Comprehensive Management of Humeral Nonunions and Prosthetic Reconstruction
Key Takeaway
This comprehensive guide details the surgical management of complex humeral nonunions and proximal humeral prosthetic reconstruction. It provides step-by-step protocols for open reduction, intramedullary nailing, compression plating, and fibular strut grafting. Designed for orthopedic surgeons, it emphasizes biomechanical principles, precise surgical approaches, and evidence-based biological augmentation to optimize functional recovery in challenging upper extremity nonunions.
Introduction to Humeral Reconstruction
The surgical management of humeral nonunions and the execution of proximal humeral prosthetic reconstruction represent significant challenges in orthopedic trauma and reconstructive surgery. Successful outcomes demand a profound understanding of upper extremity biomechanics, meticulous soft tissue handling, and the strategic application of osteosynthesis principles. This comprehensive guide expands upon established operative techniques, detailing the step-by-step execution of open reduction and prosthetic insertion, the biological and mechanical management of diaphyseal nonunions, and the nuanced salvage of complex condylar nonunions.
Open Reduction and Insertion of a Proximal Humeral Prosthesis
Prosthetic replacement of the proximal humerus is primarily indicated for severe fracture-dislocations, head-splitting fractures, or established nonunions of the surgical neck where the articular segment is devascularized or mechanically unviable. The primary goals are pain relief and the restoration of a stable fulcrum to allow deltoid and rotator cuff function.
Surgical Approach and Preparation
Optimal visualization is paramount. The procedure is typically performed with the patient in the beach-chair position, allowing full mobility of the arm and access to the shoulder girdle.
- Incision and Exposure: Expose the shoulder through an extended deltopectoral (anterior) approach or the anterolateral (Henry) approach. The deltopectoral interval is preferred as it preserves the anterior deltoid origin and minimizes the risk of axillary nerve injury.
- Debridement: Identify the fracture site and meticulously remove all interposed fibrous tissue and hematoma from the fracture surface of the humeral shaft fragment. Freshen the cortical edges to healthy, bleeding bone to promote subsequent tuberosity healing.
🔪 Surgical Technique: Articular Fragment Extraction
Extracting a devascularized or impacted humeral head fragment can be technically demanding. A highly effective technique involves inserting a Knowles pin or a threaded half-pin directly into the articular fragment. This pin serves as a "joystick" to manipulate and extract the head without causing further iatrogenic comminution to the surrounding tuberosities.
Prosthetic Preparation and Implantation
Once the head is extracted, it can be used as a template to size the prosthesis and harvest cancellous autograft.
- Canal Preparation: Sequentially ream and broach the humeral canal. Make a hole through the center of the extracted head fragment large enough to accommodate the stem of the trial prosthesis if a custom or biological reconstruction is being attempted, though modern modular prostheses have largely replaced this historical technique.
- Tuberosity Management: If the greater and lesser tuberosities are separate fragments, pass heavy, nonabsorbable sutures (e.g., #5 braided polyester or high-strength polyethylene) through the tendon-bone interface. These sutures must be passed through the appropriate medial and lateral fin holes in the prosthesis prior to final seating.
- Version Control: Seat the definitive prosthesis in the humeral canal in approximately 30 to 35 degrees of retroversion. This is clinically referenced by aligning the fin of the prosthesis posterior to the bicipital groove, or by referencing the forearm (flexed to 90 degrees) and dialing the implant 35 degrees posterior to the axis of the forearm.
- Impaction and Fixation: Pass the stem into the canal and impact the prosthesis firmly. Tie the previously passed nonabsorbable sutures securely, reducing the tuberosities anatomically around the prosthetic neck to restore the rotator cuff force couples.
- Closure: Close the incision in layers with interrupted sutures, ensuring meticulous repair of the deltopectoral fascia.
Postoperative Care
Postoperative rehabilitation is identical to standard proximal humeral arthroplasty protocols. The shoulder is immobilized in a sling for 4 to 6 weeks to protect the tuberosity repair. Passive range of motion (ROM) begins early, progressing to active-assisted ROM at 6 weeks, and strengthening at 10 to 12 weeks once radiographic tuberosity healing is confirmed.
Management of Humeral Shaft Nonunions
Humeral shaft nonunions occur in up to 10% of diaphyseal fractures, often secondary to inadequate immobilization, soft tissue interposition, or compromised biology. Treatment requires a dual approach: maximizing mechanical stability and optimizing the biological environment.
