Mini-Invasive Quadricepsplasty: Advanced Techniques and Surgical Protocols
Key Takeaway
Mini-invasive quadricepsplasty is an advanced, stepwise surgical intervention designed to treat severe knee arthrofibrosis. By combining arthroscopic intra-articular lysis of adhesions with targeted, extra-articular percutaneous releases of the quadriceps mechanism, surgeons can systematically restore knee flexion. This technique minimizes soft tissue trauma compared to traditional open approaches, significantly reducing the risk of extensive scarring while achieving excellent functional outcomes and minimizing postoperative extension lag.
Introduction to Knee Arthrofibrosis and Quadricepsplasty
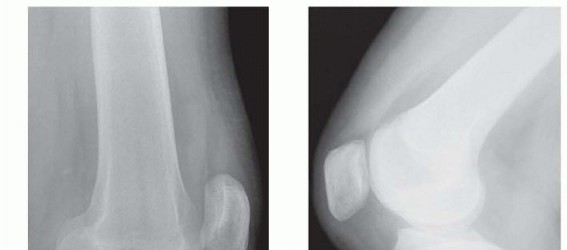
Severe knee stiffness, or arthrofibrosis, remains one of the most debilitating complications following distal femoral fractures, complex intra-articular knee trauma, and major reconstructive knee surgeries. The profound loss of knee flexion not only impairs normal gait biomechanics but also severely restricts activities of daily living, such as ascending stairs, sitting in confined spaces, and rising from a chair. Historically, the management of refractory knee stiffness relied heavily on extensive open surgical procedures, most notably the Thompson and Judet quadricepsplasties. While these traditional open techniques are effective at restoring a functional arc of motion, they are inherently fraught with significant morbidity, including massive surgical trauma, extensive postoperative hematoma formation, wound healing complications, and a high incidence of postoperative extension lag due to the profound disruption of the extensor mechanism.
In recent years, the paradigm has shifted toward joint-preserving, minimally invasive interventions. Endoscopically and arthroscopically assisted percutaneous techniques have been described for quadricepsplasty, offering a compelling alternative to traditional open exposures. Although long-term follow-up reports in the literature remain relatively sparse and these techniques are not yet universally established as the gold standard, they represent a critical evolution in operative orthopaedics.
Pioneering work by Wang, Zhao, and He described an innovative extra-articular "mini-invasive" quadricepsplasty followed by intra-articular arthroscopic lysis of adhesions. Their procedure is meticulously executed in five sequential stages. The fundamental philosophy of this approach is the incremental release of tethering structures; the range of flexion is objectively measured after each stage of release, and the procedure is immediately terminated when the desired degree of flexion—ideally 120 degrees—is obtained. This stepwise methodology is paramount in preventing over-release, thereby mitigating the risk of iatrogenic extensor lag.
Pathoanatomy and Biomechanics of the Stiff Knee
To effectively execute a mini-invasive quadricepsplasty, the orthopaedic surgeon must possess an intimate understanding of the pathoanatomy of knee arthrofibrosis. The loss of flexion is rarely attributable to a single anatomical structure; rather, it is a multi-compartmental cascade of fibrosis.
The Quadriceps Mechanism
The quadriceps femoris consists of four distinct muscle bellies. In the setting of femoral trauma, the vastus intermedius is the most frequently implicated culprit in the genesis of knee stiffness. Because of its direct anatomical apposition to the anterior femoral cortex, the vastus intermedius is highly susceptible to scarring, fibrosis, and tethering to the healing fracture callus or periosteum. This creates an unyielding tether that physically prevents the distal excursion of the patella during knee flexion.
The Suprapatellar Pouch and Gutters
The suprapatellar pouch is a critical bursa that allows the extensor mechanism to glide smoothly over the anterior distal femur. In arthrofibrosis, this pouch is often completely obliterated by dense, intra-articular adhesive bands. Similarly, the medial and lateral parapatellar gutters become contracted, effectively cementing the patella to the underlying femoral condyles.
The Rectus Femoris and Retinacula
The rectus femoris, being a biarticular muscle, can develop adaptive shortening and contracture, particularly if the knee has been immobilized in extension for a prolonged period. Furthermore, the medial and lateral retinacula undergo fibrotic thickening, contributing to patellar immobility and increased patellofemoral contact pressures.
Clinical Pearl: The "patellar glide test" is a critical preoperative assessment. A patella that is rigidly fixed and cannot be translated superiorly, inferiorly, medially, or laterally indicates severe obliteration of the suprapatellar pouch and parapatellar gutters, necessitating an initial intra-articular arthroscopic lysis before any extra-articular release is attempted.
