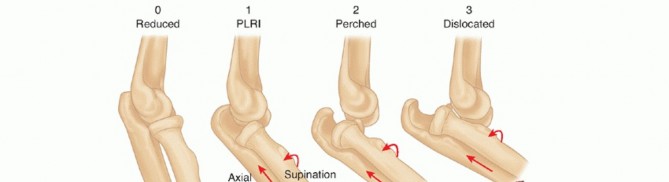
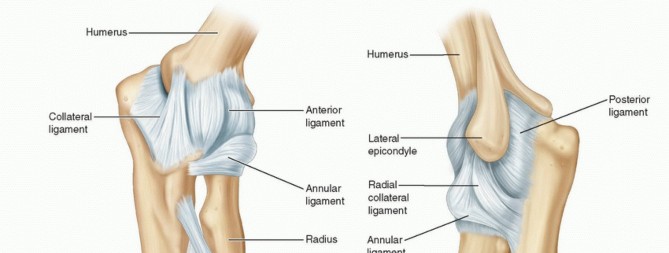
Rotator Cuff Arthropathy: A Comprehensive Clinical & Imaging Diagnosis Case Study
Key Takeaway
Rotator Cuff Arthropathy (RCA) is diagnosed by chronic shoulder pain, progressive pseudoparalysis, and specific clinical signs. Key findings include supraspinatus/infraspinatus atrophy, significant active ROM loss with preserved passive ROM, positive external rotation lag and drop arm tests. Radiographs confirm superior humeral head migration, acromiohumeral interval narrowing, and glenohumeral joint space narrowing, often with acromial erosion.
Patient Presentation & History
A 72-year-old male presented with a chief complaint of chronic, progressive left shoulder pain and significant functional impairment for the past three years. He described the pain as a deep, aching sensation, worse with any active movement, especially elevation and external rotation, and frequently disrupting his sleep. The pain was recalcitrant to over-the-counter analgesics, oral anti-inflammatories, and three prior subacromial corticosteroid injections administered over the last 18 months.
His functional limitations included an inability to lift his arm above shoulder height, difficulty reaching overhead, putting on a coat, and performing personal hygiene activities such as washing his hair or reaching his back pocket. He reported a gradual onset of weakness, progressively worsening to a "pseudoparalysis" of the left shoulder, where he felt he could not actively lift his arm despite his best efforts. There was no history of acute trauma. He denied any radiating pain or neurological deficits in the ipsilateral limb.
His past medical history included well-controlled hypertension, Type 2 Diabetes Mellitus managed with oral agents, and hyperlipidemia. He was a former smoker (quit 10 years ago, 30 pack-year history) and had no history of prior shoulder surgery on the affected side. He was retired and lived independently, but his shoulder condition severely impacted his ability to perform daily tasks and hobbies.
Clinical Examination
General Inspection:
The patient appeared to be in mild distress due to chronic pain. Inspection of the left shoulder revealed subtle atrophy of the supraspinatus and infraspinatus fossae, consistent with chronic rotator cuff pathology. There was a notable prominence of the acromion, and the humeral head appeared to sit more superiorly within the glenohumeral joint compared to the contralateral side. No obvious skin changes, scars, or swelling were noted. Scapular dyskinesis was evident during active movement attempts, with excessive scapular elevation and protraction ("shrug" sign) compensating for glenohumeral motion.
Palpation:
Palpation elicited tenderness over the anterior and lateral aspects of the acromion, the greater tuberosity, and the anterior glenohumeral joint line. No palpable warmth or significant swelling was present. There was palpable crepitus during passive range of motion. The biceps groove was non-tender. The acromioclavicular (AC) joint was non-tender to direct palpation.
Range of Motion (ROM):
*
Active Range of Motion (AROM):
* Forward Flexion: 60 degrees (contralateral 170 degrees)
* Abduction: 50 degrees (contralateral 170 degrees), demonstrating the characteristic "shrug" sign with marked compensatory scapulothoracic motion.
* External Rotation: 10 degrees with the arm adducted (contralateral 60 degrees)
* Internal Rotation: Reached the buttock (contralateral T7 level)
*
Passive Range of Motion (PROM):
* Forward Flexion: 120 degrees
* Abduction: 110 degrees
* External Rotation: 30 degrees with the arm adducted
* Internal Rotation: Reached T10 level
* The discrepancy between active and passive range of motion, particularly for abduction and forward flexion, was significant and indicative of rotator cuff pathology leading to pseudoparalysis. Secondary stiffness was also evident as PROM was not completely full.
