Fundamental Principles, Equipment, and Complication Management in Arthroscopic Surgery
Key Takeaway
Arthroscopic surgery requires a profound understanding of joint biomechanics, fluid dynamics, and energy device applications. This comprehensive guide details the critical principles of patient positioning, anesthesia, and intraoperative equipment management. Furthermore, it provides evidence-based protocols for mitigating severe complications, including surgical site infections, neurovascular injuries, and venous thromboembolism, ensuring optimal outcomes for orthopedic patients undergoing minimally invasive joint procedures.
Introduction to Advanced Arthroscopic Principles
Arthroscopic surgery has revolutionized the field of orthopedics, transitioning from a purely diagnostic modality to a highly sophisticated therapeutic intervention. The evolution of high-definition imaging, specialized instrumentation, and advanced energy devices allows for the minimally invasive management of complex intra-articular pathology across the knee, shoulder, hip, elbow, wrist, and ankle. However, the minimally invasive nature of arthroscopy belies the profound physiological and biomechanical alterations it induces within the joint space.
Mastery of arthroscopic surgery requires far more than technical dexterity; it demands a rigorous understanding of fluid dynamics, thermal energy tissue interactions, neurovascular anatomy, and evidence-based complication mitigation. This masterclass synthesizes decades of peer-reviewed literature to provide a comprehensive, textbook-level guide for orthopedic residents, fellows, and practicing consultants.
Preoperative Optimization and Anesthesia
The success of an arthroscopic procedure begins long before portal placement. Preoperative optimization and the selection of appropriate anesthetic modalities directly influence intraoperative visualization, hemodynamic stability, and postoperative rehabilitation.
Anesthetic Modalities
The choice of anesthesia—local, regional, neuraxial, or general—must be tailored to the specific joint, the anticipated duration of the procedure, and patient comorbidities.
- Knee Arthroscopy: Routine elective knee arthroscopy (e.g., partial meniscectomy, chondroplasty) can often be performed under local anesthesia with intravenous sedation, spinal anesthesia, or general anesthesia. Evidence suggests that local anesthesia, when combined with intra-articular infiltration, offers comparable efficacy to general anesthesia for short procedures, with the added benefits of reduced cost and faster discharge times.
- Shoulder Arthroscopy: Regional anesthesia, specifically the interscalene brachial plexus block, is the gold standard. It provides profound intraoperative muscle relaxation and exceptional postoperative analgesia.
- Hip Arthroscopy: General anesthesia with profound muscle relaxation is typically required to overcome the robust muscular envelope of the hip and allow for adequate joint distraction.
Multimodal Analgesia and Intra-articular Therapeutics
Pre-emptive and multimodal analgesia are critical for outpatient arthroscopy. The intra-articular instillation of local anesthetics (e.g., bupivacaine, ropivacaine) combined with adjuncts such as morphine or clonidine has been shown to significantly reduce postoperative opioid consumption.
Clinical Pearl: When utilizing intra-articular local anesthetics, particularly bupivacaine, surgeons must be cognizant of the risk of chondrotoxicity. Continuous infusion pumps delivering high concentrations of local anesthetics directly into the joint space have been implicated in devastating cases of post-arthroscopic glenohumeral chondrolysis (PAGCL).
Patient Positioning and Biomechanics of Setup
Meticulous patient positioning is paramount. It dictates portal accessibility, instrument triangulation, and the safe application of traction.
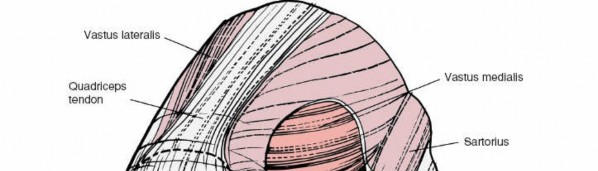
The Knee: Tourniquet Application and Hemostasis
The use of a pneumatic tourniquet in knee arthroscopy remains a topic of debate. While it provides a bloodless field, it is associated with postoperative thigh pain, delayed quadriceps activation, and a theoretical increased risk of deep vein thrombosis (DVT).
Many experienced arthroscopists advocate for a "tourniquet-less" approach, relying instead on the hydrostatic pressure of the irrigation fluid and the addition of dilute epinephrine (e.g., 1 mg of epinephrine per 3 liters of irrigation fluid) to maintain hemostasis. If a tourniquet is utilized, inflation pressures should be minimized (typically 100 mm Hg above systolic blood pressure), and inflation time should strictly not exceed 120 minutes.
The Shoulder: Beach-Chair vs. Lateral Decubitus
Shoulder arthroscopy is performed in either the beach-chair (modified Fowler) or lateral decubitus position.
