INTRODUCTION TO PROXIMAL FIFTH METATARSAL FRACTURES
Fractures of the proximal fifth metatarsal represent a significant proportion of foot and ankle trauma encountered in orthopaedic practice. A great deal of academic and clinical attention has been directed toward the treatment of these injuries due to their notoriously unpredictable healing rates. The primary culprit for this delayed healing or nonunion is the unique vascular anatomy of the fifth metatarsal, which features a critical "watershed" area of diminished blood supply at the metaphyseal-diaphyseal junction.
Historically described by Sir Robert Jones in 1902 after he sustained the injury while dancing, the "Jones fracture" has since become a catch-all term often incorrectly applied to all proximal fifth metatarsal fractures. Modern orthopaedic practice demands a rigorous, anatomically precise classification system to dictate appropriate conservative or surgical management.
VASCULAR ANATOMY AND BIOMECHANICS
Understanding the vascularity and biomechanical forces acting on the fifth metatarsal is paramount for the treating surgeon.
The Watershed Blood Supply
The blood supply to the fifth metatarsal is derived from three primary sources:
1. The Nutrient Artery: Enters the medial aspect of the middle third of the diaphysis and provides intramedullary blood flow directed proximally.
2. Metaphyseal Arteries: Enter the base of the metatarsal, supplying the tuberosity and the proximal articular surfaces.
3. Periosteal Network: Supplies the outer cortical bone.
The metaphyseal-diaphyseal junction relies on a tenuous anastomotic network between the proximally directed intramedullary supply and the distally directed metaphyseal supply. This creates a relative avascular "watershed" zone. Fractures in this region disrupt the intraosseous blood supply, leaving the fracture site dependent on the limited periosteal network, thereby significantly increasing the risk of delayed union and nonunion.
Biomechanical Forces
The proximal fifth metatarsal is subjected to immense bending moments during the gait cycle, particularly during heel rise and toe-off. Furthermore, it serves as the attachment site for critical tendinous and ligamentous structures:
* Peroneus Brevis Tendon: Inserts onto the dorsolateral tuberosity, exerting a strong eversion force.
* Lateral Band of the Plantar Fascia: Inserts onto the plantar aspect of the tuberosity, resisting arch collapse.
* Peroneus Tertius: Inserts dorsally on the metaphysis.
Clinical Pearl: The competing forces of the peroneus brevis and the lateral band of the plantar fascia create a dynamic distraction force across proximal fifth metatarsal fractures, further complicating the healing process in an already vascularly compromised zone.
ANATOMICAL CLASSIFICATION: THE THREE ZONES
To standardize treatment and predict outcomes, fractures of the proximal fifth metatarsal are divided into three distinct anatomical zones, originally popularized by Lawrence and Botte.
Zone I: Tuberosity Avulsion Fractures
Zone I is the most proximal zone. It includes the metatarsocuboid articulation but remains strictly proximal to the fourth and fifth intermetatarsal articulation.
* Mechanism of Injury: Typically an avulsion-type injury secondary to acute hindfoot inversion with the foot in plantarflexion. The fracture is propagated by the sudden tension of the lateral band of the plantar fascia and the peroneus brevis tendon.
* Clinical Presentation: Often referred to as a "pseudo-Jones" or "tennis" fracture.
Zone II: The True Jones Fracture
Zone II extends from the distal extent of Zone I to the metaphyseal-diaphyseal junction. Crucially, this zone includes the articulation between the fourth and fifth metatarsals.
* Mechanism of Injury: Usually the result of a strong adduction force applied to the forefoot while the ankle is plantarflexed, causing a severe bending moment at the metaphyseal-diaphyseal junction.
* Clinical Significance: This is the area of the true Jones fracture and lies directly within the watershed vascular zone.
Zone III: Diaphyseal Stress Fractures
Zone III encompasses the proximal 1.5 cm of the diaphysis, extending distally from the fourth and fifth intermetatarsal articulation.
* Mechanism of Injury: This is the classic location for stress fractures, typically occurring in athletes due to repetitive microtrauma and cyclical loading.
* Clinical Nuance: Recent literature and specific outcome studies suggest that the clinical distinction between Zone II and Zone III fractures may be largely academic, as the treatment algorithms and functional outcomes are virtually identical in both groups.