Biological Augmentation and Fixation Strategies
When the fracture site is opened for open reduction, the addition of bone graft is highly recommended to stimulate osteogenesis.
- Autograft vs. Allograft: Iliac crest bone graft (ICBG) remains the gold standard due to its osteogenic, osteoinductive, and osteoconductive properties. However, morselized allograft has been found to perform comparably to ICBG in achieving union for midshaft humeral nonunions when combined with rigid intramedullary nailing and interfragmentary wire placement.
- Advanced Biological Adjuncts: Multiple modalities used simultaneously provide the highest union rates for recalcitrant nonunions. Neel advocated for a comprehensive "belt and suspenders" approach: utilizing a broad dynamic compression plate (DCP), an implantable electrical bone stimulator, and a composite bone graft substitute consisting of calcium sulfate, crushed cancellous bone chips, and demineralized bone matrix (DBM) (e.g., AlloMatrix).
- Structural Augmentation: Van Houwelingen and McKee successfully described the use of lateral compression plating combined with an allograft cortical strut placed medially. This strut not only provides medial column support but also enhances screw purchase in osteoporotic bone. This construct is often augmented with ICBG or recombinant human bone morphogenetic protein (rhBMP-7).
Plate Osteosynthesis
Compression plating remains the workhorse for humeral nonunions, particularly those with angular deformity or atrophic characteristics.

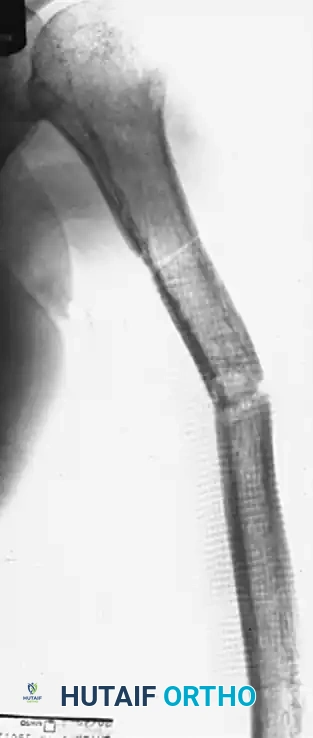
FIGURE 59-30 A: Nonunion of the middle third of the humeral shaft demonstrating significant angulation and regional osteoporosis.
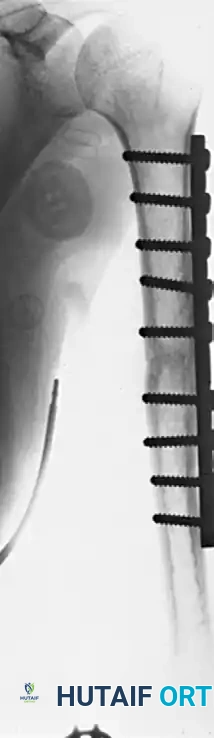
FIGURE 59-30 B: Solid union achieved 5 months after open reduction, rigid fixation with a nine-hole broad compression plate, and the application of autologous iliac bone grafts.
Intramedullary Nailing
While plating is standard, intramedullary (IM) nailing is highly effective, particularly for segmental nonunions or pathological fractures. Locked IM nails provide load-sharing biomechanics and allow for early mobilization.

FIGURE 59-31 A: Preoperative radiograph of a recalcitrant humeral diaphyseal nonunion.
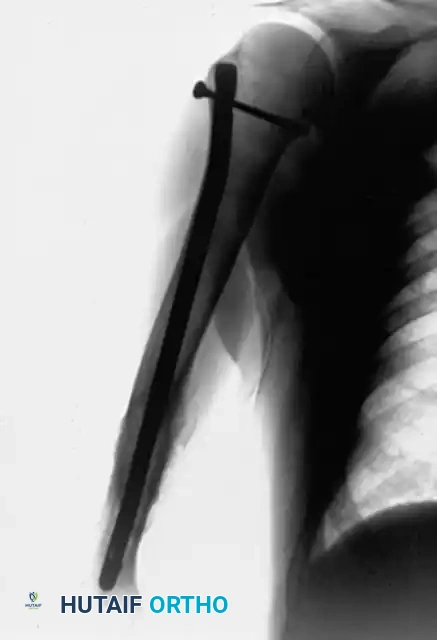
FIGURE 59-31 B: Postoperative radiograph demonstrating successful stabilization and healing after fixation with a locked intramedullary nail.
Management of Segmental Bone Defects
Bridging a massive bone defect is less frequently required in the humerus compared to the lower extremity. The upper extremity tolerates shortening exceptionally well.