* Beach-Chair Position: Offers an anatomical orientation, ease of conversion to an open procedure, and excellent visualization of the anterior and superior compartments. However, it carries a risk of cerebral hypoperfusion (cerebral desaturation events) due to the upright posture.
* Lateral Decubitus Position: Utilizes longitudinal and lateral traction to distract the glenohumeral joint, providing superior visualization of the inferior capsule and labrum. Care must be taken to avoid traction neurapraxia of the brachial plexus.
The Hip: Traction Mechanics and Perineal Safety
Hip arthroscopy requires significant traction (often 50 to 100 lbs) to overcome the suction seal of the labrum and distract the joint by 10 mm for safe instrument insertion.
Surgical Warning: Prolonged traction against a perineal post can result in devastating complications, including pudendal nerve palsy, vulvar or scrotal necrosis, and neuropraxia of the sciatic or femoral nerves. Traction time must be strictly monitored and ideally limited to less than 2 hours.
Intraoperative Fluid Dynamics and Energy Devices
The arthroscopic environment is entirely dependent on the continuous flow of irrigation fluid to distend the joint, clear debris, and maintain hemostasis.
Irrigation Solutions and Pump Systems
- Fluid Selection: Normal saline (0.9% NaCl) and Lactated Ringer's (LR) are the most commonly used irrigants. In vitro studies suggest that LR is more physiologic and less detrimental to human meniscus-derived cells and articular cartilage than normal saline during prolonged exposure.
- Fluid Management Systems: Automated arthroscopic pumps maintain a constant intra-articular pressure and flow rate. The pressure should be set to the lowest level necessary to maintain visualization—typically 30 to 40 mm Hg for the knee and shoulder, and up to 60 mm Hg for the hip.
Radiofrequency, Electrocautery, and Thermal Energy
Energy devices are indispensable for tissue ablation, synovectomy, and hemostasis.
* Electrocautery: Traditional monopolar and bipolar electrocautery are effective but generate significant collateral thermal spread.
* Radiofrequency (RF) Ablation: Bipolar RF devices operate at lower temperatures than monopolar devices and are highly effective for soft tissue debridement. However, thermal energy must be used judiciously.
Pitfall: Excessive use of thermal energy, particularly in the knee or shoulder, can lead to thermal chondrolysis, capsular necrosis, and even osteonecrosis of the underlying subchondral bone. The RF probe must be kept in constant motion, and adequate fluid flow must be maintained to dissipate heat.
Principles of Portal Placement and Triangulation
The foundational skill of arthroscopy is triangulation—the ability to manipulate an instrument and an arthroscope from two different portals to converge on a single intra-articular target.
- Diagnostic Tour: Every procedure must begin with a systematic, reproducible diagnostic tour of the joint to ensure no pathology is missed.
- Portal Placement: Portals must be placed precisely using anatomical landmarks. "Make the portal where the pathology dictates, not where the textbook says." The use of a spinal needle to localize the optimal trajectory before making a scalpel incision is mandatory.
- Safety Zones: Surgeons must possess an intimate knowledge of the neurovascular "danger zones" (e.g., the popliteal neurovascular bundle in the posterior knee, the axillary nerve in the inferior shoulder, and the lateral femoral cutaneous nerve in the anterior hip).
Comprehensive Management of Arthroscopic Complications
While arthroscopy is minimally invasive, it is not without risk. A thorough understanding of potential complications is essential for the practicing orthopedic surgeon.
Surgical Site Infections and Septic Arthritis
The incidence of septic arthritis following elective arthroscopy is remarkably low (approximately 0.1% to 0.4%).
* Prophylaxis: The routine use of prophylactic intravenous antibiotics for simple diagnostic arthroscopy or partial meniscectomy remains controversial. However, prophylaxis (e.g., Cefazolin 2g IV) is strictly indicated for procedures involving implants (e.g., ACL reconstruction, rotator cuff repair, meniscal repair).
* Management: Any patient presenting with disproportionate postoperative pain, swelling, erythema, and restricted range of motion must be evaluated for septic arthritis. Aspiration yielding a synovial fluid white blood cell count > 50,000 cells/mm³ (with > 90% polymorphonuclear leukocytes) mandates emergent arthroscopic irrigation and debridement.
Neurovascular Compromise
Vascular injuries are rare but potentially limb-threatening.
* Popliteal Artery Injury: The popliteal artery is at extreme risk during posterior meniscal repairs, posterior capsular releases, and PCL reconstructions. Penetration of the posterior capsule can lead to arterial laceration or the formation of a pseudoaneurysm.