Strength Testing (against resistance):
*
Abduction (Supraspinatus):
Grade 1/5 (flicker of deltoid activity, unable to lift against gravity)
*
External Rotation (Infraspinatus/Teres Minor):
Grade 1/5
*
Internal Rotation (Subscapularis):
Grade 3/5 (weak against resistance, but able to move against gravity)
*
Forward Flexion (Anterior Deltoid):
Grade 2/5
*
Elbow Flexion (Biceps):
Grade 5/5
*
Elbow Extension (Triceps):
Grade 5/5
* Specific rotator cuff tests:
*
External Rotation Lag Sign:
Positive (unable to hold the arm in passively achieved external rotation).
*
Drop Arm Test:
Positive (unable to slowly lower the arm from 90 degrees abduction).
*
Lift-off Test (Subscapularis):
Negative (patient could perform, indicating relatively preserved subscapularis function compared to the posterior cuff).
*
Belly-Press Test (Subscapularis):
Positive (elbow fell back with press).
Special Tests:
*
Neer's Impingement Sign:
Positive and painful.
*
Hawkins-Kennedy Impingement Sign:
Positive and painful.
*
AC Joint Compression Test:
Negative.
*
Speed's Test (Biceps Tendon):
Negative.
*
Yergason's Test (Biceps Tendon):
Negative.
Neurological Assessment:
Sensation to light touch was intact in the C5-T1 dermatomes. Motor strength in distal upper extremity muscle groups was 5/5. Deep tendon reflexes (biceps, brachioradialis, triceps) were 2+ bilaterally and symmetrical. There was no evidence of axillary nerve palsy, which can be seen in chronic superior migration with traction.
Vascular Assessment:
Radial and ulnar pulses were 2+ bilaterally and symmetrical. Capillary refill was prompt in all digits.
Imaging & Diagnostics
Plain Radiographs:
Standard shoulder radiographs (AP, true AP/Grashey, axillary lateral, outlet views) were obtained. These revealed significant findings characteristic of rotator cuff arthropathy (RCA):
*
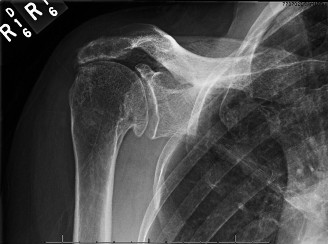
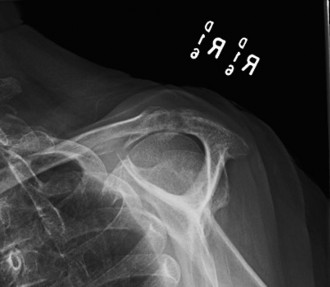
AP View:
Marked superior migration of the humeral head with severe narrowing of the acromiohumeral interval, measuring approximately 2mm (normal > 7mm). There was evidence of glenohumeral joint space narrowing, particularly superiorly. Significant osteophyte formation was present around the glenoid rim and humeral head. Scalloping and acetabularization of the undersurface of the acromion and coracoacromial arch were visible, a direct consequence of the chronically superiorly migrated humeral head eroding the arch. Subchondral sclerosis and cystic changes were noted on both the humeral head and glenoid.
*
*
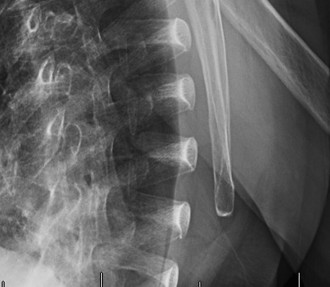
Interpretation of the provided image
: This X-ray appears to be an AP view of a shoulder demonstrating classic features of severe rotator cuff arthropathy (Hamada Grade 4 or 5). Key findings include: severe superior migration of the humeral head with obliteration of the acromiohumeral interval, marked glenohumeral joint space narrowing, large superior osteophytes on the glenoid, and acetabularization of the acromion. There is also evidence of cystic changes and sclerosis in the humeral head.
Magnetic Resonance Imaging (MRI):
An MRI of the left shoulder was performed to further evaluate the soft tissue structures, particularly the rotator cuff, biceps tendon, and cartilage.
