Patient Presentation & History
A 42-year-old male, previously fit and active with no significant medical comorbidities, presented to the emergency department following a high-energy industrial crush injury involving a large press. The mechanism involved the right lower extremity being trapped for approximately 45 minutes. Pre-hospital care included initial hemorrhage control with direct pressure and tourniquet application, intravenous access, and fluid resuscitation.
Upon arrival, the patient was hemodynamically stable after initial resuscitation, though tachycardic at 110 bpm, with a blood pressure of 105/60 mmHg. He reported severe pain localized to his right lower leg. There was no history of alcohol or recreational drug use. His tetanus status was up-to-date. Social history was pertinent for a physically demanding occupation as a heavy machine operator.
Clinical Examination
Primary Survey (ATLS Protocol):
*
Airway:
Patent, protected.
*
Breathing:
Spontaneous, symmetrical chest rise, clear breath sounds bilaterally.
*
Circulation:
Tachycardic (110 bpm), BP 105/60 mmHg, Capillary Refill Time (CRT) <2 seconds centrally. Tourniquet in place on the right thigh. Radial pulses palpable bilaterally.
*
Disability:
GCS 15. Pupils equal, round, reactive to light.
*
Exposure:
Full body examination revealed no other significant injuries apart from the right lower extremity. Patient was warm and covered.
Secondary Survey - Right Lower Extremity:
*
Inspection:
Grossly deformed right lower leg with extensive soft tissue avulsion, degloving injuries, and exposed bone fragments. A large open wound was noted circumferentially around the mid-shaft tibia and fibula. Significant muscle crush and contamination with grease and debris were evident. The foot appeared mottled and cool distally to the ankle. The tourniquet was removed transiently to assess for active bleeding, revealing brisk arterial bleeding from multiple small vessels, necessitating reapplication and conversion to a more proximal pneumatic tourniquet in the operating room. There was obvious shortening and external rotation of the distal limb segment. Compartment swelling was significant in the proximal leg, even with obvious open wounds distally.
*
Palpation:
Intense tenderness over the entire mid-to-distal tibia and fibula. Absence of palpable dorsalis pedis and posterior tibial pulses. Significant crepitus was elicited with gentle manipulation.
*
Range of Motion:
Grossly unstable tibia and fibula. Ankle and foot range of motion could not be assessed due to pain and instability.
*
Neurological Assessment:
*
Motor:
No voluntary movement of the ankle or toes.
*
Sensory:
Anaesthesia in the distribution of the common peroneal nerve (dorsum of foot, lateral leg) and superficial peroneal nerve. Hypoesthesia in the distribution of the tibial nerve (plantar aspect of foot). Deep peroneal nerve sensation (1st web space) was absent.
*
Vascular Assessment:
Absent dorsalis pedis and posterior tibial pulses on palpation. Doppler signal confirmed absence of flow in both vessels. Ankle-Brachial Index (ABI) could not be reliably obtained due to the extent of injury. The foot was cool, pale, and mottled, indicating critical ischemia.
*
Soft Tissue Assessment (Gustilo-Anderson Classification):
Initial assessment suggested a Gustilo-Anderson Type IIIC open fracture of the tibia and fibula with extensive soft tissue loss, gross contamination, neurovascular compromise, and significant muscle crush.
Imaging & Diagnostics
Immediate imaging focused on defining the skeletal injury and assessing for other concurrent trauma.
-
Plain Radiographs (Right Tibia/Fibula AP and Lateral):
- Demonstrated a comminuted, segmental open fracture of the mid-diaphyseal tibia, extending proximally into the metaphysis, with significant bone loss and displacement.
- Associated comminuted fractures of the fibula at multiple levels, suggestive of high-energy impact.
- Substantial soft tissue swelling and gas tracking were noted, consistent with the clinical findings of an open injury and contamination.
- Critical finding: Significant shortening and angular deformity, indicative of substantial skeletal instability and likely compromise of surrounding neurovascular structures.