💡 Clinical Pearl: Humeral Shortening
When a defect occurs, the fragments can often be apposed and grafted directly. Shortening of 4 to 5 cm causes minimal functional disability. The cosmetic alteration is generally of little consequence compared to the high complication rates associated with complex defect-bridging procedures.
Gap nonunions of the humeral shaft are thus more easily managed than those in weight-bearing bones. The sclerotic ends of the fragments are freshened, apposed, and stabilized with a compression plate, while the surrounding area is packed with cancellous and corticocancellous grafts.
Fibular Strut Grafting for Massive Defects
When preserving the exact length of the humerus is absolutely necessary (e.g., defects >5 cm), the defect can be bridged with a structural autograft or allograft. A whole fibular transplant is the procedure of choice for massive intercalary defects.
- Technique: The distal end of the fibular transplant is applied to the humeral condyle that retains the longest metaphyseal segment (preferably the lateral column). The distal fragment must be large enough to engage at least two cortical screws. The normal metaphyseal expansion is then restored by packing the junctions with cancellous iliac bone.
- Postoperative Protection: Extreme care must be taken to avoid disrupting the repair during wound closure and the application of a postoperative cast or abduction humeral brace.
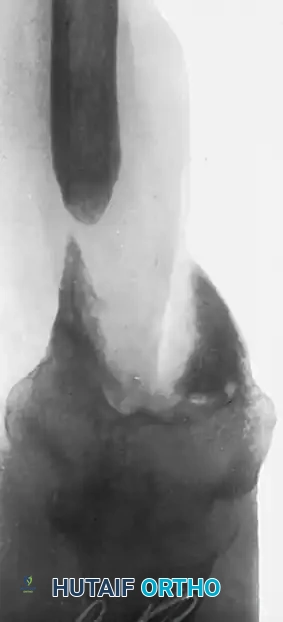
FIGURE 59-32 A: Large defect in the distal metaphysis of the humerus following an open fracture with the extrusion of a large segment of bone.
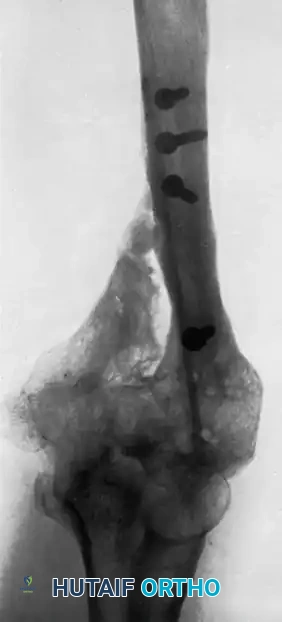
FIGURE 59-32 B: Radiographic appearance 20 months after bridging the massive defect with a whole fibular transplant.
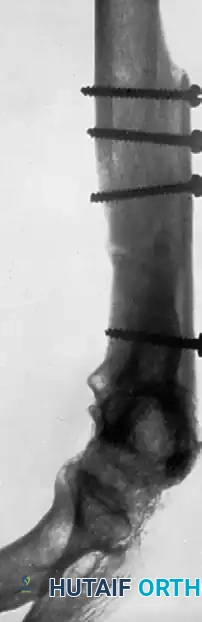
FIGURE 59-32 C: Cancellous bone was utilized to bridge the expanded portion of the metaphysis and shaft, resulting in robust incorporation.
Alternatively, the Ilizarov method of internal bone transport (distraction osteogenesis) can be utilized for humeral nonunions complicated by massive bone loss or active infection.
Management of Condylar and Epicondylar Nonunions
Nonunions of the distal humerus present unique challenges due to the complex articular anatomy and the proximity of critical neurovascular structures, particularly the ulnar nerve.
Medial Epicondyle Nonunions
Nonunion of the medial humeral epicondyle frequently occurs following the nonoperative treatment of acute pediatric fractures.
- Clinical Presentation: Although the fracture surfaces may be widely separated radiographically, a strong fibrous union typically joins the small fragment to the medial condyle. Function is usually near-normal.
- Surgical Indications: Intervention is rarely required unless the patient develops symptomatic ulnar neuritis or severe valgus instability.
- Surgical Technique: Attempting to achieve bony union between the epicondyle and the condyle in chronic cases is generally futile and unnecessary. The definitive procedure involves freeing the ulnar nerve and performing an anterior transposition. The ununited bone fragment is excised from the common flexor-pronator origin. The flexor muscles are then advanced and reattached directly to the medial condyle using heavy nonabsorbable sutures through drill holes.