Indications and Patient Selection
Mini-invasive quadricepsplasty is indicated for patients with severe, refractory knee stiffness who have failed a comprehensive regimen of conservative management, including aggressive physical therapy, dynamic splinting, and manipulation under anesthesia (MUA) performed in the early postoperative period.
Primary Indications:
* Post-traumatic arthrofibrosis (e.g., following distal femur, proximal tibia, or patella fractures).
* Post-surgical stiffness (e.g., following anterior cruciate ligament reconstruction or total knee arthroplasty, provided there is no component malposition or infection).
* Stiffness secondary to prolonged immobilization.
Contraindications:
* Active intra-articular or periarticular infection.
* Ununited fractures of the distal femur or proximal tibia (releases may displace the non-union).
* Severe intra-articular incongruity or advanced post-traumatic osteoarthritis (where a total knee arthroplasty might be the more appropriate primary intervention).
* Inadequate soft tissue coverage or active wound breakdown over the anterior knee.
Surgical Technique: The Stepwise Mini-Invasive Approach
The procedure is performed under general or regional anesthesia. A thorough preoperative examination under anesthesia (EUA) is conducted to document the baseline range of motion and assess the exact nature of the mechanical block. The patient is positioned supine on a radiolucent operating table. A high thigh tourniquet is applied but typically inflated only if visualization becomes compromised during the arthroscopic phase.
Stage 1: Arthroscopic Intra-Articular Lysis of Adhesions
The procedure begins with the establishment of standard anterolateral and anteromedial arthroscopic portals. In severely stiff knees, portal placement must be precise to avoid iatrogenic damage to the articular cartilage, as the joint space is often severely contracted.
- Anterior Interval Release: Using a motorized shaver and radiofrequency ablation wand, the dense scar tissue in the anterior interval (between the infrapatellar fat pad and the anterior tibia) is meticulously resected.
- Gutter Clearance: The arthroscope is directed into the medial and lateral parapatellar gutters. Adhesions tethering the patella to the femoral condyles are released.
- Suprapatellar Pouch Reconstitution: A superolateral or superomedial portal is often required. The obliterated suprapatellar pouch is systematically recreated by excising the fibrotic bands bridging the deep surface of the quadriceps tendon and the anterior femur.
Surgical Warning: Extreme caution must be exercised when clearing the suprapatellar pouch to avoid inadvertently penetrating the quadriceps tendon or the anterior joint capsule, which could lead to extravasation of irrigation fluid into the thigh compartments, precipitating compartment syndrome.
Stage 2: Mini-Invasive Extra-Articular Releases
If satisfactory flexion (target 120 degrees) is not achieved following intra-articular lysis, the surgeon proceeds to the extra-articular phases. The raw text highlights a progressive approach that can be tailored based on intraoperative flexion measurements.
Phase 2A: Parapatellar and Suprapatellar Gutter Release
Release of the adhesions in the suprapatellar gutter and between the patella and femoral condyles is performed through a limited longitudinal or medial (or both) parapatellar incision. This mini-open approach allows for direct visualization and sharp dissection of the dense retinacular tissues that could not be safely addressed via arthroscopy.
Phase 2B: Vastus Intermedius Release
If the vastus intermedius is heavily scarred to the femur, a release is performed. As described in alternative open techniques, this can be achieved through a long posterolateral incision extending from the superior pole of the patella to the greater trochanter. In the "mini-invasive" iteration, this is modified. Using specialized periosteal elevators or endoscopic assistance through small stab incisions, the vastus intermedius is bluntly and sharply elevated off the anterior femoral cortex. The goal is to create a gliding plane between the muscle and the bone without completely transecting the muscle belly, thereby preserving its contribution to active extension.
Stage 3: Rectus Femoris Detachment (The Final Phase)
The final phase is utilized only if flexion remains unacceptably limited after manipulation subsequent to the first two phases. This involves the detachment of the rectus femoris from its insertion at the anterior inferior iliac spine (AIIS).
This is typically accessed through a proximal anterolateral extension of the posterolateral incision, or via a separate proximal mini-incision. By releasing the proximal origin of the rectus femoris, the biarticular tether is eliminated, allowing for significant distal excursion of the extensor mechanism.
Stage 4: Sequential Manipulation Under Anesthesia
Throughout the procedure, gentle manipulation of the knee is performed. The range of flexion is measured after each stage of release.
Pitfall: Forceful, aggressive manipulation of a stiff knee is strictly contraindicated. Using the tibia as a long lever arm against a tethered quadriceps mechanism places immense stress on the patellar tendon and the patella itself. This can result in catastrophic iatrogenic complications, including patellar tendon avulsion, transverse patella fracture, or supracondylar femur fracture. Always apply pressure directly over the proximal pole of the patella to push it distally while gently flexing the knee.
The procedure is terminated immediately when the desired degree of flexion (ideally 120 degrees) is obtained.
