INTRODUCTION TO ISOLATED MALLEOLAR FRACTURES
The ankle joint is a highly congruent, inherently stable hinge joint (ginglymus) whose biomechanical integrity relies on the precise anatomical relationship between the talus, the distal tibia (plafond and medial malleolus), and the distal fibula (lateral malleolus). Isolated fractures of the medial or lateral malleoli represent a significant portion of orthopedic trauma. While they may appear deceptively simple on initial radiographic evaluation, these injuries demand rigorous assessment to rule out occult ligamentous instability—particularly of the deltoid ligament and the distal tibiofibular syndesmosis.
Failure to recognize instability or achieve anatomical reduction can lead to altered joint kinematics. Classic biomechanical studies have demonstrated that a mere 1 mm of lateral talar shift can decrease tibiotalar contact area by up to 42%, exponentially increasing peak contact stresses and predisposing the patient to rapid post-traumatic osteoarthritis.
ISOLATED FRACTURES OF THE MEDIAL MALLEOLUS
The medial malleolus serves as the primary medial buttress of the ankle mortise and the origin of the robust deltoid ligament complex. Isolated fractures here are relatively uncommon compared to lateral malleolar fractures and often result from supination-external rotation or pronation-abduction mechanisms.
Indications for Nonoperative Management
Nondisplaced fractures of the medial malleolus can usually be treated successfully with cast immobilization. Studies by Herscovici et al. have demonstrated a high rate of union and excellent functional outcomes with conservative management of truly isolated, nondisplaced medial malleolar fractures.
Avulsion fractures involving only the very tip of the medial malleolus (superficial deltoid avulsions) are generally not as unstable as fractures involving the axilla of the mortise. These tip avulsions do not routinely require internal fixation unless the displacement is significant or there is concomitant lateral-sided instability.
Indications for Operative Management
Operative intervention is indicated for:
* Displaced Fractures: Any displacement greater than 2 mm, as persistent displacement allows the talus to tilt into varus, disrupting the congruency of the mortise.
* High-Demand Patients: In athletes or individuals with high functional demands, internal fixation may be appropriate even for minimally displaced fractures to hasten healing, allow early range of motion, and accelerate rehabilitation.
* Fractures Involving the Axilla: Fractures extending into the corner (axilla) of the tibial plafond inherently destabilize the medial mortise and require anatomical reduction.
* Delayed Fixation: Can be performed if conservative management fails or if symptoms warrant intervention later in the clinical course.
Clinical Pearl: Always assess the integrity of the lateral structures when evaluating a seemingly "isolated" medial malleolus fracture. An isolated medial malleolus fracture with a widened syndesmosis or lateral talar shift indicates a Maisonneuve-type injury or a highly unstable variant requiring comprehensive stabilization.
Surgical Technique: Medial Malleolus ORIF
Positioning and Approach
- Positioning: The patient is placed supine on a radiolucent operating table. A bump may be placed under the ipsilateral hip to correct natural external rotation of the lower extremity, bringing the foot into a neutral position. A thigh tourniquet is applied.
- Incision: A longitudinal or slightly curvilinear incision is made centered over the medial malleolus, curving slightly anteriorly at its distal extent.
- Dissection: Careful subcutaneous dissection is performed to protect the great saphenous vein and the saphenous nerve, which typically run anterior to the medial malleolus.
- Exposure: The fracture site is exposed. The periosteum should not be excessively stripped, but the fracture edges must be clearly visualized. Often, a fold of periosteum or a fragment of the deltoid ligament is interposed in the fracture site, preventing closed reduction. This must be meticulously cleared using a curette or dental pick.
Reduction and Fixation
- Reduction: The fracture is anatomically reduced using a pointed reduction clamp. One tine is placed on the distal tip of the malleolus and the other on the intact medial tibial metaphysis.
- Provisional Fixation: Two 1.25-mm or 1.6-mm Kirschner wires (K-wires) are driven from the tip of the medial malleolus, perpendicular to the fracture plane, into the distal tibia.
- Radiographic Confirmation: Fluoroscopy is used to confirm anatomical reduction of the articular surface and appropriate trajectory of the K-wires.