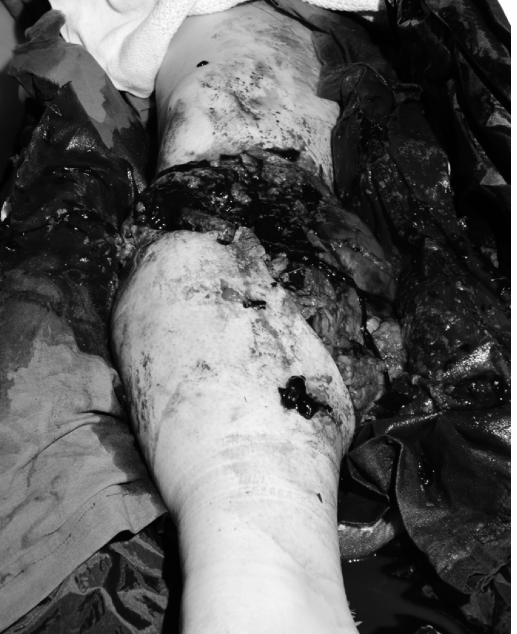
(Illustrative example of severe open tibia/fibula fracture with significant bone and soft tissue damage requiring immediate surgical attention.) -
Computed Tomography (CT) Angiography of the Right Lower Extremity:
- Performed urgently due to absent distal pulses and clinical suspicion of vascular injury.
- Revealed complete transection of the posterior tibial artery and significant intimal disruption and thrombosis of the anterior tibial artery at the level of the fracture.
- The peroneal artery appeared patent but was assessed to be insufficient for sole revascularization given the extent of muscle injury and the patient's age.
- Confirmed the multi-fragmentary nature of the tibial and fibular fractures and quantified the bone defect size.
- Provided detailed assessment of surrounding soft tissue planes, identifying areas of hematoma and potential devitalized muscle, aiding in surgical planning for debridement.
- No acute intracranial or thoracoabdominal injuries were identified on concurrent trauma CT scans (head, C-spine, chest, abdomen/pelvis).
-
Laboratory Investigations:
- Complete Blood Count: Hb 10.2 g/dL (post-resuscitation), WBC 16.5 x 10^9/L (stress leukocytosis).
- Coagulation Profile: PT/INR, aPTT within normal limits.
- Metabolic Panel: Electrolytes, renal function within normal limits. Lactate 3.8 mmol/L, indicating ongoing tissue hypoperfusion.
- Blood Gas Analysis: pH 7.32, PaCO2 40 mmHg, HCO3 20 mEq/L, BE -5, consistent with mild metabolic acidosis.
- Type and Crossmatch: 6 units PRBCs, 4 units FFP, 1 unit platelets.
Differential Diagnosis
The initial presentation of severe lower extremity trauma necessitates rapid differentiation and concurrent management of life-threatening and limb-threatening conditions. While the ultimate diagnosis was a Gustilo IIIC mangled extremity, the immediate differential included:
| Feature | Mangled Extremity (Case Presentation) | Severe Open Tibia/Fibula Fracture (Gustilo IIIB) | Isolated Critical Limb Ischemia with Fracture | Acute Compartment Syndrome (ACS) with Fracture |
|---|---|---|---|---|
| Mechanism | High-energy crush, avulsion, degloving. | High-energy, direct trauma (e.g., MVC, fall). | Variable, often minor trauma, or pre-existing vascular disease. | High-energy trauma, often closed or minimally open fracture. |
| Vascular Status | Absent pulses, Doppler loss, critical ischemia (definitive injury). | Pulses present but potentially diminished, or transiently absent then reperfused; may evolve. | Absent pulses, Doppler loss, critical ischemia (primary insult). | Pulses often present early; arterial flow compromised by rising compartment pressure. |
| Neurological Status | Gross motor/sensory deficit (definitive injury). | Variable, often nerve contusion or stretch, rarely transection initially. | Variable, may have sensory deficit if nerve ischemia occurs. | Progressive motor weakness, sensory deficits (late finding). |
| Soft Tissue Injury | Extensive avulsion, degloving, contamination, muscle crush. | Extensive soft tissue loss, wound >10cm, periosteal stripping, bone exposure. | Minor superficial wounds, or no open wound; deep tissue injury minimal. | Skin often intact or small laceration; tense, swollen compartment. |
| Skeletal Injury | Highly comminuted, segmental, bone loss, gross instability. | Comminuted, significant displacement, but potentially less bone loss. | Simple or comminuted fracture, often less displacement. | Fracture (often tibia) is common associated injury. |
| Prognosis for Limb Salvage | Guarded to poor, high amputation rate. | Challenging, but generally better than mangled extremity if vascular intact. | Highly dependent on revascularization success. | Excellent if early fasciotomy; poor if delayed. |
| Initial Management Priority | Hemorrhage control, provisional stabilization, vascular assessment/repair. | Hemorrhage control, provisional stabilization, urgent debridement. | Revascularization, often before fracture fixation. | Emergent fasciotomy. |
| Key Discriminator | Concomitant severe skeletal, soft tissue, vascular, and nerve injury. | Severe soft tissue and bone injury without primary critical vascular/nerve transection. | Primary vascular injury without extensive soft tissue/nerve or bone loss. | Tense compartment, pain out of proportion, pain with passive stretch. |
Surgical Decision Making & Classification
The decision-making process for a mangled extremity is complex, often requiring a multidisciplinary approach involving Orthopedic Trauma, Vascular Surgery, Plastic Surgery, and Anesthesiology. The primary goal is often limb salvage, but this must be balanced against the potential for prolonged morbidity, functional limitations, and an ultimately inferior outcome compared to primary amputation.