*
Rotator Cuff:
Confirmed a massive, irreparable rotator cuff tear involving the supraspinatus, infraspinatus, and teres minor tendons, with significant retraction to the glenoid level. There was severe fatty infiltration of the supraspinatus and infraspinatus muscles (Goutallier Grade 3-4), indicative of chronic denervation and atrophy, precluding a direct repair. The subscapularis tendon showed thinning and partial delamination but was not completely ruptured or severely retracted.
*
Humeral Head Migration:
Reiterated the superior migration of the humeral head, eroding the undersurface of the acromion.
*
Glenohumeral Joint:
Demonstrated diffuse cartilage loss, particularly in the superior and posterior aspects of the glenoid and corresponding humeral head, consistent with advanced degenerative changes. Minimal joint effusion was noted.
*
Biceps Tendon:
The long head of the biceps tendon appeared dislocated and partially degenerated within the bicipital groove.
*

*
Interpretation of the provided image
: This image appears to be a coronal or sagittal MRI slice through a shoulder, clearly depicting a massive rotator cuff tear. We can observe: a large gap where the supraspinatus tendon should be inserting onto the greater tuberosity, significant retraction of the muscle belly, and possibly fatty infiltration (though difficult to definitively grade from a single image without comparison sequences). The superior humeral head migration seen on X-ray would be the consequence of this long-standing, irreparable tear.
Computed Tomography (CT) Scan:
Given the advanced changes on plain radiographs and the consideration for reverse total shoulder arthroplasty (RTSA), a dedicated CT scan of the glenoid was obtained to precisely assess glenoid bone stock, morphology, and retroversion.
*
Glenoid Morphology:
Revealed severe superior and posterior glenoid erosion with significant eccentric wear, resulting in a B2 or C-type glenoid according to the Walch classification, characterized by severe posterior erosion and retroversion. The erosion compromised a significant portion of the superior and posterior glenoid bone stock, necessitating careful preoperative planning for glenoid baseplate fixation and potential bone grafting.
*
Humeral Head:
Confirmed severe degenerative changes and cystic lesions.
*

*
Interpretation of the provided image
: This image appears to be a post-operative AP X-ray of a shoulder following Reverse Total Shoulder Arthroplasty (RTSA). We can clearly see the components: a humeral stem with a polyethylene cup and a glenosphere affixed to the glenoid, superiorly offset and slightly inferiorly positioned. This image is crucial for demonstrating the definitive surgical treatment for Rotator Cuff Arthropathy.
Laboratory Investigations:
Erythrocyte Sedimentation Rate (ESR) and C-Reactive Protein (CRP) were within normal limits, ruling out an acute inflammatory or infectious process. A complete blood count (CBC) was unremarkable. HbA1c was slightly elevated at 7.2%, indicating suboptimal diabetic control, which was discussed with the patient and his endocrinologist for optimization prior to surgery.
Differential Diagnosis
The clinical presentation and imaging findings strongly point towards Rotator Cuff Arthropathy. However, it is essential to consider other conditions that can cause shoulder pain and dysfunction.
| Feature | Rotator Cuff Arthropathy (RCA) | Adhesive Capsulitis (Frozen Shoulder) | Primary Glenohumeral Osteoarthritis (GHOA) | Cervical Radiculopathy (C5/C6) |
|---|---|---|---|---|
| Pathophysiology | Chronic massive irreparable rotator cuff tear leading to superior migration of humeral head and secondary glenohumeral arthrosis | Idiopathic inflammatory fibrosis and contracture of the glenohumeral joint capsule | Degenerative cartilage loss and osteophyte formation without massive rotator cuff tear | Nerve root compression (e.g., disc herniation, spondylosis) leading to referred pain & weakness |
| Onset | Insidious, progressive over years, often history of chronic cuff pain | Insidious, often no clear precipitating event, progressive "freezing" phase | Insidious, progressive over years, often activity-related | Acute (e.g., whiplash, disc herniation) or insidious (e.g., spondylosis) |
| Chief Complaint | Chronic pain, marked weakness ("pseudoparalysis"), inability to elevate arm actively, night pain | Global shoulder pain, stiffness, significant restriction of active AND passive ROM | Deep aching pain, stiffness, crepitus, activity-related pain | Neck pain radiating to shoulder/arm, numbness, tingling, weakness in specific myotomes |