- Definitive Fixation:
- Traditional Construct: Fixation usually consists of two 4.0-mm partially threaded cancellous lag screws. The K-wires are overdrilled with a 2.5-mm drill bit, tapped (if non-self-tapping screws are used), and the screws are inserted.
- Alternative Construct: Some authors advocate for fixation using bicortical 3.5-mm fully threaded cortical lag screws rather than 4.0-mm cancellous screws. Biomechanical data suggest that bicortical fixation (engaging the lateral tibial cortex) provides increased construct strength, which is particularly advantageous in osteoporotic bone or vertical shear fracture patterns.
ISOLATED FRACTURES OF THE LATERAL MALLEOLUS
The lateral malleolus is the most frequently fractured bone in the ankle. The fibula acts as a lateral buttress, preventing lateral talar subluxation.
Classification Systems
Understanding the mechanism of injury is paramount. The Danis-Weber classification is based on the location of the fibular fracture relative to the distal tibiofibular syndesmosis and is highly predictive of syndesmotic integrity. Malek et al. reported high interobserver and intraobserver reliability using the Danis-Weber classification system (78% and 85%, respectively).
Danis-Weber Type A
Caused by a supination-adduction mechanism. These injuries produce a transverse avulsion fracture of the lateral malleolus at or below the level of the tibial plafond. They may occur with or without an oblique shear fracture of the medial malleolus. The syndesmosis remains intact.
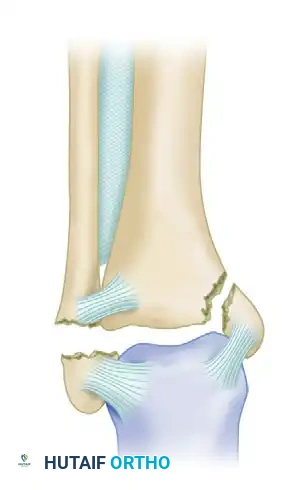
Danis-Weber Type B
Caused by a supination-external rotation (SER) mechanism. This results in an oblique or spiral fracture of the lateral malleolus, beginning on the anteromedial surface at the level of the syndesmosis and extending proximally to the posterolateral aspect.
* Approximately 80% to 90% of all lateral malleolar fractures fall into the Danis-Weber Type B category.
* The injury may include rupture or avulsion of the anterior inferior tibiofibular ligament (AITFL), fracture of the medial malleolus, or rupture of the deltoid ligament.
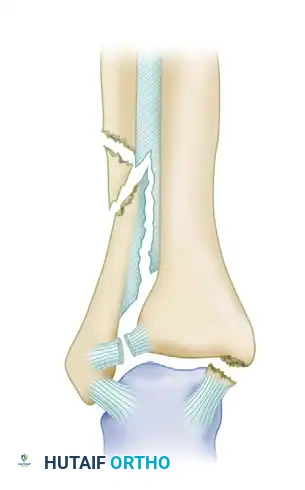
Danis-Weber Type C
Caused by pronation-abduction or pronation-external rotation mechanisms. These are characterized by a fibular fracture proximal to the syndesmosis, indicating disruption of the syndesmotic ligament complex.
* Type C-1: Abduction injuries with an oblique fracture of the fibula just proximal to the disrupted tibiofibular ligaments.
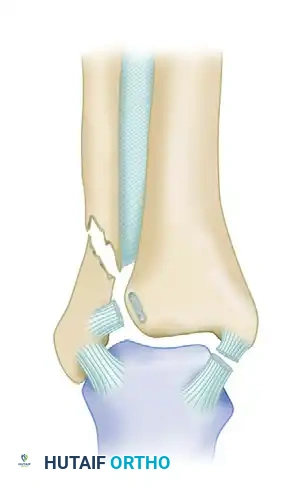
* Type C-2: Abduction-external rotation injuries with a more proximal diaphyseal fracture of the fibula and extensive disruption of the interosseous membrane.
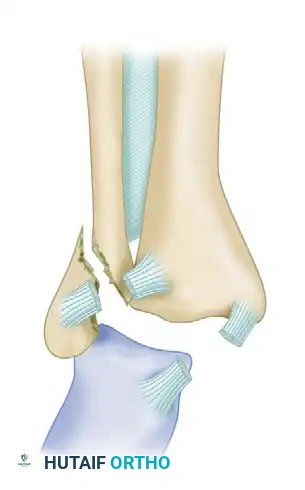
Type C injuries frequently involve a medial malleolar fracture or a complete deltoid ligament rupture. Fracture of the posterior malleolus may accompany any of the three types.