Mangled Extremity Severity Score (MESS):
The MESS score, while widely used, has limitations and should not be the sole determinant. Our patient's injury characteristics would yield a high MESS score:
*
Skeletal/Soft-Tissue Injury:
High-energy (3 points - crush)
*
Limb Ischemia:
>6 hours, complete ischemia (4 points - absent pulses after initial 6hr mark)
*
Shock:
Systolic BP <90 mmHg (1 point - transiently below 90 mmHg on arrival)
*
Age:
42 years (<30 years = 0 points, 30-50 years = 1 point, >50 years = 2 points)
*
Total MESS Score:
3 + 4 + 1 + 1 = 9 points.
A MESS score of ≥7 is classically associated with a high likelihood of amputation. However, it's crucial to acknowledge that MESS is a predictor, not a definitive rule. Factors such as warm ischemia time, extent of muscle crush, and reconstructive capabilities often outweigh the absolute score.
Rationale for Operative Salvage (Initial Decision):
Despite the high MESS score and significant vascular injury, several factors initially favored an attempt at limb salvage:
1.
Patient Age and Pre-injury Functional Status:
A relatively young, active patient with no comorbidities.
2.
Unilateral Injury:
No other major limb injuries, allowing full focus on this extremity.
3.
Potential for Functional Recovery:
While challenging, the goal was to achieve a functional limb superior to a prosthesis, considering advanced reconstructive options.
4.
Availability of Multidisciplinary Team:
Immediate access to specialized vascular and plastic surgery teams.
5.
Patient Preference:
The patient, once stable and after comprehensive discussion, expressed a strong desire to attempt salvage.
Indications for Primary Amputation (Considered and Discussed):
Primary amputation is typically indicated when:
* Irreversible limb ischemia (e.g., >6-8 hours of complete warm ischemia).
* Complete transection of the tibial nerve or significant irreparable nerve damage at multiple levels with predicted poor functional outcome.
* Massive bone loss >6-8 cm, especially in critical weight-bearing segments, coupled with extensive soft tissue damage and vascular injury.
* Uncontrolled hemorrhage requiring ongoing critical care support.
* Severe muscle crush, predicting a high risk of systemic complications (rhabdomyolysis, renal failure).
* Patient factors: Moribund patient, severe polytrauma, limited reconstructive options, patient refusal for prolonged, complex reconstruction.
In this case, while the vascular injury was severe and warm ischemia time approaching the critical threshold, the perceived potential for viable muscle, relatively contained bone loss (despite being segmental), and the patient's strong motivation led to the decision for an initial attempt at salvage. This approach aligns with the principle of Damage Control Orthopedics (DCO).
Damage Control Orthopedics (DCO) Principles Applied:
1.
Life Before Limb:
Initial focus on ATLS, hemodynamic stability, and hemorrhage control.
2.
Rapid Provisional Stabilization:
Application of an external fixator to the tibia and fibula to restore length, align the limb, and protect the soft tissues and neurovascular repairs. This reduces pain, blood loss, and prevents further injury.
3.
Expeditious Debridement and Lavage:
Urgent debridement of all devitalized tissue and thorough irrigation to reduce bacterial load.
4.
Early Vascular Repair:
Prompt revascularization is paramount to prevent irreversible ischemia and muscle necrosis.