| Active ROM | Severely limited (especially abduction, ER), "shrug" sign; significant active-passive discrepancy | Severely restricted in all planes (ER > Abduction > IR/Flexion pattern) | Restricted, painful, especially rotation and elevation | Often full or pain-limited shoulder ROM, but limited neck ROM; weakness in specific myotomes |
| Passive ROM | Often better than active, but can be restricted with secondary stiffness (capsular tightness) | Severely restricted in all planes ("capsular pattern") | Restricted, painful, especially rotation and elevation | Full shoulder PROM |
| Strength Testing | Marked weakness (Grade 1-2/5 for abduction/ER); positive lag signs and drop arm | Pain-limited strength, but intrinsic muscle strength often preserved; no true rotator cuff weakness | Pain-limited strength, but rotator cuff usually intact and strong | Weakness corresponds to specific myotomes (e.g., C5-C6 for deltoid, biceps, wrist extensors) |
| Imaging (X-ray) | Superior humeral head migration (A-H interval < 7mm), glenohumeral joint space narrowing, acetabularization of acromion, osteophytes, erosions | Normal or mild osteopenia; no superior migration or significant arthritis | Inferior humeral head migration, concentric or eccentric joint space narrowing, osteophytes, subchondral sclerosis/cysts | Normal shoulder X-rays; cervical spine X-rays may show degenerative changes |
| Imaging (MRI) | Massive, irreparable rotator cuff tear, severe fatty infiltration, cartilage loss, superior migration, +/- biceps pathology | Thickened joint capsule, loss of axillary recess; intact rotator cuff and cartilage (early stages) | Cartilage loss, osteophytes, often intact rotator cuff; no superior migration | Normal shoulder MRI; cervical spine MRI shows nerve root compression |
| Key Differentiating Feature | Superior humeral head migration + massive irreparable RCT + secondary arthrosis | Global restriction of active and passive ROM in all planes (capsular pattern) | Intact rotator cuff + concentric joint space narrowing + osteophytes | Referred pain pattern, dermatomal sensory changes, specific myotomal weakness, normal shoulder imaging |
Surgical Decision Making & Classification
The patient's advanced age, chronic and progressive nature of pain, severe functional limitation (pseudoparalysis), and radiographic evidence of massive, irreparable rotator cuff tear with advanced glenohumeral arthropathy (Rotator Cuff Arthropathy, RCA) strongly indicated the failure of conservative management. The presence of significant superior humeral head migration, glenoid erosion, and fatty infiltration of the rotator cuff muscles (Goutallier Grade 3-4 on MRI) effectively ruled out primary rotator cuff repair or alternative procedures like latissimus dorsi transfer as viable options for restoring function and providing lasting pain relief.
Hamada Classification (Radiographic assessment of RCA):
Based on the plain radiographs, the patient's shoulder demonstrated:
* Grade 1: AC interval > 6 mm.
* Grade 2: AC interval < 6 mm.
* Grade 3: Acetabularization of the acromion.
* Grade 4: Glenohumeral arthritis (4A – no humeral head collapse, 4B – humeral head collapse).
* Grade 5: Humeral head collapse with avascular necrosis (AVN).
Our patient's findings of severe superior migration with an acromiohumeral interval of 2mm, marked acetabularization of the acromion, and significant glenohumeral joint space narrowing with osteophytes and cystic changes, placed him squarely in Hamada Grade 4A (or possibly 4B depending on exact definition of collapse), indicating advanced RCA.
Surgical Indication:
Given the patient's symptomatic Hamada Grade 4A RCA, severe pseudoparalysis, and failure of comprehensive non-operative treatment, the gold standard surgical intervention is
Reverse Total Shoulder Arthroplasty (RTSA)
. RTSA fundamentally alters the biomechanics of the shoulder, moving the center of rotation medially and inferiorly. This change allows the deltoid muscle, which is typically preserved in RCA, to become the primary elevator and abductor of the arm, compensating for the deficient rotator cuff.
Glenoid Classification (Pre-operative CT assessment for RTSA):
The preoperative CT scan was critical for assessing the glenoid bone stock, which is paramount for successful RTSA. The glenoid erosion pattern was classified using the
Seebauer Classification
and implicitly, the
Walch Classification
for primary osteoarthritis, which provides insights into glenoid retroversion and wear patterns relevant to RTSA.
*
Walch Classification (for glenoid retroversion and wear):
* Type A: Centered glenoid wear.
* A1: Centered wear, no retroversion.
* A2: Centered wear, some retroversion, but posterior subluxation is reducible.
* Type B: Posterior glenoid wear and retroversion.