* Nerve Palsies: Most nerve injuries are neuropraxias secondary to traction, tourniquet ischemia, or direct compression. Direct laceration (e.g., the infrapatellar branch of the saphenous nerve during anteromedial portal placement) can result in painful neuromas.
Venous Thromboembolism (VTE)
The incidence of symptomatic DVT after knee arthroscopy is generally less than 1%, though venographically proven asymptomatic DVT rates are higher.
* Risk Factors: Age > 50, obesity, tourniquet time > 60 minutes, history of VTE, and oral contraceptive use.
* Prophylaxis: Routine pharmacologic thromboprophylaxis is not recommended for all patients. However, in high-risk patients, the use of Low-Molecular-Weight Heparin (LMWH) or direct oral anticoagulants (DOACs) for 7 to 14 days postoperatively is strongly advised.
Instrument Breakage and Iatrogenic Chondral Injury
The confined intra-articular space and the use of fragile instruments (e.g., arthroscopic biters, shaver blades) predispose to instrument breakage.
* Prevention: Never force an instrument. If an instrument breaks, the surgeon must immediately halt fluid flow (to prevent the fragment from migrating), keep the arthroscope focused on the fragment, and introduce a magnetic retriever or grasper through a secondary portal.
* Chondral Injury: Scuffing of the articular cartilage is a hallmark of poor portal placement or aggressive instrument manipulation. Meticulous technique and the use of switching sticks or cannulas can minimize iatrogenic damage.
Fluid Extravasation
Prolonged procedures or capsular defects can lead to massive fluid extravasation into the surrounding soft tissues. In the knee, this can cause a symptomatic calf or thigh swelling; in the shoulder, it can lead to airway compromise (if fluid tracks into the neck) or deltoid compartment syndrome. Monitoring the patient's soft tissues intraoperatively and utilizing the lowest effective pump pressure are critical preventative measures.
Postoperative Rehabilitation Protocols
The surgical intervention is only one-half of the clinical equation; rigorous, phase-appropriate rehabilitation is essential for optimal outcomes.
- Phase I (Immediate Postoperative): Focus on controlling inflammation, protecting the surgical repair, and restoring early passive range of motion (ROM). Cryotherapy and elevation are paramount.
- Phase II (Intermediate): Gradual restoration of active ROM and initiation of isometric and closed-kinetic-chain strengthening.
- Phase III (Advanced): Proprioceptive training, open-kinetic-chain exercises, and sport-specific functional drills.
Return to play or unrestricted activity must be dictated by objective criteria, including full, painless ROM, symmetrical muscle strength (typically > 90% of the contralateral limb on isokinetic testing), and psychological readiness.
Conclusion
Arthroscopic surgery represents a pinnacle of modern orthopedic intervention, blending intricate anatomical knowledge with advanced technological application. By adhering to strict evidence-based principles regarding patient positioning, fluid dynamics, energy device utilization, and complication prophylaxis, the orthopedic surgeon can consistently deliver safe, effective, and transformative care to their patients. Continuous education and a profound respect for the physiological impact of minimally invasive techniques remain the hallmarks of the master arthroscopist.
📚 Medical References
- arthroscopic surgery, Anesth Analg 93:776, 2001.
- Horowitz MC, Friedlaender GE: Immunologic aspects of bone transplantation: a rationale for future studies, Orthop Clin North Am 18:227, 1987.
- Inclan A: The use of preserved bone graft in orthopedic surgery, J Bone Joint Surg 24:81, 1942.
- Jones AAM, Dougherty PJ, Sharkey NA, et al: Iliac crest bone graft: saw versus osteotome, Spine 18:2048, 1993.
- Khuri S, Uhl RL, Martino J, et al: Clinical application of the forearm tourniquet, J Hand Surg 19A:861, 1994.
- Kirn TF: Developments like major resection bone allografts foster progress in tissue-banking technology, JAMA 258:305, 1987.
- Klenerman L, Biswas M, Hulands GH, et al: Systemic and local effects of the application of a tourniquet, J Bone Joint Surg 62B:385, 1980.
- Krackow KA: A maneuver for improved positioning of a tourniquet in the obese patient, Clin Orthop Relat Res 168:80, 1982.
- Krackow KA, Cohn BT: A new technique for passing tendon through bone: brief note, J Bone Joint Surg 69A:922, 1987.
- Krackow KA, Thomas SC, Jones LC: Ligament-tendon fixation: analysis of a new stitch and comparison with standard techniques, Orthopedics 11:909, 1988.
- Kutty S, McElwain JP: Padding under tourniquets in tourniquet controlled surgery: Bruner’s ten rules revisited, Injury 33:75, 2002.
- Lane JM, Sandhu HS: Current approaches to experimental
You Might Also Like