5.
Staged Reconstruction:
Recognition that definitive fixation and soft tissue coverage would be staged procedures after the initial life- and limb-saving interventions.
Surgical Technique / Intervention
The patient was taken to the operating theatre within 90 minutes of arrival.
1. Resuscitation and Anaesthesia:
* Continuous hemodynamic monitoring, large-bore IV access, arterial line insertion.
* General anaesthesia with close collaboration between anaesthesia and surgical teams given potential for significant blood loss and fluid shifts during tourniquet release and vascular repair.
* Foley catheter inserted for urine output monitoring.
* Prophylactic broad-spectrum antibiotics (e.g., Cefazolin and Gentamicin) administered pre-incision.
2. Initial Debridement, Lavage, and Fasciotomies:
* A high thigh pneumatic tourniquet was applied but not inflated initially.
* The limb was meticulously debrided. All devitalized skin, subcutaneous tissue, muscle (identifiable by loss of contractility, dark color, and lack of bleeding), and contaminated bone fragments were excised. This was a radical debridement, recognizing the need to remove all non-viable tissue.
* A total of 8 liters of sterile saline solution was used for pulse lavage at low pressure.
* Full-length four-compartment fasciotomies (anterior, lateral, deep posterior, superficial posterior) were performed in the leg. Given the extensive soft tissue damage and crush component, even with an open fracture, there was significant swelling and risk of compartment syndrome once reperfusion was established. These were performed through two separate incisions: an anterolateral incision for the anterior and lateral compartments, and a posteromedial incision for the deep and superficial posterior compartments.
3. Provisional Skeletal Stabilization (External Fixation):
* Following debridement, a multiplanar external fixator (e.g., Orthofix, Stryker Hoffman 3) was applied to the tibia and fibula.
* Proximal pins were inserted into the tibia (medial, anteromedial) and distal pins into the talus or calcaneus. For a segmental tibia fracture, pins were placed proximal and distal to the fracture zone, sometimes spanning the knee or ankle joint for additional stability, depending on the fracture extension.
* The frame was constructed to restore length and alignment, providing stability for the subsequent vascular repair. This significantly reduced stress on the vascular anastomoses.
* The fibula fracture was not directly addressed in this initial phase beyond debridement and external fixation of the tibia.
4. Vascular Reconstruction:
* Vascular surgery team performed the reconstruction under microscope guidance.
* The transected posterior tibial artery and the severely damaged anterior tibial artery were exposed.
* Given the significant contusion and intimal damage to the anterior tibial artery, it was deemed irreparable in its current state. The decision was made to reconstruct the posterior tibial artery, which was transected cleanly, and address the anterior tibial flow via runoff from the posterior tibial artery and the peroneal artery.
* An interposition saphenous vein graft (harvested from the contralateral leg by a second team concurrently) was used to repair the posterior tibial artery, after appropriate debridement of damaged vessel ends.
* An end-to-end anastomosis was performed using 7-0 Prolene sutures.
* Completion angiogram confirmed patency of the graft and good distal runoff into the foot, with collateral supply to the anterior compartment via the peroneal artery.
* The tourniquet was then released. Close monitoring for reperfusion injury, swelling, and bleeding was maintained.
5. Nerve Exploration and Repair:
* The common peroneal nerve was found to be in continuity but severely contused and avulsed from surrounding tissue, indicating a stretch injury. No direct transection was observed.
* The tibial nerve was also contused but grossly intact.
* No primary neurorrhaphy was performed in this acute, contaminated setting. The nerves were protected within the wound bed. A delayed repair or grafting procedure would be considered in a clean secondary setting if function did not recover.
6. Wound Management and Temporary Closure:
* After vascular repair and nerve protection, the extensive soft tissue defects remained.
* The wound was thoroughly re-irrigated.
* A negative pressure wound therapy (NPWT) system (e.g., VAC therapy) was applied over sterile sponges. This helps manage exudate, reduce edema, and promote granulation tissue formation, while awaiting definitive soft tissue coverage.
* The leg was gently wrapped in sterile dressings.
7. Post-Operative Management (Acute Phase):
* Transferred to ICU for close monitoring.
* Systemic anticoagulation (e.g., IV Heparin followed by LMWH) initiated immediately post-operatively to maintain vascular graft patency, once hemostasis was secured.
