosen nail diameter to facilitate insertion and reduce impaction forces.
2.
Nail Insertion:
The appropriately sized intramedullary nail was slowly advanced across the fracture site and into the distal fragment under fluoroscopic guidance. The tip of the nail was seated just proximal to the femoral condyles, ensuring it spanned the entire length of the femur for maximum stability and to prevent subsequent fracture propagation distally, a known risk in HPP.
3.
Proximal Locking:
Two cephalic screws were inserted through the nail into the femoral head, providing rotational and axial stability in the proximal fragment. A third proximal locking screw was inserted into the neck (if available on the chosen nail system) or into the trochanteric region to enhance rotational control.
4.
Distal Locking:
Static distal locking was performed using two interlocking screws in both AP and lateral planes. Careful fluoroscopic technique with perfect circle was used to ensure accurate placement and adequate purchase in the distal fragment.
5.
Wound Closure:
The wounds were thoroughly irrigated, and hemostasis was achieved. The muscle layers and fascia were closed, followed by subcutaneous tissue and skin closure.
Post-Operative Protocol & Rehabilitation
The post-operative management of a patient with an atypical femoral fracture due to Hypophosphatasia requires a nuanced approach, balancing stability with the known challenges of bone healing in this condition.
Immediate Post-Operative Period (Days 0-7)
- Pain Management: Multimodal analgesia, including epidural, regional blocks, and oral analgesics, to facilitate early mobilization.
- Weight-Bearing: Strict protected weight-bearing (toe-touch or minimal partial weight-bearing, 10-15 kg) on the operative leg, using crutches or a walker. This limitation is critical due to the impaired healing potential in HPP.
-
Physical Therapy (PT):
- Initiate active and passive range of motion (ROM) exercises for the hip and knee.
- Ankle pumps and quadriceps/gluteal isometric exercises to prevent stiffness and deep vein thrombosis (DVT).
- Bed mobility and transfer training.
- DVT Prophylaxis: Standard chemical and mechanical DVT prophylaxis.
- Metabolic Management: Initiation of enzyme replacement therapy (ERT) with asfotase alfa was commenced under endocrinology guidance. This therapy aims to normalize ALP levels and improve bone mineralization.
Early Rehabilitation (Weeks 1-6)
- Weight-Bearing Progression: Progress to partial weight-bearing (25-50% body weight) as tolerated, provided there is radiographic evidence of early callus formation and no pain at the fracture site. This progression is slower than typical femoral fracture protocols.
-
PT Focus:
- Gradual increase in hip and knee ROM.
- Strengthening exercises for hip abductors, quadriceps, and hamstrings.
- Gait training with assistive devices, emphasizing proper biomechanics.
- Balance and proprioception exercises.
- Radiographic Follow-up: AP and lateral radiographs of the femur every 3-4 weeks to monitor fracture healing progress.
Intermediate Rehabilitation (Weeks 6-12)
- Weight-Bearing Progression: Progress to full weight-bearing as tolerated, only with clear radiographic evidence of significant callus formation and bridging, coupled with clinical signs of union (minimal pain, stable on single-leg stance).
-
PT Focus:
- Advanced strengthening exercises for the entire lower kinetic chain.
- Progression to more functional activities (stairs, uneven surfaces).
- Discontinuation of assistive devices when appropriate.
- Metabolic Follow-up: Regular endocrinology follow-up to monitor ALP, PLP, and PEA levels and titrate ERT as needed.
Long-Term Rehabilitation (>12 Weeks)
- Full Activity: Return to full activities, including sports, once radiographic union is complete and the patient has regained full strength and function. This can take significantly longer in HPP patients (often 6-12+ months) compared to standard femoral fractures.
- Monitoring: Continued long-term monitoring for potential refractures or non-union.
- Hardware Removal: Elective hardware removal is generally not recommended unless symptomatic, as the risk of refracture through screw holes or poor bone quality can be high. In patients with HPP, hardware is typically left in situ unless compelling reasons dictate removal.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- High Index of Suspicion: Always consider metabolic bone disease in patients presenting with atypical femoral fractures, especially with a history of recurrent low-energy fractures, stress fractures, or unusual dental history (premature tooth loss).
- Comprehensive Metabolic Workup: A low serum alkaline phosphatase is the cardinal sign for Hypophosphatasia. Always include serum ALP, PLP, and urine PEA in the workup for suspected metabolic bone disease, in addition to calcium, phosphate, PTH, and vitamin D. Do not assume normal ALP rules out all metabolic bone diseases.
- Pre-operative Optimization: Collaborate with endocrinology to consider initiating enzyme replacement therapy (asfotase alfa) for HPP patients. While not an acute "fix," it improves bone quality over time, potentially aiding long-term healing.
- Robust Fixation: A long cephalomedullary nail, spanning the entire length of the femur, is the preferred construct for atypical femoral fractures. This provides maximum stability and minimizes the risk of subsequent fracture propagation or refracture.
- Judicious Reaming: Over-reaming by 1.0-1.5 mm may be beneficial to reduce insertion forces and stress risers in compromised bone.
- Protected Weight-Bearing: Emphasize slow and protected weight-bearing progression. Bone healing in HPP is significantly delayed due to impaired mineralization. Aggressive weight-bearing can lead to hardware failure or non-union.
- Multidisciplinary Approach: Management of HPP requires a team approach involving orthopedic surgeons, endocrinologists, pain specialists, physical therapists, and potentially dentists.
Pitfalls
- Misdiagnosis: Overlooking Hypophosphatasia or other metabolic bone diseases. Assuming all atypical fractures are bisphosphonate-related without a thorough workup is a critical error.
- Inadequate Workup: Failing to perform a full metabolic bone panel, especially omitting serum ALP or its substrates (PLP, PEA), can lead to missed diagnoses and inappropriate treatment.
- Under-Fixation: Using shorter nails, non-locking plates, or less stable constructs in patients with compromised bone quality. This increases the risk of fixation failure, delayed union, or non-union.
- Aggressive Rehabilitation: Premature progression to full weight-bearing before radiographic evidence of robust callus formation can lead to hardware failure, loss of reduction, or refracture.
- Ignoring Systemic Disease: Focusing solely on the fracture without addressing the underlying Hypophosphatasia. This can lead to recurrent fractures or complications from the systemic disease.
- Lack of Long-Term Follow-up: HPP is a chronic condition. Long-term follow-up is essential to monitor bone healing, adjust ERT, and address potential long-term complications or new fractures.
- Hardware Removal Without Indication: Elective hardware removal in HPP patients can lead to refracture through previous screw holes due to poor bone quality and altered remodeling. It should generally be avoided unless symptoms are directly attributable to the implant.