Clinical Outcomes and Evidence-Based Results
Currently, the most prominent report of the results of this specific 5-stage mini-invasive technique is that of the technique developers (Wang, Zhao, and He). In their cohort of 22 patients with severely arthrofibrotic knees, observed for an average follow-up of 44 months, the results were highly encouraging:
- Excellent Results: 16 patients
- Good Results: 5 patients
- Fair Results: 1 patient
The objective metrics demonstrated a profound improvement in the functional arc of motion. Average maximal flexion increased dramatically from a preoperative baseline of 15 degrees to 115 degrees at the most recent follow-up.
Crucially, the incidence of postoperative extension lag—the most feared complication of traditional open quadricepsplasty—was remarkably low. Only one patient in the cohort had a persistent 15-degree extension lag. While independent, multi-center validation of this technique is still required, it represents a highly reasonable and biomechanically sound alternative to open quadricepsplasty. Furthermore, the mini-invasive nature of the incisions produces a significantly more pleasing cosmetic result and reduces the risk of extensive wound healing complications.
When comparing this to the broader literature on modified open procedures (which utilize the 3-phase approach of parapatellar release, posterolateral vastus intermedius release, and AIIS rectus detachment), most reports are small with relatively short follow-up. However, the aggregate data suggests that excellent or good results can be expected in approximately 81% of patients, with fair results in the remaining 19%.
Postoperative Rehabilitation Protocol
The success of a mini-invasive quadricepsplasty is inextricably linked to the postoperative rehabilitation protocol. The surgery merely creates the potential for motion; aggressive, immediate, and sustained physical therapy is required to maintain it.
Pain Management
Optimal pain control is the cornerstone of postoperative rehabilitation. A continuous femoral nerve block, adductor canal block, or epidural analgesia is highly recommended for the first 48 to 72 hours. This allows the patient to tolerate aggressive early motion without being inhibited by severe pain.
Early Mobilization (Days 0-7)
- Continuous Passive Motion (CPM): A CPM machine is applied immediately in the recovery room. The machine is initially set to the maximum flexion achieved intraoperatively (minus 10 degrees to account for tissue tension) and is utilized for 6 to 8 hours daily.
- Active-Assisted Range of Motion: Physical therapy initiates active-assisted flexion and extension exercises on postoperative day one.
- Extension Splinting: To prevent the development of an extension lag or flexion contracture, the knee is maintained in a rigid extension splint at night.
Subacute Phase (Weeks 2-6)
- Quadriceps Strengthening: As the acute surgical inflammation subsides, the focus shifts to restoring the strength of the quadriceps mechanism. Straight leg raises, isometric quadriceps sets, and closed-kinetic-chain exercises are initiated.
- Scar Mobilization: Aggressive patellar mobilization and soft tissue massage around the portal sites and mini-incisions are performed to prevent the recurrence of superficial adhesions.
Long-Term Maintenance (Months 2-6)
Patients must understand that the biological tendency of the knee is to re-scar. A daily home exercise program emphasizing terminal stretching in both flexion and extension must be maintained for a minimum of six months postoperatively.
Complications and Management
While the mini-invasive approach mitigates many risks associated with open surgery, complications can still occur:
- Extensor Lag: As noted, this occurred in one patient (15 degrees) in the Wang et al. series. It is usually the result of over-release of the vastus intermedius or rectus femoris, or failure of the patient to actively recruit the quadriceps postoperatively. Management includes aggressive quadriceps strengthening and electrical muscle stimulation.
- Hemarthrosis: Intra-articular bleeding can lead to recurrent fibrosis. Meticulous intraoperative hemostasis using radiofrequency ablation and the judicious use of postoperative intra-articular drains (if a mini-open approach was utilized) are preventative measures.
- Recurrent Arthrofibrosis: Occurs primarily in patients who are non-compliant with the rigorous postoperative rehabilitation protocol or those who experience inadequate postoperative pain control.
- Iatrogenic Fractures or Tendon Ruptures: Prevented by adhering to the principle of gentle, sequential manipulation rather than forceful, single-stage bending of the knee.
Conclusion
Mini-invasive quadricepsplasty, combining arthroscopic intra-articular lysis with sequential extra-articular releases, represents a sophisticated, evidence-based evolution in the management of the severely stiff knee. By adhering to a strict, stepwise protocol—measuring flexion at each stage and terminating the procedure once 120 degrees is achieved—the orthopaedic surgeon can maximize functional recovery while minimizing the surgical morbidity and extensor lag historically associated with traditional open techniques. Mastery of this procedure requires not only technical surgical proficiency but also a deep understanding of knee pathoanatomy and a commitment to rigorous postoperative rehabilitation.
You Might Also Like