* Continued broad-spectrum antibiotics.
* Aggressive fluid management to prevent reperfusion injury and acute kidney injury.
* Pain control with patient-controlled analgesia (PCA).
* Limb elevated to reduce swelling.
* Daily clinical assessment of the limb for viability, swelling, infection, and neurovascular status.
* Second look surgery within 24-48 hours for further debridement and assessment of tissue viability, wound bed preparation.
8. Subsequent Staged Reconstructions:
*
Second Look Surgery (Day 2):
Extensive re-debridement of residual devitalized muscle and soft tissue. The vascular graft was patent, and the limb showed improved perfusion. NPWT was reapplied.
*
Definitive Skeletal Fixation (Day 5 - after first clean debridement and stable wound):
* Once the wound was clean and viable, and the patient was medically stable, the external fixator was revised. Given the bone loss and comminution, an intramedullary nail (IMN) was chosen for definitive fixation of the tibia, to allow for earlier weight bearing and potentially better functional outcome than plates in this context.
* The IMN was inserted after careful reaming and alignment. The fibula was left to heal with the tibia stabilized.
* The bone defect was initially managed with bone graft substitutes and careful alignment. A delayed bone grafting procedure (e.g., cancellous autograft from iliac crest or fibular osteocutaneous flap) would be considered after soft tissue coverage was secure.
*
Soft Tissue Coverage (Day 7 - after definitive fixation and pristine wound bed):
* Following multiple debridements and a healthy, granulating wound bed, the plastic surgery team performed a large free anterolateral thigh (ALT) flap to cover the extensive soft tissue defect over the tibia. Microvascular anastomoses were performed to the posterior tibial artery and concomitant veins distal to the original repair site. This provided well-vascularized tissue for coverage and future bone grafting.
* The fasciotomy wounds were closed secondarily after adequate skin coverage was achieved.
Post-Operative Protocol & Rehabilitation
Phase 1: Acute Post-Operative (Weeks 0-4)
*
ICU/Ward Care:
Continuous monitoring of flap viability (clinical checks, Doppler signals), neurovascular status of the foot, and signs of infection.
*
Anticoagulation:
Continued for vascular graft and flap patency (e.g., aspirin 81mg, LMWH then potentially warfarin in select cases).
*
Antibiotics:
Tailored based on intraoperative cultures, typically 48-72 hours post-definitive closure, or longer if significant contamination/infection suspected.
*
Pain Management:
Multimodal approach (opioids, NSAIDs, regional blocks) to facilitate early mobilization.
*
Edema Control:
Limb elevation, gentle compression where appropriate, monitoring for compartment issues.
*
Early Mobilization:
As soon as pain allows, gentle active and passive range of motion (ROM) of knee and ankle (if IMN allows), non-weight bearing ambulation with crutches/walker, transfers. No weight-bearing on the affected limb.
*
Wound Care:
Meticulous flap care, monitoring for hematoma, seroma, infection.
*
Psychological Support:
Early engagement with psychology services for trauma and adjustment to potential long-term disability.
Phase 2: Subacute Rehabilitation (Weeks 4-12)
*
Fracture Healing:
Regular radiographic assessment of fracture union.
*
Weight Bearing:
Gradual progression to protected weight-bearing (e.g., 25% to 50% body weight) in a boot or brace, depending on IMN stability, callus formation, and soft tissue healing. Full weight-bearing allowed only upon radiological signs of union.
*
Range of Motion:
Aggressive physical therapy to regain full knee and ankle ROM. Scar massage and desensitization for flap and wound areas.
*
Strengthening:
Progressive strengthening exercises for all lower extremity muscle groups, especially quadriceps, hamstrings, and hip abductors. Isometric exercises initially, then isotonic.
*
Gait Training:
Focus on proper gait mechanics, balance, and proprioception.
*
Bone Grafting:
If significant bone defect or delayed union, secondary bone grafting (autograft or allograft) considered, typically 3-6 months post-injury, once soft tissues are quiescent.
Phase 3: Long-Term Rehabilitation and Functional Restoration (Months 3-12+)
*
Full Weight-Bearing:
Once fracture union is confirmed radiologically and clinically.
*
Advanced Strengthening:
Plyometric exercises, sport-specific training (if applicable), occupational therapy for return to work.