* B1: Posterior erosion, often minimal retroversion.
* B2: Biconcave glenoid with significant posterior erosion and retroversion, difficult to correct.
* B3: Severe posterior glenoid bone loss.
* Type C: Dysplastic glenoid with severe retroversion (>25 degrees).
Our patient's CT findings of severe superior and posterior glenoid erosion with significant eccentric wear and retroversion corresponded most closely to a Walch Type B2 or B3 glenoid . This presented a significant challenge for glenoid baseplate fixation and necessitated specific surgical considerations for correction of the retroversion and management of bone defects to ensure stable and well-positioned implant components. These findings further solidified the decision for RTSA, as it offers the most reliable solution for managing complex glenoid pathology in the setting of RCA.
Non-Operative vs. Operative Considerations:
Non-operative management had been exhausted. Continued conservative care would lead to ongoing pain, progressive functional decline, and potential further bone loss. The patient's functional demands, while not exceptionally high (retired), were significant enough to warrant improvement in activities of daily living. No absolute contraindications to surgery (e.g., active infection, deltoid insufficiency, paralyzed axillary nerve) were identified, though diabetes control needed optimization.
Surgical Technique / Intervention
The definitive procedure chosen was a Reverse Total Shoulder Arthroplasty (RTSA) .
1. Patient Positioning and Anesthesia:
The patient was placed in a modified beach chair position under general anesthesia with interscalene block for post-operative pain management. The left upper extremity was prepped and draped freely to allow for full intraoperative range of motion assessment. Adequate padding was applied to all pressure points.
2. Surgical Approach:
A standard deltopectoral approach was utilized.
* An incision was made from the posterior aspect of the acromion extending inferomedially towards the deltoid insertion.
* The interval between the deltoid and pectoralis major muscles was identified. The cephalic vein was identified and typically retracted laterally with the deltoid.
* The clavipectoral fascia was incised, and the conjoined tendon (coracobrachialis and short head of biceps) was identified and retracted medially.
* The subscapularis tendon was identified. In this case of massive RCA, the subscapularis was often found to be thinned or partially torn, but usually less severely retracted than the superior cuff. Its repair potential was assessed. The superior capsule was released, and extensive adhesions were meticulously dissected to allow for adequate exposure and mobility.
* The humeral head was dislocated anteriorly, bringing it out of the glenoid.
3. Humeral Head Resection:
* Osteophytes around the humeral head were carefully removed.
* A humeral head cutting guide was used to perform a precise osteotomy of the humeral head, typically at an angle of 155 degrees to match the prosthesis's neck-shaft angle, ensuring adequate bone removal while preserving as much of the humeral metaphysis as possible for stem fit. The humeral head was then removed and sent for pathological examination.
4. Glenoid Preparation and Baseplate Implantation:
This is a critical step in RTSA, especially with a Walch B2/B3 glenoid.
* The glenoid fossa was meticulously exposed, and any remaining articular cartilage, fibrous tissue, and osteophytes were removed to reveal bleeding subchondral bone.
* Central drilling for the baseplate peg was performed. Given the superior and posterior erosion and retroversion, careful reaming was performed to correct retroversion and achieve an optimal perpendicular orientation of the glenoid face relative to the scapular spine, or aiming for slight inferior tilt (5-10 degrees) to reduce scapular notching. Bone grafting (autograft or allograft) was considered and employed if severe glenoid defects persisted after initial reaming, to provide a stable, concentric platform for the baseplate. In this case, a structural allograft wedge was utilized to augment the posterior glenoid and restore version.
* A glenoid baseplate trial was inserted to assess fit, stability, and potential notching.
* The definitive glenoid baseplate was then implanted, usually a central compression peg with multiple peripheral locking screws. The screws were directed to engage the dense bone of the scapular spine and lateral scapular pillar for maximum purchase and stability.
* The glenosphere (typically a 36-42mm sphere) was then affixed to the baseplate. Careful attention was paid to its eccentric positioning – usually inferiorly and slightly lateralized – to optimize deltoid tension, reduce impingement with the scapular neck, and improve range of motion.
5. Humeral Stem Implantation:
* The humeral canal was prepared using sequential reamers and broaches to match the chosen humeral stem size.
* The definitive humeral stem was then implanted. For this patient, a cementless metaphyseal-sparing stem was chosen for its ability to preserve bone stock and facilitate future revisions if necessary.