Torg Classification for Zone III Stress Fractures
To further guide the management of Zone III injuries, the Torg classification is utilized based on radiographic appearance:
* Type I (Acute): Early stress fracture with no intramedullary sclerosis. Radiolucent line with sharp margins.
* Type II (Delayed Union): Widening of the fracture line, evidence of periosteal reaction, and early intramedullary sclerosis.
* Type III (Nonunion): Complete obliteration of the medullary canal by sclerotic bone, blunted fracture edges, and a wide fracture gap.
CLINICAL EVALUATION AND RADIOGRAPHIC IMAGING
Patients typically present with lateral foot pain, swelling, and difficulty weight-bearing. Point tenderness over the base of the fifth metatarsal is the hallmark physical finding.
Radiographic Series
A standard three-view radiographic series of the foot is mandatory for accurate zone classification.
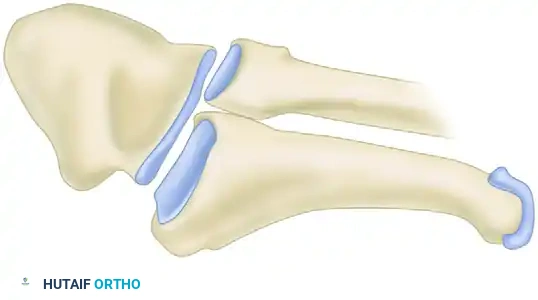
Anteroposterior (AP) radiograph demonstrating the overall alignment and medial cortical integrity of the fifth metatarsal.
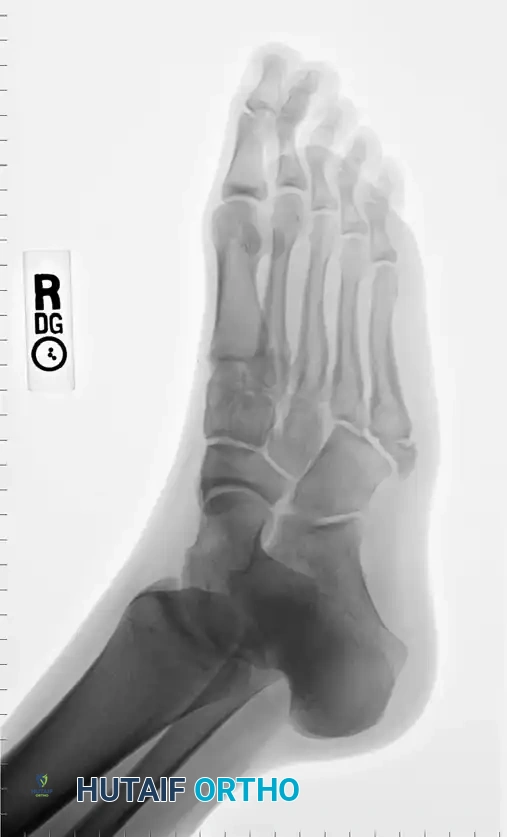
Oblique radiograph, which is often the most sensitive view for identifying non-displaced Zone II and Zone III fractures, as it profiles the fourth and fifth intermetatarsal articulation.
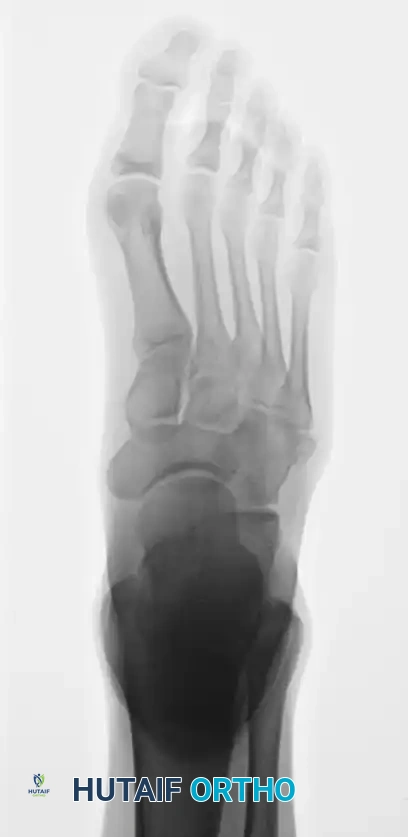
Lateral radiograph, essential for assessing plantar gapping and the sagittal alignment of the metatarsal shaft.
