Management of Chronic Unreduced Hip Dislocations
Key Takeaway
Chronic unreduced hip dislocations present a formidable challenge in orthopedic surgery, characterized by severe soft-tissue contractures, acetabular fibrosis, and a high risk of osteonecrosis. Management depends on the direction of dislocation, chronicity, and femoral head viability. Techniques range from heavy skeletal traction for delayed posterior dislocations to intertrochanteric osteotomy as a temporizing measure for chronic anterior dislocations in young patients prior to definitive arthroplasty. This guide details evidence-based protocols for achieving concentric reduction and restoring biomechanical stability.
Introduction to Chronic Unreduced Hip Dislocations
Chronic, unreduced (old) dislocations of the hip are rare but devastating orthopedic presentations, most frequently encountered in developing nations, polytrauma patients with missed injuries, or individuals with delayed access to specialized surgical care. A hip dislocation is generally considered "chronic" or "neglected" when it remains unreduced for more than 3 to 4 weeks. Beyond this critical timeframe, profound pathoanatomic changes occur: the acetabulum fills with dense fibrous tissue, the joint capsule contracts and thickens, the surrounding musculature undergoes severe adaptive shortening, and the articular cartilage begins to degenerate.
Furthermore, the vascular supply to the femoral head—primarily the medial femoral circumflex artery (MFCA)—is severely compromised, leading to a high incidence of osteonecrosis (avascular necrosis, AVN). The management of these complex cases requires a highly individualized approach, balancing the patient's age, the viability of the femoral head, the direction of the dislocation, and the presence of associated acetabular or femoral head fractures.
Pathoanatomy and Biomechanics
Understanding the biomechanical alterations in chronic hip dislocations is paramount for successful surgical intervention.
In anterior dislocations, the femoral head is displaced anteriorly and inferiorly (obturator) or superiorly (pubic). The limb is typically locked in a position of severe external rotation, abduction, and flexion. Over time, the iliopsoas and adductor musculature contract rigidly, tethering the femur in this non-functional position.
In posterior dislocations, which are significantly more common, the femoral head rests on the ilium posterior to the acetabulum. The limb is held in internal rotation, adduction, and flexion. The massive gluteal muscles, short external rotators, and hamstrings undergo severe contracture. The acetabulum rapidly fills with a hypertrophic pulvinar, organized hematoma, and fibrous tissue, obliterating the socket and making closed reduction impossible after approximately 12 weeks.
Clinical Pearl: The primary obstacle to reduction in a chronic posterior dislocation is not merely the contracted musculature, but the dense fibrotic obliteration of the acetabular fossa and the contracture of the transverse acetabular ligament. Attempting forceful closed reduction in these cases without adequate skeletal traction or surgical release will inevitably result in iatrogenic femoral neck fracture or severe chondral shearing.
Chronic Anterior Dislocation of the Hip
Chronic anterior dislocations present a unique reconstructive challenge. When the dislocation has been present for more than 6 months, the articular cartilage is often irreparably damaged, and the femoral head may be entirely avascular. In young patients, definitive total hip arthroplasty (THA) may be undesirable due to the high risk of premature implant wear and the complexity of restoring the anatomic center of rotation in a chronically distorted pelvis.
In such scenarios, an intertrochanteric osteotomy serves as a highly effective temporizing procedure. The goal is not to reduce the joint, but to realign the mechanical axis of the lower extremity, correcting the severe external rotation and abduction deformity to allow for functional, plantigrade ambulation.
Indications for Intertrochanteric Osteotomy
The Aggarwal and Singh intertrochanteric osteotomy is specifically indicated for:
* Chronic anterior hip dislocations unreduced for 6 months or longer.
* Young, active patients where primary THA is contraindicated or ideally delayed.
* Severe, fixed rotational and angular deformities precluding ambulation.
* Cases where the femoral head is firmly ankylosed or stable in its ectopic anterior position, providing a fulcrum for weight-bearing.
Surgical Technique: Aggarwal and Singh
The objective of this procedure is to divide the proximal femur and reposition the distal segment into a neutral, functional alignment.
- Patient Positioning and Anesthesia: The patient is placed in the lateral decubitus position on a radiolucent operating table. General anesthesia with complete neuromuscular blockade is required.