*
Endurance Training:
Cardiovascular fitness.
*
Neuro-rehabilitation:
Continued focus on nerve recovery, if any, with serial EMG/NCS if indicated. Addressing neuropathic pain.
*
Adaptive Equipment:
Assessment for orthoses or specialized footwear to compensate for residual deficits (e.g., ankle-foot orthosis for foot drop).
*
Addressing Complications:
Vigilant monitoring for nonunion, malunion, chronic osteomyelitis, hardware failure, flap failure, chronic pain, heterotopic ossification, and complex regional pain syndrome (CRPS). Surgical intervention for these complications as needed.
*
Psychosocial Reintegration:
Ongoing psychological support, vocational counseling.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Multidisciplinary Approach is Paramount: A "Mangled Extremity Team" (Orthopedics, Vascular, Plastics, Anesthesia, Critical Care) should be activated immediately.
-
Time is Tissue:
- Warm Ischemia Time: <6 hours is critical for muscle viability. Aim for revascularization within this window.
- Early Debridement: Aggressive, radical debridement of all devitalized tissue is crucial to prevent infection and promote healing. Often requires serial debridements ("second look").
- Damage Control Orthopedics (DCO): Provisional external fixation stabilizes the limb, controls hemorrhage, reduces pain, and allows for rapid transfer to vascular/plastic surgery without protracted definitive bone fixation.
- Vascular First (after stability): Re-establishing blood flow is the highest priority after life-threatening issues are addressed and provisional stabilization achieved. Prioritize reconstruction of dominant vessels. Consider shunting in highly unstable patients or prolonged transfers.
- Soft Tissue Coverage is Key: Early, adequate soft tissue coverage with well-vascularized tissue (local or free flaps) is essential for preventing infection, promoting bone healing, and facilitating rehabilitation. NPWT is an invaluable temporizing measure.
- Nerve Assessment & Protection: Meticulous documentation of pre-op neurological status. Protect exposed nerves. Primary repair is rarely indicated in the acute, contaminated setting; delayed repair or grafting is preferred if spontaneous recovery does not occur.
- Antibiotic Prophylaxis: High-dose, broad-spectrum IV antibiotics initiated early and continued as per protocol, adjusted based on culture results.
- Nutritional Support: Crucial for wound healing and overall recovery in these hypermetabolic patients.
- Patient Expectations & Psychological Support: Realistic discussions about the long and arduous recovery, potential for residual deficits, and the possibility of delayed amputation. Early psychological intervention.
- Vigilance for Complications: High index of suspicion for compartment syndrome, infection, vascular thrombosis, nonunion, and CRPS.
Pitfalls:
- Missed or Delayed Diagnosis of Vascular Injury: Leads to irreversible ischemia and potentially primary amputation or systemic complications. Relying solely on palpable pulses is insufficient; Doppler and ABI are essential.
- Inadequate Debridement: Retention of devitalized tissue is a prime cause of deep infection (osteomyelitis), flap failure, and nonunion.
- Premature Definitive Fixation/Closure: Trying to "finish" the case in a single setting before the wound is clean, and soft tissue coverage is secure. This almost invariably leads to disaster.
- Failure to Perform Fasciotomies: Even with open fractures, crush injuries can lead to significant swelling and compartment syndrome, particularly after reperfusion.
- Poor Surgical Planning/Lack of Multidisciplinary Team: Attempting complex salvage without adequate resources or coordinated subspecialty input.
- Ignoring Systemic Factors: Neglecting resuscitation, coagulopathy, nutrition, or infection control can doom a technically successful salvage.
- Ignoring Patient Factors: Attempting salvage in an elderly, frail, or highly comorbid patient, or one with limited social support, can lead to prolonged suffering and eventual amputation.
- Inadequate Rehabilitation: A technically successful salvage without comprehensive and prolonged rehabilitation will result in a poor functional outcome.
- Underestimating the Risk of Amputation: Despite best efforts, a significant percentage of mangled extremities will still require delayed amputation due to complications. This needs to be communicated honestly to the patient.
- Choosing the Wrong Fixation: While IMN is preferred for tibial diaphysis, in a highly unstable, contaminated, or bone-loss scenario, an external fixator may be the only initial viable option, sometimes remaining definitive. Plates may increase soft tissue stripping and infection risk.