NON-OPERATIVE MANAGEMENT
Zone I Fractures
Fractures in Zone I generally heal predictably and are treated satisfactorily with conservative measures. Depending on the patient's symptom severity, treatment consists of a rigid postoperative shoe, a controlled ankle motion (CAM) walking boot, or a short-leg walking cast.
* Healing Timeline: In comprehensive studies of proximal fifth metatarsal tuberosity fractures, clinical and radiographic union is typically achieved in all patients at an average of 44 days, with virtually no fractures requiring longer than 65 days to heal.
* Complications: Although nonunions of Zone I fractures can occur, they are rarely painful. If a symptomatic nonunion persists, it can be definitively treated with simple excision of the avulsed fragment and reattachment of the peroneus brevis.
Zone II and Zone III Fractures (Non-Athlete)
Acute, non-displaced Zone II and Torg Type I Zone III fractures in sedentary or non-athletic individuals can be managed non-operatively. This requires strict non-weight-bearing in a short-leg cast for 6 to 8 weeks. However, patients must be counseled on the high risk of delayed union (up to 30-40%) and the potential need for delayed surgical intervention.
SURGICAL MANAGEMENT: INDICATIONS AND TECHNIQUES
Surgical intervention is increasingly favored to minimize the risk of nonunion, expedite return to play, and restore normal biomechanics.
Surgical Indications
- Displaced Zone I Fractures: Intra-articular displacement > 2mm involving the cuboid articulation.
- Acute Zone II/III Fractures in Athletes: High-demand patients require rigid fixation to prevent deconditioning and ensure rapid return to sport.
- Torg Type II and III Fractures: Delayed unions and nonunions require surgical debridement, fixation, and often bone grafting.
- Failed Conservative Management: Persistent pain and radiographic nonunion after 8-12 weeks of immobilization.
Intramedullary Screw Fixation (The Gold Standard)
Intramedullary screw fixation is the workhorse procedure for Zone II and Zone III fractures. It provides rigid biomechanical stability, compressing the fracture site while acting as an internal splint.
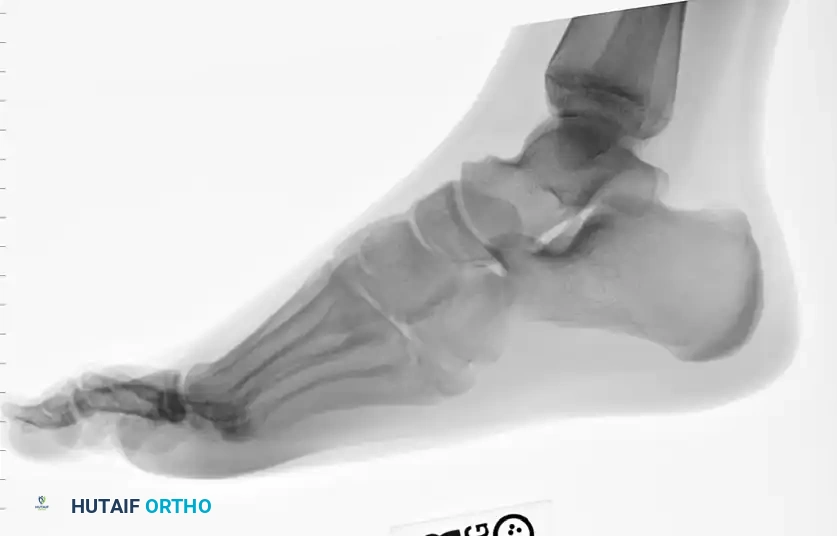
Diagrammatic representation of the surgical approach and anatomical considerations for intramedullary fixation.
1. Preoperative Planning
Careful templating on AP and lateral radiographs is required to determine the appropriate screw diameter and length. The screw must be robust enough to withstand bending forces (typically 4.5 mm to 5.5 mm) and long enough to bypass the fracture site so that all threads engage the dense diaphyseal bone distal to the fracture.
2. Patient Positioning
The patient is placed in the lateral decubitus position or supine with a large bump under the ipsilateral hip to internally rotate the leg. A radiolucent table is utilized, and the fluoroscopy C-arm is brought in from the contralateral side. A thigh tourniquet is applied.