* A trial humeral polyethylene liner (often 0-8mm offset) was attached to the trial stem. The choice of offset and thickness was critical for optimizing soft tissue tension and stability.
6. Reduction and Stability Assessment:
* The humeral component was reduced onto the glenosphere.
* The shoulder was taken through a full range of motion to assess stability, impingement, and deltoid tension. Particular attention was paid to avoiding hyperextension with internal rotation, which can be a common dislocation mechanism in RTSA. Impingement with the inferior scapular neck (scapular notching) was assessed and adjusted by optimizing glenosphere position and humeral offset.
7. Closure:
* The wound was irrigated thoroughly.
* The subscapularis was repaired if tissue quality allowed, or a superior capsule reconstruction could be considered using dermal allograft, though not routinely performed in all RTSA cases. In this patient, given the poor quality, direct repair was not possible, but the deltopectoral interval was closed.
* The deltopectoral interval was loosely approximated, and the subcutaneous tissues and skin were closed in layers. A drain was typically placed and removed post-operatively.
Post-Operative Protocol & Rehabilitation
The post-operative rehabilitation protocol for RTSA is critical for successful outcomes, focusing on protecting the implant, allowing soft tissue healing, and gradually restoring functional range of motion and strength.
Phase I: Immobilization and Early Passive Motion (0-6 weeks)
- Immobilization: The arm was placed in a sling with an abduction pillow for 4-6 weeks to protect the deltoid repair (if applicable) and other soft tissues. The sling was removed only for hygiene and exercises.
- Pain Management: Opioid and non-opioid analgesics, as well as the preoperative interscalene block, were used to manage pain.
-
Early Passive Range of Motion (PROM):
- Pendulum Exercises: Initiated on Post-operative Day 1, focusing on gravity-assisted circular motions.
- External Rotation: Gentle PROM in the scapular plane, maintaining the elbow close to the body, typically to 0-30 degrees of external rotation.
- Forward Flexion/Elevation: Assisted PROM in the scapular plane, limited to 90-120 degrees, to avoid excessive deltoid stretch or stress on the implant-bone interface.
- Internal Rotation: Gentle PROM, avoiding combined adduction and internal rotation initially.
- Scapular Stabilization: Gentle scapular retraction and depression exercises without shoulder movement.
- Elbow/Wrist/Hand ROM: Active exercises to prevent stiffness.
- Weight Bearing: No weight bearing through the operative arm.
- Restrictions: NO active range of motion of the shoulder. No lifting, pushing, or pulling. Avoid hyperextension and combined adduction/internal rotation.
Phase II: Active Assisted and Gentle Active Motion (6-12 weeks)
- Sling Discontinuation: The sling was typically discontinued around 6 weeks post-op, or when adequate deltoid control was demonstrated.
-
Active Assisted Range of Motion (AAROM):
- Progressive AAROM exercises using the non-operative arm or a pulley system for forward flexion, abduction, and rotation.
-
Gentle Active Range of Motion (AROM):
- Initiation of gentle AROM for shoulder flexion, abduction, and rotation as tolerated, focusing on deltoid activation.
-
Light Isometric Strengthening:
- Isometrics for the deltoid and periscapular muscles against light resistance, avoiding impingement positions.
-
Scapular Strengthening:
- Progressive exercises for scapular protractors and retractors (e.g., rows, push-ups against a wall).
- Restrictions: Continue to avoid heavy lifting, pushing, pulling. Avoid provocative positions that could lead to dislocation (e.g., combined adduction, internal rotation, and hyperextension).
Phase III: Strengthening and Functional Activities (12+ weeks)
-
Progressive Strengthening:
- Introduction of light resistance exercises using resistance bands or light weights for deltoid, biceps, and periscapular muscles.
- Focus on functional strengthening patterns.
-
Functional Activities:
- Gradual return to light activities of daily living.
- Emphasis on proper body mechanics.
-
Advanced ROM:
- Continued progression of AROM to maximize functional overhead reach and rotational capabilities within the limits of the prosthesis and soft tissues.
-
Return to Activity:
- Low-impact activities like walking, swimming (avoiding aggressive strokes), and golf (gentle swings) can be gradually introduced. High-impact sports or heavy overhead lifting are generally discouraged due to the risk of implant complications and accelerated wear.
