Extraarticular Ankylosis of the Knee: Comprehensive Surgical Management
Key Takeaway
Extraarticular ankylosis of the knee presents a complex reconstructive challenge, often resulting from femoral fractures or severe soft tissue trauma. Surgical management typically involves a meticulous quadricepsplasty to release fibrotic adhesions, particularly of the vastus intermedius, while preserving the rectus femoris. In cases with significant patellofemoral involvement, adjunctive tibial tubercle elevation may be indicated to decompress the joint. Successful outcomes rely heavily on rigorous postoperative rehabilitation and early mobilization.
INTRODUCTION TO EXTRAARTICULAR ANKYLOSIS OF THE KNEE
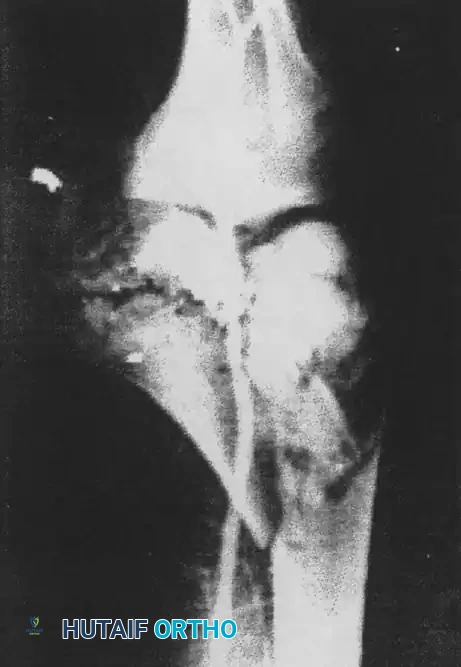
Ankylosis of the knee represents a profound loss of joint mobility that severely compromises a patient's functional independence, gait biomechanics, and overall quality of life. This pathology is broadly classified into intraarticular and extraarticular etiologies. Extraarticular ankylosis typically arises from severe soft tissue contractures, heterotopic ossification, or extensive fibrosis of the extensor mechanism, often sparing the articular cartilage itself. Consequently, preoperative radiographs may reveal an apparently normal joint space, distinguishing this condition from end-stage intraarticular arthrofibrosis or advanced osteoarthritis.
The deformity may present with the knee locked in complete extension, in isolated flexion, or in a complex multi-planar deformity characterized by flexion, external rotation, and valgus malalignment. When extraarticular ankylosis and contracture limit mobility—regardless of whether the primary deformity is in flexion or extension—a comprehensive soft tissue release procedure is generally indicated. Procedures such as quadricepsplasty or extensive posterior capsulotomy form the cornerstone of surgical intervention.
Clinical Pearl: The presence of a preserved radiographic joint space in a rigidly stiff knee is the hallmark of extraarticular ankylosis. This finding should immediately direct the surgeon’s focus toward the periarticular soft tissues, specifically the quadriceps mechanism and capsular structures, rather than intraarticular joint replacement.
PATHOANATOMY OF EXTRAARTICULAR ANKYLOSIS IN EXTENSION
Extraarticular ankylosis in extension is most frequently encountered following high-energy fractures of the femur or extensive soft tissue trauma to the anterior aspect of the thigh. The resulting hematoma, prolonged immobilization, and subsequent inflammatory cascade lead to profound scarring and fibrosis of all or part of the quadriceps mechanism.
This rigid extension deformity is typically driven by a combination of four distinct pathoanatomical factors:
- Fibrosis of the Vastus Intermedius: The vastus intermedius muscle, due to its direct apposition to the anterior femur, is highly susceptible to post-traumatic scarring. It frequently fibroses and tethers the rectus femoris directly to the femur, obliterating the suprapatellar pouch and extending proximally along the femoral shaft.
- Patellofemoral Adhesions: Dense intraarticular and extraarticular adhesions form between the undersurface of the patella and the anterior femoral condyles, effectively welding the patellofemoral joint in place.
- Contracture of the Retinacular Expansions: The lateral and medial expansions of the vasti undergo severe fibrosis and shortening, adhering rigidly to the femoral condyles and preventing distal excursion of the patella.
- Shortening of the Rectus Femoris: In chronic cases, the rectus femoris muscle itself undergoes myostatic contracture and actual physical shortening, losing its native elasticity and excursion.