3. Surgical Approach and Nerve Protection
A 2 to 3 cm longitudinal incision is made slightly dorsal to the lateral border of the plantar skin, directly over the base of the fifth metatarsal.
Surgical Warning: A great deal of attention must be directed toward the dorsolateral cutaneous branch of the sural nerve. Sufficient exposure must be obtained to identify and protect this cutaneous nerve branch, which frequently crosses directly over the surgical field. Neuroma formation in this area is highly symptomatic and difficult to treat.
4. Guidewire Placement
The peroneus brevis tendon is identified and retracted plantarly. The starting point for the guidewire is critical. It must be placed "high and tight"—slightly dorsal and medial on the tuberosity.
* Pitfall: If the starting point is too lateral or plantar, the straight guidewire will impinge on the medial cortex of the curved metatarsal shaft, leading to medial cortex blowout or fracture distraction during screw insertion.
5. Drilling and Tapping
Under fluoroscopic guidance, the guidewire is advanced down the medullary canal, ensuring it remains centralized on both AP and lateral views. A cannulated drill is used to open the proximal cortex. Depending on the density of the bone and the specific screw system (solid vs. cannulated), tapping the canal may be necessary to prevent iatrogenic comminution.
6. Screw Insertion
A partially threaded cancellous or specific Jones fracture screw is inserted. The threads must completely bypass the fracture line to achieve interfragmentary compression. The screw head should be countersunk slightly into the tuberosity to prevent prominent hardware irritation beneath the skin.
7. Management of Sclerosis (Torg Type II/III)
If operating on a delayed union or nonunion, passing a drill or curette across the fracture site to break up the sclerotic medullary bone is mandatory to re-establish the intramedullary blood supply. In recalcitrant Torg Type III nonunions, an open approach with autologous bone grafting (e.g., calcaneal autograft) may be required in conjunction with screw fixation.
POSTOPERATIVE PROTOCOL AND REHABILITATION
The postoperative rehabilitation protocol must balance the need for fracture protection with the desire for early mobilization.
- Phase I (Weeks 0-2): The patient is placed in a bulky Jones dressing and a posterior splint. Strict non-weight-bearing (NWB) is enforced. Elevation and ice are prioritized to control edema.
- Phase II (Weeks 2-6): Sutures are removed at 14 days. The patient is transitioned to a CAM walking boot. Weight-bearing status depends on the fracture type and fixation rigidity. For acute fractures with excellent compression, progressive partial weight-bearing may be initiated. For nonunions or revision surgeries, NWB is maintained for up to 6 weeks.
- Phase III (Weeks 6-10): Radiographs are obtained to assess bridging callus and obliteration of the fracture line. Once clinical and radiographic union is progressing, the patient transitions to a stiff-soled shoe with a custom orthotic. Physical therapy focuses on peroneal strengthening, proprioception, and Achilles stretching.
- Return to Sport: Athletes may begin sport-specific drills once they are pain-free with single-leg hopping and demonstrate complete radiographic union (typically 8-12 weeks). The use of a turf toe plate or custom orthotic is recommended for the first season back to play to reduce bending moments across the metatarsal.
COMPLICATIONS
- Delayed Union / Nonunion: The most common complication, particularly if conservative management is chosen for Zone II/III injuries, or if the intramedullary screw is too small in diameter, allowing micromotion.
- Sural Nerve Injury: Iatrogenic injury during the surgical approach can lead to painful neuromas or lateral foot numbness. Meticulous blunt dissection is required.
- Hardware Prominence: A screw head that is not adequately countersunk can cause severe pain with footwear, necessitating hardware removal after fracture consolidation.
- Refracture: Premature return to sport or removal of the intramedullary screw before complete cortical remodeling significantly increases the risk of refracture. Screws should generally be left in situ permanently unless symptomatic.
CONCLUSION
Fractures of the proximal fifth metatarsal demand a high level of clinical acumen. By accurately differentiating between Zone I tuberosity avulsions, Zone II Jones fractures, and Zone III diaphyseal stress fractures, the orthopaedic surgeon can implement the most effective, evidence-based treatment strategy. While conservative management remains highly successful for Zone I injuries, the precarious watershed blood supply of Zones II and III often necessitates precise intramedullary screw fixation to ensure reliable union and optimal functional recovery.
