Anatomy and physiology of the peripheral nervous system (PNS)
-
- Neuron (see Fig. 1.49)
- Cell body (metabolic center; 10% of size of a neuron)
- Tapers into axon at axon hillock
- Axons: one or more processes that connect the neuron to the spinal cord or end-organ
- Dendrites: processes extending from the cell body that receive signals from surrounding nerve cells
- Myelin sheath
- Neurophysiology
- Composed primarily of galactocerebroside
-
Speeds wave propagation or conduction (thicker sheath increases conduction speed)
- Produced by Schwann cells in PNS
- Schwann cells originate in neural crest and are important in posttraumatic nerve regeneration.
- Produce nerve growth factor-β, brain-derived growth factor, insulin-like growth factor 1 (IGF-1), and erythropoietin
- One Schwann cell surrounds a single axon in myelinated fibers
- Footprint of approximately 100 µm
-
Space between cells is called node of
Ranvier (concentrated Na+ channels) - Allows for salutatory conduction between nodes of Ranvier
- One Schwann cell surrounds multiple axons in unmyelinated fibers
- Axolemma
- Specialized membrane that surrounds axon and maintains membrane potential
- Maintains resting potential utilizing Na-K pumps
- Approximately −70 mV (cell interior has relative negative charge)
- Action potential (AP)
-
Neurotransmitters cross synapse and trigger
opening of Na+ channel. -
This triggers voltage-gated Na + channels (responsible for generation of AP) in axon hillock when membrane potential increases to −50 mV.
- Membrane potential spikes to 30 mV as membrane depolarizes.
-
Potential propagates down axon and triggers
voltage-gated Ca2+ channel at axon terminus. - Ca2+ enters axon and triggers neurotransmitter release
- Voltage-gated K+ channels stay open longer than Na+ channels.
- Leads to hyperpolarization (−75 mV)
- Peripheral nerves
- Propagation faster in myelinated and larger nerves
- Absolute refractory period
- Period when voltage-gated Na+ channels cannot be activated
- Responsible for antegrade propagation of signal
- Relative refractory period
- Period when larger than normal stimuli propagate a second AP
- Result of the hyperpolarization phase of the previous
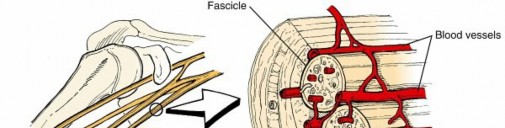
- Highly organized structures composed of nerve fibers, blood vessels, and connective tissues ( Fig. 1.46)
- Nerve fibers vary in size according to function ( Table 1.27).
- Erlanger and Gasser classification
- Afferent and efferent nerves
-
Uses Roman and Greek letters




FIG. 1.46 Nerve architecture. From Brinker MR, Miller MD: Fundamentals of orthopaedics, Philadelphia, 1999, Saunders, p 13.
Table 1.27 Types and Characteristics of Nerve Fibers Type | Diameter (mm) | Myelination | Speed | Examples | ---|---|---|---|---| A | 10–20
| Heavy
| Fast
| Touch B | <3
| Intermediate
| Medium
| Autonomic nervous system C | <1.3
| None
| Slow
| Pain
4. Lloyd and Hunt classification
1. Only afferent nerves
2. Uses Roman numerals
5. Can be composed of one fascicle (monofascicular), a few fascicles (oligofascicular), or several fascicles (polyfascicular)
6. Axons coated with a fibrous tissue called endoneurium
7. Groups of axons (fascicles) covered by perineurium
8. Nerve covered by epineurium
1. External epineurium is continuous with dural sleeve of spinal cord.
9. Afferent nerves convey information from sensory organ to CNS.
1. Pseudounipolar neuron with cell body in dorsal root ganglia (DRG)
2. Central branch extends away from neuron and travels through spinal cord via dorsal horn.
10. Efferent nerves convey information from CNS to periphery.
1. Unipolar neuron with cell body in ventral horn of spinal cord
2. Motor unit: an α-motoneuron and the muscle fibers it innervates
11. Internal topography
1. Cross section of nerve changes along length of nerve (divisions, anastomosis, and migration)
2. Fibers within fascicle organized by locations they innervate.
3. Around joints, nerves typically have more and smaller fascicles to accommodate joint motion and decrease risk of injury.
1. Radial nerve at spiral groove has fewer and larger fascicles (higher risk of neurapraxia with humeral fracture)
1.