PREOPERATIVE PLANNING AND SOFT TISSUE OPTIMIZATION
The success of a quadricepsplasty or capsulotomy is heavily dependent on the viability of the surrounding soft tissue envelope. Patients with posttraumatic knee joint stiffness often present with compromised anterior thigh skin, adherent surgical scars, or split-thickness skin grafts directly overlying bone.
The Role of Free Tissue Transfers
In cases of severe soft tissue compromise, the use of free tissue transfers (such as an anterolateral thigh flap or latissimus dorsi flap) is highly recommended for soft tissue augmentation prior to, or concurrent with, the release procedure.
The integration of vascularized soft tissue serves several critical functions:
* Minimization of Wound Complications: It drastically reduces the risk of wound edge necrosis, wound dehiscence, and deep infection over the anterior knee.
* Facilitation of Early Rehabilitation: A robust, vascularized soft tissue envelope allows for the early initiation of aggressive postoperative physical therapy, which is the single most important determinant of functional outcome.
* Cosmesis: It provides a more acceptable cosmetic result by filling contour defects left by previous trauma or debridement.
Surgical Warning: Attempting a massive quadricepsplasty through thin, adherent, or irradiated skin without prior soft tissue optimization is a recipe for catastrophic wound dehiscence and secondary joint sepsis. Always respect the soft tissue envelope.
SURGICAL MANAGEMENT: QUADRICEPSPLASTY
Quadricepsplasty (such as the Thompson or Judet techniques) was specifically devised to correct extraarticular ankylosis in extension. The ultimate success of this procedure depends on three critical variables:
1. Whether the rectus femoris muscle has escaped irreversible structural injury.
2. How meticulously the rectus femoris can be isolated from the scarred, fibrotic components of the surrounding quadriceps mechanism.
3. How effectively the muscle can be rehabilitated and developed by active use postoperatively.
Step-by-Step Quadricepsplasty Principles
While specific techniques vary, the fundamental approach involves a systematic, sequential release of the tethering structures:
- Incision and Exposure: An extensile anterior midline incision is typically utilized. Full-thickness fasciocutaneous flaps are elevated to expose the entire extensor mechanism.
- Release of the Retinaculum: The medial and lateral retinacular expansions are incised, freeing the patella from its adherence to the femoral condyles.
- Excision of the Vastus Intermedius: The rectus femoris is carefully identified and separated from the underlying vastus intermedius. The fibrotic vastus intermedius, which often forms a dense scar mass tethering the rectus to the anterior femur, is radically excised.
- Mobilization of the Rectus Femoris: The rectus femoris is mobilized proximally to its origin if necessary. Care must be taken to preserve its neurovascular pedicle entering from the posterior aspect of the proximal third of the muscle.
ADJUNCTIVE TIBIAL TUBERCLE ELEVATION (MAQUET-TYPE PROCEDURE)
In cases where extraarticular ankylosis is complicated by severe patellofemoral arthrosis, or when the newly achieved flexion places excessive, destructive pressure on the patellofemoral joint, an adjunctive tibial tubercle elevation may be indicated. This procedure decompresses the patellofemoral joint by anteriorizing the extensor mechanism, thereby increasing the moment arm and reducing joint reactive forces.
Surgical Technique for Tubercle Elevation
- Osteotomy Preparation: Outline a tongue of bone incorporating the tibial tuberosity. The osteotomy should be sufficiently long to allow anterior levering without fracturing the distal cortical hinge.
- Executing the Cut: Leave the distal attachment of the tibial crest intact. The proximal and lateral cuts can be made with an oscillating saw, or by drilling multiple contiguous holes and connecting them with thin osteotomy cuts to prevent thermal necrosis and micro-fracture propagation.
- Bone Graft Harvesting: Through a separate incision, harvest a block of corticocancellous bone from the anterior iliac crest in the area of the iliac tubercle. The block should measure approximately 2.5 cm wide, 2.5 cm thick, and 5 cm long. Alternatively, structural structural allograft (bank bone) has been found to be just as satisfactory and eliminates donor-site morbidity.
- Tubercle Elevation: Carefully lever the tongue of bone and the tibial tuberosity anteriorly, away from the proximal tibia.
- Graft Insertion: Insert the prepared block of iliac or allograft bone beneath the elevated tuberosity at its most proximal extent. Prior to final insertion, trim the block of bone to approximately 2.5 cm on all sides to ensure a precise fit.
- Degree of Elevation: It is highly recommended to elevate the tibial tuberosity by only 1.5 cm. The major biomechanical decompression of the patellofemoral joint occurs within this initial amount of elevation. Exceeding 1.5 cm significantly increases the risk of skin necrosis, nonunion, and cosmetic deformity.