- Surgical Approach: The Gibson posterolateral approach is utilized. An incision is made starting from the posterior superior iliac spine (PSIS), curving distally and anteriorly to the greater trochanter, and extending distally along the line of the femoral shaft.
- Deep Dissection: The interval between the gluteus maximus and gluteus medius is developed. The gluteus maximus is split in line with its fibers. This exposes the posterior aspect of the greater trochanter and the intertrochanteric region.
- Osteotomy Execution: The femur is exposed subperiosteally along the intertrochanteric line. Using an oscillating saw or osteotomes, the femur is divided precisely along the line joining the greater and lesser trochanters.
- Deformity Correction: Once the osteotomy is complete, the distal femoral segment is mobilized. The surgeon must systematically adduct, extend, and internally rotate the distal limb to correct the fixed anterior dislocation deformity. The limb is brought into neutral alignment (0 degrees of rotation, neutral abduction/adduction, and full extension).
- Fixation (Historical vs. Modern): While the original technique described by Aggarwal and Singh relied heavily on postoperative traction and casting for union, modern orthopedic principles strongly advocate for rigid internal fixation using a dynamic hip screw (DHS), blade plate, or proximal femoral locking plate to maintain the correction and allow for earlier mobilization.
Postoperative Protocol and Rehabilitation
If rigid internal fixation is not utilized, strict adherence to the historical postoperative protocol is mandatory to prevent the recurrence of the rotational deformity.
- Traction: The patient is placed in continuous skin traction for 6 weeks. This maintains the corrected alignment and prevents the powerful adductor and external rotator muscles from displacing the osteotomy.
- Casting Alternative: Hamada recommended immediate postoperative immobilization in a one and one-half spica cast. This cast must include the operative leg down to the toes and the contralateral normal leg down to the knee, locking the pelvis and preventing any rotational forces across the osteotomy site.
- Weight-Bearing: The patient is allowed to mobilize with crutches (non-weight-bearing) at 6 weeks post-surgery.
- Union: Clinical and radiographic union of the intertrochanteric osteotomy is typically complete within 3 to 4 months, at which point full weight-bearing is permitted.
Chronic Unreduced Posterior Dislocations
Unreduced posterior dislocations are significantly more common than their anterior counterparts. The prognosis and treatment algorithm are heavily dictated by the presence of associated fractures and the viability of the femoral head.
Diagnostic Workup and Imaging
Two critical factors contribute to poor outcomes in posterior dislocations:
1. Associated Fractures: Fractures of the femoral head (Pipkin classification) or the medial/posterior acetabular wall (Epstein Types II-V).
2. Osteonecrosis (AVN): An unpredictable and devastating complication resulting from the tearing or stretching of the MFCA.
Surgical Warning: Osteonecrosis may not become apparent on standard plain radiographs for many months following the injury. Relying solely on X-rays to determine femoral head viability in a chronic dislocation is a critical error.
While historical literature often omitted advanced imaging, modern orthopedic standards mandate the use of Magnetic Resonance Imaging (MRI) or a Technetium-99m bone scan prior to surgical intervention. These modalities are essential to detect the vascularity of the femoral head. In young patients, if the femoral head is deemed viable, every surgical effort must be exhausted to save it and achieve a concentric reduction.
Treatment Algorithm Based on Chronicity
Type I Posterior Dislocations (No fracture or minor rim fracture):
* Less than 12 weeks from injury: If the femoral head is viable, a closed reduction under general anesthesia with profound muscle relaxation should be attempted.
* More than 12 weeks from injury: The acetabulum is invariably filled with dense fibrous tissue. A concentric closed reduction is anatomically impossible. Attempting forceful closed reduction at this stage will fail and likely cause iatrogenic fractures. These patients require heavy skeletal traction followed by open reduction if traction fails.
Heavy Skeletal Traction Technique
For Type I posterior dislocations present for more than 12 weeks with a viable femoral head, the heavy skeletal traction technique described by Gupta and Shravat is the treatment of choice. This method utilizes sustained, massive force to overcome severe soft-tissue contractures, gradually pulling the femoral head distally and laterally until it can be levered back into the acetabulum.