Sensory receptors (
Table 1.28)
1. The four attributes of a stimulus are quality, intensity, duration, and location.
Receptor Type Fiber Type Quality
---
Nociceptors
Mechanical
| Aδ
| Sharp, pricking pain
Thermal and mechanothermal
| Aγ
| Sharp, pricking pain
Thermal and mechanothermal
| C
| Slow, burning pain
Polymodal
| C
| Slow, burning pain
Cutaneous and Subcutaneous Mechanoreceptors
Meissner corpuscle
| Aβ
| Touch
Pacini corpuscle
| Aβ
| Flutter
Ruffini corpuscle
| Aβ
| Vibration
Merkel receptor
| Aβ
| Steady skin indentation
Hair-guard, tylotrich hair
| Aβ
| Steady skin indentation
Hair down
| Aβ
| Flutter
Muscle and Skeletal Mechanoreceptors
Muscle spindle, primary
| Aα
| Limb proprioception
Muscle spindle, secondary
| Aβ
| Limb proprioception
Golgi tendon organ
| Aα
| Limb proprioception
Joint capsule mechanoreceptor
| Aβ
| Limb proprioception
Table 1.28 Receptor Types
Adapted from Kandel ER et al, editors: Principles of neural science, ed 3, Norwalk, CT, 1991, Appleton & Lange, p 342.
Table 1.29 Summary of Spinal Reflexes Segmental Receptor Organ Afferent Fiber Reflex --- Phasic stretch reflex | Muscle spindle (primary endings)
| Type Ia (large myelinated) Tonic stretch reflex | Muscle spindle (secondary endings)
| Type II (intermediate myelinated) Clasp-knife response | Muscle spindle (secondary endings)
| Type II (intermediate myelinated) Flexion withdrawal reflex | Nociceptors (free nerve endings), touch and pressure receptors
| Flexor-reflex afferents: small unmyelinated cutaneous afferents (Aδ, C, and muscle afferent fibers, group III) Autogenic inhibition
| Golgi tendon organ
| Type Ib (large myelinated)
From Simon SR, editor:
Orthopaedic basic science,
Rosemont, IL, 1994, American Academy of Orthopaedic Surgeons, p 350.
2. Modalities
1. Nociceptors (pain and temperature)
2. Cutaneous and subcutaneous mechanoreceptors (touch and vibration)
3. Muscle and skeletal mechanoreceptors (proprioception)
2.
Spinal cord reflexes (
Table 1.29)
1. These reflexes are “stereotyped responses” to a specific sensory stimulus.
2. A reflex pathway involves a sensory organ (receptor), an interneuron, and a motoneuron.
3. Monosynaptic reflex: only one synapse is involved between receptor and effector.
4. Polysynaptic reflex: one or more interneurons are involved. Most reflexes are polysynaptic.
1. #### Intervertebral discs (IVDs)
1. Allow spinal motion and stability
2. Also function as cushioning for axial loads on the spine
3. Two components
1. Central nucleus pulposus
1. #### Derived from notochord
2. Hydrated gel with compressibility
3. Low collagen (type II)/high proteoglycan (and
glycosaminoglycan) content
4. #### Proteoglycans make up higher percentage of dry weight.
5. #### With time, the nucleus pulposus undergoes loss of proteoglycans and water (desiccation).
2. Surrounding annulus fibrosis
1. #### Derived from mesoderm
2. Extensibility and increased tensile strength
3. High collagen (type I)/low proteoglycan content
4. Proteoglycans make up lower percentage of dry weight.
5. Superficial layer contains nerve fibers.
4. Composition:
1. Water (85%)
2. Proteoglycans
3. Type II collagen (20% of dry weight) in the nucleus pulposus
4. Type I collagen (60% of dry weight) in the annulus fibrosis
5. Neurovascularity
1. Dorsal root ganglion gives rise to the sinuvertebral nerve, which then innervates the superficial fibers of the annulus.
2. #### Avascular—nutrients and fluid diffuse from the vertebral end plates. This diffusion is impaired by calcification with aging.
6. Aging disc
1. Early degenerative disc disease is an irreversible process, with IL-1β stimulating the release of MMPs, nitric oxide, IL-6, and prostaglandin E2 (PGE2).
2. Decreased water content and conversion to fibrocartilage
1. #### A result of decreased hydrostatic pressure due to fewer large proteoglycans (aggrecan)
3. #### Fibronectin cleavage or fragmentation is also associated with degeneration.
4. Increase in keratan sulfate concentration and decrease in chondroitin sulfate
5. Increase in relative collagen concentration, with no change in absolute quantity