- Fixation: Usually, the inherent tension and pressure of the elevated tongue of tibial bone will hold the structural block securely in place. However, for further stability, a single 5 cm long stainless steel or titanium screw can be inserted as a lag screw through the tubercle and into the posterior tibial cortex.
- Management of Intraoperative Fractures: If the distal end of the tongue of bone inadvertently fractures from the tibial diaphysis during elevation, the hinge is lost. In this scenario, rigid internal fixation is mandatory; insert three bicortical screws along the length of the tongue to secure it to the tibia.
Pitfall: Over-elevation of the tibial tubercle (greater than 2.0 cm) places extreme tension on the overlying skin, frequently leading to wound edge necrosis and exposure of the hardware or bone graft. Strictly adhere to the 1.5 cm elevation rule.
Prophylactic Anterior Compartment Fasciotomy
Following the elevation of the tibial tubercle, the biomechanics and fascial tension of the anterior leg are altered. To prevent postoperative compartment syndrome, it is imperative to perform a prophylactic anterior compartment fasciotomy. This is done by longitudinally releasing the fascia of the anterior compartment adjacent to the tibial crest.
WOUND CLOSURE AND DRAINAGE
Meticulous hemostasis is critical, as the extensive soft tissue release creates a massive dead space prone to hematoma formation.
- Tissue Undermining: Undermine the subcutaneous tissues extensively, if necessary, to allow the skin edges to approximate without tension. If tension is unavoidable, reconsider the need for a local or free flap.
- Drainage: Insert a large-bore suction drain deep under the subcutaneous tissue and muscle flaps to evacuate postoperative bleeding and reduce the risk of arthrofibrosis recurrence driven by hematoma organization.
- Closure: Close the wound in layers using non-reactive sutures.
POSTOPERATIVE CARE AND REHABILITATION PROTOCOL
The surgical release of an extraarticular ankylosis is only the first step in treatment; the ultimate functional outcome is dictated by the postoperative rehabilitation phase. The primary goal is to maintain the intraoperatively achieved range of motion while protecting the extensor mechanism repair and any osteotomies.
Immediate Postoperative Phase (Days 0-14)
- Immobilization: Immediately postoperatively, the extremity is placed in a rigid knee immobilizer splint to protect the wound and allow initial soft tissue resting.
- Weight-Bearing: The patient is allowed to bear weight to tolerance using crutches starting on the first postoperative day. Early weight-bearing stimulates proprioception and bone healing (especially if a tubercle osteotomy was performed).
- Muscle Activation: Quadriceps isometric exercises, straight leg-lifting exercises, and calf raises are initiated on postoperative day one. Preventing quadriceps inhibition is paramount.
Intermediate Phase (Weeks 2-6)
- Range of Motion (ROM): Active and active-assisted range-of-motion exercises are initiated once the surgical wound has definitively healed, which is usually at the 2-week mark.
- Continuous Passive Motion (CPM): The use of a CPM machine can be highly beneficial during this phase to prevent the reformation of intraarticular and extraarticular adhesions.
- Duration of Immobilization: The use of the knee immobilizer should be progressively weaned. Total immobilization time should not exceed 6 weeks, as prolonged static positioning will inevitably lead to recurrent ankylosis.
Late Phase (Weeks 6 and Beyond)
- Strengthening: Once full active ROM is achieved and the osteotomy (if performed) shows radiographic signs of union, aggressive progressive resistance exercises are introduced.
- Functional Training: Focus shifts to closed kinetic chain exercises, gait normalization, and return to activities of daily living.
Clinical Pearl: Adequate pain control is the linchpin of successful rehabilitation following quadricepsplasty. Consider the use of continuous epidural analgesia or indwelling peripheral nerve catheters (e.g., adductor canal blocks) for the first 48 to 72 hours to allow the patient to tolerate early, aggressive mobilization.
CONCLUSION
The management of extraarticular ankylosis of the knee requires a profound understanding of extensor mechanism pathoanatomy and meticulous surgical execution. Whether performing an isolated quadricepsplasty or combining it with an adjunctive tibial tubercle elevation, the surgeon must balance aggressive soft tissue release with the preservation of the soft tissue envelope. Through precise surgical technique, appropriate use of structural bone grafts, and a rigorous, early-mobilization rehabilitation protocol, surgeons can successfully restore functional mobility to the severely stiff knee.
You Might Also Like