Lateral Condyle Nonunions
Disability from nonunion in the condylar area is most frequently caused by the nonunion of a lateral condyle fracture sustained in childhood (Milch classification). If these acute pediatric fractures are not perfectly reduced and immobilized, nonunion, progressive cubitus valgus deformity, and tardy ulnar nerve palsy may ensue.
Pediatric Considerations
In children, surgery for an established, late nonunion is rarely indicated. Symptoms are often minimal, and aggressive attempts to freshen and appose the fragments frequently fail, potentially leading to avascular necrosis of the condyle or premature physeal closure.
- Exception: Early nonunion of the lateral humeral condyle where the fragment remains in acceptable alignment and the physis is open. Flynn, Richards, and Saltzman recommend in situ fixation using a screw and peg bone graft placed proximal to the physis, disturbing the surrounding soft tissues as little as possible.
- Toh et al. recommend early intervention for nonunions of Milch Type I fractures before skeletal maturity to prevent pain, instability, and tardy ulnar nerve palsy. Conversely, Milch Type II nonunions often present with less severe functional deficits and may not require further surgical intervention.
Adult Reconstruction
In adults, if the elbow is asymptomatic, no treatment is indicated other than anterior transposition of the ulnar nerve if tardy ulnar neuritis develops. However, if the joint is painful and grossly unstable, reconstructive surgery is justified. While stability and strength can be restored, patients must be counseled that elbow motion is usually permanently decreased following reconstruction.
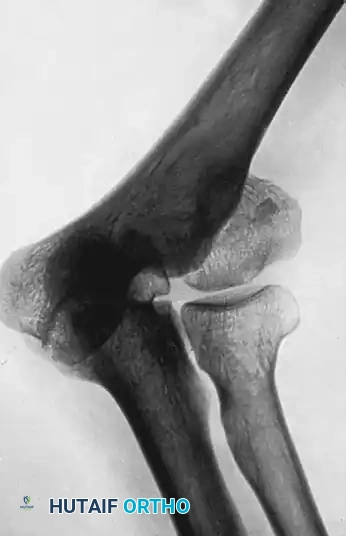
FIGURE 59-33 A: Old fracture of the lateral condyle of the humerus sustained in childhood, demonstrating marked cubitus valgus and established nonunion.

FIGURE 59-33 B: Radiograph taken immediately after complex intra-articular reconstruction and osteosynthesis.
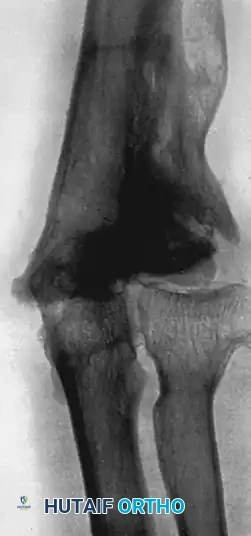
FIGURE 59-33 C: Follow-up at 12 months. A functional range of flexion and extension is restored, with a normal carrying angle and fair stability, despite expected degenerative changes.
Total Elbow Arthroplasty (TEA) as a Salvage Procedure
For elderly patients with complex, un-reconstructible distal humeral nonunions, Total Elbow Arthroplasty (linked semi-constrained prosthesis) serves as an excellent salvage option.
⚠️ Surgical Warning: TEA Indications and Limitations
TEA yields the best outcomes when strictly reserved for patients older than 65 years who have pre-existing arthritic changes, severely compromised bone stock precluding internal fixation, and low functional demands on the upper extremity. Active infection is an absolute contraindication.
Postoperative Restrictions: Patients must strictly adhere to lifetime lifting restrictions to prevent aseptic loosening or catastrophic implant failure. This includes the avoidance of repetitive lifting of 2 lbs (0.9 kg) or more, and a strict one-time lifting limit of 10 lbs (4.5 kg).
Conclusion
The surgical management of humeral nonunions and the execution of prosthetic reconstruction require a highly individualized approach. Whether employing a Knowles pin for articular extraction during arthroplasty, utilizing dual-plate constructs with rhBMP-7 for diaphyseal nonunions, or executing a massive fibular strut graft for segmental defects, the surgeon must balance mechanical stability with biological optimization. Strict adherence to these evidence-based principles ensures the highest probability of restoring anatomy, alleviating pain, and maximizing upper extremity function.
You Might Also Like