Step-by-Step Protocol: Gupta and Shravat
- Pin Placement: Under local or regional anesthesia, a heavy threaded Steinmann pin or Denham pin is inserted into the proximal tibia, specifically in the region of the tibial tubercle, avoiding the proximal tibial physis (if open) and the joint capsule.
- Application of Massive Traction: The patient is placed supine in bed. An initial weight of 18 kg (approximately 40 lbs) of longitudinal skeletal traction is applied.
- Medical Management: The patient must be kept under continuous sedation and profound muscle relaxation during the initial days of this massive traction to tolerate the force and allow the contracted gluteal and pelvifemoral muscles to yield. Strict deep vein thrombosis (DVT) prophylaxis and meticulous skin care are mandatory.
- Radiographic Monitoring: Anteroposterior (AP) radiographs of the pelvis are obtained on alternate days to monitor the descent of the femoral head.

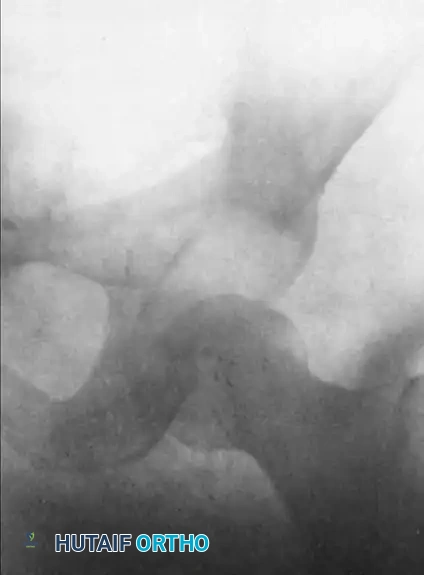
FIGURE 61-3 A: Anteroposterior radiograph of the left hip in a 27-year-old man, illustrating a chronic posterior dislocation with early myositis ossificans, presenting 37 days after the initial injury.
- Descent of the Femoral Head: Usually, by the fifth day of continuous 18 kg traction, the femoral head will have been pulled distally to a level at or slightly below the superior rim of the acetabulum.
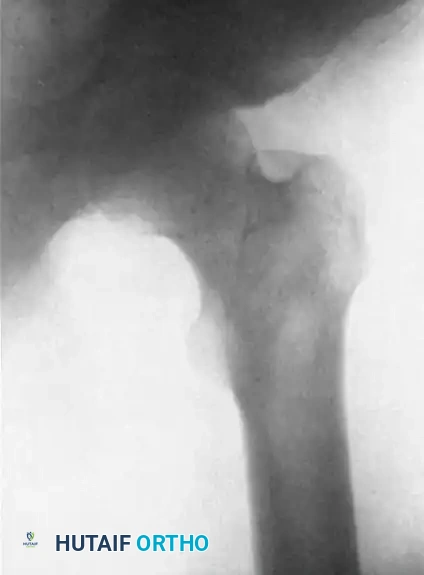
FIGURE 61-3 B: The same hip on the fifth day of heavy skeletal traction. The massive longitudinal force has successfully overcome the soft-tissue contractures, bringing the head of the femur partially below the level of the acetabular roof.
- Abduction and Weight Reduction: Once the head is at the level of the acetabulum, the limb is gradually abducted. This abduction uses the intact anterior capsule (iliofemoral ligament) as a hinge to lever the femoral head laterally and anteriorly over the posterior rim of the acetabulum. Simultaneously, the traction weight is reduced by 3.6 kg every fourth day to prevent over-distraction of the joint.
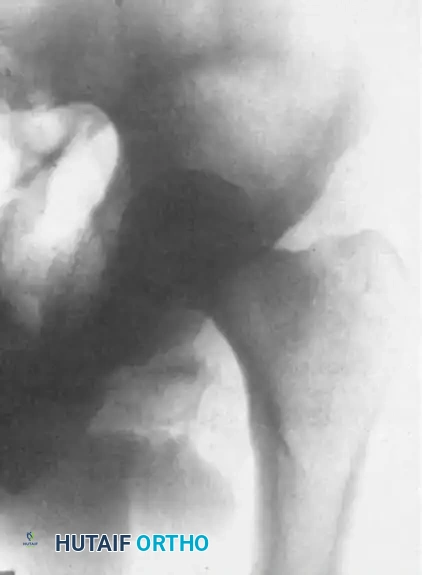
FIGURE 61-3 C: The same hip on the 17th day. The extremity is now in abduction with reduced traction, demonstrating a successful concentric reduction of the femoral head into the acetabulum.