The AO/OTA Classification
The AO classification further divides the three Danis-Weber types based on associated medial and posterior injuries, providing a more granular framework for surgical planning.
AO Classification of Malleolar Fractures (Box 54-2)
Type A: Fibula Fracture Below Syndesmosis (Infrasyndesmotic)
* A1 — Isolated
* A2 — With fracture of medial malleolus
* A3 — With a posteromedial fractureType B: Fibula Fracture at Level of Syndesmosis (Transsyndesmotic)
* B1 — Isolated
* B2 — With medial lesion (malleolus or ligament)
* B3 — With a medial lesion and fracture of posterolateral tibiaType C: Fibula Fracture Above Syndesmosis (Suprasyndesmotic)
* C1 — Diaphyseal fracture of the fibula, simple
* C2 — Diaphyseal fracture of the fibula, complex
* C3 — Proximal fracture of the fibula
Clinical Evaluation and the "Bimalleolar Equivalent"
The indications for operative reduction of isolated lateral malleolar fractures remain a topic of intense academic debate.
Acceptable Displacement: The maximal acceptable displacement of the fibula reported in the literature ranges from 0 to 5 mm. In most patients, 2 to 3 mm of fibular displacement is accepted, provided the talus is perfectly reduced and the patient's functional demands are considered.
Talar Displacement: Displacement of the talus frequently accompanies displacement of the lateral malleolus in bimalleolar ankle fractures; therefore, anatomical reduction of the lateral malleolus is absolutely necessary in these injuries to restore the mortise.
Isolated vs. Bimalleolar Equivalent: Biomechanical studies have shown that truly isolated fractures of the lateral malleolus do not disturb joint kinematics or cause talar displacement with axial loading. Long-term clinical follow-up of closed treatment for Supination-External Rotation (SER) stage II fractures demonstrates 94% to 98% good functional results, even with up to 3 mm of fibular displacement. Results after operative treatment for SER II injuries are similar to closed treatment, regardless of whether anatomical reduction was obtained.
However, if a lateral malleolus fracture is accompanied by a complete rupture of the deltoid ligament, it is termed a "Bimalleolar Equivalent" fracture. This is highly unstable and requires operative fixation of the fibula.
Assessing Medial Stability
If the stability of a lateral malleolar fracture is uncertain (e.g., medial tenderness, swelling, or ecchymosis without a medial fracture), stress radiographs must be obtained to detect talar shift indicative of medial injury.
* Gravity Stress View: The patient lies in the lateral decubitus position with the affected ankle facing downward. Gravity acts to subluxate the talus laterally if the deltoid is incompetent. A medial clear space > 4 mm (or > 1 mm wider than the superior clear space) is diagnostic of deltoid rupture.
* MRI and Ultrasound: Koval et al. evaluated whether a positive stress test definitively predicts the need for operative fixation. In their study, patients with positive stress radiographs underwent MRI to evaluate the deltoid ligament complex. They found that only complete ruptures required operative stabilization. Patients with partial disruptions had successful nonoperative management. Others have proposed ultrasonographic evaluation of the deltoid ligament to differentiate between a bimalleolar equivalent fracture and an isolated lateral injury. However, the ideal preoperative diagnostic modality remains a subject of ongoing research.
Surgical Warning: Never accept lateral talar shift. If the medial clear space is widened on static or stress views, the deltoid is incompetent. The fibula must be anatomically reduced and plated to restore the lateral buttress and realign the talus.
Surgical Technique: Lateral Malleolus ORIF
Positioning and Approach
- Positioning: Supine with a bump under the ipsilateral hip to internally rotate the leg, bringing the lateral malleolus directly anterior. A thigh tourniquet is utilized.
- Incision: A direct lateral or slightly posterolateral longitudinal incision is made over the fibula. The posterolateral approach allows for thicker soft tissue coverage over the plate and easier access to the posterior malleolus if needed.
- Nerve Protection: The superficial peroneal nerve (anteriorly) and the sural nerve (posteriorly) must be identified and protected during superficial dissection.