Expected Outcomes:
Patients undergoing RTSA for RCA typically experience significant pain relief and improved active range of motion, particularly forward flexion and abduction, often achieving functional arcs sufficient for most activities of daily living (e.g., 120-140 degrees of active elevation). Rotational range, particularly internal rotation, may remain somewhat limited.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Diagnosis Recognition: Rotator Cuff Arthropathy (RCA) should be high on the differential for an elderly patient presenting with chronic shoulder pain, pseudoparalysis (active-passive discrepancy in ROM), and superior humeral head migration on plain radiographs. Hamada classification is key for grading severity and guiding treatment.
- Preoperative Imaging: A dedicated CT scan of the glenoid is mandatory for surgical planning of RTSA to precisely assess glenoid bone stock, version, and wear patterns (e.g., Walch/Seebauer classifications). This guides baseplate placement and identifies the need for bone grafting.
- Reverse Total Shoulder Arthroplasty (RTSA): This is the gold standard for symptomatic RCA. It changes the center of rotation, allowing the deltoid to become the primary elevator, effectively compensating for an irreparable rotator cuff.
- Glenoid Preparation: Achieving a stable and concentric glenoid base for the baseplate is paramount. In cases of severe eccentric wear (Walch B2/B3 or C glenoid), bone grafting (autograft or allograft) or specific reaming techniques are essential to restore proper glenoid version and provide robust fixation.
-
Inferior and Lateral Glenosphere Placement:
Positioning the glenosphere as inferiorly as possible and using a lateralized glenosphere or lateralizing humeral offset is crucial. This helps to:
- Reduce impingement of the humeral component on the inferior scapular neck (scapular notching).
- Increase deltoid tension, improving active range of motion and stability.
- Increase the effective moment arm of the deltoid.
- Soft Tissue Balancing: Careful soft tissue release and balancing during surgery are necessary to optimize implant stability and range of motion. Adhesions are often extensive in chronic RCA.
- Axillary Nerve Protection: Maintain vigilance for the axillary nerve, which runs just inferior to the inferior glenoid. It is at risk during inferior glenoid exposure, reaming, and screw placement.
- Post-operative Rehabilitation: Adherence to a structured, gradual rehabilitation protocol is critical. Early PROM protects soft tissue healing, while progressive strengthening activates the deltoid and periscapular muscles. Avoidance of specific dislocation-prone positions (e.g., combined adduction, internal rotation, and hyperextension) is vital.
Pitfalls:
- Misdiagnosis: Confusing RCA with adhesive capsulitis or primary glenohumeral osteoarthritis can lead to inappropriate treatment. Differentiate by the active-passive ROM discrepancy, imaging findings of superior migration/massive tear (RCA), global active and passive ROM restriction (AC), or preserved rotator cuff (GHOA).
- Inadequate Glenoid Bone Stock: Attempting RTSA on a severely deficient glenoid without adequate bone augmentation will lead to baseplate loosening, failure, and poor outcomes. Preoperative CT is non-negotiable.
- Axillary Nerve Injury: Iatrogenic injury to the axillary nerve can result in deltoid paralysis, severely compromising the function of an RTSA. Careful surgical dissection and protection are essential.
- Scapular Notching: This is the most common radiographic complication of RTSA, caused by impingement of the humeral polyethylene liner on the inferior scapular neck. It can lead to wear debris, pain, and eventual implant loosening. Preventative measures include inferior glenosphere positioning, lateralization, and appropriate implant sizing.
- Dislocation: While less common with RTSA than anatomic TSA, dislocation can occur, especially with specific movements (adduction, internal rotation, hyperextension) or poor soft tissue tensioning. This is a devastating complication.
- Infection: As with any arthroplasty, periprosthetic joint infection (PJI) is a severe complication, especially challenging in the shoulder due to deep soft tissue planes and proximity to neurovascular structures. Meticulous sterile technique and appropriate prophylactic antibiotics are crucial.
- Humeral Fracture (Intraoperative/Periprosthetic): Can occur during humeral canal preparation or post-operatively, requiring additional fixation or revision.
- Poor Deltoid Function: If the deltoid muscle is compromised (e.g., from prior surgery, trauma, or axillary nerve palsy), RTSA will fail as it relies on a functional deltoid for elevation. This is an absolute contraindication.
- Failure to Address Cervical Spine Pathology: Co-existing cervical radiculopathy can mimic or exacerbate shoulder pain. It's important to rule out significant cervical spine pathology before proceeding with shoulder surgery, especially if symptoms are atypical.
Clinical & Radiographic Imaging
You Might Also Like