- Maintenance Phase: Once a concentric reduction is confirmed radiographically, the traction is reduced to a maintenance weight of 7 kg. This is maintained for the next 2 weeks to allow the posterior capsule to heal and the joint to stabilize.
- Rehabilitation: After 2 weeks of maintenance traction, the tibial pin is removed. The patient begins active, non-weight-bearing range-of-motion exercises in bed for the next 4 weeks. Strict non-weight-bearing status is enforced for a total of 3 months to protect the vulnerable articular cartilage and allow for revascularization.
Open Reduction for Chronic Posterior Dislocations
The ultimate success of the heavy traction technique relies entirely on achieving a concentric reduction. If the post-traction radiographs reveal an eccentric or widened joint space, it indicates that interposed soft tissue (inverted limbus, capsule, piriformis tendon) or osteochondral fragments are blocking the joint.
In these cases, or in cases of Type II (large uncomminuted posterior wall fracture) and Type III (comminuted posterior wall fracture) dislocations, an immediate open reduction is indicated.
Surgical Approach and Acetabular Preparation
- Approach: The Kocher-Langenbeck posterior approach is the gold standard for accessing the posterior hip and acetabulum. The patient is placed in the lateral decubitus position.
- Sciatic Nerve Protection: The sciatic nerve is frequently encased in dense scar tissue or draped over the dislocated femoral head. Meticulous neurolysis is the first critical step. The nerve must be identified proximally at the sciatic notch and traced distally, protecting it throughout the procedure.
- Joint Exposure: The short external rotators (if still intact) are tagged and released. The posterior capsule, which is often thickened and contracted, is incised.
- Acetabular Débridement: This is the most crucial step of the open reduction. The surgeon must meticulously clear the acetabular fossa. The hypertrophic pulvinar, organized hematoma, and any fibrous tissue must be excised using rongeurs and curettes. The transverse acetabular ligament is often contracted and may need to be released to allow the femoral head to seat deeply into the socket.
- Reduction: Once the acetabulum is completely clear, longitudinal traction is applied to the femur, combined with gentle internal and external rotation, to guide the femoral head back into the concentric socket.
- Fracture Management: If a Type II or III posterior wall fracture is present, the fragments are mobilized, the joint is irrigated to remove loose bodies, and the posterior wall is anatomically reduced and fixed using a reconstruction plate and lag screws.
Pitfall: Avoid excessive force during open reduction. If the head does not reduce smoothly, re-evaluate the acetabulum for residual fibrous tissue or an inverted labrum. Forcing the reduction can cause devastating iatrogenic cartilage damage or femoral neck fracture.
Complications and Salvage Procedures
The management of chronic hip dislocations is fraught with high complication rates, even in the hands of experienced surgeons.
- Osteonecrosis (AVN): The most common long-term complication. If AVN progresses to subchondral collapse, the patient will develop severe secondary osteoarthritis.
- Post-Traumatic Arthritis: Resulting from the initial chondral insult or prolonged joint incongruity.
- Heterotopic Ossification (HO): Highly prevalent following extensive surgical releases around the hip. Prophylaxis with Indomethacin or localized radiation therapy should be strongly considered postoperatively.
- Sciatic Nerve Palsy: Can occur from the initial trauma, the massive traction forces, or iatrogenic injury during open reduction.
Salvage Options:
In cases where the femoral head is dead (AVN), the articular cartilage is destroyed, or concentric reduction is impossible, joint preservation is no longer viable. In older patients, definitive Total Hip Arthroplasty (THA) is the procedure of choice, though it carries a higher risk of instability and requires complex soft-tissue balancing. In very young, heavy laborers with unilateral disease and profound destruction, a Hip Arthrodesis may still be considered to provide a stable, painless limb, though its use is increasingly rare in modern practice.
===
You Might Also Like