- Exposure: The fracture site is exposed. The fracture hematoma is evacuated, and the fracture ends are irrigated. The periosteum is elevated only 1-2 mm from the fracture edges to preserve blood supply.
Reduction and Fixation
- Reduction: The fracture is reduced anatomically. For oblique Type B fractures, a pointed reduction clamp is placed across the fracture to compress the fragments. Restoring fibular length and rotation is critical; the lateral malleolus must not be shortened or malrotated.
- Interfragmentary Lag Screw: A 3.5-mm cortical lag screw is placed perpendicular to the fracture plane. The near cortex is overdrilled (3.5 mm), the far cortex is drilled (2.5 mm), the hole is countersunk, measured, tapped, and the screw is inserted to provide absolute stability and interfragmentary compression.
- Neutralization Plate: A one-third tubular plate or a pre-contoured anatomical locking plate is applied to the lateral (or posterolateral) surface of the fibula to neutralize torsional and bending forces.
- The plate should ideally span at least three cortices proximal and three cortices distal to the fracture.
- In osteoporotic bone, locking plates provide superior pull-out strength.
- Syndesmotic Evaluation: Following fibular fixation, the syndesmosis must be tested using the "Cotton test" (lateral pull on the fibula with a bone hook) or external rotation stress under fluoroscopy. If widening occurs, syndesmotic fixation (screws or flexible suture buttons) is required.
POSTOPERATIVE PROTOCOL AND REHABILITATION
Optimal postoperative care is essential for maximizing functional recovery and minimizing complications such as stiffness or complex regional pain syndrome (CRPS).
- Immediate Postoperative Phase (Weeks 0-2):
- The ankle is placed in a well-padded posterior splint or a bulky Jones dressing in neutral dorsiflexion.
- Strict non-weight-bearing status is maintained.
- Elevation and cryotherapy are emphasized to reduce edema.
- Early Rehabilitation Phase (Weeks 2-6):
- Sutures are removed at 10-14 days.
- The patient is transitioned to a removable controlled ankle motion (CAM) boot.
- Active and active-assisted range of motion (ROM) exercises (plantarflexion and dorsiflexion) are initiated to prevent capsular contracture. Inversion/eversion is introduced cautiously.
- Weight-bearing status depends on fracture stability and bone quality. For isolated, rigidly fixed malleolar fractures, partial weight-bearing may be initiated, progressing to full weight-bearing as tolerated in the CAM boot.
- Advanced Rehabilitation (Weeks 6-12):
- Radiographs are obtained at 6 weeks to confirm callus formation and maintenance of reduction.
- Weaning from the CAM boot to a supportive lace-up ankle brace.
- Physical therapy focuses on proprioception, balance training (e.g., BAPS board), and progressive strengthening of the peroneal and tibial musculature.
- Return to Activity: High-impact activities and sports are generally restricted until 3 to 4 months postoperatively, contingent upon radiographic union and the restoration of symmetric strength and dynamic stability.
CONCLUSION
The management of isolated medial and lateral malleolar fractures requires a nuanced understanding of ankle biomechanics, precise radiographic interpretation, and meticulous surgical technique. While many isolated, nondisplaced fractures can be managed conservatively with excellent outcomes, the presence of displacement, talar shift, or occult ligamentous instability mandates operative intervention. By adhering to the principles of anatomical reduction, stable internal fixation, and structured rehabilitation, orthopedic surgeons can reliably restore joint congruency and optimize long-term patient function.
📚 Medical References
- [Malleolar fractures. In Weber BG, Brunner C, Freuler F, eds: Treatment of fractures in children and adolescents, New York, 1980, Springer-Verlag.
Foot Fractures Alexander AH, Lichtman DM: Surgical treatment of transchondral talar dome fractures (](https://pubmed.ncbi.nlm.nih.gov/?term=Malleolar%20fractures.%20In%20Weber%20BG%2C%20Brunner%20C%2C%20Freuler%20F%2C%20eds%3A%20Treatment%20of%20fractures%20in%20children%20and%20adolescents%2C%20New%20York%2C%201980%2C%20Springer-Verlag.%0A%0AFoot%20Fractures%20Alexander%20AH%2C%20Lichtman%20DM%3A%20Surgical%20treatment%20of%20transchondral%20talar%20dome%20fractures%20%28)
